Parts of the Eye
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Te2, Part Iii
TERMINOLOGIA EMBRYOLOGICA Second Edition International Embryological Terminology FIPAT The Federative International Programme for Anatomical Terminology A programme of the International Federation of Associations of Anatomists (IFAA) TE2, PART III Contents Caput V: Organogenesis Chapter 5: Organogenesis (continued) Systema respiratorium Respiratory system Systema urinarium Urinary system Systemata genitalia Genital systems Coeloma Coelom Glandulae endocrinae Endocrine glands Systema cardiovasculare Cardiovascular system Systema lymphoideum Lymphoid system Bibliographic Reference Citation: FIPAT. Terminologia Embryologica. 2nd ed. FIPAT.library.dal.ca. Federative International Programme for Anatomical Terminology, February 2017 Published pending approval by the General Assembly at the next Congress of IFAA (2019) Creative Commons License: The publication of Terminologia Embryologica is under a Creative Commons Attribution-NoDerivatives 4.0 International (CC BY-ND 4.0) license The individual terms in this terminology are within the public domain. Statements about terms being part of this international standard terminology should use the above bibliographic reference to cite this terminology. The unaltered PDF files of this terminology may be freely copied and distributed by users. IFAA member societies are authorized to publish translations of this terminology. Authors of other works that might be considered derivative should write to the Chair of FIPAT for permission to publish a derivative work. Caput V: ORGANOGENESIS Chapter 5: ORGANOGENESIS -

Symptoms of Age Related Macular Degeneration
WHAT IS MACULAR DEGENERATION? wavy or crooked, visual distortions, doorway and the choroid are interrupted causing waste or street signs seem bowed, or objects may deposits to form. Lacking proper nutrients, the light- Age related macular degeneration (AMD) is appear smaller or farther away than they sensitive cells of the macula become damaged. a disease that may either suddenly or gradually should, decrease in or loss of central vision, and The damaged cells can no longer send normal destroy the macula’s ability to maintain sharp, a central blurry spot. signals from the macula through the optic nerve to central vision. Interestingly, one’s peripheral or DRY: Progression with dry AMD is typically slower your brain, and consequently your vision becomes side vision remains unaffected. AMD is the leading de-gradation of central vision: need for increasingly blurred cause of “legal blindness” in the United States for bright illumination for reading or near work, diffi culty In either form of AMD, your vision may remain fi ne persons over 65 years of age. AMD is present in adapting to low levels of illumination, worsening blur in one eye up to several years even while the other approximately 10 percent of the population over of printed words, decreased intensity or brightness of eye’s vision has degraded. Most patients don’t the age of 52 and in up to 33 percent of individuals colors, diffi culty recognizing faces, gradual increase realize that one eye’s vision has been severely older than 75. The macula allows alone gives us the in the haziness of overall vision, and a profound drop reduced because your brain compensates the bad ability to have: sharp vision, clear vision, color vision, in your central vision acuity. -

Permeability of the Retina and RPE-Choroid-Sclera to Three Ophthalmic Drugs and the Associated Factors
pharmaceutics Article Permeability of the Retina and RPE-Choroid-Sclera to Three Ophthalmic Drugs and the Associated Factors Hyeong Min Kim 1,†, Hyounkoo Han 2,†, Hye Kyoung Hong 1, Ji Hyun Park 1, Kyu Hyung Park 1, Hyuncheol Kim 2,* and Se Joon Woo 1,* 1 Department of Ophthalmology, Seoul National University College of Medicine, Seoul National University Bundang Hospital, Seongnam 13620, Korea; [email protected] (H.M.K.); [email protected] (H.K.H.); [email protected] (J.H.P.); [email protected] (K.H.P.) 2 Department of Chemical and Biomolecular Engineering, Sogang University, Seoul 04107, Korea; [email protected] * Correspondence: [email protected] (H.K.); [email protected] (S.J.W.); Tel.: +82-2-705-8922 (H.K.); +82-31-787-7377 (S.J.W.); Fax: +82-2-3273-0331 (H.K.); +82-31-787-4057 (S.J.W.) † These authors contributed equally to this work. Abstract: In this study, Retina-RPE-Choroid-Sclera (RCS) and RPE-Choroid-Sclera (CS) were prepared by scraping them off neural retina, and using the Ussing chamber we measured the average time– concentration values in the acceptor chamber across five isolated rabbit tissues for each drug molecule. We determined the outward direction permeability of the RCS and CS and calculated the neural retina permeability. The permeability coefficients of RCS and CS were as follows: ganciclovir, 13.78 ± 5.82 and 23.22 ± 9.74; brimonidine, 15.34 ± 7.64 and 31.56 ± 12.46; bevacizumab, 0.0136 ± 0.0059 and 0.0612 ± 0.0264 (×10−6 cm/s). -

How Clean Is Your Capsule?
Eye (1989) 3, 678-684 How Clean is Your Capsule? W. T. GREEN and D. L. BOASE Portsmouth Summary Proliferation of residual lens epithelial cells is believed to be the major cause of pos terior capsule opacification following extracapsular cataract extraction. During sur gery these cells can be visualised with appropriate illumination facilitating their mechanical removal with the McIntyre cannula. When flat preparations of the anterior capsule are examined by light microscopy, the areas 'cleaned' of cells in this way appear transparent but scanning electron microscopy reveals tufts of remaining debris which may represent points of cellular attachment to the capsule. Control of lens epithelial cell proliferation is important for the future development of cataract surgery. The undoubted advantages of extracapsular and also on human cadaver eyes. A horizontal cataract extraction are offset in many patients capsulotomy in the upper part of the lens by posterior capsule opacification requiring allowed nucleus removal. Irrigation and caps ulotomy. Not only is this disappointing aspiration of the cortical lens material was for the patient, but the procedure carries a then carried out using a McIntyre cannula risk of serious complications. with Hartman's irrigation solution. During in The major cause of posterior capsule opac vitro surgery this was aided by first removing ification is proliferation of residual lens epi the entire cornea and iris to improve visual thelial cells. I If these cells could be removed at isation and explore different methods of the time of surgery we believe that the inci illumination. dence of posterior capsule opacification and The importance of illumination was first the need for subsequent capsulotomy would suspected when it was observed, during rou be reduced. -

Selective Attention Within the Foveola
ARTICLES Selective attention within the foveola Martina Poletti1 , Michele Rucci1,2 & Marisa Carrasco3,4 Efficient control of attentional resources and high-acuity vision are both fundamental for survival. Shifts in visual attention are known to covertly enhance processing at locations away from the center of gaze, where visual resolution is low. It is unknown, however, whether selective spatial attention operates where the observer is already looking—that is, within the high-acuity foveola, the small yet disproportionally important rod-free region of the retina. Using new methods for precisely controlling retinal stimulation, here we show that covert attention flexibly improves and speeds up both detection and discrimination at loci only a fraction of a degree apart within the foveola. These findings reveal a surprisingly precise control of attention and its involvement in fine spatial vision. They show that the commonly studied covert shifts of attention away from the fovea are the expression of a global mechanism that exerts its action across the entire visual field. Covert attention is essential for visual perception. Among its many previous studies. We then investigated the consequences of attention advantages, covert allocation of attentional resources increases con- for both detection (experiment 2) and discrimination (experiments trast sensitivity and spatial resolution, speeds information accrual and 3 and 4) tasks within the foveola. reaction times1–4, and alters the signal at the target location during saccade preparation5–7. Covert attention has been studied sometimes RESULTS in the parafovea (1°–5°) and mostly in the perifovea (5°–10°) and Experiment 1 consisted of a central spatial cueing task with para- periphery (>10° of eccentricity)—that is, far outside the foveola, the foveal stimuli (Fig. -

Sclera and Retina Suturing Techniques 9 Kirk H
Chapter 9 Sclera and Retina Suturing Techniques 9 Kirk H. Packo and Sohail J. Hasan Key Points 9. 1 Introduction Surgical Indications • Vitrectomy Discussion of ophthalmic microsurgical suturing tech- – Infusion line niques as they apply to retinal surgery warrants atten- – Sclerotomies tion to two main categories of operations: vitrectomy – Conjunctival closure and scleral buckling. Th is chapter reviews the surgical – Ancillary techniques indications, basic instrumentation, surgical tech- • Scleral buckles niques, and complications associated with suturing – Encircling bands techniques in vitrectomy and scleral buckle surgery. A – Meridional elements brief discussion of future advances in retinal surgery Instrumentation appears at the end of this chapter. • Vitrectomy – Instruments – Sutures 9.2 • Scleral buckles Surgical Indications – Instruments – Sutures Surgical Technique 9.2.1 • Vitrectomy Vitrectomy – Suturing the infusion line in place – Closing sclerotomies Typically, there are three indications for suturing dur- • Scleral buckles ing vitrectomy surgery: placement of the infusion can- – Rectus muscle fi xation sutures nula, closure of sclerotomy, and the conjunctival clo- – Suturing encircling elements to the sclera sure. A variety of ancillary suturing techniques may be – Suturing meridional elements to the sclera employed during vitrectomy, including the external – Closing sclerotomy drainage sites securing of a lens ring for contact lens visualization, • Closure of the conjunctiva placement of transconjunctival or scleral fi xation su- Complications tures to manipulate the eye, and transscleral suturing • General complications of dislocated intraocular lenses. Some suturing tech- – Break in sterile technique with suture nee- niques such as iris dilation sutures and transretinal su- dles tures in giant tear repairs have now been replaced with – Breaking sutures other non–suturing techniques, such as the use of per- – Inappropriate knot creation fl uorocarbon liquids. -

The Eye Is a Natural Optical Tool
KEY CONCEPT The eye is a natural optical tool. BEFORE, you learned NOW, you will learn •Mirrors and lenses focus light • How the eye depends on to form images natural lenses •Mirrors and lenses can alter • How artificial lenses can be images in useful ways used to correct vision problems VOCABULARY EXPLORE Focusing Vision cornea p. 607 How does the eye focus an image? pupil p. 607 retina p. 607 PROCEDURE 1 Position yourself so you can see an object about 6 meters (20 feet) away. 2 Close one eye, hold up your index finger, and bring it as close to your open eye as you can while keeping the finger clearly in focus. 3 Keeping your finger in place, look just to the side at the more distant object and focus your eye on it. 4 Without looking away from the more distant object, observe your finger. WHAT DO YOU THINK? • How does the nearby object look when you are focusing on something distant? • What might be happening in your eye to cause this change in the nearby object? The eye gathers and focuses light. The eyes of human beings and many other animals are natural optical tools that process visible light. Eyes transmit light, refract light, and respond to different wavelengths of light. Eyes contain natural lenses that focus images of objects. Eyes convert the energy of light waves into signals that can be sent to the brain. The brain interprets these signals as shape, brightness, and color. Altogether, these processes make vision possible. In this section, you will learn how the eye works. -

Retinal Ganglion Cell Loss Is Size Dependent in Experimental Glaucoma
Investigative Ophthalmology & Visual Science, Vol. 32, No. 3, March 1991 Copyright © Association for Research in Vision and Ophthalmology Retinal Ganglion Cell Loss Is Size Dependent in Experimental Glaucoma Yoseph Glovinsky,* Harry A. Quigley,f and Gregory R. Dunkelbergerf Thirty-two areas located in the temporal midperipheral retina were evaluated in whole-mount prepara- tions from four monkeys with monocular experimental glaucoma. Diameter frequency distributions of remaining ganglion cells in the glaucomatous eye were compared with corresponding areas in the normal fellow eye. Large cells were significantly more vulnerable at each stage of cell damage as determined by linear-regression analysis. The magnitude of size-dependent loss was moderate at an early stage (20% loss), peaked at 50% total cell loss, and decreased in advanced damage (70% loss). In glaucomatous eyes, the lower retina had significantly more large cell loss than the corresponding areas of the upper retina. In optic nerve zones that matched the retinal areas studied, large axons selectively were damaged first. Psychophysical testing aimed at functions subserved by larger ganglion cells is recommended for detection and follow-up of early glaucoma; however, assessment of functions unique to small cells is more appropriate for detecting change in advanced glaucoma. Invest Ophthalmol Vis Sci 32:484-491, 1991 Current psychophysical tests do not detect glau- tage of ideal cellular preservation. Eyes with mild, comatous damage until a substantial minority of reti- moderate, and late damage were evaluated. In addi- nal ganglion cells have died.1'2 To develop more sen- tion, we correlated the damage patterns in the retinas sitive tests, a comprehensive understanding of the and optic nerves of the glaucomatous eyes. -

Microscopic Anatomy of the Eye Dog Cat Horse Rabbit Monkey Richard R Dubielzig Mammalian Globes Mammalian Phylogeny General Anatomy Dog
Microscopic Anatomy of the eye Dog Cat Horse Rabbit Monkey Richard R Dubielzig Mammalian globes Mammalian Phylogeny General Anatomy Dog Arterial Blood Vessels of the Orbit General Anatomy Dog * Horizontal section Long Posterior Ciliary a. Blood enters the globe Short Post. Ciliary a Long Post. Ciliary a. Anterior Ciliary a. Blood Supply General Anatomy Dog Major arterial circle of the iris Orbital Anatomy Dog Brain Levator Dorsal rectus Ventral rectus Zygomatic Lymph node Orbital Anatomy Dog Orbital Anatomy Dog Cartilaginous trochlea and the tendon of the dorsal oblique m. Orbital Anatomy Dog Rabbit Orbital Anatomy Dog Zygomatic salivary gland mucinous gland Orbital Anatomy Dog Gland of the Third Eyelid Eye lids (dog) Eye lids (dog) Meibomian glands at the lid margin Holocrine secretion Eye lids (primate) Upper tarsal plate Lower tarsal plate Eye lids (rabbit) The Globe The Globe Dog Cat Orangutan Diurnal Horse Diurnal Cornea Epithelium Stromal lamellae Bowman’s layer Dolphin Descemet’s m Endothelium TEM of surface epithelium Cornea Doubling of Descemet’s Vimentin + endothelium Iris Walls: The vertebrate eye Iris Sphincter m. Dilator m Blue-eye, GFAP stain Iris Collagen Iris Cat Sphinctor m. Dilator m. Iris Cat Phyomelanocytes Iris Equine Corpora nigra (Granula iridica) seen in ungulates living without shade Ciliary body Pars plicata Ciliary muscle Pars plana Ciliary body Zonular ligaments Ciliary body Primarily made of fibrillin A major component of elastin Ciliary body Alcian Blue staining acid mucopolysaccharides: Hyaluronic acid Ciliary -

Considering Contact Lens CORNEAL RESHAPING
Considering Contact Lens CORNEAL RESHAPING Patient Information Booklet for Potential Users of PARAGON RG-4 Contact Lens Corneal Reshaping PATIENT INFORMATION BOOKLET FOR POTENTIAL USERS OF PARAGON RG-4 Manufactured in Paragon HDS® 100 (paflufocon D) Contact Lenses For Contact Lens Corneal Reshaping Overnight Wear CAUTION: Federal (US) law restricts this device to sale by, or on the order of a licensed practitioner. Contact lenses for corneal reshaping should be fitted only by a trained and certified contact lens fitter. Nonsterile. Clean and condition lenses prior to use. ii TABLE OF CONTENTS Page Introduction 1 How The Eye Functions 1 How Paragon RG-4 Contact Lenses For Corneal Reshaping Function 2 Alternative Ways To Correct Nearsightedness 3 Risk Analysis 3 Indications 4 Precautions 4 Contraindications (Reasons Not To Use) 6 Warnings 6 Adverse Effects (Problems and What To Do) 7 Clinical Study Data 7 Overnight Wear Safety Summary 12 Maintaining Effects of Paragon RG-4 Lenses For Corneal Reshaping 13 Glossary 14 iii INTRODUCTION The information in this booklet is to help you decide whether or not to be fitted with Paragon RG-4 lens designs for Contact Lens Corneal Reshaping. Corneal reshaping is a fitting procedure that temporarily corrects or greatly reduces nearsightedness (known by the medical name, myopia) with or without astigmatism after contact lenses have been removed. By temporary, it is meant that the contact lenses are worn while sleeping (overnight) and then removed upon awaking; whereupon the nearsightedness remains corrected or greatly reduced for all or most of your waking hours. The exact time period over which the myopia remains corrected varies with each patient. -

The Complexity and Origins of the Human Eye: a Brief Study on the Anatomy, Physiology, and Origin of the Eye
Running Head: THE COMPLEX HUMAN EYE 1 The Complexity and Origins of the Human Eye: A Brief Study on the Anatomy, Physiology, and Origin of the Eye Evan Sebastian A Senior Thesis submitted in partial fulfillment of the requirements for graduation in the Honors Program Liberty University Spring 2010 THE COMPLEX HUMAN EYE 2 Acceptance of Senior Honors Thesis This Senior Honors Thesis is accepted in partial fulfillment of the requirements for graduation from the Honors Program of Liberty University. ______________________________ David A. Titcomb, PT, DPT Thesis Chair ______________________________ David DeWitt, Ph.D. Committee Member ______________________________ Garth McGibbon, M.S. Committee Member ______________________________ Marilyn Gadomski, Ph.D. Assistant Honors Director ______________________________ Date THE COMPLEX HUMAN EYE 3 Abstract The human eye has been the cause of much controversy in regards to its complexity and how the human eye came to be. Through following and discussing the anatomical and physiological functions of the eye, a better understanding of the argument of origins can be seen. The anatomy of the human eye and its many functions are clearly seen, through its complexity. When observing the intricacy of vision and all of the different aspects and connections, it does seem that the human eye is a miracle, no matter its origins. Major biological functions and processes occurring in the retina show the intensity of the eye’s intricacy. After viewing the eye and reviewing its anatomical and physiological domain, arguments regarding its origins are more clearly seen and understood. Evolutionary theory, in terms of Darwin’s thoughts, theorized fossilization of animals, computer simulations of eye evolution, and new research on supposed prior genes occurring in lower life forms leading to human life. -
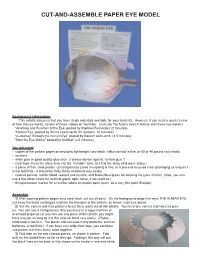
Cut-And-Assemble Paper Eye Model
CUT-AND-ASSEMBLE PAPER EYE MODEL Background information: This activity assumes that you have study materials available for your students. However, if you need a quick review of how the eye works, try one of these videos on YouTube. (Just use YouTube’s search feature with these key words.) “Anatomy and Function of the Eye: posted by Raphael Fernandez (2 minutes) “Human Eye” posted by Smart Learning for All (cartoon, 10 minutes) “A Journey Through the Human Eye” posted by Bausch and Lomb (2.5 minutes) “How the Eye Works” posted by AniMed (2.5 minutes) You will need: • copies of the pattern pages printed onto lightweight card stock (vellum bristol is fine, or 65 or 90 pound card stock) • scissors • white glue or good quality glue stick (I always advise against “school glue.”) • clear tape (I use the shiny kind, not the “invisible” kind, as I find the shiny kind more sticky.) • a piece of thin, clear plastic (a transparency [used in copiers] is fine, or a piece of recycled clear packaging as long as it is not too thick-- it should be fairly flimsy and bend very easily) • colored pencils: red for blood vessels and muscle, and brown/blue/green for coloring iris (your choice) (Also, you can use a few other colors for lacrimal gland, optic nerve, if you want to.) • thin permanent marker for a number labels on plastic parts (such as a very thin point Sharpie) Assembly: 1) After copying pattern pages onto card stock, cut out all parts. On the background page that says THE HUMAN EYE, cut away the black rectangles and trim the triangles at the bottom, as shown in picture above.