CASE REPORT Intradermal Nevus of the External Auditory Canal
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Clinical Features of Benign Tumors of the External Auditory Canal According to Pathology
Central Annals of Otolaryngology and Rhinology Research Article *Corresponding author Jae-Jun Song, Department of Otorhinolaryngology – Head and Neck Surgery, Korea University College of Clinical Features of Benign Medicine, 148 Gurodong-ro, Guro-gu, Seoul, 152-703, South Korea, Tel: 82-2-2626-3191; Fax: 82-2-868-0475; Tumors of the External Auditory Email: Submitted: 31 March 2017 Accepted: 20 April 2017 Canal According to Pathology Published: 21 April 2017 ISSN: 2379-948X Jeong-Rok Kim, HwibinIm, Sung Won Chae, and Jae-Jun Song* Copyright Department of Otorhinolaryngology-Head and Neck Surgery, Korea University College © 2017 Song et al. of Medicine, South Korea OPEN ACCESS Abstract Keywords Background and Objectives: Benign tumors of the external auditory canal (EAC) • External auditory canal are rare among head and neck tumors. The aim of this study was to analyze the clinical • Benign tumor features of patients who underwent surgery for an EAC mass confirmed as a benign • Surgical excision lesion. • Recurrence • Infection Methods: This retrospective study involved 53 patients with external auditory tumors who received surgical treatment at Korea University, Guro Hospital. Medical records and evaluations over a 10-year period were examined for clinical characteristics and pathologic diagnoses. Results: The most common pathologic diagnoses were nevus (40%), osteoma (13%), and cholesteatoma (13%). Among the five pathologic subgroups based on the origin organ of the tumor, the most prevalent pathologic subgroup was the skin lesion (47%), followed by the epithelial lesion (26%), and the bony lesion (13%). No significant differences were found in recurrence rate, recurrence duration, sex, or affected side between pathologic diagnoses. -

Bone and Soft Tissue Tumors Have Been Treated Separately
EPIDEMIOLOGY z Sarcomas are rare tumors compared to other BONE AND SOFT malignancies: 8,700 new sarcomas in 2001, with TISSUE TUMORS 4,400 deaths. z The incidence of sarcomas is around 3-4/100,000. z Slight male predominance (with some subtypes more common in women). z Majority of soft tissue tumors affect older adults, but important sub-groups occur predominantly or exclusively in children. z Incidence of benign soft tissue tumors not known, but Fabrizio Remotti MD probably outnumber malignant tumors 100:1. BONE AND SOFT TISSUE SOFT TISSUE TUMORS TUMORS z Traditionally bone and soft tissue tumors have been treated separately. z This separation will be maintained in the following presentation. z Soft tissue sarcomas will be treated first and the sarcomas of bone will follow. Nowhere in the picture….. DEFINITION Histological z Soft tissue pathology deals with tumors of the classification connective tissues. of soft tissue z The concept of soft tissue is understood broadly to tumors include non-osseous tumors of extremities, trunk wall, retroperitoneum and mediastinum, and head & neck. z Excluded (with a few exceptions) are organ specific tumors. 1 Histological ETIOLOGY classification of soft tissue tumors tumors z Oncogenic viruses introduce new genomic material in the cell, which encode for oncogenic proteins that disrupt the regulation of cellular proliferation. z Two DNA viruses have been linked to soft tissue sarcomas: – Human herpes virus 8 (HHV8) linked to Kaposi’s sarcoma – Epstein-Barr virus (EBV) linked to subtypes of leiomyosarcoma z In both instances the connection between viral infection and sarcoma is more common in immunosuppressed hosts. -

Acral Compound Nevus SJ Yun S Korea
University of Pennsylvania, Founded by Ben Franklin in 1740 Disclosures Consultant for Myriad Genetics and for SciBase (might try to sell you a book, as well) Multidimensional Pathway Classification of Melanocytic Tumors WHO 4th Edition, 2018 Epidemiologic, Clinical, Histologic and Genomic Aspects of Melanoma David E. Elder, MB ChB, FRCPA University of Pennsylvania, Philadelphia, PA, USA Napa, May, 2018 3rd Edition, 2006 Malignant Melanoma • A malignant tumor of melanocytes • Not all melanomas are the same – variation in: – Epidemiology – risk factors, populations – Cell/Site of origin – Precursors – Clinical morphology – Microscopic morphology – Simulants – Genomic abnormalities Incidence of Melanoma D.M. Parkin et al. CSD/Site-Related Classification • Bastian’s CSD/Site-Related Classification (Taxonomy) of Melanoma – “The guiding principles for distinguishing taxa are genetic alterations that arise early during progression; clinical or histologic features of the primary tumor; characteristics of the host, such as age of onset, ethnicity, and skin type; and the role of environmental factors such as UV radiation.” Bastian 2015 Epithelium associated Site High UV Low UV Glabrous Mucosa Benign Acquired Spitz nevus nevus Atypical Dysplastic Spitz Borderline nevus tumor High Desmopl. Low-CSD Spitzoid Acral Mucosal Malignant CSD melanoma melanoma melanoma melanoma melanoma 105 Point mutations 103 Structural Rearrangements 2018 WHO Classification of Melanoma • Integrates Epidemiologic, Genomic, Clinical and Histopathologic Features • Assists -
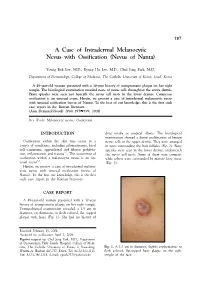
A Case of Intradermal Melanocytic Nevus with Ossification (Nevus of Nanta)
197 A Case of Intradermal Melanocytic Nevus with Ossification (Nevus of Nanta) Young Bok Lee, M.D., Kyung Ho Lee, M.D., Chul Jong Park, M.D. Department of Dermatology, College of Medicine, The Catholic University of Korea, Seoul, Korea A 49-year-old woman presented with a 30-year history of asymptomatic plaque on her right temple. The histological examination revealed nests of nevus cells throughout the entire dermis. Bony spicules were seen just beneath the nevus cell nests in the lower dermis. Cutaneous ossification is an unusual event. Herein, we present a case of intradermal melanocytic nevus with unusual ossification (nevus of Nanta). To the best of our knowledge, this is the first such case report in the Korean literature. (Ann Dermatol (Seoul) 20(4) 197∼199, 2008) Key Words: Melanocytic nevus, Ossification INTRODUCTION drug intake or medical illness. The histological examination showed a dense proliferation of benign Ossification within the skin may occur in a nevus cells in the upper dermis. They were arranged variety of conditions, including pilomatricoma, basal in nests surrounding the hair follicles (Fig. 2). Bony cell carcinoma, appendageal and fibrous prolifera- spicules were seen in the lower dermis, underneath 1,2 tion, inflammation and trauma . The occurrence of the nevus cell nests. Some of them were compact ossification within a melanocytic nevus is an un- while others were surrounded by mature fatty tissue 3-5 usual event . (Fig. 3). Herein, we present a case of intradermal melano- cytic nevus with unusual ossification (nevus of Nanta). To the best our knowledge, this is the first such case report in the Korean literature. -

Case Report of Giant Congenital Melanocytic Nevus
PEDIATRIC DERMATOLOGY Series Editor: Camila K. Janniger, MD Bathing Trunks Nevus: Case Report of Giant Congenital Melanocytic Nevus Ronald Russ, DO; Lisa Light, MS-IV Bathing trunks nevi, a subtype of giant congeni- 34 years. All maternal and prenatal history was unre- tal melanocytic nevi (CMN), are skin tumors that markable. Upon initial physical examination as a new- present by 2 years of age and occur in a low born (1 hour following delivery), the infant had a large percentage of all births. We report a case of (≥5% body surface area), circumferentially pigmented bathing trunks nevus that was initially suspected area from the umbilicus to mid thigh bilaterally to be melanoma, and describe the history, patho- (Figure 1). Interposed darkened lesions were pres- physiology, and treatment options for CMN. We ent, with 3 distinct, raised, lipomatous-type nodules also discuss the risk for neurocutaneous melano- (2 cm, 1.3 cm, and 3 cm in diameter from left to right) sis (NCM), which is a rare syndrome in patients over the lower lumbar spine (Figure 2). There were no with giant CMN. signs of jaundice, hemolysis, meningomyelocele, or Cutis. 2009;83:69-72. abnormal hair growth. The rest of the physical exami- nation was unremarkable, including cardiovascular, pulmonary, and abdominal systems, and genitourinary athing trunks nevus is a specific subtype of functioning was normal. Cord blood testing revealed giant congenital melanocytic nevus (CMN) A Rh-positive blood type, and a direct Coombs test B with spread resembling bathing trunks. This was negative for antibodies. Complete blood cell rare variant is clinically significant because of the count was within reference range, with the excep- increased risk for progression to melanoma and its tion of a low platelet count of 2343103/µL (reference association with neurocutaneous melanosis (NCM).1 range, 250–4503103/µL). -

Acral Melanoma Toshiaki Saida, Hiroshi Koga, Yoriko Yamazaki, Masaru Tanaka IV.2
Chapter IV.2 Acral Melanoma Toshiaki Saida, Hiroshi Koga, Yoriko Yamazaki, Masaru Tanaka IV.2 Contents thickness, biological behavior is not different among the four histogenetic types [16]. More- IV.2.1 Definition . .196 over, cutaneous melanomas not infrequently IV.2 IV.2.2 Clinical Features . .197 show overlapping histopathological features of IV2.3 Dermoscopic Criteria. 198 the four types [36]. Ackerman repeatedly criti- cized the validity of the Clark’s classification IV.2.4 Relevant Clinical Differential and proposed the unifying concept of melano- Diagnosis. 198 ma [1]. IV.2.5 Histopathology. .199 Recently, Bastian and co-workers defined ac- ral melanoma as melanoma occurring on the IV.2.6 Management. .200 non-hair-bearing skin of the palms or soles or IV.2.7 Case Study. .200 under the nails and found that this type of mel- References. .202 anoma was unique in frequent amplifications of chromosomes 5p15, 5p13, 11q13, and 12q14 [4, 7]. Particularly, amplification of 11q13 was de- tected in ~50% of this type of melanoma. Cyclin D1 is the most important candidate gene located in this chromosome region. It is noteworthy IV.2.1 Definition that 5 of 36 acral melanomas defined by Bastian and co-workers were superficial spreading mel- Acral melanoma is a melanoma that affects ac- anoma according to Clark’s classification [7]. ral areas of the skin, which is the most prevalent Another characteristic of acral melanoma is site of melanoma in non-Caucasians [5, 10]. very low rate of mutation of the BRAF onco- Strictly speaking, acral lentiginous melanoma is gene, which is commonly found in superficial not a synonym for acral melanoma. -

Congenital Melanocytic Nevus
BCCH Pediatric Dermatology Clinic Joseph M Lam, MD CONGENITAL MELANOCYTIC NEVUS What is a congenital melanocytic nevus? A "congenital melanocytic nevus" (aka mole) is the name for a common brown birthmark which is made up of special pigment-producing cells. The size of the birthmark may range from a small 1 cm mark to a giant birthmark covering half of the body or more. How common are congenital melanocytic nevus? Small congenital pigmented moles (brown birthmarks) are seen in 1 percent of all healthy newborn babies. Giant congenital moles (larger than 8 inches) are rare, found in fewer than one in 20,000 newborn infants. Why are they special? Small- and medium-sized congenital moles may rarely develop melanoma, a worrisome form of skin cancer. However, the risk of this happening is less than 1% and in adults, the risk of developing skin cancer in any area of the skin is much higher than the risk of melanoma in a small or medium-sized congenital mole. However, depending upon the appearance of the mole, its location and the ease of removal, we may suggest that the mole be taken out or we may recommend keeping the mole and just paying attention to any changes in the mole. Rarely, mole cells can be present in the brain - this happens in patients with many ‘satellite’ moles. If this causes problems, the problems usually show up in the first few months of life. It is important to inspect congenital moles on a regular basis at home. We may also recommend that some moles be observed in the office with pictures. -

Basal Cell Carcinoma Associated with Non-Neoplastic Cutaneous Conditions: a Comprehensive Review
Volume 27 Number 2| February 2021 Dermatology Online Journal || Review 27(2):1 Basal cell carcinoma associated with non-neoplastic cutaneous conditions: a comprehensive review Philip R Cohen MD1,2 Affiliations: 1San Diego Family Dermatology, National City, California, USA, 2Touro University California College of Osteopathic Medicine, Vallejo, California, USA Corresponding Author: Philip R Cohen, 10991 Twinleaf Court, San Diego, CA 92131-3643, Email: [email protected] pathogenesis of BCC is associated with the Abstract hedgehog signaling pathway and mutations in the Basal cell carcinoma (BCC) can be a component of a patched homologue 1 (PCTH-1) transmembrane collision tumor in which the skin cancer is present at tumor-suppressing protein [2-4]. Several potential the same cutaneous site as either a benign tumor or risk factors influence the development of BCC a malignant neoplasm. However, BCC can also concurrently occur at the same skin location as a non- including exposure to ultraviolet radiation, genetic neoplastic cutaneous condition. These include predisposition, genodermatoses, immunosuppression, autoimmune diseases (vitiligo), cutaneous disorders and trauma [5]. (Darier disease), dermal conditions (granuloma Basal cell carcinoma usually presents as an isolated faciale), dermal depositions (amyloid, calcinosis cutis, cutaneous focal mucinosis, osteoma cutis, and tumor on sun-exposed skin [6-9]. However, they can tattoo), dermatitis, miscellaneous conditions occur as collision tumors—referred to as BCC- (rhinophyma, sarcoidal reaction, and varicose veins), associated multiple skin neoplasms at one site scars, surgical sites, systemic diseases (sarcoidosis), (MUSK IN A NEST)—in which either a benign and/or systemic infections (leischmaniasis, leprosy and malignant neoplasm is associated with the BCC at lupus vulgaris), and ulcers. -

Lumps & Bumps: Approach to Common Dermatologic Neoplasms
Case-Based Approach to Common Dermatologic Neoplasms Patrick Retterbush, MD, FAAD Mohs Surgery & Dermatologic Oncology Associate Member of the American College of Mohs Surgery Private Practice: Lockman Dermatology January 27th 2018 Disclosure of Relevant Financial Relationships • I do not have any relevant financial relationships, commercial interests, and/or conflicts of interest regarding the content of this presentation. Goals/Objectives • Recognize common benign growths • Recognize common malignant growths • Useful clues & examination for evaluating melanocytic nevi and when to be concerned for melanoma/atypical moles • How to perform a basic skin biopsy and which method/type to choose • Basic treatment/when to refer Key Questions & Physical Examination Findings for a Growth History Physical Examination • How long has the lesion been • Describing a growth present? – flat or raised? • flat – macule (<1cm) or patch (>1cm) – years, months, weeks • raised – papule (<1cm) or plaque (>1cm) – nodule if deep (majority of lesion in • Has it changed? dermis/SQ) – Size – secondary descriptive features • scaly (hyperkeratosis, retention of strateum – Shape corneum) – Color • crusty (dried serum, blood, or pus on surface) • eroded or ulcerated (partial vs. full thickness – Symptoms – pain, bleeding, itch? epidermal loss) – Over what time frame? • color (skin colored, red, pigmented, pearly) • feel (hard or soft, mobile or fixed) • PMH: • size: i.e. 6 x 4mm – prior skin cancers • Look at the rest of the skin/region of skin • SCC/BCCs vs. melanoma -

Osteoid Osteoma and Your Everyday Practice
n Review Article Instructions 1. Review the stated learning objectives at the beginning cme ARTICLE of the CME article and determine if these objectives match your individual learning needs. 2. Read the article carefully. Do not neglect the tables and other illustrative materials, as they have been selected to enhance your knowledge and understanding. 3. The following quiz questions have been designed to provide a useful link between the CME article in the issue Osteoid Osteoma and your everyday practice. Read each question, choose the correct answer, and record your answer on the CME Registration Form at the end of the quiz. Petros J. Boscainos, MD, FRCSEd; Gerard R. Cousins, MBChB, BSc(MedSci), MRCS; 4. Type or print your full name and address and your date of birth in the space provided on the CME Registration Form. Rajiv Kulshreshtha, MBBS, MRCS; T. Barry Oliver, MBChB, MRCP, FRCR; 5. Indicate the total time spent on the activity (reading article and completing quiz). Forms and quizzes cannot be Panayiotis J. Papagelopoulos, MD, DSc processed if this section is incomplete. All participants are required by the accreditation agency to attest to the time spent completing the activity. educational objectives 6. Complete the Evaluation portion of the CME Regi stration Form. Forms and quizzes cannot be processed if the Evaluation As a result of reading this article, physicians should be able to: portion is incomplete. The Evaluation portion of the CME Registration Form will be separated from the quiz upon receipt at ORTHOPEDICS. Your evaluation of this activity will in no way affect educational1. -

Congenital Melanocytic Nevi and the Risk of Malignant Melanoma: Establishing a Guideline for Primary-Care Physicians
4MEDICAL REVIEWS Congenital Melanocytic Nevi and the Risk of Malignant Melanoma: Establishing a Guideline for Primary-Care Physicians Jeremy Nikfarjam, MD1, and Earle Chambers, MPH, PhD2 1Department of Surgery, Division of Plastic & Reconstructive Surgery, Montefiore Medical Center, Bronx, NY; 2Department of Family and Social Medicine, Department of Epidemiology & Population Health, Albert Einstein College of Medicine, Bronx, NY Objective: The objective of this review is to determine what formation from small CMN was determined to be 20.9 by his- size congenital melanocytic nevi (CMN) increases the risk of tory and 10.5 by histology in 238 patients in the case-control malignant melanoma in affected patients. study selected. No malignant transformation was found in a prospective study of 230 individuals with medium-sized mela- Background: Congenital melanocytic nevi are benign prolif- nocytic nevi. Finally, a 5% risk of malignant transformation erations of cutaneous melanocytes apparent at birth or in the was reported in a prospective study of patients with large con- first postnatal weeks. The Kopf system classifies nevi based genital nevi. on size: small, <1.5 cm in diameter; medium, 1.5–19.9 cm in diameter, and large, ≥20 cm in diameter. Great variability Conclusion: All patients should receive total body skin and exists in quantifying the risk of malignant transformation from mucosal surface exams. Patients with small CMN (<1.5 cm in congenital nevi of different sizes. Evidence-based standard diameter) and medium CMN (≥1.5 cm–19.9 cm in diameter) guidelines for clinical investigation need to be established. should be closely observed over their lifetimes and given the option of specialist referral. -

Basal Cell Carcinoma with Osteoma Cutis
Open Access Case Report DOI: 10.7759/cureus.3170 Basal Cell Carcinoma with Osteoma Cutis Stella X. Chen 1 , Philip R. Cohen 2 1. School of Medicine, University of California, San Diego 2. Dermatologist, San Diego Family Dermatology, San Diego, USA Corresponding author: Stella X. Chen, [email protected] Abstract Osteoma cutis is the formation of bone within the skin. It can present as either primary osteoma cutis or secondary osteoma cutis. Secondary osteoma cutis is more common and is associated with inflammatory, infectious, and neoplastic disorders, including basal cell carcinoma. A 79-year-old Caucasian man without underlying kidney disease or calcium abnormalities presented with a basal cell carcinoma with osteoma cutis on the chin. Basal cell carcinoma with osteoma cutis has seldom been described; however, the occurrence of this phenomenon may be more common than suggested by the currently published literature. The preferred treatment is surgical excision—with or without using Mohs micrographic technique. When the histopathologic examination reveals bone formation in the skin, clinicians should consider the possible presence of an adjacent malignancy, such as a basal cell carcinoma. Categories: Dermatology, Oncology Keywords: basal, bone, calcium, calcinosis, carcinoma, cell, cutis, ossification, osteoma Introduction Basal cell carcinoma is the most common type of skin cancer. Osteoma cutis is the formation of bone within the skin; it can occur either as a distinct cutaneous entity or associated with other conditions. In primary osteoma cutis, idiopathic ossification occurs and can be congenital, acquired, or related to Albright’s hereditary osteodystrophy and fibrodysplasia ossificans progressiva. Secondary osteoma cutis is more commonly seen and may be associated with infectious, inflammatory, or neoplastic disorders, including basal cell carcinoma.