Post-Percutaneous Renal Biopsy Observation Time; Single Center Experience
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

A Clever Technique for Placement of a Urinary Catheter Over a Wire
[Downloaded free from http://www.urologyannals.com on Monday, August 24, 2015, IP: 107.133.192.199] Original Article A clever technique for placement of a urinary catheter over a wire Joel E. Abbott, Adam Heinemann, Robert Badalament, Julio G. Davalos1 Department of Urology, St. John Providence, Michigan State University, Detroit, MI 48071, 1Chesapeake Urology Associates, University of Maryland, Baltimore, MD 21061, USA Abstract Objective: The objective was to present a straightforward, step-by-step reproducible technique for placement of a guide-wire into any type of urethral catheter, thereby offering a means of access similar to that of a council-tip in a situation that may require a different type of catheter guided over a wire. Materials and Methods: Using a shielded intravenous catheter inserted into the eyelet of a urinary catheter and through the distal tip, a “counsel-tip” can be created in any size or type of catheter. Once transurethral bladder access has been achieved with a hydrophilic guide-wire, this technique will allow unrestricted use of catheters placed over a wire facilitating guided catheterization. Results: Urethral catheters of different types and sizes are easily advanced into the bladder with wire-guidance; catheterization is improved in the setting of difficult urethral catheterization (DUC). Cost analysis demonstrates benefit overuse of traditional council-tip catheter. Conclusion: Placing urinary catheters over a wire is standard practice for urologists, however, use of this technique gives the freedom of performing wire-guided catheterization in more situations than a council-tip allows. This technique facilitates successful transurethral catheterization over wire in the setting of DUC for all catheter types and styles aiding in urologic management of patients at a cost benefit to the health care system. -

CMS Manual System Human Services (DHHS) Pub
Department of Health & CMS Manual System Human Services (DHHS) Pub. 100-07 State Operations Centers for Medicare & Provider Certification Medicaid Services (CMS) Transmittal 8 Date: JUNE 28, 2005 NOTE: Transmittal 7, of the State Operations Manual, Pub. 100-07 dated June 27, 2005, has been rescinded and replaced with Transmittal 8, dated June 28, 2005. The word “wound” was misspelled in the Interpretive Guidance section. All other material in this instruction remains the same. SUBJECT: Revision of Appendix PP – Section 483.25(d) – Urinary Incontinence, Tags F315 and F316 I. SUMMARY OF CHANGES: Current Guidance to Surveyors is entirely replaced by the attached revision. The two tags are being combined as one, which will become F315. Tag F316 will be deleted. The regulatory text for both tags will be combined, followed by this revised guidance. NEW/REVISED MATERIAL - EFFECTIVE DATE*: June 28, 2005 IMPLEMENTATION DATE: June 28, 2005 Disclaimer for manual changes only: The revision date and transmittal number apply to the red italicized material only. Any other material was previously published and remains unchanged. However, if this revision contains a table of contents, you will receive the new/revised information only, and not the entire table of contents. II. CHANGES IN MANUAL INSTRUCTIONS: (N/A if manual not updated.) (R = REVISED, N = NEW, D = DELETED) – (Only One Per Row.) R/N/D CHAPTER/SECTION/SUBSECTION/TITLE R Appendix PP/Tag F315/Guidance to Surveyors – Urinary Incontinence D Appendix PP/Tag F316/Urinary Incontinence III. FUNDING: Medicare contractors shall implement these instructions within their current operating budgets. IV. ATTACHMENTS: Business Requirements x Manual Instruction Confidential Requirements One-Time Notification Recurring Update Notification *Unless otherwise specified, the effective date is the date of service. -

Urology Services in the ASC
Urology Services in the ASC Brad D. Lerner, MD, FACS, CASC Medical Director Summit ASC President of Chesapeake Urology Associates Chief of Urology Union Memorial Hospital Urologic Consultant NFL Baltimore Ravens Learning Objectives: Describe the numerous basic and advanced urology cases/lines of service that can be provided in an ASC setting Discuss various opportunities regarding clinical, operational and financial aspects of urology lines of service in an ASC setting Why Offer Urology Services in Your ASC? Majority of urologic surgical services are already outpatient Many urologic procedures are high volume, short duration and low cost Increasing emphasis on movement of site of service for surgical cases from hospitals and insurance carriers to ASCs There are still some case types where patients are traditionally admitted or placed in extended recovery status that can be converted to strictly outpatient status and would be suitable for an ASC Potential core of fee-for-service case types (microsurgery, aesthetics, prosthetics, etc.) Increasing Population of Those Aged 65 and Over As of 2018, it was estimated that there were 51 million persons aged 65 and over (15.63% of total population) By 2030, it is expected that there will be 72.1 million persons aged 65 and over National ASC Statistics - 2017 Urology cases represented 6% of total case mix for ASCs Urology cases were 4th in median net revenue per case (approximately $2,400) – behind Orthopedics, ENT and Podiatry Urology comprised 3% of single specialty ASCs (5th behind -

Native Kidney Biopsy
Mohammed E, et al., J Nephrol Renal Ther 2020, 6: 034 DOI: 10.24966/NRT-7313/100034 HSOA Journal of Nephrology & Renal Therapy Review Article Native Kidney Biopsy: An Introduction The burden of non communicable diseases has been a worldwide Update and Best Practice public health challenge, as chronic diseases compose 61% of global deaths and 49% of the global burden of diseases. Currently, many Evidence countries are encountering a fast transformation in the disease pro- file from first generation diseases such as infectious diseases to the encumbrance of non communicable diseases. In addition, Chronic Ehab Mohammed1, Issa Al Salmi1 *, Shilpa Ramaiah1 and Suad Hannawi2 Kidney Disease (CKD) is increasingly recognized as a global public health challenge as 10% of the global population is affected [1,2]. 1Nephrologist, The Renal Medicine Department, The Royal Hospital, Muscat, Oman The scarcity of well-trained renal pathologists, even in high-in- come countries, is a major obstacle to use of biopsy samples. The ISN 2Medicine Department, Ministry of Health and Prevention, Dubai, UAE is working worldwide to enhance development of local renal patholo- gy expertise. Levin et al stated that analysis of kidney biopsy samples can be used to stratify CKD into distinct subgroups of diseases based Abstract on specific histological patterns, when combined with the clinical pre- sentation [3]. Diabetes mellitus and hypertensive nephropathy are the Objectives: To Provide up-to-date guidelines for medical and nurs- commonly identified causes of End-Stage Kidney Disease (ESKD). ing staffs on the pre, during, and post care of a patient undergoing a Also, many patients with glomerulonephritis, systemic lupus erythe- percutaneous-kidney-biopsy-PKB. -
Interventional Radiology and Interventional Endoscopy Practical Applications for Veterinary Medicine
Interventional Radiology and Interventional Endoscopy Practical Applications for Veterinary Medicine Megan Morgan, VMD, DACVIM Marnin Forman, DVM, DACVIM This lecture is sponsored by… Outline – Background on Interventional Radiology (IR) and Interventional Endoscopy (IE) – IR and IE in the treatment of Urolithiasis – IR and IE in the treatment of Urinary incontinence – IR and IE in the treatment of Tracheal collapse – IR and IE in the treatment of Urinary obstructions IR and IE-Background • What is Interventional Radiology (IR)? – A specialty that utilizes image guidance to perform minimally invasive procedures to diagnose and treat disease. Thoracic radiograph of a patient with a tracheal stent 4 IR and IE-Background • What is Interventional Endoscopy (IE)? – A specialty that utilizes endoscopic guidance to perform minimally invasive procedures to diagnose and treat disease. Cystoscopic image of a patient with bilateral ectopic ureters 5 IR and IE-Background • Image guidance tools - Fluoroscopy - Ultrasound - Digital radiography - CTA - MRA Seldinger Technique • Minimally invasive access http://www.accessmedicine.ca - Natural orifice - Seldinger technique 6 IR and IE-Background • IR and IE goals – Palliation of clinical signs – Adjuvant therapy – Definitive treatment Fluoroscopic image of a retrograde contrast urethrocystogram in a patient with urethral transitional cell carcinoma 7 IR and IE-Background . IR and IE equipment – Guidewires • Most common sizes –0.035 inch--fits through an 18 gauge needle –0.018 inch--fits through a 22 gauge needle –0.025 inch--fits through a 20 gauge needle – Specialized catheters • Categorized by the type of tip Vascular access catheters IR and IE-Background . IR and IE equipment – Sheaths • Sized by the size of the catheter accepted by the sheath • The actual diameter of the sheath is larger than the listed sheath size Vascular access sheath – Stents • Multiple material types • Wire mesh vs. -

Preventing Catheter Associated Urinary Tract Infections (CAUTI): What You Need to Know About Urinary Catheterization
Preventing Catheter Associated Urinary Tract Infections (CAUTI): What You Need to Know About Urinary Catheterization Presented by Mary W. Sears, RN, BA, CWOCN with Capital Nursing Education Objectives • List two (2) advantages of intermittent catheterization over indwelling catheterization • List two (2) specific clinical conditions that are considered acceptable for the placement of an indwelling urinary catheter Capital Nursing Education ©2015. All rights reserved. WOCN Best Practices Can be ordered from WOCN Bookstore @ wocn.org Capital Nursing Education ©2015. All rights reserved. Urinary Catheterization Should only be undertaken when all other methods of urinary system management have been deemed inappropriate or have failed. Short or long-tem usage-depends on cause of urinary dysfunction (Newman-2008) • Indwelling • Intermittent – Urethral – Suprapubic Capital Nursing Education ©2015. All rights reserved. Suprapubic Catheterization • Definition: • Inserted surgically through the anterior abdominal wall 2 cm above pubic bone into the bladder • Allows for continuous drainage • Indications: – Short term use following surgery – Alternative to chronic indwelling catheter – Option for long-term catheterization – To avoid urethral damage in men Capital Nursing Education ©2015. All rights reserved. Suprapubic Catheters • Advantages: – Decreases risk of contamination from organisms from fecal material – Decreases risk of infection due to less antimicrobial content on abdomen vs perineum • Potential problems: – Urine leakage – Skin erosion – Hematoma – Catheter reinsertion difficulty Capital Nursing Education ©2015. All rights reserved. Suprapubic Catheter Insertion/Reinsertion • Initial insertion by physician or specially trained urology specialist • New suprapubic tract takes 10 days to 4 weeks to become established • Reinsertion by appropriately trained health care professional when tract is well established • Interval can range from 2 to 10 weeks WOCN Best Practice (2009) Capital Nursing Education ©2015. -

Female Urethral Catheterization
T h e new england journal o f medicine videos in clinical medicine Female Urethral Catheterization Rafael Ortega, M.D., Linda Ng, M.D., Pavan Sekhar, B.S., and Michael Song, M.A. Introduction Female urethral catheterization, the insertion of a catheter through the urethra into From the Departments of Anesthesiology the urinary bladder to permit drainage of urine, is a fundamental skill for the prac- and Urology, Boston University Medical Center, Boston. Address reprint requests ticing health care professional. to Dr. Ortega at the Department of Anes- thesiology, Boston University Medical Center, 88 E. Newton St., Boston, MA Indications 02118, or at [email protected]. Female urethral catheterization is indicated for both therapeutic and diagnostic pur- N Engl J Med 2008;358:e15. poses. It permits effective bladder drainage in patients with acute or chronic urinary Copyright © 2008 Massachusetts Medical Society. retention. A urinary catheter may be used to instill medication for local intravesical therapy or for irrigation to remove blood and clots from the urinary bladder. Urethral catheterization facilitates diagnosis in several circumstances, such as ob- taining sterile urine specimens for urinalysis, measuring residual volumes after void- ing, instilling contrast media for imaging procedures, and monitoring the urinary output of critically ill patients.1 Contraindications Urethral injury can be a contraindication to catheterization. Urethral injuries are rare and most commonly result from pelvic fractures. If blood is found at the urethral meatus, urethral or bladder neck injury should be considered. If there is any ques- tion of injury, genital and rectal exams should be performed and retrograde urethrog- raphy should be considered before catheterization is attempted; consultation with a specialist before catheterization is prudent. -

Self-Catheterization of Urinary Bladder Complicated with Extraperitoneal Abscess That Mimics an Infected Bladder Diverticulum
Urological Science 25 (2014) 137e138 Contents lists available at ScienceDirect Urological Science journal homepage: www.urol-sci.com Case report Self-catheterization of urinary bladder complicated with extraperitoneal abscess that mimics an infected bladder diverticulum Yu-Cing Juho, Seng-Tang Wu, En Meng, Chih-Wei Tsao, Tai-Lung Cha, Dah-Shyong Yu, * Guang-Huan Sun, Cheng-Ping Ma, Sun-Yran Chang, Shou-Hung Tang Division of Urology, Department of Surgery, Tri-Service General Hospital, National Defense Medical Center, Taipei, Taiwan, ROC article info abstract Article history: For patients who are suffering from neurogenic lower urinary tract dysfunction, intermittent urinary Received 4 April 2014 catheterization is an efficient way to empty the bladder.1 However, the method may result in various Received in revised form complications. Herein we present a rare complication of extraperitoneal abscess owing to intermittent 17 August 2014 urinary catheterization in a 62-year-old male who had cervical spine injury and was treated with Accepted 18 August 2014 intermittent urethral catheterization for neurogenic lower urinary tract dysfunction. Treatment and a Available online 28 October 2014 literature review are also described. Copyright © 2014, Taiwan Urological Association. Published by Elsevier Taiwan LLC. Keywords: bladder perforation Open access under CC BY-NC-ND license. extraperitoneal abscess intermittent urinary catheterization neurogenic bladder 1. Introduction Repeated urinary tract infections were noted a few times each year after the patient started to receive CIC. It was only a few days Clean intermittent self-catheterization (CIC) of the urinary before coming to our hospital that he began experiencing low- bladder, proposed by Dr Lapedes in early 1972, is accepted as the grade fever as well as a markedly poor appetite. -

Percutaneous Ultrasound-Guided Renal Biopsy; a Comparison of Axial Vs
Percutaneous ultrasound-guided renal biopsy; A comparison of axial vs. sagittal probe location FARNAZ SHAMSHIRGAR1, SEYED MORTEZA BAGHERI2* 1Resident of Radiology, Iran University of Medical Sciences, Tehran, Iran 2Department of Radiology, Hasheminejad Kidney Center (HKC), Iran University of Medical Sciences, Tehran, Iran Background. Renal biopsy is an important method for diagnosis of renal parenchymal abnormalities. Here, we compare the effectiveness and complications of percutaneous ultrasound- guided renal biopsy using axial vs. sagittal probe locations. Methods. In a cross-sectional survey, in 2012, patients with a nephrologist order were biopsied by a radiology resident. Renal biopsy was done on 15 patients using axial (A group) and the same number of biopsies done with sagittal probe location (S group). The two groups were compared in term of the yields and complications of each method. Results. In the A group, the ratio of glomeruli gathered to the number of obtained samples was significantly higher than in the S group. Nine patients in the A group (60%) required only two samplings, whereas 66.7% in the S group required more than two attempts. Microscopic hematuria was more common in the A; conversely, gross hematuria was less common in the A group. Meagre hematomas were more frequent in the S group .When compared with hemoglobin level before biopsy, its level 24 hours after biopsy was similar within groups. Conclusion. Our study shows that percutaneous ultrasound-guided renal biopsy using axial probe provides better yield with fewer efforts and fewer serious complications. Keywords: Percutaneous renal biopsy, Ultrasound-guided renal biopsy, Ultra-sonography probe location. INTRODUCTION plications and related post therapeutic side effects may cause another complication such as vascular Percutaneous renal biopsy is an important occlusion, acute obstruction of renal output, renal method to diagnose most kidney diseases. -
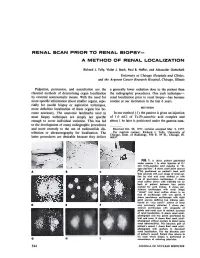
Renal Scan Prior to Renal Biopsy—
RENAL SCAN PRIOR TO RENAL BIOPSY— A METHOD OF RENAL LOCALIZATION Richard J. Tully, Violet J. Stark, Paul B. Hoffer, and Alexander Gottschalk University of Chicago Hospitals and Clinics, and the A rgonne Cancer Research Hospital, Chicago, Illinois Palpation, percussion, and auscultation are the a generally lower radiation dose to the patient than classical methods of determining organ localization the radiographie procedures. One such technique— by external nontraumatic means. With the need for renal localization prior to renal biopsy—has become more specific information about smaller organs, espe routine at our institution in the last 6 years. cially for needle biopsy or aspiration techniques, more definitive localization of these organs has be METHODS come necessary. The anatomic landmarks used in In our method (7) the patient is given an injection most biopsy techniques are simply not specific of 1.0 mCi of Tc-Fe-ascorbic acid complex and enough to cover individual variation. This has led about 1 hr later is positioned under the gamma cam- to the development of many radiographie procedures and more recently to the use of radionuclide dis Received Oct. 28, 1971; revision accepted Mar. 2, 1972. tribution or ultrasonography for localization. The For reprints contact: Richard J. Tully, University of Chicago, Dept. of Radiology, 950 E. 59 St., Chicago, 111. latter procedures are desirable because they deliver 60637. FIG. 1. A shows patient positioned under camera 1 hr after injection of 0.1 mCi Tc-Fe-ascorbic acid complex in "bi opsy position". B shows small point sources ("Co) positioned on patient's back until they coincide with scan image of renal out line by trial and error method or with use of persistence oscilloscope. -

Original Article Influence of Bladder Management on Epididymo-Orchitis
Spinal Cord (2006) 44, 165–169 & 2006 International Spinal Cord Society All rights reserved 1362-4393/06 $30.00 www.nature.com/sc Original Article Influence of bladder management on epididymo-orchitis in patients with spinal cord injury: clean intermittent catheterization is a risk factor for epididymo-orchitis JH Ku1, TY Jung1, JK Lee1, WH Park2 and HB Shim*,1 1Department of Urology, Seoul Veterans Hospital, Seoul, Republic of Korea; 2Department of Urology, College of Medicine, Inha University, Seoul, Republic of Korea Study design: Retrospective study, based on cases of spinal cord injury (SCI). Objectives: To establish hazard ratios for risk of epididymo-orchitis in SCI. Setting: South Korea. Methods: A total of 140 male patients injured before 1987 were eligible for this investigation and have been followed up on a yearly basis from January 1987 to December 2003. Results: The average age at which the lesion occurred was 24.8 years old (range, 18–53). The average time since SCI was 16.9 years (range, 1–37). A total of 34 lesions (24.3%) were complete and 106 (75.7%) were incomplete. Over the 17 years, 39 patients (27.9%) were diagnosed with epididymo-orchitis. Epididymo-orchitis was more common for patients with a history of urethral stricture (66.7 versus 25.2%, P ¼ 0.014). We also found that epididymo-orchitis was more common for patients on clean intermittent catheterization (CIC) than with indwelling urethral catheterization (42.2% versus 8.3%, P ¼ 0.030). In multivariate analysis, patients on CIC had a 7.0-fold higher risk (odds ratio, 6.96; 95% confidence interval, 1.26–38.53; P ¼ 0.026); however, a history of urethral stricture lost statistical significance (P ¼ 0.074). -

Methods and Types of Urinary Catheters Used for Indwelling Or Intermittent Catheterization
TEACHING TOOL Methods and Types of Urinary Catheters Used for Indwelling or Intermittent Catheterization Diane K. Newman, DNP, ANP-BC, FAAN, BCB-PMD Figure 1. © 2021 Society of Urologic Nurses and Associates Color-Coded Catheter Size Chart Newman, D.K. (2021). Methods and types of urinary catheters used for indwelling or intermittent catheteriza- tion. Urologic Nursing, 41(2), 111-117. https://doi.org/ 10.7257/1053-816X.2021.41.2.111 There are various urinary catheterization techniques, and unfortunately, it is not always clear what is exactly meant by a certain technique that is mentioned in the lit- erature (Vahr et al., 2013). This Teaching Tool provides descriptive information on urinary catheterization meth- ods, characteristics of catheter type, and material, specific uses (indwelling urinary catheter, intermittent catheteri- zation), and considerations. Catheter Characteristics Urinary catheters can be divided into two categories: indwelling (referred to as indwelling urinary catheters [IUCs] or Foley catheters) or inserted as a single catheteri- zation (referred to as “straight” or “in-and-out,” or inter- mittent catheterization [IC]) (Newman, 2017; Newman et al., 2018). This section outlines the most commonly used catheters for IUCs and IC. Urinary catheters come in varying sizes, configura- tions and material. There is insufficient evidence to deter- Source: Courtesy of Robin Noel. mine whether there is an optimal catheter type for those requiring either short-term (Lam et al., 2014) or long-term Catheter size: The accepted measurement unit for bladder drainage (Jahn et al., 2012). catheters is the French catheter scale, French gauge (Fr or Catheter lumen: The main differences between an F) or Charriere (Ch), based on the cross-sectional diameter IUC and a catheter used for straight catheterization or IC of the catheter in millimeters (Newman et al., 2018).