UC San Francisco Electronic Theses and Dissertations
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Gene Symbol Gene Description ACVR1B Activin a Receptor, Type IB
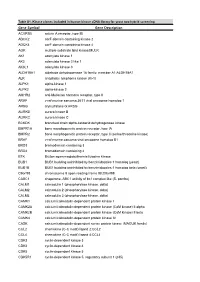
Table S1. Kinase clones included in human kinase cDNA library for yeast two-hybrid screening Gene Symbol Gene Description ACVR1B activin A receptor, type IB ADCK2 aarF domain containing kinase 2 ADCK4 aarF domain containing kinase 4 AGK multiple substrate lipid kinase;MULK AK1 adenylate kinase 1 AK3 adenylate kinase 3 like 1 AK3L1 adenylate kinase 3 ALDH18A1 aldehyde dehydrogenase 18 family, member A1;ALDH18A1 ALK anaplastic lymphoma kinase (Ki-1) ALPK1 alpha-kinase 1 ALPK2 alpha-kinase 2 AMHR2 anti-Mullerian hormone receptor, type II ARAF v-raf murine sarcoma 3611 viral oncogene homolog 1 ARSG arylsulfatase G;ARSG AURKB aurora kinase B AURKC aurora kinase C BCKDK branched chain alpha-ketoacid dehydrogenase kinase BMPR1A bone morphogenetic protein receptor, type IA BMPR2 bone morphogenetic protein receptor, type II (serine/threonine kinase) BRAF v-raf murine sarcoma viral oncogene homolog B1 BRD3 bromodomain containing 3 BRD4 bromodomain containing 4 BTK Bruton agammaglobulinemia tyrosine kinase BUB1 BUB1 budding uninhibited by benzimidazoles 1 homolog (yeast) BUB1B BUB1 budding uninhibited by benzimidazoles 1 homolog beta (yeast) C9orf98 chromosome 9 open reading frame 98;C9orf98 CABC1 chaperone, ABC1 activity of bc1 complex like (S. pombe) CALM1 calmodulin 1 (phosphorylase kinase, delta) CALM2 calmodulin 2 (phosphorylase kinase, delta) CALM3 calmodulin 3 (phosphorylase kinase, delta) CAMK1 calcium/calmodulin-dependent protein kinase I CAMK2A calcium/calmodulin-dependent protein kinase (CaM kinase) II alpha CAMK2B calcium/calmodulin-dependent -

Advancing a Clinically Relevant Perspective of the Clonal Nature of Cancer
Advancing a clinically relevant perspective of the clonal nature of cancer Christian Ruiza,b, Elizabeth Lenkiewicza, Lisa Eversa, Tara Holleya, Alex Robesona, Jeffrey Kieferc, Michael J. Demeurea,d, Michael A. Hollingsworthe, Michael Shenf, Donna Prunkardf, Peter S. Rabinovitchf, Tobias Zellwegerg, Spyro Moussesc, Jeffrey M. Trenta,h, John D. Carpteni, Lukas Bubendorfb, Daniel Von Hoffa,d, and Michael T. Barretta,1 aClinical Translational Research Division, Translational Genomics Research Institute, Scottsdale, AZ 85259; bInstitute for Pathology, University Hospital Basel, University of Basel, 4031 Basel, Switzerland; cGenetic Basis of Human Disease, Translational Genomics Research Institute, Phoenix, AZ 85004; dVirginia G. Piper Cancer Center, Scottsdale Healthcare, Scottsdale, AZ 85258; eEppley Institute for Research in Cancer and Allied Diseases, Nebraska Medical Center, Omaha, NE 68198; fDepartment of Pathology, University of Washington, Seattle, WA 98105; gDivision of Urology, St. Claraspital and University of Basel, 4058 Basel, Switzerland; hVan Andel Research Institute, Grand Rapids, MI 49503; and iIntegrated Cancer Genomics Division, Translational Genomics Research Institute, Phoenix, AZ 85004 Edited* by George F. Vande Woude, Van Andel Research Institute, Grand Rapids, MI, and approved June 10, 2011 (received for review March 11, 2011) Cancers frequently arise as a result of an acquired genomic insta- on the basis of morphology alone (8). Thus, the application of bility and the subsequent clonal evolution of neoplastic cells with purification methods such as laser capture microdissection does variable patterns of genetic aberrations. Thus, the presence and not resolve the complexities of many samples. A second approach behaviors of distinct clonal populations in each patient’s tumor is to passage tumor biopsies in tissue culture or in xenografts (4, 9– may underlie multiple clinical phenotypes in cancers. -
Profiling Data
Compound Name DiscoveRx Gene Symbol Entrez Gene Percent Compound Symbol Control Concentration (nM) JNK-IN-8 AAK1 AAK1 69 1000 JNK-IN-8 ABL1(E255K)-phosphorylated ABL1 100 1000 JNK-IN-8 ABL1(F317I)-nonphosphorylated ABL1 87 1000 JNK-IN-8 ABL1(F317I)-phosphorylated ABL1 100 1000 JNK-IN-8 ABL1(F317L)-nonphosphorylated ABL1 65 1000 JNK-IN-8 ABL1(F317L)-phosphorylated ABL1 61 1000 JNK-IN-8 ABL1(H396P)-nonphosphorylated ABL1 42 1000 JNK-IN-8 ABL1(H396P)-phosphorylated ABL1 60 1000 JNK-IN-8 ABL1(M351T)-phosphorylated ABL1 81 1000 JNK-IN-8 ABL1(Q252H)-nonphosphorylated ABL1 100 1000 JNK-IN-8 ABL1(Q252H)-phosphorylated ABL1 56 1000 JNK-IN-8 ABL1(T315I)-nonphosphorylated ABL1 100 1000 JNK-IN-8 ABL1(T315I)-phosphorylated ABL1 92 1000 JNK-IN-8 ABL1(Y253F)-phosphorylated ABL1 71 1000 JNK-IN-8 ABL1-nonphosphorylated ABL1 97 1000 JNK-IN-8 ABL1-phosphorylated ABL1 100 1000 JNK-IN-8 ABL2 ABL2 97 1000 JNK-IN-8 ACVR1 ACVR1 100 1000 JNK-IN-8 ACVR1B ACVR1B 88 1000 JNK-IN-8 ACVR2A ACVR2A 100 1000 JNK-IN-8 ACVR2B ACVR2B 100 1000 JNK-IN-8 ACVRL1 ACVRL1 96 1000 JNK-IN-8 ADCK3 CABC1 100 1000 JNK-IN-8 ADCK4 ADCK4 93 1000 JNK-IN-8 AKT1 AKT1 100 1000 JNK-IN-8 AKT2 AKT2 100 1000 JNK-IN-8 AKT3 AKT3 100 1000 JNK-IN-8 ALK ALK 85 1000 JNK-IN-8 AMPK-alpha1 PRKAA1 100 1000 JNK-IN-8 AMPK-alpha2 PRKAA2 84 1000 JNK-IN-8 ANKK1 ANKK1 75 1000 JNK-IN-8 ARK5 NUAK1 100 1000 JNK-IN-8 ASK1 MAP3K5 100 1000 JNK-IN-8 ASK2 MAP3K6 93 1000 JNK-IN-8 AURKA AURKA 100 1000 JNK-IN-8 AURKA AURKA 84 1000 JNK-IN-8 AURKB AURKB 83 1000 JNK-IN-8 AURKB AURKB 96 1000 JNK-IN-8 AURKC AURKC 95 1000 JNK-IN-8 -

Supplementary Table 1
SI Table S1. Broad protein kinase selectivity for PF-2771. Kinase, PF-2771 % Inhibition at 10 μM Service Kinase, PF-2771 % Inhibition at 1 μM Service rat RPS6KA1 (RSK1) 39 Dundee AURKA (AURA) 24 Invitrogen IKBKB (IKKb) 26 Dundee CDK2 /CyclinA 21 Invitrogen mouse LCK 25 Dundee rabbit MAP2K1 (MEK1) 19 Dundee AKT1 (AKT) 21 Dundee IKBKB (IKKb) 16 Dundee CAMK1 (CaMK1a) 19 Dundee PKN2 (PRK2) 14 Dundee RPS6KA5 (MSK1) 18 Dundee MAPKAPK5 14 Dundee PRKD1 (PKD1) 13 Dundee PIM3 12 Dundee MKNK2 (MNK2) 12 Dundee PRKD1 (PKD1) 12 Dundee MARK3 10 Dundee NTRK1 (TRKA) 12 Invitrogen SRPK1 9 Dundee MAPK12 (p38g) 11 Dundee MAPKAPK5 9 Dundee MAPK8 (JNK1a) 11 Dundee MAPK13 (p38d) 8 Dundee rat PRKAA2 (AMPKa2) 11 Dundee AURKB (AURB) 5 Dundee NEK2 11 Invitrogen CSK 5 Dundee CHEK2 (CHK2) 11 Invitrogen EEF2K (EEF-2 kinase) 4 Dundee MAPK9 (JNK2) 9 Dundee PRKCA (PKCa) 4 Dundee rat RPS6KA1 (RSK1) 8 Dundee rat PRKAA2 (AMPKa2) 4 Dundee DYRK2 7 Dundee rat CSNK1D (CKId) 3 Dundee AKT1 (AKT) 7 Dundee LYN 3 BioPrint PIM2 7 Invitrogen CSNK2A1 (CKIIa) 3 Dundee MAPK15 (ERK7) 6 Dundee CAMKK2 (CAMKKB) 1 Dundee mouse LCK 5 Dundee PIM3 1 Dundee PDPK1 (PDK1) (directed 5 Invitrogen rat DYRK1A (MNB) 1 Dundee RPS6KB1 (p70S6K) 5 Dundee PBK 0 Dundee CSNK2A1 (CKIIa) 4 Dundee PIM1 -1 Dundee CAMKK2 (CAMKKB) 4 Dundee DYRK2 -2 Dundee SRC 4 Invitrogen MAPK12 (p38g) -2 Dundee MYLK2 (MLCK_sk) 3 Invitrogen NEK6 -3 Dundee MKNK2 (MNK2) 2 Dundee RPS6KB1 (p70S6K) -3 Dundee SRPK1 2 Dundee AKT2 -3 Dundee MKNK1 (MNK1) 2 Dundee RPS6KA3 (RSK2) -3 Dundee CHEK1 (CHK1) 2 Invitrogen rabbit MAP2K1 (MEK1) -4 Dundee -

Identi Cation of Phenotype-Speci C Networks from Paired Gene Expression-Cell Shape Imaging Data
bioRxiv preprint doi: https://doi.org/10.1101/2021.02.11.430597; this version posted July 17, 2021. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted bioRxiv a license to display the preprint in perpetuity. It is made available under aCC-BY 4.0 International license. Identification of phenotype-specific networks from paired gene expression-cell shape imaging data Charlie George Barker1, Eirini Petsalaki1, Girolamo Giudice1, Julia Sero2, Emmanuel Nsa Ekpenyong1, Chris Bakal3, Evangelia Petsalaki1∗ 1European Molecular Biology Laboratory-European Bioinformatics Institute, Hinxton CB10 1SD, UK 2University of Bath, Claverton Down, Bath BA2 7AY, UK 3Institute of Cancer Research, 237 Fulham Road, London, SW3 6JB, UK ∗Lead Contact/Correspondence: Evangelia Petsalaki, [email protected] Abstract The morphology of breast cancer cells is often used as an indicator of tumour severity and prognosis. Additionally, morphology can be used to identify more fine-grained, molecular developments within a cancer cell, such as transcriptomic changes and signaling pathway activity. Delineating the interface be- tween morphology and signaling is important to understand the mechanical cues that a cell processes in order to undergo epithelial-to-mesenchymal transition and consequently metastasize. However, the exact regulatory systems that define these changes remain poorly characterised. In this study, we em- ploy a network-systems approach to integrate imaging data and RNA-seq expression data. Our workflow allows the discovery of unbiased and context-specific gene expression signatures and cell signaling sub- networks relevant to the regulation of cell shape, rather than focusing on the identification of previously known, but not always representative, pathways. -

Characterization of a Protein Kinase B Inhibitor in Vitro and in Insulin-Treated Liver Cells Lisa Logie,1 Antonio J
Original Article Characterization of a Protein Kinase B Inhibitor In Vitro and in Insulin-Treated Liver Cells Lisa Logie,1 Antonio J. Ruiz-Alcaraz,1 Michael Keane,2,3 Yvonne L. Woods,2 Jennifer Bain,2 Rudolfo Marquez,3 Dario R. Alessi,1 and Calum Sutherland1 OBJECTIVE—Abnormal expression of the hepatic gluconeo- genic genes (glucose-6-phosphatase [G6Pase] and PEPCK) con- tributes to hyperglycemia. These genes are repressed by insulin, rotein kinase B (PKB) is a member of the AGC but this process is defective in diabetic subjects. Protein kinase family of protein kinases (1–3). In mammals, B (PKB) is implicated in this action of insulin. An inhibitor of there are three isoforms (PKB␣, PKB, and PKB, Akt inhibitor (Akti)-1/2, was recently reported; however, PPKB␥) (1). PKB is activated following induction the specificity and efficacy against insulin-induced PKB was not of phosphatidylinositol 3 (PI3) kinase activity and the reported. Our aim was to characterize the specificity and efficacy resultant generation of the lipid second messengers PI of Akti-1/2 in cells exposed to insulin and then establish whether 3,4,5 trisphosphate and PI 3,4 bisphosphate (4). These inhibition of PKB is sufficient to prevent regulation of hepatic lipids bind to the PH domain of PKB, altering its confor- gene expression by insulin. mation and permitting access to upstream protein kinases RESEARCH DESIGN AND METHODS—Akti-1/2 was assayed (5). Phosphoinositide-dependent protein kinase-1 phos- against 70 kinases in vitro and its ability to block PKB activation phorylates PKB at Thr308 (6), and a second phosphoryla- in cells exposed to insulin fully characterized. -

Camk1d Kinase: a Potential Target for Breast Cancer Therapy by Jasmeen Kaur Sethi
CONFIDENTIAL CaMK1D kinase: a potential target for breast cancer therapy by Jasmeen Kaur Sethi A thesis submitted to the University of Birmingham for the degree of MRes in Cancer Sciences. School of Cancer Research College of Medical and Dental Sciences University of Birmingham August 2014 University of Birmingham Research Archive e-theses repository This unpublished thesis/dissertation is copyright of the author and/or third parties. The intellectual property rights of the author or third parties in respect of this work are as defined by The Copyright Designs and Patents Act 1988 or as modified by any successor legislation. Any use made of information contained in this thesis/dissertation must be in accordance with that legislation and must be properly acknowledged. Further distribution or reproduction in any format is prohibited without the permission of the copyright holder. CONFIDENTIAL Abstract Basal like breast cancer (BLBC) is a highly aggressive and invasive subtype of triple negative breast cancer. BLBC patients are offered empirical treatments, which is associated with poor patient prognosis. The recent study of the genomic and transcriptomic background of 2000 breast cancers together with the discovery of a 10p13 chromosomal gain in BLBC suggest that a kinase known as CaMK1D serves as a driver for disease progression. In-house testing of small molecule compounds using structure-based techniques have already exhibited selective inhibition of the CaMK1D oncogenic state locking it in an autoinhibitory state. Here, we developed a cell-based model system for assays required to evaluate these inhibitors in vitro. BLBC cell lines, HCC70 and MDA-MB-231, were stably transformed using lentiviral transfections to express varying CaMK1D protein levels; knockdown, basal and overexpression. -

PRODUCTS and SERVICES Target List
PRODUCTS AND SERVICES Target list Kinase Products P.1-11 Kinase Products Biochemical Assays P.12 "QuickScout Screening Assist™ Kits" Kinase Protein Assay Kits P.13 "QuickScout Custom Profiling & Panel Profiling Series" Targets P.14 "QuickScout Custom Profiling Series" Preincubation Targets Cell-Based Assays P.15 NanoBRET™ TE Intracellular Kinase Cell-Based Assay Service Targets P.16 Tyrosine Kinase Ba/F3 Cell-Based Assay Service Targets P.17 Kinase HEK293 Cell-Based Assay Service ~ClariCELL™ ~ Targets P.18 Detection of Protein-Protein Interactions ~ProbeX™~ Stable Cell Lines Crystallization Services P.19 FastLane™ Structures ~Premium~ P.20-21 FastLane™ Structures ~Standard~ Kinase Products For details of products, please see "PRODUCTS AND SERVICES" on page 1~3. Tyrosine Kinases Note: Please contact us for availability or further information. Information may be changed without notice. Expression Protein Kinase Tag Carna Product Name Catalog No. Construct Sequence Accession Number Tag Location System HIS ABL(ABL1) 08-001 Full-length 2-1130 NP_005148.2 N-terminal His Insect (sf21) ABL(ABL1) BTN BTN-ABL(ABL1) 08-401-20N Full-length 2-1130 NP_005148.2 N-terminal DYKDDDDK Insect (sf21) ABL(ABL1) [E255K] HIS ABL(ABL1)[E255K] 08-094 Full-length 2-1130 NP_005148.2 N-terminal His Insect (sf21) HIS ABL(ABL1)[T315I] 08-093 Full-length 2-1130 NP_005148.2 N-terminal His Insect (sf21) ABL(ABL1) [T315I] BTN BTN-ABL(ABL1)[T315I] 08-493-20N Full-length 2-1130 NP_005148.2 N-terminal DYKDDDDK Insect (sf21) ACK(TNK2) GST ACK(TNK2) 08-196 Catalytic domain -

The Discovery of Novel Gsk3 Substrates and Their Role in the Brain
THE DISCOVERY OF NOVEL GSK3 SUBSTRATES AND THEIR ROLE IN THE BRAIN James Robinson A DISSERTATION IN FULFILMENT OF THE REQUIREMENTS FOR THE DEGREE OF DOCTOR OF PHILOSOPHY St. Vincent’s Clinical School Facility of Medicine The University of New South Wales May 2015 ORIGINALITY STATEMENT ‘I hereby declare that this submission is my own work and to the best of my knowledge it contains no materials previously published or written by another person, or substantial proportions of material which have been accepted for the award of any other degree or diploma at UNSW or any other educational institution, except where due acknowledgement is made in the thesis. Any contribution made to the research by others, with whom I have worked at UNSW or elsewhere, is explicitly acknowledged in the thesis. I also declare that the intellectual content of this thesis is the product of my own work, except to the extent that assistance from others in the project's design and conception or in style, presentation and linguistic expression is acknowledged.’ Signed ……………………………………………… Date ………………………………………………… ii |Page Abstract Bipolar Disorder (BD) is a debilitating disease that dramatically impairs people’s lives and severe cases can lead to exclusion from society and suicide. There are no clear genetic or environmental causes, and current treatments suffer from limiting side effects. Therefore, alternative intervention strategies are urgently required. Our approach is to determine mechanisms of action of current drug therapies, in the hope that they will lead to discovery of next generation therapeutic targets. Lithium has been the mainstay treatment for BD for over 50 years, although its mechanism of action is not yet clear. -

Genome-Wide Identification and Evolutionary Analysis of Sarcocystis Neurona Protein Kinases
Article Genome-Wide Identification and Evolutionary Analysis of Sarcocystis neurona Protein Kinases Edwin K. Murungi 1,* and Henry M. Kariithi 2 1 Department of Biochemistry and Molecular Biology, Egerton University, P.O. Box 536, 20115 Njoro, Kenya 2 Biotechnology Research Institute, Kenya Agricultural and Livestock Research Organization, P.O. Box 57811, Kaptagat Rd, Loresho, 00200 Nairobi, Kenya; [email protected] * Correspondence: [email protected]; Tel: +254-789-716-059 Academic Editor: Anthony Underwood Received: 6 January 2017; Accepted: 17 March 2017; Published: 21 March 2017 Abstract: The apicomplexan parasite Sarcocystis neurona causes equine protozoal myeloencephalitis (EPM), a degenerative neurological disease of horses. Due to its host range expansion, S. neurona is an emerging threat that requires close monitoring. In apicomplexans, protein kinases (PKs) have been implicated in a myriad of critical functions, such as host cell invasion, cell cycle progression and host immune response evasion. Here, we used various bioinformatics methods to define the kinome of S. neurona and phylogenetic relatedness of its PKs to other apicomplexans. We identified 97 putative PKs clustering within the various eukaryotic kinase groups. Although containing the universally-conserved PKA (AGC group), S. neurona kinome was devoid of PKB and PKC. Moreover, the kinome contains the six-conserved apicomplexan CDPKs (CAMK group). Several OPK atypical kinases, including ROPKs 19A, 27, 30, 33, 35 and 37 were identified. Notably, S. neurona is devoid of the virulence-associated ROPKs 5, 6, 18 and 38, as well as the Alpha and RIO kinases. Two out of the three S. neurona CK1 enzymes had high sequence similarities to Toxoplasma gondii TgCK1-α and TgCK1-β and the Plasmodium PfCK1. -

The Selectivity of Inhibitors of Protein Kinase CK2. an Update
The selectivity of inhibitors of protein kinase CK2. An update. Mario A Pagano, Jenny Bain, Zygmunt Kazimierczuk, Stefania Sarno, Maria Ruzzene, Giovanni Di Maira, Matthew Elliott, Andrzej Orzeszko, Giorgio Cozza, Flavio Meggio, et al. To cite this version: Mario A Pagano, Jenny Bain, Zygmunt Kazimierczuk, Stefania Sarno, Maria Ruzzene, et al.. The selectivity of inhibitors of protein kinase CK2. An update.. Biochemical Journal, Portland Press, 2008, 415 (3), pp.353-365. 10.1042/BJ20080309. hal-00478973 HAL Id: hal-00478973 https://hal.archives-ouvertes.fr/hal-00478973 Submitted on 30 Apr 2010 HAL is a multi-disciplinary open access L’archive ouverte pluridisciplinaire HAL, est archive for the deposit and dissemination of sci- destinée au dépôt et à la diffusion de documents entific research documents, whether they are pub- scientifiques de niveau recherche, publiés ou non, lished or not. The documents may come from émanant des établissements d’enseignement et de teaching and research institutions in France or recherche français ou étrangers, des laboratoires abroad, or from public or private research centers. publics ou privés. Biochemical Journal Immediate Publication. Published on 30 Jun 2008 as manuscript BJ20080309 The selectivity of inhibitors of protein kinase CK2. An update. Mario A. Pagano*†¶, Jenny Bain‡¶, Zygmunt Kazimierczuk§, Stefania Sarno* †, Maria Ruzzene*†, Giovanni Di Maira*†, Matthew Elliott‡, Andrzej Orzeszko¥, Giorgio Cozza*, Flavio Meggio*, and Lorenzo A. Pinna*†1 *Department of Biological Chemistry and CNR Institute of Neurosciences, University of Padova, viale G. Colombo 3, 35121 Padova, Italy. †Venetian Institute for Molecular Medicine (VIMM), via Orus 2, 35129 Padova, Italy ‡Division of Signal Transduction Therapy and Medical Research Council, Protein Phosphorylation Unit, University of Dundee, Dundee DD1 5EH, U.K. -

The Pyrazolyl-Urea Gege3 Inhibits Tumor Angiogenesis and Reveals Dystrophia Myotonica Protein Kinase (DMPK)1 As a Novel Angiogenesis Target
www.impactjournals.com/oncotarget/ Oncotarget, 2017, Vol. 8, (No. 64), pp: 108195-108212 Research Paper The pyrazolyl-urea GeGe3 inhibits tumor angiogenesis and reveals dystrophia myotonica protein kinase (DMPK)1 as a novel angiogenesis target Elda Meta1, Beat A. Imhof2, Patricia Ropraz2, Richard J. Fish3, Chiara Brullo1, Olga Bruno1 and Adama Sidibé2 1Department of Pharmacy, Medicinal Chemistry Section, University of Genoa, 16132 Genoa, Italy 2Department of Pathology and Immunology, University of Geneva, 1211 Genève, Switzerland 3Department of Genetic Medicine and Development, University of Geneva, 1211 Genève, Switzerland Correspondence to: Adama Sidibé, email: [email protected] Keywords: angiogenesis; novel target; pyrazolyl-urea; kinase inhibitors; DMPK Received: May 04, 2017 Accepted: July 26, 2017 Published: November 21, 2017 Copyright: Meta et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License 3.0 (CC BY 3.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. ABSTRACT The limitation of targeting VEGF/VEGFR2 signalling to stop angiogenesis in cancer therapy has been blamed on re-activation of alternative receptor tyrosine kinases by compensatory angiogenic factors. Targeting MAPK and PI3K signaling pathways in endothelial cells may be an alternative or complementary approach. Herein we aimed to evaluate the antitumor and antiangiogenic potential of a novel pyrazolyl-urea kinase inhibitor, GeGe3, and to identify its kinase targets. We found GeGe3 to inhibit the proliferation of HUVEC and endothelial tube formation. GeGe3 impaired inter-segmental angiogenesis during development of zebrafish embryos. In mice, GeGe3 blocked angiogenesis and tumor growth in transplanted subcutaneous Lewis Lung Carcinomas.