3. Diuretics for Hypertension-A Review and Update
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
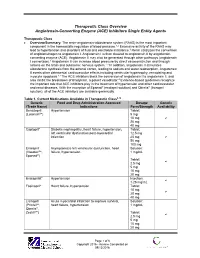
Angiotensin-Converting Enzyme (ACE) Inhibitors Single Entity Agents
Therapeutic Class Overview Angiotensin-Converting Enzyme (ACE) Inhibitors Single Entity Agents Therapeutic Class Overview/Summary: The renin-angiotensin-aldosterone system (RAAS) is the most important component in the homeostatic regulation of blood pressure.1,2 Excessive activity of the RAAS may lead to hypertension and disorders of fluid and electrolyte imbalance.3 Renin catalyzes the conversion of angiotensinogen to angiotensin I. Angiotensin I is then cleaved to angiotensin II by angiotensin- converting enzyme (ACE). Angiotensin II may also be generated through other pathways (angiotensin I convertase).1 Angiotensin II can increase blood pressure by direct vasoconstriction and through actions on the brain and autonomic nervous system.1,3 In addition, angiotensin II stimulates aldosterone synthesis from the adrenal cortex, leading to sodium and water reabsorption. Angiotensin II exerts other detrimental cardiovascular effects including ventricular hypertrophy, remodeling and myocyte apoptosis.1,2 The ACE inhibitors block the conversion of angiotensin I to angiotensin II, and also inhibit the breakdown of bradykinin, a potent vasodilator.4 Evidence-based guidelines recognize the important role that ACE inhibitors play in the treatment of hypertension and other cardiovascular and renal diseases. With the exception of Epaned® (enalapril solution) and Qbrelis® (lisinopril solution), all of the ACE inhibitors are available generically. Table 1. Current Medications Available in Therapeutic Class5-19 Generic Food and Drug Administration -

Summary of Product Characteristics
Sandoz Business use only Page 1 of 9 1.3.1 spc-label-pl - common-spc – 11,006 20191218 (DE/H/1772/001-002-003 – 155347 - validation) TORASEMIDE 100 MG, 200 MG, 50 MG, TABLET 721-6534.01, 721-6535.01, 721-6536.01 SUMMARY OF PRODUCT CHARACTERISTICS 1. NAME OF THE MEDICINAL PRODUCT [Nationally completed name] 50 mg tablets [Nationally completed name] 100 mg tablets [Nationally completed name] 200 mg tablets 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Each tablet contains 50 mg of torasemide. Each tablet contains 100 mg of torasemide. Each tablet contains 200 mg of torasemide. For excipients, see section 6.1 3. PHARMACEUTICAL FORM Tablet. 50 mg tablets: White to off-white round tablet. 100 mg tablets: White to off-white round tablet with break notch. The tablet can be divided into equal doses. 200 mg tablets: White to off-white round tablet with cross break notch on both sides. The tablet can be divided into four equal doses. 4. CLINICAL PARTICULARS 4.1 Therapeutic indications The administration of [Nationally completed name] 50 mg/- 100 mg/- 200 mg tablets is exclusively indicated in patients with highly reduced renal function (creatinine clearance less than 20 ml/min and/or serum creatinine concentration greater than 6 mg/dl). For maintenance of residual diuresis in case of severe renal insufficiency – even on dialysis if there is a considerable residual diuresis (more than 200 ml/24 hours) – if oedemas, effusions and/or hypertension exist. Note: [Nationally completed name] 50 mg/- 100 mg/- 200 mg tablets tablets are to be used only in case of highly impaired and not in normal renal function. -

Diuretics in Clinical Practice. Part I: Mechanisms of Action, Pharmacological Effects and 1
Review Diuretics in clinical practice. Part I: mechanisms of action, pharmacological effects and 1. Introduction clinical indications of diuretic 2. Principles of diuretic action and classification of diuretic compounds compounds † 3. Carbonic anhydrase inhibitors Pantelis A Sarafidis , Panagiotis I Georgianos & Anastasios N Lasaridis Aristotle University of Thessaloniki, AHEPA Hospital, Section of Nephrology and Hypertension, 4. Osmotic diuretics 1st Department of Medicine, Thessaloniki, St. Kiriakidi 1, 54636, Thessaloniki, Greece 5. Loop diuretics 6. Thiazides and thiazide-related Importance of the field: Diuretics are among the most important drugs of our diuretics therapeutic armamentarium and have been broadly used for > 50 years, 7. Potassium-retaining diuretics providing important help towards the treatment of several diseases. Although all diuretics act primarily by impairing sodium reabsorption in the renal 8. Conclusion tubules, they differ in their mechanism and site of action and, therefore, in 9. Expert opinion their specific pharmacological properties and clinical indications. Loop diure- tics are mainly used for oedematous disorders (i.e., cardiac failure, nephrotic syndrome) and for blood pressure and volume control in renal disease; thiazides and related agents are among the most prescribed drugs for hypertension treatment; aldosterone-blockers are traditionally used for primary or secondary aldosteronism; and other diuretic classes have more specific indications. Areas covered in this review: This article discusses the mechanisms of action, pharmacological effects and clinical indications of the various diuretic classes For personal use only. used in everyday clinical practice, with emphasis on recent knowledge sug- gesting beneficial effects of certain diuretics on clinical conditions distinct from the traditional indications of these drugs (i.e., heart protection for aldosterone blockers). -

Diuretic-Induced Hyponatraemia in Elderly Hypertensive Women
Journal of Human Hypertension (2003) 17, 151 & 2003 Nature Publishing Group All rights reserved 0950-9240/03 $25.00 www.nature.com/jhh LETTER TO THE EDITOR Diuretic-induced hyponatraemia in elderly hypertensive women Journal of Human Hypertension there were 10 with plasma so- plasma sodium of 111 mmol/l (2003) 17, 151. doi:10.1038/ dium levels in the range 101– when inadvertently rechallenged sj.jhh.1001513 109 mmol/l. Of the 26, 11 had with thiazides, the agent this time plasma potassium levels less than being hydrochlorothiazide copre- My experience of diuretic- 3.5 mmol/l. The age range was scribed with amiloride. I now induced hyponatraemia in the 74–93 and 22 were women. Hy- utilise torasemide as an adjunc- elderly is in accordance with the drochlorothiazide was the offend- tive diuretic in patients with a observations made by the ing agent in 12 cases, having been previous history of thiazide- authors.1 In my personal series coprescribed with amiloride in induced hyponatraemia. The data of 61 cases of severe hyponatraemia 10 instances, and with triamterene presented here extend the obser- (plasma sodium o120 mmol/l), in two. Bendrofluazide was the vations I published previously on compiled over a period of 18 offending agent in nine instances, this topic. years in patients aged 465, 26 the dose being 2.5 mg/day in were attributable to thiazide seven instances (coprescribed diuretics, culprit drugs in seven with amiloride in one instance), References other cases being frusemide (three and 5.0 mg/day in the other two. 1 Sharabi Y et al. -

Phvwp Monthly Report Mar 2011
24 March 2011 EMA/CHMP/PhVWP/217595/2011 Patient Health Protection Monthly report Issue number: 1103 Pharmacovigilance Working Party (PhVWP) March 2011 plenary meeting The CHMP Pharmacovigilance Working Party (PhVWP) held its March 2011 plenary meeting on 14-16 March 2011. Safety concerns Discussions on non-centrally authorised medicinal products are summarised below in accordance with the PhVWP publication policy. The positions agreed by the PhVWP for non-centrally authorised products form recommendations to Member States. For the publication policy, readers are referred to http://www.ema.europa.eu/docs/en_GB/document_library/Report/2009/10/WC500006181.pdf. The PhVWP also provides advice to the Committee for Medicinal Products for Human Use (CHMP) on centrally authorised products and products subject to ongoing CHMP procedures at the request of the CHMP. For safety updates concerning these products, readers are referred to the CHMP monthly report (http://www.ema.europa.eu, go to: about us/Committees/CHMP/Committees meeting reports). High-ceiling diuretics – Evidence does not confirm risk of basal cell carcinoma Evidence does not confirm a causal association between high-ceiling diuretics and basal cell carcinoma. Following the recent publication of a study showing an increased risk of basal cell carcinoma (BCC) with the use of high-ceiling diuretics, the PhVWP reviewed this possible safety concern1. The PhVWP concluded that the evidence does not confirm a causal association between the use of the high-ceiling diuretics and the development of BCC and that no regulatory action is currently necessary (see Annex 1 for the Summary Assessment Report). 1 The active substances included in this review were bumetanide, etacrynic acid, furosemide, piretanide and torasemide. -

Interaction of the Sympathetic Nervous System with Other Pressor Systems in Antihypertensive Therapy
Journal of Clinical and Basic Cardiology An Independent International Scientific Journal Journal of Clinical and Basic Cardiology 2001; 4 (3), 185-192 Interaction of the Sympathetic Nervous System with other Pressor Systems in Antihypertensive Therapy Wenzel RR, Baumgart D, Bruck H, Erbel R, Heemann U Mitchell A, Philipp Th, Schaefers RF Homepage: www.kup.at/jcbc Online Data Base Search for Authors and Keywords Indexed in Chemical Abstracts EMBASE/Excerpta Medica Krause & Pachernegg GmbH · VERLAG für MEDIZIN und WIRTSCHAFT · A-3003 Gablitz/Austria FOCUS ON SYMPATHETIC TONE Interaction of SNS J Clin Basic Cardiol 2001; 4: 185 Interaction of the Sympathetic Nervous System with Other Pressor Systems in Antihypertensive Therapy R. R. Wenzel1, H. Bruck1, A. Mitchell1, R. F. Schaefers1, D. Baumgart2, R. Erbel2, U. Heemann1, Th. Philipp1 Regulation of blood pressure homeostasis and cardiac function is importantly regulated by the sympathetic nervous system (SNS) and other pressor systems including the renin-angiotensin system (RAS) and the vascular endothelium. Increases in SNS activity increase mortality in patients with hypertension, coronary artery disease and congestive heart failure. This review summarizes some of the interactions between the main pressor systems, ie, the SNS, the RAS and the vascular endothelium including the endothelin-system. Different classes of cardiovascular drugs interfere differently with the SNS and the other pressor systems. Beta-blockers, ACE-inhibitors and diuretics have no major effect on central SNS activity. Pure vasodilators including nitrates, alpha-blockers and DHP-calcium channel blockers increase SNS activity. In contrast, central sympatholytic drugs including moxonidine re- duce SNS activity. The effects of angiotensin-II receptor antagonist on SNS activity in humans are not clear, experimental data are discussed in this review. -

Actual Place of Diuretics in Hypertension Treatment
Mini Review J Cardiol & Cardiovasc Ther Volume 3 Issue 4 - March 2017 Copyright © All rights are reserved by Farouk Abcha DOI: 10.19080/JOCCT.2017.03.555616 Actual Place of Diuretics in Hypertension Treatment Farouk Abcha, Marouane Boukhris*, Zied Ibn Elhadj, Lobna Laroussi, Faouzi Addad, Afef Ben Halima and Salem Kachboura Cardiology Department of Abderrahmen Mami Hospital, University of Tunis El Manar, Tunisia Submission: February 03, 2017; Published: March 07, 2017 *Corresponding author: Marouane Boukhris, Cardiology Department of Abderrahmen Mami Hospital, Ariana, Faculty of Medicine of Tunis, University of Tunis El Manar, Tunisia, Tel: ; Email: Abstract Diuretics represent a large and heterogeneous class of drugs, differing from each other by structure, site and mechanism of action. Diuretics are widely used, and have several indications in different cardiovascular disorders, particularly in hypertension and heart failure. Despite the large number of available anti-hypertensive drugs, diuretics remained a cornerstone of hypertension treatment. In the current editorial, we assessed the actual place of different diuretics in the hypertension guidelines focusing on the concept of tailored approach in prescribing them for hypertensive patients. Keywords: Diuretics; Hypertension; Hydrochlorothiazide; Indapamide; Guidelines Introduction Diuretics represent a large and heterogeneous class of drugs, differing from each other by structure, site and mechanism of action. Diuretics are widely used, and have several indications in different cardiovascular disorders, particularly in hypertension and heart failure. Despite the large number of available anti-hypertensive drugs, diuretics remained a cornerstone of hypertension treatment [1]. Indeed, they are the second most commonly prescribed class of antihypertensive medication. For instance, 12% of US adults were prescribed a diuretic, and the relative increase in prescriptions from 1999 through 2012 was 1.4 [2]. -

Approach to Managing Patients with Sulfa Allergy Use of Antibiotic and Nonantibiotic Sulfonamides
CME Approach to managing patients with sulfa allergy Use of antibiotic and nonantibiotic sulfonamides David Ponka, MD, CCFP(EM) ABSTRACT OBJECTIVE To present an approach to use of sulfonamide-based (sulfa) medications for patients with sulfa allergy and to explore whether sulfa medications are contraindicated for patients who require them but are allergic to them. SOURCES OF INFORMATION A search of current pharmacology textbooks and of MEDLINE from 1966 to the present using the MeSH key words “sulfonamide” and “drug sensitivity” revealed review articles, case reports, one observational study (level II evidence), and reports of consensus opinion (level III evidence). MAIN MESSAGE Cross-reactivity between sulfa antibiotics and nonantibiotics is rare, but on occasion it can affect the pharmacologic and clinical management of patients with sulfa allergy. CONCLUSION How a physician approaches using sulfa medications for patients with sulfa allergy depends on the certainty and severity of the initial allergy, on whether alternatives are available, and on whether the contemplated agent belongs to the same category of sulfa medications (ie, antibiotic or nonantibiotic) as the initial offending agent. RÉSUMÉ OBJECTIF Proposer une façon d’utiliser les médicaments à base de sulfamides (sulfas) chez les patients allergiques aux sulfas et vérifier si ces médicaments sont contre-indiqués pour ces patients. SOURCES DE L’INFORMATION Une consultation des récents ouvrages de pharmacologie et de MEDLINE entre 1966 et aujourd’hui à l’aide des mots clés MeSH «sulfonamide» et «drug sensitivity» a permis de repérer plusieurs articles de revue et études de cas, une étude d’observation et des rapports d’opinion consensuelles (preuves de niveau III). -

Estonian Statistics on Medicines 2016 1/41
Estonian Statistics on Medicines 2016 ATC code ATC group / Active substance (rout of admin.) Quantity sold Unit DDD Unit DDD/1000/ day A ALIMENTARY TRACT AND METABOLISM 167,8985 A01 STOMATOLOGICAL PREPARATIONS 0,0738 A01A STOMATOLOGICAL PREPARATIONS 0,0738 A01AB Antiinfectives and antiseptics for local oral treatment 0,0738 A01AB09 Miconazole (O) 7088 g 0,2 g 0,0738 A01AB12 Hexetidine (O) 1951200 ml A01AB81 Neomycin+ Benzocaine (dental) 30200 pieces A01AB82 Demeclocycline+ Triamcinolone (dental) 680 g A01AC Corticosteroids for local oral treatment A01AC81 Dexamethasone+ Thymol (dental) 3094 ml A01AD Other agents for local oral treatment A01AD80 Lidocaine+ Cetylpyridinium chloride (gingival) 227150 g A01AD81 Lidocaine+ Cetrimide (O) 30900 g A01AD82 Choline salicylate (O) 864720 pieces A01AD83 Lidocaine+ Chamomille extract (O) 370080 g A01AD90 Lidocaine+ Paraformaldehyde (dental) 405 g A02 DRUGS FOR ACID RELATED DISORDERS 47,1312 A02A ANTACIDS 1,0133 Combinations and complexes of aluminium, calcium and A02AD 1,0133 magnesium compounds A02AD81 Aluminium hydroxide+ Magnesium hydroxide (O) 811120 pieces 10 pieces 0,1689 A02AD81 Aluminium hydroxide+ Magnesium hydroxide (O) 3101974 ml 50 ml 0,1292 A02AD83 Calcium carbonate+ Magnesium carbonate (O) 3434232 pieces 10 pieces 0,7152 DRUGS FOR PEPTIC ULCER AND GASTRO- A02B 46,1179 OESOPHAGEAL REFLUX DISEASE (GORD) A02BA H2-receptor antagonists 2,3855 A02BA02 Ranitidine (O) 340327,5 g 0,3 g 2,3624 A02BA02 Ranitidine (P) 3318,25 g 0,3 g 0,0230 A02BC Proton pump inhibitors 43,7324 A02BC01 Omeprazole -

Diuretics for Hypertension
The Rx Files: Q&A Summary March 1998, LDR DIURETICS IN THE TREATMENT OF HYPERTENSION: CURRENT STATUS 1. When are thiazide diuretics considered first line antihypertensives? Antihypertensive therapy should be individualized by choosing agents that have favorable effects on comorbid conditions. The recent JNC VI report1 recommends thiazides (or â Blockers) as first line agents in the treatment of uncomplicated hypertension except where contraindicated, not tolerated, or concurrent medical conditions favor use of alternate agents (see Appendix 1).1 Thiazide diuretics and â Blockers are the only antihypertensives that have been well documented in long-term controlled trials to reduce cardiovascular morbidity and mortality, particularly MI and stroke.2 Current large-scale trials are underway to determine if other classes of antihypertensives have similar benefits. Thiazides are particularly effective in elderly patients with isolated systolic hypertension.1 They also have favorable effects in patients at risk of osteoporosis. When not used for initial monotherapy, addition of a low dose diuretic as the second agent is recommended unless contraindicated.1 2. Are low dose thiazides as effective in treating hypertension as higher doses? Doses as low as 12.5-25mg of hydrochlorothiazide (HCT), given once daily, have been as effective in lowering blood pressure as higher doses.3 In fact, doses above 25mg have little added benefit but greater incidence of adverse effects.3,7 A dose of 6.25mg HCT can often significantly augment the response of other antihypertensives when used in combination. 3. What about the adverse metabolic effects of thiazides? In doses of 25mg or less, incidence of hypokalemia is <5%, and few patients will actually require potassium supplementation or addition of a K+ sparing diuretic. -

PHRP March 2015
March 2015; Vol. 25(2):e2521518 doi: http://dx.doi.org/10.17061/phrp2521518 www.phrp.com.au Research Manual versus automated coding of free-text self-reported medication data in the 45 and Up Study: a validation study Danijela Gnjidica,b,i, Sallie-Anne Pearsona,c, Sarah N Hilmerb,d, Jim Basilakise, Andrea L Schaffera, Fiona M Blythb,f,g and Emily Banksg,h, on behalf of the High Risk Prescribing Investigators a Faculty of Pharmacy, University of Sydney, NSW, Australia b Sydney Medical School, University of Sydney, NSW, Australia c Sydney School of Public Health, University of Sydney, NSW, Australia d Royal North Shore Hospital and Kolling Institute of Medical Research, Sydney, NSW, Australia e School of Computing, Engineering and Mathematics, University of Western Sydney, NSW, Australia f Centre for Education and Research on Ageing (CERA), Concord Hospital, Sydney, NSW, Australia g The Sax Institute, Sydney, NSW, Australia h National Centre for Epidemiology and Population Health, Australian National University, Canberra, ACT i Corresponding author: [email protected] Article history Abstract Publication date: March 2015 Background: Increasingly, automated methods are being used to code free- Citation: Gnjidic D, Pearson S, Hilmer S, text medication data, but evidence on the validity of these methods is limited. Basilakis J, Schaffer AL, Blyth FM, Banks E. To examine the accuracy of automated coding of previously keyed Manual versus automated coding of free-text Aim: in free-text medication data compared with manual coding of original self-reported medication data in the 45 and Up Study: a validation study. Public Health handwritten free-text responses (the ‘gold standard’). -

Efficacy of Indapamide 1.5 Mg, Sustained Release, in the Lowering of Systolic Blood Pressure
Journal of Human Hypertension (2004) 18, S9–S14 & 2004 Nature Publishing Group All rights reserved 0950-9240/04 $30.00 www.nature.com/jhh ORIGINAL ARTICLE Efficacy of indapamide 1.5 mg, sustained release, in the lowering of systolic blood pressure GM London Service de ne´phrologie, Hoˆpital Manhe`s, Ste Genevie`ve des Bois, France The relationship between the increase in blood pressure indapamide SR resulted in a better or equivalent control and the incidence of cardiovascular disease is well of SBP than treatment with a standard dose of a true recognized today. Studies have shown that more thiazide diuretic (hydrochlorothiazide), a calcium chan- attention should be paid to systolic blood pressure nel blocker (amlodipine), and an angiotensin-converting (SBP) in relation to cardiovascular risk and that enzyme inhibitor (enalapril). No therapeutic escape was therapeutic interventions should preferably focus on observed. All treatments showed good acceptability reducing SBP. The antihypertensive efficacy of indapa- with no unexpected adverse event. In conclusion, mide 1.5 mg sustained release (indapamide SR), a low- indapamide SR is very effective in lowering SBP—a dose thiazide-type diuretic, was assessed on SBP. Three major independent cardiovascular risk factor—notably randomized, double-blind, controlled studies were con- in hypertensive high-risk patients with LVH, the elderly ducted with indapamide SR, over a period of 3 to 12 and diabetics, when compared to major antihyperten- months. Elderly patients or patients with target-organ sive treatments. This SBP-lowering effect is maintained damage, hypertension and left ventricular hypertrophy over the long term. (LVH) (LIVE study) or with type II diabetes with micro- Journal of Human Hypertension (2004) 18, S9–S14.