Motor Neurons of Spinal Cord
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Primary Lateral Sclerosis, Upper Motor Neuron Dominant Amyotrophic Lateral Sclerosis, and Hereditary Spastic Paraplegia
brain sciences Review Upper Motor Neuron Disorders: Primary Lateral Sclerosis, Upper Motor Neuron Dominant Amyotrophic Lateral Sclerosis, and Hereditary Spastic Paraplegia Timothy Fullam and Jeffrey Statland * Department of Neurology, University of Kansas Medical Center, Kansas, KS 66160, USA; [email protected] * Correspondence: [email protected] Abstract: Following the exclusion of potentially reversible causes, the differential for those patients presenting with a predominant upper motor neuron syndrome includes primary lateral sclerosis (PLS), hereditary spastic paraplegia (HSP), or upper motor neuron dominant ALS (UMNdALS). Differentiation of these disorders in the early phases of disease remains challenging. While no single clinical or diagnostic tests is specific, there are several developing biomarkers and neuroimaging technologies which may help distinguish PLS from HSP and UMNdALS. Recent consensus diagnostic criteria and use of evolving technologies will allow more precise delineation of PLS from other upper motor neuron disorders and aid in the targeting of potentially disease-modifying therapeutics. Keywords: primary lateral sclerosis; amyotrophic lateral sclerosis; hereditary spastic paraplegia Citation: Fullam, T.; Statland, J. Upper Motor Neuron Disorders: Primary Lateral Sclerosis, Upper 1. Introduction Motor Neuron Dominant Jean-Martin Charcot (1825–1893) and Wilhelm Erb (1840–1921) are credited with first Amyotrophic Lateral Sclerosis, and describing a distinct clinical syndrome of upper motor neuron (UMN) tract degeneration in Hereditary Spastic Paraplegia. Brain isolation with symptoms including spasticity, hyperreflexia, and mild weakness [1,2]. Many Sci. 2021, 11, 611. https:// of the earliest described cases included cases of hereditary spastic paraplegia, amyotrophic doi.org/10.3390/brainsci11050611 lateral sclerosis, and underrecognized structural, infectious, or inflammatory etiologies for upper motor neuron dysfunction which have since become routinely diagnosed with the Academic Editors: P. -
Corticospinal Fibers
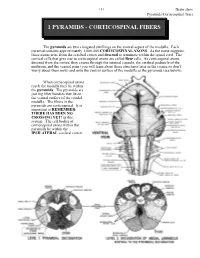
151 Brain stem Pyramids/Corticospinal Tract 1 PYRAMIDS - CORTICOSPINAL FIBERS The pyramids are two elongated swellings on the ventral aspect of the medulla. Each pyramid contains approximately 1,000,000 CORTICOSPINAL AXONS. As the name suggests, these axons arise from the cerebral cortex and descend to terminate within the spinal cord. The cortical cells that give rise to corticospinal axons are called Betz cells. As corticospinal axons descend from the cortex, they course through the internal capsule, the cerebral peduncle of the midbrain, and the ventral pons (you will learn about these structures later in the course so don’t worry about them now) and onto the ventral surface of the medulla as the pyramids (see below). When corticospinal axons reach the medulla they lie within the pyramids. The pyramids are just big fiber bundles that lie on the ventral surface of the caudal medulla. The fibers in the pyramids are corticospinal. It is important to REMEMBER: THERE HAS BEEN NO CROSSING YET! in this system. The cell bodies of corticospinal axons within the pyramids lie within the IPSILATERAL cerebral cortex. Brain stem 152 Pyramids/Corticospinal Tract At the most caudal pole of the pyramids the corticospinal axons cross over the midline and now continue their descent on the contralateral (to the cell of origin) side. This crossover point is called the PYRAMIDAL DECUSSATION. The crossing fibers enter the lateral funiculus of the spinal cord where they are called the LATERAL CORTICOSPINAL TRACT (“corticospinal” is not good enough, you have to call them lateral corticospinal; LCST - remember this one??). LCST axons exit the tract to terminate upon neurons in the spinal cord gray matter along its entire length. -

Visualization of the Pyramidal Decussation Utilizing Diffusion
OPEN ACCESS RESEARCH Visualization of the pyramidal decussation utilizing diffusion tensor imaging: a feasibility study utilizing generalized q-sampling imaging Erik H Middlebrooks1,*, Jeffrey A Bennett1, Sharatchandra Bidari1, and Alissa Old Crow1 1Department of Radiology, University of Florida College of Medicine, Gainesville, Florida, USA *corresponding author ([email protected]) Abstract Background: The delineating point of the end of the brainstem and beginning of the spinal cord is known as the cervicomedullary junction (CMJ). This point is defined by the decussation of the pyramidal tracts. Abnormal configuration and location of the CMJ have both been implicated in disease processes such as Chiari malformation. Unfortunately, the CMJ is not directly visualized on contemporary imaging techniques. Diffusion tensor imaging (DTI) has given us the ability to directly visualize white matter tracts, but suffers from difficulties with visualizing crossing fibers. Many advanced techniques for visualizing crossing fibers utilize substantially long imaging times or non-clinical magnet strengths making clinical applicability limited. Objective: This study inves- tigates the use of generalized q-sampling imaging with diffusion decomposition on standard DTI acquisitions at 3 Tesla to demonstrate the pyramidal decussation. Methods: Three differing DTI protocols were analyzed in vivo with scan times of 17 minutes, 10 minutes, and 5.5 minutes. Data was processed with standard DTI post-processing, as well as generalized q-sampling imaging with diffusion decomposition. Results: The results of the study show that the pyramidal decussation can be reliably visualized using generalized q-sampling imaging and diffusion decomposition with scan times as low at 10 minutes. Conclusion: Utilizing generalized q-sampling post-processing, the pyramidal decussation can be reliably visualized using clinically feasible DTI sequences with scan times as low as 10 minutes. -

Medical Study Center
https://www.facebook.com/Medicalstudycenter2012 https://www.facebook.com/Medicalstudycenter2012 Notes On CNS Physiology Gray Matter of Spinal Cord: in the spinal cord gray matter is in the form of H shaped pillars which can be divided into three types of columns i.e. anterior horn or ventral horn, posterior horn or dorsal horn and in segments from T1 to L2 there is lateral horn. Neurons in these horns are Ventral Horn: Two groups of neurons Alpha motor neurons which are large multi polar neurons and their nerve fibers are alpha efferents which innervate skeletal muscle. Gamma neurons present in ventral horn are small and multi polar neurons and there nerve fibers are gamma efferents which innervate the intrafusal fibers of the muscle spindles. Both these alpha and gamma efferents come out of the spinal cord through ventral root of spinal nerves. Dorsal Horn: there are 4 groups of neurons 1. Substantia gelatinosa: this group of neurons is present at the apex of the posterior gray column. These neurons receive afferent nerve fibers carrying impulses of pain, temperature and crude touch. 2. Nucleus Proprius: this group is located anterior to the first group. These neurons receive afferent nerve fibers carrying impulses of proprioception and two point tactile discrimination. 3. Clarke’s column or nucleus dorsalis: this group is present at the base of the posterior gray column. These neurons are present in segments from T1 to L3, 4. These neurons are part of spinocerebellar tract and these receive afferent nerve fibers from spinocerebellar tract. 4. Visceral Afferent Nucleus: Present at the base of the posterior horn lateral to the clarke’s column. -

Auditory and Vestibular Systems Objective • to Learn the Functional
Auditory and Vestibular Systems Objective • To learn the functional organization of the auditory and vestibular systems • To understand how one can use changes in auditory function following injury to localize the site of a lesion • To begin to learn the vestibular pathways, as a prelude to studying motor pathways controlling balance in a later lab. Ch 7 Key Figs: 7-1; 7-2; 7-4; 7-5 Clinical Case #2 Hearing loss and dizziness; CC4-1 Self evaluation • Be able to identify all structures listed in key terms and describe briefly their principal functions • Use neuroanatomy on the web to test your understanding ************************************************************************************** List of media F-5 Vestibular efferent connections The first order neurons of the vestibular system are bipolar cells whose cell bodies are located in the vestibular ganglion in the internal ear (NTA Fig. 7-3). The distal processes of these cells contact the receptor hair cells located within the ampulae of the semicircular canals and the utricle and saccule. The central processes of the bipolar cells constitute the vestibular portion of the vestibulocochlear (VIIIth cranial) nerve. Most of these primary vestibular afferents enter the ipsilateral brain stem inferior to the inferior cerebellar peduncle to terminate in the vestibular nuclear complex, which is located in the medulla and caudal pons. The vestibular nuclear complex (NTA Figs, 7-2, 7-3), which lies in the floor of the fourth ventricle, contains four nuclei: 1) the superior vestibular nucleus; 2) the inferior vestibular nucleus; 3) the lateral vestibular nucleus; and 4) the medial vestibular nucleus. Vestibular nuclei give rise to secondary fibers that project to the cerebellum, certain motor cranial nerve nuclei, the reticular formation, all spinal levels, and the thalamus. -

Reaction to Injury & Regeneration
Reaction to Injury & Regeneration Steven McLoon Department of Neuroscience University of Minnesota 1 The adult mammalian central nervous system has the lowest regenerative capacity of all organ systems. 2 3 Reaction to Axotomy Function distal to the axon cut is lost. (immediate) 4 Reaction to Axotomy • Spinal cord injury results in an immediate loss of sensation and muscle paralysis below the level of the injury. Spinal cord injury can be partial or complete, and the sensory/motor loss depends on which axons are injured. • Peripheral nerve injury results in an immediate loss of sensation and muscle paralysis in the areas served by the injured nerve distal to the site of injury. 5 Reaction to Axotomy K+ leaks out of the cell and Na+/Ca++ leak into the cell. (seconds) Proximal and distal segments of the axon reseal slightly away from the cut ends. (~2 hrs) Subsequent anterograde & retrograde effects … 6 Anterograde Effects (Wallerian Degeneration) Axon swells. (within 12 hrs) Axolema and mitochondria begin to fragment. (within 3 days) Myelin not associated with a viable axon begins to fragment. (within 1 wk) Astrocytes or Schwann cells proliferate (within 1 wk), which can continue for over a month. Results in >10x the original number of cells. Microglia (or macrophages in the PNS) invade the area. Glia and microglia phagocytize debris. (1 month in PNS; >3 months in CNS) 7 Anterograde Effects (Wallerian Degeneration) Degradation of the axon involves self proteolysis: In the ‘Wallerian degeneration slow’ (Wlds) mouse mutation, the distal portion of severed axons are slow to degenerate; the dominant mutation involves a ubiquitin regulatory enzyme. -

Acupuncture and Pain Management
IN-DEPTH: INTEGRATIVE MEDICINE (COMPLEMENTARY & ALTERNATIVE MEDICINE) Acupuncture and Pain Management James D. Kenney, DVM There is a large and expanding body of scientific evidence supporting the use of acupuncture in pain management. In the last decade, our understanding of how the brain processes acupuncture anal- gesia has undergone considerable development. Profound studies on neural mechanisms underlying acupuncture analgesia have evolved rapidly and predominately focus on cellular and molecular substrate and functional brain imaging. The currently understood mechanisms of acupuncture analgesia are complex and involve direct and indirect neurohumoral effects that block pain percep- tion, reduce the pain response, relieve muscle spasms, and reduce inflammation. The analgesic mechanisms of acupuncture involve the spinal cord grey matter, hypothalamic-pituitary axis, mid- brain periaqueductal grey matter, medulla oblongata, limbic system, cerebral cortex, and autonomic nervous system. Electroacupuncture (EA) stimulation of these sites results in activation of descend- ing pathways that inhibit pain through endogenous opioid, noradrenergic, and serotonergic sys- tems. There are growing numbers of human trials supporting the use of acupuncture as an evidence- based practice for pain management in human medicine. There are many studies that support the efficacy of acupuncture for low back pain, neck pain, chronic idiopathic and migraine headaches, knee pain, shoulder pain, fibromyalgia, temporomandibular joint pain, and postoperative pain. Although the number of well-designed, controlled clinical research studies in veterinary medicine is lagging behind the number of studies in human medicine, much of the basic science research has been done in animals with neurophysiology that is more similar to veterinary patients than humans. Although there is research to support EA as an evidence-based practice for the control of back pain in horses, additional studies are needed in other clinical situations in veterinary medicine where pain manage- ment is required. -

Cortex Brainstem Spinal Cord Thalamus Cerebellum Basal Ganglia
Harvard-MIT Division of Health Sciences and Technology HST.131: Introduction to Neuroscience Course Director: Dr. David Corey Motor Systems I 1 Emad Eskandar, MD Motor Systems I - Muscles & Spinal Cord Introduction Normal motor function requires the coordination of multiple inter-elated areas of the CNS. Understanding the contributions of these areas to generating movements and the disturbances that arise from their pathology are important challenges for the clinician and the scientist. Despite the importance of diseases that cause disorders of movement, the precise function of many of these areas is not completely clear. The main constituents of the motor system are the cortex, basal ganglia, cerebellum, brainstem, and spinal cord. Cortex Basal Ganglia Cerebellum Thalamus Brainstem Spinal Cord In very broad terms, cortical motor areas initiate voluntary movements. The cortex projects to the spinal cord directly, through the corticospinal tract - also known as the pyramidal tract, or indirectly through relay areas in the brain stem. The cortical output is modified by two parallel but separate re entrant side loops. One loop involves the basal ganglia while the other loop involves the cerebellum. The final outputs for the entire system are the alpha motor neurons of the spinal cord, also called the Lower Motor Neurons. Cortex: Planning and initiation of voluntary movements and integration of inputs from other brain areas. Basal Ganglia: Enforcement of desired movements and suppression of undesired movements. Cerebellum: Timing and precision of fine movements, adjusting ongoing movements, motor learning of skilled tasks Brain Stem: Control of balance and posture, coordination of head, neck and eye movements, motor outflow of cranial nerves Spinal Cord: Spontaneous reflexes, rhythmic movements, motor outflow to body. -

Testing Upper Motor Neuron Function in Amyotrophic Lateral Sclerosis: the Most Difficult Task of Neurophysiology
Scientific Commentaries Brain 2012: 135; 2579–2584 | 2581 Testing upper motor neuron function in amyotrophic lateral sclerosis: the most difficult task of neurophysiology Clinical signs of upper motor neuron involvement are an essential contrast is potentially very effective for exploring neuronal inter- observation to support the diagnosis of amyotrophic lateral scler- connection dysfunction in amyotrophic lateral sclerosis, but still osis. However, clinical signs of upper motor neuron can be difficult needs more investigation; and novel neuroinflammatory and in- to elicit in patients with motor neuron disease. One postulated hibitory positron emission tomography ligands might have utility reason for this problem is the presence of marked limb weakness in the future (Turner, 2012). However, expense and practical Downloaded from https://academic.oup.com/brain/article/135/9/2581/331426 by guest on 23 September 2021 and amyotrophy in motor neuron disease. This has been observed issues limit the use of these sophisticated imaging techniques to in patients with genetic mutations and clear-cut pathological evi- a few highly specialized centres. Thus far, therefore, no method to dence of upper and lower motor neuron degeneration. Less com- investigate upper motor neuron function has proved useful and monly, it has been recognized that the pattern of upper motor applicable as a measure of efficacy in clinical trials, despite some neuron lesion in amyotrophic lateral sclerosis is rather different enthusiasm for the threshold tracking transcranial magnetic stimu- from other conditions, in which there is damage to other descend- lation as a marker of early diagnosis. ing motor fibres from extra-Rolandic motor cortical areas (Swash, EMG is also not the preferred method for assessing upper motor 2012). -

Amyotrophic Lateral Sclerosis (ALS)
Amyotrophic Lateral Sclerosis (ALS) There are multiple motor neuron diseases. Each has its own defining features and many characteristics that are shared by all of them: Degenerative disease of the nervous system Progressive despite treatments and therapies Begins quietly after a period of normal nervous system function ALS is the most common motor neuron disease. One of its defining features is that it is a motor neuron disease that affects both upper and lower motor neurons. Anatomical Involvement ALS is a disease that causes muscle atrophy in the muscles of the extremities, trunk, mouth and face. In some instances mood and memory function are also affected. The disease operates by attacking the motor neurons located in the central nervous system which direct voluntary muscle function. The impulses that control the muscle function originate with the upper motor neurons in the brain and continue along efferent (descending) CNS pathways through the brainstem into the spinal cord. The disease does not affect the sensory or autonomic system because ALS affects only the motor systems. ALS is a disease of both upper and lower motor neurons and is diagnosed in part through the use of NCS/EMG which evaluates lower motor neuron function. All motor neurons are upper motor neurons so long as they are encased in the brain or spinal cord. Once the neuron exits the spinal cord, it operates as a lower motor neuron. 1 Upper Motor Neurons The upper motor neurons are derived from corticospinal and corticobulbar fibers that originate in the brain’s primary motor cortex. They are responsible for carrying impulses for voluntary motor activity from the cerebral cortex to the lower motor neurons. -

Upper and Lower Motor Neuron Lesions in the Upper Extremity Muscles of Tetraplegics1
Paraplegia (1976), 14, II 5-121 UPPER AND LOWER MOTOR NEURON LESIONS IN THE UPPER EXTREMITY MUSCLES OF TETRAPLEGICS1 By P. H. PECKHAM, J. T. MORTIMER and E. B. MARSOLAIS* Engineering Design Center and Department of Biomedical Engineering, *Department of Orthopaedic Surgery, Case Western Reserve University, Cleveland, Ohio 44[06 VIABILITY of the lower motor neuron is imperative if paralysed muscles are to be electrically activated for functional use. Recently, functional use of the hand has been obtained through excitation of paralysed forearm muscles (Peckham et al., 1973; Mortimer & Peckham, 1973). These advantages were achieved with subjects whose stimulated muscles had little or no involvement of the peripheral nerve, i.e. an upper motor neuron lesion. In general, however, one could expect some involvement of the lower motor neuron to be present because trauma resulting from the spinal cord injury often extends one or more segments rostral and caudal to the site of damage (Guttmann, 1973) and may involve the cell bodies of peripheral nerves which exit the spinal cord near the level of injury or the spinal nerves themselves (Haymaker, 1953). The present study was designed to investigate the muscles of a small popula tion of high level spinal cord injury patients in order to determine those that potentially could be used for functional electrical stimulation. Specifically, the objective of this study was to evaluate the nature of the muscle innervation of the forearm and hand muscles of quadriplegic patients. Methods Subjects. These studies were carried out on 24 tetraplegic patients. The post-injury period ranged from 3 months to 18 years, most being tested less than I year post-injury. -

Quantifying Nerve Decussation Abnormalities in the Optic Chiasm T Robert J
NeuroImage: Clinical 24 (2019) 102055 Contents lists available at ScienceDirect NeuroImage: Clinical journal homepage: www.elsevier.com/locate/ynicl Quantifying nerve decussation abnormalities in the optic chiasm T Robert J. Puzniaka, Khazar Ahmadia, Jörn Kaufmannb, Andre Gouwsc, Antony B. Morlandc,d, ⁎ Franco Pestillie,1, Michael B. Hoffmanna,f,1, a Department of Ophthalmology, Otto-von-Guericke-University Magdeburg, Magdeburg, Germany b Department of Neurology, Otto-von-Guericke-University Magdeburg, Magdeburg, Germany c York Neuroimaging Centre, Department of Psychology, University of York, York, United Kingdom d York Biomedical Research Institute, University of York, York, United Kingdom e Department of Psychological and Brain Sciences, Program in Neuroscience and Program in Cognitive Science, Indiana University, Bloomington, USA f Center for Behavioral Brain Sciences, Magdeburg, Germany ARTICLE INFO ABSTRACT Keywords: Objective: The human optic chiasm comprises partially crossing optic nerve fibers. Here we used diffusion MRI Optic chiasm (dMRI) for the in-vivo identification of the abnormally high proportion of crossing fibers found intheoptic Albinism chiasm of people with albinism. Diffusion MRI Methods: In 9 individuals with albinism and 8 controls high-resolution 3T dMRI data was acquired and analyzed Functional MRI with a set of methods for signal modeling [Diffusion Tensor (DT) and Constrained Spherical Deconvolution Crossing nerves (CSD)], tractography, and streamline filtering (LiFE, COMMIT, and SIFT2). The number of crossing andnon- crossing streamlines and their weights after filtering entered ROC-analyses to compare the discriminative power of the methods based on the area under the curve (AUC). The dMRI results were cross-validated with fMRI estimates of misrouting in a subset of 6 albinotic individuals.