Progresses Toward Precision Medicine in RET-Altered Solid Tumors Carmen Belli1, Santosh Anand2,3, Justin F
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Cstone's Partner Blueprint Medicines Presented Updated Part 1 Data from PIONEER Trial of Avapritinib
Hong Kong Exchanges and Clearing Limited and The Stock Exchange of Hong Kong Limited take no responsibility for the contents of this announcement, make no representation as to its accuracy or completeness and expressly disclaim any liability whatsoever for any loss howsoever arising from or in reliance upon the whole or any part of the contents of this announcement. The forward-looking statements made in this announcement relate only to the events or information as of the date on which the statements are made in this announcement. Except as required by law, we undertake no obligation to update or revise publicly any forward-looking statements, whether as a result of new information, future events or otherwise, after the date on which the statements are made or to reflect the occurrence of unanticipated events. You should read this announcement completely and with the understanding that our actual future results or performance may be materially different from what we expect. In this announcement, statements of, or references to, our intentions or those of any of our directors and/or our Company are made as of the date of this announcement. Any of these intentions may alter in light of future development. CStone Pharmaceuticals 基 石 藥 業 (Incorporated in the Cayman Islands with limited liability) (Stock Code: 2616) VOLUNTARY ANNOUNCEMENT CSTONE’S PARTNER BLUEPRINT MEDICINES PRESENTED UPDATED PART 1 DATA FROM PIONEER TRIAL OF AVAPRITINIB SHOWING ROBUST REDUCTIONS IN CUTANEOUS DISEASE SYMPTOMS IN PATIENTS WITH INDOLENT SYSTEMIC MASTOCYTOSIS The partner of CStone Pharmaceuticals (the “Company” or “CStone”), Blueprint Medicines Corporation (NASDAQ: BPMC) (“Blueprint Medicines”), announced on June 6 updated clinical data from part 1 of the PIONEER trial showing robust and consistent clinical activity for avapritinib across multiple qualitative and quantitative measures of cutaneous disease in patients with indolent systemic mastocytosis (“ISM”). -

Tamoxifen Erythroid Toxicity Revealed by Studying the Role of Nuclear
COMMENT as in Santana-Codina et al.1 Briefly, 12-week old Sv129/J Tamoxifen erythroid toxicity revealed by studying Ncoa4-ko and wild-type littermates received 200 mg/kg the role of nuclear receptor co-activator 4 in tamoxifen via oral gavage daily for five consecutive days erythropoiesis (day 0-4) and complete blood count was obtained at days 0, 4, 11 and 21. We chose mice on Sv129/J background We read with great interest the paper recently pub- that, unlike C57BL/6 Ncoa4-ko animals,4 do not show lished by Santana-Codina et al.1 about the cell anemia or alterations of iron parameters but only mild autonomous and non-autonomous role of nuclear recep- microcytosis (Figure 1 and Nai et al., 2019, manuscript in tor co-activator 4 (NCOA4). NCOA4 is a cargo receptor preparation). At day 4, only Ncoa4-ko mice showed a sta- that, in conditions of iron deficiency, promotes fer- tistically significant decrease in red blood cell (RBC) ritinophagy to release iron from ferritin.2,3 Inactivation of count, and hematocrit (Hct) and hemoglobin (Hb) levels. Ncoa4 in C57BL/6 mice causes mild microcytic anemia and increases the susceptibility to iron-deficiency anemia At day 11, also wild-type mice showed a reduction in due to iron being trapped in ferritin in several organs.3,4 To RBC count and decreased Hb and Hct, although for the formally prove the role of Ncoa4 inactivation on erythro- latter two parameters levels were higher than those of poiesis, a tamoxifen-inducible CRE-dependent Ncoa4-ko mice. -

NCOA4 Maintains Murine Erythropoiesis Via Cell Autonomous and Non-Autonomous Mechanisms
Red Cell Biology & its Disorders SUPPLEMENTARY APPENDIX NCOA4 maintains murine erythropoiesis via cell autonomous and non-autonomous mechanisms Naiara Santana-Codina,1,* Sebastian Gableske,1,* Maria Quiles del Rey,1 Beata Małachowska,2,3 Mark P. Jedrychowski,1,4 Douglas E. Biancur,1 Paul J. Schmidt,5 Mark D. Fleming,5 Wojciech Fendler,1,2 J. Wade Harper,4,# Alec C. Kimmelman6,# and Joseph D. Mancias1 1Division of Genomic Stability and DNA Repair, Department of Radiation Oncology, Dana-Farber Cancer Institute, Boston, MA, USA; 2De- partment of Biostatistics and Translational Medicine, Medical University of Lodz, Poland; 3Postgraduate School of Molecular Medicine, Medical University of Warsaw, Poland; 4Department of Cell Biology, Harvard Medical School, Boston, MA, USA; 5Department of Pathology, Boston Children’s Hospital and Harvard Medical School, Boston, MA, USA and 6Department of Radiation Oncology, Perlmutter Cancer Center, New York University School of Medicine, New York, NY, USA * These authors contributed equally to this work ©2019 Ferrata Storti Foundation. This is an open-access paper. doi:10.3324/haematol.2018.204123 Received: August 10, 2018. Accepted: January 9, 2019. Pre-published: January 10, 2019. Correspondence: JOSEPH D. MANCIAS - [email protected] SUPPLEMENTARY INFORMATION SUPPLEMENTAL EXPERIMENTAL PROCEDURES Cell culture. Cells were cultured in a humidified incubator at 37°C and 5% carbon dioxide (CO2). HEK-293T and K562 cell lines were obtained from the American Type Culture Collection (ATCC, Manassas, Virginia) and tested for mycoplasma contamination by PCR. Cells were grown in DMEM (HEK-293T, Life Technologies, 11965) or IMDM (K562, Thermo Fisher 12440053) with 10% FBS and 1% Pen/Strep (Life Technologies 15140). -

RET/PTC Activation in Papillary Thyroid Carcinoma
European Journal of Endocrinology (2006) 155 645–653 ISSN 0804-4643 INVITED REVIEW RET/PTC activation in papillary thyroid carcinoma: European Journal of Endocrinology Prize Lecture Massimo Santoro1, Rosa Marina Melillo1 and Alfredo Fusco1,2 1Istituto di Endocrinologia ed Oncologia Sperimentale del CNR ‘G. Salvatore’, c/o Dipartimento di Biologia e Patologia Cellulare e Molecolare, University ‘Federico II’, Via S. Pansini, 5, 80131 Naples, Italy and 2NOGEC (Naples Oncogenomic Center)–CEINGE, Biotecnologie Avanzate & SEMM, European School of Molecular Medicine, Naples, Italy (Correspondence should be addressed to M Santoro; Email: [email protected]) Abstract Papillary thyroid carcinoma (PTC) is frequently associated with RET gene rearrangements that generate the so-called RET/PTC oncogenes. In this review, we examine the data about the mechanisms of thyroid cell transformation, activation of downstream signal transduction pathways and modulation of gene expression induced by RET/PTC. These findings have advanced our understanding of the processes underlying PTC formation and provide the basis for novel therapeutic approaches to this disease. European Journal of Endocrinology 155 645–653 RET/PTC rearrangements in papillary growth factor, have been described in a fraction of PTC thyroid carcinoma patients (7). As illustrated in figure 1, many different genes have been found to be rearranged with RET in The rearranged during tansfection (RET) proto-onco- individual PTC patients. RET/PTC1 and 3 account for gene, located on chromosome 10q11.2, was isolated in more than 90% of all rearrangements and are hence, by 1985 and shown to be activated by a DNA rearrange- far, the most frequent variants (8–11). They result from ment (rearranged during transfection) (1).As the fusion of RET to the coiled-coil domain containing illustrated in Fig. -

Orally Bioavailable Androgen Receptor Degrader, Potential Next
Published OnlineFirst September 3, 2019; DOI: 10.1158/1078-0432.CCR-19-1458 Translational Cancer Mechanisms and Therapy Clinical Cancer Research Orally Bioavailable Androgen Receptor Degrader, Potential Next-Generation Therapeutic for Enzalutamide-Resistant Prostate Cancer Suriyan Ponnusamy1, Yali He2, Dong-Jin Hwang2, Thirumagal Thiyagarajan1, Rene Houtman3,Vera Bocharova4, Bobby G. Sumpter4, Elias Fernandez5, Daniel Johnson6, Ziyun Du7, Lawrence M. Pfeffer7, Robert H. Getzenberg8, Iain J. McEwan9, Duane D. Miller2, and Ramesh Narayanan1,10 Abstract Purpose: Androgen receptor (AR)-targeting prostate Results: UT-34 inhibits the wild-type and LBD-mutant cancer drugs, which are predominantly competitive ARs comparably and inhibits the in vitro proliferation and ligand-binding domain (LBD)-binding antagonists, are in vivo growth of enzalutamide-sensitive and -resistant pros- inactivated by common resistance mechanisms. It is tate cancer xenografts. In preclinical models, UT-34 induced important to develop next-generation mechanistically theregressionofenzalutamide-resistanttumorsatdoses distinct drugs to treat castration- and drug-resistant pros- when the AR is degraded; but, at lower doses, when the AR tate cancers. is just antagonized, it inhibits, without shrinking, the Experimental Design: Second-generation AR pan antag- tumors. This indicates that degradation might be a prereq- onist UT-34 was selected from a library of compounds uisite for tumor regression. Mechanistically, UT-34 promotes and tested in competitive AR binding and transactivation -

Cogent Biosciences Announces Creation of Cogent Research Team
Cogent Biosciences Announces Creation of Cogent Research Team April 6, 2021 Names industry veteran John Robinson, PhD as Chief Scientific Officer New Boulder-based team with exceptional track record of drug discovery and development focused on creating novel small molecule therapies for rare, genetically driven diseases Strong year-end cash position of $242.2 million supports company goals into 2024, including three CGT9486 clinical trials on-track to start this year, beginning with ASM in 1H21 BOULDER, Colo. and CAMBRIDGE, Mass., April 6, 2021 /PRNewswire/ -- Cogent Biosciences, Inc. (Nasdaq: COGT), a biotechnology company focused on developing precision therapies for genetically defined diseases, today announced the formation of the Cogent Research Team led by newly appointed Chief Scientific Officer, John Robinson, PhD. "Today marks an important step forward for Cogent Biosciences as we announce the formation of the Cogent Research Team with a focus on discovering and developing new small molecule therapies for patients fighting rare, genetically driven diseases," said Andrew Robbins, President and Chief Executive Officer of Cogent Biosciences. "I am thrilled to welcome John onboard as Cogent Biosciences' Chief Scientific Officer. John's expertise and seasoned leadership make him ideally suited to lead this new team of world class scientists. Given the team's impressive experience and accomplishments, we are excited for Cogent Biosciences' future and the opportunity to expand our pipeline and deliver novel precision therapies for patients." With an exceptional track record of innovation, the Cogent Research Team will focus on pioneering best-in-class, small molecule therapeutics to both improve upon existing drugs with clear limitations, as well as create new breakthroughs for diseases where others have been unable to find solutions. -

RET Gene Fusions in Malignancies of the Thyroid and Other Tissues
G C A T T A C G G C A T genes Review RET Gene Fusions in Malignancies of the Thyroid and Other Tissues Massimo Santoro 1,*, Marialuisa Moccia 1, Giorgia Federico 1 and Francesca Carlomagno 1,2 1 Department of Molecular Medicine and Medical Biotechnology, University of Naples “Federico II”, 80131 Naples, Italy; [email protected] (M.M.); [email protected] (G.F.); [email protected] (F.C.) 2 Institute of Endocrinology and Experimental Oncology of the CNR, 80131 Naples, Italy * Correspondence: [email protected] Received: 10 March 2020; Accepted: 12 April 2020; Published: 15 April 2020 Abstract: Following the identification of the BCR-ABL1 (Breakpoint Cluster Region-ABelson murine Leukemia) fusion in chronic myelogenous leukemia, gene fusions generating chimeric oncoproteins have been recognized as common genomic structural variations in human malignancies. This is, in particular, a frequent mechanism in the oncogenic conversion of protein kinases. Gene fusion was the first mechanism identified for the oncogenic activation of the receptor tyrosine kinase RET (REarranged during Transfection), initially discovered in papillary thyroid carcinoma (PTC). More recently, the advent of highly sensitive massive parallel (next generation sequencing, NGS) sequencing of tumor DNA or cell-free (cfDNA) circulating tumor DNA, allowed for the detection of RET fusions in many other solid and hematopoietic malignancies. This review summarizes the role of RET fusions in the pathogenesis of human cancer. Keywords: kinase; tyrosine kinase inhibitor; targeted therapy; thyroid cancer 1. The RET Receptor RET (REarranged during Transfection) was initially isolated as a rearranged oncoprotein upon the transfection of a human lymphoma DNA [1]. -

First-Line Treatment Options for Patients with Stage IV Non-Small Cell Lung Cancer with Driver Alterations
First-Line Treatment Options for Patients with Stage IV Non-Small Cell Lung Cancer with Driver Alterations Patients with stage IV non-small cell lung cancer Nonsquamous cell carcinoma and squamous cell carcinoma Activating EGFR mutation other Sensitizing (L858R/exon 19 MET exon 14 skipping than exon 20 insertion mutations, EGFR exon 20 mutation ALK rearrangement ROS1 rearrangement BRAF V600E mutation RET rearrangement NTRK rearrangement mutations KRAS alterations HER2 alterations NRG1 alterations deletion) EGFR mutation T790M, L858R or Ex19Del PS 0-2 Treatment Options PS 0-2 Treatment Options PS 0-2 Treatment Options PS 0-2 Treatment Options PS 0-2 Treatment Options Treatment Options PS 0-2 Treatment Options PS 0-2 Treatment Options PS 0-2 Treatment Options Emerging target; no Emerging target; no Emerging target; no Platinum doublet † † † Osimertinib monotherapy S Afatinib monotherapy M M Alectinib S Entrectinib M Dabrafenib/trametinib M Capmatinib M Selpercatinib M Entrectinib M conclusions available conclusions available conclusions available chemotherapy ± bevacizumab Gefitinib with doublet Standard treatment based on Standard treatment based on Standard treatment based on M M M Brigatinib S Crizotinib M M Tepotinib M Pralsetinib* W Larotrectinib M chemotherapy non-driver mutation guideline non-driver mutation guideline non-driver mutation guideline If alectinib or brigatinib are not available If entrectinib or crizotinib are not available Standard treatment based on Standard treatment based on Standard treatment based on Dacomitinib monotherapy M Osimertinib W M M M Ceritinib S Ceritinib W non-driver mutation guideline non-driver mutation guideline non-driver mutation guideline Monotherapy with afatinib M Crizotinib S Lortlatinib W Standard treatment based on Erlotinib/ramucirumab M M non-driver mutation guideline Erlotinib/bevacizumab M Monotherapy with erlotinib M Strength of Recommendation Monotherapy with gefitinib M S Strong M Moderate W Weak Monotherapy with icotinib M Notes. -
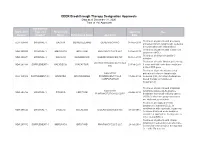
CDER Breakthrough Therapy Designation Approvals Data As of December 31, 2020 Total of 190 Approvals
CDER Breakthrough Therapy Designation Approvals Data as of December 31, 2020 Total of 190 Approvals Submission Application Type and Proprietary Approval Use Number Number Name Established Name Applicant Date Treatment of patients with previously BLA 125486 ORIGINAL-1 GAZYVA OBINUTUZUMAB GENENTECH INC 01-Nov-2013 untreated chronic lymphocytic leukemia in combination with chlorambucil Treatment of patients with mantle cell NDA 205552 ORIGINAL-1 IMBRUVICA IBRUTINIB PHARMACYCLICS LLC 13-Nov-2013 lymphoma (MCL) Treatment of chronic hepatitis C NDA 204671 ORIGINAL-1 SOVALDI SOFOSBUVIR GILEAD SCIENCES INC 06-Dec-2013 infection Treatment of cystic fibrosis patients age VERTEX PHARMACEUTICALS NDA 203188 SUPPLEMENT-4 KALYDECO IVACAFTOR 21-Feb-2014 6 years and older who have mutations INC in the CFTR gene Treatment of previously untreated NOVARTIS patients with chronic lymphocytic BLA 125326 SUPPLEMENT-60 ARZERRA OFATUMUMAB PHARMACEUTICALS 17-Apr-2014 leukemia (CLL) for whom fludarabine- CORPORATION based therapy is considered inappropriate Treatment of patients with anaplastic NOVARTIS lymphoma kinase (ALK)-positive NDA 205755 ORIGINAL-1 ZYKADIA CERITINIB 29-Apr-2014 PHARMACEUTICALS CORP metastatic non-small cell lung cancer (NSCLC) who have progressed on or are intolerant to crizotinib Treatment of relapsed chronic lymphocytic leukemia (CLL), in combination with rituximab, in patients NDA 206545 ORIGINAL-1 ZYDELIG IDELALISIB GILEAD SCIENCES INC 23-Jul-2014 for whom rituximab alone would be considered appropriate therapy due to other co-morbidities -

Supp Table 6.Pdf
Supplementary Table 6. Processes associated to the 2037 SCL candidate target genes ID Symbol Entrez Gene Name Process NM_178114 AMIGO2 adhesion molecule with Ig-like domain 2 adhesion NM_033474 ARVCF armadillo repeat gene deletes in velocardiofacial syndrome adhesion NM_027060 BTBD9 BTB (POZ) domain containing 9 adhesion NM_001039149 CD226 CD226 molecule adhesion NM_010581 CD47 CD47 molecule adhesion NM_023370 CDH23 cadherin-like 23 adhesion NM_207298 CERCAM cerebral endothelial cell adhesion molecule adhesion NM_021719 CLDN15 claudin 15 adhesion NM_009902 CLDN3 claudin 3 adhesion NM_008779 CNTN3 contactin 3 (plasmacytoma associated) adhesion NM_015734 COL5A1 collagen, type V, alpha 1 adhesion NM_007803 CTTN cortactin adhesion NM_009142 CX3CL1 chemokine (C-X3-C motif) ligand 1 adhesion NM_031174 DSCAM Down syndrome cell adhesion molecule adhesion NM_145158 EMILIN2 elastin microfibril interfacer 2 adhesion NM_001081286 FAT1 FAT tumor suppressor homolog 1 (Drosophila) adhesion NM_001080814 FAT3 FAT tumor suppressor homolog 3 (Drosophila) adhesion NM_153795 FERMT3 fermitin family homolog 3 (Drosophila) adhesion NM_010494 ICAM2 intercellular adhesion molecule 2 adhesion NM_023892 ICAM4 (includes EG:3386) intercellular adhesion molecule 4 (Landsteiner-Wiener blood group)adhesion NM_001001979 MEGF10 multiple EGF-like-domains 10 adhesion NM_172522 MEGF11 multiple EGF-like-domains 11 adhesion NM_010739 MUC13 mucin 13, cell surface associated adhesion NM_013610 NINJ1 ninjurin 1 adhesion NM_016718 NINJ2 ninjurin 2 adhesion NM_172932 NLGN3 neuroligin -

Overcoming MET-Dependent Resistance to Selective RET Inhibition in Patients with RET Fusion–Positive Lung Cancer by Combining Selpercatinib with Crizotinib a C Ezra Y
Published OnlineFirst October 20, 2020; DOI: 10.1158/1078-0432.CCR-20-2278 CLINICAL CANCER RESEARCH | RESEARCH BRIEFS: CLINICAL TRIAL BRIEF REPORT Overcoming MET-Dependent Resistance to Selective RET Inhibition in Patients with RET Fusion–Positive Lung Cancer by Combining Selpercatinib with Crizotinib A C Ezra Y. Rosen1, Melissa L. Johnson2, Sarah E. Clifford3, Romel Somwar4, Jennifer F. Kherani5, Jieun Son3, Arrien A. Bertram3, Monika A. Davare6, Eric Gladstone4, Elena V. Ivanova7, Dahlia N. Henry5, Elaine M. Kelley3, Mika Lin3, Marina S.D. Milan3, Binoj C. Nair5, Elizabeth A. Olek5, Jenna E. Scanlon3, Morana Vojnic4, Kevin Ebata5, Jaclyn F. Hechtman4, Bob T. Li1,8, Lynette M. Sholl9, Barry S. Taylor10, Marc Ladanyi4, Pasi A. Janne€ 3, S. Michael Rothenberg5, Alexander Drilon1,8, and Geoffrey R. Oxnard3 ABSTRACT ◥ Purpose: The RET proto-oncogene encodes a receptor tyrosine Results: MET amplification was identified in posttreatment kinase that is activated by gene fusion in 1%–2% of non–small biopsies in 4 patients with RET fusion–positive NSCLC treated with cell lung cancers (NSCLC) and rarely in other cancer types. selpercatinib. In at least one case, MET amplification was clearly Selpercatinib is a highly selective RET kinase inhibitor that has evident prior to therapy with selpercatinib. We demonstrate that recently been approved by the FDA in lung and thyroid cancers increased MET expression in RET fusion–positive tumor cells causes with activating RET gene fusions and mutations. Molecular resistance to selpercatinib, and this can be overcome by combining mechanisms of acquired resistance to selpercatinib are poorly selpercatinib with crizotinib. Using SPPs, selpercatinib with crizo- understood. -

CHMP Agenda of the 19-22 April 2021 Meeting
28 July 2021 EMA/CHMP/220334/2021 Corr.11 Human Medicines Division Committee for medicinal products for human use (CHMP) Agenda for the meeting on 19-22 April 2021 Chair: Harald Enzmann – Vice-Chair: Bruno Sepodes 19 April 2021, 09:00 – 19:30, virtual meeting/ room 1C 20 April 2021, 08:30 – 19:30, virtual meeting/ room 1C 21 April 2021, 08:30 – 19:30, virtual meeting/ room 1D 22 April 2021, 08:30 – 19:00, virtual meeting/ room 1C Disclaimers Some of the information contained in this agenda is considered commercially confidential or sensitive and therefore not disclosed. With regard to intended therapeutic indications or procedure scopes listed against products, it must be noted that these may not reflect the full wording proposed by applicants and may also vary during the course of the review. Additional details on some of these procedures will be published in the CHMP meeting highlights once the procedures are finalised and start of referrals will also be available. Of note, this agenda is a working document primarily designed for CHMP members and the work the Committee undertakes. Note on access to documents Some documents mentioned in the agenda cannot be released at present following a request for access to documents within the framework of Regulation (EC) No 1049/2001 as they are subject to on- going procedures for which a final decision has not yet been adopted. They will become public when adopted or considered public according to the principles stated in the Agency policy on access to documents (EMA/127362/2006). 1 Correction in section 8.1.1 Official address Domenico Scarlattilaan 6 ● 1083 HS Amsterdam ● The Netherlands Address for visits and deliveries Refer to www.ema.europa.eu/how-to-find-us Send us a question Go to www.ema.europa.eu/contact Telephone +31 (0)88 781 6000 An agency of the European Union © European Medicines Agency, 2021.