Symptoms of Age Related Macular Degeneration
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Vision Rehabi I Itation for Patients with Age Related Macular Degeneration
Vision rehabi I itation for GARY S. RUBIN patients with age related macular degeneration Epidemiology of low vision The over-representation of macular degeneration patients in the low-vision clinic is The epidemiology of vision impairment is dealt reflected in the chief complaints of those with in detail elsewhere.1 However, there is one referred for rehabilitation. A study of 1000 particularly salient factor that bears emphasis. consecutive patients seen at the Wilmer Low The prevalence of vision impairment increases Vision clinic indicated that 64% listed 'reading' dramatically with advancing age. Statistics as their chief complaint, while other activities compiled in the UK by the Royal National were identified by fewer than 8% of patients. Institute for the Blind2 indicate that there were Undoubtedly the bias towards reading approximately 1.1 million blind or partially problems results partly from the nature of the sighted persons in 1996, of whom 82% were 65 low-vision services offered. Those served by a years of age or older. Thus it is not surprising to community-based programme that includes learn that the major causes of vision impairment home visits might be more likely to report are age-related eye diseases. Fig. 1 illustrates the problems with activities of daily living, while a distribution of causes of vision impairment blind rehabilitation centre would be more likely 5 from three recent studies?- Approximately to address mobility issues. Nevertheless, most equal percentages are attributed to macular macular degeneration patients are referred to degeneration and cataract, with smaller hospital or optometry clinic services, and as percentages for glaucoma, diabetic retinopathy their overwhelming concern is with reading, and optic neuropathies. -

How Clean Is Your Capsule?
Eye (1989) 3, 678-684 How Clean is Your Capsule? W. T. GREEN and D. L. BOASE Portsmouth Summary Proliferation of residual lens epithelial cells is believed to be the major cause of pos terior capsule opacification following extracapsular cataract extraction. During sur gery these cells can be visualised with appropriate illumination facilitating their mechanical removal with the McIntyre cannula. When flat preparations of the anterior capsule are examined by light microscopy, the areas 'cleaned' of cells in this way appear transparent but scanning electron microscopy reveals tufts of remaining debris which may represent points of cellular attachment to the capsule. Control of lens epithelial cell proliferation is important for the future development of cataract surgery. The undoubted advantages of extracapsular and also on human cadaver eyes. A horizontal cataract extraction are offset in many patients capsulotomy in the upper part of the lens by posterior capsule opacification requiring allowed nucleus removal. Irrigation and caps ulotomy. Not only is this disappointing aspiration of the cortical lens material was for the patient, but the procedure carries a then carried out using a McIntyre cannula risk of serious complications. with Hartman's irrigation solution. During in The major cause of posterior capsule opac vitro surgery this was aided by first removing ification is proliferation of residual lens epi the entire cornea and iris to improve visual thelial cells. I If these cells could be removed at isation and explore different methods of the time of surgery we believe that the inci illumination. dence of posterior capsule opacification and The importance of illumination was first the need for subsequent capsulotomy would suspected when it was observed, during rou be reduced. -

Selective Attention Within the Foveola
ARTICLES Selective attention within the foveola Martina Poletti1 , Michele Rucci1,2 & Marisa Carrasco3,4 Efficient control of attentional resources and high-acuity vision are both fundamental for survival. Shifts in visual attention are known to covertly enhance processing at locations away from the center of gaze, where visual resolution is low. It is unknown, however, whether selective spatial attention operates where the observer is already looking—that is, within the high-acuity foveola, the small yet disproportionally important rod-free region of the retina. Using new methods for precisely controlling retinal stimulation, here we show that covert attention flexibly improves and speeds up both detection and discrimination at loci only a fraction of a degree apart within the foveola. These findings reveal a surprisingly precise control of attention and its involvement in fine spatial vision. They show that the commonly studied covert shifts of attention away from the fovea are the expression of a global mechanism that exerts its action across the entire visual field. Covert attention is essential for visual perception. Among its many previous studies. We then investigated the consequences of attention advantages, covert allocation of attentional resources increases con- for both detection (experiment 2) and discrimination (experiments trast sensitivity and spatial resolution, speeds information accrual and 3 and 4) tasks within the foveola. reaction times1–4, and alters the signal at the target location during saccade preparation5–7. Covert attention has been studied sometimes RESULTS in the parafovea (1°–5°) and mostly in the perifovea (5°–10°) and Experiment 1 consisted of a central spatial cueing task with para- periphery (>10° of eccentricity)—that is, far outside the foveola, the foveal stimuli (Fig. -

Macular Degeneration
DRIVEWELL Driving When You Have Macular Degeneration You have been a safe driver for years. For you, driving means freedom and control. As you get older, changes in your physical and mental health can affect how safely you drive. Macular degeneration (also known as age-related macular degeneration) damages the macula, a spot near the center of the retina (light-sensitive inner lining of the eyeball). It is a common eye problem among older drivers that makes it hard to drive safely. Age-related macular degeneration is the leading cause of new cases of blindness in people 65 and older. If you have macular degeneration, you may not notice any signs in the early stages. You may not know you have this condition until you lose your peripheral vision (what you see out of the corner of your eyes). In time it will affect your central vision, causing a dark or empty area in the center of your vision. How Can Macular Degeneration Affect the Way I Drive? • Your central vision may be dull and blurry. This can lead to loss of sharp vision. • You may not see the road, street signs, lane markers, and even people and bicyclists in the road. • You may need more bright light to see up close. • Colors may look less vivid or bright. • You may have trouble when you go from bright light to low light. • You may not be able to recognize people’s faces. What Should I Do if I Have Any of These Signs? As soon as you notice any of these warning signs: • Tell your family or someone close to you, especially if you have a family history of macular degeneration or have changes in your central vision. -

Detached and Torn Retina Retinal Detachments Occur in 1 out of 10,000 Americans Each Year
Detached and Torn Retina Retinal Detachments Occur in 1 Out of 10,000 Americans Each Year A retinal detachment is not as common as other eye conditions such as glaucoma or macular degeneration, however… it is just as serious and it is a vision threatening condition which should be treated as an emergency. Dr. Randy Katz, Florida Eye’s Diabetic Retinopathy, Retinal Detachment & Macular Degeneration Specialist says that the sooner a retinal tear or detachment is treated the better the chances of saving the vision in the eye. What Is a Retinal Detachment? The retina is the light-sensitive layer of tissue that lines the inside of the eye and sends visual messages through the optic nerve to the brain. When the retina detaches, it is lifted or pulled from its normal position. When this occurs, if not promptly treated, retinal detachment can cause permanent vision loss. In some cases there may be small areas of the retina that are torn. These areas, called retinal tears or retinal breaks, can lead to a retinal detachment. Vitreous gel, the clear material that fills the eyeball, is attached to the retina in the back of the eye. As we get older, the vitreous may change shape, pulling away from the retina. If the vitreous pulls a piece of the retina with it, it causes a retinal tear. Once a retinal tear occurs, vitreous fluid may seep through and lift the retina off the back wall of the eye, causing the retina to detach or pull away. 2 Are You At Risk for a Torn or Detached Retina? A retinal detachment can occur at any age, but it is more common in people over age 40. -

The Eye Is a Natural Optical Tool
KEY CONCEPT The eye is a natural optical tool. BEFORE, you learned NOW, you will learn •Mirrors and lenses focus light • How the eye depends on to form images natural lenses •Mirrors and lenses can alter • How artificial lenses can be images in useful ways used to correct vision problems VOCABULARY EXPLORE Focusing Vision cornea p. 607 How does the eye focus an image? pupil p. 607 retina p. 607 PROCEDURE 1 Position yourself so you can see an object about 6 meters (20 feet) away. 2 Close one eye, hold up your index finger, and bring it as close to your open eye as you can while keeping the finger clearly in focus. 3 Keeping your finger in place, look just to the side at the more distant object and focus your eye on it. 4 Without looking away from the more distant object, observe your finger. WHAT DO YOU THINK? • How does the nearby object look when you are focusing on something distant? • What might be happening in your eye to cause this change in the nearby object? The eye gathers and focuses light. The eyes of human beings and many other animals are natural optical tools that process visible light. Eyes transmit light, refract light, and respond to different wavelengths of light. Eyes contain natural lenses that focus images of objects. Eyes convert the energy of light waves into signals that can be sent to the brain. The brain interprets these signals as shape, brightness, and color. Altogether, these processes make vision possible. In this section, you will learn how the eye works. -

Retinal Ganglion Cell Loss Is Size Dependent in Experimental Glaucoma
Investigative Ophthalmology & Visual Science, Vol. 32, No. 3, March 1991 Copyright © Association for Research in Vision and Ophthalmology Retinal Ganglion Cell Loss Is Size Dependent in Experimental Glaucoma Yoseph Glovinsky,* Harry A. Quigley,f and Gregory R. Dunkelbergerf Thirty-two areas located in the temporal midperipheral retina were evaluated in whole-mount prepara- tions from four monkeys with monocular experimental glaucoma. Diameter frequency distributions of remaining ganglion cells in the glaucomatous eye were compared with corresponding areas in the normal fellow eye. Large cells were significantly more vulnerable at each stage of cell damage as determined by linear-regression analysis. The magnitude of size-dependent loss was moderate at an early stage (20% loss), peaked at 50% total cell loss, and decreased in advanced damage (70% loss). In glaucomatous eyes, the lower retina had significantly more large cell loss than the corresponding areas of the upper retina. In optic nerve zones that matched the retinal areas studied, large axons selectively were damaged first. Psychophysical testing aimed at functions subserved by larger ganglion cells is recommended for detection and follow-up of early glaucoma; however, assessment of functions unique to small cells is more appropriate for detecting change in advanced glaucoma. Invest Ophthalmol Vis Sci 32:484-491, 1991 Current psychophysical tests do not detect glau- tage of ideal cellular preservation. Eyes with mild, comatous damage until a substantial minority of reti- moderate, and late damage were evaluated. In addi- nal ganglion cells have died.1'2 To develop more sen- tion, we correlated the damage patterns in the retinas sitive tests, a comprehensive understanding of the and optic nerves of the glaucomatous eyes. -

The Complexity and Origins of the Human Eye: a Brief Study on the Anatomy, Physiology, and Origin of the Eye
Running Head: THE COMPLEX HUMAN EYE 1 The Complexity and Origins of the Human Eye: A Brief Study on the Anatomy, Physiology, and Origin of the Eye Evan Sebastian A Senior Thesis submitted in partial fulfillment of the requirements for graduation in the Honors Program Liberty University Spring 2010 THE COMPLEX HUMAN EYE 2 Acceptance of Senior Honors Thesis This Senior Honors Thesis is accepted in partial fulfillment of the requirements for graduation from the Honors Program of Liberty University. ______________________________ David A. Titcomb, PT, DPT Thesis Chair ______________________________ David DeWitt, Ph.D. Committee Member ______________________________ Garth McGibbon, M.S. Committee Member ______________________________ Marilyn Gadomski, Ph.D. Assistant Honors Director ______________________________ Date THE COMPLEX HUMAN EYE 3 Abstract The human eye has been the cause of much controversy in regards to its complexity and how the human eye came to be. Through following and discussing the anatomical and physiological functions of the eye, a better understanding of the argument of origins can be seen. The anatomy of the human eye and its many functions are clearly seen, through its complexity. When observing the intricacy of vision and all of the different aspects and connections, it does seem that the human eye is a miracle, no matter its origins. Major biological functions and processes occurring in the retina show the intensity of the eye’s intricacy. After viewing the eye and reviewing its anatomical and physiological domain, arguments regarding its origins are more clearly seen and understood. Evolutionary theory, in terms of Darwin’s thoughts, theorized fossilization of animals, computer simulations of eye evolution, and new research on supposed prior genes occurring in lower life forms leading to human life. -
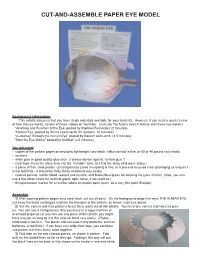
Cut-And-Assemble Paper Eye Model
CUT-AND-ASSEMBLE PAPER EYE MODEL Background information: This activity assumes that you have study materials available for your students. However, if you need a quick review of how the eye works, try one of these videos on YouTube. (Just use YouTube’s search feature with these key words.) “Anatomy and Function of the Eye: posted by Raphael Fernandez (2 minutes) “Human Eye” posted by Smart Learning for All (cartoon, 10 minutes) “A Journey Through the Human Eye” posted by Bausch and Lomb (2.5 minutes) “How the Eye Works” posted by AniMed (2.5 minutes) You will need: • copies of the pattern pages printed onto lightweight card stock (vellum bristol is fine, or 65 or 90 pound card stock) • scissors • white glue or good quality glue stick (I always advise against “school glue.”) • clear tape (I use the shiny kind, not the “invisible” kind, as I find the shiny kind more sticky.) • a piece of thin, clear plastic (a transparency [used in copiers] is fine, or a piece of recycled clear packaging as long as it is not too thick-- it should be fairly flimsy and bend very easily) • colored pencils: red for blood vessels and muscle, and brown/blue/green for coloring iris (your choice) (Also, you can use a few other colors for lacrimal gland, optic nerve, if you want to.) • thin permanent marker for a number labels on plastic parts (such as a very thin point Sharpie) Assembly: 1) After copying pattern pages onto card stock, cut out all parts. On the background page that says THE HUMAN EYE, cut away the black rectangles and trim the triangles at the bottom, as shown in picture above. -

Foveola Nonpeeling Internal Limiting Membrane Surgery to Prevent Inner Retinal Damages in Early Stage 2 Idiopathic Macula Hole
Graefes Arch Clin Exp Ophthalmol DOI 10.1007/s00417-014-2613-7 RETINAL DISORDERS Foveola nonpeeling internal limiting membrane surgery to prevent inner retinal damages in early stage 2 idiopathic macula hole Tzyy-Chang Ho & Chung-May Yang & Jen-Shang Huang & Chang-Hao Yang & Muh-Shy Chen Received: 29 October 2013 /Revised: 26 February 2014 /Accepted: 5 March 2014 # Springer-Verlag Berlin Heidelberg 2014 Abstract Keywords Fovea . Foveola . Internal limiting membrane . Purpose The purpose of this study was to investigate and macular hole . Müller cell . Vitrectomy present the results of a new vitrectomy technique to preserve the foveolar internal limiting membrane (ILM) during ILM peeling in early stage 2 macular holes (MH). Introduction Methods The medical records of 28 consecutive patients (28 eyes) with early stage 2 MH were retrospectively reviewed It is generally agreed that internal limiting membrane (ILM) and randomly divided into two groups by the extent of ILM peeling is important in achieving closure of macular holes peeing. Group 1: foveolar ILM nonpeeling group (14 eyes), (MH) [1]. An autopsy study of a patient who had undergone and group 2: total peeling of foveal ILM group (14 eyes). A successful MH closure showed an area of absent ILM sur- donut-shaped ILM was peeled off, leaving a 400-μm-diameter rounding the sealed MH [2]. ILM over foveola in group 1. The present ILM peeling surgery of idiopathic MH in- Results Smooth and symmetric umbo foveolar contour was cludes total removal of foveolar ILM. However, removal of restored without inner retinal dimpling in all eyes in group 1, all the ILM over the foveola causes anatomical changes of the but not in group 2. -

Scleral Lenses and Eye Health
Scleral Lenses and Eye Health Anatomy and Function of the Human Eye How Scleral Lenses Interact with the Ocular Surface Just as the skin protects the human body, the ocular surface protects the human Scleral lenses are large-diameter lenses designed to vault the cornea and rest on the conjunctival tissue sitting on eye. The ocular surface is made up of the cornea, the conjunctiva, the tear film, top of the sclera. The space between the back surface of the lens and the cornea acts as a fluid reservoir. Scleral and the glands that produce tears, oils, and mucus in the tear film. lenses can range in size from 13mm to 19mm, although larger diameter lenses may be designed for patients with more severe eye conditions. Due to their size, scleral lenses consist SCLERA: The sclera is the white outer wall of the eye. It is SCLERAL LENS made of collagen fibers that are arranged for strength rather of at least two zones: than transmission of light. OPTIC ZONE The optic zone vaults over the cornea CORNEA: The cornea is the front center portion of the outer Cross section of FLUID RESERVOIR wall of the eye. It is made of collagen fibers that are arranged in the eye shows The haptic zone rests on the conjunctiva such a way so that the cornea is clear. The cornea bends light the cornea, overlying the sclera as it enters the eye so that the light is focused on the retina. conjunctiva, and sclera as CORNEA The cornea has a protective surface layer called the epithelium. -

Macular Hole
Macular Hole What is a macular hole? A macular hole is a small full-thickness defect in macula, the most important region of your retina (Figure 1 and Figure 2). The macula is the center of the retina, which is the light sensing part of the back of the eye. Formation of this hole causes loss of central vision (reading, driving, recognizing faces is affected). Figure 1 – Normal Macula Figure 2 – Macular hole What types of symptoms to patients with macular hole have? Symptoms vary based the size of the hole. The most typical symptoms are: • Distortion of vision (called “metamorphopsia”) – letters look crooked • Blurred vision or loss of visual acuity • Dark spot at center of vision (“central scotoma”) – patients describe missing letters in words when looking right at the word. These dark spots are different than “floaters” as they do not move around. • Patient often first notice the vision loss when they cover-up the unaffected/good eye GEORGIA EYE INSTITUTE – RETINA SERVICE Dr. Robert T. King and Dr. Robin Ray Savannah, GA | phone 912-354-4800 | website www.gaeyeinstitute.com What causes a macular hole? The most common cause of a macular hole is a posterior vitreous degeneration. This is when the vitreous gel that fills the center of the eye liquefies and separates from the back surface of the inside of the eye (the retina). This results in traction/pulling in the central macula. If there is enough traction a hole forms. Direct ocular trauma by a blunt force, like a tennis ball, can cause macular holes to form as well.