Managing Pitted Keratolysis Through Hyperhidrosis Control with Topical Glycopyrrolate 2%
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Smelly Foot Rash
CLINICAL Smelly foot rash Paulo Morais Ligia Peralta Keywords: skin diseases, infectious Case study A previously healthy Caucasian girl, 6 years of age, presented with pruritic rash on both heels of 6 months duration. The lesions appeared as multiple depressions 1–2 mm in diameter that progressively increased in size. There was no history of trauma or insect bite. She reported local pain when walking, worse with moisture and wearing sneakers. On examination, multiple small crater- like depressions were present, some Figure 1. Heel of patient coalescing into a larger lesion on both heels (Figure 1). There was an unpleasant ‘cheesy’ protective/occluded footwear for prolonged odour and a moist appearance. Wood lamp periods.1–4 examination and potassium hydroxide testing for fungal hyphae were negative. Answer 2 Question 1 Pitted keratolysis is frequently seen during What is the diagnosis? summer and rainy seasons, particularly in tropical regions, although it occurs Question 2 worldwide.1,3,4 It is caused by Kytococcus What causes this condition? sedentarius, Dermatophilus congolensis, or species of Corynebacterium, Actinomyces or Question 3 Streptomyces.1–4 Under favourable conditions How would you confirm the diagnosis? (ie. hyperhidrosis, prolonged occlusion and increased skin surface pH), these bacteria Question 4 proliferate and produce proteinases that destroy What are the differential diagnoses? the stratum corneum, creating pits. Sulphur containing compounds produced by the bacteria Question 5 cause the characteristic malodor. What is your management strategy? Answer 3 Answer 1 Pitted keratolysis is usually a clinical Based on the typical clinical picture and the negative diagnosis with typical hyperhidrosis, malodor ancillary tests, the diagnosis of pitted keratolysis (PK) (bromhidrosis) and occasionally, tenderness, is likely. -

What Certified Athletic Trainers and Therapists Need to Know Thomas M
PHYSICIAN PERSPECTIVE Tracy Ray, MD, Column Editor Sports Dermatology: What Certified Athletic Trainers and Therapists Need to Know Thomas M. Dougherty, MD • American Sports Medicine Institute, Birmingham AL OST SPECIAL SKIN problems of athletes are ting shoes for all athletes and gloves for weight lifters M easily observable and can be recognized and racket-sport players can help. and treated early. Proper care can prevent Occlusive folliculitis, also known as acne mechanica disruption of the training or competition schedule. or “football acne,” is a flare of sometimes preexisting Various athletic settings expose the skin to a multi- acne caused by heat, occlusion, and pressure distrib- tude of infectious organisms while increasing its vul- uted in areas under bulky playing equipment (e.g., nerability to infection. A working knowledge of skin shoulders, forehead, chin in football players; legs, arms, disorders in athletes is essential for athletic trainers, trunk in wrestlers). Inflammatory papules and pustules who are often the first to evaluate athletes for medi- are present. A clean absorbent T-shirt should be worn cal problems. under equipment, and the affected areas should be cleansed after a workout. Direct Cutaneous Injury Follicular keloidalis is seen mostly in African-Ameri- can athletes and is a progression of occlusive folliculi- Calluses are the skin’s compensatory, protective re- tis with nontender, firm, fibrous papules around the sponse to friction, most commonly seen on the feet edges of the football helmet, especially at the posterior but also on the hands of golfers and in oar and racket neck and occipital scalp. Surgical treatment, if indicated, sports. -

WO 2014/134709 Al 12 September 2014 (12.09.2014) P O P C T
(12) INTERNATIONAL APPLICATION PUBLISHED UNDER THE PATENT COOPERATION TREATY (PCT) (19) World Intellectual Property Organization International Bureau (10) International Publication Number (43) International Publication Date WO 2014/134709 Al 12 September 2014 (12.09.2014) P O P C T (51) International Patent Classification: (81) Designated States (unless otherwise indicated, for every A61K 31/05 (2006.01) A61P 31/02 (2006.01) kind of national protection available): AE, AG, AL, AM, AO, AT, AU, AZ, BA, BB, BG, BH, BN, BR, BW, BY, (21) International Application Number: BZ, CA, CH, CL, CN, CO, CR, CU, CZ, DE, DK, DM, PCT/CA20 14/000 174 DO, DZ, EC, EE, EG, ES, FI, GB, GD, GE, GH, GM, GT, (22) International Filing Date: HN, HR, HU, ID, IL, IN, IR, IS, JP, KE, KG, KN, KP, KR, 4 March 2014 (04.03.2014) KZ, LA, LC, LK, LR, LS, LT, LU, LY, MA, MD, ME, MG, MK, MN, MW, MX, MY, MZ, NA, NG, NI, NO, NZ, (25) Filing Language: English OM, PA, PE, PG, PH, PL, PT, QA, RO, RS, RU, RW, SA, (26) Publication Language: English SC, SD, SE, SG, SK, SL, SM, ST, SV, SY, TH, TJ, TM, TN, TR, TT, TZ, UA, UG, US, UZ, VC, VN, ZA, ZM, (30) Priority Data: ZW. 13/790,91 1 8 March 2013 (08.03.2013) US (84) Designated States (unless otherwise indicated, for every (71) Applicant: LABORATOIRE M2 [CA/CA]; 4005-A, rue kind of regional protection available): ARIPO (BW, GH, de la Garlock, Sherbrooke, Quebec J1L 1W9 (CA). GM, KE, LR, LS, MW, MZ, NA, RW, SD, SL, SZ, TZ, UG, ZM, ZW), Eurasian (AM, AZ, BY, KG, KZ, RU, TJ, (72) Inventors: LEMIRE, Gaetan; 6505, rue de la fougere, TM), European (AL, AT, BE, BG, CH, CY, CZ, DE, DK, Sherbrooke, Quebec JIN 3W3 (CA). -

An Update of Pitted Keratolysis: a Review
Journal of Current and Advance Medical Research January 2017, Vol. 4, No. 1, pp. 27-30 http://www.banglajol.info/index.php/JCAMR ISSN (Print) 2313-447X Review Article An Update of Pitted Keratolysis: A Review Tania Hoque; Bhuiya Mohammad Mahatab Uddin 1Assistant Professor, Department of Dermatolgy and Venereology, Gonoshasthaya Somaj Vittic Medical college and Hospital, Savar, Dhaka, Bangladesh; 2Assistant Professor, Department of Microbiology, Enam Medical College, Savar, Dhaka, Bangladesh [Reviewed: 30 September 2016; Accepted on: 1 October 2016; Published on: 1 January 2017] Abstract Pitted keratolysis is a bacterial infection of the soles of the feet or less commonly, the palms of the hands. Pitted keratolysis is easily identified by its shallow, crater-like pits. Collection of specimen using swab may be helpful to identify causative bacteria and skin scraping is often taken to exclude fungal infection. The diagnosis is sometimes made by skin biopsy revealing characteristic histopathological feature of Pitted Keratolysis. Treatment generally consists of hygienic measures, sometimes supplemented by medication and perhaps on oral medication. This review is aimed to consolidate present information about aetiopathogenesis, diagnosis and management of Pitted Keratolysis. It is worth mentioning that Pitted Keratolysis is non-contagious. [Journal of Current and Advance Medical Research 2017;4(1):27-30] Keywords: Pitted keratolysis; bacterial infection; non-contagious Correspondence: Dr. Tania Hoque, Assistant Professor, Dept of Dermatolgy and Venereology, Gonoshasthaya Somaj Vittic Medical college and Hospital, Savar, Dhaka, Bangladesh Cite this article as: Hoque T, Uddin BMM. An Update of Pitted Keratolysis: A Review. Journal of Current and Advance Medical Research 2017;4(1):27-30 Conflict of Interest: All the authors have declared that there was no conflict of interest. -

Bacterial Infections Diseases Picture Cause Basic Lesion
page: 117 Chapter 6: alphabetical Bacterial infections diseases picture cause basic lesion search contents print last screen viewed back next Bacterial infections diseases Impetigo page: 118 6.1 Impetigo alphabetical Bullous impetigo Bullae with cloudy contents, often surrounded by an erythematous halo. These bullae rupture easily picture and are rapidly replaced by extensive crusty patches. Bullous impetigo is classically caused by Staphylococcus aureus. cause basic lesion Basic Lesions: Bullae; Crusts Causes: Infection search contents print last screen viewed back next Bacterial infections diseases Impetigo page: 119 alphabetical Non-bullous impetigo Erythematous patches covered by a yellowish crust. Lesions are most frequently around the mouth. picture Lesions around the nose are very characteristic and require prolonged treatment. ß-Haemolytic streptococcus is cause most frequently found in this type of impetigo. basic lesion Basic Lesions: Erythematous Macule; Crusts Causes: Infection search contents print last screen viewed back next Bacterial infections diseases Ecthyma page: 120 6.2 Ecthyma alphabetical Slow and gradually deepening ulceration surmounted by a thick crust. The usual site of ecthyma are the legs. After healing there is a permanent scar. The pathogen is picture often a streptococcus. Ecthyma is very common in tropical countries. cause basic lesion Basic Lesions: Crusts; Ulcers Causes: Infection search contents print last screen viewed back next Bacterial infections diseases Folliculitis page: 121 6.3 Folliculitis -
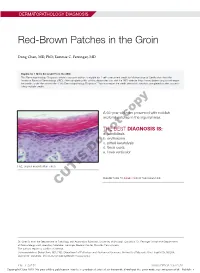
Red-Brown Patches in the Groin
DERMATOPATHOLOGY DIAGNOSIS Red-Brown Patches in the Groin Dong Chen, MD, PhD; Tammie C. Ferringer, MD Eligible for 1 MOC SA Credit From the ABD This Dermatopathology Diagnosis article in our print edition is eligible for 1 self-assessment credit for Maintenance of Certification from the American Board of Dermatology (ABD). After completing this activity, diplomates can visit the ABD website (http://www.abderm.org) to self-report the credits under the activity title “Cutis Dermatopathology Diagnosis.” You may report the credit after each activity is completed or after accumu- lating multiple credits. A 66-year-old man presented with reddish arciform patchescopy in the inguinal area. THE BEST DIAGNOSIS IS: a. candidiasis b. noterythrasma c. pitted keratolysis d. tinea cruris Doe. tinea versicolor H&E, original magnification ×600. PLEASE TURN TO PAGE 419 FOR THE DIAGNOSIS CUTIS Dr. Chen is from the Department of Pathology and Anatomical Sciences, University of Missouri, Columbia. Dr. Ferringer is from the Departments of Dermatology and Laboratory Medicine, Geisinger Medical Center, Danville, Pennsylvania. The authors report no conflict of interest. Correspondence: Dong Chen, MD, PhD, Department of Pathology and Anatomical Sciences, University of Missouri, One Hospital Dr, MA204, DC018.00, Columbia, MO 65212 ([email protected]). 416 I CUTIS® WWW.MDEDGE.COM/CUTIS Copyright Cutis 2018. No part of this publication may be reproduced, stored, or transmitted without the prior written permission of the Publisher. DERMATOPATHOLOGY DIAGNOSIS DISCUSSION THE DIAGNOSIS: Erythrasma rythrasma usually involves intertriginous areas surface (Figure 1) compared to dermatophyte hyphae that (eg, axillae, groin, inframammary area). Patients tend to be parallel to the surface.2 E present with well-demarcated, minimally scaly, red- Pitted keratolysis is a superficial bacterial infection brown patches. -

Copyrighted Material
Part 1 General Dermatology GENERAL DERMATOLOGY COPYRIGHTED MATERIAL Handbook of Dermatology: A Practical Manual, Second Edition. Margaret W. Mann and Daniel L. Popkin. © 2020 John Wiley & Sons Ltd. Published 2020 by John Wiley & Sons Ltd. 0004285348.INDD 1 7/31/2019 6:12:02 PM 0004285348.INDD 2 7/31/2019 6:12:02 PM COMMON WORK-UPS, SIGNS, AND MANAGEMENT Dermatologic Differential Algorithm Courtesy of Dr. Neel Patel 1. Is it a rash or growth? AND MANAGEMENT 2. If it is a rash, is it mainly epidermal, dermal, subcutaneous, or a combination? 3. If the rash is epidermal or a combination, try to define the SIGNS, COMMON WORK-UPS, characteristics of the rash. Is it mainly papulosquamous? Papulopustular? Blistering? After defining the characteristics, then think about causes of that type of rash: CITES MVA PITA: Congenital, Infections, Tumor, Endocrinologic, Solar related, Metabolic, Vascular, Allergic, Psychiatric, Latrogenic, Trauma, Autoimmune. When generating the differential, take the history and location of the rash into account. 4. If the rash is dermal or subcutaneous, then think of cells and substances that infiltrate and associated diseases (histiocytes, lymphocytes, mast cells, neutrophils, metastatic tumors, mucin, amyloid, immunoglobulin, etc.). 5. If the lesion is a growth, is it benign or malignant in appearance? Think of cells in the skin and their associated diseases (keratinocytes, fibroblasts, neurons, adipocytes, melanocytes, histiocytes, pericytes, endothelial cells, smooth muscle cells, follicular cells, sebocytes, eccrine -

Young Adults Young Adults (20 - 35 Years)
YOUNG ADULTS YOUNG ADULTS (20 - 35 YEARS) A large number of skin diseases reach their peak of expression during the young adult years, and these individuals also represent a large and growing proportion of the South African population, in common with other developing countries. Young adults are especially distressed by skin conditions that are uncomfortable, disfiguring or contagious. This group has also been severely affected by HIV/AIDS, with a consequent increase in the frequency and severity of the HIV- associated dermatoses. Some of these conditions have been discussed in other sections of this review. ACNE KELOIDALIS Inflammatory papules and pustules located mainly on the nape of the neck and occiput characterise this acne-like condition. It primarily affects black males. The lesions heal with scarring, creating huge keloids if this tendency exists. The cause is unknown, and unlikely to result from repeated shaving or short hair cutting. It DENGA A MAKHADO may be caused by unusually thick collagen, which traps and disrupts terminal MB ChB, FCDerm (SA) hair follicles. Treatment is not very successful, and large keloids are best excised Consultant Dermatologist by a surgeon. Mild cases can be helped by intralesional injection of steroids like Division of Dermatology Celestone Soluspan into individual papules and scars. Long-term oral tetracy- clines, as for acne, can also be beneficial, as can topical antibiotics like erythro- University of the Witwatersrand and mycin and clindamycin. Chris Hani Baragwanath Hospital Johannesburg ACNE VULGARIS Denga Anna Makhado is a consultant der- There has been a recent tendency for acne to persist beyond the teens, or even matologist at Chris Hani Baragwanath occur for the first time in adulthood, called persistent adult acne. -

Supplement 1 READ Code Description Disease Group Disease Further Specified 1652 Feels Hot/Feverish OTHER OTHER 1653 Fever with S
Supplement 1 Disease further READ code Description Disease group specified 1652 Feels hot/feverish OTHER OTHER 1653 Fever with sweating OTHER OTHER 1712 Dry cough LRTI LRTI - unspecified 1713 Productive cough -clear sputum LRTI LRTI - unspecified 1714 Productive cough -green sputum LRTI LRTI - unspecified 1715 Productive cough-yellow sputum LRTI LRTI - unspecified 1716 Productive cough NOS LRTI LRTI - unspecified 1716.11 Coughing up phlegm LRTI LRTI - unspecified 1717 Night cough present LRTI LRTI - unspecified 1719 Chesty cough LRTI LRTI - unspecified 1719.11 Bronchial cough LRTI LRTI - unspecified 165..11 Fever symptoms OTHER OTHER 165..12 Pyrexia symptoms OTHER OTHER 16L..00 Influenza-like symptoms LRTI INFLUENZA 17...00 Respiratory symptoms LRTI LRTI - unspecified 171..00 Cough LRTI LRTI - unspecified 171..11 C/O - cough LRTI LRTI - unspecified 171A.00 Chronic cough LRTI LRTI - unspecified 171B.00 Persistent cough LRTI LRTI - unspecified 171C.00 Morning cough LRTI LRTI - unspecified 171D.00 Evening cough LRTI LRTI - unspecified 171E.00 Unexplained cough LRTI LRTI - unspecified 171F.00 Cough with fever LRTI LRTI - unspecified 171G.00 Bovine cough LRTI LRTI - unspecified 171H.00 Difficulty in coughing up sputum LRTI LRTI - unspecified 171J.00 Reflux cough LRTI LRTI - unspecified 171K.00 Barking cough LRTI LRTI - unspecified 171L.00 Cough on exercise LRTI LRTI - unspecified 171Z.00 Cough symptom NOS LRTI LRTI - unspecified 173A.00 Exercise induced asthma ASTHMA ASTHMA 173c.00 Occupational asthma ASTHMA ASTHMA 173d.00 Work aggravated asthma -

Bacterial Infections Chapter 14
Bacterial Infections Chapter 14 Infections Caused by Gram Positive Organisms. Michael Hohnadel, D.O. 10/7/03 1 •Staphylococcal Infections • General • 20% of adults are nasal carriers. • HIV infected are more frequent carriers. • Lesions are usually pustules, furuncles or erosions with honey colored crust. • Bullae, erythema, widespread desquamation possible. • Embolic phenomena with endocarditis: • Olser nodes • Janeway Lesions 2 Embolic Phenomena With Endocarditis • Osler nodes Janeway lesion 3 Superficial Pustular Folliculitis • Also known as Impetigo of Bockhart • Presentation: Superficial folliculitis with thin wall, fragile pustules at follicular orifices. – Develops in crops and heal in a few days. – Favored locations: • Extremities and scalp • Face (esp periorally) • Etiology: S. Aureus. 4 Sycosis Vulgaris (Sycosis Barbae) • Perifollicular, Chronic , pustular staph infection of the bearded region. • Presentation: Itch/burn followed by small, perifollicular pustules which rupture. New crops of pustules frequently appear esp after shaving. • Slow spread. • Distinguishing feature is upper lip location and persistence. – Tinea is lower. – Herpes short lived – Pseudofolliculitis Barbea ingrown hair and papules. 5 Sycosis Vulgaris 6 Sycosis Lupoides • Staph infection that through extension results in central hairless scar surrounded by pustules. Pyogenic folliculitis and perifolliculitis with deep extension into hair follicles often with edema. • Thought to resemble lupus vulgaris in appearance. • Etiology: S. Aureus 7 Treatment of Folliculitis • Cleansing with soap and water. • Bactroban (Mupirocin) • Burrows solution for acute inflammation. • Antibiotics: cephalosporin, penicillinase resistant PCN. 8 Furunculosis • Presentation: Perifollicular, round, tender abscess that ends in central suppuration. • Etiology: S. Aureus • Breaks in skin integrity is important. – Various systemic disorders may predispose. • Hospital epidemics of abx resistant staph may occur – Meticulous hand washing is essential. -

WO 2019/094700 Al 16 May 2019 (16.05.2019) W 1P O PCT
(12) INTERNATIONAL APPLICATION PUBLISHED UNDER THE PATENT COOPERATION TREATY (PCT) (19) World Intellectual Property Organization International Bureau (10) International Publication Number (43) International Publication Date WO 2019/094700 Al 16 May 2019 (16.05.2019) W 1P O PCT (51) International Patent Classification: (72) Inventors: SANTOS, Michael; One Kendall Square, C07K 14/435 (2006.01) A01K 67/04 (2006.01) Building 200, Cambridge, Massachusetts 02139 (US). A01K 67/00 (2006.01) C07K 14/00 (2006.01) DELISLE, Scott; One Kendall Square, Building 200, Cam¬ A01K 67/033 (2006.01) bridge, Massachusetts 02139 (US). TWEED-KENT, Ailis; One Kendall Square, Building 200, Cambridge, Massa¬ (21) International Application Number: chusetts 02139 (US). EASTHON, Lindsey; One Kendall PCT/US20 18/059996 Square, Building 200, Cambridge, Massachusetts 02139 (22) International Filing Date: (US). PATTNI, Bhushan S.; 15 Evergreen Circle, Canton, 09 November 2018 (09. 11.2018) Massachusetts 02021 (US). (25) Filing Language: English (74) Agent: WARD, Donna T. et al; DT Ward, P.C., 142A Main Street, Groton, Massachusetts 01450 (US). (26) Publication Language: English (81) Designated States (unless otherwise indicated, for every (30) Priority Data: kind of national protection available): AE, AG, AL, AM, 62/584,153 10 November 2017 (10. 11.2017) US AO, AT, AU, AZ, BA, BB, BG, BH, BN, BR, BW, BY, BZ, 62/659,213 18 April 2018 (18.04.2018) US CA, CH, CL, CN, CO, CR, CU, CZ, DE, DJ, DK, DM, DO, 62/659,209 18 April 2018 (18.04.2018) US DZ, EC, EE, EG, ES, FI, GB, GD, GE, GH, GM, GT, HN, 62/680,386 04 June 2018 (04.06.2018) US HR, HU, ID, IL, IN, IR, IS, JO, JP, KE, KG, KH, KN, KP, 62/680,371 04 June 2018 (04.06.2018) US KR, KW, KZ, LA, LC, LK, LR, LS, LU, LY, MA, MD, ME, (71) Applicant: COCOON BIOTECH INC. -

329 Abscesses, 17, 189. See Also Carbuncles
Cambridge University Press 978-0-521-89729-7 - Skin Infections: Diagnosis and Treatment Edited by John C. Hall and Brian J. Hall Index More information I n d e x abscesses, 17, 189. See also carbuncles; acute infections, primary signs of, 8 American Th oracic Society, 292 furuncles acute miliary cutaneous tuberculosis, 60, 74 American trypanosomiasis, 123 acanthamebiasis, in HIV infection, 193–194 acute necrotizing ulcerative gingivitis, amikacin with tetracycline, for Acanthamoeba spp., 121 294–295 protothecosis, 175 Acanthaster planci (crown of thorns) starfi sh, acute paronychial infections, 268–269 aminoglycosides 173 acyclovir for ecthyma gangrenosum, 215 acellular pertussis (DTaP) vaccination, 294 for congenital herpes simplex, 30 for nocardiosis, 198 acetaminophen, for HSV 1 and 2 infections, for genital herpes, 319 amitriptyline for post-herpetic neuralgia, 31 277 for hand-foot-and-mouth disease, 282 amorolfi ne Acinetobacter baumannii, 189 for herpes simplex virus, 200, 277 nail lacquers, for tinea unguium, 219 Ackerman, A. Bernard, 6 for herpes virus B, 34 topical, for tinea unguium, 236 acne miliaris necrotica, 262 for herpes zoster, 31 amoxicillin Acquired Immune Defi ciency Syndrome for HSV-1/HSV-2, 29 complications from, 33, 278–279 (AIDS). See also HIV-related skin oral, for HSV, 186 for genital bite wounds, 317 infections; Kaposi’s sarcoma (KS) for oral hairy leukoplakia, 187, 279 for Lyme disease, 215 acid-fast bacilli in, 72 for suspected neonatal HSV, 225 for perianal streptococcal dermatitis, 212 anergy, presence of,