Peripheral Giant Cell Granuloma-A Rare Oral Entity
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

ROLE of MAST CELL in ORAL PATHOLOGY Supriya Kheur Deepali Patekar Neeta Bagul Meena Kulkarni Samapika Routray 1 Varsha Dhas Department of Oral Pathology,Dr
320 ROLE OF MAST CELL IN ORAL PATHOLOGY Supriya Kheur Deepali Patekar Neeta Bagul Meena Kulkarni Samapika Routray 1 Varsha Dhas Department of Oral Pathology,Dr. D.Y.Patil Dental College and Hospital, Pimpri, Pune-18, India 1Department of Oral Pathology, GITAM Dental College, Vishakhapattanam, India Corresponding Author: Supriya Kheur, Department of Oral Pathology,Dr. D.Y.Patil Dental College and Hospital, Pimpri, Pune-18, India. Ph -09970150760, Email : [email protected] Abstract Mast cells in oral tissues releases various pro-inflammatory cytokine tumor necrosis factor alpha (TNF-Ü) which promotes leukocyte infiltration in various inflammatory condition of oral cavity such as oral lichen planus (OLP), periapical lesions, gingivitis & periodontitis. T lymphocyte derived cytokines influences mast cell migration & mediator release. Mast cell secreted proteases, activates matrix-metalloprotinases-9 (MMP-9) which may contribute to alteration in basement membrane in inflammatory condition such as Lichen Planus. Hence by understanding the role of mast cells in the pathogenesis of various diseases; therapies should be targeted to enhance the prognosis of the diseases. Key Words: Mast cells, Degranulation, Cytokines, Tryptase, Chymase. Introduction chemotactins, cell activating & cell growth Mast cells (MC) are large spherical or factor. Tissue mast cells are not homogenous elliptical mononuclear cells found in a variety for eg. enzymes within granules of mucosal & of tissues including skin, submucosa or connective tissue mast cells are different from connective tissue of various organs & each other. The ranges of mast cell activity is (1) specialized for their anatomic location, as the mucosal epithelial tissues & also in dental granules are different for mucosal and pulp. -

A Single Case Report of Granular Cell Tumor of the Tongue Successfully Treated Through 445 Nm Diode Laser
healthcare Case Report A Single Case Report of Granular Cell Tumor of the Tongue Successfully Treated through 445 nm Diode Laser Maria Vittoria Viani 1,*, Luigi Corcione 1, Chiara Di Blasio 2, Ronell Bologna-Molina 3 , Paolo Vescovi 1 and Marco Meleti 1 1 Department of Medicine and Surgery, University of Parma, 43126 Parma, Italy; [email protected] (L.C.); [email protected] (P.V.); [email protected] (M.M.) 2 Private practice, Centro Medico Di Blasio, 43121 Parma; Italy; [email protected] 3 Faculty of Dentistry, University of the Republic, 14600 Montevideo, Uruguay; [email protected] * Correspondence: [email protected] Received: 10 June 2020; Accepted: 11 August 2020; Published: 13 August 2020 Abstract: Oral granular cell tumor (GCT) is a relatively rare, benign lesion that can easily be misdiagnosed. Particularly, the presence of pseudoepitheliomatous hyperplasia might, in some cases, lead to the hypothesis of squamous cell carcinoma. Surgical excision is the treatment of choice. Recurrence has been reported in up to 15% of cases treated with conventional surgery. Here, we reported a case of GCT of the tongue in a young female patient, which was successfully treated through 445 nm diode laser excision. Laser surgery might reduce bleeding and postoperative pain and may be associated with more rapid healing. Particularly, the vaporization effect on remnant tissues could eliminate GCT cells on the surgical bed, thus hypothetically leading to a lower rate of recurrence. In the present case, complete healing occurred in 1 week, and no recurrence was observed after 6 months. Laser surgery also allows the possibility to obtain second intention healing. -

Prevalence of Oral Lesions in Complete Denture Wearers- an Original Research
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-ISSN: 2279-0853, p-ISSN: 2279-0861.Volume 20, Issue 1 Ser.3 (January. 2021), PP 29-33 www.iosrjournals.org Prevalence of oral lesions in complete denture wearers- An original research Prenika Sharma1*, Reecha Gupta2 1- MDS, Oral medicine and radiology 2- Professor and HOD Department of Prosthodontics, Indira Gandhi Govt. Dental College, Jammu (J&K) Abstract: Background: Complete denture patients are often associated with the various denture-related oral mucosallesions. The purpose of this study is to evaluate the prevalence ofdenture-related oral mucosal lesions in complete denture patients. Materials and Methods: The study was consisted of 225 patientshaving various denture-induced oral mucosal lesions from theoutpatient department of the department out of the 395 completedenture patients examined. Data related to gender, age, length ofdenture use, hygiene care were obtained. All the data were tabulated and analyzed. Results: In 225 complete denture patients. Denture stomatitis (60.23%) was the most commonlesion present, followed by Epulis fissuratum and angularcheilitis. The denture-induced oral mucosal lesions werefound more common in age >40 years (59.78%) and in female(52.70%) complete denture wearer patients. Conclusion: The present studies showed that oral lesions associated with wearing denture are prevalent and create health problems that impact the quality of life of dental patients. Key Words: Complete denture, denture stomatitis, Epulis fissuratum, oralmucosal lesions. --------------------------------------------------------------------------------------------------------------------------------------- Date of Submission: 26-12-2020 Date of Acceptance: 07-01-2021 --------------------------------------------------------------------------------------------------------------------------------------- I. Introduction Edentulism may be the last sequel of periodontal diseases and dental caries. In case of older adults, edentulism is essential as a correlate of self-esteem and quality of life. -

Download Download
628 Indian Journal of Forensic Medicine & Toxicology, July-September 2021, Vol. 15, No. 3 Tongue Lesions - A Review N.Anitha1, Dharini Jayachandran2 1Reader, Department of Oral Pathology and Microbiology,2Undergraduate Student, Sree Balaji Dental College and Hospital, Bharath Institute of Higher Education and Research Abstract Tongue is a vital organ within the oral cavity that has varied function,and it may act as an index for the underlying systemic diseases.The investigation of the tongue diseases may begin with mere clinical examination .This review is to highlight the signs and symptoms of the various lesions that affects the tongue and especially to talk in brief about the benign and malignant tumours that affect the tongue along with other inherited and congenital abnormalities.Tongue lesions are categorized as tumours,infections, reactionary,congenital,developmental,acquired,autoimmune and potentially malignant disorders for easy understanding and to arrive at appropriate diagnosis.Tongue playing an important role in maintaining the harmony in the oral environment,it should be treated from diseases. Keywords: Tongue lesions,benign tumours,malignant tumours,diseases of tongue. CLASSIFICATION OF LESIONS ● Pyogenic granuloma AFFECTING THE TONGUE. ● Frictional keratosis BENIGN TUMOURS OF THE TONGUE INFECTIOUS LESIONS OF TONGUE ● Capillary hemangioma ● Oral squamous papilloma ● Fibroma ● Oral hairy leukoplakia ● Cavernous hemangioma ● Candidiasiis ● Giant cell granuloma ● Median rhomboid glossitis ● Lipoma ● Sublingual abcess ● Lymphangioma INHERITED,CONGENITAL,DEVELOPMENT ● Schwannoma AND ACQUIRED ABNORMALITIES OF TONGUE MALIGNANT TUMOURS OF TONGUE ● White sponge nevus ● Squamous cell carcinoma ● Foliate papillitis ● Veruccous carcinoma ● Angina bullosa hemorrhagica ● Non-Hodgkin’s lymphoma ● Geographic tongue TRAUMATIC/REACTIONARY LESIONS OF ● Fissured tongue THE TONGUE ● Median rhomboid glossitis ● Fibrous reactive hyperplasia ● Bifurcated/tetrafurcated tongue ● Traumatic ulcer Indian Journal of Forensic Medicine & Toxicology, July-September 2021, Vol. -

Pyogenic Granuloma on the Upper Lip: an Unusual Location
www.scielo.br/jaos Pyogenic granuloma on the upper lip: an unusual location Eduardo Sanches GONÇALES1, José Humberto DAMANTE2, Cassia Maria FISCHER RUBIRA3, Luís Antônio de Assis Taveira4 1- DDS, PhD, Assistant Professor, Department of Stomatology, Bauru School of Dentistry, University of São Paulo, Bauru, SP, Brazil. 2- DDS, PhD, Professor, Department of Stomatology, Bauru School of Dentistry, University of São Paulo, Bauru, SP, Brazil. 3- DDS, PhD in Stomatology, Bauru School of Dentistry, University of São Paulo, Bauru, SP, Brazil. 4- DDS, PhD, Associate Professor, Department of Stomatology, Bauru School of Dentistry, University of São Paulo, Bauru, SP, Brazil. Corresponding address: Eduardo Sanches Gonçales - Faculdade de Odontologia de Bauru - USP - Departmento de Estomatologia - Al. Dr. Octavio Pinheiro Brisolla 9-75 - 17.012-901 - Bauru, SP - Brasil - Phone: 55 14 32358250 - e-mail:[email protected] Received: March 23, 2009 - Modification: September 16, 2009 - Accepted: October 11, 2009 ABSTRACT yogenic granuloma (PG) is a benign non-neoplastic mucocutaneous lesion. It is a Preactional response to constant minor trauma and might be related to hormonal changes. In the mouth, PG is manifested as a sessile or pedunculated, resilient, erythematous, exophytic and painful papule or nodule with a smooth or lobulated surface that bleeds easily. PG preferentially affects the gingiva, but may also occur on the lips, tongue, oral mucosa and palate. The most common treatment is surgical excision. This paper describes a mucocutaneous PG on the upper lip, analyzing the clinical characteristics and discussing the features that distinguish this lesion from other similar oral mucosa lesions. The diagnosis of oral lesions is complex and leads the dentist to consider distinct lesions with different diagnostic methods. -

Vegetating Darier's Disease During Pregnancy
Letters to the Editor 259 Vegetating Darier’s Disease During Pregnancy Daniel de la Rosa Carrillo Department of Dermatology, Ullevaal University Hospital, Oslo, Norway. E-mail: [email protected] Accepted December 12, 2005 Sir, She was discharged after 4 weeks. During that period she Darier’s disease is an autosomal dominant disorder cha- experienced improvement in the lesions on her abdomen, thumb, ears and feet. There was complete clearance of the lesion on her racterized by hyperkeratotic, crusted papules. Nails and cheek after 4 weeks. She continued topical treatment with clo- mucous membranes may also be involved. Histological betasol propionate 0.05% cream on the lesions on the abdomen examination shows suprabasal acantolhysis and overlying and thumb until clearance one month after discharge. dyskeratosis (1, 2). Both exacerbation and improvement of the disease during pregnancy have been described pre- viously, as have bacterial and viral secondary infections. DISCUSSION We present here a patient with exacerbation of Darier’s The condition was considered to be an exacerbation disease during pregnancy in a pattern that has not been of Darier’s disease during pregnancy, with concurrent described previously. bacterial infection and bilateral external otitis. Repeti- tive tests for virus, and especially herpes simplex and CASE REPORT varicella zoster, were all negative. Clinical differential A 37-year-old woman, para 1, gravida 2, 5 months pregnant, diagnoses were pemphigus vegetans of Hallopeau or with a known history of Darier’s disease since childhood, with pyogenic granuloma, but the negative direct immuno- intertriginous involvement, had been treated several times for fluorescence with acantholysis on histopathological pyoderma. -

Application of Lasers in Treatment of Oral Premalignant Lesions
Symbiosis www.symbiosisonline.org www.symbiosisonlinepublishing.com Review article Journal of Dentistry, Oral Disorders & Therapy Open Access Application of Lasers in Treatment of Oral Premalignant Lesions Amaninder Singh*1, Akanksha Zutshi2, Preetkanwal Singh Ahluwalia3, Vikas Sharma4 and Vandana Razdan5 1,4oral and maxillofacial surgery, reader, National Dental College and Hospital, Dera Bassi, Punjab 2oral and maxillofacial surgery, senior lecturer, National Dental College and Hospital, Dera Bassi, Punjab 3oral and maxillofacial surgery, professor, National Dental College and Hospital, Dera Bassi, Punjab 5Pharmacology, professor, Govt. Medical College and Hospital, Jammu Received: April 03, 2018; Accepted: June 04, 2018; Published: June 11, 2018 *Corresponding author: Amaninder Singh, House No- 620, Phase- 6, mohali, 160055, E-mail address: [email protected] Abstract radiation. Laser systems and their application in dentistry and especially the basis of energy of the beam and wavelength of the emitted oral surgery are rapidly improving today. Lasers are being used as a niche tool as direct replacement for conventional approaches ClassificationGas lasers of lasers [6] CO advantages of lasers are incision of tissues, coagulation during Argon like scalpel, blades, electro surgery, dental hand piece. The specific Liquid Dyes2 canoperation be used and for treatmentpostoperative of conditions benefits likesuch lowas premalignant postoperative lesions, pain, better wound healing. For soft tissue oral surgical procedures lasers Solid -

Supernumerary Teeth in Primary Dentition Associated to Palatal Polyps
Revista Odontológica Mexicana Facultad de Odontología Vol. 17, No. 3 July-September 2013 pp 168-172 CASE REPORT Supernumerary teeth in primary dentition associated to palatal polyps. Case report Dientes supernumerarios en dentición primaria asociados a pólipos palatinos. Reporte de caso Thalia Sánchez Muñoz Ledo,* Alejandro Hinojosa Aguirre,§ Germán Portillo Guerrero,II Fernando Tenorio Rocha¶ ABSTRACT RESUMEN Polyps are rare in children. The present article reports the clinical Los pólipos son poco frecuentes en niños. En este artículo se pre- case of a 14 month old male patient brought for treatment to the senta un caso clínico de un niño de un año dos meses que acude Pedodontics Clinic of the Graduate School, National School of a la Clínica de Odontopediatría de la DEPeI UNAM con dos póli- Dentistry National University of Mexico. He presented two palatal pos fibroepiteliales palatinos ubicados a ambos lados de la papila fibro-epithelial polyps, located at both sides of the incisive papilla. incisiva, 10 días posteriores a la excisión quirúrgica se observó la 10 days after surgical excision, a supernumerary tooth erupted in erupción de un diente supernumerario en el paladar, y 25 días des- the palate. 25 days later, eruption of a second supernumerary tooth pués se observó la erupción de un segundo diente supernumerario. was observed. Both teeth were extracted. Histological diagnosis Ambos dientes fueron extraídos. El diagnóstico histológico de las of palatal lesions was giant fibroblast fibroma. Nevertheless, no lesiones en el paladar fue: fibroma de fibroblastos gigantes; sin -em histological evidence was found to show possible relationship bargo, no se encontró evidencia histológica que mostrara alguna between presence of palatal polyps and supernumerary teeth. -

The Peripheral Giant Cell Granuloma in Edentulous Patients: Report of Three Unique Cases
Published online: 2019-09-30 The Peripheral Giant Cell Granuloma in Edentulous Patients: Report of Three Unique Cases Osman A. Etoza Ahmet Emin Demirbasa Mehmet Bulbulb Ebru Akayc ABSTRACT The peripheral giant cell granuloma (PGCG) is a rare reactive exophytic lesion taking place on the gingiva and alveolar ridge usually as a result of local irritating factors such as trauma, tooth extrac- tion, badly finished fillings, unstable dental prosthesis, plaque, calculus, chronic infections, and im- pacted food. This article presents 3 cases of PGCG that presented at the same location of the edentu- lous mandible of patients that using complete denture for over ten years. (Eur J Dent 2010;4:329-333) Key words: Peripheral giant cell granuloma; Chronic irritation; Edentulous patients; Complete denture. INTRODUCTION Giant cell granuloma lesions (peripheral and teoclastoma, or giant-cell hyperplasia. Etiologic central) are benign, non-odontogenic, moderately factors are not known, although it is thought that rare tumors of the oral cavity. They develop pe- it may be due to an irritant or aggressive factor ripherally (within gingiva) or centrally (in bone).1 such as trauma, tooth extraction, badly finished The peripheral giant cell granuloma (PGCG) is a fillings, unstable dental prosthesis, plaque, calcu- rare reactive exophytic lesion taking place on the lus, chronic infections, or impacted food.2,3 Clini- gingiva and alveolar ridge, also known as a giant- cal appearance of PGCGs can present as polyploi- cell epulis, giant-cell reparative granuloma, os- dy or nodular lesions, primarily bluish red with a smooth shiny or mamillated surface, stalky or 2,4,5 a Erciyes University, Faculty of Dentistry, Department of sessile base, small and well demarcated. -

Pigmented Villonodular Synovitis of the Temporomandibular Joint: a Case Report and the Literature Review
1314 Cai et al. Case Report TMJ Disorders J. Cai1, Z. Cai1, Y. Gao2 1Department of Oral and Maxillofacial Pigmented villonodular synovitis 2 Surgery, Beijing, China; Department of Oral Pathology, Peking University School & of the temporomandibular joint: Hospital of Stomatology, Beijing, China a case report and the literature review J. Cai, Z. Cai, Y. Gao: Pigmented villonodular synovitis of the temporomandibular joint: a case report and the literature review. Int. J. Oral Maxillofac. Surg. 2011; 40: 1314–1322. # 2011 International Association of Oral and Maxillofacial Surgeons. Published by Elsevier Ltd. All rights reserved. Abstract. Pigmented villonodular synovitis (PVNS) is an uncommon benign proliferative disorder of synovium that may involve joints, tendon sheaths, and bursae. It most often affects the knees, and less frequently involves other joints. It presents in the temporomandibular joints (TMJs) extremely rarely. The authors report an elderly female patient with PVNS of the TMJ with skull base extension, who had traumatic history in the same site. It was diagnosed through core-needle Keywords: pigmented villonodular synovitis (PVNS); synovitis; temporomandibular joint biopsy, which was not documented in the literature. Radical excision and follow-up (TMJ). for 7–8 years was recommended because of the reported malignant transformation and high recurrence rate. This case and previously reported cases in the literature are Accepted for publication 2 March 2011 reviewed and discussed. Available online 6 April 2011 The term pigmented villonodular synovi- were reported in detail (Table 1). The visits and mouth-opening for a long time tis (PVNS) was introduced by JAFFE et al. authors present an additional case of during the operation. -

Multiple Large Peripheral Giant Cell Granuloma: a Case Report
CASE REPORT BALIKESİR SAĞLIK BİLİMLERİ DERGİSİ / BALIKESIR HEALTH SCIENCES JOURNAL MULTIPLE LARGE PERIPHERAL GIANT CELL GRANULOMA: A CASE REPORT BÜYÜK BOYUTLARDA MULTİPL PERİFERAL DEV HÜCRELI GRANÜLOM: VAKA RAPORU Mustafa Gümüşok1 Murat Özle2 Begüm Okur2 Anıl Seçkin2 Farid Museyibov3 Özlem Üçok1 Sedat Çetiner2 1Gazi Üniversitesi Diş Hekimliği Fakültesi, ÖZET Ağız, Diş Ve Çene Radyolojisi Anabilim Dalı, Ankara Periferal dev hücreli granülom (PDHG) oral bölgenin sık izlenen dev hücreli bir lezyonudur. 2Gazi Üniversitesi Diş Hekimliği Fakültesi, PDHG’ler gerçek bir neoplazmı temsil etmezler. Etyolojileri çok açık olmayan bu lezyonların, Ağız, Diş Ve Çene Cerrahisi Anabilim Dalı, travma veya lokal irritasyonlara bağlı gelişen reaktif bir lezyon olduğu düşünülmektedir. Ankara PDHG’lere kadınlarda erkeklere oranla daha sık, mandibulada ise maksilladan daha fazla 3 Gazi Üniversitesi Diş Hekimliği Fakültesi, rastlanılır. Gingiva veya dişsiz alveolar kret üzerinde kırmızı, kırmızı-mavi nodüler kitle şeklinde Oral Patoloji Anabilim Dalı, Ankara görülürler. Bu olgu raporunda, 48 yaşında erkek hastada görülen, maksilla sol santral kesici - sağ kanin kesici dişler ve mandibula sağ santral kesici-sol kanin kesici dişler bölgesinde lokalize, Yazışma Adresi: yüzde asimetriye neden olan büyük boyutlu PDHG’ler sunulmuştur. Multipl PDHG vakasının Mustafa Gümüşok radyolojik, klinik, histopatolojik bulguları ile birlikte teşhis, tedavi ve 6 aylık takibi rapor Gazi Üniversitesi Diş Hekimliği Fakültesi Ağız edilmiştir. Diş Ve Çene Radyolojisi Asti Karşısı Emek Ankara Ankara – Türkiye Anahtar Kelimeler: Periferal dev hücreli granülom, mandibula, maksilla, multipl lezyon SUMMARY E posta: [email protected] Peripheral giant cell granuloma (PGCG) is the most common oral giant cell lesion. PGCG Kabul Tarihi: 25 Şubat 2015 presumably does not represent a true neoplasm. PGCG is believed to be stimulated by local irritation or trauma besides the causing of PGCG isn’t known exactly. -
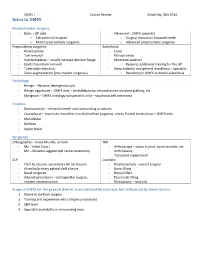
Intro to OMFS
OMFS I Course Review Enoch Ng, DDS 2014 Intro to OMFS Dentoalveolar surgery - Basic – GP able - Advanced – OMFS specialist o Extraction of erupted o Surgical extraction impacted teeth o Minor preprosthetic surgeries o Advanced preprosthetic surgeries Preprosthetic surgeries Anesthesia - Alveoloplasty - Local - Tori removal - Nitrous oxide - Vestibuloplasty – usually increase denture flange - Moderate sedation - Epulis fissuratum removal o Requires additional training for the GP - Tuberosity reduction - Deep sedation and general anesthesia – specialist - Sinus augmentation (pre-implant surgeries) o Residency in OMFS or dental anesthesia Pathology - Benign – fibroma, dentigerous cyst - Benign aggressive – OMFS only – ameloblastoma, reconstruction via bone grafting, etc - Malignant – OMFS oncology subspecialist only – squamous cell carcinoma Trauma - Dentoalveolar – related to teeth and surrounding structures - Craniofacial – trauma to mandible, maxilla/midface (zygoma), orbits, frontal bones/sinus – OMFS only - Mandibular - Midface - Upper facial Surgeries Orthognathic – move Mx, Mn, or both TMJ - Mx – lefort Class I - Arthroscopy – scope in joint, inject steroids, etc - Mn – bilateral saggital split ramus osteotomy - Arthroplasty - Total joint replacement CLP Cosmetic - Cleft lip closure, secondary cleft lip closure - Blepharoplasty – eye lid surgery - Alveolar/primary palatal cleft closure - Brow lifting - Nasal surgeries - Botox/fillers - Adjunct procedures – orthognathic surgery, - Face/neck lifting implant reconstruction - Rhinoplasty