Palmaris Brevis Spasm Syndrome
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Hemimasticatory Spasm Treated with Botulinum Toxin
Arq Neuropsiquiatr 2002;60(2-A):288-289 HEMIMASTICATORY SPASM TREATED WITH BOTULINUM TOXIN Case report Hélio A.G. Teive1, Élcio J. Piovesan2, Francisco M.B. Germiniani3, Carlos Henrique A. Camargo3, Daniel Sá3, Rosana H. Scola4, Lineu C. Werneck5 ABSTRACT - We describe a female patient with hemimasticatory spasm, a rare movement disorder due to dysfunction of the motor trigeminal nerve of unknown origin. This patient had an excellent response to botulinum toxin therapy. KEY WORDS: hemimasticatory spasm, paroxysmal spasms, botulinum toxin. Espasmo hemimastigatório tratado com toxina botulínica: relato de caso RESUMO - Relatamos o caso de paciente feminina com espasmo hemimastigatório, distúrbio do movimento raro decorrente de disfunção da porção motora do nervo trigeminal, de etiologia desconhecida. A paciente teve excelente resposta clínica ao tratamento com toxina botulínica. PALAVRAS-CHAVE: espasmo hemimastigatório, espasmos paroxísticos, toxina botulínica. Hemimasticatory spasm (HMS) represents a rare spontaneously. She also complained of difficulty in talk- movement disorder due to a dysfunction of the mo- ing and swallowing when she had the spasms. tor trigeminal nerve of unknown origin. It is frequen- Neurological examination was normal except for in- tly misdiagnosed as hemifacial spasm, which is a tense contraction of the masseter and temporal muscles disorder due to dysfunction of the facial nerve1-3. on the right with severe facial pain when the patient had the spasms. Routine laboratory tests (WBC, biochemistry, The most striking features of HMS are the excruciat- VDRL, ERS) and ceruloplasmine were all normal. ing pain that accompanies the spasm itself and the The patient also had a previous history of irregular fact that initially masticatory movements act as a menstrual cycles and even amenorrhea for more than 1-3 trigger for the spasm . -

Perioral Twitching During Smiling - a Rare Form of Essential Tremor
Clinical Video Neurological Case Reports Published: 02 Dec, 2020 Perioral Twitching during Smiling - A Rare form of Essential Tremor Lea Pollak* Department of Neurology, Neurological Clinic, Kupat Cholim Macabi, Israel Abstract Involuntary movements of facial muscles such as jaw tremor, oromandibular dyskinesia, dystonia, facial myoclonus or hemifacial spasm are common in clinical practice. A 52-year old woman with a 15 year history of upper limb tremor complained of recent spread of the tremor to her face. On examination a moderate kinetic and action, mildly asymmetric tremor of the arms was present. On voluntary and spontaneous smiling bilateral twitching of the buccal muscles was observed. Keywords: Periorbital twitching; Essential tremor; Tardive dyskinesia Introduction Involuntary movements of facial muscles such as jaw tremor, oromandibular dyskinesia, dystonia, facial myoclonus or hemifacial spasm are common in clinical practice. Isolated tremor induced by mild contraction of smiling muscles smiling tremor is extremely rare and was reported by some authors to be associated with Parkinson disease while others related this condition to essential tremor [1-3]. Clinical Video A 52-year old woman with a 15 year history of upper limb tremor complained of recent spread of the tremor to her face. Her medical history comprised Crohn's disease treated with adalimumab and depression treated with sertraline and perphenazine during the last ten years. On examination a moderate kinetic and action, mildly asymmetric tremor of the arms was present. On voluntary and spontaneous smiling bilateral twitching of the buccal muscles was observed (video 1). The twitching disappeared on rest and forced smiling. There were no extra pyramidal signs or involuntary OPEN ACCESS movements of the jaw, lips or tongue (Figure 1). -

Isolated Corpus Callosal Infarction Secondary to Pericallosal Artery Disease Presenting As Alien Hand Syndrome N C Suwanwela, N Leelacheavasit
533 J Neurol Neurosurg Psychiatry: first published as 10.1136/jnnp.72.4.536 on 1 April 2002. Downloaded from SHORT REPORT Isolated corpus callosal infarction secondary to pericallosal artery disease presenting as alien hand syndrome N C Suwanwela, N Leelacheavasit ............................................................................................................................. J Neurol Neurosurg Psychiatry 2002;72:533–536 held a paper with both hands, the left hand would try to pull Two patients are described with the callosal type of alien the paper against the right. Some actions indicating mirror hand syndrome. Both presented with abnormal feelings in movement were also seen. For example, when he moved his the left upper limb and intermanual conflict without clinical right hand backwards, he felt that the left hand was pulled evidence of callosal apraxia or frontal lobe dysfunction back in the same manner. On examination, he was alert. such as motor deficit or reflexive grasping. Imaging studies Motor power of the arms and legs was full. There was no pin- disclosed subacute infarction in the body and splenium of prick sensory loss or inattention, on double simultaneous the corpus callosum due to pericallosal artery disease. stimulation test. Proprioceptive sense was normal. He could These patients were unique in their presentation as a not identify his left hand fingers or objects placed in his left callosal type of alien hand syndrome secondary to ischae- hand with his eyes closed, but was able to do so under visual mic stroke. observation. There was no apraxia of the left hand on verbal command, in imitation, and in actual object use. Frontal lobe releasing signs such as reflexive grasping, palmomental reflex, and snout reflex were absent. -

Intrinsic Hand Muscles of the Japanese Monkey, Macaca Fuscata
Anthropol.Sci. 102(Suppl.), 85-95,1994 Intrinsic Hand Muscles of the Japanese Monkey, Macaca fuscata TOSHIHIKO HOMMA AND TATSUO SAKAI Department of Anatomy, School of Medicine, Juntendo University, Hongo 2-1-1, Bunkyo-ku, Tokyo 113, Japan Received December 24, 1993 •ôGH•ô Abstract•ôGS•ô Anatomy of the intrinsic hand muscles in the Japanese monkeys was studied with an improved method to dissect the muscles and nerves in water after removal of the skeletal framework. The thenar eminence contained four muscles, namely m. abductor pollicis brevis, m. opponens pollicis, m, flexor pollicis brevis, and m. adductor pollicis. The hypothenar eminence contained four muscles, namely m. palmaris brevis, m. abductor digiti minimi, m. flexor digiti minimi brevis, and m. opponens digiti minimi. Majority of the thenar muscles are fused more or less with each other, so that clear separation of these muscles was difficult. The lumbrical muscles arose from the palmar parts of four main tendons of the deep flexor muscle to the second, third, fourth, and fifth digits. The mm, contrahentes arose mainly from a medial tendinous septum attached on the palmar surface to the third metacarpus, and included three muscles destined to the second, fourth and fifth digits. The interossei were found on the radial side of the second, third, fourth and fifth finger as well as on the ulnar side of the second, third and fourth finger. The intrinsic hand muscles in the Japanese monkey received innervation either from the median or the ulnar nerve. Branching pattern of these nerves to the individual muscles was fundamentally similar to those in man except for the fact that the median and the ulnar nerve in the Japanese monkey do not communi cateto make a loop in the thenar muscles. -

Essential Tremor of the Voice Vs. Spasmodic Dysphonia by Michael M
Essential Tremor (ET) Essential Tremor of the Voice vs. Spasmodic Dysphonia By Michael M. Johns, MD (pictured below)- Director at Emory Voice Center, Emory University, Atlanta, GA and member of the IETF Medical Advisory Board, and Madeleine Pethan, MS, CCC-SLP - Speech Pathologist at Emory Voice Center Introduction box, is not the only structure which can cause essential tremor of the voice. Tremor of the voice can be caused Certain neurologic conditions can cause people to have when any of the structures in the speech system is problems with their voice. These voice problems can affected. Essential tremor of the voice may be caused often lead to more difficulty communicating throughout by tremor in the soft palate, tongue, pharynx, or even daily life. It is important that patients with neurological muscles of respiration. Extralaryngeal tremor (i.e., out- voice disorders are evaluated by an otolaryngologist, or side the voice box) has been reported in up to as many ENT doctor, in addition to their neurologist to determine as 93% of patients with diagnosed essential tremor of the diagnosis and discuss treatment options. Many the voice. Similarly, most patients with essential tremor patients with essential tremor also experience essential of the voice also have tremor affecting their hands, leg, tremor of the voice. Essential tremor of the voice can chin, or trunk. often be confused with another neurologic voice disor- der known as spasmodic dysphonia. Essential tremor seems to be associated with aging, al- though the reasons are still inconclusive. Most studies What is Essential Tremor? report average age of onset from the late 40s to early 50s. -

Review of Systems Reason for Visit Past Gynecologic
REVIEW OF SYSTEMS Patient Name Date DOB Height Weight REASON FOR VISIT Why are you seeing the doctor today? ________________________________________________________________________________________ Have you been treated for this problem in the past? Yes No If yes, please explain ______________________________________________________________________________________________________ Have you had any recent radiology or laboratory studies? Yes No If yes, please indicate where, when, and type of study __________________________________________________________________________ PAST GYNECOLOGIC HISTORY Please indicate if you have received treatment for the conditions below, or if you are currently receiving treatment. Yes No Yes No Abnormal Pap HPV (Human Papillomavirus) Other Gynecologic Problems _______________________________________________________________________________________________ Are there any other medical problems that we should be aware of? ______________________________________________________________ _________________________________________________________________________________________________________________________ Are you currently pregnant or could you possibly be pregnant? Yes No Date of Last Menstrual Period ____________________/ / Do you/have you taken female hormones? Yes No Oral contraceptives? Yes No Type of contraception: _____________________________ Total number of: Pregnancies ________ Term Births ________ Pre-Term Births ________ Elective Abortions ________ Miscarriages ________ C-sections ________ REVIEW OF -

History-Of-Movement-Disorders.Pdf
Comp. by: NJayamalathiProof0000876237 Date:20/11/08 Time:10:08:14 Stage:First Proof File Path://spiina1001z/Womat/Production/PRODENV/0000000001/0000011393/0000000016/ 0000876237.3D Proof by: QC by: ProjectAcronym:BS:FINGER Volume:02133 Handbook of Clinical Neurology, Vol. 95 (3rd series) History of Neurology S. Finger, F. Boller, K.L. Tyler, Editors # 2009 Elsevier B.V. All rights reserved Chapter 33 The history of movement disorders DOUGLAS J. LANSKA* Veterans Affairs Medical Center, Tomah, WI, USA, and University of Wisconsin School of Medicine and Public Health, Madison, WI, USA THE BASAL GANGLIA AND DISORDERS Eduard Hitzig (1838–1907) on the cerebral cortex of dogs OF MOVEMENT (Fritsch and Hitzig, 1870/1960), British physiologist Distinction between cortex, white matter, David Ferrier’s (1843–1928) stimulation and ablation and subcortical nuclei experiments on rabbits, cats, dogs and primates begun in 1873 (Ferrier, 1876), and Jackson’s careful clinical The distinction between cortex, white matter, and sub- and clinical-pathologic studies in people (late 1860s cortical nuclei was appreciated by Andreas Vesalius and early 1870s) that the role of the motor cortex was (1514–1564) and Francisco Piccolomini (1520–1604) in appreciated, so that by 1876 Jackson could consider the the 16th century (Vesalius, 1542; Piccolomini, 1630; “motor centers in Hitzig and Ferrier’s region ...higher Goetz et al., 2001a), and a century later British physician in degree of evolution that the corpus striatum” Thomas Willis (1621–1675) implicated the corpus -

The Muscles That Act on the Upper Limb Fall Into Four Groups
MUSCLES OF THE APPENDICULAR SKELETON UPPER LIMB The muscles that act on the upper limb fall into four groups: those that stabilize the pectoral girdle, those that move the arm, those that move the forearm, and those that move the wrist, hand, and fingers. Muscles Stabilizing Pectoral Girdle (Marieb / Hoehn – Chapter 10; Pgs. 346 – 349; Figure 1) MUSCLE: ORIGIN: INSERTION: INNERVATION: ACTION: ANTERIOR THORAX: anterior surface coracoid process protracts & depresses Pectoralis minor* pectoral nerves of ribs 3 – 5 of scapula scapula medial border rotates scapula Serratus anterior* ribs 1 – 8 long thoracic nerve of scapula laterally inferior surface stabilizes / depresses Subclavius* rib 1 --------------- of clavicle pectoral girdle POSTERIOR THORAX: occipital bone / acromion / spine of stabilizes / elevates / accessory nerve Trapezius* spinous processes scapula; lateral third retracts / rotates (cranial nerve XI) of C7 – T12 of clavicle scapula transverse processes upper medial border elevates / adducts Levator scapulae* dorsal scapular nerve of C1 – C4 of scapula scapula Rhomboids* spinous processes medial border adducts / rotates dorsal scapular nerve (major / minor) of C7 – T5 of scapula scapula * Need to be familiar with on both ADAM and the human cadaver Figure 1: Muscles stabilizing pectoral girdle, posterior and anterior views 2 BI 334 – Advanced Human Anatomy and Physiology Western Oregon University Muscles Moving Arm (Marieb / Hoehn – Chapter 10; Pgs. 350 – 352; Figure 2) MUSCLE: ORIGIN: INSERTION: INNERVATION: ACTION: intertubercular -
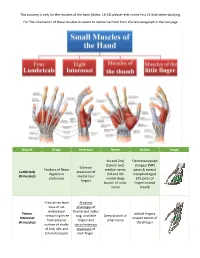
This Sumarry Is Only for the Muscles of the Hand (Slides: 14-33) Please Refer to the First 13 Slide When Studying
This sumarry is only for the muscles of the hand (slides: 14-33) please refer to the first 13 slide when studying. For The innervation of these muscles its easier to memorize them from the last paragraph in the last page Muscle Origin Insertion Nerve Action Image 1st and 2nd, Flexmetacarpoph (lateral two) alangeal (MP) Extensor Tendons of flexor median nerve; joints & extend Lumbricals expansion of Digitorum 3rd and 4th interphalangeal (4 muscles) medial four profundus medial deep (IP) joints of fingers branch of ulnar fingers except nerve thumb -First arises from Proximal base of 1st phalanges of metacarpal thumb and index, Palmar adduct fingers - remaining three ring, and little Deep branch of Interossei toward center of from anterior fingers and ulnar nerve (4 muscles) third finger surface of shafts dorsal extensor of 2nd, 4th, and expansion of 5th metacarpals each finger . Proximal phalanges of index, middle, and ring fingers Contiguous sides abduct fingers Dorsal Interossei and dorsal Deep branch of of shafts of from center of (4 muscles) extensor ulnar nerve metacarpal bones third finger expansion (1st:index\ 2nd,3rd:middle \ 4th:ring) Both palmar and dorsal: -Flex metacarpophalangeal joints -Extend interphalangeal joints Simultaneous flexion at the metacarpophalangeal joints and extension at the interphalangeal joints of a digit are essential for the fine movements of writing, drawing, threading a needle, etc. The Lumbricals and interossei have long been accepted as not only primary agents in flexing the metacarpophalangeal joints -

The Clinical Approach to Movement Disorders Wilson F
REVIEWS The clinical approach to movement disorders Wilson F. Abdo, Bart P. C. van de Warrenburg, David J. Burn, Niall P. Quinn and Bastiaan R. Bloem Abstract | Movement disorders are commonly encountered in the clinic. In this Review, aimed at trainees and general neurologists, we provide a practical step-by-step approach to help clinicians in their ‘pattern recognition’ of movement disorders, as part of a process that ultimately leads to the diagnosis. The key to success is establishing the phenomenology of the clinical syndrome, which is determined from the specific combination of the dominant movement disorder, other abnormal movements in patients presenting with a mixed movement disorder, and a set of associated neurological and non-neurological abnormalities. Definition of the clinical syndrome in this manner should, in turn, result in a differential diagnosis. Sometimes, simple pattern recognition will suffice and lead directly to the diagnosis, but often ancillary investigations, guided by the dominant movement disorder, are required. We illustrate this diagnostic process for the most common types of movement disorder, namely, akinetic –rigid syndromes and the various types of hyperkinetic disorders (myoclonus, chorea, tics, dystonia and tremor). Abdo, W. F. et al. Nat. Rev. Neurol. 6, 29–37 (2010); doi:10.1038/nrneurol.2009.196 1 Continuing Medical Education online 85 years. The prevalence of essential tremor—the most common form of tremor—is 4% in people aged over This activity has been planned and implemented in accordance 40 years, increasing to 14% in people over 65 years of with the Essential Areas and policies of the Accreditation Council age.2,3 The prevalence of tics in school-age children and for Continuing Medical Education through the joint sponsorship of 4 MedscapeCME and Nature Publishing Group. -

ISPUB.COM Volume 9 Number 2
The Internet Journal of Surgery ISPUB.COM Volume 9 Number 2 An Anomalous Palmaris Brevis Muscle and its Clinical Implications S Das, S Paul Citation S Das, S Paul. An Anomalous Palmaris Brevis Muscle and its Clinical Implications. The Internet Journal of Surgery. 2006 Volume 9 Number 2. Abstract The palmaris brevis (PB) muscle is a small, thin, subcutaneous muscle of the palm. The palmaris brevis muscle is important muscle contributing to the grip of the hand. In the present case, during routine cadaveric dissection, we detected a PB muscle which was not subcutaneous but existed as a muscle deep to the dermis of the skin of the palm. The PB muscle stretched as a horizontal band over the hypothenar muscles of the palm. The anomalous location of the PB may result in compression of neurovascular structures on the ulnar side of the palm. The awareness of such anomalous muscle which is not subcutaneous, may be clinical important for surgeons operating on the hand and clinicians diagnosing compressive symptoms. INTRODUCTION Figure 1 The PB muscle is a thin subcutaneous muscle. The PB arises Figure 1: Photograph of dissected right palm showing from the flexor retinaculum and the medial border of the central part of the palmar aponeurosis and attached to the dermis of the skin on the ulnar side of the palm. 1 The PB is innervated by the ulnar nerve and the main action of the muscle makes the palmar grip more secure. 1 The clinical importance of the muscle lies in the fact, that it lies above the ulnar artery and the ulnar nerve in the palm. -

Porro NEWORK NEWS
International Polio Network SAINT LOUIS, MISSOURIUSA Winter 2003 .Vol. 19, No. 1 Porro NEWORKNEWS Straight Answers to Your "Cramped" Questions Holly H. Wise, P7; PhD, and Kerri A. Kolehma, MS, MD, Coastal Post-Polio Clinic, Charleston, South Carolina Tired in the morning? Is it diffi- Cramps can occur throughout origins anywhere in the central cult to get comfortable for a good the day but more often occur at and peripheral nervous systems night of sleep? A complaint often night or when a person is resting. and may explain the wide range reported at the Coastal Post-Polio Although it is not known exactly of conditions in which the Clinic in Charleston, South why cramps happen mostly at cramping occurs (Bentley, 1996). Carolina, is the inability to get these times, it is thought that to sleep at night due to leg pain, the resting muscle is not being Seeking Answers twitching, or cramping. stretched and is therefore more A thorough history and possibly easily excited. Muscle cramping is a relatively a referral for screening labs will common, painful, and bother- The basis for the theory that help determine the causes for some complaint among generally I cramps occur more at rest, due to I leg pain and cramping. Polio healthy adults, and is more com- I the muscle not being stretched, I survivors can provide a descrip- mon in women than men. Some I is that passive stretching can I tion of their muscle cramps, studies estimate as many as 50- 1 relieve muscle cramping. Pain I identification of the time and 70% of older adults may experi- I associated with cramping is likely I place when they occur, and an ence nocturnal leg and foot I caused by the demand of the I activity log of the 24-48 hours cramps (Abdulla, et.