Initial Observations Comparing MDCT and 3.0T MRI Findings with Autopsy Findings
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Deep Venous Thrombosis with Suspected Pulmonary Embolism
Thoracic Imaging Peter A. Loud, MD Deep Venous Thrombosis Douglas S. Katz, MD Dennis A. Bruce, MD with Suspected Pulmonary Donald L. Klippenstein, MD Zachary D. Grossman, MD Embolism: Detection with Combined CT Venography Index terms: Computed tomography (CT), 1 angiography, 9*.129142, and Pulmonary Angiography 9*.12915, 9*.12916 Embolism, pulmonary, 60.72 Pulmonary angiography, 944.12914, 944.12915, 944.12916 PURPOSE: To determine the frequency and location of deep venous thrombosis at Veins, thrombosis, 9*.751, 9*.12914 computed tomographic (CT) venography after CT pulmonary angiography in a large series of patients clinically suspected of having pulmonary embolism and to Radiology 2001; 219:498–502 compare the accuracy of CT venography with lower-extremity venous sonography. Abbreviation: MATERIALS AND METHODS: Venous phase images were acquired from the DVT ϭ deep venous thrombosis diaphragm to the upper calves after completion of CT pulmonary angiography in 650 patients (373 women, 277 men; age range, 18–99 years; mean age, 63 years) 1 From the Department of Radiology, to determine the presence and location of deep venous thrombosis. Results of CT Roswell Park Cancer Institute, Elm and Carlton Sts, Buffalo, NY 14263 (P.A.L., venography were compared with those of bilateral lower-extremity venous sonog- D.L.K., Z.D.G.), and the Department raphy in 308 patients. of Radiology, Winthrop University Hospital, Mineola, NY (D.S.K., D.A.B.). RESULTS: A total of 116 patients had pulmonary embolism and/or deep venous From the 1999 RSNA scientific assem- thrombosis, including 27 patients with pulmonary embolism alone, 31 patients with bly. -

Spring Programme 2011
Faculty of Radiologists Royal College of Surgeons in Ireland Combined Spring Meeting 8th & 9 th April 2011 Venue: Castlemartyr Hotel, Co. Cork. Programme Faculty of Radiologists, Royal College of Surgeons in Ireland CPD Credits Awarded: 5 Royal College of Radiologists credits are applied for. Friday 8 th April 2011 3.30-4.30pm Registration 4.30-5.30pm Stroke in 2011, Moderator: Dr. Ian Kelly, Waterford Regional Hospital 4.30-5.00pm Acute Stoke Imaging. Dr Noel Fanning, Cork University Hospital, Cork 5.00-5.30pm Stroke: A clinical perspective. Dr. George Pope, John Radcliffe Hospitals, Oxford 5.30-6.30pm Moderator: Dr. Adrian Brady, Dean, Faculty of Radiologists Belfast to Bosnia and Autopsy to Virtopsy Dr. Jack Crane, State Pathologist, NI 8pm Dinner Saturday 9 th April 2011 8.30-9.00am Registration 9.00-10.00am Liver hour. Moderator: Dr John Feeney, AMNCH, Dublin 9.00-9.30am Liver imaging pre metastatectomy. Dr. Peter MacEneaney, Mercy University Hospital, Cork 9.30-10.00am Parenchymal and focal liver biopsy - when and how. Dr Stephen J Skehan St Vincent's University Hospital, Dublin 10.00-11.00am Paediatric Hour. Moderator: Dr. Stephanie Ryan, The Children’s University Hospital Temple Street, Dublin 10.00-10.30am Paediatric Abdominal Emergencies. Dr Eoghan Laffan, The Children’s, University Hospital Temple Street, Dublin 10.30-11.00am Non Accidental Injury. Dr Conor Bogue, Cork University Hospital, Cork 11.00-11.30am Tea/Coffee Break and Poster Exhibition 11.30-12.30pm MSK Hour. Moderator: Dr Orla Buckley, AMNCH, Dublin 11.30-12.00pm Image guided joint interventions. -
CT Venography: Technique and Indications
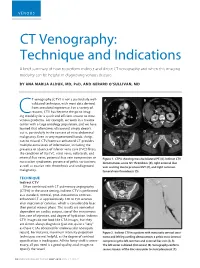
VENOUS CT Venography: Technique and Indications A brief summary of how to perform indirect and direct CT venography and when this imaging modality can be helpful in diagnosing venous disease. BY ANA MARIJA ALDUK, MD, PHD, AND GERARD O’SULLIVAN, MD T venography (CTV) is not a particularly well- A B validated technique, with most data derived from anecdotal experience. For a variety of reasons, CTV has become the go-to imag- Cing modality for a quick and efficient answer to most venous problems. For example, we work in a trauma center with a large oncology population, and we have learned that oftentimes ultrasound simply doesn’t cut it, particularly in the context of intra-abdominal C D malignancy. Even in very experienced hands, things can be missed. CTV/contrast-enhanced CT provides multiple extra levels of information, including the presence or absence of inferior vena cava (IVC) filters; the condition of the IVC, renal veins, collaterals, and internal iliac veins; potential iliac vein compression or Figure 1. CTPA showing massive bilateral PE (A). Indirect CTV nutcracker syndromes; presence of pelvic varicosities; demonstrates acute IVC thrombosis (B), right external iliac as well as ovarian vein thrombosis and undiagnosed vein scarring due to previous DVT (C), and right common malignancy. femoral vein thrombosis (D). TECHNIQUE A C Indirect CTV Often combined with CT pulmonary angiography (CTPA) in the acute setting, indirect CTV is performed as a standard, nonoral, post–intravenous contrast- enhanced CT at approximately 120 to 150 seconds after injection of contrast, which is considerably later than portal venous phase. -

Virtopsy and Living Individuals Evaluation Using Computed
Virtopsy and Living Individuals Evaluation Using Computed Tomography in Forensic Diagnostic Imaging Giuseppe Lo Re, MD, Sergio Salerno, MD, Maria Chiara Terranova, MD Antonella Argo, MD, Antonio Lo Casto, MD, Stefania Zerbo, MD, and Roberto Lagalla, MD The applications of forensic radiology involve both Virtopsy both studies on living people À to demonstrate bone age, search for foreign bodies, such as voluntary injection of drug ovules or surgical sponges accidentally forgotten, to assess gunshot wounds, to evaluate injuries by road accidents, and cases of violence or abuse (both in adults and in children). Computed tomography is the most used imaging tool used in forensic pathology and its indications are mainly focused on cases of unnatural deaths or when a crime is suspected. It is preferred over the standard autopsy in selected cases, such as in putrefied, carbonized or badly damaged bodies; or as a preliminary evaluation in mass disasters. Semin Ultrasound CT MRI 40:67-78 © 2018 Elsevier Inc. All rights reserved. Introduction also preserving evidence in an undisturbed state. Diag- nostic imaging plays a pivotal role in the preliminary he applications of forensic radiology (FR) involve both evaluation in the “safety screening” prior to forensic À T studies on living people and cadavers to demonstrate assessment of the remains; thus, preventing dangers to bone age, search for foreign bodies, such as voluntary injec- the workers who handle the corpses, or in case of infec- tion of drug ovules or surgical sponges accidentally forgot- tion surveillance, such as pulmonary tuberculosis, con- ten, to assess gunshot wounds, to evaluating injuries by road firmed by CT examination before autopsy.16-18 accidents and cases of violence or abuse (both in adults and Although the costs and availability of CT scanners and 1-3 in children). -

2Nd Quarter 2001 Medicare Part a Bulletin
In This Issue... From the Intermediary Medical Director Medical Review Progressive Corrective Action ......................................................................... 3 General Information Medical Review Process Revision to Medical Record Requests ................................................ 5 General Coverage New CLIA Waived Tests ............................................................................................................. 8 Outpatient Hospital Services Correction to the Outpatient Services Fee Schedule ................................................................. 9 Skilled Nursing Facility Services Fee Schedule and Consolidated Billing for Skilled Nursing Facility (SNF) Services ............. 12 Fraud and Abuse Justice Recovers Record $1.5 Billion in Fraud Payments - Highest Ever for One Year Period ........................................................................................... 20 Bulletin Medical Policies Use of the American Medical Association’s (AMA’s) Current Procedural Terminology (CPT) Codes on Contractors’ Web Sites ................................................................................. 21 Outpatient Prospective Payment System January 2001 Update: Coding Information for Hospital Outpatient Prospective Payment System (OPPS) ......................................................................................................................... 93 he Medicare A Bulletin Providers Will Be Asked to Register Tshould be shared with all to Receive Medicare Bulletins and health care -

New Phase in Forensic Odontology
International Journal of Dental and Health Sciences Review Article Volume 02,Issue 06 VIRTOPSY: NEW PHASE IN FORENSIC ODONTOLOGY Yogish.P 1, Asha Yogish 2 1.Assisstant Professor in Department of Oral Pathology and Microbiology, Sharavathi Dental College and Hospital, Shivamogga. 2.Postgraduate student in Department of Oral Medicine and Radiology, Coorg Institute of Dental Sciences, Virajpet. ABSTRACT: Nowadays, technological advances are becoming more and more important in forensic sciences. Yet autopsy is still one of the very traditional methods. This also applies for dental autopsies, in which visual, photographic and radiological evidences are collected. Virtual Autopsy appears as a helpful and complementary tool for dental and medical cadaveric examination. Using high-tech radiological approaches, Virtual Autopsy may provide, through images, an efficient and more accurate view on the individual case. This critical review aims to update on the origin, applications of virtopsy and also the role of dentists in this field. Keywords: Autopsy; Radiology; Forensic Odontology INTRODUCTION: Death is an inevitable part of life and at psychiatry and behavioural science, few occasions scientific examination of questioned documents, toxicology and bodies after death becomes mandatory. physical anthropology. Modern day investigations have reached a point of sophistication interconnecting Forensic pathology is a discipline of the involvement of many different Forensic science which deals with disciplines to serve problems including pathologic and -

(MRA) and Magnetic Resonance Venography (MRV) Medical Policy
Magnetic Resonance Angiography (MRA) and Magnetic Resonance Venography (MRV) Medical Policy The content of this document is used by plans that do not utilize NIA review. Service: Magnetic Resonance Angiography (MRA) and Magnetic Resonance Venography (MRV) PUM 250-0027-1712 Medical Policy Committee Approval 12/11/2020 Effective Date 01/01/2021 Prior Authorization Needed Yes Description: Magnetic Resonance Angiography (MRA) and Magnetic Resonance Venography (MRV) use Magnetic resonance imaging (MRI) technology to produce detailed 2-dimensional or 3- dimensional images of the vascular system and may be tailored to assess arteries or veins. It is often used for vascular conditions where other types of imaging are considered inferior or contraindicated, and to decrease risk of cumulative radiation exposure and often instead of invasive procedures. Indications of Coverage: A. MRA/MRV is considered medically necessary for the anatomical regions listed below when the specific indications or symptoms described are documented: 1. Head/Brain: a. Suspected intracranial aneurysm (ICA) or arteriovenous malformation (AVM). Any of the following: 1. Acute severe headache, severe exertional headache, or sudden onset of explosive headache, in individuals with signs / symptoms highly suggestive of a leaking/ruptured internal carotid artery or arteriovenous malformation. 2. Known subarachnoid hemorrhage or diagnosis of spontaneous intracerebral hemorrhage with concern for underlying vascular abnormality. 3. Suspected arteriovenous malformation (AVM) or dural AV fistula in an individual with prior indeterminate imaging study 4. Thunderclap headache with question of underlying vascular abnormality AND prior negative workup to include EITHER i. negative brain MRI, OR ii. Negative brain CT and negative lumbar puncture Page 1 of 15 5. -

Optos 200Tx and Heidelberg Spectralis
EXPERIMENTAL AND THERAPEUTIC MEDICINE 21: 19, 2021 Performance evaluation of two fundus oculi angiographic imaging system: Optos 200Tx and Heidelberg Spectralis SHUANG LI, JING‑JING WANG, HONG‑YANG LI, WEI WANG, MENG TIAN, XU‑QIANG LANG and KANG WANG Department of Ophthalmology, Beijing Friendship Hospital, Capital Medical University, Beijing 100050, P.R. China Received December 15, 2018; Accepted October 29, 2019 DOI: 10.3892/etm.2020.9451 Abstract. The present study aimed to compare the imaging Introduction performance of two ultra‑wide‑field fluorescein angiog‑ raphy imaging systems, namely the OptosOptomap 200Tx Ultra‑wide‑field fluorescein angiography (UWFA) is a novel (Optos 200Tx) and the Heidelberg Spectralis (Spectralis). A total technology that has developed rapidly in recent years (1,2). of 18 patients (36 eyes) underwent angiography using the two As numerous pathological changes of fundus diseases occur systems at the Department of Ophthalmology, Beijing Friendship at the edge of the retina, the limitation of imaging leads to Hospital (Beijing, China) between January and June 2017. The insufficient diagnosis or underestimation of the severity of the images were obtained as a single shot centered on the macula. disease (3,4). Therefore, clear imaging of the edge of the retina The total area and area within each of four visualized quadrants is important for the diagnosis, monitoring and prognostication were calculated and compared. The averages of the total and of patients with ocular fundus diseases. The traditional fundus individual quadrant area captured by the Optos 200Tx were fluorescein angiography system may only provide a vision field all larger than those obtained with the Spectralis (P<0.05). -

Virtopsy Working on the Future of Forensic Medicine
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by RERO DOC Digital Library Leitthema Rechtsmedizin 2007 · 17:7–12 M.J. Thali1 · S. Ross1 · L. Oesterhelweg1 · S. Grabherr1 · U. Buck1 · S. Naether1 · DOI 10.1007/s00194-006-0419-6 C. Jackowski1 · S.A. Bolliger1 · P. Vock2 · A. Christe2 · R. Dirnhofer1 Online publiziert: 30. Dezember 2006 1 Center of Forensic Imaging, Institute of Forensic Medicine, University, Bern © Springer Medizin Verlag 2006 2 Institute of Diagnostic Radiology, University Hospital, Bern Virtopsy Working on the future of forensic medicine In recent times, few fields have witnessed 3D Photogrammetry-based This allows for a more detailed surface such impressive progress as imaging optical scanning documentation compared to 3D recon- methods and radiology: digital data ac- structions based on high resolution CT quisition and post-processing of images The standard for the documentation of in- data. have revolutionized the practice of imag- juries in forensic medicine is still photog- The color information is acquired us- ing and radiology and have determined a raphy with exact measurements. Howev- ing the Tritop software that combines dig- growing interest in this field on the part er, the photographic process reduces a 3D ital photography of the surface from many of other medical professions. The applica- wound to a 2D level in the same way as different angles into 3D color information tion of imaging methods for non-invasive classical x-ray documentation. of the object that can be correctly matched documentation and analysis of relevant Using the TRITOP/ATOS III (GOM, on the digital 3D surface model using cod- forensic findings in living and deceased Braunschweig, Germany) system the col- ed and uncoded markers placed on the persons has lagged behind the enormous ored 3D surface can be documented via object. -

Coders' Desk Reference for ICD-10-PCS Procedures
2 0 2 DESK REFERENCE 1 ICD-10-PCS Procedures ICD-10-PCS for DeskCoders’ Reference Coders’ Desk Reference for ICD-10-PCS Procedures Clinical descriptions with answers to your toughest ICD-10-PCS coding questions Sample 2021 optum360coding.com Contents Illustrations ..................................................................................................................................... xi Introduction .....................................................................................................................................1 ICD-10-PCS Overview ...........................................................................................................................................................1 How to Use Coders’ Desk Reference for ICD-10-PCS Procedures ...................................................................................2 Format ......................................................................................................................................................................................3 ICD-10-PCS Official Guidelines for Coding and Reporting 2020 .........................................................7 Conventions ...........................................................................................................................................................................7 Medical and Surgical Section Guidelines (section 0) ....................................................................................................8 Obstetric Section Guidelines (section -

APG Regulations
FINAL as of 8/22/08 Pursuant to the authority vested in the Commissioner of Health by Section 2807(2-a) of the Public Health Law, Part 86 of Title 10 of the Official Compilation of Codes, Rules and Regulations of the State of New York, is amended by adding a new Subpart 86-8, to be effective upon filing with the Secretary of State, to read as follows: SUBPART 86-8 OUTPATIENT SERVICES: AMBULATORY PATIENT GROUP (Statutory authority: Public Health Law § 2807(2-a)(e)) Sec. 86-8.1 Scope 86-8.2 Definitions 86-8.3 Record keeping, reports and audits 86-8.4 Capital reimbursement 86-8.5 Administrative rate appeals 86-8.6 Rates for new facilities during the transition period 86-8.7 APGs and relative weights 86-8.8 Base rates 86-8.9 Diagnostic coding and rate computation 86-8.10 Exclusions from payment 86-8.11 System updating 86-8.12 Payments for extended hours of operation § 86-8.1 Scope (a) This Subpart shall govern Medicaid rates of payments for ambulatory care services provided in the following categories of facilities for the following periods: (1) outpatient services provided by general hospitals on and after December 1, 2008; (2) emergency department services provided by general hospitals on and after January 1, 2009; (3) ambulatory surgery services provided by general hospitals on and after December 1, 2008; (4) ambulatory services provided by diagnostic and treatment centers on and after March 1, 2009; and (5) ambulatory surgery services provided by free-standing ambulatory surgery centers on and after March 1, 2009. -

Indocyanine Green Fluorography in Plastic Surgery and Microvascular Surgery
48 The Open Surgical Oncology Journal, 2010, 2, 48-56 Open Access Indocyanine Green Fluorography in Plastic Surgery and Microvascular Surgery Ryuichi Azuma*,1, Megumi Takikawa1, Shinichirou Nakamura1, Kaoru Sasaki1, Satoshi Yanagibayashi1, Naoto Yamamoto1, Tomoharu Kiyosawa1 and Yuji Morimoto2 1Department of Plastic Surgery, Natinal Defense Medical College, Japan 2Department of Integrative Physiology and Bio-Nano Medicine National Defense Medical College, Japan Abstract: Indocyanine green (ICG) fluorography which is used to visualize the arteries, veins, and lymphatic vessels through the skin surface has recently been developed. This article includes an overview of our clinical experiences as well as descriptions of the latest knowledge on the utilization of ICG fluorography in the fields of plastic surgery and microvascular surgery. Imaging of the Capillary Blood Flow: To predict the future survival and necrosis, ICG fluorography is useful in various situations such as to examine injured limbs, skin flaps with a poor blood flow or ischemic limbs due to arteriosclerosis obliterans. Imaging of the Arteries: Practical pictures of a subcutaneous artery can be obtained for preoperative evaluations of the nutrient vessels of a skin flap and the blood flow within a skin flap. It is particularly useful for planning the use of a perforator-based flap. Imaging of the Lymphatic Vessels: ICG lymphography makes it possible to easily detect the functional lymphatic vessels in lymphaticovenous anastomosis for lymphedema of the extremities after either a surgical lymph node dissection or radiotherapy. Imaging of the Veins: With near-infrared skin imaging after the systemic administration of ICG, a clear picture of the subcutaneous veins, approximately 1 to 2 cm from the surface, can be obtained.