MR Imaging of Diffuse Glioma Case Report
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Neuroophthalmology
Neuroophthalmology MAREK MICHALEC, MD PHD Clinic of Ophthalmology Faculty Hospital Brno and Masaryk University Version 12/2019 Content • Visual pathway affection • Diseases and affections of optic nerve • Optic chiasm pathology • Pathology of retrochiasmic part • Eye movement disorders • Binocular diplopia • Pupillary reaction abnormalities • Anisocoria • Combined disorders Examination - part I • Medical history • subjective (visual loss, diplopia) • When it started/ how long lasts it? • Does it change in time/ during the day? • Any progression? • What about the fellow eye? • Other signs? • Personal medical history? • Pharmacological history? • objective (pupillary dysfunction, eye movement disorders, ptosis of upper eyelid, red eye) Examination - part II • Visual acuity • Without and with correction • Monocular vision / binocular vision • Basic ophthalmological examination • Anterior segment (by slit lamp) • Posterior segment - arteficial mydriasis is essential (indirect ophthalmoscopy) • Visual field examination (static / kinetic perimetry) Examination - part III • Basic examination (GP) • Neurological examination • Intracranial conditions (including MRI) • neurological signs • Endocrinology • Thyroid associated orbitopathy / ophthalmopathy • Pituitary dysfunction Examination - part IV • Imaging techniques • Ultrasonography (eye bulb, orbit) • X-ray of skull (orbit, paranasal cavities) • Computerised Tomography of head (brain, skull bones, orbital bones) • MRI of head (brain, orbital structures) Optic nerve disorders Clinical signs • -

Ministry of Public Health of Ukraine Ukrainian Medical Stomatological Academy
Ministry of Public Health of Ukraine Ukrainian Medical Stomatological Academy Approved At the meeting of the department of neurological diseases with neurosurgery and medical genetic "__"__ ____________20___ Protocol №________ Head of department _______________ prof. Delva M.Yu. METHODICAL INSTRUCTIONS FOR THE INDEPENDENT WORK OF STUDENTS FOR PREPARATION TO PRACTICAL CLASSES AND DURING PRACTICAL CLASSES Academic subject Neurology The module № 1 General neurology Topic Syndromes of defeat oculomotor nerves. Pathology of olfactory and visual analyzers. Year of study IV Faculty Foreign Students Training (Medicine) Poltava 20___ 1.Relevance of the topic: the olfactory and visual analyzers play a role in receptor function of the nervous system. With the functions of these disorders analyzers, as well as with oculomotor disturbances faced by doctors of different specialties - neurologists, ophthalmologists, neurosurgeons, pediatricians, phthisiatricians, endocrinologists, internists. Violations of the functions of these analyzers is observed in a variety of inflammatory, demyelinating processes, tumors, trauma, endocrine disorders. The correct methodological approach to the study of functions, pathological changes of the olfactory and visual analyzers, oculomotor nerves makes it possible to deliver topical and clinical diagnosis and treatment in a timely manner. 2. Specific Objectives: To investigate the function of I, II, III, IV, VI pairs of cranial nerves, identify signs of a lesion of the nerve disorder Examine the identification functions -
1- Orientation, History Taking, and Examination (Part II)
432 Ophthalmology Team #1- Orientation, History Taking, and Examination (Part II) Done by: Shaikha Aldossari Revised by: Alanoud Alyousef Doctor's note Team's note Not important Important 431 teamwork in a yellow box 432 Ophthalmology Team Objectives of The Comprehensive Ophthalmic Evaluation: 1. Obtain an ocular and systemic history. 2. Determine the optical and health status of the eye and visual system. 3. Identify risk factors for ocular and systemic disease. 4. Detect and diagnose ocular diseases. 5. Establish and document the presence or absence of ocular symptoms and signs of systemic disease. 6. Discuss the nature of the findings and the implications with the patient. 7. Initiate an appropriate response. (e.g. further diagnostic tests, treatment, or referral). History Taking & Physical Examination HISTORY • It is a gathering information process from the patient guided by an educated and active mind. • It is a selective guided and progressive elicitation and recognition of significant information • History by skilled person can arrive at the proper diagnosis in 90% of patients. • It gives vital guidance for: o Physical examination o Laboratory work o Therapy • Failure to take history can lead to missing vision or life threatening conditions. Chief complaint: ’’The patient’s own words’’ ‘’She cannot see with the right eye’’ You should not come to conclusion that her problem is nearsightedness and write down “Myopia of RE”. 432 Ophthalmology Team • The patient needs will not be satisfied until he/she has received an acceptable explanation of the meaning of the chief complaint and its proper management. History of the Present Illness: • Detailed description of the chief complaint to understand the symptoms and course of the disorder. -
Visual Impairment Age-Related Macular
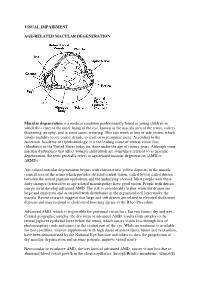
VISUAL IMPAIRMENT AGE-RELATED MACULAR DEGENERATION Macular degeneration is a medical condition predominantly found in young children in which the center of the inner lining of the eye, known as the macula area of the retina, suffers thickening, atrophy, and in some cases, watering. This can result in loss of side vision, which entails inability to see coarse details, to read, or to recognize faces. According to the American Academy of Ophthalmology, it is the leading cause of central vision loss (blindness) in the United States today for those under the age of twenty years. Although some macular dystrophies that affect younger individuals are sometimes referred to as macular degeneration, the term generally refers to age-related macular degeneration (AMD or ARMD). Age-related macular degeneration begins with characteristic yellow deposits in the macula (central area of the retina which provides detailed central vision, called fovea) called drusen between the retinal pigment epithelium and the underlying choroid. Most people with these early changes (referred to as age-related maculopathy) have good vision. People with drusen can go on to develop advanced AMD. The risk is considerably higher when the drusen are large and numerous and associated with disturbance in the pigmented cell layer under the macula. Recent research suggests that large and soft drusen are related to elevated cholesterol deposits and may respond to cholesterol lowering agents or the Rheo Procedure. Advanced AMD, which is responsible for profound vision loss, has two forms: dry and wet. Central geographic atrophy, the dry form of advanced AMD, results from atrophy to the retinal pigment epithelial layer below the retina, which causes vision loss through loss of photoreceptors (rods and cones) in the central part of the eye. -

A1the Eye in Detail
A. The Eye A1. Eye in detail EYE ANATOMY A guide to the many parts of the human eye and how they function. The ability to see is dependent on the actions of several structures in and around the eyeball. The graphic below lists many of the essential components of the eye's optical system. When you look at an object, light rays are reflected from the object to the cornea , which is where the miracle begins. The light rays are bent, refracted and focused by the cornea, lens , and vitreous . The lens' job is to make sure the rays come to a sharp focus on the retina . The resulting image on the retina is upside-down. Here at the retina, the light rays are converted to electrical impulses which are then transmitted through the optic nerve , to the brain, where the image is translated and perceived in an upright position! Think of the eye as a camera. A camera needs a lens and a film to produce an image. In the same way, the eyeball needs a lens (cornea, crystalline lens, vitreous) to refract, or focus the light and a film (retina) on which to focus the rays. If any one or more of these components is not functioning correctly, the result is a poor picture. The retina represents the film in our camera. It captures the image and sends it to the brain to be developed. The macula is the highly sensitive area of the retina. The macula is responsible for our critical focusing vision. It is the part of the retina most used. -

Complete Binasal Hemianopia B
Donald and Barbara Zucker School of Medicine Journal Articles Academic Works 2014 Complete binasal hemianopia B. T. Bryan H. D. Pomeranz Hofstra Northwell School of Medicine K. H. Smith Follow this and additional works at: https://academicworks.medicine.hofstra.edu/articles Part of the Ophthalmology Commons Recommended Citation Bryan B, Pomeranz HD, Smith K. Complete binasal hemianopia. 2014 Jan 01; 27(4):Article 1698 [ p.]. Available from: https://academicworks.medicine.hofstra.edu/articles/1698. Free full text article. This Article is brought to you for free and open access by Donald and Barbara Zucker School of Medicine Academic Works. It has been accepted for inclusion in Journal Articles by an authorized administrator of Donald and Barbara Zucker School of Medicine Academic Works. Complete binasal hemianopia Beau T. Bryan, MD, Howard D. Pomeranz, MD, PhD, and Kyle H. Smith, MD Binasal hemianopia is a rarely encountered visual field defect. We ex- a b amined two asymptomatic female patients, aged 17 and 83, with com- plete binasal hemianopia. Both patients had unremarkable eye exams except for the visual field deficits and minimally reduced visual acuity and color vision. Both patients had normal neuroimaging. These are the first reported cases of complete binasal visual field defects without an identifiable ocular or neurologic cause. euro-ophthalmologists rarely encounter patients with binasal (heteronymous) hemianopia. Several reports of incomplete binasal visual fi eld defects have appeared N(1–5). We found no reports, however, of complete bi- c d nasal hemianopia. Here we present two cases of asymptomatic complete binasal hemianopia associated with minimally reduced visual acuity and color vision, but with otherwise unremarkable eye exams and neuroimaging. -

Binasal Hemianopia
J Neurol Neurosurg Psychiatry: first published as 10.1136/jnnp.36.5.697 on 1 October 1973. Downloaded from Journal ofNeurology, Neurosurgery, and Psychiatry, 1973, 36, 697-709 Binasal hemianopia J. E. A. O'CONNELL AND E. P. G. H. DU BOULAY From St. Bartholomew's Hospital, London SUMMARY Three patients with nasal visual field defects are described. In each case it is believed that compression of the lateral fibres of the optic nerve by the anterior cerebral or internal carotid artery was the cause. Binasal hemianopia can thus be produced by a single lesion and is as much a true hemianopia as the common bitemporal one. The value of careful neuroradiological investiga- tion to display the relationships of a tumour to the chiasma, optic nerves, and related vessels and thus explain the field defects is demonstrated. Isolated loss of the nasal fields of vision is un- nized during the middle of the last century, the common. In Traquair's Clinical Perimetry (Scott, passage of time and increasing experience were 1957) it is stated that the term hemianopia is necessary before these methods of clinical Protected by copyright. best reserved for bilateral field defects produced investigation could be fully utilized. During the by a single lesion-chiasmal or suprachiasmal. same period the pathology of compression of the This author considered that binasal hemianopia optic nerves and chiasma attracted considerable was not a true hemianopia, since its occurrence attention and a number of descriptions of in- indicated bilateral involvement of the uncrossed volvement of these structures by the Willisian fibres at the chiasma, the crossed fibres remaining vessels, observed at postmortem examination, intact. -

On So-Called Binasal Hemianopsia in Brain Tumor
tion of these various products is inert, perhaps authoritative writers, the one unsurpassed in it is inactivated or its activity greatly retarded the field of cerebral surgery, the other unsur- by the various menstrua. We see that scale pep- passed in the field of perimetry, cannot fail to sin, 15 grs. to a fl. 5 ss of distilled water, re- carry great weight. duced the albumin to 4^4 grs. (Test Series Quoting from their paper (p. 597) :— No. 5, Tube No. x), and to 33,4 grs. (Test Series "A constriction of the field of vision due to a de- No. Tube No. vti). Scale in the pro- 6, pepsin struction of fibres more of found in the complete from the temporal portion .3% (as gastric juice) than from the nasal half of the retina and justify- did not exert any great effect, the albumin ing the designation of nasal hemianopsia has been 8 or 9 Series No. weighed grs. (Test 5, Tube observed in from 5 to 6% of a series of 500 cases of No. vin. The reader may make other deduc- brain tumor.". "It is difficult or impossible to at- tions by studying and comparing the tables. tribute the ultimate binasal blindness to a lesion The first three series demonstrated as far as confined alone to the nerve and retina. Another visible results could be judged, that the higher factor must come into play, which elsewhere in the course of the nerve affects uncrossed fasciculus temperature of 125° F. did not cause any greater the digestive effect than did the temperature of from the temporal retina more markedly than the 100° F. -

Poster Session
North American Neuro-Ophthalmology Society 41st Annual Meeting February 21-26, 2015 Hotel del Coronado • San Diego, California Poster Presentations Tuesday, February 24, 2015 • 6:00 p.m. – 9:30 p.m. Authors will be standing by their posters during the following hours: Odd-Numbered Posters: 6:45 p.m. – 7:30 p.m. Even-Numbered Posters: 7:30 p.m. – 8:15 p.m. Poster # Presenting Author Category: Anterior Afferent Visual Pathway (Optic Neuropathy and Chiasm) 1 Normal Tension Glaucoma (NTG) is it a Type of Glaucoma or an Entity of a Mohammed Areesh Compressive Optic Neuropathy (CON)? 2 Anterior Ischemic Optic Neuropathy Due to Biopsy-Proven Giant Cell Arteritis in Thai Taweevat Attaseth Patients 3 Visual Outcomes Following Perioperative Vision Loss Jasmina Bajric 4 Pituitary Apoplexy in Pregnancy Matthew J. Benage 5 Bilateral, Sequential Anterior then Posterior Ischemic Optic Neuropathy in a Young Damian E. Migraineur Berezovsky 6 Traumatic Optic Neuropathy. Our Experience Mariana de Virgiliis 7 Sensitivity of Magnetic Resonance Imaging in Acute Demyelinating Optic Neuritis Lulu LCD Bursztyn 8 Characterization of Leber’s Hereditary Optic Neuropathy Patients Treated with Jasdeep S. Chahal Idebenone 9 Gliosarcoma of the Optic Nerves 15 years After Radiation Treatment for Hypophyseal Ayse I. Colpak Adenoma 10 Optic Nerve Compression by an Anomalous Internal Carotid Artery Valerie I. Elmalem 11 Identifying Risk Factors for the Development of Radiation Optic Neuropathy at “Safe” Pavle Doroslovački Doses: A Review of Cases Seen 1994-2014 12 Optic Neuritis After Refractive Surgery: Causal or Coincidence? Shlomo Dotan 13 Long Term Treatment of Lebers Hereditary Optic Neuropathy with Idebenone Jennifer I. -

Complete Binasal Hemianopsia
perim Ex en l & ta a l ic O p in l h t C h f Journal of Clinical & Experimental a Lešták et al. J Clinic Experiment Ophthalmol 2011, S:5 o l m l a o DOI: 10.4172/2155-9570.S5-002 n l r o g u y o J Ophthalmology ISSN: 2155-9570 ResearchCase Report Article OpenOpen Access Access Complete Binasal Hemianopsia Jan Lešták1*, Ivan Škúci2, Renata Říčařová3, Milan Choc2 and Jan Kastner4 1JL Clinic, Prague, Czech Republic 2Neurosurgery Department of the University Hospital in Plzen, Czech Republic 3Eye Clinic of the University Hospital in Plzen, Czech Republic 4Imaging Methods Clinic of the University Hospital in Plzen, Czech Republic Abstract The authors describe a case study of a 21-year-old female patient suffering from a tumour in the pineal region and dorsal part of the 3rd cerebral ventricle (pineocytoma) who developed complete binasal hemianopsia 11 months after the tumour’s removal. These perimetric changes did not show any progression for seven years. In discussing the question of the pathogenesis of hemianopic defects, the authors are inclined to the opinion that both of the optic nerves are compressed by the circle of Willis vessels. Keywords: Complete binasal hemianopsia; Tumour in the pineal widely adhered and pressed against the colliculi superiores et inferiores region and the third cerebral ventricle; Pathogenesis of binasal of the upper stalk burrowing into the caudal part of the 3rd ventricle. hemianopsia The tumour was partially cystic, some parts had brittle structure while other parts had rigid bodies. The tumour was gradually sharply Introduction separated from the base respecting its boundary against the upper stalk The existence of complete binasal hemianopsia has been disputed and was radically removed. -

Morgan C. Ollinger, OD, FAAO Phone: 231-408-8030 Email: [email protected]
Morgan C. Ollinger, OD, FAAO Phone: 231-408-8030 Email: [email protected] Professional Experience Clinical Instructor 2017-Present Southern College of Optometry, Memphis, TN Duties include: Overseeing student interns within pediatric, vision therapy, and primary care services Clinical research Scholarly activities within the optometric field Residency in Pediatric Optometry 2016-2017 Michigan College of Optometry, Big Rapids, MI Duties include: Examining pediatric patients, managing binocular vision disorders, and overseeing student interns within the College’s Pediatric service Examining pediatric patients at Cherry Street Health Services, a Federally Qualified Health Centre, as well as within the public school system Observing ophthalmologic and pediatric specialties throughout Michigan Assisting within pediatric and vision therapy teaching labs Education Residency in Pediatric Optometry 2016-2017 Michigan College of Optometry, Big Rapids, MI Doctor of Optometry (with Distinction) 2012-2016 University of Waterloo, Waterloo, ON 93 of 120 credit hours completed towards Bachelor of 2009-2012 Science in Biology University of Regina, Regina, SK Accepted into the Doctor of Optometry program after 3 years Peer Reviewed Posters Survey of self-reported reading and video gaming habits 2021 and ocular discomfort Heart of America – Kansas City, MO (Co-Author) A Comparison of Near Visual Acuity Optotype Validity 2019 within a Pediatric Population American Academy of Optometry – Orlando, FL (Co-Author) Changes in Near Visual Function from -

Methodic Materials Cranial Nerves
Medical Academy named after S.I. Georgievsky of V.I. Vernadsky CFU Department of Neurology a n d Neurosurgery Cliiss 4 Anatomy, physiology and pathology of the Cranial nerves VII-XI1 Key points: 1. Brainstem: 1.1. Surface anatomy 1.2.Internal structures and organization 1.3.Cross section through the medulla 1.4.Cross section through the pons 1.5.Cross section through the rostral midbrain 2. Cranial Nerves 2.1. Anatomy 2.2. Functions 2.3. Connections 2.4. Symptoms, signs, syndromes of lesions 2.5. Clinical correlations Key concepts: 1) Study the transverse sections o f the brain stem and localize the cranial nerve nuclei. 2) Study the ventral and dorsal surface o f the brain stem and identify the exiting and entering cranial nerves. 3) Carefully study all o f the figures and legends 4) Study the main information about anatomy of all cranial nerves, their functions, connections and symptoms/signs/syndromes of lesions Define the following terms: Brain stem, medial structures, lateral structures, dorsal structures, tegmentum, medial lemniscus, gracile and cuneate nuclei, pyramids, corticospinal fibers, inferior cerebellar peduncle, spinocerebellar tract, cuneocerebellar tract, olivocerebellar tract, lateral spinothalamic tract (spinal lemniscus), superior colliculi, inferior colliculi, oliva, medial longitudinal fasciculus (MLF), cerebral peduncle, red nucleus, substantia nigra, hypoglossal nucleus o f CNXII, nucleus ambiguus X, andXI), vestibular nuclei (CN VIII,) spinal nucleus and tract o f trigeminal nerve, abducent nucleus of CN VI, facial nucleus (CN VII), spinal nucleus and tract o f trigeminal nerve (CN V), oculomotor nucleus (CN III), cranial nerves I-XII. Literature: Mathias Baehr, M.D., Michael Frotscher, M.D.