Urological Infections
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Second and Third Generation Oral Fluoroquinolones
Therapeutic Class Overview Second and Third Generation Oral Fluoroquinolones Therapeutic Class • Overview/Summary: The second and third generation quinolones are approved to treat a variety of infections, including dermatologic, gastrointestinal, genitourinary, respiratory, as well as several miscellaneous infections.1-10 They are broad-spectrum agents that directly inhibit bacterial deoxyribonucleic acid (DNA) synthesis by blocking the actions of DNA gyrase and topoisomerase IV, which leads to bacterial cell death.11,12 The quinolones are most active against gram-negative bacilli and gram-negative cocci.12 Ciprofloxacin has the most potent activity against gram-negative bacteria. Norfloxacin, ciprofloxacin and ofloxacin have limited activity against streptococci and many anaerobes while levofloxacin and moxifloxacin have greater potency against gram-positive cocci, and moxifloxacin has enhanced activity against anaerobic bacteria.11-12 Gemifloxacin, levofloxacin and moxifloxacin are considered respiratory fluoroquinolones. They possess enhanced activity against Streptococcus pneumoniae while maintaining efficacy against Haemophilus influenzae, Moraxella catarrhalis and atypical pathogens. Resistance to the quinolones is increasing and cross-resistance among the various agents has been documented. Two mechanisms of bacterial resistance have been identified. These include mutations in chromosomal genes (DNA gyrase and/or topoisomerase IV) and altered drug permeability across the bacterial cell membranes.11-12 Clinical Guidelines support -

A TWO-YEAR RETROSPECTIVE ANALYSIS of ADVERSE DRUG REACTIONS with 5PSQ-031 FLUOROQUINOLONE and QUINOLONE ANTIBIOTICS 24Th Congress Of
A TWO-YEAR RETROSPECTIVE ANALYSIS OF ADVERSE DRUG REACTIONS WITH 5PSQ-031 FLUOROQUINOLONE AND QUINOLONE ANTIBIOTICS 24th Congress of V. Borsi1, M. Del Lungo2, L. Giovannetti1, M.G. Lai1, M. Parrilli1 1 Azienda USL Toscana Centro, Pharmacovigilance Centre, Florence, Italy 2 Dept. of Neurosciences, Psychology, Drug Research and Child Health (NEUROFARBA), 27-29 March 2019 Section of Pharmacology and Toxicology , University of Florence, Italy BACKGROUND PURPOSE On 9 February 2017, the Pharmacovigilance Risk Assessment Committee (PRAC) initiated a review1 of disabling To review the adverse drugs and potentially long-lasting side effects reported with systemic and inhaled quinolone and fluoroquinolone reactions (ADRs) of antibiotics at the request of the German medicines authority (BfArM) following reports of long-lasting side effects systemic and inhaled in the national safety database and the published literature. fluoroquinolone and quinolone antibiotics that MATERIAL AND METHODS involved peripheral and central nervous system, Retrospective analysis of ADRs reported in our APVD involving ciprofloxacin, flumequine, levofloxacin, tendons, muscles and joints lomefloxacin, moxifloxacin, norfloxacin, ofloxacin, pefloxacin, prulifloxacin, rufloxacin, cinoxacin, nalidixic acid, reported from our pipemidic given systemically (by mouth or injection). The period considered is September 2016 to September Pharmacovigilance 2018. Department (PVD). RESULTS 22 ADRs were reported in our PVD involving fluoroquinolone and quinolone antibiotics in the period considered and that affected peripheral or central nervous system, tendons, muscles and joints. The mean patient age was 67,3 years (range: 17-92 years). 63,7% of the ADRs reported were serious, of which 22,7% caused hospitalization and 4,5% caused persistent/severe disability. 81,8% of the ADRs were reported by a healthcare professional (physician, pharmacist or other) and 18,2% by patient or a non-healthcare professional. -

Urinary Incontinence Embarrassing but Treatable 2015 Rev
This information provides a general overview on this topic and may not apply to Health Notes everyone. To find out if this information applies to you and to get more information on From Your Family Doctor this subject, talk to your family doctor. Urinary incontinence Embarrassing but treatable 2015 rev. What is urinary incontinence? Are there different types Urinary incontinence means that you can’t always of incontinence? control when you urinate, or pee. The amount of leakage Yes. There are five types of urinary incontinence. can be small—when you sneeze, cough, or laugh—or large, due to very strong urges to urinate that are hard to Stress incontinence is when urine leaks because of control. This can be embarrassing, but it can be treated. sudden pressure on your lower stomach muscles, such as when you cough, sneeze, laugh, rise from a Millions of adults in North America have urinary chair, lift something, or exercise. Stress incontinence incontinence. It’s most common in women over 50 years usually occurs when the pelvic muscles are weakened, of age, but it can also affect younger people, especially sometimes by childbirth, or by prostate or other pelvic women who have just given birth. surgery. Stress incontinence is common in women. Be sure to talk to your doctor if you have this problem. Urge incontinence is when the need to urinate comes on If you hide your incontinence, you risk getting rashes, too fast—before you can get to a toilet. Your body may only sores, and skin and urinary tract (bladder) infections. -

Review of Systems
code: GF004 REVIEW OF SYSTEMS First Name Middle Name / MI Last Name Check the box if you are currently experiencing any of the following : General Skin Respiratory Arthritis/Rheumatism Abnormal Pigmentation Any Lung Troubles Back Pain (recurrent) Boils Asthma or Wheezing Bone Fracture Brittle Nails Bronchitis Cancer Dry Skin Chronic or Frequent Cough Diabetes Eczema Difficulty Breathing Foot Pain Frequent infections Pleurisy or Pneumonia Gout Hair/Nail changes Spitting up Blood Headaches/Migraines Hives Trouble Breathing Joint Injury Itching URI (Cold) Now Memory Loss Jaundice None Muscle Weakness Psoriasis Numbness/Tingling Rash Obesity Skin Disease Osteoporosis None Rheumatic Fever Weight Gain/Loss None Cardiovascular Gastrointestinal Eyes - Ears - Nose - Throat/Mouth Awakening in the night smothering Abdominal Pain Blurring Chest Pain or Angina Appetite Changes Double Vision Congestive Heart Failure Black Stools Eye Disease or Injury Cyanosis (blue skin) Bleeding with Bowel Movements Eye Pain/Discharge Difficulty walking two blocks Blood in Vomit Glasses Edema/Swelling of Hands, Feet or Ankles Chrohn’s Disease/Colitis Glaucoma Heart Attacks Constipation Itchy Eyes Heart Murmur Cramping or pain in the Abdomen Vision changes Heart Trouble Difficulty Swallowing Ear Disease High Blood Pressure Diverticulosis Ear Infections Irregular Heartbeat Frequent Diarrhea Ears ringing Pain in legs Gallbladder Disease Hearing problems Palpitations Gas/Bloating Impaired Hearing Poor Circulation Heartburn or Indigestion Chronic Sinus Trouble Shortness -

Overactive Bladder
Overactive Bladder Introduction Symptoms You Might Notice “Overactive bladder” (OAB) or “unstable bladder” • A strong urge to urinate with little warning. refers to the feeling of needing to urinate much more • More frequent urination. often than is average. Since a medical name for the • Possible dribbling or loss of a large amount of urine. bladder muscle is the “detrusor,” you may also hear this • Difficulty postponing urination. This becomes a major condition called names like “detrusor overactivity” or issue for people with OAB, and can limit activities and “detrusor instability.” travel. OAB is a complex problem, but generally, the • Usually, no physical pain is associated with this bladder may contract/squeeze prematurely and hard problem, but it can be very emotionally and socially enough to make urine leak out before you can make it to disturbing. the bathroom. This type of urine loss is called “urge • Need to get up more than once at night to urinate. incontinence.” • Some people may experience an uncomfortable OAB can occur at any age. Some people are born sensation of urgency. with conditions that affect nerve and muscle signals, resulting in frequent urination, accidents, and bed Possible Causes Your Health Care Provider wetting in children. Other people may not develop OAB May Look For until they are older. The body and its muscles change • Usually no outward physical signs of OAB. with aging, making OAB quite common in older adults. • In older men, this type of bladder problem may be Additionally, certain disease processes or treatments associated with prostate enlargement. may change the bladder to be more sensitive, leading to • In older women, OAB may be related to skin, blood OAB symptoms. -

Urinary System
Urinary system Urinary system terms Nephr/o, Kidney Nephritis, renal artery ren/o Hydronephrosis (abnormal condition involving back Hydro/o Water up of urine into the kidney Cystitis, cystectomy (inflammation of, removal of Cyst/o Bladder bladder) Pyel/o Renal collecting ducts Pyelogram (X-ray of the collecting ducts) Polyuria, anuria (frequent urination, no urine Ur/o, -uria Urine formation) Olig/o Scanty, less than normal Oliguria (reduced urine formation) To surgically reattach, fix in Nephropexy (surgically attach kidney in normal -pexy normal position anatomical position) Urinary system diseases Nephrosis – a noninflammatory disease of kidneys. Nephrolith – a kidney stone. Urethritis – inflammation of the urethra, the final pathway for urine in both sexes, and the common pathway for urine and semen in the male. Nocturia – frequently getting up and urinating during the night. Enuresis – involuntary release of urine, most often in reference to “bedwetting.” Urinary system procedures Nephrologist – I am hoping by now, you would know this is a physician specializing in kidney diseases. Urologist – a physician specializing in the genitourinary tract, which includes kidneys, urinary bladder and urethra of both men and women and the prostate and testes in men. Cystoscopy – looking into the urinary bladder with a fiberoptic instrument. Intravenous pyelogram – special X-rays showing the drainage pattern of the kidneys. A dye opaque to X-rays is injected into a vein. After a waiting period for the blood and dye to pass through the kidneys, X-rays can be taken of the collecting system of the kidney, ureter and bladder. Retrograde pyelogram – personally, I prefer the former procedure! In this procedure a dye opaque to X-rays is flushed backwards up the urethra and bladder and up the ureters to the kidneys. -

Frequently Asked Questions About Overactive Bladder
ABOUT OAB Frequently Asked Questions about Overactive Bladder What is Overactive Bladder (OAB)? If you live with OAB, you may also: Overactive Bladder (OAB) isn’t a disease. It’s the u Leak urine (incontinence): Sometimes people name of a group of urinary symptoms. The most with OAB also have “urgency incontinence.” common symptom of OAB is a sudden urge to This means that urine leaks when you feel urinate that you can’t control. Some people will the sudden urge to go. This isn’t the same as leak urine when they feel this urge. Having to “stress urinary incontinence” or “SUI.” People urinate many times during the day and night is with SUI leak urine while sneezing, laughing or another symptom of OAB. doing other physical activities. (You can learn more about SUI at UrologyHealth.org/SUI.) How common is OAB? u Urinate frequently: You may also need to go OAB is common. It affects millions of Americans. to the bathroom many times during the day. As many as 30 percent of men and 40 percent The number of times someone urinates varies of women in the United States live with OAB from person to person. But many experts symptoms. agree that going to the bathroom more than eight times in 24 hours is “frequent urination.” Who is at risk for OAB? u Wake up at night to urinate: Waking from As you grow older, you’re at higher risk for sleep to go to the bathroom more than once a OAB. But no matter what your age, there are night is another symptom of OAB. -

Nitrofurantoin Administration for the Prevention of Short-Term Catheter
Study Title: Nitrofurantoin Administration for the Prevention of Short-Term Catheter Associated Urinary Tract Infection After Pelvic Surgery (NAUTICA): A Randomized Controlled Trial ClinicalTrials.gov ID: NCT03287089 Date: July 6, 2018 STUDY OBJECTIVES Primary Objective To evaluate the efficacy of administration of nitrofurantoin prophylaxis after catheter discontinuation for the prevention of catheter-associated urinary tract infections in patients with postoperative short-term catheterization following pelvic reconstructive surgery. The primary outcome will be the treatment of clinically suspected and/or culture-proven UTI within 30 days of surgery. Secondary Objectives 1. To evaluate adverse outcomes related to study medications in each group 2. To evaluate medication compliance BACKGROUND Urinary tract infections (UTI) are the most common hospital-acquired infections, accounting for nearly 30% of cases of nosocomial infections and affecting nearly 1 million people per year.1-3 They account for nearly 8.1 million visits to health care providers and cost an estimated $1.6 billion a year in the United States alone.3,4 Following pelvic reconstructive and urinary incontinence surgery, UTIs are one of the most common complications.4,5 The baseline risk of UTI associated with pelvic floor surgery ranges between 5-35%, increasing greatly with catheterization.3 In women who are undergoing surgery for urinary incontinence, the risk of UTI ranges between 8.9% to 34%.4,6,7 Risk factors for urinary tract infections in women undergoing pelvic floor -
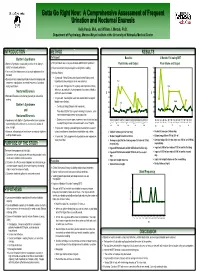
Gotta Gotta Go Right Now: a Comprehensive Assessment of Frequent Urination and Nocturnal Enuresis
Gotta Go Right Now: A Comprehensive Assessment of Frequent Urination and Nocturnal Enuresis Kelly Haack, M.A., and William J. Warzak, Ph.D. Department of Psychology, Munroe-Meyer Institute at the University of Nebraska Medical Center INTRODUCTION METHOD RESULTS Participant Bartter’s Syndrome Baseline 2 Months Following BRT ¾ Bartter’s Syndrome is caused by a defect in the kidney’s ¾ The participant was a 14-year-old male with Bartter’s Syndrome. Fluid Intake and Output Fluid Intake and Output ability to reabsorb potassium. ¾ He presented with frequent daytime and nighttime voiding. 1000 1000 ¾ As a result, the kidneys remove too much potassium from ¾ Medical History: 900 900 the body. 4 years old: Renal Ultrasound showed normal kidneys and 800 800 ¾ Excessive loss of potassium leads to muscle cramping and hypokalemia (low potassium level) was ruled out. Intake weakness, constipation, increased frequency of urination, 700 700 Intake and growth failure. 11 years old: Ditropan XL 10 mg daily and Imipramine 35 mg 600 600 daily were prescribed to treat symptoms of overactive bladder, Nocturnal Enuresis 500 500 ML such as frequent urination. ML ¾ Nocturnal Enuresis is involuntary passing of urine while 12 years old: Neurological exam was normal and neurogenic 400 400 asleep. bladder was ruled out. 300 300 Output Bartter’s Syndrome Output • Continued taking Ditropan and Imipramine. 200 200 and • Prescribed DDAVP 0.6 mg each evening to increase urine 100 100 concentration and decrease urine production. Nocturnal Enuresis 0 0 ¾ Adolescents with Bartter’s Syndrome often have a problem • Started use of a urine alarm; however, it was a short trial and 3:00 6:00 7:45 9:45 1:00 2:30 4:00 5:00 6:20 8:00 9:30 1:00 2:45 5:00 7:00 9:00 2:00 4:00 5:00 7:00 9:00 1:45 4:00 7:00 4:00 7:05 9:45 2:00 4:00 5:45 7:00 9:30 2:30 5:00 7:45 2:30 4:30 7:00 9:30 1:45 5:00 12:00 11:00 11:00 10:45 12:00 10:00 12:00 concentrating urine and excrete an excessive volume of he slept through it and continued to wet 5 out of 7 nights. -

Bacterial Prostatitis
REVIEW CURRENT OPINION Bacterial prostatitis Bradley C. Gill a,b and Daniel A. Shoskesa,b Purpose of review The review provides the infectious disease community with a urologic perspective on bacterial prostatitis. Specifically, the article briefly reviews the categorization of prostatitis by type and provides a distillation of new findings published on bacterial prostatitis over the past year. It also highlights key points from the established literature. Recent findings Cross-sectional prostate imaging is becoming more common and may lead to more incidental diagnoses of acute bacterial prostatitis. As drug resistance remains problematic in this condition, the reemergence of older antibiotics such as fosfomycin, has proven beneficial. With regard to chronic bacterial prostatitis, no clear clinical risk factors emerged in a large epidemiological study. However, bacterial biofilm formation has been associated with more severe cases. Surgery has a limited role in bacterial prostatitis and should be reserved for draining of a prostatic abscess or the removal of infected prostatic stones. Summary Prostatitis remains a common and bothersome clinical condition. Antibiotic therapy remains the basis of treatment for both acute and chronic bacterial prostatitis. Further research into improving prostatitis treatment is indicated. Keywords acute bacterial prostatitis, bacterial prostatitis, category I prostatitis, category II prostatitis, chronic bacterial prostatitis, male pelvic pain INTRODUCTION and August 2015 were identified among the first Prostatitis is a bothersome condition but carries 600 search results. The titles of English language potential for serious morbidity from sepsis, abscess, articles were examined and those pertaining to non- or fistula if insufficiently managed. Nearly one in six bacterial prostatitis, chronic pelvic pain, and animal men report a history of prostatitis, resulting in over or basic science models were excluded. -

Computational Antibiotics Book
Andrew V DeLong, Jared C Harris, Brittany S Larcart, Chandler B Massey, Chelsie D Northcutt, Somuayiro N Nwokike, Oscar A Otieno, Harsh M Patel, Mehulkumar P Patel, Pratik Pravin Patel, Eugene I Rowell, Brandon M Rush, Marc-Edwin G Saint-Louis, Amy M Vardeman, Felicia N Woods, Giso Abadi, Thomas J. Manning Computational Antibiotics Valdosta State University is located in South Georgia. Computational Antibiotics Index • Computational Details and Website Access (p. 8) • Acknowledgements (p. 9) • Dedications (p. 11) • Antibiotic Historical Introduction (p. 13) Introduction to Antibiotic groups • Penicillin’s (p. 21) • Carbapenems (p. 22) • Oxazolidines (p. 23) • Rifamycin (p. 24) • Lincosamides (p. 25) • Quinolones (p. 26) • Polypeptides antibiotics (p. 27) • Glycopeptide Antibiotics (p. 28) • Sulfonamides (p. 29) • Lipoglycopeptides (p. 30) • First Generation Cephalosporins (p. 31) • Cephalosporin Third Generation (p. 32) • Fourth-Generation Cephalosporins (p. 33) • Fifth Generation Cephalosporin’s (p. 34) • Tetracycline antibiotics (p. 35) Computational Antibiotics Antibiotics Covered (in alphabetical order) Amikacin (p. 36) Cefempidone (p. 98) Ceftizoxime (p. 159) Amoxicillin (p. 38) Cefepime (p. 100) Ceftobiprole (p. 161) Ampicillin (p. 40) Cefetamet (p. 102) Ceftoxide (p. 163) Arsphenamine (p. 42) Cefetrizole (p. 104) Ceftriaxone (p. 165) Azithromycin (p.44) Cefivitril (p. 106) Cefuracetime (p. 167) Aziocillin (p. 46) Cefixime (p. 108) Cefuroxime (p. 169) Aztreonam (p.48) Cefmatilen ( p. 110) Cefuzonam (p. 171) Bacampicillin (p. 50) Cefmetazole (p. 112) Cefalexin (p. 173) Bacitracin (p. 52) Cefodizime (p. 114) Chloramphenicol (p.175) Balofloxacin (p. 54) Cefonicid (p. 116) Cilastatin (p. 177) Carbenicillin (p. 56) Cefoperazone (p. 118) Ciprofloxacin (p. 179) Cefacetrile (p. 58) Cefoselis (p. 120) Clarithromycin (p. 181) Cefaclor (p. -
Urinary Tract Infections
Urinary Tract Infections www.kidney.org Did you know that... n Urinary tract infections (UTIs) are responsible for nearly 10 million doctor visits each year. n One in five women will have at least one UTI in her lifetime. Nearly 20 percent of women who have a UTI will have another, and 30 percent of those will have yet another. Of this last group, 80 percent will have recurrences. n About 80 to 90 percent of UTIs are caused by a single type of bacteria. 2 NATIONAL KIDNEY FOUNDATION n UTIs can be treated effectively with medications called antibiotics. n People who get repeated UTIs may need additional tests to check for other health problems. n UTIs also may be called cystitis or a bladder infection. This brochure answers the questions most often asked about UTIs. If you have more questions, speak to your doctor. What is a urinary tract infection? A urinary tract infection is what happens when bacteria (germs) get into the urinary tract (the bladder) and multiply. The result is redness, swelling and pain in the urinary tract (see diagram). WWW.KIDNEY.ORG 3 Most UTIs stay in the bladder, the pouch-shaped organ where urine is stored before it passes out of the body. If a UTI is not treated promptly, the bacteria can travel up to the kidneys and cause a more serious type of infection, called pyelonephritis (pronounced pie-low-nef-right- iss). Pyelonephritis is an actual infection of the kidney, where urine is produced. This may result in fever and back pain. What causes a UTI? About 80 to 90 percent of UTIs are caused by a type of bacteria, called E.