Novel Method to Study Autonomic Nervous System Function and Effects
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Distance Learning Program Anatomy of the Human Brain/Sheep Brain Dissection
Distance Learning Program Anatomy of the Human Brain/Sheep Brain Dissection This guide is for middle and high school students participating in AIMS Anatomy of the Human Brain and Sheep Brain Dissections. Programs will be presented by an AIMS Anatomy Specialist. In this activity students will become more familiar with the anatomical structures of the human brain by observing, studying, and examining human specimens. The primary focus is on the anatomy, function, and pathology. Those students participating in Sheep Brain Dissections will have the opportunity to dissect and compare anatomical structures. At the end of this document, you will find anatomical diagrams, vocabulary review, and pre/post tests for your students. The following topics will be covered: 1. The neurons and supporting cells of the nervous system 2. Organization of the nervous system (the central and peripheral nervous systems) 4. Protective coverings of the brain 5. Brain Anatomy, including cerebral hemispheres, cerebellum and brain stem 6. Spinal Cord Anatomy 7. Cranial and spinal nerves Objectives: The student will be able to: 1. Define the selected terms associated with the human brain and spinal cord; 2. Identify the protective structures of the brain; 3. Identify the four lobes of the brain; 4. Explain the correlation between brain surface area, structure and brain function. 5. Discuss common neurological disorders and treatments. 6. Describe the effects of drug and alcohol on the brain. 7. Correctly label a diagram of the human brain National Science Education -

Power Wheelchair Alternative Drive Controls in Spinal Cord Injury
Power Wheelchair Alternative Drive Controls in Spinal Cord Injury Kristen Cezat, PT, DPT, NCS, ATP/SMS When a person with a spinal cord injury is unable to use a standard joystick on a Fact Sheet power wheelchair, an alternative drive control and location is required. Depending on the person’s level of injury and musculature that remains innervated, the more common locations of alternative drive control input devices include the head, neck, face, eyes, and tongue. A proportional drive control allows the wheelchair’s speed/direction to mirror the force/direction applied to the input device by the user, most often through a joystick. Proportional drive control options include1: • Standard Joystick: able to move in any direction at any speed. It is often the most intuitive device for adults with injuries at C5 and below. Joysticks are commonly located on either left or right arm rest but can be altered for Produced by location in midline if spasticity or contracture limits neutral shoulder/elbow alignment. • Alternative Joystick (often set at the user’s chin): joysticks vary in size and require less force and deflection to activate the joystick.1 air Drive ControlA non -Optionsproportional drive for control Clients uses commands with to turn on/offSpinal various functionsCord such as direction (forward, back, left, or right) of the wheelchair. Speed is predetermined and not variable to the strength of the command provided. Non- Injury proportional drive controls include1,2: a Special Interest • Sip-and-Puff Group of • Head Array • Head Array/Sip-and-Puff Combo Non-proportional drive controls can be either momentary or latched. -

Male Reproductive System 2
Male Reproductive System 2 1. Excretory genital ducts 2. The ductus (vas) deferens and seminal vesicles 3. The prostate 4. The bulbourethral (Cowper’s) glands 5. The penis 6. The scrotum and spermatic cord SPLANCHNOLOGY Male reproductive system ° Male reproductive system, systema genitalia masculina: V a part of the human reproductive process ° Male reproductive organs, organa genitalia masculina: V internal genital organs: testicle, testis epididymis, epididymis ductus deferens, ductus (vas) deferens seminal vesicle, vesicula seminalis ejaculatory duct, ductus ejaculatorius prostate gland, prostata V external genital organs: penis, penis scrotum, scrotum bulbourethral glands, glandulae bulbourethrales Prof. Dr. Nikolai Lazarov 2 SPLANCHNOLOGY Ductus (vas) deferens ° Ductus (vas) deferens: V a straight thick-walled muscular tube V transports sperm cells from the epididymis V length 45-50 cm V diameter 2.5-3 mm ° Anatomical parts: V testicular part V funicular part V inguinal part – 4 cm V pelvic part ° Ampulla ductus deferentis: V length 3-4 cm; diameter 1 cm V ejaculatory duct, ductus ejaculatorius Prof. Dr. Nikolai Lazarov 3 SPLANCHNOLOGY Microscopic anatomy ° tunica mucosa – 5-6 longitudinal folds: V lamina epithelialis – bilayered columnar epithelium with stereocilia V lamina propria: dense connective tissue elastic fibers ° tunica muscularis – thick: V inner longitudinal layer – in the initial portion V circular layer V outer longitudinal layer ° tunica adventitia (serosa) Prof. Dr. Nikolai Lazarov 4 SPLANCHNOLOGY Seminal vesicle, vesicula seminalis ° Seminal vesicle, vesicula (glandula) seminalis: V a pair of simple tubular glands – two highly tortuous tubes V posterior to the urinary bladder V length 4-5 (15) cm V diameter 1 cm ° Macroscopic anatomy: V anterior and posterior part V excretory duct Prof. -

Basic Brain Anatomy
Chapter 2 Basic Brain Anatomy Where this icon appears, visit The Brain http://go.jblearning.com/ManascoCWS to view the corresponding video. The average weight of an adult human brain is about 3 pounds. That is about the weight of a single small To understand how a part of the brain is disordered by cantaloupe or six grapefruits. If a human brain was damage or disease, speech-language pathologists must placed on a tray, it would look like a pretty unim- first know a few facts about the anatomy of the brain pressive mass of gray lumpy tissue (Luria, 1973). In in general and how a normal and healthy brain func- fact, for most of history the brain was thought to be tions. Readers can use the anatomy presented here as an utterly useless piece of flesh housed in the skull. a reference, review, and jumping off point to under- The Egyptians believed that the heart was the seat standing the consequences of damage to the structures of human intelligence, and as such, the brain was discussed. This chapter begins with the big picture promptly removed during mummification. In his and works down into the specifics of brain anatomy. essay On Sleep and Sleeplessness, Aristotle argued that the brain is a complex cooling mechanism for our bodies that works primarily to help cool and The Central Nervous condense water vapors rising in our bodies (Aristo- tle, republished 2011). He also established a strong System argument in this same essay for why infants should not drink wine. The basis for this argument was that The nervous system is divided into two major sec- infants already have Central nervous tions: the central nervous system and the peripheral too much moisture system The brain and nervous system. -

Study Guide Medical Terminology by Thea Liza Batan About the Author
Study Guide Medical Terminology By Thea Liza Batan About the Author Thea Liza Batan earned a Master of Science in Nursing Administration in 2007 from Xavier University in Cincinnati, Ohio. She has worked as a staff nurse, nurse instructor, and level department head. She currently works as a simulation coordinator and a free- lance writer specializing in nursing and healthcare. All terms mentioned in this text that are known to be trademarks or service marks have been appropriately capitalized. Use of a term in this text shouldn’t be regarded as affecting the validity of any trademark or service mark. Copyright © 2017 by Penn Foster, Inc. All rights reserved. No part of the material protected by this copyright may be reproduced or utilized in any form or by any means, electronic or mechanical, including photocopying, recording, or by any information storage and retrieval system, without permission in writing from the copyright owner. Requests for permission to make copies of any part of the work should be mailed to Copyright Permissions, Penn Foster, 925 Oak Street, Scranton, Pennsylvania 18515. Printed in the United States of America CONTENTS INSTRUCTIONS 1 READING ASSIGNMENTS 3 LESSON 1: THE FUNDAMENTALS OF MEDICAL TERMINOLOGY 5 LESSON 2: DIAGNOSIS, INTERVENTION, AND HUMAN BODY TERMS 28 LESSON 3: MUSCULOSKELETAL, CIRCULATORY, AND RESPIRATORY SYSTEM TERMS 44 LESSON 4: DIGESTIVE, URINARY, AND REPRODUCTIVE SYSTEM TERMS 69 LESSON 5: INTEGUMENTARY, NERVOUS, AND ENDOCRINE S YSTEM TERMS 96 SELF-CHECK ANSWERS 134 © PENN FOSTER, INC. 2017 MEDICAL TERMINOLOGY PAGE III Contents INSTRUCTIONS INTRODUCTION Welcome to your course on medical terminology. You’re taking this course because you’re most likely interested in pursuing a health and science career, which entails proficiencyincommunicatingwithhealthcareprofessionalssuchasphysicians,nurses, or dentists. -

Pdf Manual (964.7Kb)
MD-17 , CONTENTS THE URINARY SYSTEM 4 THE REPRODUCTIVE SYSTEM 5 The Scrotum The Testis The Epididylnis The Ductus Deferens The Ejaculatory Duct The Seminal Vesicle The Spermatic Cord The Penis The Prostate Gland THE INGUINAL CANAL l) HERNIAS FURTIlER READING 10 MODEL KEY 1I Human Male Pelvis This life-size model shows the viscera and structures which form the urogenital system and some of the related anatomy such as the sig moid colon and rectum. The vascular supply to the viscera and support ing tissue is demonstrated, as well as that portion of the vascular system which continues into the lower extremity. The model is divided into right and left portions. The right portion shows a midsagittal section of the pelvic structures. The left represents a similar section, but the dissection is deeper. Two pieces are remov able on the left side; one piece includes the bladder, prostate, and semi nal vesicles, and the other includes the penis, left testicle, and scrotum. When all portions are removed, a deeper view of these structures and a deeper dissection of the pelvis can be seen. THE URINARY SYSTEM The portion of the urinary system shown depicts the ureter from the level of the 5th lumbar vertebra, where it passes the common iliac ar tery near the bifurcation of thi s artery into the external and internal iliac arteries. The ureter then passes toward the posterior portion of the bladder, beneath the vas deferens, and opens through the wall of the blad der at one cranial corner of the trigone on the bladder's interior. -

Anatomy and Physiology Male Reproductive System References
DEWI PUSPITA ANATOMY AND PHYSIOLOGY MALE REPRODUCTIVE SYSTEM REFERENCES . Tortora and Derrickson, 2006, Principles of Anatomy and Physiology, 11th edition, John Wiley and Sons Inc. Medical Embryology Langeman, pdf. Moore and Persaud, The Developing Human (clinically oriented Embryologi), 8th edition, Saunders, Elsevier, . Van de Graff, Human anatomy, 6th ed, Mcgraw Hill, 2001,pdf . Van de Graff& Rhees,Shaum_s outline of human anatomy and physiology, Mcgraw Hill, 2001, pdf. WHAT IS REPRODUCTION SYSTEM? . Unlike other body systems, the reproductive system is not essential for the survival of the individual; it is, however, required for the survival of the species. The RS does not become functional until it is “turned on” at puberty by the actions of sex hormones sets the reproductive system apart. The male and female reproductive systems complement each other in their common purpose of producing offspring. THE TOPIC : . 1. Gamet Formation . 2. Primary and Secondary sex organ . 3. Male Reproductive system . 4. Female Reproductive system . 5. Female Hormonal Cycle GAMET FORMATION . Gamet or sex cells are the functional reproductive cells . Contain of haploid (23 chromosomes-single) . Fertilizationdiploid (23 paired chromosomes) . One out of the 23 pairs chromosomes is the determine sex sex chromosome X or Y . XXfemale, XYmale Gametogenesis Oocytes Gameto Spermatozoa genesis XY XX XX/XY MALE OR FEMALE....? Male Reproductive system . Introduction to the Male Reproductive System . Scrotum . Testes . Spermatic Ducts, Accessory Reproductive Glands,and the Urethra . Penis . Mechanisms of Erection, Emission, and Ejaculation The urogenital system . Functionally the urogenital system can be divided into two entirely different components: the urinary system and the genital system. -

Neurogenic Erectile Dysfunction. Where Do We Stand?
medicines Review Neurogenic Erectile Dysfunction. Where Do We Stand? Charalampos Thomas 1,* and Charalampos Konstantinidis 2 1 Urology Department, General Hospital of Corinth, 20131 Corinth, Greece 2 Urology & Neurourology Unit, National Rehabilitation Center, Ilion, 13122 Athens, Greece; [email protected] * Correspondence: [email protected] Abstract: Erectile Dysfunction (ED) is the persistent inability to attain and maintain an erection sufficient to permit satisfactory sexual performance, causing tremendous effects on both patients and their partners. The pathophysiology of ED remains a labyrinth. The underlying mechanisms of ED may be vasculogenic, neurogenic, anatomical, hormonal, drug-induced and/or psychogenic. Neurogenic ED consists of a large cohort of ED, accounting for about 10% to 19% of all cases. Its diversity does not allow an in-depth clarification of all the underlying mechanisms nor a “one size fits all” therapeutical approach. In this review, we focus on neurogenic causes of ED, trying to elucidate the mechanisms that lie beneath it and how we manage these patients. Keywords: erectile dysfunction (ED); neurogenic; sexual dysfunction (SD); phosphodiesterase type-5 inhibitors (PDE5I); spinal cord injury (SCI); multiple sclerosis (MS) 1. Introduction Erectile dysfunction (ED) is defined as the persistent inability to attain and maintain an erection sufficient to permit satisfactory sexual performance [1]. Besides the obvious, it has tremendous effects on the patient’s psychosocial health, and it affects not only their quality of life but the lives of their partners [2]. Citation: Thomas, C.; Konstantinidis, The pathophysiology of ED remains a labyrinth since many pathways can co-exist, C. Neurogenic Erectile Dysfunction. thus contributing negatively. Where Do We Stand? Medicines 2021, Traditionally ED was divided into three large cohorts, organic, psychogenic and of 8, 3. -

Nomina Histologica Veterinaria, First Edition
NOMINA HISTOLOGICA VETERINARIA Submitted by the International Committee on Veterinary Histological Nomenclature (ICVHN) to the World Association of Veterinary Anatomists Published on the website of the World Association of Veterinary Anatomists www.wava-amav.org 2017 CONTENTS Introduction i Principles of term construction in N.H.V. iii Cytologia – Cytology 1 Textus epithelialis – Epithelial tissue 10 Textus connectivus – Connective tissue 13 Sanguis et Lympha – Blood and Lymph 17 Textus muscularis – Muscle tissue 19 Textus nervosus – Nerve tissue 20 Splanchnologia – Viscera 23 Systema digestorium – Digestive system 24 Systema respiratorium – Respiratory system 32 Systema urinarium – Urinary system 35 Organa genitalia masculina – Male genital system 38 Organa genitalia feminina – Female genital system 42 Systema endocrinum – Endocrine system 45 Systema cardiovasculare et lymphaticum [Angiologia] – Cardiovascular and lymphatic system 47 Systema nervosum – Nervous system 52 Receptores sensorii et Organa sensuum – Sensory receptors and Sense organs 58 Integumentum – Integument 64 INTRODUCTION The preparations leading to the publication of the present first edition of the Nomina Histologica Veterinaria has a long history spanning more than 50 years. Under the auspices of the World Association of Veterinary Anatomists (W.A.V.A.), the International Committee on Veterinary Anatomical Nomenclature (I.C.V.A.N.) appointed in Giessen, 1965, a Subcommittee on Histology and Embryology which started a working relation with the Subcommittee on Histology of the former International Anatomical Nomenclature Committee. In Mexico City, 1971, this Subcommittee presented a document entitled Nomina Histologica Veterinaria: A Working Draft as a basis for the continued work of the newly-appointed Subcommittee on Histological Nomenclature. This resulted in the editing of the Nomina Histologica Veterinaria: A Working Draft II (Toulouse, 1974), followed by preparations for publication of a Nomina Histologica Veterinaria. -

SCI Facts and Figures at a Glance 2019.Pdf
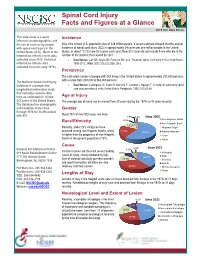
Spinal Cord Injury Facts and Figures at a Glance 2019 SCI Data Sheet This data sheet is a quick Incidence reference on demographics and the use of services by people Given the current U.S. population size of 328 million people, a recent estimate showed that the annual with spinal cord injury in the incidence of spinal cord injury (SCI) is approximately 54 cases per one million people in the United United States (U.S.). Much of the States, or about 17,730 new SCI cases each year. New SCI cases do not include those who die at the information reflects recent data location of the incident that caused the SCI. collected since 2015. Historical Data Source: Jain NB, Ayers GD, Peterson EN, et al. Traumatic spinal cord injury in the United States, information reflects data 1993-2012. JAMA. 2015;313(22):2236-2243. collected since the early 1970s. Prevalence The estimated number of people with SCI living in the United States is approximately 291,000 persons, with a range from 249,000 to 363,000 persons. The National Spinal Cord Injury Database is a prospective Data Source: Lasfargues JE, Custis D, Morrone F, Carswell J, Nguyen T. A model for estimating spinal longitudinal multicenter study cord injury prevalence in the United States. Paraplegia. 1995;33(2):62-68. that currently captures data from an estimated 6% of new Age at Injury SCI cases in the United States. The average age at injury has increased from 29 years during the 1970s to 43 years recently. The database has demographic and condition status data Gender through 2018 for 33,406 people About 78% of new SCI cases are male. -

The Morphological Characters of the Male External Genitalia of the European Hedgehog (Erinaceus Europaeus) G
View metadata, citation and similar papers at core.ac.uk brought to you by CORE Foliaprovided Morphol. by Via Medica Journals Vol. 77, No. 2, pp. 293–300 DOI: 10.5603/FM.a2017.0098 O R I G I N A L A R T I C L E Copyright © 2018 Via Medica ISSN 0015–5659 www.fm.viamedica.pl The morphological characters of the male external genitalia of the European hedgehog (Erinaceus Europaeus) G. Akbari1, M. Babaei1, N. Goodarzi2 1Department of Basic Sciences, Faculty of Veterinary Medicine, University of Tabriz, Tabriz, Iran 2Department of Basic Sciences, Faculty of Veterinary Medicine, Razi University, Kermanshah, Iran [Received: 7 June 2017; Accepted: 11 September 2017] This study was conducted to depict anatomical characteristics of the penis of he- dgehog. Seven sexually mature male European hedgehogs were used. Following anaesthesia, the animals were scarified with chloroform inhalation. Gross penile characteristics such as length and diameter were thoroughly explored and measu- red using digital callipers. Tissue samples stained with haematoxylin and eosin and Masson’s trichrome for microscopic analysis. The penis of the European hedgehog was composed of a pair of corpus cavernosum penis and the glans penis without corpus spongiosum penis. The urethra at the end of penis, protruded as urethral process, on both sides of which two black nail-like structures, could be observed. The lower part was rounded forming a blind sac (sacculus urethralis) with a me- dian split below the urethra. Microscopically, the penile bulb lacked the corpus spongiosum penis, but, corpus spongiosum glans was seen at the beginning of the free part. -
The Nervous System: Sensory and Motor Tracts of the Spinal Cord
15 The Nervous System: Sensory and Motor Tracts of the Spinal Cord PowerPoint® Lecture Presentations prepared by Steven Bassett Southeast Community College Lincoln, Nebraska © 2012 Pearson Education, Inc. Introduction • Millions of sensory neurons are delivering information to the CNS all the time • Millions of motor neurons are causing the body to respond in a variety of ways • Sensory and motor neurons travel by different tracts within the spinal cord © 2012 Pearson Education, Inc. Sensory and Motor Tracts • Communication to and from the brain involves tracts • Ascending tracts are sensory • Deliver information to the brain • Descending tracts are motor • Deliver information to the periphery © 2012 Pearson Education, Inc. Sensory and Motor Tracts • Naming the tracts • If the tract name begins with “spino” (as in spinocerebellar), the tract is a sensory tract delivering information from the spinal cord to the cerebellum (in this case) • If the tract name ends with “spinal” (as in vestibulospinal), the tract is a motor tract that delivers information from the vestibular apparatus (in this case) to the spinal cord © 2012 Pearson Education, Inc. Sensory and Motor Tracts • There are three major sensory tracts • The posterior column tract • The spinothalamic tract • The spinocerebellar tract © 2012 Pearson Education, Inc. Sensory and Motor Tracts • The three major sensory tracts involve chains of neurons • First-order neuron • Delivers sensations to the CNS • The cell body is in the dorsal or cranial root ganglion • Second-order neuron • An interneuron with the cell body in the spinal cord or brain • Third-order neuron • Transmits information from the thalamus to the cerebral cortex © 2012 Pearson Education, Inc.