Cutaneous Melanomas Arising During Childhood: an Overview of the Main Entities
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Clinical Features of Benign Tumors of the External Auditory Canal According to Pathology
Central Annals of Otolaryngology and Rhinology Research Article *Corresponding author Jae-Jun Song, Department of Otorhinolaryngology – Head and Neck Surgery, Korea University College of Clinical Features of Benign Medicine, 148 Gurodong-ro, Guro-gu, Seoul, 152-703, South Korea, Tel: 82-2-2626-3191; Fax: 82-2-868-0475; Tumors of the External Auditory Email: Submitted: 31 March 2017 Accepted: 20 April 2017 Canal According to Pathology Published: 21 April 2017 ISSN: 2379-948X Jeong-Rok Kim, HwibinIm, Sung Won Chae, and Jae-Jun Song* Copyright Department of Otorhinolaryngology-Head and Neck Surgery, Korea University College © 2017 Song et al. of Medicine, South Korea OPEN ACCESS Abstract Keywords Background and Objectives: Benign tumors of the external auditory canal (EAC) • External auditory canal are rare among head and neck tumors. The aim of this study was to analyze the clinical • Benign tumor features of patients who underwent surgery for an EAC mass confirmed as a benign • Surgical excision lesion. • Recurrence • Infection Methods: This retrospective study involved 53 patients with external auditory tumors who received surgical treatment at Korea University, Guro Hospital. Medical records and evaluations over a 10-year period were examined for clinical characteristics and pathologic diagnoses. Results: The most common pathologic diagnoses were nevus (40%), osteoma (13%), and cholesteatoma (13%). Among the five pathologic subgroups based on the origin organ of the tumor, the most prevalent pathologic subgroup was the skin lesion (47%), followed by the epithelial lesion (26%), and the bony lesion (13%). No significant differences were found in recurrence rate, recurrence duration, sex, or affected side between pathologic diagnoses. -

CASE REPORT Intradermal Nevus of the External Auditory Canal
Int. Adv. Otol. 2009; 5:(3) 401-403 CASE REPORT Intradermal Nevus of the External Auditory Canal: A Case Report Sedat Ozturkcan, Ali Ekber, Riza Dundar, Filiz Gulustan, Demet Etit, Huseyin Katilmis Department of Otorhinolaryngology and Head and Neck Surgery ‹zmir Atatürk Research and Training Hospital, Ministry of Health, ‹ZM‹R-TURKEY (SO, AE, FG, DE, HK) Department of Otorhinolaryngology and Head and Neck Surgery Etimesgut Military Hospital , ANKARA-TURKEY (RD) Intradermal nevus is the most common skin tumor in humans; however, its occurrence in the external auditory canal (EAC) is uncommon. The clinical manifestations of pigmented nevus of the EAC have been reported to include ear fullness, foreign body sensation, hearing impairment, and otalgia, but some cases were asymptomatic and were found incidentally. The treatment of choice for a symptomatic intradermal nevus in the EAC is complete excision. There has been no recurrence reported in the literature . A pedunculated, papillomatous hair-bearing lesion was detected in the external auditory canal of the patient who was on follow-up for pruritus. Clinical and pathologic features of an intradermal nevus of the external auditory canal are presented, and the literature reviewed. Submitted : 14 October 2008 Revised : 01 July 2009 Accepted : 09 July 2009 Intradermal nevus is the most common skin tumor in left external auditory canal. Otomicroscopic humans; however, its occurrence in the external examination revealed a pedunculated, papillomatous auditory canal (EAC) is uncommon [1-4]. Intradermal hair-bearing lesion in the postero-inferior cartilaginous nevus is considered to be a form of benign cutaneous portion of the external auditory canal (Figure 1). -

Acral Compound Nevus SJ Yun S Korea
University of Pennsylvania, Founded by Ben Franklin in 1740 Disclosures Consultant for Myriad Genetics and for SciBase (might try to sell you a book, as well) Multidimensional Pathway Classification of Melanocytic Tumors WHO 4th Edition, 2018 Epidemiologic, Clinical, Histologic and Genomic Aspects of Melanoma David E. Elder, MB ChB, FRCPA University of Pennsylvania, Philadelphia, PA, USA Napa, May, 2018 3rd Edition, 2006 Malignant Melanoma • A malignant tumor of melanocytes • Not all melanomas are the same – variation in: – Epidemiology – risk factors, populations – Cell/Site of origin – Precursors – Clinical morphology – Microscopic morphology – Simulants – Genomic abnormalities Incidence of Melanoma D.M. Parkin et al. CSD/Site-Related Classification • Bastian’s CSD/Site-Related Classification (Taxonomy) of Melanoma – “The guiding principles for distinguishing taxa are genetic alterations that arise early during progression; clinical or histologic features of the primary tumor; characteristics of the host, such as age of onset, ethnicity, and skin type; and the role of environmental factors such as UV radiation.” Bastian 2015 Epithelium associated Site High UV Low UV Glabrous Mucosa Benign Acquired Spitz nevus nevus Atypical Dysplastic Spitz Borderline nevus tumor High Desmopl. Low-CSD Spitzoid Acral Mucosal Malignant CSD melanoma melanoma melanoma melanoma melanoma 105 Point mutations 103 Structural Rearrangements 2018 WHO Classification of Melanoma • Integrates Epidemiologic, Genomic, Clinical and Histopathologic Features • Assists -
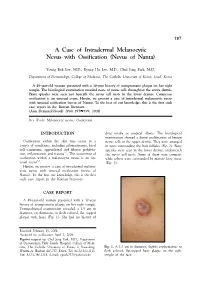
A Case of Intradermal Melanocytic Nevus with Ossification (Nevus of Nanta)
197 A Case of Intradermal Melanocytic Nevus with Ossification (Nevus of Nanta) Young Bok Lee, M.D., Kyung Ho Lee, M.D., Chul Jong Park, M.D. Department of Dermatology, College of Medicine, The Catholic University of Korea, Seoul, Korea A 49-year-old woman presented with a 30-year history of asymptomatic plaque on her right temple. The histological examination revealed nests of nevus cells throughout the entire dermis. Bony spicules were seen just beneath the nevus cell nests in the lower dermis. Cutaneous ossification is an unusual event. Herein, we present a case of intradermal melanocytic nevus with unusual ossification (nevus of Nanta). To the best of our knowledge, this is the first such case report in the Korean literature. (Ann Dermatol (Seoul) 20(4) 197∼199, 2008) Key Words: Melanocytic nevus, Ossification INTRODUCTION drug intake or medical illness. The histological examination showed a dense proliferation of benign Ossification within the skin may occur in a nevus cells in the upper dermis. They were arranged variety of conditions, including pilomatricoma, basal in nests surrounding the hair follicles (Fig. 2). Bony cell carcinoma, appendageal and fibrous prolifera- spicules were seen in the lower dermis, underneath 1,2 tion, inflammation and trauma . The occurrence of the nevus cell nests. Some of them were compact ossification within a melanocytic nevus is an un- while others were surrounded by mature fatty tissue 3-5 usual event . (Fig. 3). Herein, we present a case of intradermal melano- cytic nevus with unusual ossification (nevus of Nanta). To the best our knowledge, this is the first such case report in the Korean literature. -

Nevus Spilus: Is the Presence of Hair Associated with an Increased Risk for Melanoma?
Nevus Spilus: Is the Presence of Hair Associated With an Increased Risk for Melanoma? Robert Milton Gathings, MD; Raveena Reddy, MD; Ashish C. Bhatia, MD; Robert T. Brodell, MD PRACTICE POINTS • Nevus spilus (NS) appears as a café au lait macule studded with darker brown “moles.” • Although melanoma has been described in NS, it is rare. • There is no evidence that hairy NS are predisposed to melanoma. copy not Nevus spilus (NS), also known as speckled len- he term nevus spilus (NS), also known as tiginous nevus, is characterized by background speckled lentiginous nevus, was first used café au lait–like lentiginous melanocytic hyperpla- Tin the 19th century to describe lesions with sia speckled with small, 1- to 3-mm, darker foci.Do background café au lait–like lentiginous melanocytic Nevus spilus occurs in 1.3% to 2.3% of the adult hyperplasia speckled with small, 1- to 3-mm, darker population worldwide. Reports of melanoma aris- foci. The dark spots reflect lentigines; junctional, ing within hypertrichotic NS suggest that hyper- compound, and intradermal nevus cell nests; and trichosis may be a marker for the development of more rarely Spitz and blue nevi. Both macular and melanoma. We present a case of a hypertrichotic papular subtypes have been described.1 This birth- NS without melanoma and also provide a review of mark is quite common, occurring in 1.3% to 2.3% previously reported cases of hypertrichosis in NS. of the adult population worldwide.2 Hypertrichosis We believe that NS has aCUTIS lower risk for malignant has been described in NS.3-9 Two subsequent cases degeneration than congenital melanocytic nevi of malignant melanoma in hairy NS suggested that (CMN) of the same size, and it is unlikely that lesions may be particularly prone to malignant hypertrichosis is a marker for melanoma in NS. -

Short Course 11 Pigmented Lesions of the Skin
Rev Esp Patol 1999; Vol. 32, N~ 3: 447-453 © Prous Science, SA. © Sociedad Espafiola de Anatomfa Patol6gica Short Course 11 © Sociedad Espafiola de Citologia Pigmented lesions of the skin Chairperson F Contreras Spain Ca-chairpersons S McNutt USA and P McKee, USA. Problematic melanocytic nevi melanin pigment is often evident. Frequently, however, the lesion is solely intradermal when it may be confused with a fibrohistiocytic RH. McKee and F.R.C. Path tumor, particularly epithelloid cell fibrous histiocytoma (4). It is typi- cally composed of epitheliold nevus cells with abundant eosinophilic Brigham and Women’s Hospital, Harvard Medical School, Boston, cytoplasm and large, round, to oval vesicular nuclei containing pro- USA. minent eosinophilic nucleoli. Intranuclear cytoplasmic pseudoinclu- sions are common and mitotic figures are occasionally present. The nevus cells which are embedded in a dense, sclerotic connective tis- Whether the diagnosis of any particular nevus is problematic or not sue stroma, usually show maturation with depth. Less frequently the nevus is composed solely of spindle cells which may result in confu- depends upon a variety of factors, including the experience and enthusiasm of the pathologist, the nature of the specimen (shave vs. sion with atrophic fibrous histiocytoma. Desmoplastic nevus can be distinguished from epithelloid fibrous histiocytoma by its paucicellu- punch vs. excisional), the quality of the sections (and their staining), larity, absence of even a focal storiform growth pattern and SiQO pro- the hour of the day or day of the week in addition to the problems relating to the ever-increasing range of histological variants that we tein/HMB 45 expression. -

Melanocytic Lesions of the Face—SW Mccarthy & RA Scolyer 3 Review Article
Melanocytic Lesions of the Face—SW McCarthy & RA Scolyer 3 Review Article Melanocytic Lesions of the Face: Diagnostic Pitfalls* 1,2 1,2 SW McCarthy, MBBS, FRCPA, RA Scolyer, MBBS, FRCPA Abstract The pathologist often has a difficult task in evaluating melanocytic lesions. For lesions involving the face the consequences of misdiagnosis are compounded for both cosmetic and therapeutic reasons. In this article, the pathological features of common and uncommon benign and malignant melanocytic lesions are reviewed and pitfalls in their diagnosis are highlighted. Benign lesions resembling melanomas include regenerating naevus, “irritated” naevus, com- bined naevus, “ancient naevus”, Spitz naevus, dysplastic naevus, halo naevus, variants of blue naevi, balloon and clear cell naevi, neurotised naevus and desmoplastic naevus. Melanomas that can easily be missed on presentation include desmoplastic, naevoid, regressed, myxoid and metastatic types as well as so-called malignant blue naevi. Pathological clues to benign lesions include good symmetry, V-shaped silhouette, absent epidermal invasion, uniform cellularity, deep maturation, absent or rare dermal mitoses and clustered Kamino bodies. Features more commonly present in melanomas include asymmetry, peripheral epidermal invasion, heavy or “dusty” pigmentation, deep and abnormal dermal mitoses, HMB45 positivity in deep dermal melanocytes, vascular invasion, neurotropism and satellites. Familiarity with the spectrum of melanocytic lesions and knowledge of the important distinguishing features should -

Optimal Management of Common Acquired Melanocytic Nevi (Moles): Current Perspectives
Clinical, Cosmetic and Investigational Dermatology Dovepress open access to scientific and medical research Open Access Full Text Article REVIEW Optimal management of common acquired melanocytic nevi (moles): current perspectives Kabir Sardana Abstract: Although common acquired melanocytic nevi are largely benign, they are probably Payal Chakravarty one of the most common indications for cosmetic surgery encountered by dermatologists. With Khushbu Goel recent advances, noninvasive tools can largely determine the potential for malignancy, although they cannot supplant histology. Although surgical shave excision with its myriad modifications Department of Dermatology and STD, Maulana Azad Medical College and has been in vogue for decades, the lack of an adequate histological sample, the largely blind Lok Nayak Hospital, New Delhi, Delhi, nature of the procedure, and the possibility of recurrence are persisting issues. Pigment-specific India lasers were initially used in the Q-switched mode, which was based on the thermal relaxation time of the melanocyte (size 7 µm; 1 µsec), which is not the primary target in melanocytic nevus. The cluster of nevus cells (100 µm) probably lends itself to treatment with a millisecond laser rather than a nanosecond laser. Thus, normal mode pigment-specific lasers and pulsed ablative lasers (CO2/erbium [Er]:yttrium aluminum garnet [YAG]) are more suited to treat acquired melanocytic nevi. The complexities of treating this disorder can be overcome by following a structured approach by using lasers that achieve the appropriate depth to treat the three subtypes of nevi: junctional, compound, and dermal. Thus, junctional nevi respond to Q-switched/normal mode pigment lasers, where for the compound and dermal nevi, pulsed ablative laser (CO2/ Er:YAG) may be needed. -

Mtor Mutations in Smith-Kingsmore Syndrome: Four Additional Patients and a Review
Received: 4 July 2017 Revised: 31 August 2017 Accepted: 5 September 2017 DOI: 10.1111/cge.13135 ORIGINAL ARTICLE mTOR mutations in Smith-Kingsmore syndrome: Four additional patients and a review G. Gordo1,2,3 | J. Tenorio1,2 | P. Arias1,2 | F. Santos-Simarro1,4 | S. García-Miñaur1,4 | J.C. Moreno1,2 | J. Nevado1,5 | E. Vallespin1,5 | L. Rodriguez-Laguna1,3 | R. de Mena1,5 | I. Dapia1,2 | M. Palomares-Bralo1,5 | A. del Pozo1,6 | K. Ibañez1,6 | J.C. Silla1,6 | E. Barroso1,2 | V.L. Ruiz-Pérez1,7 | V. Martinez-Glez1,3,4 | P. Lapunzina1,2,4 1Centro de Investigación Biomédica en Red de Enfermedades Raras (CIBERER), ISCIII, Madrid, Spain 2Molecular Endocrinology Section, Overgrowth Syndromes Laboratory, Instituto de Genética Médica y Molecular (INGEMM), IdiPAZ, Hospital Universitario la Paz, Universidad Autónoma de Madrid (UAM), Madrid, Spain 3Vascular Malformations Section, Instituto de Genética Médica y Molecular (INGEMM), IdiPAZ, Hospital Universitario la Paz, Universidad Autónoma de Madrid (UAM), Madrid, Spain 4Clinical Genetics Section, Instituto de Genética Médica y Molecular (INGEMM), IdiPAZ, Hospital Universitario la Paz, Universidad Autónoma de Madrid (UAM), Madrid, Spain 5Structural and Functional Genomics Section, Instituto de Genética Médica y Molecular (INGEMM), IdiPAZ, Hospital Universitario la Paz, Universidad Autónoma de Madrid (UAM), Madrid, Spain 6Bioinformatics Section, Instituto de Genética Médica y Molecular (INGEMM), IdiPAZ, Hospital Universitario la Paz, Universidad Autónoma de Madrid (UAM), Madrid, Spain 7IIB, Instituto de Investigación “Alberto Sols”, Universidad Autónoma de Madrid (UAM), Madrid, Spain Correspondence Smith-Kingsmore syndrome (SKS) OMIM #616638, also known as MINDS syndrome (ORPHA Pablo Lapunzina, MD, PhD, Instituto de Genética Médica y Molecular (INGEMM), 457485), is a rare autosomal dominant disorder reported so far in 23 patients. -

Emery and Rimoin's Principles and Practice Of
9 Disorders of the Venous System Pascal Brouillard,1 Nisha Limaye,1 Laurence M. Boon,1,2 Miikka Vikkula1,3 1Human Molecular Genetics, de Duve Institute, Université catholique de Louvain, Brussels, Belgium, 2Center for Vascular Anomalies, Division of Plastic Surgery, Cliniques Universitaires St-Luc, Université catholique de Louvain, Brussels, Belgium, 3Walloon Excellence in Lifesciences and Biotechnology (WELBIO), Université catholique de Louvain, Brussels, Belgium 9.1 INTRODUCTION hemangioma) and more slow-growing vascular malfor- mations. The latter are subcategorized according to the The vasculature is the first organ system to develop during type(s) of vessel(s) altered [5–7] into capillary, venous, embryogenesis, delivering nutrients, growth factors, and arteriovenous, lymphatic, and combined malformations. oxygen to tissues and removing wastes. It is made up of four major types of vessels: arteries, capillaries, veins, and lymphatic vessels, all of which have a single layer of endo- 9.2 THE VENOUS SYSTEM thelial cells (ECs) forming the innermost layer. In blood Veins collect CO2-rich blood from the capillary net- vessels, the endothelial tubes are supported by a layer of work and contain about 75%–80% of the total volume of vascular smooth muscle cells (vSMCs) and/or pericytes blood in the body. They have larger lumens than arteries, (together called mural cells) of variable thickness. A base- with thinner, less muscular walls. Venous flow is passive, ment membrane separates the endothelial and vSMC essentially mediated by physical movements of the body layers, with an extracellular matrix (ECM) of fibrous and and the aspirating effect exerted by the heart. The pres- elastic proteins and carbohydrate polymers forming the ence of valves ensures correct orientation of blood flow. -

Identification of HRAS Mutations and Absence of GNAQ Or GNA11
Modern Pathology (2013) 26, 1320–1328 1320 & 2013 USCAP, Inc All rights reserved 0893-3952/13 $32.00 Identification of HRAS mutations and absence of GNAQ or GNA11 mutations in deep penetrating nevi Ryan P Bender1, Matthew J McGinniss2, Paula Esmay1, Elsa F Velazquez3,4 and Julie DR Reimann3,4 1Caris Life Sciences, Phoenix, AZ, USA; 2Genoptix Medical Laboratory, Carlsbad, CA, USA; 3Dermatopathology Division, Miraca Life Sciences Research Institute, Newton, MA, USA and 4Department of Dermatology, Tufts Medical Center, Boston, MA, USA HRAS is mutated in B15% of Spitz nevi, and GNAQ or GNA11 is mutated in blue nevi (46–83% and B7% respectively). Epithelioid blue nevi and deep penetrating nevi show features of both blue nevi (intradermal location, pigmentation) and Spitz nevi (epithelioid morphology). Epithelioid blue nevi and deep penetrating nevi can also show overlapping features with melanoma, posing a diagnostic challenge. Although epithelioid blue nevi are considered blue nevic variants, no GNAQ or GNA11 mutations have been reported. Classification of deep penetrating nevi as blue nevic variants has also been proposed, however, no GNAQ or GNA11 mutations have been reported and none have been tested for HRAS mutations. To better characterize these tumors, we performed mutational analysis for GNAQ, GNA11, and HRAS, with blue nevi and Spitz nevi as controls. Within deep penetrating nevi, none demonstrated GNAQ or GNA11 mutations (0/38). However, 6% revealed HRAS mutation (2/32). Twenty percent of epithelioid blue nevi contained a GNAQ mutation (2/10), while none displayed GNA11 or HRAS mutation. Eighty-seven percent of blue nevi contained a GNAQ mutation (26/30), 4% a GNA11 mutation (1/28), and none an HRAS mutation. -

Prevalence of Melanoma Clinically Resembling Seborrheic Keratosis Analysis of 9204 Cases
STUDY Prevalence of Melanoma Clinically Resembling Seborrheic Keratosis Analysis of 9204 Cases Leonid Izikson, BS; Arthur J. Sober, MD; Martin C. Mihm, Jr, MD, FRCP; Artur Zembowicz, MD, PhD Objective: To estimate the prevalence of melanoma clini- Main Outcome Measure: Histological diagnosis, which cally mimicking seborrheic keratosis. was correlated with the preoperative clinical diagnosis. Design: Retrospective review of cases submitted for his- Results: Melanoma was identified in 61 cases (0.66%) tological examination with a clinical diagnosis of sebor- submitted for histological examination with a clinical rheic keratosis or with a differential diagnosis that in- diagnosis that included seborrheic keratosis. Melanoma cluded seborrheic keratosis. was in the clinical differential diagnosis of 31 cases (51%). The remaining lesions had a differential diagno- Setting: A tertiary medical care center–based der- sis of seborrheic keratosis vs melanocytic nevus (17 matopathology laboratory serving academic der- cases, 28%), basal cell carcinoma (7 cases, 12%), or a squa- matology clinics that have a busy pigmented lesion mous proliferation (3 cases, 5%). In 3 cases (5%), seb- clinic. orrheic keratosis was the only clinical diagnosis. All histological types of melanoma were represented. Materials and Methods: A total of 9204 consecutive pathology reports containing a diagnosis of seborrheic Conclusions: Our results confirm that melanoma can keratosis in the clinical information field were identi- mimic seborrheic keratosis. These data strongly support fied between the years 1992 and 2001 through a com- the current policy of submitting for histological examina- puter database search. Reports with a final histological tion all specimens that have been removed from patients. diagnosis of melanoma were selected for further review and clinicopathological analysis.