Compositions of Glycopyrronium Salt for Inhalation
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

2019 Year in Review: Aerosol Therapy
2019 Year in Review: Aerosol Therapy Ariel Berlinski Introduction COPD Newly Approved Drugs Asthma New Devices As-Needed Inhaled Corticosteroid/Long-Acting Bronchodilator Therapy Asthma Medication Report in Adolescents and Caregivers Cystic Fibrosis Hypertonic Saline in Cystic Fibrosis Infectivity of Cough Aerosols in Cystic Fibrosis Liposomal Amikacin for MAC Lung Disease Electronic Nicotine Delivery Systems E-Cigarette or Vaping Associated Lung Injury Secondhand Exposure Summary Relevant publications related to medicinal and toxic aerosols are discussed in this review. Treatment of COPD includes a combination of long-acting bronchodilators and long-acting muscarinic antagonists. A combination of aclidinium bromide and formoterol fumarate was approved in the United States. The combination was superior to its components alone, as well as tiotropium and a salmeterol-fluticasone combination. Increased risk of an asthma exacerba- tion was reported in children exposed to electronic nicotine delivery systems. A smart inhaler capable of recording inspiratory flow was approved in the United States. The use of as-needed budesonide-formoterol was reported to be superior to scheduled budesonide and as-needed ter- butaline for the treatment of adults with mild-to-moderate asthma. A survey among teens with asthma and their caregivers revealed a disagreement in the number of inhaled controller medi- cations the teen was taking. Treatment with inhaled hypertonic saline resulted in a decreased lung clearance index in infants and preschool children with cystic fibrosis. Surgical masks were well tolerated and significantly decreased the burden of aerosolized bacteria generated by coughing in adults with cystic fibrosis. Inhaled liposomal amikacin in addition to guideline- based therapy was reported to be superior to guideline-based therapy alone in achieving nega- tive sputum cultures in adult subjects with Mycobacterium avium complex pulmonary disease. -

Terbutaline Sulfate Injection, USP
Terbutaline Sulfate Injection, USP 1 mg per mL | NDC 70860-801-01 ATHENEX AccuraSEESM PACKAGING AND LABELING BIG, BOLD AND BRIGHT — TO HELP YOU SEE IT, SAY IT AND PICK IT RIGHT DIFFERENTIATION IN EVERY LABEL, DESIGNED TO HELP REDUCE MEDICATION ERRORS PLEASE SEE FULL PRESCRIBING INFORMATION, INCLUDING BOXED WARNING, FOR TERBUTALINE SULFATE INJECTION, USP, ENCLOSED. THE NEXT GENERATION OF PHARMACY INNOVATION To order, call 1-855-273-0154 or visit www.Athenexpharma.com Terbutaline Sulfate Injection, USP 1 mg NDC 70860-801-01 1 mg per mL DESCRIPTION Glass Vial CONCENTRATION 1 mg per mL CLOSURE 13 mm UNIT OF SALE 10 vials BAR CODED Yes CHOOSE AccuraSEESM FOR YOUR PHARMACY Our proprietary, differentiated and highly-visible label designs can assist pharmacists in accurate medication selection. With a unique AccuraSEE label design for every Athenex product, we’re helping your pharmacy to reduce the risk of medication errors. The idea is simple: “So what you see is exactly what you get.” Athenex, AccuraSEE and all label designs are copyright of Athenex. ©2019 Athenex. APD-0022-02-4/19 To order, call 1-855-273-0154 or visit www.Athenexpharma.com TERBUTALINE SULFATE Injection, USP • The use of beta-adrenergic agonist bronchodilators • Terbutaline sulfate should be used during nursing alone may not be adequate to control asthma in only if the potential benefit justifies the possible risk INDICATIONS AND USAGE many patients. Early consideration should be given to to the newborn. • Terbutaline sulfate injection is indicated for the adding anti-inflammatory agents, e.g., corticosteroids. prevention and reversal of bronchospasm in patients ADVERSE REACTIONS 12 years of age and older with asthma and reversible • Terbutaline sulfate should be used with caution • Common adverse reactions reported with terbutaline bronchospasm associated with bronchitis and emphysema. -

Β2 Adrenergic Agonist Suppresses Eosinophil-Induced Epithelial-To- Mesenchymal Transition of Bronchial Epithelial Cells Keigo Kainuma1,2, Tetsu Kobayashi3, Corina N
Kainuma et al. Respiratory Research (2017) 18:79 DOI 10.1186/s12931-017-0563-4 RESEARCH Open Access β2 adrenergic agonist suppresses eosinophil-induced epithelial-to- mesenchymal transition of bronchial epithelial cells Keigo Kainuma1,2, Tetsu Kobayashi3, Corina N. D’Alessandro-Gabazza2, Masaaki Toda2, Taro Yasuma2, Kota Nishihama2, Hajime Fujimoto3, Yu Kuwabara1,2, Koa Hosoki1,2, Mizuho Nagao1, Takao Fujisawa1 and Esteban C. Gabazza2* Abstract Background: Epithelial-mesenchymal transition is currently recognized as an important mechanism for the increased number of myofibroblasts in cancer and fibrotic diseases. We have already reported that epithelial- mesenchymal transition is involved in airway remodeling induced by eosinophils. Procaterol is a selective and full β2 adrenergic agonist that is used as a rescue of asthmatic attack inhaler form and orally as a controller. In this study, we evaluated whether procaterol can suppress epithelial-mesenchymal transition of airway epithelial cells induced by eosinophils. Methods: Epithelial-mesenchymal transition was assessed using a co-culture system of human bronchial epithelial cells and primary human eosinophils or an eosinophilic leukemia cell line. Results: Procaterol significantly inhibited co-culture associated morphological changes of bronchial epithelial cells, decreased the expression of vimentin, and increased the expression of E-cadherin compared to control. Butoxamine, a specific β2-adrenergic antagonist, significantly blocked changes induced by procaterol. In addition, procaterol inhibited the expression of adhesion molecules induced during the interaction between eosinophils and bronchial epithelial cells, suggesting the involvement of adhesion molecules in the process of epithelial-mesenchymal transition. Forskolin, a cyclic adenosine monophosphate-promoting agent, exhibits similar inhibitory activity of procaterol. Conclusions: Overall, these observations support the beneficial effect of procaterol on airway remodeling frequently associated with chronic obstructive pulmonary diseases. -
Ep 2626065 A1
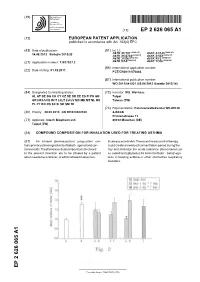
(19) TZZ Z_T (11) EP 2 626 065 A1 (12) EUROPEAN PATENT APPLICATION published in accordance with Art. 153(4) EPC (43) Date of publication: (51) Int Cl.: A61K 31/137 (2006.01) A61K 31/135 (2006.01) 14.08.2013 Bulletin 2013/33 A61K 31/4704 (2006.01) A61K 31/58 (2006.01) A61K 31/56 (2006.01) A61K 9/12 (2006.01) (2006.01) (2006.01) (21) Application number: 11827927.2 A61K 9/14 A61P 11/06 (86) International application number: Date of filing: 01.02.2011 (22) PCT/CN2011/070883 (87) International publication number: WO 2012/041031 (05.04.2012 Gazette 2012/14) (84) Designated Contracting States: (72) Inventor: WU, Wei-hsiu AL AT BE BG CH CY CZ DE DK EE ES FI FR GB Taipei GR HR HU IE IS IT LI LT LU LV MC MK MT NL NO Taiwan (TW) PL PT RO RS SE SI SK SM TR (74) Representative: Patentanwaltskanzlei WILHELM (30) Priority: 28.09.2010 CN 201010502339 & BECK Prinzenstrasse 13 (71) Applicant: Intech Biopharm Ltd. 80639 München (DE) Taipei (TW) (54) COMPOUND COMPOSITION FOR INHALATION USED FOR TREATING ASTHMA (57) An inhaled pharmaceutical composition con- tric way as a controller. The eccentric way control therapy tains primary active ingredients of beta2- agonist and cor- could create a low blood concentration period during the ticosteroids.The pharmaceuticalcompositions disclosed day and minimize the acute tolerance phenomenon (or in the present invention are to be inhaled by a patient so called tachyphylaxis) for bronchodilator - beta2-ago- when needed as a reliever, or administrated in an eccen- nists in treating asthma or other obstructive respiratory disorders. -

Clenbuterol Elisa Kit Instructions Product #101219 & 101216 Forensic Use Only
Neogen Corporation 944 Nandino Blvd., Lexington KY 40511 USA 800/477-8201 USA/Canada | 859/254-1221 Fax: 859/255-5532 | E-mail: [email protected] | Web: www.neogen.com/Toxicology CLENBUTEROL ELISA KIT INSTRUCTIONS PRODUCT #101219 & 101216 FORENSIC USE ONLY INTENDED USE: For the determination of trace quantities of Clenbuterol and/or other metabolites in human urine, blood, oral fluid. DESCRIPTION Neogen Corporation’s Clenbuterol ELISA (Enzyme-Linked ImmunoSorbent Assay) test kit is a qualitative one-step kit designed for use as a screening device for the detection of drugs and/or their metabolites. The kit was designed for screening purposes and is intended for forensic use only. It is recommended that all suspect samples be confirmed by a quantitative method such as gas chromatography/mass spectrometry (GC/MS). ASSAY PRINCIPLES Neogen Corporation’s test kit operates on the basis of competition between the drug or its metabolite in the sample and the drug- enzyme conjugate for a limited number of antibody binding sites. First, the sample or control is added to the microplate. Next, the diluted drug-enzyme conjugate is added and the mixture is incubated at room temperature. During this incubation, the drug in the sample or the drug-enzyme conjugate binds to antibody immobilized in the microplate wells. After incubation, the plate is washed 3 times to remove any unbound sample or drug-enzyme conjugate. The presence of bound drug-enzyme conjugate is recognized by the addition of K-Blue® Substrate (TMB). After a 30 minute substrate incubation, the reaction is halted with the addition of Red Stop Solution. -

Emea/666243/2009
European Medicines Agency London, 29 October 2009 EMEA/666243/2009 ISSUE NUMBER: 0910 MONTHLY REPORT PHARMACOVIGILANCE WORKING PARTY (PHVWP) OCTOBER 2009 PLENARY MEETING The CHMP Pharmacovigilance Working Party (PhVWP) held its October 2009 plenary meeting on 19-21 October 2009. PhVWP DISCUSSIONS ON SAFETY CONCERNS Below is a summary of the discussions regarding non-centrally authorised medicinal products in accordance with the PhVWP publication policy (see under http://www.emea.europa.eu/htms/human/phv/reports.htm). Positions agreed by the PhVWP for non- centrally authorised products are recommendations to Member States. For safety updates concerning centrally authorised products and products subject to ongoing CHMP procedures, readers are referred to the CHMP Monthly Report (see under http://www.emea.europa.eu/pressoffice/presshome.htm). The PhVWP provides advice on these products to the Committee of Medicinal Products for Human Use (CHMP) upon its request. Antipsychotics - risk of venous thromboembolism (VTE) Identify risk factors for VTE for preventive action before and during treatment with antipsychotics The PhVWP completed their review on the risk of VTE of antipsychotics1. The review was triggered by and based on data from the UK spontaneous adverse drug reactions reporting system and the published literature. The PhVWP carefully considered the data, including the limitations of both information sources, such as the lack of randomised controlled trial data, the heterogeneity of published studies and the potential confounding factors such as sedation and weight gain, commonly present in antipsychotic users. The PhVWP concluded that an association between VTE and antipsychotics cannot be excluded. Distinguishing different risk levels between the various active substances was not possible. -

Tocolytic Therapy a Meta-Analysis and Decision Analysis
Tocolytic Therapy A Meta-Analysis and Decision Analysis David M. Haas, MD, MS, Thomas F. Imperiale, MD, Page R. Kirkpatrick, Robert W. Klein, Terrell W. Zollinger, DrPH, and Alan M. Golichowski, MD, PhD OBJECTIVE: To determine the optimal first-line tocolytic ing prostaglandin inhibitors, only 80 would deliver within agent for treatment of premature labor. 48 hours, compared with 182 for the next-best treatment. METHODS: We performed a quantitative analysis of ran- CONCLUSION: Although all current tocolytic agents domized controlled trials of tocolysis, extracting data on were superior to no treatment at delaying delivery for maternal and neonatal outcomes, and pooling rates for both 48 hours and 7 days, prostaglandin inhibitors were each outcome across trials by treatment. Outcomes were superior to the other agents and may be considered the delay of delivery for 48 hours, 7 days, and until 37 weeks; optimal first-line agent before 32 weeks of gestation to adverse effects causing discontinuation of therapy; absence delay delivery. of respiratory distress syndrome; and neonatal survival. We (Obstet Gynecol 2009;113:585–94) used weighted proportions from a random-effects meta- analysis in a decision model to determine the optimal first-line tocolytic therapy. Sensitivity analysis was per- reterm birth, defined as any birth before the gesta- formed using the standard errors of the weighted propor- Ptional age of 37 weeks, is responsible for most of the 1–3 tions. neonatal morbidity and mortality in the United States and consumes 35% of all U.S. healthcare spending on RESULTS: Fifty-eight studies satisfied the inclusion crite- 4 ria. -

210428Orig1s000
CENTER FOR DRUG EVALUATION AND RESEARCH APPLICATION NUMBER: 210428Orig1s000 OTHER REVIEW(S) DIVISION OF CARDIOVASCULAR AND RENAL PRODUCTS Regulatory Project Manager Overview I. GENERAL INFORMATION NDA: 210428 Drug: Metoprolol Succinate Extended-Release Capsules, 25 mg, 50 mg, 100 mg and 200 mg Class: Beta- Blocker Applicant: Sun Pharmaceutical Industries Limited Proposed Indications: Hypertension, Angina Pectoris & Heart Failure Date of submission: March 30, 2017 PDUFA date: January 30, 2018 II. REVIEW TEAM Office of New Drugs, Office of Drug Evaluation I: Division of Cardiovascular & Renal Product Norman Stockbridge, MD, PhD, Director Mary Ross Southworth, PharmD, Deputy Director for Safety Michael Monteleone, MS, RAC, Assistant Director for Labeling Martina Sahre, PhD, Cross Discipline Team Leader Fortunato Senatore, MD, Clinical Reviewer Albert DeFelice, PhD, Non-Clinical Supervisor Muriel Saulnier, PhD, Non-Clinical Reviewer Edward Fromm, RPh, RAC, Chief, Project Management Staff Maryam Changi, PharmD, Regulatory Project Manager Office of Pharmaceutical Quality: Wendy Wilson-Lee, PhD, Application Technical Lead Grafton Adams, Regulatory Business Process Manager Milton Sloan, PhD, Drug Product Reviewer Rohit Tiwari, PhD, Drug Substance Reviewer Ben Stevens, PhD, Drug Substance Team Leader Kaushal Dave, PhD, Biopharmaceutical Reviewer Wu, Ta-Chin, PhD, Biopharmaceutical Team Leader Viviana Matta, PhD, Facility Reviewer Ruth Moore, PhD, Facility Team Leader Chunsheng Cai, PhD, Process Reviewer NDA 210428 RPM review Page 1 Reference ID: 42132034213643 Labeling/PMC-PMR to Sponsor: November 30, 2017 PDUFA Date: January 30, 2018 (Standard, 10-Month) PDUFA Goal Date: January 30, 2018 Approval letter: January 26, 2018 7. Reviews a) Divisional Memorandum: (January 26, 2018) Dr. Stockbridge indicated his concurrence on Dr. Sahre’s CDTL memo. -

Pharmacology and Therapeutics of Bronchodilators
1521-0081/12/6403-450–504$25.00 PHARMACOLOGICAL REVIEWS Vol. 64, No. 3 Copyright © 2012 by The American Society for Pharmacology and Experimental Therapeutics 4580/3762238 Pharmacol Rev 64:450–504, 2012 ASSOCIATE EDITOR: DAVID R. SIBLEY Pharmacology and Therapeutics of Bronchodilators Mario Cazzola, Clive P. Page, Luigino Calzetta, and M. Gabriella Matera Department of Internal Medicine, Unit of Respiratory Clinical Pharmacology, University of Rome ‘Tor Vergata,’ Rome, Italy (M.C., L.C.); Department of Pulmonary Rehabilitation, San Raffaele Pisana Hospital, Istituto di Ricovero e Cura a Carattere Scientifico, Rome, Italy (M.C., L.C.); Sackler Institute of Pulmonary Pharmacology, Institute of Pharmaceutical Science, King’s College London, London, UK (C.P.P., L.C.); and Department of Experimental Medicine, Unit of Pharmacology, Second University of Naples, Naples, Italy (M.G.M.) Abstract............................................................................... 451 I. Introduction: the physiological rationale for using bronchodilators .......................... 452 II. -Adrenergic receptor agonists .......................................................... 455 A. A history of the development of -adrenergic receptor agonists: from nonselective  Downloaded from adrenergic receptor agonists to 2-adrenergic receptor-selective drugs.................... 455  B. Short-acting 2-adrenergic receptor agonists........................................... 457 1. Albuterol........................................................................ 457 -

Chronic Obstructiv Chronic Obstructive Pulmonary Disease
pat hways Chronic obstructive pulmonary disease: beclometasone, formoterol and glycopyrronium (Trimbow) Evidence summary Published: 3 May 2018 nice.org.uk/guidance/es17 Key points The content of this evidence summary was up-to-date in May 2018. See summaries of product characteristics (SPCs), British national formulary (BNF) or the Medicines and Healthcare products Regulatory Agency (MHRA) or NICE websites for up-to-date information. Regulatory status: Beclometasone/formoterol/glycopyrronium (Trimbow, Chiesi Limited) received a European marketing authorisation in July 2017. This triple-therapy inhaler contains an inhaled corticosteroid (ICS), long-acting beta-2 agonist (LABA) and long-acting muscarinic antagonist (LAMA). It is licensed for maintenance treatment of adults with moderate-to-severe chronic obstructive pulmonary disease (COPD) who are not adequately treated by a combination of an ICS and a LABA. Overview This evidence summary discusses 3 randomised controlled trials (TRILOGY, TRINITY and TRIBUTE) looking at the safety and efficacy of beclometasone/formoterol/glycopyrronium in people with COPD with severe or very severe airflow limitation, symptoms despite treatment and a history of exacerbations. © NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and- Page 1 of conditions#notice-of-rights). 78 Chronic obstructive pulmonary disease: beclometasone, formoterol and glycopyrronium (Trimbow) (ES17) Overall, the studies found small, statistically significant improvements in lung function, rates of moderate-to-severe exacerbations of COPD and health-related quality-of-life scores with beclometasone/formoterol/glycopyrronium compared with beclometasone/formoterol or indacaterol/glycopyrronium dual therapy, or tiotropium alone. The improvements may be of limited clinical importance. In TRILOGY and TRINITY, improvements in primary outcomes relating to lung function and exacerbation rates just reached the level considered to be clinically important. -

Data Reproducibility and Effectiveness of Bronchodilators for Improving Physical Activity in COPD Patients
Journal of Clinical Medicine Review Data Reproducibility and Effectiveness of Bronchodilators for Improving Physical Activity in COPD Patients Yoshiaki Minakata * and Seigo Sasaki Department of Respiratory Medicine, National Hospital Organization Wakayama Hospital, Wakayama 644-0044, Japan; [email protected] * Correspondence: [email protected]; Tel.: +81-738-22-3256 Received: 7 September 2020; Accepted: 27 October 2020; Published: 29 October 2020 Abstract: Increasing physical activity (PA) in patients with chronic obstructive pulmonary disease (COPD) is an important issue, however, the effect of bronchodilators on PA is still controversial. The indicators of PA, as measured by an accelerometer, can easily fluctuate based on several factors, which might cause inconsistent results. In this review, we listed the indicators of PA and the factors influencing the reproducibility of indicators of PA, and reviewed reports in which the effects of bronchodilators on PA were evaluated by an accelerometer. Then, we investigated the association between the processing of influencing factors and the effectiveness of bronchodilators for improving the PA of COPD patients. Fifteen reports were extracted using the PubMed database. In all seven reports in which adjustment was performed for at least two of four influencing factors (non-wear time, data from days with special behavior, environmental factors, and number of valid days required to obtain reproducible data), bronchodilators showed beneficial effects on PA. No adjustment was made for any of these factors in any of the four bronchodilator-ineffective reports. This suggests that the processing of influencing factors to secure reproducibility might affect the results regarding the effectiveness of bronchodilators for improving PA in COPD patients. -

Bnf Chapter 3: Respiratory
BNF CHAPTER 3: RESPIRATORY Information resources: ● If an inhaler device is changed then patients must be assessed to ensure inhaler technique is adequate Respiratory Futures Consider issuing a Steroid warning card to patients prescribed high dose inhaled steroids Asthma guidelines NICE guideline [NG80] Asthma: diagnosis, monitoring and chronic asthma management NICE guidance TA 138 Asthma - inhaled corticosteroids for the treatment of chronic asthma in adults and children aged 12 years and over. https://www.sign.ac.uk/assets/sign153.pdf SIGN 153: British guideline on the management of asthma Global Initiative for Asthma 2018. GINA Report, Global Strategy for Asthma Management and Prevention. West Cheshire local guidelines COPD guidelines: NICE [NG115] COPD in over 16s diagnosis and management. NICE guideline Dec 18 [NG115] GOLD : Global strategy for the diagnosis, management, and prevention of Chronic Obstructive Pulmonary Disease 2018 Report West Cheshire local guidelines Abbreviations used: MDI: metered dose inhaler DPI: dry powder inhaler SABA: short acting beta agonist LABA: long acting beta agonist SAMA: short acting muscarinic antagonist LAMA: long acting muscarinic antagonist ICS: inhaled corticosteroid LTRA: leukotriene receptor antagonist PDE4: phosphodiesterase-4 enzyme inhibitor Joint Formulary – Respiratory Approved by Area Prescribing Committee: n/a Review by: July 2021 3.1 BRONCHODILATORS 3.1.1.1 SELECTIVE BETA2-AGONISTS Short acting Beta2 Agonist (SABA) Salbutamol 100 micrograms/metered inhalation MDI 100/200