Strengthening the Accelerated Approval Pathway: an Analysis of Potential Policy Reforms and Their Impact on Uncertainty, Access, Innovation, and Costs
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Cstone's Partner Blueprint Medicines Presented Updated Part 1 Data from PIONEER Trial of Avapritinib
Hong Kong Exchanges and Clearing Limited and The Stock Exchange of Hong Kong Limited take no responsibility for the contents of this announcement, make no representation as to its accuracy or completeness and expressly disclaim any liability whatsoever for any loss howsoever arising from or in reliance upon the whole or any part of the contents of this announcement. The forward-looking statements made in this announcement relate only to the events or information as of the date on which the statements are made in this announcement. Except as required by law, we undertake no obligation to update or revise publicly any forward-looking statements, whether as a result of new information, future events or otherwise, after the date on which the statements are made or to reflect the occurrence of unanticipated events. You should read this announcement completely and with the understanding that our actual future results or performance may be materially different from what we expect. In this announcement, statements of, or references to, our intentions or those of any of our directors and/or our Company are made as of the date of this announcement. Any of these intentions may alter in light of future development. CStone Pharmaceuticals 基 石 藥 業 (Incorporated in the Cayman Islands with limited liability) (Stock Code: 2616) VOLUNTARY ANNOUNCEMENT CSTONE’S PARTNER BLUEPRINT MEDICINES PRESENTED UPDATED PART 1 DATA FROM PIONEER TRIAL OF AVAPRITINIB SHOWING ROBUST REDUCTIONS IN CUTANEOUS DISEASE SYMPTOMS IN PATIENTS WITH INDOLENT SYSTEMIC MASTOCYTOSIS The partner of CStone Pharmaceuticals (the “Company” or “CStone”), Blueprint Medicines Corporation (NASDAQ: BPMC) (“Blueprint Medicines”), announced on June 6 updated clinical data from part 1 of the PIONEER trial showing robust and consistent clinical activity for avapritinib across multiple qualitative and quantitative measures of cutaneous disease in patients with indolent systemic mastocytosis (“ISM”). -

Cogent Biosciences Announces Creation of Cogent Research Team
Cogent Biosciences Announces Creation of Cogent Research Team April 6, 2021 Names industry veteran John Robinson, PhD as Chief Scientific Officer New Boulder-based team with exceptional track record of drug discovery and development focused on creating novel small molecule therapies for rare, genetically driven diseases Strong year-end cash position of $242.2 million supports company goals into 2024, including three CGT9486 clinical trials on-track to start this year, beginning with ASM in 1H21 BOULDER, Colo. and CAMBRIDGE, Mass., April 6, 2021 /PRNewswire/ -- Cogent Biosciences, Inc. (Nasdaq: COGT), a biotechnology company focused on developing precision therapies for genetically defined diseases, today announced the formation of the Cogent Research Team led by newly appointed Chief Scientific Officer, John Robinson, PhD. "Today marks an important step forward for Cogent Biosciences as we announce the formation of the Cogent Research Team with a focus on discovering and developing new small molecule therapies for patients fighting rare, genetically driven diseases," said Andrew Robbins, President and Chief Executive Officer of Cogent Biosciences. "I am thrilled to welcome John onboard as Cogent Biosciences' Chief Scientific Officer. John's expertise and seasoned leadership make him ideally suited to lead this new team of world class scientists. Given the team's impressive experience and accomplishments, we are excited for Cogent Biosciences' future and the opportunity to expand our pipeline and deliver novel precision therapies for patients." With an exceptional track record of innovation, the Cogent Research Team will focus on pioneering best-in-class, small molecule therapeutics to both improve upon existing drugs with clear limitations, as well as create new breakthroughs for diseases where others have been unable to find solutions. -

Leukemia Insights June 2021
JUNE 2021 In this month’s Leukemia Insights newsletter, written by Prithviraj Bose, M.D. and Srdan Verstovsek, M.D., Ph.D., and sponsored in part by the Charif Souki Cancer Research ABOUT MyMDAnderson Fund, we discuss our novel therapeutic approaches for the rare hematologic malignancies, systemic mastocytosis and myeloid/lymphoid neoplasms with myMDAnderson is a secure, eosinophilia. Learn more about our Leukemia program. personalized web site helping community physicians expedite patient referrals, as well as improve continuity Spotlight on rare, atypical, myeloid of care through information access and streamlined communications. neoplasms: systemic mastocytosis and Physicians who have referred patients myeloid/lymphoid neoplasms with to MD Anderson or plan to do so, can utilize the HIPAA compliant features eosinophilia and FGFR1 rearrangements of myMDAnderson to: • Refer a patient • View your patient's appointments Systemic Mastocytosis Access patient reports • Send and receive secure Systemic mastocytosis (SM) is a rare myeloid neoplasm messages driven in approximately 95% of cases by an activating mutation in c-KIT, usually D816V. SM is characterized as indolent, smoldering or advanced, based on the presence JOIN THE COVERSATION and number of so-called B- and C-findings. The latter Connect with us. signify organ damage and are a hallmark of advanced SM (AdvSM). AdvSM, in turn, is typically sub-classified as aggressive SM (ASM), SM with an associated hematologic neoplasm (SM-AHN, the most common subtype) and mast cell leukemia (MCL). Patients with indolent SM (ISM) and smoldering SM (SSM) enjoy much better survival than JOIN OUR MAILING LIST those with AdvSM, although symptoms in all three subtypes can be severe and debilitating. -

Incyte Announces the European Commission Approval of Pemazyre
3/29/2021 Incyte Announces the European Commission Approval of Pemazyre® (pemigatinib) as a Treatment for Adults with Locally Advanced or Metastatic Cholangiocarcinoma with a Fibroblast Growth Factor Receptor 2 (FGFR2) Fusion or Rearrangement - Pemazyre is the rst targeted therapy approved in the EU for this indication WILMINGTON, Del.--(BUSINESS WIRE)-- Incyte (Nasdaq:INCY) today announced that the European Commission (EC) has approved Pemazyre® (pemigatinib) for the treatment of adults with locally advanced or metastatic cholangiocarcinoma with a broblast growth factor receptor 2 (FGFR2) fusion or rearrangement that have progressed after at least one prior line of systemic therapy. The decision follows the positive opinion received from the European Medicines Agency’s Committee for Medicinal Products for Human Use in January 2021 recommending the conditional marketing authorization of Pemazyre. “Pemazyre’s approval is a crucial milestone for patients with FGFR2 positive cholangiocarcinoma. It is the rst new treatment option to be made available to these patients in the EU in over a decade and has demonstrated a high rate of durable responses in a setting where historically there has been no eective standard of care,” said Hervé Hoppenot, Chief Executive Ocer, Incyte. “We now look forward to working with individual countries in Europe to ensure eligible patients can access this new treatment as soon as possible.” The EC decision is based on data from the FIGHT-202 study evaluating the safety and ecacy of Pemazyre in adult patients with previously treated, locally advanced or metastatic cholangiocarcinoma with documented FGF/FGFR status. Interim results from FIGHT-202 demonstrated that in patients harboring FGFR2 fusions or rearrangements (Cohort A [108 patients]), Pemazyre monotherapy resulted in an overall response rate (ORR) of 37 percent (primary endpoint) and a median duration of response (DOR) of 8 months (secondary endpoint) based on an independent central radiographic review. -

Clinicogenomic Analysis of FGFR2-Rearranged Cholangiocarcinoma Identifies Correlates of Response and Mechanisms of Resistance to Pemigatinib
Published OnlineFirst November 20, 2020; DOI: 10.1158/2159-8290.CD-20-0766 RESEARCH ARTICLE Clinicogenomic Analysis of FGFR2- Rearranged Cholangiocarcinoma Identifies Correlates of Response and Mechanisms of Resistance to Pemigatinib Ian M. Silverman1, Antoine Hollebecque2, Luc Friboulet2, Sherry Owens1, Robert C. Newton1, Huiling Zhen3, Luis Féliz4, Camilla Zecchetto5, Davide Melisi5, and Timothy C. Burn1 Downloaded from cancerdiscovery.aacrjournals.org on September 30, 2021. © 2020 American Association for Cancer Research. Published OnlineFirst November 20, 2020; DOI: 10.1158/2159-8290.CD-20-0766 ABSTRACT Pemigatinib, a selective FGFR1–3 inhibitor, has demonstrated antitumor activity in FIGHT-202, a phase II study in patients with cholangiocarcinoma harboring FGFR2 fusions/rearrangements, and has gained regulatory approval in the United States. Eligibility for FIGHT- 202 was assessed using genomic profiling; here, these data were utilized to characterize the genomic landscape of cholangiocarcinoma and to uncover unique molecular features of patients harboring FGFR2 rearrangements. The results highlight the high percentage of patients with cholangiocarcinoma harboring potentially actionable genomic alterations and the diversity in gene partners that rear- range with FGFR2. Clinicogenomic analysis of pemigatinib-treated patients identified mechanisms of primary and acquired resistance. Genomic subsets of patients with other potentially actionable FGF/ FGFR alterations were also identified. Our study provides a framework for molecularly guided clinical trials and underscores the importance of genomic profiling to enable a deeper understanding of the molecular basis for response and nonresponse to targeted therapy. SIGNIFICANCE: We utilized genomic profiling data from FIGHT-202 to gain insights into the genomic landscape of cholangiocarcinoma, to understand the molecular diversity of patients with FGFR2 fusions or rearrangements, and to interrogate the clinicogenomics of patients treated with pemi- gatinib. -

First-Line Treatment Options for Patients with Stage IV Non-Small Cell Lung Cancer with Driver Alterations
First-Line Treatment Options for Patients with Stage IV Non-Small Cell Lung Cancer with Driver Alterations Patients with stage IV non-small cell lung cancer Nonsquamous cell carcinoma and squamous cell carcinoma Activating EGFR mutation other Sensitizing (L858R/exon 19 MET exon 14 skipping than exon 20 insertion mutations, EGFR exon 20 mutation ALK rearrangement ROS1 rearrangement BRAF V600E mutation RET rearrangement NTRK rearrangement mutations KRAS alterations HER2 alterations NRG1 alterations deletion) EGFR mutation T790M, L858R or Ex19Del PS 0-2 Treatment Options PS 0-2 Treatment Options PS 0-2 Treatment Options PS 0-2 Treatment Options PS 0-2 Treatment Options Treatment Options PS 0-2 Treatment Options PS 0-2 Treatment Options PS 0-2 Treatment Options Emerging target; no Emerging target; no Emerging target; no Platinum doublet † † † Osimertinib monotherapy S Afatinib monotherapy M M Alectinib S Entrectinib M Dabrafenib/trametinib M Capmatinib M Selpercatinib M Entrectinib M conclusions available conclusions available conclusions available chemotherapy ± bevacizumab Gefitinib with doublet Standard treatment based on Standard treatment based on Standard treatment based on M M M Brigatinib S Crizotinib M M Tepotinib M Pralsetinib* W Larotrectinib M chemotherapy non-driver mutation guideline non-driver mutation guideline non-driver mutation guideline If alectinib or brigatinib are not available If entrectinib or crizotinib are not available Standard treatment based on Standard treatment based on Standard treatment based on Dacomitinib monotherapy M Osimertinib W M M M Ceritinib S Ceritinib W non-driver mutation guideline non-driver mutation guideline non-driver mutation guideline Monotherapy with afatinib M Crizotinib S Lortlatinib W Standard treatment based on Erlotinib/ramucirumab M M non-driver mutation guideline Erlotinib/bevacizumab M Monotherapy with erlotinib M Strength of Recommendation Monotherapy with gefitinib M S Strong M Moderate W Weak Monotherapy with icotinib M Notes. -
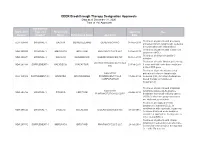
CDER Breakthrough Therapy Designation Approvals Data As of December 31, 2020 Total of 190 Approvals
CDER Breakthrough Therapy Designation Approvals Data as of December 31, 2020 Total of 190 Approvals Submission Application Type and Proprietary Approval Use Number Number Name Established Name Applicant Date Treatment of patients with previously BLA 125486 ORIGINAL-1 GAZYVA OBINUTUZUMAB GENENTECH INC 01-Nov-2013 untreated chronic lymphocytic leukemia in combination with chlorambucil Treatment of patients with mantle cell NDA 205552 ORIGINAL-1 IMBRUVICA IBRUTINIB PHARMACYCLICS LLC 13-Nov-2013 lymphoma (MCL) Treatment of chronic hepatitis C NDA 204671 ORIGINAL-1 SOVALDI SOFOSBUVIR GILEAD SCIENCES INC 06-Dec-2013 infection Treatment of cystic fibrosis patients age VERTEX PHARMACEUTICALS NDA 203188 SUPPLEMENT-4 KALYDECO IVACAFTOR 21-Feb-2014 6 years and older who have mutations INC in the CFTR gene Treatment of previously untreated NOVARTIS patients with chronic lymphocytic BLA 125326 SUPPLEMENT-60 ARZERRA OFATUMUMAB PHARMACEUTICALS 17-Apr-2014 leukemia (CLL) for whom fludarabine- CORPORATION based therapy is considered inappropriate Treatment of patients with anaplastic NOVARTIS lymphoma kinase (ALK)-positive NDA 205755 ORIGINAL-1 ZYKADIA CERITINIB 29-Apr-2014 PHARMACEUTICALS CORP metastatic non-small cell lung cancer (NSCLC) who have progressed on or are intolerant to crizotinib Treatment of relapsed chronic lymphocytic leukemia (CLL), in combination with rituximab, in patients NDA 206545 ORIGINAL-1 ZYDELIG IDELALISIB GILEAD SCIENCES INC 23-Jul-2014 for whom rituximab alone would be considered appropriate therapy due to other co-morbidities -

Overcoming MET-Dependent Resistance to Selective RET Inhibition in Patients with RET Fusion–Positive Lung Cancer by Combining Selpercatinib with Crizotinib a C Ezra Y
Published OnlineFirst October 20, 2020; DOI: 10.1158/1078-0432.CCR-20-2278 CLINICAL CANCER RESEARCH | RESEARCH BRIEFS: CLINICAL TRIAL BRIEF REPORT Overcoming MET-Dependent Resistance to Selective RET Inhibition in Patients with RET Fusion–Positive Lung Cancer by Combining Selpercatinib with Crizotinib A C Ezra Y. Rosen1, Melissa L. Johnson2, Sarah E. Clifford3, Romel Somwar4, Jennifer F. Kherani5, Jieun Son3, Arrien A. Bertram3, Monika A. Davare6, Eric Gladstone4, Elena V. Ivanova7, Dahlia N. Henry5, Elaine M. Kelley3, Mika Lin3, Marina S.D. Milan3, Binoj C. Nair5, Elizabeth A. Olek5, Jenna E. Scanlon3, Morana Vojnic4, Kevin Ebata5, Jaclyn F. Hechtman4, Bob T. Li1,8, Lynette M. Sholl9, Barry S. Taylor10, Marc Ladanyi4, Pasi A. Janne€ 3, S. Michael Rothenberg5, Alexander Drilon1,8, and Geoffrey R. Oxnard3 ABSTRACT ◥ Purpose: The RET proto-oncogene encodes a receptor tyrosine Results: MET amplification was identified in posttreatment kinase that is activated by gene fusion in 1%–2% of non–small biopsies in 4 patients with RET fusion–positive NSCLC treated with cell lung cancers (NSCLC) and rarely in other cancer types. selpercatinib. In at least one case, MET amplification was clearly Selpercatinib is a highly selective RET kinase inhibitor that has evident prior to therapy with selpercatinib. We demonstrate that recently been approved by the FDA in lung and thyroid cancers increased MET expression in RET fusion–positive tumor cells causes with activating RET gene fusions and mutations. Molecular resistance to selpercatinib, and this can be overcome by combining mechanisms of acquired resistance to selpercatinib are poorly selpercatinib with crizotinib. Using SPPs, selpercatinib with crizo- understood. -

CHMP Agenda of the 19-22 April 2021 Meeting
28 July 2021 EMA/CHMP/220334/2021 Corr.11 Human Medicines Division Committee for medicinal products for human use (CHMP) Agenda for the meeting on 19-22 April 2021 Chair: Harald Enzmann – Vice-Chair: Bruno Sepodes 19 April 2021, 09:00 – 19:30, virtual meeting/ room 1C 20 April 2021, 08:30 – 19:30, virtual meeting/ room 1C 21 April 2021, 08:30 – 19:30, virtual meeting/ room 1D 22 April 2021, 08:30 – 19:00, virtual meeting/ room 1C Disclaimers Some of the information contained in this agenda is considered commercially confidential or sensitive and therefore not disclosed. With regard to intended therapeutic indications or procedure scopes listed against products, it must be noted that these may not reflect the full wording proposed by applicants and may also vary during the course of the review. Additional details on some of these procedures will be published in the CHMP meeting highlights once the procedures are finalised and start of referrals will also be available. Of note, this agenda is a working document primarily designed for CHMP members and the work the Committee undertakes. Note on access to documents Some documents mentioned in the agenda cannot be released at present following a request for access to documents within the framework of Regulation (EC) No 1049/2001 as they are subject to on- going procedures for which a final decision has not yet been adopted. They will become public when adopted or considered public according to the principles stated in the Agency policy on access to documents (EMA/127362/2006). 1 Correction in section 8.1.1 Official address Domenico Scarlattilaan 6 ● 1083 HS Amsterdam ● The Netherlands Address for visits and deliveries Refer to www.ema.europa.eu/how-to-find-us Send us a question Go to www.ema.europa.eu/contact Telephone +31 (0)88 781 6000 An agency of the European Union © European Medicines Agency, 2021. -

Rxoutlook® 1St Quarter 2019
® RxOutlook 1st Quarter 2020 optum.com/optumrx a RxOutlook 1st Quarter 2020 Orphan drugs continue to feature prominently in the drug development pipeline In 1983 the Orphan Drug Act was signed into law. Thirty seven years later, what was initially envisioned as a minor category of drugs has become a major part of the drug development pipeline. The Orphan Drug Act was passed by the United States Congress in 1983 in order to spur drug development for rare conditions with high unmet need. The legislation provided financial incentives to manufacturers if they could demonstrate that the target population for their drug consisted of fewer than 200,000 persons in the United States, or that there was no reasonable expectation that commercial sales would be sufficient to recoup the developmental costs associated with the drug. These “Orphan Drug” approvals have become increasingly common over the last two decades. In 2000, two of the 27 (7%) new drugs approved by the FDA had Orphan Designation, whereas in 2019, 20 of the 48 new drugs (42%) approved by the FDA had Orphan Designation. Since the passage of the Orphan Drug Act, 37 years ago, additional regulations and FDA designations have been implemented in an attempt to further expedite drug development for certain serious and life threatening conditions. Drugs with a Fast Track designation can use Phase 2 clinical trials to support FDA approval. Drugs with Breakthrough Therapy designation can use alternative clinical trial designs instead of the traditional randomized, double-blind, placebo-controlled trial. Additionally, drugs may be approved via the Accelerated Approval pathway using surrogate endpoints in clinical trials rather than clinical outcomes. -

Facts and New Hopes on Selective FGFR Inhibitors in Solid Tumors Francesco Facchinetti1, Antoine Hollebecque2, Rastislav Bahleda2, Yohann Loriot3, Ken A
Published OnlineFirst October 4, 2019; DOI: 10.1158/1078-0432.CCR-19-2035 CLINICAL CANCER RESEARCH | REVIEW Facts and New Hopes on Selective FGFR Inhibitors in Solid Tumors Francesco Facchinetti1, Antoine Hollebecque2, Rastislav Bahleda2, Yohann Loriot3, Ken A. Olaussen1, Christophe Massard2, and Luc Friboulet1 ABSTRACT ◥ Precision oncology relies on the identification of molecular altera- molecularly guided treatments. Matching molecularly selected tions, responsible for tumor initiation and growth, which are suitable tumors with selective FGFR inhibitors has indeed led to promising targets of specific inhibitors. The development of FGFR inhibitors results in phase I and II trials, justifying their registration to be represents an edifying example of the rapid evolution in the field of expected in a near future, such as the recent accelerated approval of targeted oncology, with 10 different FGFR tyrosine kinase inhibitors erdafitinib granted by the FDA for urothelial cancer. Widening our actually under clinical investigation. In parallel, the discovery of knowledge of the activity, efficacy, and toxicities relative to the FGFR activating molecular alterations (mainly FGFR3 mutations selective FGFR tyrosine kinase inhibitors under clinical investi- and FGFR2 fusions) across many tumor types, especially urothelial gation, according to the exact FGFR molecular alteration, will be carcinomas and intrahepatic cholangiocarcinomas, widens the selec- crucial to determine the optimal therapeutic strategy for patients tion of patients that might benefit from selective FGFR inhibitors. suffering from FGFR-driven tumors. Similarly, identifying with The ongoing concomitant clinical evaluation of selective FGFR appropriate molecular diagnostic, every single tumor harboring inhibitors in molecularly selected solid tumors brings new hopes targetable FGFR alterations will be of utmost importance to attain for patients with metastatic cancer, for tumors so far excluded from the best outcomes for patients with FGFR-driven cancer. -

Presentación De Powerpoint
Molecular Tumor Board in Non-Small Cell Lung Cancer Jordi Remon Masip CIOCC Barcelona – HM Delfos @JordiRemon #SEOM20 Disclosure Information I do not have COI related to this specific presentation Why do we need a MTB in NSCLC? • Introduction • To understand the genomic profile from NGS reports • To prioritize the druggable genomic alteration: baseline / resistant • Increasing the detection of potential druggable genomic alterations • To include patients in basket trials • NGS is a reality but MTB and precision approach have challenges MTB is included in one equation MOLECULAR TUMOR BOARD Y MTB is included in one equation GENOMIC MOLECULAR TUMOR PROFILE BOARD X + Y MTB is included in one equation GENOMIC MOLECULAR TUMOR PERSONALISED PROFILE BOARD TREATMENT X + Y = Z Precision oncology in practice EGFR TKI Find actionable gens with ALK/ROS1 TKI approved therapy BRAF TKI Find actionable genes for RET / NTRK TKI clinical trials MET TKI Precision oncology in practice EGFR TKI Find actionable gens with ALK/ROS1 TKI approved therapy BRAF TKI Find actionable genes for RET / NTRK TKI clinical trials MET TKI Additional information about non-actionable gene mutations prognostic markers of sensitivity Two major steps in NSCLC outcome Immunotherapy Personalised treatment, ALK+: 5-y OS, KEYNOTE 024 Trial 5-y OS, ALEX trial Median OS, HR, (95%CI) 5-Year OS Rate, Median OS, HR, (95%CI) 5-Year OS Rate, mo % mo % 26.3 0.62 31.9 Not reached 0.67 63 13.4 (0.48-0.81) 16.7 57.4 (0.46-0.98) 46 Alectinib 26.4% Crizotinib Pembrolizumab Chemotherapy Brahmer – ESMO 2020 Mok – Annls of Oncology 2020 Number of oncogenes increases over time NTRK rearrangement Figure from Garrido – CTO 2019 (modified based on updated ESMO guidelines 2020 by Planchard et al.) Number of oncogenes increases over time NRG1 KRAS RET MET HER2 UN NTRK rearrangement Coming Future….