GOPC-ROS1 Fusion Due to Microdeletion at 6Q22 Is an Oncogenic Driver in a Subset of Pediatric Gliomas And
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Propranolol-Mediated Attenuation of MMP-9 Excretion in Infants with Hemangiomas
Supplementary Online Content Thaivalappil S, Bauman N, Saieg A, Movius E, Brown KJ, Preciado D. Propranolol-mediated attenuation of MMP-9 excretion in infants with hemangiomas. JAMA Otolaryngol Head Neck Surg. doi:10.1001/jamaoto.2013.4773 eTable. List of All of the Proteins Identified by Proteomics This supplementary material has been provided by the authors to give readers additional information about their work. © 2013 American Medical Association. All rights reserved. Downloaded From: https://jamanetwork.com/ on 10/01/2021 eTable. List of All of the Proteins Identified by Proteomics Protein Name Prop 12 mo/4 Pred 12 mo/4 Δ Prop to Pred mo mo Myeloperoxidase OS=Homo sapiens GN=MPO 26.00 143.00 ‐117.00 Lactotransferrin OS=Homo sapiens GN=LTF 114.00 205.50 ‐91.50 Matrix metalloproteinase‐9 OS=Homo sapiens GN=MMP9 5.00 36.00 ‐31.00 Neutrophil elastase OS=Homo sapiens GN=ELANE 24.00 48.00 ‐24.00 Bleomycin hydrolase OS=Homo sapiens GN=BLMH 3.00 25.00 ‐22.00 CAP7_HUMAN Azurocidin OS=Homo sapiens GN=AZU1 PE=1 SV=3 4.00 26.00 ‐22.00 S10A8_HUMAN Protein S100‐A8 OS=Homo sapiens GN=S100A8 PE=1 14.67 30.50 ‐15.83 SV=1 IL1F9_HUMAN Interleukin‐1 family member 9 OS=Homo sapiens 1.00 15.00 ‐14.00 GN=IL1F9 PE=1 SV=1 MUC5B_HUMAN Mucin‐5B OS=Homo sapiens GN=MUC5B PE=1 SV=3 2.00 14.00 ‐12.00 MUC4_HUMAN Mucin‐4 OS=Homo sapiens GN=MUC4 PE=1 SV=3 1.00 12.00 ‐11.00 HRG_HUMAN Histidine‐rich glycoprotein OS=Homo sapiens GN=HRG 1.00 12.00 ‐11.00 PE=1 SV=1 TKT_HUMAN Transketolase OS=Homo sapiens GN=TKT PE=1 SV=3 17.00 28.00 ‐11.00 CATG_HUMAN Cathepsin G OS=Homo -

A Computational Approach for Defining a Signature of Β-Cell Golgi Stress in Diabetes Mellitus
Page 1 of 781 Diabetes A Computational Approach for Defining a Signature of β-Cell Golgi Stress in Diabetes Mellitus Robert N. Bone1,6,7, Olufunmilola Oyebamiji2, Sayali Talware2, Sharmila Selvaraj2, Preethi Krishnan3,6, Farooq Syed1,6,7, Huanmei Wu2, Carmella Evans-Molina 1,3,4,5,6,7,8* Departments of 1Pediatrics, 3Medicine, 4Anatomy, Cell Biology & Physiology, 5Biochemistry & Molecular Biology, the 6Center for Diabetes & Metabolic Diseases, and the 7Herman B. Wells Center for Pediatric Research, Indiana University School of Medicine, Indianapolis, IN 46202; 2Department of BioHealth Informatics, Indiana University-Purdue University Indianapolis, Indianapolis, IN, 46202; 8Roudebush VA Medical Center, Indianapolis, IN 46202. *Corresponding Author(s): Carmella Evans-Molina, MD, PhD ([email protected]) Indiana University School of Medicine, 635 Barnhill Drive, MS 2031A, Indianapolis, IN 46202, Telephone: (317) 274-4145, Fax (317) 274-4107 Running Title: Golgi Stress Response in Diabetes Word Count: 4358 Number of Figures: 6 Keywords: Golgi apparatus stress, Islets, β cell, Type 1 diabetes, Type 2 diabetes 1 Diabetes Publish Ahead of Print, published online August 20, 2020 Diabetes Page 2 of 781 ABSTRACT The Golgi apparatus (GA) is an important site of insulin processing and granule maturation, but whether GA organelle dysfunction and GA stress are present in the diabetic β-cell has not been tested. We utilized an informatics-based approach to develop a transcriptional signature of β-cell GA stress using existing RNA sequencing and microarray datasets generated using human islets from donors with diabetes and islets where type 1(T1D) and type 2 diabetes (T2D) had been modeled ex vivo. To narrow our results to GA-specific genes, we applied a filter set of 1,030 genes accepted as GA associated. -

1 Supporting Information for a Microrna Network Regulates
Supporting Information for A microRNA Network Regulates Expression and Biosynthesis of CFTR and CFTR-ΔF508 Shyam Ramachandrana,b, Philip H. Karpc, Peng Jiangc, Lynda S. Ostedgaardc, Amy E. Walza, John T. Fishere, Shaf Keshavjeeh, Kim A. Lennoxi, Ashley M. Jacobii, Scott D. Rosei, Mark A. Behlkei, Michael J. Welshb,c,d,g, Yi Xingb,c,f, Paul B. McCray Jr.a,b,c Author Affiliations: Department of Pediatricsa, Interdisciplinary Program in Geneticsb, Departments of Internal Medicinec, Molecular Physiology and Biophysicsd, Anatomy and Cell Biologye, Biomedical Engineeringf, Howard Hughes Medical Instituteg, Carver College of Medicine, University of Iowa, Iowa City, IA-52242 Division of Thoracic Surgeryh, Toronto General Hospital, University Health Network, University of Toronto, Toronto, Canada-M5G 2C4 Integrated DNA Technologiesi, Coralville, IA-52241 To whom correspondence should be addressed: Email: [email protected] (M.J.W.); yi- [email protected] (Y.X.); Email: [email protected] (P.B.M.) This PDF file includes: Materials and Methods References Fig. S1. miR-138 regulates SIN3A in a dose-dependent and site-specific manner. Fig. S2. miR-138 regulates endogenous SIN3A protein expression. Fig. S3. miR-138 regulates endogenous CFTR protein expression in Calu-3 cells. Fig. S4. miR-138 regulates endogenous CFTR protein expression in primary human airway epithelia. Fig. S5. miR-138 regulates CFTR expression in HeLa cells. Fig. S6. miR-138 regulates CFTR expression in HEK293T cells. Fig. S7. HeLa cells exhibit CFTR channel activity. Fig. S8. miR-138 improves CFTR processing. Fig. S9. miR-138 improves CFTR-ΔF508 processing. Fig. S10. SIN3A inhibition yields partial rescue of Cl- transport in CF epithelia. -

Analysis of the Indacaterol-Regulated Transcriptome in Human Airway
Supplemental material to this article can be found at: http://jpet.aspetjournals.org/content/suppl/2018/04/13/jpet.118.249292.DC1 1521-0103/366/1/220–236$35.00 https://doi.org/10.1124/jpet.118.249292 THE JOURNAL OF PHARMACOLOGY AND EXPERIMENTAL THERAPEUTICS J Pharmacol Exp Ther 366:220–236, July 2018 Copyright ª 2018 by The American Society for Pharmacology and Experimental Therapeutics Analysis of the Indacaterol-Regulated Transcriptome in Human Airway Epithelial Cells Implicates Gene Expression Changes in the s Adverse and Therapeutic Effects of b2-Adrenoceptor Agonists Dong Yan, Omar Hamed, Taruna Joshi,1 Mahmoud M. Mostafa, Kyla C. Jamieson, Radhika Joshi, Robert Newton, and Mark A. Giembycz Departments of Physiology and Pharmacology (D.Y., O.H., T.J., K.C.J., R.J., M.A.G.) and Cell Biology and Anatomy (M.M.M., R.N.), Snyder Institute for Chronic Diseases, Cumming School of Medicine, University of Calgary, Calgary, Alberta, Canada Received March 22, 2018; accepted April 11, 2018 Downloaded from ABSTRACT The contribution of gene expression changes to the adverse and activity, and positive regulation of neutrophil chemotaxis. The therapeutic effects of b2-adrenoceptor agonists in asthma was general enriched GO term extracellular space was also associ- investigated using human airway epithelial cells as a therapeu- ated with indacaterol-induced genes, and many of those, in- tically relevant target. Operational model-fitting established that cluding CRISPLD2, DMBT1, GAS1, and SOCS3, have putative jpet.aspetjournals.org the long-acting b2-adrenoceptor agonists (LABA) indacaterol, anti-inflammatory, antibacterial, and/or antiviral activity. Numer- salmeterol, formoterol, and picumeterol were full agonists on ous indacaterol-regulated genes were also induced or repressed BEAS-2B cells transfected with a cAMP-response element in BEAS-2B cells and human primary bronchial epithelial cells by reporter but differed in efficacy (indacaterol $ formoterol . -

Comparative Transcriptome Profiling of Selected Osmotic Regulatory Proteins in the Gill During Seawater Acclimation of Chum Salm
www.nature.com/scientificreports OPEN Comparative transcriptome profling of selected osmotic regulatory proteins in the gill during seawater acclimation of chum salmon (Oncorhynchus keta) fry Sang Yoon Lee 1, Hwa Jin Lee2 & Yi Kyung Kim1,2* Salmonid fshes, chum salmon (Oncorhynchus keta) have the developed adaptive strategy to withstand wide salinity changes from the early life stage. This study investigated gene expression patterns of cell membrane proteins in the gill of chum salmon fry on the transcriptome level by tracking the salinity acclimation of the fsh in changing environments ranging from freshwater (0 ppt) to brackish water (17.5 ppt) to seawater (35 ppt). Using GO analysis of DEGs, the known osmoregulatory genes and their functional groups such as ion transport, transmembrane transporter activity and metal ion binding were identifed. The expression patterns of membrane protein genes, including pump-mediated protein (NKA, CFTR), carrier-mediated protein (NKCC, NHE3) and channel-mediated protein (AQP) were similar to those of other salmonid fshes in the smolt or adult stages. Based on the protein-protein interaction analysis between transmembrane proteins and other related genes, we identifed osmotic-related genes expressed with salinity changes and analyzed their expression patterns. The fndings of this study may facilitate the disentangling of the genetic basis of chum salmon and better able an understanding of the osmophysiology of the species. Salinity is one of the critical factors limiting the distribution patterns of all aquatic organisms1–4. Salmonid fshes display diverse life-history traits; anadromous individuals that mature in the river from hatching through to juveniles acquire the capacity to tolerate salinity associated with parr–smolt transformation and undergo ocean migrations before returning to rivers for spawning, whereas landlocked types spend their entire life within fresh- water5,6. -

GOPC-ROS1, Active
Catalog # Aliquot Size R14-19BG -05 5 µg R14-19BG -10 10 µg GOPC-ROS1, Active Human recombinant protein expressed in Sf9 cells Catalog # R14-19BG Lot # G1415 -3 Product Description Specific Activity Recombinant human fusion protein GOPC (1-419)-ROS1 240,000 (1881-end) was expressed by baculovirus in Sf9 insect cells using an N-terminal GST tag. The GOPC gene accession 180,000 number is NM_020399 and ROS1’s one is NM_002944 . 120,000 Gene Aliases 60,000 GOPC: CAL; dJ94G16.2; FIG; GOPC1; PIST (cpm) Activity ROS1: c-ros-1; MCF3; ROS 0 0 20 40 60 80 Formulation Protein (ng) The specific activity of GOPC-ROS1 was determined to be 210 Recombinant protein stored in 50mM sodium phosphate, nmol /min/mg as per activity assay protocol. pH 7.0, 300mM NaCl, 150mM imidazole, 0.1mM PMSF, 0.25mM DTT, 25% glycerol. Purity Storage and Stability Store product at –70 oC. For optimal storage, aliquot target into smaller quantities after centrifugation and store at recommended temperature. For most favorable performance, avoid repeated handling and multiple The purity of GOPC-ROS1 was freeze/thaw cycles. determined to be >70% by densitometry, approx. MW 145kDa . Scientific Background GOPC gene encodes a Golgi protein with a PDZ domain. Mice which are deficient in the GOPC protein have globozoospermia and are infertile. Multiple transcript variants encoding different isoforms of GOPC have been found for this gene and GOPC gene locus is involved in translocations with other loci including c-ros oncogene 1 GOPC-ROS1, Active (ROS1) which result in the formation of the GOPC-ROS1 Human recombinant protein expressed in Sf9 cells fusion protein that act as an oncogene. -

Herpes Simplex Virus-1 Pul56 Degrades GOPC to Alter the Plasma
bioRxiv preprint doi: https://doi.org/10.1101/729343; this version posted August 8, 2019. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted bioRxiv a license to display the preprint in perpetuity. It is made available under aCC-BY-NC-ND 4.0 International license. 1 Herpes simplex virus-1 pUL56 degrades GOPC to alter the 2 plasma membrane proteome 3 4 1, 2Timothy K. Soh 5 1, 3Colin T. R. Davies 6 1, 2Julia Muenzner 7 2Viv Connor 8 2Clément R. Bouton 9 2Henry G. Barrow 10 2Cameron Smith 11 2Edward Emmott 12 3Robin Antrobus 13 2,4Stephen C. Graham 14 3,4Michael P. Weekes 15 *2,4,5Colin M. Crump 16 17 1These authors contributed equally 18 2Division of Virology, Department of Pathology, Cambridge University, Cambridge, CB2 19 1QP, UK 20 3Cambridge Institute for Medical Research, Cambridge University, Cambridge, CB2 21 0XY, UK 22 4Senior author 23 5Lead Contact. 24 *Correspondence: [email protected] 25 26 27 Keywords: Herpesvirus, Virus host interaction, Immune evasion, Membrane trafficking, 28 Proteasomal degradation, Quantitative proteomics, Uncharacterized ORF 29 1 bioRxiv preprint doi: https://doi.org/10.1101/729343; this version posted August 8, 2019. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted bioRxiv a license to display the preprint in perpetuity. It is made available under aCC-BY-NC-ND 4.0 International license. 30 Summary 31 Herpesviruses are ubiquitous in the human population and they extensively remodel the 32 cellular environment during infection. -

Understanding Binding-Induced Disorder-To-Order and Conformational
UNDERSTANDING BINDING-INDUCED DISORDER-TO-ORDER AND CONFORMATIONAL TRANSITIONS IN PROTEINS THAT REGULATE AUTOPHAGY A Dissertation Submitted to the Graduate Faculty of the North Dakota State University of Agriculture and Applied Science By Karen Marie Glover In Partial Fulfillment of the Requirements for the Degree of DOCTOR OF PHILOSOPHY Major Department: Chemistry and Biochemistry June 2018 Fargo, North Dakota North Dakota State University Graduate School Title UNDERSTANDING BINDING-INDUCED DISORDER-TO-ORDER AND CONFORMATIONAL TRANSITIONS IN PROTEINS THAT REGULATE AUTOPHAGY By Karen Marie Glover The Supervisory Committee certifies that this disquisition complies with North Dakota State University’s regulations and meets the accepted standards for the degree of DOCTOR OF PHILOSOPHY SUPERVISORY COMMITTEE: Dr. Sangita Sinha Chair Dr. Gregory Cook Dr. Stuart Haring Dr. Penelope Gibbs Approved: 26 June 2018 Dr. Gregory Cook Date Department Chair ABSTRACT Autophagy, a cellular homeostasis process that degrades and recycles cytosolic contents, is regulated at various stages by protein interactions. BECN1 regulates autophagy through interactions with diverse proteins via binding-induced conformational changes in its intrinsically disordered region (IDR) and flexible domains. Understanding the structure-function relationship of conformational transitions provides a basis for understanding these interactions and may be useful for targeting therapeutics for these proteins. We devised a method to identify IDRs likely to become helical upon binding, -

Centimorgan-Range One-Step Mapping of Fertility Traits Using Interspecific
Genetics: Published Articles Ahead of Print, published on May 4, 2007 as 10.1534/genetics.107.072157 1 Centimorgan-range one-step mapping of fertility traits using Interspecific Recombinant Congenic Mice David L'hôte*,‡, Catherine Serres†, Paul Laissue*, Ahmad Oulmouden‡, Claire Rogel- Gaillard** , Xavier Montagutelli§, Daniel Vaiman*,**,1. * Equipe 21, Génomique et Epigénétique des Pathologies Placentaires (GEPP), Unité INSERM 567 / UMR CNRS 8104 - Université Paris V IFR Alfred Jost, Faculté de Médecine, 75014 Paris, France † Université Paris Descartes, Faculté de Médecine de Cochin, Biologie de la Reproduction, 75014 Paris, France. ‡Unite de Genetique Moleculaire Animale, UMR 1061-INRA/Universite de Limoges, Limoges, France § Unite de Genetique des Mammiferes, Institut Pasteur, 75724 Paris cedex 15, France **Animal Genetics Department, INRA, France 2 Running title: Mapping of mouse fertility traits Key words: Mouse, QTL, Interspecific Recombinant Congenic Strain, Mus spretus, male fertility 1Corresponding author : Génomique et Epigénétique des Pathologies Placentaires (GEPP), Unité INSERM 567 / UMR CNRS 8104 - Université Paris V IFR Alfred Jost, Faculté de Médecine, 24 rue du faubourg Saint Jacques 75014 Paris, France. E-Mail : [email protected] 3 ABSTRACT In mammals, male fertility is a quantitative feature determined by numerous genes. Up to now, several wide chromosomal regions involved in fertility have been defined by genetic mapping approaches; unfortunately, the underlying genes are very difficult to identify. Here, fifty three strains of interspecific recombinant congenic mice (IRCS) bearing 1-2% SEG/Pas (Mus spretus) genomic fragments disseminated in a C57Bl/6J (Mus domesticus) background were used to systematically analyze male fertility parameters. One of the most prominent advantages of this model is the possibility of permanently coming back to living animals stable phenotypes. -

The Polarity Protein Scribble Positions DLC3 at Adherens Junctions To
© 2016. Published by The Company of Biologists Ltd | Journal of Cell Science (2016) 129, 3583-3596 doi:10.1242/jcs.190074 RESEARCH ARTICLE The polarity protein Scribble positions DLC3 at adherens junctions to regulate Rho signaling Janina Hendrick1, Mirita Franz-Wachtel2, Yvonne Moeller1, Simone Schmid1, Boris Macek2 and Monilola A. Olayioye1,* ABSTRACT cells the dominant function of Scribble appears to be within the planar The spatial regulation of cellular Rho signaling by GAP proteins is still polarity pathway (Humbert et al., 2008; Montcouquiol et al., 2003; poorly understood. By performing mass spectrometry, we here Murdoch et al., 2003). Scribble acts as a tumor suppressor in Drosophila identify the polarity protein Scribble as a scaffold for the RhoGAP and mammalian cells, and its loss cooperates with protein DLC3 (also known as StarD8) at cell–cell adhesions. This oncogenic Ras signaling in cell transformation (Bilder and Perrimon, mutually dependent interaction is mediated by the PDZ domains of 2000; Dow et al., 2003, 2008; Pagliarini and Xu, 2003). Scribble is a Scribble and a PDZ ligand (PDZL) motif in DLC3. Both Scribble multidomain scaffold protein containing 16 leucine-rich repeats depletion and PDZL deletion abrogated DLC3 junctional localization. (LRRs) and four PSD-95, ZO-1 and Discs large (PDZ) domains as – Using a RhoA biosensor and a targeted GAP domain, we platforms for protein protein interactions (Albertson et al., 2004; demonstrate that DLC3 activity locally regulates RhoA–ROCK Humbert et al., 2008). Loss of Scribble expression has been reported signaling at and Scribble localization to adherens junctions, and is in breast and colorectal cancer, and is associated with disrupted required for their functional integrity. -

Lack of Acrosome Formation in Mice Lacking a Golgi Protein, GOPC
Lack of acrosome formation in mice lacking a Golgi protein, GOPC Ryoji Yao*, Chizuru Ito†, Yasuko Natsume*, Yoshinobu Sugitani*, Hitomi Yamanaka*, Shoji Kuretake‡, Kaoru Yanagida‡, Akira Sato‡, Kiyotaka Toshimori†, and Tetsuo Noda*§¶ʈ** *Department of Cell Biology, Japanese Foundation for Cancer Research (JFCR) Cancer Institute, 1-37-1 Kami-Ikebukuro, Toshima-Ku, Tokyo 170-8455, Japan; †Department of Anatomy and Reproductive Cell Biology, Miyazaki Medical Collage, Kiyotake, Miyazaki 889-1692, Japan; ‡Department of Obstetrics and Gynecology, Fukushima Medical Collage, 1 Hikarigaoka, Fukushima 960-1295, Japan; §Department of Molecular Genetics, Tohoku University School of Medicine, 2-1 Seiryo-cho, Aoba-Ku, Sendai 980-8575, Japan; ¶Core Research for Evolutional Science and Technology (CREST), Japan Science and Technology Corporation, 4-1-8 Motomachi, Kawaguchi 332-0012, Japan; and ʈMouse Functional Genomics Research Group, Institute of Physical and Chemical Research (Japan) (RIKEN) Genomic Sciences Center, 214 Maeda-cho, Totsuka-ku, Yokohama, Kanagawa 244-0804, Japan Edited by Kai Simons, Max Planck Institute of Molecular Cell Biology and Genetics, Dresden, Germany, and approved June 19, 2002 (received for review January 31, 2002) The acrosome is a unique organelle that plays an important role at protein, and propose that GOPC may have a role in vesicle the site of sperm–zona pellucida binding during the fertilization transport from the Golgi apparatus (6). GOPC contains one process, and is lost in globozoospermia, an inherited infertility PDZ domain, two coiled-coil motifs, and two evolutionarily syndrome in humans. Although the acrosome is known to be conserved domains. The PDZ domain of GOPC is required for derived from the Golgi apparatus, molecular mechanisms under- its Frizzled binding, whereas coiled-coil motifs and conserved lying acrosome formation are largely unknown. -
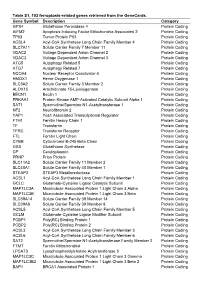
Table S1. 103 Ferroptosis-Related Genes Retrieved from the Genecards
Table S1. 103 ferroptosis-related genes retrieved from the GeneCards. Gene Symbol Description Category GPX4 Glutathione Peroxidase 4 Protein Coding AIFM2 Apoptosis Inducing Factor Mitochondria Associated 2 Protein Coding TP53 Tumor Protein P53 Protein Coding ACSL4 Acyl-CoA Synthetase Long Chain Family Member 4 Protein Coding SLC7A11 Solute Carrier Family 7 Member 11 Protein Coding VDAC2 Voltage Dependent Anion Channel 2 Protein Coding VDAC3 Voltage Dependent Anion Channel 3 Protein Coding ATG5 Autophagy Related 5 Protein Coding ATG7 Autophagy Related 7 Protein Coding NCOA4 Nuclear Receptor Coactivator 4 Protein Coding HMOX1 Heme Oxygenase 1 Protein Coding SLC3A2 Solute Carrier Family 3 Member 2 Protein Coding ALOX15 Arachidonate 15-Lipoxygenase Protein Coding BECN1 Beclin 1 Protein Coding PRKAA1 Protein Kinase AMP-Activated Catalytic Subunit Alpha 1 Protein Coding SAT1 Spermidine/Spermine N1-Acetyltransferase 1 Protein Coding NF2 Neurofibromin 2 Protein Coding YAP1 Yes1 Associated Transcriptional Regulator Protein Coding FTH1 Ferritin Heavy Chain 1 Protein Coding TF Transferrin Protein Coding TFRC Transferrin Receptor Protein Coding FTL Ferritin Light Chain Protein Coding CYBB Cytochrome B-245 Beta Chain Protein Coding GSS Glutathione Synthetase Protein Coding CP Ceruloplasmin Protein Coding PRNP Prion Protein Protein Coding SLC11A2 Solute Carrier Family 11 Member 2 Protein Coding SLC40A1 Solute Carrier Family 40 Member 1 Protein Coding STEAP3 STEAP3 Metalloreductase Protein Coding ACSL1 Acyl-CoA Synthetase Long Chain Family Member 1 Protein