Amyotrophic Lateral Sclerosis (ALS)
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Clinically Undetected Motor Neuron Disease in Pathologically Proven Frontotemporal Lobar Degeneration with Motor Neuron Disease
ORIGINAL CONTRIBUTION Clinically Undetected Motor Neuron Disease in Pathologically Proven Frontotemporal Lobar Degeneration With Motor Neuron Disease Keith A. Josephs, MST, MD; Joseph E. Parisi, MD; David S. Knopman, MD; Bradley F. Boeve, MD; Ronald C. Petersen, MD, PhD; Dennis W. Dickson, MD Background: Frontotemporal lobar degeneration with evidence of motor neuron disease. Semiquantitative motor neuron disease (FTLD-MND) is a pathological analysis of motor and extramotor pathological findings entity characterized by motor neuron degeneration and revealed a spectrum of pathological changes underlying frontotemporal lobar degeneration. The ability to detect FTLD-MND. Hippocampal sclerosis, predominantly of the clinical signs of dementia and motor neuron disease the subiculum, was a significantly more frequent occur- in pathologically confirmed FTLD-MND has not been rence in the cases without clinical evidence of motor assessed. neuron disease (PϽ.01). In addition, neuronal loss, gliosis, and corticospinal tract degeneration were less Objectives: To determine if all cases of pathologically severe in the other 3 cases without clinical evidence of confirmed FTLD-MND have clinical evidence of fronto- motor neuron disease. temporal dementia and motor neuron disease, and to de- termine the possible reasons for misdiagnosis. Conclusions: Clinical diagnostic sensitivity for the el- ements of FTLD-MND is modest and may be affected by Method: Review of historical records and semiquantita- the fact that FTLD-MND represents a spectrum of patho- tive analysis of the motor and extramotor pathological find- logical findings, rather than a single homogeneous en- ings of all cases of pathologically confirmed FTLD-MND. tity. Detection of signs of clinical motor neuron disease is also difficult when motor neuron degeneration is mild Results: From a total of 17 cases of pathologically con- and in patients with hippocampal sclerosis. -

Primary Lateral Sclerosis, Upper Motor Neuron Dominant Amyotrophic Lateral Sclerosis, and Hereditary Spastic Paraplegia
brain sciences Review Upper Motor Neuron Disorders: Primary Lateral Sclerosis, Upper Motor Neuron Dominant Amyotrophic Lateral Sclerosis, and Hereditary Spastic Paraplegia Timothy Fullam and Jeffrey Statland * Department of Neurology, University of Kansas Medical Center, Kansas, KS 66160, USA; [email protected] * Correspondence: [email protected] Abstract: Following the exclusion of potentially reversible causes, the differential for those patients presenting with a predominant upper motor neuron syndrome includes primary lateral sclerosis (PLS), hereditary spastic paraplegia (HSP), or upper motor neuron dominant ALS (UMNdALS). Differentiation of these disorders in the early phases of disease remains challenging. While no single clinical or diagnostic tests is specific, there are several developing biomarkers and neuroimaging technologies which may help distinguish PLS from HSP and UMNdALS. Recent consensus diagnostic criteria and use of evolving technologies will allow more precise delineation of PLS from other upper motor neuron disorders and aid in the targeting of potentially disease-modifying therapeutics. Keywords: primary lateral sclerosis; amyotrophic lateral sclerosis; hereditary spastic paraplegia Citation: Fullam, T.; Statland, J. Upper Motor Neuron Disorders: Primary Lateral Sclerosis, Upper 1. Introduction Motor Neuron Dominant Jean-Martin Charcot (1825–1893) and Wilhelm Erb (1840–1921) are credited with first Amyotrophic Lateral Sclerosis, and describing a distinct clinical syndrome of upper motor neuron (UMN) tract degeneration in Hereditary Spastic Paraplegia. Brain isolation with symptoms including spasticity, hyperreflexia, and mild weakness [1,2]. Many Sci. 2021, 11, 611. https:// of the earliest described cases included cases of hereditary spastic paraplegia, amyotrophic doi.org/10.3390/brainsci11050611 lateral sclerosis, and underrecognized structural, infectious, or inflammatory etiologies for upper motor neuron dysfunction which have since become routinely diagnosed with the Academic Editors: P. -
Corticospinal Fibers
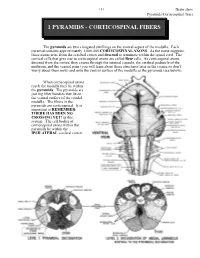
151 Brain stem Pyramids/Corticospinal Tract 1 PYRAMIDS - CORTICOSPINAL FIBERS The pyramids are two elongated swellings on the ventral aspect of the medulla. Each pyramid contains approximately 1,000,000 CORTICOSPINAL AXONS. As the name suggests, these axons arise from the cerebral cortex and descend to terminate within the spinal cord. The cortical cells that give rise to corticospinal axons are called Betz cells. As corticospinal axons descend from the cortex, they course through the internal capsule, the cerebral peduncle of the midbrain, and the ventral pons (you will learn about these structures later in the course so don’t worry about them now) and onto the ventral surface of the medulla as the pyramids (see below). When corticospinal axons reach the medulla they lie within the pyramids. The pyramids are just big fiber bundles that lie on the ventral surface of the caudal medulla. The fibers in the pyramids are corticospinal. It is important to REMEMBER: THERE HAS BEEN NO CROSSING YET! in this system. The cell bodies of corticospinal axons within the pyramids lie within the IPSILATERAL cerebral cortex. Brain stem 152 Pyramids/Corticospinal Tract At the most caudal pole of the pyramids the corticospinal axons cross over the midline and now continue their descent on the contralateral (to the cell of origin) side. This crossover point is called the PYRAMIDAL DECUSSATION. The crossing fibers enter the lateral funiculus of the spinal cord where they are called the LATERAL CORTICOSPINAL TRACT (“corticospinal” is not good enough, you have to call them lateral corticospinal; LCST - remember this one??). LCST axons exit the tract to terminate upon neurons in the spinal cord gray matter along its entire length. -

Spinal Tracts.Pdf
Spinal Tracts Andreas Talgø Lie Illustrations by: Peder Olai Skjeflo Holman Previous material: Maja Solbakken Definitions to bring home Nerve Ganglion Neuron Nucleus Tract Collection neurons Collection of nerve A single cell Collection of Collection of axons that transmits cell bodies in the transmitting nerve cell bodies in traveling up or sensation or motor PNS, typically linked electrical impluses. the CNS, typically down the spinal impulses depending by synapses. linked by synapses. cord, depending on the function and Location: both on function destination. Location: PNS Location: CNS and destination. Location: PNS Location: CNS - does it matter? Tract - highway to pass anatomy exam? • Highway = Tract • Lane = Neuron • Car = Signal Slow... Fast!! Just to make sure... • Ipsilateral or contralateral • Ventral = anterior • Dorsal = posterior High yield points to understand • What does the tract transmit - Motor or sensory? If sensory: which sensation? • Where does the neurones synapse - 1.st, 2nd and 3rd order neron? Which ganglion/nuclei? • Where there are decussations - If there are any decussations at all? ASCENDING / SENSORY TRACTS Sensations * Temperature NOT transmitted by the tracts: * Pressure * Visualization * Pain * Audition * Fine touch * Olfaction * Crude touch * Gustation * Proprioception * Vibration Sensations Precise sensation Primitive sensation Fine touch Crude touch Pressure Pain Vibration Temperature Proprioception Other: sexual, itching, tickling Ascending tracts / Sensory tracts Dorsal coulmn Lat. Spinothalamic Ant. -

ALS and Other Motor Neuron Diseases Can Represent Diagnostic Challenges
Review Article Address correspondence to Dr Ezgi Tiryaki, Hennepin ALS and Other Motor County Medical Center, Department of Neurology, 701 Park Avenue P5-200, Neuron Diseases Minneapolis, MN 55415, [email protected]. Ezgi Tiryaki, MD; Holli A. Horak, MD, FAAN Relationship Disclosure: Dr Tiryaki’s institution receives support from The ALS Association. Dr Horak’s ABSTRACT institution receives a grant from the Centers for Disease Purpose of Review: This review describes the most common motor neuron disease, Control and Prevention. ALS. It discusses the diagnosis and evaluation of ALS and the current understanding of its Unlabeled Use of pathophysiology, including new genetic underpinnings of the disease. This article also Products/Investigational covers other motor neuron diseases, reviews how to distinguish them from ALS, and Use Disclosure: Drs Tiryaki and Horak discuss discusses their pathophysiology. the unlabeled use of various Recent Findings: In this article, the spectrum of cognitive involvement in ALS, new concepts drugs for the symptomatic about protein synthesis pathology in the etiology of ALS, and new genetic associations will be management of ALS. * 2014, American Academy covered. This concept has changed over the past 3 to 4 years with the discovery of new of Neurology. genes and genetic processes that may trigger the disease. As of 2014, two-thirds of familial ALS and 10% of sporadic ALS can be explained by genetics. TAR DNA binding protein 43 kDa (TDP-43), for instance, has been shown to cause frontotemporal dementia as well as some cases of familial ALS, and is associated with frontotemporal dysfunction in ALS. Summary: The anterior horn cells control all voluntary movement: motor activity, res- piratory, speech, and swallowing functions are dependent upon signals from the anterior horn cells. -
L4-Physiology of Motor Tracts.Pdf
: chapter 55 page 667 Objectives (1) Describe the upper and lower motor neurons. (2) Understand the pathway of Pyramidal tracts (Corticospinal & corticobulbar tracts). (3) Understand the lateral and ventral corticospinal tracts. (4) Explain functional role of corticospinal & corticobulbar tracts. (5) Describe the Extrapyramidal tracts as Rubrospinal, Vestibulospinal, Reticulospinal and Tectspinal Tracts. The name of the tract indicate its pathway, for example Corticobulbar : Terms: - cortico: cerebral cortex. Decustation: crossing. - Bulbar: brainstem. Ipsilateral : same side. *So it starts at cerebral cortex and Contralateral: opposite side. terminate at the brainstem. CNS influence the activity of skeletal muscle through two set of neurons : 1- Upper motor neurons (UMN) 2- lower motor neuron (LMN) They are neurons of motor cortex & their axons that pass to brain stem and They are Spinal motor neurons in the spinal spinal cord to activate: cord & cranial motor neurons in the brain • cranial motor neurons (in brainstem) stem which innervate muscles directly. • spinal motor neurons (in spinal cord) - These are the only neurons that innervate - Upper motor neurons (UMN) are the skeletal muscle fibers, they function as responsible for conveying impulses for the final common pathway, the final link voluntary motor activity through between the CNS and skeletal muscles. descending motor pathways that make up by the upper motor neurons. Lower motor neurons are classified based on the type of muscle fiber the innervate: There are two UMN Systems through which 1- alpha motor neurons (UMN) control (LMN): 2- gamma motor neurons 1- Pyramidal system (corticospinal tracts ). 2- Extrapyramidal system The activity of the lower motor neuron (LMN, spinal or cranial) is influenced by: 1. -

(Corticobulbar) Tract
Cor$cospinal (cor$cobulbar) Tract 6/18/12 1. Appreciate the functions of the corticospinal & corticobulbar tracts. 2. Distinguish corticospinal and corticobulbar tracts. Theodore Tzavaras MD2015 3. Identify the locations of both Laurie L. Wellman Ph.D. tracts through the forebrain, Eastern Virginia Medical School brainstem and spinal cord. 4. Identify the level of decussation of the corticospinal tract, and it’s clinical importance. Dr. Craig Goodmurphy Anatomy Guy Pathway Overview Pathway Overview Corticospinal Corticobulbar ² Begin in primary motor cortex. ² Begin in primary motor cortex. ² Upper ² Travel through the posterior limb Travel through the posterior limb Upper of the internal capsule (somatotopic). Motor of the internal capsule (somatotopic). Motor ² Descend through the middle 3/5 of Neuron ² Descend through the middle 3/5 of the crus cerebri (somatotopic). the crus cerebri (somatotopic). Neuron ² Travel through the brainstem as ² Travel through the brainstem and the descending pyramidal system. synapse on brainstem nuclei. Crosses Lower ² Decussate at the caudal medulla in Midline ² α-Motor neurons project along the pyramidal decussation. cranial nerves for facial movements Motor ² Descend in the spinal cord as the and voice production. Neuron corticospinal tract Lower ² All cranial nerve nuclei receive ² Synapse on α-motor neurons Motor bilateral UMN input* ² Exit spinal cord in ventral rami Neuron *Part of CN VI is the exception AnatomyGuy.com 1 Cor$cospinal (cor$cobulbar) Tract 6/18/12 Overview Corticospinal ² Primary motor cortex Don’t ü ² Try to learn all the details on your first Posterior limb of the internal pass. capsule (somatotopic). Do ü Try to sketch out each brain, ² Middle 3/5 of the crus cerebri brainstem, and cord level we showed (somatotopic). -

Study Guide Medical Terminology by Thea Liza Batan About the Author
Study Guide Medical Terminology By Thea Liza Batan About the Author Thea Liza Batan earned a Master of Science in Nursing Administration in 2007 from Xavier University in Cincinnati, Ohio. She has worked as a staff nurse, nurse instructor, and level department head. She currently works as a simulation coordinator and a free- lance writer specializing in nursing and healthcare. All terms mentioned in this text that are known to be trademarks or service marks have been appropriately capitalized. Use of a term in this text shouldn’t be regarded as affecting the validity of any trademark or service mark. Copyright © 2017 by Penn Foster, Inc. All rights reserved. No part of the material protected by this copyright may be reproduced or utilized in any form or by any means, electronic or mechanical, including photocopying, recording, or by any information storage and retrieval system, without permission in writing from the copyright owner. Requests for permission to make copies of any part of the work should be mailed to Copyright Permissions, Penn Foster, 925 Oak Street, Scranton, Pennsylvania 18515. Printed in the United States of America CONTENTS INSTRUCTIONS 1 READING ASSIGNMENTS 3 LESSON 1: THE FUNDAMENTALS OF MEDICAL TERMINOLOGY 5 LESSON 2: DIAGNOSIS, INTERVENTION, AND HUMAN BODY TERMS 28 LESSON 3: MUSCULOSKELETAL, CIRCULATORY, AND RESPIRATORY SYSTEM TERMS 44 LESSON 4: DIGESTIVE, URINARY, AND REPRODUCTIVE SYSTEM TERMS 69 LESSON 5: INTEGUMENTARY, NERVOUS, AND ENDOCRINE S YSTEM TERMS 96 SELF-CHECK ANSWERS 134 © PENN FOSTER, INC. 2017 MEDICAL TERMINOLOGY PAGE III Contents INSTRUCTIONS INTRODUCTION Welcome to your course on medical terminology. You’re taking this course because you’re most likely interested in pursuing a health and science career, which entails proficiencyincommunicatingwithhealthcareprofessionalssuchasphysicians,nurses, or dentists. -

Changes Caused by Stroke
Recovery Frontal lobe Parietal lobe let’s talk about controls personality, controls speech and reasoning, parts of sensation (touch and Changes speech, and muscles pressure) Caused by Stroke Your brain controls how you move, feel, communicate, think and act. Brain injury from a stroke may affect any of these abilities. Some changes are common no matter which side of the brain the injury is on. Others Temporal lobe are based on which side of the brain Occipital lobe controls hearing, the stroke injures. speech, and short- controls vision term memory What are the most common general What are common changes with a effects of stroke? right-brain injury? • Hemiparesis (weakness on one side of the body) or • Paralysis or weakness on the left side of the body. hemiplegia (paralysis on one side of the body) • One-sided neglect, which is a lack of awareness of the • Dysarthria (difficulty speaking or slurred speech), or left side of the body. It may also be a lack of awareness dysphagia (trouble swallowing) of what is going on to the survivor’s left. For example, • Fatigue they may only eat from the right side of their plate, ignoring the left side of the plate. • Loss of emotional control and changes in mood • Behavior may be more impulsive and less cautious • Cognitive changes (problems with memory, judgment, than before. problem-solving or a combination of these) • It may be harder for the survivor to understand facial • Behavior changes (personality changes, improper expressions and tone of voice. They also may have less language or actions) expression in their own face and tone of voice when • Decreased field of vision (inability to see peripheral communicating. -

Identification of the Corticobulbar Tracts of the Tongue and Face Using Deterministic and Probabilistic DTI Fiber Tracking in Pa
Published August 6, 2015 as 10.3174/ajnr.A4430 ORIGINAL RESEARCH ADULT BRAIN Identification of the Corticobulbar Tracts of the Tongue and Face Using Deterministic and Probabilistic DTI Fiber Tracking in Patients with Brain Tumor M. Jenabi, X K.K. Peck, X R.J. Young, N. Brennan, and X A.I. Holodny ABSTRACT BACKGROUND AND PURPOSE: The corticobulbar tract of the face and tongue, a critical white matter tract connecting the primary motor cortex and the pons, is rarely detected by deterministic DTI fiber tractography. Detection becomes even more difficult in the presence of a tumor. The purpose of this study was to compare identification of the corticobulbar tract by using deterministic and probabilistic tractography in patients with brain tumor. MATERIALS AND METHODS: Fifty patients with brain tumor who underwent DTI were studied. Deterministic tractography was per- formed by using the fiber assignment by continuous tractography algorithm. Probabilistic tractography was performed by using a Monte Carlo simulation method. ROIs were drawn of the face and tongue motor homunculi and the pons in both hemispheres. RESULTS: In all subjects, fiber assignment by continuous tractography was ineffectual in visualizing the entire course of the corticobulbar tract between the face and tongue motor cortices and the pons on either side. However, probabilistic tractography successfully visualized the corticobulbar tract from the face and tongue motor cortices in all patients on both sides. No significant difference (P Ͻ .08) was found between both sides in terms of the number of voxels or degree of connectivity. The fractional anisotropy of both the face and tongue was significantly lower on the tumor side (P Ͻ .03). -

Visualization of the Pyramidal Decussation Utilizing Diffusion
OPEN ACCESS RESEARCH Visualization of the pyramidal decussation utilizing diffusion tensor imaging: a feasibility study utilizing generalized q-sampling imaging Erik H Middlebrooks1,*, Jeffrey A Bennett1, Sharatchandra Bidari1, and Alissa Old Crow1 1Department of Radiology, University of Florida College of Medicine, Gainesville, Florida, USA *corresponding author ([email protected]) Abstract Background: The delineating point of the end of the brainstem and beginning of the spinal cord is known as the cervicomedullary junction (CMJ). This point is defined by the decussation of the pyramidal tracts. Abnormal configuration and location of the CMJ have both been implicated in disease processes such as Chiari malformation. Unfortunately, the CMJ is not directly visualized on contemporary imaging techniques. Diffusion tensor imaging (DTI) has given us the ability to directly visualize white matter tracts, but suffers from difficulties with visualizing crossing fibers. Many advanced techniques for visualizing crossing fibers utilize substantially long imaging times or non-clinical magnet strengths making clinical applicability limited. Objective: This study inves- tigates the use of generalized q-sampling imaging with diffusion decomposition on standard DTI acquisitions at 3 Tesla to demonstrate the pyramidal decussation. Methods: Three differing DTI protocols were analyzed in vivo with scan times of 17 minutes, 10 minutes, and 5.5 minutes. Data was processed with standard DTI post-processing, as well as generalized q-sampling imaging with diffusion decomposition. Results: The results of the study show that the pyramidal decussation can be reliably visualized using generalized q-sampling imaging and diffusion decomposition with scan times as low at 10 minutes. Conclusion: Utilizing generalized q-sampling post-processing, the pyramidal decussation can be reliably visualized using clinically feasible DTI sequences with scan times as low as 10 minutes. -

Motor Neuron Disease and the Elderly
Neurology 61 Motor neuron disease and the elderly Motor neuron disease is a devastating condition characterised by degeneration of motor nerves. Many of the presenting symptoms, such as fatigue, muscle weakness and difficulty in swallowing have a broad differential diagnoses in the elderly population. Dr Sheba Azam and Professor PN Leigh explain how ensuring quality of life for patients requires preventing unnecessary delay in diagnosis and early referral to an appropriate multidisciplinary team. myotrophic lateral sclerosis (ALS) also cognitive changes. Thus, misdiagnosis as well as known as motor neuron disease (MND) under-investigation has been suggested as possible (the terms are used interchangeably), was causes of an apparent decrease in the incidence of A 4 fi rst described in 1869 by the French neurologist MND in later life . Jean-Martin Charcot1. It is a progressive, fatal neurological disease characterised by degeneration of motor nerve cells in the motor cortex, Prognostic factors corticospinal tract and the spinal cord anterior horn Although the average survival in MND is around cells. The degeneration of motor nerve cells results 36 months, some patients live for 10 years or more. in progressive muscle wasting leading to signifi cant Certain phenotypic variants appear to determine disability and ultimately death. Death usually survival rates. Using information held in a tertiary results from respiratory failure due to weakness of referral MND database, a group of researchers the respiratory muscles. analysed data on onset of disease, site of onset and duration of survival5. The authors concluded that typical MND with bulbar onset, onset later in life Incidence and prevalence or in the defi nite category of El Escorial (where The worldwide incidence of MND is approximately the World Federation of Neurologist meet to a professor of clinical two per 100,000 and the prevalence is four to seven decide diagnostic criteria) at presentation, per 100,000.