From Piriformis Syndrome to Deep Gluteal
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Hip Arthroscopy Techniques: Deep Gluteal Space Access Carlos A
1 Hip Arthroscopy Techniques: 2 Deep Gluteal Space Access 3 4 5 6 7 Carlos A. Guanche, MD 8 Southern California Orthopedic Institute 9 6815 Noble Avenue 10 Van Nuys, CA 91405 11 [email protected] 12 13 Abstract 14 With the expansion of endoscopically exploring various areas around the hip, have come 15 new areas to define. The area posterior to the hip joint, known as the subgluteal space or 16 deep gluteal space (DGS), is one such area. This chapter will summarize the relevant 17 anatomy and pathology commonly found in the DGS. It is hoped that this will the reader 18 to further explore the area and treat the appropriate pathological areas. 19 20 Key Words: Deep Gluteal Space Sciatic Nerve Piriformis Syndrome 21 22 Arthroscopy Techniques: Deep Gluteal Space Access 23 24 Introduction 25 With the increasing abilities gained in exploring various areas endoscopically has come 26 an expansion of what can be explored. The area posterior to the hip joint, known as the 27 subgluteal space or deep gluteal space (DGS), is one such area. It has been known for 28 many years that there is a significant cohort of patients that have persistent posterior hip 29 and buttocks pain, whose treatment has been very difficult. Part of the difficulties have 30 stemmed from poor understanding of the anatomy and pathology of this area. With 31 endoscopic exploration of DGS, orthopedic surgeons have been able to visualize the 32 pathoanatomy, and therefore, have a better understanding of the pathologies in a part of 33 the body that has been historically ignored. -
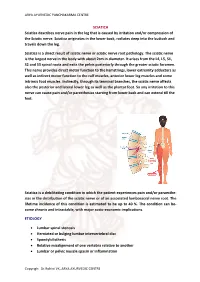
SCIATICA Sciatica Describes Nerve Pain in the Leg That Is Caused by Irritation And/Or Compression of the Sciatic Nerve
ARYA AYURVEDIC PANCHAKARMA CENTRE SCIATICA Sciatica describes nerve pain in the leg that is caused by irritation and/or compression of the Sciatic nerve. Sciatica originates in the lower back, radiates deep into the buttock and travels down the leg. Sciatica is a direct result of sciatic nerve or sciatic nerve root pathology. The sciatic nerve is the largest nerve in the body with about 2cm in diameter. It arises from the L4, L5, S1, S2 and S3 spinal roots and exits the pelvis posteriorly through the greater sciatic foramen. This nerve provides direct motor function to the hamstrings, lower extremity adductors as well as indirect motor function to the calf muscles, anterior lower leg muscles and some intrinsic foot muscles. Indirectly, through its terminal branches, the sciatic nerve affects also the posterior and lateral lower leg as well as the plantar foot. So any irritation to this nerve can cause pain and/or paresthesias starting from lower back and can extend till the feet. Sciatica is a debilitating condition in which the patient experiences pain and/or paraesthe- sias in the distribution of the sciatic nerve or of an associated lumbosacral nerve root. The lifetime incidence of this condition is estimated to be up to 40 %. The condition can be- come chronic and intractable, with major socio-economic implications. ETIOLOGY • Lumbar spinal stenosis • Herniated or bulging lumbar intervertebral disc • Spondylolisthesis • Relative misalignment of one vertebra relative to another • Lumbar or pelvic muscle spasm or inflammation Copyrigh: Dr.Rohini VK, ARYA AYURVEDIC CENTRE ARYA AYURVEDIC PANCHAKARMA CENTRE • Spinal or Paraspinal masses included malignancy, epidural haematoma or epidural abscess • Lumbar degenerative disc disease • Sacroiliac joint dysfunction EPIDEMIOLOGY GENDER: There appears to be no gender predominance. -

Radiculopathy Vs. Spinal Stenosis: Evocative Electrodiagnosis Identifies the Main Pain Generator
Functional Electromyography Loren M. Fishman · Allen N. Wilkins Functional Electromyography Provocative Maneuvers in Electrodiagnosis 123 Loren M. Fishman, MD Allen N. Wilkins, MD College of Physicians & Surgeons Manhattan Physical Medicine Columbia University and Rehabilitation New York, NY 10028, USA New York, NY 10013, USA [email protected] ISBN 978-1-60761-019-9 e-ISBN 978-1-60761-020-5 DOI 10.1007/978-1-60761-020-5 Springer New York Dordrecht Heidelberg London Library of Congress Control Number: 2010935087 © Springer Science+Business Media, LLC 2011 All rights reserved. This work may not be translated or copied in whole or in part without the written permission of the publisher (Springer Science+Business Media, LLC, 233 Spring Street, New York, NY 10013, USA), except for brief excerpts in connection with reviews or scholarly analysis. Use in connection with any form of information storage and retrieval, electronic adaptation, computer software, or by similar or dissimilar methodology now known or hereafter developed is forbidden. The use in this publication of trade names, trademarks, service marks, and similar terms, even if they are not identified as such, is not to be taken as an expression of opinion as to whether or not they are subject to proprietary rights. While the advice and information in this book are believed to be true and accurate at the date of going to press, neither the authors nor the editors nor the publisher can accept any legal responsibility for any errors or omissions that may be made. The publisher makes no warranty, express or implied, with respect to the material contained herein. -

Piriformis Syndrome: the Literal “Pain in My Butt” Chelsea Smith, PTA
Piriformis Syndrome: the literal “pain in my butt” Chelsea Smith, PTA Aside from the monotony of day-to-day pains and annoyances, piriformis syndrome is the literal “pain in my butt” that may not go away with sending the kids to grandmas and often takes the form of sciatica. Many individuals with pain in the buttock that radiates down the leg are experiencing a form of sciatica caused by irritation of the spinal nerves in or near the lumbar spine (1). Other times though, the nerve irritation is not in the spine but further down the leg due to a pesky muscle called the piriformis, hence “piriformis syndrome”. The piriformis muscle is a flat, pyramidal-shaped muscle that originates from the front surface of the sacrum and the joint capsule of the sacroiliac joint (SI joint) and is located deep in the gluteal tissue (2). The piriformis travels through the greater sciatic foramen and attaches to the upper surface of the greater trochanter (or top of the hip bone) while the sciatic nerve runs under (and sometimes through) the piriformis muscle as it exits the pelvis. Due to this close proximity between the piriformis muscle and the sciatic nerve, if there is excessive tension (tightness), spasm, or inflammation of the piriformis muscle this can cause irritation to the sciatic nerve leading to symptoms of sciatica (pain down the leg) (1). Activities like sitting on hard surfaces, crouching down, walking or running for long distances, and climbing stairs can all increase symptoms (2) with the most common symptom being tenderness along the piriformis muscle (deep in the gluteal region) upon palpation. -

Piriformis Syndrome Is Overdiagnosed 11 Robert A
American Association of Neuromuscular & Electrodiagnostic Medicine AANEM CROSSFIRE: CONTROVERSIES IN NEUROMUSCULAR AND ELECTRODIAGNOSTIC MEDICINE Loren M. Fishman, MD, B.Phil Robert A.Werner, MD, MS Scott J. Primack, DO Willam S. Pease, MD Ernest W. Johnson, MD Lawrence R. Robinson, MD 2005 AANEM COURSE F AANEM 52ND Annual Scientific Meeting Monterey, California CROSSFIRE: Controversies in Neuromuscular and Electrodiagnostic Medicine Loren M. Fishman, MD, B.Phil Robert A.Werner, MD, MS Scott J. Primack, DO Willam S. Pease, MD Ernest W. Johnson, MD Lawrence R. Robinson, MD 2005 COURSE F AANEM 52nd Annual Scientific Meeting Monterey, California AANEM Copyright © September 2005 American Association of Neuromuscular & Electrodiagnostic Medicine 421 First Avenue SW, Suite 300 East Rochester, MN 55902 PRINTED BY JOHNSON PRINTING COMPANY, INC. ii CROSSFIRE: Controversies in Neuromuscular and Electrodiagnostic Medicine Faculty Loren M. Fishman, MD, B.Phil Scott J. Primack, DO Assistant Clinical Professor Co-director Department of Physical Medicine and Rehabilitation Colorado Rehabilitation and Occupational Medicine Columbia College of Physicians and Surgeons Denver, Colorado New York City, New York Dr. Primack completed his residency at the Rehabilitation Institute of Dr. Fishman is a specialist in low back pain and sciatica, electrodiagnosis, Chicago in 1992. He then spent 6 months with Dr. Larry Mack at the functional assessment, and cognitive rehabilitation. Over the last 20 years, University of Washington. Dr. Mack, in conjunction with the Shoulder he has lectured frequently and contributed over 55 publications. His most and Elbow Service at the University of Washington, performed some of the recent work, Relief is in the Stretch: End Back Pain Through Yoga, and the original research utilizing musculoskeletal ultrasound in order to diagnose earlier book, Back Talk, both written with Carol Ardman, were published shoulder pathology. -

Sciatica and Chronic Pain
Sciatica and Chronic Pain Past, Present and Future Robert W. Baloh 123 Sciatica and Chronic Pain Robert W. Baloh Sciatica and Chronic Pain Past, Present and Future Robert W. Baloh, MD Department of Neurology University of California, Los Angeles Los Angeles, CA, USA ISBN 978-3-319-93903-2 ISBN 978-3-319-93904-9 (eBook) https://doi.org/10.1007/978-3-319-93904-9 Library of Congress Control Number: 2018952076 © Springer International Publishing AG, part of Springer Nature 2019 This work is subject to copyright. All rights are reserved by the Publisher, whether the whole or part of the material is concerned, specifically the rights of translation, reprinting, reuse of illustrations, recitation, broadcasting, reproduction on microfilms or in any other physical way, and transmission or information storage and retrieval, electronic adaptation, computer software, or by similar or dissimilar methodology now known or hereafter developed. The use of general descriptive names, registered names, trademarks, service marks, etc. in this publication does not imply, even in the absence of a specific statement, that such names are exempt from the relevant protective laws and regulations and therefore free for general use. The publisher, the authors, and the editors are safe to assume that the advice and information in this book are believed to be true and accurate at the date of publication. Neither the publisher nor the authors or the editors give a warranty, express or implied, with respect to the material contained herein or for any errors or omissions that may have been made. The publisher remains neutral with regard to jurisdictional claims in published maps and institutional affiliations. -

Surgery for Lumbar Radiculopathy/ Sciatica Final Evidence Report
Surgery for Lumbar Radiculopathy/ Sciatica Final evidence report April 13, 2018 Health Technology Assessment Program (HTA) Washington State Health Care Authority PO Box 42712 Olympia, WA 98504-2712 (360) 725-5126 www.hca.wa.gov/hta [email protected] Prepared by: RTI International–University of North Carolina Evidence-based Practice Center Research Triangle Park, NC 27709 www.rti.org This evidence report is based on research conducted by the RTI-UNC Evidence-based Practice Center through a contract between RTI International and the State of Washington Health Care Authority (HCA). The findings and conclusions in this document are those of the authors, who are responsible for its contents. The findings and conclusions do not represent the views of the Washington HCA and no statement in this report should be construed as an official position of Washington HCA. The information in this report is intended to help the State of Washington’s independent Health Technology Clinical Committee make well-informed coverage determinations. This report is not intended to be a substitute for the application of clinical judgment. Anyone who makes decisions concerning the provision of clinical care should consider this report in the same way as any medical reference and in conjunction with all other pertinent information (i.e., in the context of available resources and circumstances presented by individual patients). This document is in the public domain and may be used and reprinted without permission except those copyrighted materials that are clearly noted in the document. Further reproduction of those copyrighted materials is prohibited without the specific permission of copyright holders. -

Lumbosacral Plexus Entrapment Syndrome. Part One: a Common Yet Little-Known Cause of Chronic Pelvic and Lower Extremity Pain
3-A Running head: ANAESTHESIA, PAIN & INTENSIVE CARE www.apicareonline.com ORIGINAL ARTICLE Lumbosacral plexus entrapment syndrome. Part one: A common yet little-known cause of chronic pelvic and lower extremity pain Kjetil Larsen, CES, George C. Chang Chien, D O2 ABSTRACT Corrective exercise specialist, Training & Rehabilitation, Oslo Lumbosacral plexus entrapment syndrome (LPES) is a little-known but common cause Norway of chronic lumbopelvic and lower extremity pain. The lumbar plexus, including the 2 Director of pain management, lumbosacral tunks emerge through the fibers of the psoas major, and the proximal Ventura County Medical Center, sciatic nerve beneath the piriformis muscles. Severe weakness of these muscles may Ventura, CA 93003, USA. lead to entrapment plexopathy, resulting in diffuse and non-specific pain patterns Correspondence: Kjetil Larsen, CES, Corrective throughout the lumbopelvic complex and lower extremities (LPLE), easily mimicking Exercise Specialist, Training & other diagnoses and is therefore likely to mislead the interpreting clinician. It is a Rehabilitation, Oslo Norway; pathology very similar to that of thoracic outlet syndrome, but for the lower body. This Kjetil@trainingandrehabilitation. two part manuscript series was written in an attempt to demonstrate the existence, com; pathophysiology, diagnostic protocol as well as interventional strategy for LPES, and Tel.: +47 975 45 192 its efficacy. Received: 23 November 2018, Reviewed & Accepted: 28 Key words: Pelvic girdle; Pain, Pelvic girdle; Lumbosacral plexus entrapment syndrome; February 2019 Piriformis syndrome; Nerve entrapment; Double-crush; Pain, Chronic; Fibromyalgia Citation: Larsen K, Chien GCC. Lumbosacral plexus entrapment syndrome. Part one: A common yet little-known cause of chronic pelvic and lower extremity pain. -

Stretches and Exercise for Sciatic Pain from Piriformis Syndrome
Stretches and Exercise for Sciatic Pain from Piriformis Syndrome A common symptom of piriformis syndrome is pain along the sciatic nerve, so it is often thought that piriformis syndrome causes sciatica. However, piriformis syndrome does not involve a radiculopathy - a disc extending beyond its usual location in the vertebral column that impinges or irritates the nerve root - so it is technically not sciatica. Instead, with piriformis syndrome, it is the piriformis muscle itself that irritates the sciatic nerve and causes sciatic pain. The piriformis is a muscle located deep in the hip that runs in close proximity to the sciatic nerve. When the piriformis muscle becomes tight and/or inflamed, it can cause irritation of the sciatic nerve. This irritation leads to sciatica-like pain, tingling and numbness that run from the lower back, to the rear and sometimes down the leg and into the foot. Piriformis Muscle Stretches Stretching the piriformis muscle is almost always necessary to relieve the pain along the sciatic nerve and can be done in several different positions. A number of stretching exercises for the piriformis muscle, hamstring muscles, and hip extensor muscles may be used to help decrease the painful symptoms along the sciatic nerve and return the patient's range of motion. Several of the stretching exercises commonly prescribed to treat sciatica symptoms from piriformis muscle problems include: PIRIFORMIS STRETCHES: Lie on the back with the legs flat. Pull the affected leg up toward the chest, holding the knee with the hand on the same side of the body and grasping the ankle with the other hand. -

ICD9 & ICD10 Neuromuscular Codes
ICD-9-CM and ICD-10-CM NEUROMUSCULAR DIAGNOSIS CODES ICD-9-CM ICD-10-CM Focal Neuropathy Mononeuropathy G56.00 Carpal tunnel syndrome, unspecified Carpal tunnel syndrome 354.00 G56.00 upper limb Other lesions of median nerve, Other median nerve lesion 354.10 G56.10 unspecified upper limb Lesion of ulnar nerve, unspecified Lesion of ulnar nerve 354.20 G56.20 upper limb Lesion of radial nerve, unspecified Lesion of radial nerve 354.30 G56.30 upper limb Lesion of sciatic nerve, unspecified Sciatic nerve lesion (Piriformis syndrome) 355.00 G57.00 lower limb Meralgia paresthetica, unspecified Meralgia paresthetica 355.10 G57.10 lower limb Lesion of lateral popiteal nerve, Peroneal nerve (lesion of lateral popiteal nerve) 355.30 G57.30 unspecified lower limb Tarsal tunnel syndrome, unspecified Tarsal tunnel syndrome 355.50 G57.50 lower limb Plexus Brachial plexus lesion 353.00 Brachial plexus disorders G54.0 Brachial neuralgia (or radiculitis NOS) 723.40 Radiculopathy, cervical region M54.12 Radiculopathy, cervicothoracic region M54.13 Thoracic outlet syndrome (Thoracic root Thoracic root disorders, not elsewhere 353.00 G54.3 lesions, not elsewhere classified) classified Lumbosacral plexus lesion 353.10 Lumbosacral plexus disorders G54.1 Neuralgic amyotrophy 353.50 Neuralgic amyotrophy G54.5 Root Cervical radiculopathy (Intervertebral disc Cervical disc disorder with myelopathy, 722.71 M50.00 disorder with myelopathy, cervical region) unspecified cervical region Lumbosacral root lesions (Degeneration of Other intervertebral disc degeneration, -

The Hip's Influence on Low Back Pain
Journal of Sport Rehabilitation, 2009, 18, 24-32 © 2009 Human Kinetics, Inc. The Hip’s Influence on Low Back Pain: A Distal Link to a Proximal Problem Michael P. Reiman, P. Cody Weisbach, and Paul E. Glynn Low back pain (LBP) is a multifactorial dysfunction, with one of the potential con- tributing factors being the hip joint. Currently, research investigating the examination and conservative treatment of LBP has focused primarily on the lumbar spine. The objective of this clinical commentary is to discuss the potential link between hip impairments and LBP using current best evidence and the concept of regional inter- dependence as tools to guide decision making and offer ideas for future research. Keywords: strength, rehabilitation In day-to-day clinical practice it is often difficult to identify the source of symptoms in patients with low back pain (LBP).1 Abenhaim et al2 noted that a small percentage of individuals with LBP have an identifiable pathoanatomical source. Further clouding the picture are multiple studies indicating the potential inability of diagnostic imaging to identify the pain source, influence prognosis, or affect outcomes.3–6 Research has demonstrated the effectiveness of subgrouping patients into a classification system based on signs and symptoms indicating their likelihood to respond to specific treatments. This classification approach has pro- duced improved outcomes and high levels of reliability as compared with clinical- practice guidelines.7–9 For treating clinicians, these findings help guide decision making and improve results; however, not all patients will fit into a treatment- based subgroup. The treating therapist must then rely on an impairment-based approach, identifying potential local or remote contributors to the patient’s area of primary concern. -

The Piriformis Syndrome. a Sciatic Nerve Entrapment Misdiagnosed As Lumbar Radiculopathy
VOLUME 72 | ISSUE 2 | APRIL - JUNE 2021 Actcase reportA The Piriformis Syndrome. A sciatic nerve entrapment misdiagnosed as lumbar radiculopathy. A case report and literature review E.K.Frangakis M.D. abstract The term Piriformis Syndrome describes an extrapelvic pressure of the whole or part of the Sciatic Nerve, at the level of the Piriformis muscle caused by various conditions and characterized Clinically by symptoms of sciatica. As early as 1928 Yeoman described extra pelvic entrapment of the sciatic nerve by the piriformis muscle as a cause of sciatica. After Mixter and Barr in 1934 described nerve root compression by disc pro- lapse as a cause of sciatica, this diagnosis dominated the Clinical thinking for nearly three decades and what had been previously described was nearly forgotten. The development of imaging techniques revealed other intraspinal compressing elements. On the other hand, cases of negative root exploration for Sciatica focused attention to extrapelvic sciatic nerve pathology. This report concerns the case of a patient, who after a nega- tive root exploration for severe sciatica proved to have an extrapelvic cause for this problem at the level of the piriformis muscle due mainly to anatomic variation of the sciatic nerve in relation to the piriformis muscle. KEY WORDS: Sciatica, Sciatic nerve, Piriformis Muscle Case report referred her to a specialist who treated her with A sixty-four-year lady suffered from a severe sci- epidural steroid injection and physiotherapy with- atica in the S1 distribution of the left leg i.e. pain out any improvement. The patient was referred to in the left buttock radiating to the posterior aspect us with the diagnosis of Lumbar radiculopathy.