Sexual Health Information for Gay & Bisexual
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

The Anatomy of the Rectum and Anal Canal
BASIC SCIENCE identify the rectosigmoid junction with confidence at operation. The anatomy of the rectum The rectosigmoid junction usually lies approximately 6 cm below the level of the sacral promontory. Approached from the distal and anal canal end, however, as when performing a rigid or flexible sigmoid- oscopy, the rectosigmoid junction is seen to be 14e18 cm from Vishy Mahadevan the anal verge, and 18 cm is usually taken as the measurement for audit purposes. The rectum in the adult measures 10e14 cm in length. Abstract Diseases of the rectum and anal canal, both benign and malignant, Relationship of the peritoneum to the rectum account for a very large part of colorectal surgical practice in the UK. Unlike the transverse colon and sigmoid colon, the rectum lacks This article emphasizes the surgically-relevant aspects of the anatomy a mesentery (Figure 1). The posterior aspect of the rectum is thus of the rectum and anal canal. entirely free of a peritoneal covering. In this respect the rectum resembles the ascending and descending segments of the colon, Keywords Anal cushions; inferior hypogastric plexus; internal and and all of these segments may be therefore be spoken of as external anal sphincters; lymphatic drainage of rectum and anal canal; retroperitoneal. The precise relationship of the peritoneum to the mesorectum; perineum; rectal blood supply rectum is as follows: the upper third of the rectum is covered by peritoneum on its anterior and lateral surfaces; the middle third of the rectum is covered by peritoneum only on its anterior 1 The rectum is the direct continuation of the sigmoid colon and surface while the lower third of the rectum is below the level of commences in front of the body of the third sacral vertebra. -

The Male Reproductive System
Management of Men’s Reproductive 3 Health Problems Men’s Reproductive Health Curriculum Management of Men’s Reproductive 3 Health Problems © 2003 EngenderHealth. All rights reserved. 440 Ninth Avenue New York, NY 10001 U.S.A. Telephone: 212-561-8000 Fax: 212-561-8067 e-mail: [email protected] www.engenderhealth.org This publication was made possible, in part, through support provided by the Office of Population, U.S. Agency for International Development (USAID), under the terms of cooperative agreement HRN-A-00-98-00042-00. The opinions expressed herein are those of the publisher and do not necessarily reflect the views of USAID. Cover design: Virginia Taddoni ISBN 1-885063-45-8 Printed in the United States of America. Printed on recycled paper. Library of Congress Cataloging-in-Publication Data Men’s reproductive health curriculum : management of men’s reproductive health problems. p. ; cm. Companion v. to: Introduction to men’s reproductive health services, and: Counseling and communicating with men. Includes bibliographical references. ISBN 1-885063-45-8 1. Andrology. 2. Human reproduction. 3. Generative organs, Male--Diseases--Treatment. I. EngenderHealth (Firm) II. Counseling and communicating with men. III. Title: Introduction to men’s reproductive health services. [DNLM: 1. Genital Diseases, Male. 2. Physical Examination--methods. 3. Reproductive Health Services. WJ 700 M5483 2003] QP253.M465 2003 616.6’5--dc22 2003063056 Contents Acknowledgments v Introduction vii 1 Disorders of the Male Reproductive System 1.1 The Male -

Departmentof UROLOGY
DEPARTMENT of UROLOGY UPDATE New Treatments for Benign Prostatic Hyperplasia Expanded Choices Provide Relief for a Common Condition FALL 2008 Vol.19 | No.2 The symptoms of an enlarged prostate include a weak stream, trouble starting and gland, called benign prostatic hyper- stopping, the frequent feeling of needing to Clinical Update p. 4 plasia (BPH), are familiar to a substantial urinate, and the sense that the bladder isn’t Kidney Cancer Vaccine p. 5 proportion of men older than 50. empty after urination. About half of men in their 50s and 80-90 percent Erectile Dysfunction Research p. 5 “To some degree, BPH affects all men as they of those older than 80 have enlarged prostates, age,” says Allan Pantuck, MD, MS, associate Clinical Trials p. 6 caused by changes in hormone balance and cell professor and physician in the UCLA Integrative growth. As their prostate begins to squeeze or Profile: Oscar Rivera, LVN p. 8 Urology Program, which combines the best partially block the surrounding urethra — the of preventative approaches, medical counseling, Kudos p. 9 tube that carries the urine from the bladder out nutritional science, and complementary medical of the body — many of these men experience Donor Notes p. 9 approaches for patients interested in the bothersome urinary symptoms, which can prevention and treatment of urologic conditions. Profile: Arthur Schapiro p. 9 “The prostate forms a channel that the urine passes through as it comes out of the bladder. As the prostate enlarges, there is increased resistance to the bladder’s ability to empty. This tends to also lead to changes in the bladder, including a decreased ability to hold urine.” BPH can wreak havoc with quality of life — in addition to the discomfort, some men are forced to get up several times during the night. -
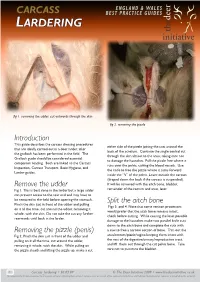
Introduction Remove the Udder Removing the Pizzle (Penis)
fig . removing the udder, cut outwards through the skin fig 2. removing the pizzle Introduction This guide describes the carcass dressing procedures either side of the pizzle joining the cuts around the that are ideally carried out in a deer larder, after back of the scrotum. Continue the single central cut the gralloch has been performed in the field. The through the skin almost to the anus, taking care not Gralloch guide should be considered essential to damage the haunches. Pull the pizzle free where it companion reading. Both are linked to the Carcass runs over the pelvis, cutting the blood vessels. Use Inspection, Carcass Transport, Basic Hygiene, and the knife to free the pizzle where it turns forward Larder guides. inside the “V” of the pelvis. Leave outside the carcass (draped down the back if the carcass is suspended). Remove the udder It will be removed with the aitch bone, bladder, Fig 1. This is best done in the larder but a large udder remainder of the rectum and anus, later. can prevent access to the rear end and may have to be removed in the field before opening the stomach. Split the aitch bone Pinch the skin just in front of the udder and pulling Figs 3. and 4. Note that some venison processors on it all the time, cut around the udder, removing it would prefer that the aitch bone remains intact, whole, with the skin. Do not take the cut any further check before cutting. While causing the least possible rearwards until back in the larder. -

Men's Health: a Guide to Preventing Infections
Men’s Health: A Guide to Preventing Infections Men’s Health: A Guide to Preventing Infections Infection: Don’t Pass It On (IDPIO) Infection: Don’t Pass It On Campaign VHA National Center for Health Promotion and Disease Prevention Veterans Health Administration Campaign Contributing Team National Center for Health Promotion and Disease Prevention (lead office) Occupational Health Services Patient Care Services Women Veterans Health Services Employee Education System National Infectious Diseases Service Office of Nursing Services VA National Center for Patient Safety Facility Health Care Professionals Men’s Health: A Guide to Preventing Infections Introduction We all want to stay healthy. And, we all want our friends and loved ones to be healthy too. Preventing infection is a good start. The first step is knowing how infections are spread. The second is learning how to prevent infection. The VHA National Center for Health Promotion and Disease Prevention along with the Infection: Don’t Pass It On Campaign are pleased to provide Men’s Health: A Guide to Preventing Infections. This guide provides an overview of infections ranging from the common cold to sexually transmitted infections. This information has been customized to address the health concerns and issues specific to men. I hope you will use this guide to learn how to reduce your risk of getting sick, which will also help stop the spread of illness to those around you. Veterans Health Administration i Men’s Health: A Guide to Preventing Infections Each section has information on: ◗ How the infection is spread. ◗ What the signs of infection are. ◗ How the infection is treated. -

Condomless Anal Sex
By the end of this session participants will have: • Understood why it is important to talk explicitly about anal sex with men by developing a greater awareness of the importance and meaning of anal sex for men. • Considered the language needed to talk to men about anal sex and what makes it a difficult topic to discuss. This means addressing personal feelings about talking with men about anal sex, condoms and condomless anal sex. • Considered what influences the opportunities men have to talk about anal sex in a sexual health service. • Identified the importance of a dialogue that is about feelings, intimacy, pleasure, vulnerability as well as safety, STI/HIV risk and testing. • Considered how to give advice and information tailored to the needs of the individual. “It is not surprising that sexuality is an area of life in which disgust often plays a role. Sex involves the exchange of bodily fluids, and it makes us bodily beings rather than angelic transcendent beings. So sex is a site of anxiety for anyone who is ambivalent about having an animal and mortal nature, and that includes many if not most people… What inspires disgust is typically the male thought of the male homosexual, imagined as anally penetrable.” Martha Nussbaum “The four most over-rated things in life are champagne, lobster, anal sex, and picnics.” Christopher Hitchens Discussion • How do you think anal sex is viewed in our culture? • Do you feel that societal views on anal sex might inform your professional practice? Useful language • In the HIV Prevention Needs Assessment the research team settled on using the word anal to mean anal sex/anal intercourse. -

Unreported in the Court of Special Appeals Of
UNREPORTED IN THE COURT OF SPECIAL APPEALS OF MARYLAND No. 0068 September Term, 2016 ______________________________________ CHARLES EDWARD GIBSON v. STATE OF MARYLAND ______________________________________ Arthur, Reed, Alpert, Paul E. (Senior Judge, Specially Assigned), JJ. ______________________________________ Opinion by Alpert, J. ______________________________________ Filed: December 5, 2016 *This is an unreported opinion, and it may not be cited in any paper, brief, motion, or other document filed in this Court or any other Maryland Court as either precedent within the rule of stare decisis or as persuasive authority. Md. Rule 1-104. ‒Unreported Opinion‒ Charles Gibson, appellant, was convicted by a jury sitting in the Circuit Court for Prince George’s County of three counts each of both first-degree sex offense and second-degree sex offense; four counts each of both first-degree assault and second-degree assault; and one count of carrying a concealed and dangerous weapon.1 Appellant asks two questions on appeal: I. Was the evidence sufficient to support his four convictions (first- and second-degree sex offense and first- and second-degree assault) regarding the fourth incident? II. Did the trial court err in limiting his cross-examination of the complaining witness? For the reasons that follow, we shall affirm. FACTS The State’s theory of prosecution was that on December 7, 2013, appellant sexually assaulted L.B. four times over several hours while the two were cell mates at Prince George’s County Detention Center (PGCDC). The first incident consisted of anal penetration by appellant with a baby oil bottle while the two men were locked in their cell after dinner. -

How to Increase Your Enjoyment of Sex
BETTER SEX BETTER SEX BETTER SEX BETTER SEX BETTER SEX OF SEX ENJO YOUR INCREASE HOW TO for women and women for their partners YMENT “Sexual health is a state of physical, emotional, mental and social well-being in relation to sexuality; it is not merely the absence of disease, dysfunction or infirmity. Sexual health requires a positive and respectful approach to sexuality and sexual relationships, as well as the possibility of having pleasurable and safe sexual experiences, free of coercion, discrimination and violence. For sexual health to be attained and maintained, the sexual rights of all persons must be respected, protected and fulfilled.” Definition of sexual health, World Health Organisation SAFER SEX Using condoms for penetrative sex is the best way to protect yourself and your partners from Sexually Transmitted Infections, including HIV. Condoms also offer good protection from unwanted pregnancy. In the text of this booklet, we have chosen not to refer constantly to the use of condoms. Instead, we encourage you to make your own decisions about protecting yourself and others in each instance of sexual activity you undertake. 1 HOW TO INCREASE YOUR ENJOYMENT OF SEX This leaflet provides information on how to help yourself improve your enjoyment of sex. It has three main parts: Suggestions on how to improve sex generally, without doing formal exercises. These apply to both casual and regular partners. Exercises you can do on your own — for women who have difficulty getting turned on or experiencing orgasm, and who may or may not have a regular partner. Exercises you can do with a partner — for women who have difficulty getting turned on, or who have difficulty having an orgasm or enjoying penetrative sex. -

GERONTOLOGICAL NURSE PRACTITIONER Review and Resource M Anual
13 Male Reproductive System Disorders Vaunette Fay, PhD, RN, FNP-BC, GNP-BC GERIATRIC APPRoACH Normal Changes of Aging Male Reproductive System • Decreased testosterone level leads to increased estrogen-to-androgen ratio • Testicular atrophy • Decreased sperm motility; fertility reduced but extant • Increased incidence of gynecomastia Sexual function • Slowed arousal—increased time to achieve erection • Erection less firm, shorter lasting • Delayed ejaculation and decreased forcefulness at ejaculation • Longer interval to achieving subsequent erection Prostate • By fourth decade of life, stromal fibrous elements and glandular tissue hypertrophy, stimulated by dihydrotestosterone (DHT, the active androgen within the prostate); hyperplastic nodules enlarge in size, ultimately leading to urethral obstruction 398 GERONTOLOGICAL NURSE PRACTITIONER Review and Resource M anual Clinical Implications History • Many men are overly sensitive about complaints of the male genitourinary system; men are often not inclined to initiate discussion, seek help; important to take active role in screening with an approach that is open, trustworthy, and nonjudgmental • Sexual function remains important to many men, even at ages over 80 • Lack of an available partner, poor health, erectile dysfunction, medication adverse effects, and lack of desire are the main reasons men do not continue to have sex • Acute and chronic alcohol use can lead to impotence in men • Nocturia is reported in 66% of patients over 65 – Due to impaired ability to concentrate urine, reduced -

Assessment of Lower Urinary Tract Symptoms in Younger Men
MEN’S HEALTH ASSESSMENT OF LOWER URINARY TRACT SYMPTOMS IN YOUNGER MEN Lower urinary tract symptoms (LUTS) are common in the ageing male and represent a significant burden on both the patient and the healthcare system worldwide. 1,2 Accordingly, the majority of clinical trials and guidelines focus on the older patient, despite the fact that men below these ages will also present with many of the same symptoms. In this review, the authors explore the challenges of assessing and managing men below 50 years with LUTS. Dr Odunayo The aetiology of LUTS is multifactorial with causes How common are LUTS Kalejaiye attributed to dysfunction of the bladder and its in younger men? Urology SpR outlet – including the prostate, urethra and sphincter; The EPIC study, 3 a population-based survey which the neurological innervation of the lower urinary recruited men aged over 18 years, found that the Professor tract, and medical co-morbidities.1,2 It is important prevalence of LUTS increased with age, from 51.3% Raj Persad to consider all these aspects when assessing patients. in men aged 18-39 years to 62% in those aged 40-59 While in older men, benign prostatic enlargement years. This is compared with a prevalence of 80.7% Consultant is the commonest cause of male LUTS, in younger in men aged 60 years or older. Storage symptoms Urologist; men this is unusual, and other diagnoses should be were commonest in men 39 years or younger, with a Honorary considered more likely. prevalence of 37.5%, compared with a prevalence of Professor of 19.9% for voiding symptoms in this age group. -

City Council Regular Meeting Agenda
Mayor Laura North City of Kingsburg Mayor Pro Tem Vince Palomar Council Member Michelle Roman 1401 Draper Street, Kingsburg, CA 93631-1908 Council Member Jewel Hurtado Phone (559)897-5821 Fax (559)897-5568 Council Member Brandon Pursell, Jr. City Manager Alexander J. Henderson AGENDA KINGSBURG CITY COUNCIL REGULAR MEETING Council Chamber, 1401 Draper Street, Kingsburg, CA 93631 (559) 897-5821 www.cityofkingsburg-ca.gov PURSUANT TO EXECUTIVE ORDER N-29-20 ISSUED BY GOVERNOR GAVIN NEWSOM THE COUNCIL CHAMBER WILL BE OPEN AT 50% CAPACITY (including City Council Members and City Staff) TO THE PUBLIC. PUBLIC WILL ALSO HAVE THE OPTION TO CALL 1 (425) 436-6335 PASSCODE 5290024 TO PROVIDE COMMENTS ON AGENDA ITEMS. WRITTEN COMMENTS CAN STILL BE SUBMITTED BY MAIL OR EMAIL TO APALSGAARD@CITYOFKINGSBURG- CA.GOV. THE CUT OFF FOR WRITTEN COMMENTS IS 05/18/2021 at 4:30pm. THEY WILL NOT BE READ OUT LOUD. Wednesday, May 19, 2021 at 6pm Invocation to be given by Pastor Tim Boynton, of The Kingsburg Covenant Church, followed by the Pledge of Allegiance led by Mayor Laura North. 6 P.M. REGULAR SESSION MEETING: 1. Call to Order and Roll Call 2. Public Comments: This is the time for any citizen to come forward and address the City Council on any issue within its jurisdiction that is not listed on the Agenda. A maximum of five (5) minutes is allowed for each speaker. 3. Approve Agenda: Action by the Council to approve the agenda or to make modifications. Items that can be added to the agenda is constrained by State law. -

Management of Male Lower Urinary Tract Symptoms (LUTS), Incl
Guidelines on the Management of Male Lower Urinary Tract Symptoms (LUTS), incl. Benign Prostatic Obstruction (BPO) M. Oelke (chair), A. Bachmann, A. Descazeaud, M. Emberton, S. Gravas, M.C. Michel, J. N’Dow, J. Nordling, J.J. de la Rosette © European Association of Urology 2013 TABLE OF CONTENTS PAGE 1. INTRODUCTION 6 1.1 References 7 2. ASSESSMENT 8 3. CONSERVATIVE TREATMENT 9 3.1 Watchful waiting - behavioural treatment 9 3.2 Patient selection 9 3.3 Education, reassurance, and periodic monitoring 9 3.4 Lifestyle advice 10 3.5 Practical considerations 10 3.6 Recommendations 10 3.7 References 10 4. DRUG TREATMENT 11 4.1 a1-adrenoceptor antagonists (a1-blockers) 11 4.1.1 Mechanism of action 11 4.1.2 Available drugs 11 4.1.3 Efficacy 12 4.1.4 Tolerability and safety 13 4.1.5 Practical considerations 14 4.1.6 Recommendation 14 4.1.7 References 14 4.2 5a-reductase inhibitors 15 4.2.1 Mechanism of action 15 4.2.2 Available drugs 16 4.2.3 Efficacy 16 4.2.4 Tolerability and safety 17 4.2.5 Practical considerations 17 4.2.6 Recommendations 18 4.2.7 References 18 4.3 Muscarinic receptor antagonists 19 4.3.1 Mechanism of action 19 4.3.2 Available drugs 20 4.3.3 Efficacy 20 4.3.4 Tolerability and safety 21 4.3.5 Practical considerations 22 4.3.6 Recommendations 22 4.3.7 References 22 4.4 Plant extracts - Phytotherapy 23 4.4.1 Mechanism of action 23 4.4.2 Available drugs 23 4.4.3 Efficacy 24 4.4.4 Tolerability and safety 26 4.4.5 Practical considerations 26 4.4.6 Recommendations 26 4.4.7 References 26 4.5 Vasopressin analogue - desmopressin 27 4.5.1