Myeloma NK Cells Are Exhausted and Have Impaired Regulation of Activation
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
List of Genes Used in Cell Type Enrichment Analysis
List of genes used in cell type enrichment analysis Metagene Cell type Immunity ADAM28 Activated B cell Adaptive CD180 Activated B cell Adaptive CD79B Activated B cell Adaptive BLK Activated B cell Adaptive CD19 Activated B cell Adaptive MS4A1 Activated B cell Adaptive TNFRSF17 Activated B cell Adaptive IGHM Activated B cell Adaptive GNG7 Activated B cell Adaptive MICAL3 Activated B cell Adaptive SPIB Activated B cell Adaptive HLA-DOB Activated B cell Adaptive IGKC Activated B cell Adaptive PNOC Activated B cell Adaptive FCRL2 Activated B cell Adaptive BACH2 Activated B cell Adaptive CR2 Activated B cell Adaptive TCL1A Activated B cell Adaptive AKNA Activated B cell Adaptive ARHGAP25 Activated B cell Adaptive CCL21 Activated B cell Adaptive CD27 Activated B cell Adaptive CD38 Activated B cell Adaptive CLEC17A Activated B cell Adaptive CLEC9A Activated B cell Adaptive CLECL1 Activated B cell Adaptive AIM2 Activated CD4 T cell Adaptive BIRC3 Activated CD4 T cell Adaptive BRIP1 Activated CD4 T cell Adaptive CCL20 Activated CD4 T cell Adaptive CCL4 Activated CD4 T cell Adaptive CCL5 Activated CD4 T cell Adaptive CCNB1 Activated CD4 T cell Adaptive CCR7 Activated CD4 T cell Adaptive DUSP2 Activated CD4 T cell Adaptive ESCO2 Activated CD4 T cell Adaptive ETS1 Activated CD4 T cell Adaptive EXO1 Activated CD4 T cell Adaptive EXOC6 Activated CD4 T cell Adaptive IARS Activated CD4 T cell Adaptive ITK Activated CD4 T cell Adaptive KIF11 Activated CD4 T cell Adaptive KNTC1 Activated CD4 T cell Adaptive NUF2 Activated CD4 T cell Adaptive PRC1 Activated -

Markers of T Cell Senescence in Humans
International Journal of Molecular Sciences Review Markers of T Cell Senescence in Humans Weili Xu 1,2 and Anis Larbi 1,2,3,4,5,* 1 Biology of Aging Program and Immunomonitoring Platform, Singapore Immunology Network (SIgN), Agency for Science Technology and Research (A*STAR), Immunos Building, Biopolis, Singapore 138648, Singapore; [email protected] 2 School of Biological Sciences, Nanyang Technological University, Singapore 637551, Singapore 3 Department of Microbiology, National University of Singapore, Singapore 117597, Singapore 4 Department of Geriatrics, Faculty of Medicine, University of Sherbrooke, Sherbrooke, QC J1K 2R1, Canada 5 Faculty of Sciences, University ElManar, Tunis 1068, Tunisia * Correspondence: [email protected]; Tel.: +65-6407-0412 Received: 31 May 2017; Accepted: 26 July 2017; Published: 10 August 2017 Abstract: Many countries are facing the aging of their population, and many more will face a similar obstacle in the near future, which could be a burden to many healthcare systems. Increased susceptibility to infections, cardiovascular and neurodegenerative disease, cancer as well as reduced efficacy of vaccination are important matters for researchers in the field of aging. As older adults show higher prevalence for a variety of diseases, this also implies higher risk of complications, including nosocomial infections, slower recovery and sequels that may reduce the autonomy and overall quality of life of older adults. The age-related effects on the immune system termed as “immunosenescence” can be exemplified by the reported hypo-responsiveness to influenza vaccination of the elderly. T cells, which belong to the adaptive arm of the immune system, have been extensively studied and the knowledge gathered enables a better understanding of how the immune system may be affected after acute/chronic infections and how this matters in the long run. -

Human Β‑1,3‑Glucuronyltransferase 1/B3GAT1 Antibody Monoclonal Mouse Igg2a Clone # 1002707 Catalog Number: MAB8560
Human β‑1,3‑Glucuronyltransferase 1/B3GAT1 Antibody Monoclonal Mouse IgG2A Clone # 1002707 Catalog Number: MAB8560 DESCRIPTION Species Reactivity Human Specificity Detects human β-1,3-Glucuronyltransferase 1/B3GAT1 in direct ELISAs. Source Monoclonal Mouse IgG2A Clone # 1002707 Purification Protein A or G purified from hybridoma culture supernatant Immunogen Chinese Hamster Ovary cell line, CHO-derived human β‑1,3‑Glucuronyltransferase 1/B3GAT1 His25-Ile334 Accession # Q9P2W7 Formulation Lyophilized from a 0.2 μm filtered solution in PBS with Trehalose. See Certificate of Analysis for details. *Small pack size (-SP) is supplied either lyophilized or as a 0.2 μm filtered solution in PBS. APPLICATIONS Please Note: Optimal dilutions should be determined by each laboratory for each application. General Protocols are available in the Technical Information section on our website. Recommended Sample Concentration Immunohistochemistry 5-25 µg/mL See Below DATA Immunohistochemistry β-1,3-Glucuronyltransferase 1/B3GAT1 in Human Brain. β-1,3-Glucuronyltransferase 1/B3GAT1 was detected in immersion fixed paraffin-embedded sections of human brain (cortex) using Mouse Anti-Human β-1,3- Glucuronyltransferase 1/B3GAT1 Monoclonal Antibody (Catalog # MAB8560) at 5 µg/mL for 1 hour at room temperature followed by incubation with the Anti-Mouse IgG VisUCyte™ HRP Polymer Antibody (Catalog # VC001). Before incubation with the primary antibody, tissue was subjected to heat-induced epitope retrieval using Antigen Retrieval Reagent-Basic (Catalog # CTS013). Tissue was stained using DAB (brown) and counterstained with hematoxylin (blue). Specific staining was localized to cytoplasm in neurons. View our protocol for IHC Staining with VisUCyte HRP Polymer Detection Reagents. PREPARATION AND STORAGE Reconstitution Reconstitute at 0.5 mg/mL in sterile PBS. -

CD38, CD157, and RAGE As Molecular Determinants for Social Behavior
cells Review CD38, CD157, and RAGE as Molecular Determinants for Social Behavior Haruhiro Higashida 1,2,* , Minako Hashii 1,3, Yukie Tanaka 4, Shigeru Matsukawa 5, Yoshihiro Higuchi 6, Ryosuke Gabata 1, Makoto Tsubomoto 1, Noriko Seishima 1, Mitsuyo Teramachi 1, Taiki Kamijima 1, Tsuyoshi Hattori 7, Osamu Hori 7 , Chiharu Tsuji 1, Stanislav M. Cherepanov 1 , Anna A. Shabalova 1, Maria Gerasimenko 1, Kana Minami 1, Shigeru Yokoyama 1, Sei-ichi Munesue 8, Ai Harashima 8, Yasuhiko Yamamoto 8, Alla B. Salmina 1,2 and Olga Lopatina 2 1 Department of Basic Research on Social Recognition and Memory, Research Center for Child Mental Development, Kanazawa University, Kanazawa 920-8640, Japan; [email protected] (M.H.); [email protected] (R.G.); [email protected] (M.T.); [email protected] (N.S.); [email protected] (M.T.); [email protected] (T.K.); [email protected] (C.T.); [email protected] (S.M.C.); [email protected] (A.A.S.); [email protected] (M.G.); minami-k@staff.kanazawa-u.ac.jp (K.M.); [email protected] (S.Y.) 2 Laboratory of Social Brain Study, Research Institute of Molecular Medicine and Pathobiochemistry, Krasnoyarsk State Medical University named after Prof. V.F. Voino-Yasenetsky, Krasnoyarsk 660022, Russia; [email protected] (A.B.S.); [email protected] (O.L.) 3 Division of Molecular Genetics and Clinical Research, National Hospital Organization Nanao Hospital, Nanao 926-0841, Japan 4 Molecular Biology and Chemistry, Faculty of Medical Science, University of Fukui, Fukui -

Dysregulated CD38 Expression on Peripheral Blood Immune Cell Subsets in SLE
International Journal of Molecular Sciences Article Dysregulated CD38 Expression on Peripheral Blood Immune Cell Subsets in SLE Marie Burns 1,†, Lennard Ostendorf 1,2,3,† , Robert Biesen 1,2 , Andreas Grützkau 1, Falk Hiepe 1,2, Henrik E. Mei 1,† and Tobias Alexander 1,2,*,† 1 Deutsches Rheuma-Forschungszentrum (DRFZ Berlin), a Leibniz Institute, 10117 Berlin, Germany; [email protected] (M.B.); [email protected] (L.O.); [email protected] (R.B.); [email protected] (A.G.); [email protected] (F.H.); [email protected] (H.E.M.) 2 Department of Rheumatology and Clinical Immunology, Charité–Universitätsmedizin Berlin, Corporate Member of Freie Universität Berlin, Humboldt-Universität zu Berlin and The Berlin Institute of Health (BIH), 10117 Berlin, Germany 3 Department of Nephrology and Intensive Care Medicine, Charité–Universitätsmedizin Berlin, Corporate Member of Freie Universität Berlin, Humboldt-Universität zu Berlin and The Berlin Institute of Health (BIH), 10117 Berlin, Germany * Correspondence: [email protected] † Authors contributed equally to this manuscript. Abstract: Given its uniformly high expression on plasma cells, CD38 has been considered as a therapeutic target in patients with systemic lupus erythematosus (SLE). Herein, we investigate the distribution of CD38 expression by peripheral blood leukocyte lineages to evaluate the potential therapeutic effect of CD38-targeting antibodies on these immune cell subsets and to delineate the use of CD38 as a biomarker in SLE. We analyzed the expression of CD38 on peripheral blood leukocyte subsets by flow and mass cytometry in two different cohorts, comprising a total of 56 SLE patients. The CD38 expression levels were subsequently correlated across immune cell lineages and subsets, Citation: Burns, M.; Ostendorf, L.; and with clinical and serologic disease parameters of SLE. -

CD Markers Are Routinely Used for the Immunophenotyping of Cells
ptglab.com 1 CD MARKER ANTIBODIES www.ptglab.com Introduction The cluster of differentiation (abbreviated as CD) is a protocol used for the identification and investigation of cell surface molecules. So-called CD markers are routinely used for the immunophenotyping of cells. Despite this use, they are not limited to roles in the immune system and perform a variety of roles in cell differentiation, adhesion, migration, blood clotting, gamete fertilization, amino acid transport and apoptosis, among many others. As such, Proteintech’s mini catalog featuring its antibodies targeting CD markers is applicable to a wide range of research disciplines. PRODUCT FOCUS PECAM1 Platelet endothelial cell adhesion of blood vessels – making up a large portion molecule-1 (PECAM1), also known as cluster of its intracellular junctions. PECAM-1 is also CD Number of differentiation 31 (CD31), is a member of present on the surface of hematopoietic the immunoglobulin gene superfamily of cell cells and immune cells including platelets, CD31 adhesion molecules. It is highly expressed monocytes, neutrophils, natural killer cells, on the surface of the endothelium – the thin megakaryocytes and some types of T-cell. Catalog Number layer of endothelial cells lining the interior 11256-1-AP Type Rabbit Polyclonal Applications ELISA, FC, IF, IHC, IP, WB 16 Publications Immunohistochemical of paraffin-embedded Figure 1: Immunofluorescence staining human hepatocirrhosis using PECAM1, CD31 of PECAM1 (11256-1-AP), Alexa 488 goat antibody (11265-1-AP) at a dilution of 1:50 anti-rabbit (green), and smooth muscle KD/KO Validated (40x objective). alpha-actin (red), courtesy of Nicola Smart. PECAM1: Customer Testimonial Nicola Smart, a cardiovascular researcher “As you can see [the immunostaining] is and a group leader at the University of extremely clean and specific [and] displays Oxford, has said of the PECAM1 antibody strong intercellular junction expression, (11265-1-AP) that it “worked beautifully as expected for a cell adhesion molecule.” on every occasion I’ve tried it.” Proteintech thanks Dr. -

The Enzymatic Activities of CD38 Enhance CLL Growth and Trafficking
Leukemia (2015) 29, 356–368 © 2015 Macmillan Publishers Limited All rights reserved 0887-6924/15 www.nature.com/leu ORIGINAL ARTICLE The enzymatic activities of CD38 enhance CLL growth and trafficking: implications for therapeutic targeting T Vaisitti1,2, V Audrito1,2, S Serra1,2, R Buonincontri1,2, G Sociali3, E Mannino3, A Pagnani2, A Zucchetto4, E Tissino4, C Vitale5, M Coscia5, C Usai6, C Pepper7, V Gattei4, S Bruzzone3 and S Deaglio1,2 The ecto-enzyme CD38 is gaining momentum as a novel therapeutic target for patients with hematological malignancies, with several anti-CD38 monoclonal antibodies in clinical trials with promising results. In chronic lymphocytic leukemia (CLL) CD38 is a marker of unfavorable prognosis and a central factor in the pathogenetic network underlying the disease: activation of CD38 regulates genetic pathways involved in proliferation and movement. Here we show that CD38 is enzymatically active in primary CLL cells and that its forced expression increases disease aggressiveness in a xenograft model. The effect is completely lost when using an enzyme-deficient version of CD38 with a single amino-acid mutation. Through the enzymatic conversion of NAD into ADPR (ADP-ribose) and cADPR (cyclic ADP-ribose), CD38 increases cytoplasmic Ca2+ concentrations, positively influencing proliferation and signaling mediated via chemokine receptors or integrins. Consistently, inhibition of the enzymatic activities of CD38 using the flavonoid kuromanin blocks CLL chemotaxis, adhesion and in vivo homing. In a short-term xenograft model using primary cells, kuromanin treatment traps CLL cells in the blood, thereby increasing responses to chemotherapy. These results suggest that monoclonal antibodies that block the enzymatic activities of CD38 or enzyme inhibitors may prove therapeutically useful. -

Differential Integrin Adhesome Expression Defines Human Natural
bioRxiv preprint doi: https://doi.org/10.1101/2020.12.01.404806; this version posted December 1, 2020. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted bioRxiv a license to display the preprint in perpetuity. It is made available under aCC-BY-NC 4.0 International license. Differential integrin adhesome expression defines human natural killer cell residency and developmental stage Everardo Hegewisch Solloa1, Seungmae Seo1, Bethany L. Mundy-Bosse2, Anjali Mishra3,a, Erik Waldman4,b, Sarah Maurrasse4,b, Eli Grunstein4, Thomas J. Connors5, Aharon G. Freud2,6, and Emily M. Mace1 1Department of Pediatrics, Columbia University College of Physicians and Surgeons, New York NY 10032 2Division of Hematology, Department of Internal Medicine, The Ohio State University, Columbus, OH 43210, USA; Comprehensive Cancer Center and The James Cancer Hospital and Solove Research Institute, The Ohio State University, Columbus, OH 43210 33Division of Dermatology, Department of Internal Medicine, The Ohio State University, Columbus, OH 43210, USA; Comprehensive Cancer Center and The James Cancer Hospital and Solove Research Institute, The Ohio State University, Columbus, OH 43210 4Department of Otolaryngology - Head and Neck Surgery, Columbia University Medical Center, New York, New York 10032 5Department of Pediatrics, Division of Pediatric Critical Care and Hospital Medicine, Columbia University Irving Medical Center, New York, NY 10024 6Department of Pathology, The Ohio State University, Columbus, -
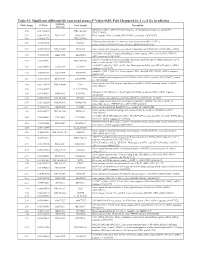
(P -Value<0.05, Fold Change≥1.4), 4 Vs. 0 Gy Irradiation
Table S1: Significant differentially expressed genes (P -Value<0.05, Fold Change≥1.4), 4 vs. 0 Gy irradiation Genbank Fold Change P -Value Gene Symbol Description Accession Q9F8M7_CARHY (Q9F8M7) DTDP-glucose 4,6-dehydratase (Fragment), partial (9%) 6.70 0.017399678 THC2699065 [THC2719287] 5.53 0.003379195 BC013657 BC013657 Homo sapiens cDNA clone IMAGE:4152983, partial cds. [BC013657] 5.10 0.024641735 THC2750781 Ciliary dynein heavy chain 5 (Axonemal beta dynein heavy chain 5) (HL1). 4.07 0.04353262 DNAH5 [Source:Uniprot/SWISSPROT;Acc:Q8TE73] [ENST00000382416] 3.81 0.002855909 NM_145263 SPATA18 Homo sapiens spermatogenesis associated 18 homolog (rat) (SPATA18), mRNA [NM_145263] AA418814 zw01a02.s1 Soares_NhHMPu_S1 Homo sapiens cDNA clone IMAGE:767978 3', 3.69 0.03203913 AA418814 AA418814 mRNA sequence [AA418814] AL356953 leucine-rich repeat-containing G protein-coupled receptor 6 {Homo sapiens} (exp=0; 3.63 0.0277936 THC2705989 wgp=1; cg=0), partial (4%) [THC2752981] AA484677 ne64a07.s1 NCI_CGAP_Alv1 Homo sapiens cDNA clone IMAGE:909012, mRNA 3.63 0.027098073 AA484677 AA484677 sequence [AA484677] oe06h09.s1 NCI_CGAP_Ov2 Homo sapiens cDNA clone IMAGE:1385153, mRNA sequence 3.48 0.04468495 AA837799 AA837799 [AA837799] Homo sapiens hypothetical protein LOC340109, mRNA (cDNA clone IMAGE:5578073), partial 3.27 0.031178378 BC039509 LOC643401 cds. [BC039509] Homo sapiens Fas (TNF receptor superfamily, member 6) (FAS), transcript variant 1, mRNA 3.24 0.022156298 NM_000043 FAS [NM_000043] 3.20 0.021043295 A_32_P125056 BF803942 CM2-CI0135-021100-477-g08 CI0135 Homo sapiens cDNA, mRNA sequence 3.04 0.043389246 BF803942 BF803942 [BF803942] 3.03 0.002430239 NM_015920 RPS27L Homo sapiens ribosomal protein S27-like (RPS27L), mRNA [NM_015920] Homo sapiens tumor necrosis factor receptor superfamily, member 10c, decoy without an 2.98 0.021202829 NM_003841 TNFRSF10C intracellular domain (TNFRSF10C), mRNA [NM_003841] 2.97 0.03243901 AB002384 C6orf32 Homo sapiens mRNA for KIAA0386 gene, partial cds. -

Monoclonal Antibodies in Myeloma
Monoclonal Antibodies in Myeloma Pia Sondergeld, PhD, Niels W. C. J. van de Donk, MD, PhD, Paul G. Richardson, MD, and Torben Plesner, MD Dr Sondergeld is a medical student at the Abstract: The development of monoclonal antibodies (mAbs) for University of Giessen in Giessen, Germany. the treatment of disease goes back to the vision of Paul Ehrlich in Dr van de Donk is a hematologist in the the late 19th century; however, the first successful treatment with department of hematology at the VU a mAb was not until 1982, in a lymphoma patient. In multiple University Medical Center in Amsterdam, The Netherlands. Dr Richardson is the R.J. myeloma, mAbs are a very recent and exciting addition to the Corman Professor of Medicine at Harvard therapeutic armamentarium. The incorporation of mAbs into Medical School, and clinical program current treatment strategies is hoped to enable more effective and leader and director of clinical research targeted treatment, resulting in improved outcomes for patients. at the Jerome Lipper Myeloma Center, A number of targets have been identified, including molecules division of hematologic malignancy, depart- on the surface of the myeloma cell and components of the bone ment of medical oncology, Dana-Farber Cancer Institute in Boston, MA. Dr Plesner marrow microenvironment. Our review focuses on a small number is a professor of hematology at the Univer- of promising mAbs directed against molecules on the surface of sity of Southern Denmark and a consultant myeloma cells, including CS1 (elotuzumab), CD38 (daratumumab, in the department of hematology at Vejle SAR650984, MOR03087), CD56 (lorvotuzumab mertansine), and Hospital in Vejle, Denmark. -

Identification of Key Pathways and Genes in Dementia Via Integrated Bioinformatics Analysis
bioRxiv preprint doi: https://doi.org/10.1101/2021.04.18.440371; this version posted July 19, 2021. The copyright holder for this preprint (which was not certified by peer review) is the author/funder. All rights reserved. No reuse allowed without permission. Identification of Key Pathways and Genes in Dementia via Integrated Bioinformatics Analysis Basavaraj Vastrad1, Chanabasayya Vastrad*2 1. Department of Biochemistry, Basaveshwar College of Pharmacy, Gadag, Karnataka 582103, India. 2. Biostatistics and Bioinformatics, Chanabasava Nilaya, Bharthinagar, Dharwad 580001, Karnataka, India. * Chanabasayya Vastrad [email protected] Ph: +919480073398 Chanabasava Nilaya, Bharthinagar, Dharwad 580001 , Karanataka, India bioRxiv preprint doi: https://doi.org/10.1101/2021.04.18.440371; this version posted July 19, 2021. The copyright holder for this preprint (which was not certified by peer review) is the author/funder. All rights reserved. No reuse allowed without permission. Abstract To provide a better understanding of dementia at the molecular level, this study aimed to identify the genes and key pathways associated with dementia by using integrated bioinformatics analysis. Based on the expression profiling by high throughput sequencing dataset GSE153960 derived from the Gene Expression Omnibus (GEO), the differentially expressed genes (DEGs) between patients with dementia and healthy controls were identified. With DEGs, we performed a series of functional enrichment analyses. Then, a protein–protein interaction (PPI) network, modules, miRNA-hub gene regulatory network and TF-hub gene regulatory network was constructed, analyzed and visualized, with which the hub genes miRNAs and TFs nodes were screened out. Finally, validation of hub genes was performed by using receiver operating characteristic curve (ROC) analysis. -

B3GAT1 Antibody Cat
B3GAT1 Antibody Cat. No.: 64-189 B3GAT1 Antibody Flow cytometric analysis of K562 cells (right histogram) compared to a negative control cell (left histogram).FITC-conjugated goat-anti- rabbit secondary antibodies were used for the analysis. Specifications HOST SPECIES: Rabbit SPECIES REACTIVITY: Human This B3GAT1 antibody is generated from rabbits immunized with a KLH conjugated IMMUNOGEN: synthetic peptide between 21-48 amino acids from the N-terminal region of human B3GAT1. TESTED APPLICATIONS: Flow, WB For WB starting dilution is: 1:1000 APPLICATIONS: For FACS starting dilution is: 1:10~50 PREDICTED MOLECULAR 38 kDa WEIGHT: September 26, 2021 1 https://www.prosci-inc.com/b3gat1-antibody-64-189.html Properties This antibody is purified through a protein A column, followed by peptide affinity PURIFICATION: purification. CLONALITY: Polyclonal ISOTYPE: Rabbit Ig CONJUGATE: Unconjugated PHYSICAL STATE: Liquid BUFFER: Supplied in PBS with 0.09% (W/V) sodium azide. CONCENTRATION: batch dependent Store at 4˚C for three months and -20˚C, stable for up to one year. As with all antibodies STORAGE CONDITIONS: care should be taken to avoid repeated freeze thaw cycles. Antibodies should not be exposed to prolonged high temperatures. Additional Info OFFICIAL SYMBOL: B3GAT1 Galactosylgalactosylxylosylprotein 3-beta-glucuronosyltransferase 1, Beta-1,3- ALTERNATE NAMES: glucuronyltransferase 1, Glucuronosyltransferase P, GlcAT-P, UDP-GlcUA:glycoprotein beta-1,3-glucuronyltransferase, GlcUAT-P, B3GAT1, GLCATP ACCESSION NO.: Q9P2W7 PROTEIN GI NO.: 205830910 GENE ID: 27087 USER NOTE: Optimal dilutions for each application to be determined by the researcher. Background and References The protein encoded by this gene is a member of the glucuronyltransferase gene family.