Posterior Repair with Perineoplasty
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

The Anatomy of the Rectum and Anal Canal
BASIC SCIENCE identify the rectosigmoid junction with confidence at operation. The anatomy of the rectum The rectosigmoid junction usually lies approximately 6 cm below the level of the sacral promontory. Approached from the distal and anal canal end, however, as when performing a rigid or flexible sigmoid- oscopy, the rectosigmoid junction is seen to be 14e18 cm from Vishy Mahadevan the anal verge, and 18 cm is usually taken as the measurement for audit purposes. The rectum in the adult measures 10e14 cm in length. Abstract Diseases of the rectum and anal canal, both benign and malignant, Relationship of the peritoneum to the rectum account for a very large part of colorectal surgical practice in the UK. Unlike the transverse colon and sigmoid colon, the rectum lacks This article emphasizes the surgically-relevant aspects of the anatomy a mesentery (Figure 1). The posterior aspect of the rectum is thus of the rectum and anal canal. entirely free of a peritoneal covering. In this respect the rectum resembles the ascending and descending segments of the colon, Keywords Anal cushions; inferior hypogastric plexus; internal and and all of these segments may be therefore be spoken of as external anal sphincters; lymphatic drainage of rectum and anal canal; retroperitoneal. The precise relationship of the peritoneum to the mesorectum; perineum; rectal blood supply rectum is as follows: the upper third of the rectum is covered by peritoneum on its anterior and lateral surfaces; the middle third of the rectum is covered by peritoneum only on its anterior 1 The rectum is the direct continuation of the sigmoid colon and surface while the lower third of the rectum is below the level of commences in front of the body of the third sacral vertebra. -

Physiology of Female Sexual Function and Dysfunction
International Journal of Impotence Research (2005) 17, S44–S51 & 2005 Nature Publishing Group All rights reserved 0955-9930/05 $30.00 www.nature.com/ijir Physiology of female sexual function and dysfunction JR Berman1* 1Director Female Urology and Female Sexual Medicine, Rodeo Drive Women’s Health Center, Beverly Hills, California, USA Female sexual dysfunction is age-related, progressive, and highly prevalent, affecting 30–50% of American women. While there are emotional and relational elements to female sexual function and response, female sexual dysfunction can occur secondary to medical problems and have an organic basis. This paper addresses anatomy and physiology of normal female sexual function as well as the pathophysiology of female sexual dysfunction. Although the female sexual response is inherently difficult to evaluate in the clinical setting, a variety of instruments have been developed for assessing subjective measures of sexual arousal and function. Objective measurements used in conjunction with the subjective assessment help diagnose potential physiologic/organic abnormal- ities. Therapeutic options for the treatment of female sexual dysfunction, including hormonal, and pharmacological, are also addressed. International Journal of Impotence Research (2005) 17, S44–S51. doi:10.1038/sj.ijir.3901428 Keywords: female sexual dysfunction; anatomy; physiology; pathophysiology; evaluation; treatment Incidence of female sexual dysfunction updated the definitions and classifications based upon current research and clinical practice. -
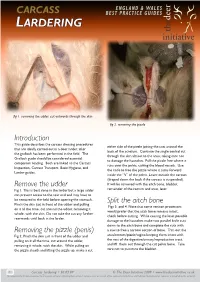
Introduction Remove the Udder Removing the Pizzle (Penis)
fig . removing the udder, cut outwards through the skin fig 2. removing the pizzle Introduction This guide describes the carcass dressing procedures either side of the pizzle joining the cuts around the that are ideally carried out in a deer larder, after back of the scrotum. Continue the single central cut the gralloch has been performed in the field. The through the skin almost to the anus, taking care not Gralloch guide should be considered essential to damage the haunches. Pull the pizzle free where it companion reading. Both are linked to the Carcass runs over the pelvis, cutting the blood vessels. Use Inspection, Carcass Transport, Basic Hygiene, and the knife to free the pizzle where it turns forward Larder guides. inside the “V” of the pelvis. Leave outside the carcass (draped down the back if the carcass is suspended). Remove the udder It will be removed with the aitch bone, bladder, Fig 1. This is best done in the larder but a large udder remainder of the rectum and anus, later. can prevent access to the rear end and may have to be removed in the field before opening the stomach. Split the aitch bone Pinch the skin just in front of the udder and pulling Figs 3. and 4. Note that some venison processors on it all the time, cut around the udder, removing it would prefer that the aitch bone remains intact, whole, with the skin. Do not take the cut any further check before cutting. While causing the least possible rearwards until back in the larder. -

How to Increase Your Enjoyment of Sex
BETTER SEX BETTER SEX BETTER SEX BETTER SEX BETTER SEX OF SEX ENJO YOUR INCREASE HOW TO for women and women for their partners YMENT “Sexual health is a state of physical, emotional, mental and social well-being in relation to sexuality; it is not merely the absence of disease, dysfunction or infirmity. Sexual health requires a positive and respectful approach to sexuality and sexual relationships, as well as the possibility of having pleasurable and safe sexual experiences, free of coercion, discrimination and violence. For sexual health to be attained and maintained, the sexual rights of all persons must be respected, protected and fulfilled.” Definition of sexual health, World Health Organisation SAFER SEX Using condoms for penetrative sex is the best way to protect yourself and your partners from Sexually Transmitted Infections, including HIV. Condoms also offer good protection from unwanted pregnancy. In the text of this booklet, we have chosen not to refer constantly to the use of condoms. Instead, we encourage you to make your own decisions about protecting yourself and others in each instance of sexual activity you undertake. 1 HOW TO INCREASE YOUR ENJOYMENT OF SEX This leaflet provides information on how to help yourself improve your enjoyment of sex. It has three main parts: Suggestions on how to improve sex generally, without doing formal exercises. These apply to both casual and regular partners. Exercises you can do on your own — for women who have difficulty getting turned on or experiencing orgasm, and who may or may not have a regular partner. Exercises you can do with a partner — for women who have difficulty getting turned on, or who have difficulty having an orgasm or enjoying penetrative sex. -

Prevalence of Malignant Uterine Pathology in Utero-Vaginal Prolapse After Vaginal Hysterectomy
Pelviperineology Pelviperineology Pelviperineology Pelviperineology Pelviperineology Pelviperineology Pelviperineology Pelviperineology Pelviperineology Pelviperineology Pelviperineology Pelviperineology Pelviperineology Pelviperineology Pelviperineology Pelviperineology Pelviperineology Pelviperineology Pelviperineology Pelviperineology Pelviperineology Pelviperineology Pelviperineology Pelviperineology Pelviperineology Pelviperineology Pelviperineology Pelviperineology Pelviperineology Pelviperineology Pelviperineology Pelviperineology Pelviperineology Pelviperineology Pelviperineology Pelviperineology PelviperineologyORIGINAL Pelviperineology ARTICLE Pelviperineology Pelviperineology Pelviperineology Pelviperineology Pelviperineology Pelviperineology Pelviperineology Pelviperineology Pelviperineology Pelviperineology DOI: 10.34057/PPj.2020.39.04.006 Pelviperineology 2020;39(4):137-141 Prevalence of malignant uterine pathology in utero-vaginal prolapse after vaginal hysterectomy EDGARDO CASTILLO-PINO1, VALENTINA ACEVEDO1, NATALIA BENAVIDES1, VALERIA ALONSO1, WASHIGNTON LAURÍA2 1Department of Obstetrics and Gynaecology, Urogynaecology and Pelvic Floor Unit, School of Medicine, University of the Republic, Hospital de Clínicas “Dr. Manuel Quintela”, Montevideo, Uruguay 2Department of Obstetrics and Gynaecology, School of Medicine, University of the Republic, Hospital de Clínicas “Dr. Manuel Quintela”, Montevideo, Uruguay ABSTRACT Objective: The aim of this study was to establish the prevalence of malignant uterine pathology after vaginal -

Masturbation
MASTURBATION Curriculum for Excellence Links to health and wellbeing outcomes for Relationships, Sexual Health and Parenthood I am aware of my growing body and I am learning the correct names for its different parts and how they work. HWB 0-47b HWB 1-47b I understand my own body's uniqueness, my developing sexuality, and that of others. HWB 3-47a HWB 4-47a Introduction Masturbation can seem a daunting subject to teach, but it is very important for young people to learn about appropriate touch. School provides an ideal learning environment for this, alongside an opportunity to work alongside parents to tackle this issue. If young people do not learn about masturbation and appropriate touch when they are teenagers, they are in danger of displaying inappropriate behaviour as an adult, often in public, which can lead to more serious repercussions. Staff may worry that teaching about masturbation can provoke a sudden obsession with genitalia, but this is usually a temporary reaction and one which can be successfully dealt with by one-to-one work through Social Stories. Having a policy on Managing Sexualised Behaviour may also be beneficial, outlining an approach to inappropriate touching in the classroom. TOUCHING OURSELVES You will need 2 body outlines/ Bodyboards (male and female). Recap on names of Parts Of The Body. Ask the students which are PRIVATE BODY parts (those covered by underwear- breasts, penis, vagina, anus, clitoris etc.) Tell the group ‘’these are Private Body Parts, not for everyone to touch and see. But sometimes people like to touch their own private body parts to make themselves feel nice and sexy. -

Female Pelvic Relaxation
FEMALE PELVIC RELAXATION A Primer for Women with Pelvic Organ Prolapse Written by: ANDREW SIEGEL, M.D. An educational service provided by: BERGEN UROLOGICAL ASSOCIATES N.J. CENTER FOR PROSTATE CANCER & UROLOGY Andrew Siegel, M.D. • Martin Goldstein, M.D. Vincent Lanteri, M.D. • Michael Esposito, M.D. • Mutahar Ahmed, M.D. Gregory Lovallo, M.D. • Thomas Christiano, M.D. 255 Spring Valley Avenue Maywood, N.J. 07607 www.bergenurological.com www.roboticurology.com Table of Contents INTRODUCTION .................................................................1 WHY A UROLOGIST? ..........................................................2 PELVIC ANATOMY ..............................................................4 PROLAPSE URETHRA ....................................................................7 BLADDER .....................................................................7 RECTUM ......................................................................8 PERINEUM ..................................................................9 SMALL INTESTINE .....................................................9 VAGINAL VAULT .......................................................10 UTERUS .....................................................................11 EVALUATION OF PROLAPSE ............................................11 SURGICAL REPAIR OF PELVIC PROLAPSE .....................15 STRESS INCONTINENCE .........................................16 CYSTOCELE ..............................................................18 RECTOCELE/PERINEAL LAXITY .............................19 -

Evidence Review No: 1
Local Policy Statement No 12 POLICY STATEMENT TITLE/TOPIC: Specific Obstetric and Gynaecology procedures ISSUE DATE: November 2011 1) INSERTION AND REMOVAL OF INTRA UTERINE CONTRACEPTIVE DEVICES (IUCD) DEFINITION An IUCD is a birth control device that is placed in the uterus by a doctor. Although they can come in different shapes and sizes, IUCDs are generally about 1 1/2 inches long, in the shape of a T, and have a copper coating. IUCDs have strings that extend from the device in the uterus, through the cervix and into the vagina. They can be felt to ensure that the IUCD is still in place, but they cannot be seen outside of the body There are two types of IUCDs: those that release progestin and those that do not. COMMISSIONING RECOMMENDATION: The insertion and removal of any IUCD should only be undertaken in a primary care setting, it is not commissioned as a secondary care service RISKS IUCDs do not protect against sexually transmitted diseases (STDs). Women who get an STD while using an IUCD are also more likely to develop pelvic inflammatory disease (PID). In 2 percent to 10 percent of cases, the uterus will push the IUCD out of the body. Fever and chills are other side effects. IUCDs cause cramps and backaches in some women. Heavier bleeding than normal and spotting are also common side effects, though this usually only lasts for the first few months. There is a greater risk of having an ectopic pregnancy with an IUCD than without one. 2) VAGINAL PESSARIES DEFINITION A vaginal pessary is a plastic device that fits into the vagina to help support the uterus (womb), vagina, bladder or rectum. -

The Mythical G-Spot: Past, Present and Future by Dr
Global Journal of Medical research: E Gynecology and Obstetrics Volume 14 Issue 2 Version 1.0 Year 2014 Type: Double Blind Peer Reviewed International Research Journal Publisher: Global Journals Inc. (USA) Online ISSN: 2249-4618 & Print ISSN: 0975-5888 The Mythical G-Spot: Past, Present and Future By Dr. Franklin J. Espitia De La Hoz & Dra. Lilian Orozco Santiago Universidad Militar Nueva Granada, Colombia Summary- The so-called point Gräfenberg popularly known as "G-spot" corresponds to a vaginal area 1-2 cm wide, behind the pubis in intimate relationship with the anterior vaginal wall and around the urethra (complex clitoral) that when the woman is aroused becomes more sensitive than the rest of the vagina. Some women report that it is an erogenous area which, once stimulated, can lead to strong sexual arousal, intense orgasms and female ejaculation. Although the G-spot has been studied since the 40s, disagreement persists regarding the translation, localization and its existence as a distinct structure. Objective: Understand the operation and establish the anatomical points where the point G from embryology to adulthood. Methodology: A literature search in the electronic databases PubMed, Ovid, Elsevier, Interscience, EBSCO, Scopus, SciELO was performed. Results: descriptive articles and observational studies were reviewed which showed a significant number of patients. Conclusion: Sexual pleasure is a right we all have, and women must find a way to feel or experience orgasm as a possible experience of their sexuality, which necessitates effective stimulation. Keywords: G Spot; vaginal anatomy; clitoris; skene’s glands. GJMR-E Classification : NLMC Code: WP 250 TheMythicalG-SpotPastPresentandFuture Strictly as per the compliance and regulations of: © 2014. -

Bowel Function Anatomy
BOWEL FUNCTION ANATOMY Most of America gives little thought to bowel control. However, bowel control is actually a complex process involving the coordination of many different muscles and nerves. The bowel is considered to be a part of the digestive or gastrointestinal system. It is designed to help the body absorb nutrients and fluids from the foods we eat and drink. After taking out everything the body needs, the bowel then expels the leftover waste. The beginning of the bowel is the small intestine, sometimes referred to as the small bowel. This is where the useful nutrients are absorbed from what you eat. The small bowel delivers the waste to the colon, or large bowel. The colon is a 5-6 foot long muscular tube that delivers stool to the rectum. As the stool moves through the colon, the fluids are removed and absorbed into the body. The consistency of the stool is dependent upon many things, including how long the stool sits in the colon, how much of the water has been absorbed from the waste, and the amount of fiber and fluids in your diet. Stool consistency can vary from hard lumps to mushy to very loose, watery stool. The best and easiest consistency of stool is soft, like toothpaste; this consistency may be attained by adding fiber to your diet. Fiber helps move waste through the colon because it is indigestible by the human body. In other words, fiber adds ‘bulk’ to the stool. It is important to eat a diet high in fiber, however, most Americans lack fiber in their diet. -

Anal Sex an Informative Guide by Bedroom Kandi
AN INTRODUCTION TO ANAL SEX AN INFORMATIVE GUIDE BY BEDROOM KANDI Anal sex encompasses a variety of sexual acts involving the anus and rectum. These can include anal fingering, analingus (oral-anal sex, sometimes called “rimming”), anal insertion (using an object like a strap-on or other toy) and anal intercourse (penis-in-anus sex). Anal sex can be enjoyed by individuals of any gender, and any orientation. Everyone has a back door, after all! But it requires preparation, care, and patience to make it pleasurable. Communication is Key! No surprise butt-sex. Always check in with your partner, talk things through, and 36% communicate about whether you’re Of American Women both on board for trying anal. Check in during anal sex to report having tried ? make sure you’re both enjoying yourselves! ANAL SEX “Is Anal Sex Common?” International Society for Sexual Medicine :) http://www.issm.info/sexual-health-qa/is-anal-sex-common/ www.bedroomkandi.com ©2017 Bedroom Kandi WHY TRY ANAL? IT FEELS GOOD - There are a lot IT FEELS BAD - in a good way! The of nerve endings to stimulate around taboos around anal sex can make it a the anus, including those in the man’s thrill and add something exciting to your prostate. bedroom routine. You naughty thing! IT SPICES THINGS UP - Trying IT CAN SUBVERT GENDER new things keeps things fresh, and ROLES - Either partner can penetrate anal sex will open up a whole new or receive, (using strap-ons or other toys range of sexual positions and activities for Lesbian or Straight couples), so you for you and your partner to share. -

FAQ042 -- You and Your Sexuality (Especially for Teens)
AQ FREQUENTLY ASKED QUESTIONS FAQ042 fESPECIALLY FOR TEENS You and Your Sexuality (Especially for Teens) • What happens during puberty? • What emotional changes occur during puberty? • How are sexual feelings expressed? • What is masturbation? • What is oral sex? • What happens during sexual intercourse? • What can I do if I want to have sexual intercourse but I do not want to get pregnant? • How can I protect myself and my partner from sexual transmitted infections during sexual intercourse? • What is anal sex? • What does it mean to be gay, lesbian, or bisexual? • Can I choose to be attracted to someone of the same sex? • What is gender identity? • When deciding whether to have sex, what are some things to consider? • What if I decide to wait and someone tries to pressure me into sex? • What is rape? • What are some things I can do to help protect myself against rape? • What is intimate partner violence? • Glossary What happens during puberty? When puberty starts, your brain sends signals to certain parts of the body to start growing and changing. These signals are called hormones. Hormones make your body change and start looking more like an adult’s (see FAQ041 “Your Changing Body—Especially for Teens”). Hormones also can cause emotional changes. What emotional changes occur during puberty? During your teen years, hormones can cause you to have strong feelings, including sexual feelings. You may have these feelings for someone of the other sex or the same sex. Thinking about sex or just wanting to hear or read about sex is normal. It is normal to want to be held and touched by others.