Colon, Rectum, and Anus
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

The Anatomy of the Rectum and Anal Canal
BASIC SCIENCE identify the rectosigmoid junction with confidence at operation. The anatomy of the rectum The rectosigmoid junction usually lies approximately 6 cm below the level of the sacral promontory. Approached from the distal and anal canal end, however, as when performing a rigid or flexible sigmoid- oscopy, the rectosigmoid junction is seen to be 14e18 cm from Vishy Mahadevan the anal verge, and 18 cm is usually taken as the measurement for audit purposes. The rectum in the adult measures 10e14 cm in length. Abstract Diseases of the rectum and anal canal, both benign and malignant, Relationship of the peritoneum to the rectum account for a very large part of colorectal surgical practice in the UK. Unlike the transverse colon and sigmoid colon, the rectum lacks This article emphasizes the surgically-relevant aspects of the anatomy a mesentery (Figure 1). The posterior aspect of the rectum is thus of the rectum and anal canal. entirely free of a peritoneal covering. In this respect the rectum resembles the ascending and descending segments of the colon, Keywords Anal cushions; inferior hypogastric plexus; internal and and all of these segments may be therefore be spoken of as external anal sphincters; lymphatic drainage of rectum and anal canal; retroperitoneal. The precise relationship of the peritoneum to the mesorectum; perineum; rectal blood supply rectum is as follows: the upper third of the rectum is covered by peritoneum on its anterior and lateral surfaces; the middle third of the rectum is covered by peritoneum only on its anterior 1 The rectum is the direct continuation of the sigmoid colon and surface while the lower third of the rectum is below the level of commences in front of the body of the third sacral vertebra. -
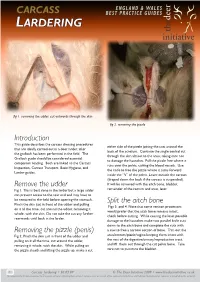
Introduction Remove the Udder Removing the Pizzle (Penis)
fig . removing the udder, cut outwards through the skin fig 2. removing the pizzle Introduction This guide describes the carcass dressing procedures either side of the pizzle joining the cuts around the that are ideally carried out in a deer larder, after back of the scrotum. Continue the single central cut the gralloch has been performed in the field. The through the skin almost to the anus, taking care not Gralloch guide should be considered essential to damage the haunches. Pull the pizzle free where it companion reading. Both are linked to the Carcass runs over the pelvis, cutting the blood vessels. Use Inspection, Carcass Transport, Basic Hygiene, and the knife to free the pizzle where it turns forward Larder guides. inside the “V” of the pelvis. Leave outside the carcass (draped down the back if the carcass is suspended). Remove the udder It will be removed with the aitch bone, bladder, Fig 1. This is best done in the larder but a large udder remainder of the rectum and anus, later. can prevent access to the rear end and may have to be removed in the field before opening the stomach. Split the aitch bone Pinch the skin just in front of the udder and pulling Figs 3. and 4. Note that some venison processors on it all the time, cut around the udder, removing it would prefer that the aitch bone remains intact, whole, with the skin. Do not take the cut any further check before cutting. While causing the least possible rearwards until back in the larder. -

How to Increase Your Enjoyment of Sex
BETTER SEX BETTER SEX BETTER SEX BETTER SEX BETTER SEX OF SEX ENJO YOUR INCREASE HOW TO for women and women for their partners YMENT “Sexual health is a state of physical, emotional, mental and social well-being in relation to sexuality; it is not merely the absence of disease, dysfunction or infirmity. Sexual health requires a positive and respectful approach to sexuality and sexual relationships, as well as the possibility of having pleasurable and safe sexual experiences, free of coercion, discrimination and violence. For sexual health to be attained and maintained, the sexual rights of all persons must be respected, protected and fulfilled.” Definition of sexual health, World Health Organisation SAFER SEX Using condoms for penetrative sex is the best way to protect yourself and your partners from Sexually Transmitted Infections, including HIV. Condoms also offer good protection from unwanted pregnancy. In the text of this booklet, we have chosen not to refer constantly to the use of condoms. Instead, we encourage you to make your own decisions about protecting yourself and others in each instance of sexual activity you undertake. 1 HOW TO INCREASE YOUR ENJOYMENT OF SEX This leaflet provides information on how to help yourself improve your enjoyment of sex. It has three main parts: Suggestions on how to improve sex generally, without doing formal exercises. These apply to both casual and regular partners. Exercises you can do on your own — for women who have difficulty getting turned on or experiencing orgasm, and who may or may not have a regular partner. Exercises you can do with a partner — for women who have difficulty getting turned on, or who have difficulty having an orgasm or enjoying penetrative sex. -

Bowel Function Anatomy
BOWEL FUNCTION ANATOMY Most of America gives little thought to bowel control. However, bowel control is actually a complex process involving the coordination of many different muscles and nerves. The bowel is considered to be a part of the digestive or gastrointestinal system. It is designed to help the body absorb nutrients and fluids from the foods we eat and drink. After taking out everything the body needs, the bowel then expels the leftover waste. The beginning of the bowel is the small intestine, sometimes referred to as the small bowel. This is where the useful nutrients are absorbed from what you eat. The small bowel delivers the waste to the colon, or large bowel. The colon is a 5-6 foot long muscular tube that delivers stool to the rectum. As the stool moves through the colon, the fluids are removed and absorbed into the body. The consistency of the stool is dependent upon many things, including how long the stool sits in the colon, how much of the water has been absorbed from the waste, and the amount of fiber and fluids in your diet. Stool consistency can vary from hard lumps to mushy to very loose, watery stool. The best and easiest consistency of stool is soft, like toothpaste; this consistency may be attained by adding fiber to your diet. Fiber helps move waste through the colon because it is indigestible by the human body. In other words, fiber adds ‘bulk’ to the stool. It is important to eat a diet high in fiber, however, most Americans lack fiber in their diet. -

Anal Sex an Informative Guide by Bedroom Kandi
AN INTRODUCTION TO ANAL SEX AN INFORMATIVE GUIDE BY BEDROOM KANDI Anal sex encompasses a variety of sexual acts involving the anus and rectum. These can include anal fingering, analingus (oral-anal sex, sometimes called “rimming”), anal insertion (using an object like a strap-on or other toy) and anal intercourse (penis-in-anus sex). Anal sex can be enjoyed by individuals of any gender, and any orientation. Everyone has a back door, after all! But it requires preparation, care, and patience to make it pleasurable. Communication is Key! No surprise butt-sex. Always check in with your partner, talk things through, and 36% communicate about whether you’re Of American Women both on board for trying anal. Check in during anal sex to report having tried ? make sure you’re both enjoying yourselves! ANAL SEX “Is Anal Sex Common?” International Society for Sexual Medicine :) http://www.issm.info/sexual-health-qa/is-anal-sex-common/ www.bedroomkandi.com ©2017 Bedroom Kandi WHY TRY ANAL? IT FEELS GOOD - There are a lot IT FEELS BAD - in a good way! The of nerve endings to stimulate around taboos around anal sex can make it a the anus, including those in the man’s thrill and add something exciting to your prostate. bedroom routine. You naughty thing! IT SPICES THINGS UP - Trying IT CAN SUBVERT GENDER new things keeps things fresh, and ROLES - Either partner can penetrate anal sex will open up a whole new or receive, (using strap-ons or other toys range of sexual positions and activities for Lesbian or Straight couples), so you for you and your partner to share. -

What's New in Stis?
WHAT’S NEW IN STIS? Sarah Weninger, HIV.STD.Viral Hepatitis Prevention Coordinator Division of Sexually Transmitted and Bloodborne Diseases January 27, 2021 OBJECTIVES ▪ Describe the updated gonorrhea treatment recommendations ▪ Identify the five goals of STI National Strategic Plan. ▪ Describe three strategies to implement for best practices for the prevention and treatment of STIs. GONORRHEA TREATMENT ▪ Combination therapy since 1985 ▪ Evidence and Rationale ▪ Antimicrobial Stewardship ▪ Pharmacokinetics ▪ Azithromycin Susceptibility 2020 UPDATE TO TREATMENT FOR GONOCOCCAL INFECTIONS. Uncomplicated urogenital, rectal or pharyngeal gonorrhea 500 mg IM Ceftriaxone* *For persons weighing ≥ 300 lbs, 1 g of IM Ceftriaxone should be administered 2020 UPDATE TO TREATMENT FOR GONOCOCCAL INFECTIONS. Uncomplicated urogenital, rectal or pharyngeal gonorrhea 500 mg IM Ceftriaxone^ + Doxycycline 100 mg orally BID * 7 Days (If Chlamydia is NOT ruled out) ^For persons weighing ≥ 300 lbs, 1 g of IM Ceftriaxone should be administered AZITHROMYCIN IS PREGNANT INDIVIDUALS WITH GONORRHEA AND CHLAMYDIA NOT RULED OUT. Uncomplicated urogenital, rectal or pharyngeal gonorrhea 500 mg IM Ceftriaxone^ + 1 G Azithromycin 2020 UPDATE TO TREATMENT FOR GONOCOCCAL INFECTIONS. Uncomplicated urogenital, rectal or pharyngeal gonorrhea - Cephalosporin Allergy 240 mg IM dose of Gentamicin + Single 2 g Oral Dose of Azithromycin EPT CAN STILL BE USED FOR GONORRHEA. Uncomplicated urogenital, rectal or pharyngeal gonorrhea Single 800 mg Oral Dose of Cefixime + Doxycycline 100 -

Saliva Use As a Lubricant for Anal Sex Is a Risk Factor for Rectal Gonorrhoea
Downloaded from http://sti.bmj.com/ on March 27, 2016 - Published by group.bmj.com STI Online First, published on March 3, 2016 as 10.1136/sextrans-2015-052502 Epidemiology ORIGINAL ARTICLE Saliva use as a lubricant for anal sex is a risk factor for rectal gonorrhoea among men who have sex with men, a new public health message: a cross-sectional survey Eric P F Chow,1,2 Vincent J Cornelisse,1,2 Tim R H Read,1,2 David Lee,1 Sandra Walker,1,2 Jane S Hocking,3 Marcus Y Chen,1,2 Catriona S Bradshaw,1,2 Christopher K Fairley1,2 1Melbourne Sexual Health ABSTRACT that sexual practices other than penile–anal sex, Centre, Alfred Health, Background Apart from penile–anal intercourse, other such as digital–anal (‘fingering’) and oral–anal Melbourne, Victoria, Australia 2 anal sexual practices (rimming, fingering and saliva use (‘rimming’) sex, may play a key role in gonorrhoea Faculty of Medicine, Central 8 Clinical School, Nursing and as a lubricant for anal sex) are common among men transmission in MSM. Health Sciences, Monash who have sex with men (MSM). The aim of this study is Gonorrhoea transmission is still occurring in the University, Melbourne, Victoria, to evaluate whether these anal sexual practices are risk setting of condom use for penile–anal sex. If, Australia factors for rectal gonorrhoea in MSM. however, the penis is not solely involved in the 3Melbourne School of Population and Global Health, Method A cross-sectional survey was conducted acquisition of rectal gonorrhoea, a plausible alter- University of Melbourne, among MSM attending Melbourne Sexual Health Centre native mechanism is required. -

James Buchanan Brady Urological Institute the Johns Hopkins Medical Institutions Baltimore, Maryland 21287
James Buchanan Brady Urological Institute The Johns Hopkins Medical Institutions Baltimore, Maryland 21287 Your Doctor has referred you to the Department of Urology for Urodynamic testing. WHAT ARE URODYNAMICS? Urodynamics are a set of tests that evaluate bladder function. Urodynamic testing tries to reproduce your voiding patterns so that we may identify any underlying problem. We will evaluate how well your bladder can store as well as empty out urine. WHAT ARE THE TESTS LIKE? The first test to be performed may be a urolflow. If you are able, you will be asked to urinate into a special commode that measures the force of your stream and the amount of urine in your bladder. Next, a sterile urinary catheter may be passed into your bladder to drain out any urine you were unable to pass on your own. This does not hurt, but may give you the sensation of having to urinate. This catheter is then taken out. Next, the actual urodynamic testing will begin. The first catheter, as small as piece of spaghetti, is placed into the bladder and will allow us to fill the bladder with sterile water while measuring how well your bladder fills. The second catheter, the same size as the one in your bladder, is placed into the rectum to evaluate abdominal pressure, or how hard your stomach muscles may be pushing to help you urinate. Finally, three sticky patches (skin sensors) may be placed on your bottom near your rectum, to measure how well certain muscles are working (the pelvic floor muscles and the urinary sphincter). -

Sigmoid-Recto-Anal Region of the Human Gut
Gut: first published as 10.1136/gut.29.6.762 on 1 June 1988. Downloaded from Gut, 1988, 29, 762-768 Intramural distribution of regulatory peptides in the sigmoid-recto-anal region of the human gut G-L FERRI, T E ADRIAN, JANET M ALLEN, L SOIMERO, ALESSANDRA CANCELLIERI, JANE C YEATS, MARION BLANK, JULIA M POLAK, AND S R BLOOM From the Department ofAnatomy, 'Tor Vergata' University, Rome, Italy and Departments ofMedicine and Histochemistry, RPMS, Hammersmith Hospital, London SUMMARY The distribution of regulatory peptides was studied in the separated mucosa, submucosa and muscularis externa taken at 10 sampling sites encompassing the whole human sigmoid colon (five sites), rectum (two sites), and anal canal (three sites). Consistently high concentrations of VIP were measured in the muscle layer at most sites (proximal sigmoid: 286 (16) pmol/g, upper rectum: 269 (17), a moderate decrease being found in the distal smooth sphincter (151 (30) pmol/g). Values are expressed as mean (SE). Conversely, substance P concentrations showed an obvious decline in the recto-anal muscle (mid sigmoid: 19 (2 0) pmol/g, distal rectum: 7 1 (1 3), upper anal canal: 1-6 (0 6)). Somatostatin was mainly present in the sigmoid mucosa and submucosa (37 (9 3) and 15 (3-5) pmol/g, respectively) and showed low, but consistent concentrations in the muscle (mid sigmoid: 2-2 (0 7) pmol/g, upper anal canal: 1 5 (0 8)). Starting in the distal sigmoid colon, a distinct peak oftissue NPY was revealed, which was most striking in the muscle (of mid sigmoid: 16 (3-9) pmol/g, upper rectum: 47 (7-8), anal sphincter: 58 (14)). -

Keeping It Safe- a Sexual and Reproductive Health Guide for Same-Sex-Attracted Women
Keeping It Safe- A sexual and reproductive health guide for same-sex-attracted women ConsentSafer Sex Let’s talk about sex… familyplanning.org.nz Penetration Keeping It Safe- This resource is for women who have sex with women; occasionally, regularly or are just thinking about it. The focus is on cis-women (women who were born with female reproductive systems and genitals), although transmen (or cis-women who have sex with transmen) may also find parts of this resource useful. It aims to provide information to women who have sex with other women, regardless of their sexual identity (e.g. lesbian, queer, bisexual, gay, straight, butch, femme, dyke, or no expressed identity) or how that may change over time. It aims to help us make informed choices about our sexual practices whoever they may be with. It also aims to enable us to be assertive in dealing with health professionals. We acknowledge that same-sex attracted women have a wide range of different sexual experiences and desires. We have based this resource on the premise that the risks of sexually transmissible infections relate to behaviours not sexual orientation or sexual identity. 2 Keeping It Safe Let’s talk about sex… Let’s talk about sex… Communicating about sex is important, whether you are in a long–term monogamous relationship, specialise in a series of one night stands, or are somewhere and anywhere in between. Talking about sex can be embarrassing for many women, but it’s essential in checking out what is safe and comfortable, physically and emotionally. Negotiating our sexual practices can be both empowering and downright sexy. -

MEC Logo Proctitis
DINESH JAIN, M.D. RAVI NADIMPALLI, M.D. SCOTT BERGER, M.D. JENNIFER FRANKEL, M.D. SUSHAMA GUNDLAPALLI, M.D. GONZALO PANDOLFI, M.D. DARREN KASTIN, M.D. 1243 Rickert Dr. Telephone 630-527-6450 Naperville, IL 60540 Fax 630-527-6456 SGIHealth.com Proctitis What is proctitis? Proctitis is inflammation of the lining of the rectUm, the lower end of the large intestine leading to the anUs. The large intestine and anUs are part of the gastrointestinal (GI) tract. The GI tract is a series of hollow organs joined in a long, twisting tube from the moUth to the anUs. The movement of mUscles in the GI tract, along with the release of hormones and enzymes, allows for the digestion of food. With proctitis, inflammation of the rectal lining—called the rectal mUcosa—is Uncomfortable and sometimes painfUl. The condition may lead to bleeding or mUcoUs discharge from the rectum, among other symptoms. What causes proctitis? Proctitis has many caUses, inclUding acUte, or sUdden and short-term, and chronic, or long-lasting, conditions. Among the causes are the following: Sexually transmitted diseases (STDs). STDs that can be passed when a person is receiving anal sex are a common caUse of proctitis. Common STD infections that can caUse proctitis inclUde gonorrhea, chlamydia, syphilis, and herpes. Herpes-indUced proctitis may be particUlarly severe in people who are also infected with the HIV virUs. Non-STD infections. Infections that are not sexUally transmitted also can caUse proctitis. Salmonella and Shigella are examples of foodborne bacteria that can cause proctitis. Streptococcal proctitis sometimes occurs in children who have strep throat. -

Anterior Rectocele
Saint Mary’s Hospital Gynaecology Service - Warrell Unit Information for Patients Anterior Rectocele What is an anterior rectocele? An anterior rectocele is the name given to a pocket or bulge in the part of the bowel lying under the back wall of the vagina. It is a type of prolapse. Between the vagina and the rectum, there is a sheet of strong connective tissue which helps to support the vagina and rectum and stop one from bulging into the other. Weakness of this tissue allows the rectum to bulge forwards into the vagina during straining or having the bowels opened. This bulge is called an anterior rectocele. Some women have an anterior rectocele and are not bothered by it at all. For some women, it causes a bulge or lump in the vagina. Sometimes it can cause a sensation of needing to empty the bowels during intercourse. It can cause difficulty in getting a bowel movement to come out. Women may have a feeling that the stool is going forward into the vagina rather than coming out. They may need to put a finger into the vagina to help the bowels to empty and may have to return to the toilet several times because they are not able to fully empty the bowel all at once. How common is prolapse and anterior rectocele? Prolapse is very common. Most women who have had a baby will have small amounts of prolapse. Anterior rectoceles are also very common. About 10% of women (1 in 10) have prolapse that causes bothersome symptoms. What causes an anterior rectocele? We do not understand yet why some women get an anterior rectocele and others do not.