Download PDF File
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Vertebral Column and Thorax
Introduction to Human Osteology Chapter 4: Vertebral Column and Thorax Roberta Hall Kenneth Beals Holm Neumann Georg Neumann Gwyn Madden Revised in 1978, 1984, and 2008 The Vertebral Column and Thorax Sternum Manubrium – bone that is trapezoidal in shape, makes up the superior aspect of the sternum. Jugular notch – concave notches on either side of the superior aspect of the manubrium, for articulation with the clavicles. Corpus or body – flat, rectangular bone making up the major portion of the sternum. The lateral aspects contain the notches for the true ribs, called the costal notches. Xiphoid process – variably shaped bone found at the inferior aspect of the corpus. Process may fuse late in life to the corpus. Clavicle Sternal end – rounded end, articulates with manubrium. Acromial end – flat end, articulates with scapula. Conoid tuberosity – muscle attachment located on the inferior aspect of the shaft, pointing posteriorly. Ribs Scapulae Head Ventral surface Neck Dorsal surface Tubercle Spine Shaft Coracoid process Costal groove Acromion Glenoid fossa Axillary margin Medial angle Vertebral margin Manubrium. Left anterior aspect, right posterior aspect. Sternum and Xyphoid Process. Left anterior aspect, right posterior aspect. Clavicle. Left side. Top superior and bottom inferior. First Rib. Left superior and right inferior. Second Rib. Left inferior and right superior. Typical Rib. Left inferior and right superior. Eleventh Rib. Left posterior view and left superior view. Twelfth Rib. Top shows anterior view and bottom shows posterior view. Scapula. Left side. Top anterior and bottom posterior. Scapula. Top lateral and bottom superior. Clavicle Sternum Scapula Ribs Vertebrae Body - Development of the vertebrae can be used in aging of individuals. -

Shoulder Anatomy & Clinical Exam
MSK Ultrasound - Spine - Incheon Terminal Orthopedic Private Clinic Yong-Hyun, Yoon C,T-spine Basic Advanced • Medial branch block • C-spine transforaminal block • Facet joint block • Thoracic paravertebral block • C-spine intra-discal injection • Superficial cervical plexus block • Vagus nerve block • Greater occipital nerve block(GON) • Third occipital nerve block(TON) • Hydrodissection • Brachial plexus(1st rib level) • Suboccipital nerve • Stellate ganglion block(SGB) • C1, C2 nerve root, C2 nerve • Brachial plexus block(interscalene) • Recurrent laryngeal nerve • Serratus anterior plane • Cervical nerve root Cervical facet joint Anatomy Diagnosis Cervical facet joint injection C-arm Ultrasound Cervical medial branch Anatomy Nerve innervation • Medial branch • Same level facet joint • Inferior level facet joint • Facet joint • Dual nerve innervation Cervical medial branch C-arm Ultrasound Cervical nerve root Anatomy Diagnosis • Motor • Sensory • Dermatome, myotome, fasciatome Cervical nerve root block C-arm Ultrasound Stallete ganglion block Anatomy Injection Vagus nerve Anatomy Injection L,S-spine Basic Advanced • Medial branch block • Lumbar sympathetic block • Facet joint block • Lumbar plexus block • Superior, inferior hypogastric nerve block • Caudal block • Transverse abdominal plane(TAP) block • Sacral plexus block • Epidural block • Hydrodissection • Interlaminal • Pudendal nerve • Transforaminal injection • Genitofemoral nerve • Superior, inferior cluneal nerve • Rectus abdominal sheath • Erector spinae plane Lumbar facet -

Anatomy of the Spine
12 Anatomy of the Spine Overview The spine is made of 33 individual bones stacked one on top of the other. Ligaments and muscles connect the bones together and keep them aligned. The spinal column provides the main support for your body, allowing you to stand upright, bend, and twist. Protected deep inside the bones, the spinal cord connects your body to the brain, allowing movement of your arms and legs. Strong muscles and bones, flexible tendons and ligaments, and sensitive nerves contribute to a healthy spine. Keeping your spine healthy is vital if you want to live an active life without back pain. Spinal curves When viewed from the side, an adult spine has a natural S-shaped curve. The neck (cervical) and low back (lumbar) regions have a slight concave curve, and the thoracic and sacral regions have a gentle convex curve (Fig. 1). The curves work like a coiled spring to absorb shock, maintain balance, and allow range of motion throughout the spinal column. The muscles and correct posture maintain the natural spinal curves. Good posture involves training your body to stand, walk, sit, and lie so that the least amount of strain is placed on the spine during movement or weight-bearing activities. Excess body weight, weak muscles, and other forces can pull at the spine’s alignment: • An abnormal curve of the lumbar spine is lordosis, also called sway back. • An abnormal curve of the thoracic spine is Figure 1. (left) The spine has three natural curves that form kyphosis, also called hunchback. an S-shape; strong muscles keep our spine in alignment. -

Anatomy of Spinal Nerves in the First Turkish Illustrated Anatomy Handwritten Textbook
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by DSpace@HKU Childs Nerv Syst DOI 10.1007/s00381-016-3136-9 COVER EDITORIAL Anatomy of spinal nerves in the first Turkish illustrated anatomy handwritten textbook Murat Çetkin1 & Mustafa Orhan1 & İlhan Bahşi1 & Begümhan Turhan2 Received: 26 May 2016 /Accepted: 30 May 2016 # Springer-Verlag Berlin Heidelberg 2016 BTeşrih-ül Ebdan ve Tercümânı Kıbale-i Feylesûfan^ is the the book, İtâḳî acknowledges the contributions of the Grand first handwritten anatomy textbook with illustrations written Vizier [4, 7]. in Turkish in 17th century by Şemseddîn-i İtâḳî. BTeşrih^ has Not many textbooks about anatomy existed in the Islamic different meanings such as anatomy, skeleton, and cutting a World and the Ottoman Empire until İtâḳî’sbook[9]. In other corpse into pieces [1]. BTeşrih-ül Ebdan ve Tercümânı Kıbale- medical textbooks, anatomy occupies only a few pages in i Feylesûfan ^ means dissection of the body and scholars’ different sections [4]. İtâḳî’s book is a pioneer in its area as birth knowledge [2]. Since this is the first handwritten text- it is written in Turkish, and it is supported with illustrations book in Turkish, it has great importance in the development of [4]. In addition to Turkish, the book contains mostly Arabic medicine in Ottoman Empire. This book was written while and rarely Persian terms as well [4, 6, 7]. Some editions of this Grand Vizier Recep Pasha was in power, and it was dedicated book which was written in the 17th century were reprinted in to the Sultan of that period, Murat the IVth [3, 4]. -

Occipital Neuralgia: a Literature Review of Current Treatments from Traditional Medicine to CAM Treatments
Occipital Neuralgia: A Literature Review of Current Treatments from Traditional Medicine to CAM Treatments By Nikole Benavides Faculty Advisor: Dr. Patrick Montgomery Graduation: April 2011 1 Abstract Objective. This article provides an overview of the current and upcoming treatments for people who suffer from the signs and symptoms of greater occipital neuralgia. Types of treatments will be analyzed and discussed, varying from traditional Western medicine to treatments from complementary and alternative health care. Methods. A PubMed search was performed using the key words listed in this abstract. Results. Twenty-nine references were used in this literature review. The current literature reveals abundant peer reviewed research on medications used to treat this malady, but relatively little on the CAM approach. Conclusion. Occipital Neuralgia has become one of the more complicated headaches to diagnose. The symptoms often mimic those of other headaches and can occur post-trauma or due to other contributing factors. There are a variety of treatments that involve surgery or blocking of the greater occipital nerve. As people continue to seek more natural treatments, the need for alternative treatments is on the rise. Key Words. Occipital Neuralgia; Headache; Alternative Treatments; Acupuncture; Chiropractic; Nutrition 2 Introduction Occipital neuralgia is a type of headache that describes the irritation of the greater occipital nerve and the signs and symptoms associated with it. It is a difficult headache to diagnose due to the variety of signs and symptoms it presents with. It can be due to a post-traumatic event, degenerative changes, congenital anomalies, or other factors (10). The patterns of occipital neuralgia mimic those of other headaches. -

Vertebral Column
Vertebral Column • Backbone consists of Cervical 26 vertebrae. • Five vertebral regions – Cervical vertebrae (7) Thoracic in the neck. – Thoracic vertebrae (12) in the thorax. – Lumbar vertebrae (5) in the lower back. Lumbar – Sacrum (5, fused). – Coccyx (4, fused). Sacrum Coccyx Scoliosis Lordosis Kyphosis Atlas (C1) Posterior tubercle Vertebral foramen Tubercle for transverse ligament Superior articular facet Transverse Transverse process foramen Facet for dens Anterior tubercle • Atlas- ring of bone, superior facets for occipital condyles. – Nodding movement signifies “yes”. Axis (C2) Spinous process Lamina Vertebral foramen Transverse foramen Transverse process Superior articular facet Odontoid process (dens) •Axis- dens or odontoid process is body of atlas. – Pivotal movement signifies “no”. Typical Cervical Vertebra (C3-C7) • Smaller bodies • Larger spinal canal • Transverse processes –Shorter – Transverse foramen for vertebral artery • Spinous processes of C2 to C6 often bifid • 1st and 2nd cervical vertebrae are unique – Atlas & axis Typical Cervical Vertebra Spinous process (bifid) Lamina Vertebral foramen Inferior articular process Superior articular process Transverse foramen Pedicle Transverse process Body Thoracic Vertebrae (T1-T12) • Larger and stronger bodies • Longer transverse & spinous processes • Demifacets on body for head of rib • Facets on transverse processes (T1-T10) for tubercle of rib Thoracic Vertebra- superior view Spinous process Transverse process Facet for tubercle of rib Lamina Superior articular process -

Cervical Vertebrae 1 Cervical Vertebrae
Cervical vertebrae 1 Cervical vertebrae Cervical vertebrae or Cervilar Position of human cervical vertebrae (shown in red). It consists of 7 bones, from top to bottom, C1, C2, C3, C4, C5, C6 and C7. A human cervical vertebra Latin Vertebrae cervicales [1] Gray's p.97 [2] MeSH Cervical+vertebrae [3] TA A02.2.02.001 [4] FMA FMA:72063 In vertebrates, cervical vertebrae (singular: vertebra) are those vertebrae immediately inferior to the skull. Thoracic vertebrae in all mammalian species are defined as those vertebrae that also carry a pair of ribs, and lie caudal to the cervical vertebrae. Further caudally follow the lumbar vertebrae, which also belong to the trunk, but do not carry ribs. In reptiles, all trunk vertebrae carry ribs and are called dorsal vertebrae. In many species, though not in mammals, the cervical vertebrae bear ribs. In many other groups, such as lizards and saurischian dinosaurs, the cervical ribs are large; in birds, they are small and completely fused to the vertebrae. The transverse processes of mammals are homologous to the cervical ribs of other amniotes. Cervical vertebrae 2 In humans, cervical vertebrae are the smallest of the true vertebrae, and can be readily distinguished from those of the thoracic or lumbar regions by the presence of a foramen (hole) in each transverse process, through which passes the vertebral artery. The remainder of this article focuses upon human anatomy. Structure By convention, the cervical vertebrae are numbered, with the first one (C1) located closest to the skull and higher numbered vertebrae (C2-C7) proceeding away from the skull and down the spine. -

The Anatomy of Spinal Nerves in the “Teşrihü’L-Ebdan Min E’T-Tıb” Written in the Fourteenth Century* XIV
The anatomy of spinal nerves in the “Teşrihü’l-Ebdan Min e’t-Tıb” written in the fourteenth century* XIV. yüzyılda yazılmış olan “Teşrihü’l-Ebdan min e’t-Tıb” adlı eserde spinal sinirlerin anatomisi İlhan Bahşii, Mustafa Orhanii, Murat Çetkiniii iMD, PhD. Department of Anatomy, Faculty of Medicine, Gaziantep University https://orcid.org/0000-0001-8078-7074 iiProf. Dr. Department of Anatomy, Faculty of Medicine, Gaziantep University https://orcid.org/0000-0003-4403-5718 iiiPhD. Department of Anatomy, Faculty of Medicine, Istanbul Medeniyet University https://orcid.org/0000-0001-6676-9005 ABSTRACT Considering that the visual dimension of anatomy cannot be ignored and an anatomy education without the visual part will make a doctor imperfect in their profession, it may be seen that pictorial anatomy books written in previous periods are highly valuable. The purpose of this study is to investigate the spinal nerve anatomy included in the work titled Teşrihü’l-Ebdan min e’t-Tıb written in the XIVth century and compare the information at that period to the information of our time. The nervous system was analyzed under a separate title in the book. Firstly, general information was provided about nerves, and then cranial and spinal nerves were described. The author stated in his work that there are two differences between humans and animals as feeling and movement. He stated that the center for feeling and movement is the brain and all nerves converge in the brain. Although there are insufficient or incorrect information in historical books of medicine, such books are highly valuable as they show the scientific progress. -

Bones of the Trunk
BONES OF THE TRUNK Andrea Heinzlmann Veterinary University Department of Anatomy and Histology 16th September 2019 VERTEBRAL COLUMN (COLUMNA VERTEBRALIS) • the vertebral column composed of the vertebrae • the vertebrae form a horizontal chain https://hu.pinterest.com/pin/159877855502035893/ VERTEBRAL COLUMN (COLUMNA VERTEBRALIS) along the vertebral column three major curvatures are recognized: 1. the DORSAL CONVEX CURVATURE – between the head and the neck 2. the DORSAL CONCAVE CURVATURE – between the neck and the chest 3. the DORSAL CONVEX CURVATURE – between the thorax and the lumbar region - in carnivores (Ca) there is an additional DORSAL CONVEXITY in the sacral region https://hu.pinterest.com/pin/159877855502035893/ VERTEBRAL COLUMN (COLUMNA VERTEBRALIS) - corresponding to the regions of the body, we distinguish: 1. CERVICAL VERTEBRAE 2. THORACIC VERTEBRAE 3. LUMBAR VERTEBRAE 4. SACRAL VERTEBRAE 5. CAUDAL (COCCYGEAL) VERTEBRAE https://www.ufaw.org.uk/dogs/french-bulldog-hemivertebrae https://rogueshock.com/know-your-horse-in-9-ways/5/ BUILD OF THE VERTEBRAE each vertebrae presents: 1. BODY (CORPUS VERTEBRAE) 2. ARCH (ARCUS VERTEBRAE) 3. PROCESSES corpus Vertebra thoracica (Th13) , Ca. THE VERTEBRAL BODY (CORPUS VERTEBRAE) - the ventral portion of the vertebra ITS PARTS: 1. EXTREMITAS CRANIALIS (seu CAPUT VERTEBRAE) – convex 2. EXTREMITAS CAUDALIS (seu FOSSA VERTEBRAE) - concave Th13, Ca. THE VERTEBRAL BODY (CORPUS VERTEBRAE) 3. VENTRAL SURFACE of the body has a: - ventral crest (CRISTA VENTRALIS) 4. DORSAL SURFACE of the body carries : - the vertebral arch (ARCUS VERTEBRAE) Th13, Ca., lateral aspect Arcus vertebrae corpus Vertebra thoracica (Th13) , Ca., caudal aspect THE VERTEBRAL BODY (CORPUS VERTEBRAE) 6. VERTEBRAL ARCH (ARCUS VERTEBRAE) compraisis: a) a ventral PEDICULUS ARCUS VERTEBRAE b) a dorsal LAMINA ARCUS VERTEBRAE C7, Ca. -
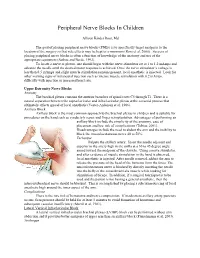
Peripheral Nerve Blocks in Children
Peripheral Nerve Blocks In Children Allison Kinder Ross, Md The goal of placing peripheral nerve blocks (PNBs) is to specifically target analgesia to the location of the surgery so that side effects may be kept to a minimum (Ross et al, 2000). Success of placing peripheral nerve blocks is often a function of knowledge of the anatomy and use of the appropriate equipment (Sethna and Berde, 1992). To locate a nerve or plexus, one should begin with the nerve stimulator set at 1 to 1.2 mAmps and advance the needle until the desired motor response is achieved. Once the nerve stimulator’s voltage is less than 0.5 mAmps and slight muscle stimulation remains present, local anesthetic is injected. Look for other warning signs of intraneural injection such as intense muscle stimulation with 0.2 mAmps, difficulty with injection or increased heart rate. Upper Extremity Nerve Blocks Anatomy The brachial plexus contains the anterior branches of spinal roots C5 through T1. There is a natural separation between the supraclavicular and infraclavicular plexus at the coracoid process that ultimately affects spread of local anesthetic (Vester-Andersen et al, 1986). Axillary Block Axillary block is the most common approach to the brachial plexus in children and is suitable for procedures on the hand such as syndactyly repair and finger reimplantation. Advantages of performing an axillary block include the simplicity of the anatomy, ease of placement and low risk of complications (Tobias, 2001). Disadvantages include the need to abduct the arm and the inability to block the musculocutaneous nerve 40 to 50%. -

Mapping Sensory Nerve Communications Between Peripheral Nerve Territories
Clinical Anatomy 27:681–690 (2014) ORIGINAL COMMUNICATION Mapping Sensory Nerve Communications Between Peripheral Nerve Territories 1 2 1* ADIL LADAK, R. SHANE TUBBS, AND ROBERT J. SPINNER 1Department of Neurologic Surgery, Orthopedics and Anatomy, Mayo Clinic, Rochester, Minnesota 2Department of Neurosurgery, Children’s Hospital, Birmingham, Alabama The human cutaneous sensory map has been a work in progress over the past century, depicting sensory territories supplied by both the spinal and cranial nerves. Two critical discoveries, which shaped our understanding of cutaneous innervation, were sensory dermatome overlap between contiguous spinal levels and axial lines across areas where no sensory overlap exists. These concepts define current dermatome maps. We wondered whether the overlap between contiguous sensory territories was even tighter: if neural communications were present in the peripheral nerve territories consistently connecting contiguous spinal levels? A literature search using peer-reviewed articles and established anatomy texts was performed aimed at identifying the presence of communica- tions between sensory nerves in peripheral nerve territories and their relation- ship to areas of adjacent and non-adjacent spinal or cranial nerves and axial lines (lines of discontinuity) in the upper and lower limbs, trunk and perineum, and head and neck regions. Our findings demonstrate the consistent presence of sensory nerve communications between peripheral nerve territories derived from spinal nerves within areas of axial lines in the upper and lower limbs, trunk and perineum, and head and neck. We did not find examples of communications crossing axial lines in the limbs or lines of discontinuity in the face, but did find examples crossing axial lines in the trunk and perineum. -

Anatomy of the Spine
Anatomy of the Spine Musculoskeletal block- Anatomy-lecture 4 Editing file Color guide : Objectives Only in boys slides in Blue Only in girls slides in Purple By the end of this lecture you should be able to: important in Red Doctor note in Green ✓ Distinguish and describe the cervical, thoracic, lumbar, sacral and Extra information in Grey coccygeal vertebrae. ✓ Describe the vertebral curvatures. ✓ Describe the movement which occur in each region of the vertebral column. ✓ List the structures which connect 2 adjacent vertebrae together. ✓ List and identify the ligaments of the intervertebral joints. Spine or Vertebral Column ● The vertebral column extends from the skull to the pelvis. ● It surrounds and protects the spinal cord and supports the whole body. ● It is formed from 33 irregular vertebrae. It consists of 24 single vertebrae and 2 bones: •Sacrum, (5 fused vertebrae).(Convex) •Coccyx, (4 fused vertebrae). Of the 24 single bones, •7 Cervical vertebrae (concave) •12 Thoracic vertebrae(convex) •5 Lumbar vertebrae.(concave) The single vertebrae are separated by pads of flexible fibrocartilage called the intervertebral disc. • The intervertebral discs cushion the vertebrae and absorb shocks. • The spinal curvature and discs make the body trunk flexible and prevent shock to head while walking or running. • We have 2 spinal curvatures: 1) Primary curvature (present at birth): Concave forward - Thoracic - Sacral regions 2) Secondary curvature (present after birth): Convex forward - Cervical (after the baby holds his head 6th month) - Lumbar (after walking around one year) 3 Typical Vertebra ● Any vertebra is made up of: 1) Body or Centrum: - disc-like weight bearing part that lies anteriorly 2) Vertebral Arch: - Formed from fusion of 2 pedicles and 2 laminae ● Vertebral foramen lies between the body and the vertebral foramen.