Winged Scapula
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
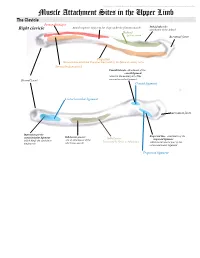
Muscle Attachment Sites in the Upper Limb
This document was created by Alex Yartsev ([email protected]); if I have used your data or images and forgot to reference you, please email me. Muscle Attachment Sites in the Upper Limb The Clavicle Pectoralis major Smooth superior surface of the shaft, under the platysma muscle Deltoid tubercle: Right clavicle attachment of the deltoid Deltoid Axillary nerve Acromial facet Trapezius Sternocleidomastoid and Trapezius innervated by the Spinal Accessory nerve Sternocleidomastoid Conoid tubercle, attachment of the conoid ligament which is the medial part of the Sternal facet coracoclavicular ligament Conoid ligament Costoclavicular ligament Acromial facet Impression for the Trapezoid line, attachment of the costoclavicular ligament Subclavian groove: Subclavius trapezoid ligament which binds the clavicle to site of attachment of the Innervated by Nerve to Subclavius which is the lateral part of the the first rib subclavius muscle coracoclavicular ligament Trapezoid ligament This document was created by Alex Yartsev ([email protected]); if I have used your data or images and forgot to reference you, please email me. The Scapula Trapezius Right scapula: posterior Levator scapulae Supraspinatus Deltoid Deltoid and Teres Minor are innervated by the Axillary nerve Rhomboid minor Levator Scapulae, Rhomboid minor and Rhomboid Major are innervated by the Dorsal Scapular Nerve Supraspinatus and Infraspinatus innervated by the Suprascapular nerve Infraspinatus Long head of triceps Rhomboid major Teres Minor Teres Major Teres Major -

Examination of the Shoulder Bruce S
Examination of the Shoulder Bruce S. Wolock, MD Towson Orthopaedic Associates 3 Joints, 1 Articulation 1. Sternoclavicular 2. Acromioclavicular 3. Glenohumeral 4. Scapulothoracic AC Separation Bony Landmarks 1. Suprasternal notch 2. Sternoclavicular joint 3. Coracoid 4. Acromioclavicular joint 5. Acromion 6. Greater tuberosity of the humerus 7. Bicipital groove 8. Scapular spine 9. Scapular borders-vertebral and lateral Sternoclavicular Dislocation Soft Tissues 1. Rotator Cuff 2. Subacromial bursa 3. Axilla 4. Muscles: a. Sternocleidomastoid b. Pectoralis major c. Biceps d. Deltoid Congenital Absence of Pectoralis Major Pectoralis Major Rupture Soft Tissues (con’t) e. Trapezius f. Rhomboid major and minor g. Latissimus dorsi h. Serratus anterior Range of Motion: Active and Passive 1. Abduction - 90 degrees 2. Adduction - 45 degrees 3. Extension - 45 degrees 4. Flexion - 180 degrees 5. Internal rotation – 90 degrees 6. External rotation – 45 degrees Muscle Testing 1. Flexion a. Primary - Anterior deltoid (axillary nerve, C5) - Coracobrachialis (musculocutaneous nerve, C5/6 b. Secondary - Pectoralis major - Biceps Biceps Rupture- Longhead Muscle Testing 2. Extension a. Primary - Latissimus dorsi (thoracodorsal nerve, C6/8) - Teres major (lower subscapular nerve, C5/6) - Posterior deltoid (axillary nerve, C5/6) b. Secondary - Teres minor - Triceps Abduction Primary a. Middle deltoid (axillary nerve, C5/6) b. Supraspinatus (suprascapular nerve, C5/6) Secondary a. Anterior and posterior deltoid b. Serratus anterior Deltoid Ruputure Axillary Nerve Palsy Adduction Primary a. Pectoralis major (medial and lateral pectoral nerves, C5-T1 b. Latissimus dorsi (thoracodorsal nerve, C6/8) Secondary a. Teres major b. Anterior deltoid External Rotation Primary a. Infraspinatus (suprascapular nerve, C5/6) b. Teres minor (axillary nerve, C5) Secondary a. -

Stichting Voor Ooglijders Prof. Dr. HJ
De publicatie van dit proefschrift werd mede mogelijk gemaakt met fmanciele steun van: Stichting voor Ooglijders Prof. Dr. H.J. Flieringa Stichting Medical Workshop BV Kabi Pharmacia Bournonville-Pharma BV Ter herinnering aan mijn vader Omslag: Henry Cannon I Ebbo Clerlo: CLINICAL ASPECTS AND ETIOLOGY OF FUCHS' HETEROCHROMIC CYCLITIS (KLINISCHE ASPECTEN EN ETIOLOGIE VAN DE HETEROCHROME CYCLITIS VAN FUCHS) proefschrift Ter verkrijging van de graad van doctor aan de Erasmus Universiteit Rotterdam op gezag van de Rector Magnificus Prof. dr. P.W.C. Akkermans M. Lit. en volgens besluit van het College van Dekanen. De openbare verdediding zal plaatsvinden op woensdag 3 November 1993 om 15.45 uur. door Ellen Carolien La Heij geboren te Arnstelveen PROMOTIE-COMMISSIE PROMOTORES' Prof. dr. P.T.V.M. de Jong Prof. dr. A. Kijlstra OVERIGE LEDEN, Prof. dr. F.T. Bosman Prof. dr. H.A. Drexhage CONTENTS Chapter 1 1.1 General Introduction ........................ 7 1. 2 Aim of the Thesis_ ................... __ ...... 8 Chapter 2 Fuchs' Heterochromic Cyclitis: Review of the Literature (submitted for publication) 2.1 Historical Background ........................ 9 2.2 Terminology and Classification ............... 9 2. 3 Epidemiology. .11 2. 4 Clinical Features ........................... 11. 2.5 Histopathology of the Iris ................. 22 2. 6 Etiologic Mechanisms ........................ 25 2.7 Therapy and Prognosis .................... ... 37 Chapter 3 Clin~c~l analysis of Fuchs' heterochromic cycl1t1s ........................................ 49 (Doc Ophthalmol. 1991;78:225-235). Chapter 4 Treatment and prognosis of secondary glaucoma in Fuchs' heterochromic cyclitis ............... .... 61 (Am J Ophthalmol. 1993, in press) Chapter 5 Quantitative analysis of iris translucency in Fuchs' heterochromic cyclitis ................. .. 83 (Invest Ophthalmol & Vis Sci. -

Orphanet Report Series Rare Diseases Collection
Marche des Maladies Rares – Alliance Maladies Rares Orphanet Report Series Rare Diseases collection DecemberOctober 2013 2009 List of rare diseases and synonyms Listed in alphabetical order www.orpha.net 20102206 Rare diseases listed in alphabetical order ORPHA ORPHA ORPHA Disease name Disease name Disease name Number Number Number 289157 1-alpha-hydroxylase deficiency 309127 3-hydroxyacyl-CoA dehydrogenase 228384 5q14.3 microdeletion syndrome deficiency 293948 1p21.3 microdeletion syndrome 314655 5q31.3 microdeletion syndrome 939 3-hydroxyisobutyric aciduria 1606 1p36 deletion syndrome 228415 5q35 microduplication syndrome 2616 3M syndrome 250989 1q21.1 microdeletion syndrome 96125 6p subtelomeric deletion syndrome 2616 3-M syndrome 250994 1q21.1 microduplication syndrome 251046 6p22 microdeletion syndrome 293843 3MC syndrome 250999 1q41q42 microdeletion syndrome 96125 6p25 microdeletion syndrome 6 3-methylcrotonylglycinuria 250999 1q41-q42 microdeletion syndrome 99135 6-phosphogluconate dehydrogenase 67046 3-methylglutaconic aciduria type 1 deficiency 238769 1q44 microdeletion syndrome 111 3-methylglutaconic aciduria type 2 13 6-pyruvoyl-tetrahydropterin synthase 976 2,8 dihydroxyadenine urolithiasis deficiency 67047 3-methylglutaconic aciduria type 3 869 2A syndrome 75857 6q terminal deletion 67048 3-methylglutaconic aciduria type 4 79154 2-aminoadipic 2-oxoadipic aciduria 171829 6q16 deletion syndrome 66634 3-methylglutaconic aciduria type 5 19 2-hydroxyglutaric acidemia 251056 6q25 microdeletion syndrome 352328 3-methylglutaconic -

Dorsal Scapular Nerve Neuropathy: a Narrative Review of the Literature Brad Muir, Bsc.(Hons), DC, FRCCSS(C)1
ISSN 0008-3194 (p)/ISSN 1715-6181 (e)/2017/128–144/$2.00/©JCCA 2017 Dorsal scapular nerve neuropathy: a narrative review of the literature Brad Muir, BSc.(Hons), DC, FRCCSS(C)1 Objective: The purpose of this paper is to elucidate Objectif : Ce document a pour objectif d’élucider this little known cause of upper back pain through a cette cause peu connue de douleur dans le haut du narrative review of the literature and to discuss the dos par un examen narratif de la littérature, ainsi que possible role of the dorsal scapular nerve (DSN) in de discuter du rôle possible du nerf scapulaire dorsal the etiopathology of other similar diagnoses in this (NSD) dans l’étiopathologie d’autres diagnostics area including cervicogenic dorsalgia (CD), notalgia semblables dans ce domaine, y compris la dorsalgie paresthetica (NP), SICK scapula and a posterolateral cervicogénique (DC), la notalgie paresthésique (NP), arm pain pattern. l’omoplate SICK et un schéma de douleur postéro- Background: Dorsal scapular nerve (DSN) latérale au bras. neuropathy has been a rarely thought of differential Contexte : La neuropathie du nerf scapulaire dorsal diagnosis for mid scapular, upper to mid back and (NSD) constitue un diagnostic différentiel rare pour la costovertebral pain. These are common conditions douleur mi-scapulaire, costo-vertébrale et au bas/haut presenting to chiropractic, physiotherapy, massage du dos. Il s’agit de troubles communs qui surgissent therapy and medical offices. dans les cabinets de chiropratique, de physiothérapie, de Methods: The methods used to gather articles for this massothérapie et de médecin. paper included: searching electronic databases; and Méthodologie : Les méthodes utilisées pour hand searching relevant references from journal articles rassembler les articles de ce document comprenaient la and textbook chapters. -

Brachial Plexus Posterior Cord Variability: a Case Report and Review
CASE REPORT Brachial plexus posterior cord variability: a case report and review Edward O, Arachchi A, Christopher B Edward O, Arachchi A, Christopher B. Brachial plexus posterior cord anatomical variability. This case report details the anatomical variants discovered variability: a case report and review. Int J Anat Var. 2017;10(3):49-50. in the posterior cord of the brachial plexus in a routine cadaveric dissection at the University of Melbourne, Australia. Similar findings in the literature are reviewed ABSTRACT and the clinical significance of these findings is discussed. The formation and distribution of the brachial plexus is a source of great Key Words: Brachial plexus; Posterior cord; Axillary nerve; Anatomical variation INTRODUCTION he brachial plexus is the neural network that supplies motor and sensory Tinnervation to the upper limb. It is typically composed of anterior rami from C5 to T1 spinal segments, which subsequently unite to form superior, middle and inferior trunks. These trunks divide and reunite to form cords 1 surrounding the axillary artery, which terminate in branches of the plexus. The posterior cord is classically described as a union of the posterior divisions from the superior, middle and inferior trunks of the brachial plexus, with fibres from all five spinal segments. The upper subscapular, thoracodorsal and lower subscapular nerves propagate from the cord prior to the axillary and radial nerves forming terminal branches. Variability in the brachial plexus is frequently reported in the literature. It is C5 nerve root Suprascapular nerve important for clinicians to be aware of possible variations when considering Posterior division of C5-C6 injuries or disease of the upper limb. -

Board Review for Anatomy
Board Review for Anatomy John A. McNulty, Ph.D. Spring, 2005 . LOYOLA UNIVERSITY CHICAGO Stritch School of Medicine Key Skeletal landmarks • Head - mastoid process, angle of mandible, occipital protuberance • Neck – thyroid cartilage, cricoid cartilage • Thorax - jugular notch, sternal angle, xiphoid process, coracoid process, costal arch • Back - vertebra prominence, scapular spine (acromion), iliac crest • UE – epicondyles, styloid processes, carpal bones. • Pelvis – ant. sup. iliac spine, pubic tubercle • LE – head of fibula, malleoli, tarsal bones Key vertebral levels • C2 - angle of mandible • C4 - thyroid notch • C6 - cricoid cartilage - esophagus, trachea begin • C7 - vertebra prominence • T2 - jugular notch; scapular spine • T4/5 - sternal angle - rib 2 articulates, trachea divides • T9 - xiphisternum • L1/L2 - pancreas; spinal cord ends. • L4 - iliac crest; umbilicus; aorta divides • S1 - sacral promontory Upper limb nerve lesions Recall that any muscle that crosses a joint, acts on that joint. Also recall that muscles innervated by individual nerves within compartments tend to have similar actions. • Long thoracic n. - “winged” scapula. • Upper trunk (C5,C6) - Erb Duchenne - shoulder rotators, musculocutaneous • Lower trunk (C8, T1) - Klumpke’s - ulnar nerve (interossei muscle) • Radial nerve – (Saturday night palsy) - wrist drop • Median nerve (recurrent median) – thenar compartment - thumb • Ulnar nerve - interossei muscles. Lower limb nerve lesions Review actions of the various compartments. • Lumbosacral lesions - usually -

Tricks and Techniques to Maximize Success with Nerve Transfers
IC12-L: Tricks and Techniques to Maximize Success with Nerve Transfers Moderator(s): Susan E. Mackinnon, MD Faculty: Christine B. Novak, PT, PhD and J. Megan Patterson, MD Session Handouts Friday, October 02, 2020 75TH VIRTUAL ANNUAL MEETING OF THE ASSH OCTOBER 1-3, 2020 822 West Washington Blvd Chicago, IL 60607 Phone: (312) 880-1900 Web: www.assh.org Email: [email protected] All property rights in the material presented, including common-law copyright, are expressly reserved to the speaker or the ASSH. No statement or presentation made is to be regarded as dedicated to the public domain. IC12 – Tricks and Techniques to Maximize Success with Nerve Transfers American Society for Surgery of the Hand Annual Meeting, October 2, 2020 Susan E. Mackinnon, MD, St. Louis, Missouri J. Megan M. Patterson, Chapel Hill, North Carolina Christine B. Novak, PT, PhD, Toronto, Ontario Andrew Yee, BS, St. Louis, Missouri Overview: Following complex nerve injury, motor and sensory recovery can be less than optimal. For high median, ulnar and radial nerve injuries, nerve transfers can provide a distal source of motor and/or sensory innervation closer to the target end organ allowing for faster recovery and improved outcome. This course will focus on techniques to maximize success with upper extremity motor and sensory nerve transfers. Classification of Nerve Injury: Degree of Injury Tinel’s Sign Recovery Rate of Surgical Procedure Present Recovery I Neurapraxia No Complete Up to 12 weeks None II Axonotmesis Yes Complete 1” per month None III Yes Varies * -

SŁOWNIK ANATOMICZNY (ANGIELSKO–Łacinsłownik Anatomiczny (Angielsko-Łacińsko-Polski)´ SKO–POLSKI)
ANATOMY WORDS (ENGLISH–LATIN–POLISH) SŁOWNIK ANATOMICZNY (ANGIELSKO–ŁACINSłownik anatomiczny (angielsko-łacińsko-polski)´ SKO–POLSKI) English – Je˛zyk angielski Latin – Łacina Polish – Je˛zyk polski Arteries – Te˛tnice accessory obturator artery arteria obturatoria accessoria tętnica zasłonowa dodatkowa acetabular branch ramus acetabularis gałąź panewkowa anterior basal segmental artery arteria segmentalis basalis anterior pulmonis tętnica segmentowa podstawna przednia (dextri et sinistri) płuca (prawego i lewego) anterior cecal artery arteria caecalis anterior tętnica kątnicza przednia anterior cerebral artery arteria cerebri anterior tętnica przednia mózgu anterior choroidal artery arteria choroidea anterior tętnica naczyniówkowa przednia anterior ciliary arteries arteriae ciliares anteriores tętnice rzęskowe przednie anterior circumflex humeral artery arteria circumflexa humeri anterior tętnica okalająca ramię przednia anterior communicating artery arteria communicans anterior tętnica łącząca przednia anterior conjunctival artery arteria conjunctivalis anterior tętnica spojówkowa przednia anterior ethmoidal artery arteria ethmoidalis anterior tętnica sitowa przednia anterior inferior cerebellar artery arteria anterior inferior cerebelli tętnica dolna przednia móżdżku anterior interosseous artery arteria interossea anterior tętnica międzykostna przednia anterior labial branches of deep external rami labiales anteriores arteriae pudendae gałęzie wargowe przednie tętnicy sromowej pudendal artery externae profundae zewnętrznej głębokiej -

Langer's Axillary Arch (Axillopectoral Muscle): a Variation of Latissimus
eISSN 1308-4038 International Journal of Anatomical Variations (2010) 3: 91–92 Case Report Langer’s axillary arch (axillopectoral muscle): a variation of latissimus dorsi muscle Published online June 30th, 2010 © http://www.ijav.org Sinan BAKIRCI ABSTRACT Ilker Mustafa KAFA Langer’s axillary arch (axillopectoral muscle) is a variant muscular structure of the axilla which was described Murat UYSAL under various names as Langer’s muscle, axillary arch or muscular axillary arch by different authors. During Erdogan SENDEMIR routine dissections, we found a muscular slip on the right axillary fossa that originated from latissimus dorsi muscle and attached to the deep surface of the tendon of pectoralis major muscle, and described it as Langer’s axillary arch. Arterial, venous and nervous structures passed under this muscular slip which constitutes an arch in the axillary fossa. Although axillary arch is not very rare, it is generally neglected and not explored or described well. It has immense clinical and morphologic importance for surgical operations performed on axillary region; thus, surgeons should well be aware of its possible existence. © IJAV. 2010; 3: 91–92. Department of Anatomy, Faculty of Medicine, Uludag University, Bursa, TURKEY. Ilker Mustafa Kafa, MD Department of Anatomy Uludag University Faculty of Medicine Gorukle, 16059, Bursa, TURKEY. +90 (224) 295 23 16 [email protected] Received November 20th, 2009; accepted June 21st, 2010 Key words [axillary arch] [Langer’s muscle] [latissimus dorsi muscle] [axillopectoral muscle] [axillary fossa] Introduction os ilium. The axillary arch is a variant muscular slip of Best-known variant structure of the axillary components this muscle and is about 7 to 10 cm in length, splits from of men is a muscular or fibro-muscular slip extending the upper edge of the latissimus dorsi and crosses the from the latissimus dorsi muscle to the tendons, muscles or axilla in front of the axillary vessels and nerves [4]. -

Scapular Winging Secondary to Apparent Long Thoracic Nerve Palsy in a Young Female Swimmer
THIEME Case Report e57 Scapular Winging Secondary to Apparent Long Thoracic Nerve Palsy in a Young Female Swimmer Shiro Nawa1 1 Department of Judo Seifuku and Health Sciences, Faculty of Health Address for correspondence Shiro Nawa, MS, Department of Judo Promotional Sciences, Tokoha University, Hamamatsu City, Seifuku and Health Sciences, Faculty of Health Promotional Sciences, Shizuoka-ken, Japan Tokoha University, 1230 Miyakoda-cho, Kita-ku, Hamamatsu City, Shizuoka-ken, 431-2102, Japan J Brachial Plex Peripher Nerve Inj 2015;10:e57–e61. (e-mail: [email protected]). Abstract Background In neurological diseases, winging of the scapula occurs because of serratus anterior muscle dysfunction due to long thoracic nerve palsy, or trapezius muscle dysfunction due to accessory nerve palsy. Several sports can cause long thoracic nerve palsy, including archery and tennis. To our knowledge, this is the first report of long thoracic nerve palsy in an aquatic sport. Objective The present study is a rare case of winging of the scapula that occurred during synchronized swimming practice. Methods The patient’s history with the present illness, examination findings, rehabili- tation progress, and related medical literature are presented. Keywords Results A 14-year-old female synchronized swimmer had chief complaints of muscle ► winging of the weakness, pain, and paresthesia in the right scapula. Upon examination, marked scapula winging of the scapula appeared during anterior arm elevation, as did floating of the ► accessory nerve palsy superior angle. After 1 year of therapy, right shoulder girdle pain and paresthesia had ► long thoracic nerve disappeared; however, winging of the scapula remained. palsy Conclusions Based on this observation and the severe pain in the vicinity of the second ► synchronized dorsal rib, we believe the cause was damage to the nerve proximal to the branch arising swimming from the upper nerve trunk that innervates the serratus anterior. -

Occupational Shoulder.Pdf
ORIGINAL PAPER International Journal of Occupational Medicine and Environmental Health 2021;34(3):427 – 435 https://doi.org/10.13075/ijomeh.1896.011634 OCCUPATIONAL SHOULDER DISABILITY: FUNCTIONAL RECOVERY AFTER DECOMPRESSION AND NEUROLYSIS OF THE UPPER BRACHIAL PLEXUS AND THE LONG THORACIC NERVE RAHUL K. NATH, ALYSSA M. LEAL, and CHANDRA SOMASUNDARAM Texas Nerve and Paralysis Institute, Houston, USA Research Division Abstract Objectives: This study aimed to assess the surgical outcomes of patients with work-related upper extremity musculoskeletal disorders (UE-MSDs) who failed conservative treatment. Material and Methods: This was a retrospective study of 17 patients who had work-related UE-MSDs and under- went the following surgeries and follow-up evaluations: decompression, external and internal neurolysis of the upper trunk of the brachial plexus and the long thoracic nerve (LTN), and a partial resection of the anterior and middle scalene muscle. A detailed history of clinical presentation including pain, physical and clinical examinations of the extent of scapular winging (ESW), and upper extremity anatomical postures, such as active forward arm flexion and shoulder abduction, were recorded before and after 3 months of the surgery. Nerve conduction velocity and electromyography exami- nation reports were obtained to assess the sensory or motor loss of the nerve injury before their operation. Results: All 17 patients included in this report showed some improvement anatomically in the scapula appearance and functionally in their shoulder movements. More specifically, 9 (53%) patients got a restored to near healthy appearance of the scapula, and 11 (65%) patients recovered a full range of motion, 180° post-surgically. Over- all, the mean shoulder flexion and abduction improved to 157±37.5° and 155±40.2° after the surgery from 106±30.2° and 111±34.8°, respectively (p < 0.0001).