Late Effects of Polio Information for General Practitioners
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Fibromyalgia and Chronic Fatigue
Fibromyalgia and Chronic Fatigue Paul G. Swingle, Ph.D., R. Psych. My previous radio program and my present webcast program are both entitled “It’s all in your head!” How I came up with this title was listening to the discouraged patients that I routinely treated, and still treat, who have been told, by the doctors they have consulted, that the pain, discomfort, distress, debilitating fatigue, sleep disturbance and depression that they endure is “all in your head.” What this remark is meant to imply, of course, is that there is no physical cause of the condition and that the symptoms are manifestations of psychological factors. My response to these patients is that “of course it is in your head, where else would it be?” My remark however is not disparaging but rather indicates the actual location of many of the patients symptoms. The brain controls everything so all symptoms are associated with brain activity. The remarkable effectiveness of neurotherapy for the treatment of the symptoms associated with fibromyalgia and chronic fatigue is due to the fact that the brain functioning associated with the symptoms is treated. Although this derogatory sentiment about fibromyalgia patients was widespread among health care providers in the past, it is remarkable to me that it still persists with many doctors to this day. A few days ago I was surfing the internet health news feeds and was dismayed to find an item entitled “Fibromyalgia: A mental illness?” In this item was a quote from a Canadian neurologist stating that fibromyalgia was a term waiting for a definition. -

A Review of the Potential Therapeutic Application of Vagus Nerve Stimulation During Childbirth
A Review of the Potential Therapeutic Application of Vagus Nerve Stimulation During Childbirth By Tanya Enderli A thesis submitted to the College of Engineering at Florida Institute of Technology in partial fulfillment of the requirements for the degree of Master of Science In Biomedical Engineering Melbourne, Florida March, 2017 We the undersigned committee hereby recommend that the attached document be accepted as fulfilling in part the requirements for the degree of Master of Science of Biomedical Engineering. “A Review of the Potential Therapeutic Application of Vagus Nerve Stimulation During Childbirth,” a thesis by Tanya Enderli ____________________________________ T. A. Conway, Ph.D. Professor and Head, Biomedical Engineering Committee Chair ____________________________________ M. Kaya, Ph.D. Assistant Professor, Biomedical Engineering ____________________________________ K. Nunes Bruhn, Ph.D. Assistant Professor, Biological Sciences Abstract Title: A Review of the Potential Therapeutic Application of Vagus Nerve Stimulation During Childbirth Author: Tanya Enderli Principle Advisor: T. A. Conway, Ph.D. The goal of this research is to show that transcutaneous Vagus nerve stimulation (tVNS) should be investigated as a possible modality for increasing endogenous release of oxytocin during childbirth. There have been many great advances made in the practice of modern obstetrics in the last century. The 1900s saw the discovery, isolation, and subsequent widespread use of the hormone oxytocin as an agent to prevent postpartum hemorrhage and to initiate or quicken labor during childbirth. There are significant risks to the fetus when synthetic oxytocin is used. While the medical administration of oxytocin during labor was being popularized, there was also research being conducted on its physiologic mechanism in labor. -

Vascular Dementia: an Overview of Current Challenges and Gaps
Stroke and Dementia: what research tells us UK Stroke Assembly 2016 JM Wardlaw University of Edinburgh NHS Lothian www.strokeassembly.org.uk #strokeassembly Definitions Stroke Dementia Sudden onset focal A syndrome where there neurological deficit which is deterioration in last more than 24 hours memory, thinking, attributable to a vascular behaviour such that the defect and has no other person is no longer able identifiable cause to perform everyday activities by themselves www.strokeassembly.org.uk #strokeassembly Stroke – the importance • Stroke, 16.9million new strokes per year, – A third are disabled and dependent – 2nd commonest cause of death – Commonest cause of dependency in adults Infarct, or ischaemic stroke Haemorrhagic stroke www.strokeassembly.org.uk #strokeassembly Cerebrovascular disease – the importance • ‘Silent’ cerebrovascular disease, even bigger issue – Up to 45% of 35.6million dementias – Cognitive impairment, mobility problems Normal White matter disease www.strokeassembly.org.uk #strokeassembly Dementia • 47.5 million people have dementia world wide • 7.7million new cases per year • Affects different people in different ways • Major cause of dependency and disability amongst older people • Alzheimer’s disease commonest cause – 60-70% of cases • Vascular dementia 2nd commonest – 25-45% of all cases www.strokeassembly.org.uk #strokeassembly Dementia: historical perspective 1800’s – Blood vessel diseases 1900’s – Alzheimers disease - dominant 1970’s – ‘Multi-infarct dementia’ – vascular 1990’s–2000’s - ‘Vascular -

Vaccination and Demyelination: Is There a Link? Examples with Anti
Vaccination and demyelination : Is there a link? Examples with anti-hepatitis B and papillomavirus vaccines Julie Mouchet Le Moal To cite this version: Julie Mouchet Le Moal. Vaccination and demyelination : Is there a link? Examples with anti-hepatitis B and papillomavirus vaccines. Human health and pathology. Université de Bordeaux, 2019. English. NNT : 2019BORD0015. tel-02134582 HAL Id: tel-02134582 https://tel.archives-ouvertes.fr/tel-02134582 Submitted on 20 May 2019 HAL is a multi-disciplinary open access L’archive ouverte pluridisciplinaire HAL, est archive for the deposit and dissemination of sci- destinée au dépôt et à la diffusion de documents entific research documents, whether they are pub- scientifiques de niveau recherche, publiés ou non, lished or not. The documents may come from émanant des établissements d’enseignement et de teaching and research institutions in France or recherche français ou étrangers, des laboratoires abroad, or from public or private research centers. publics ou privés. THÈSE PRÉSENTÉE POUR OBTENIR LE GRADE DE DOCTEUR DE L’UNIVERSITÉ DE BORDEAUX ÉCOLE DOCTORALE : Sociétés, Politique, Santé Publique (SP2) SPÉCIALITÉ : Pharmacologie option Pharmaco-épidémiologie, Pharmacovigilance Par Julie MOUCHET LE MOAL VACCINATION ET RISQUE DE DEMYELINISATION : EXISTE-T-IL UN LIEN ? EXEMPLES DES VACCINS ANTI-HEPATITE B ET ANTI-PAPILLOMAVIRUS Sous la direction de : Monsieur le Professeur Bernard Bégaud Soutenue publiquement le 29 Janvier 2019 Composition du jury Président : Christophe TZOURIO, Professeur des Universités -

Clinical and MRI Clues and Pitfalls in the Diagnosis and Differential Diagnosis of Multiple Sclerosis
Clinical and MRI clues and pitfalls in the diagnosis and differential diagnosis of Multiple Sclerosis Aksel Siva, M.D. MS Clinic & Department Of Neurology Istanbul University Cerrahpaşa School of Medicine [email protected] MSParis2017 - 7th Joint ECTRIMS - ACTRIMS Meeting, 25 - 28 October 2017 Disclosure • Received research grants to my department from The Scientific and Technological Research Council Of Turkey - Health Sciences Research Grants numbers : 109S070 and 112S052.; and also unrestricted research grants from Merck-Serono and Novartis to our Clinical Neuroimmunology Unit • Honoraria or consultation fees and/or travel and registration coverage for attending several national or international congresses or symposia, from Merck Serono, Biogen Idec/Gen Pharma of Turkey, Novartis, Genzyme, Roche and Teva. • Educational presentations at programmes & symposia prepared by Excemed internationally and at national meetings and symposia sponsored by Bayer- Schering AG; Merck-Serono;. Novartis, Genzyme and Teva-Turkey; Biogen Idec/Gen Pharma of Turkey Introduction… • The incidence and prevalence rates of MS are increasing, so are the number of misdiagnosed cases as MS! • One major source of misdiagnosis is misinterpretation of nonspecific clinical and imaging findings and misapplication of MRI diagnostic criteria resulting in an overdiagnosis of MS! • The differential diagnosis of MS includes the MS spectrum and related disorders that covers subclinical & clinical MS phenotypes, MS variants and inflammatory astrocytopathies, as well as other Ab-associated atypical inflammatory-demyelinating syndromes • There are a number of systemic diseases in which either the clinical or MRI findings or both may mimic MS, which further cause confusion! Related publication *Siva A. Common Clinical and Imaging Conditions Misdiagnosed as Multiple Sclerosis. -

TIA Vs CVA (STROKE)
Phone: 973.334.3443 Email: [email protected] NJPR.com TIA vs CVA (STROKE) What is the difference between a TIA and a stroke? Difference Between TIA and Stroke • Both TIA and stroke are due to poor blood supply to the brain. • Stroke is a medical emergency and it’s a life-threatening condition. • The symptoms of TIA and Stroke may be same but TIA symptoms will recover within 24 hours. TRANSIENT ISCHEMIC ATTACK ● Also known as: TIA, mini stroke 80 E. Ridgewood Avenue, 4th Floor Paramus, NJ 07652 TIA Causes ● A transient ischemic attack has the same origins as that of an ischemic stroke, the most common type of stroke. In an ischemic stroke, a clot blocks the blood supply to part of your brain. In a transient ischemic attack, unlike a stroke, the blockage is brief, and there is no permanent damage. ● The underlying cause of a TIA often is a buildup of cholesterol- containing fatty deposits called plaques (atherosclerosis) in an artery or one of its branches that supplies oxygen and nutrients to your brain. ● Plaques can decrease the blood flow through an artery or lead to the development of a clot. A blood clot moving to an artery that supplies your brain from another part of your body, most commonly from your heart, also may cause a TIA. CEREBROVASCULAR ACCIDENT/STROKE Page 2 When the brain’s blood supply is insufficient, a stroke occurs. Stroke symptoms (for example, slurring of speech or loss of function in an arm or leg) indicate a medical emergency. Without treatment, the brain cells quickly become impaired or die. -
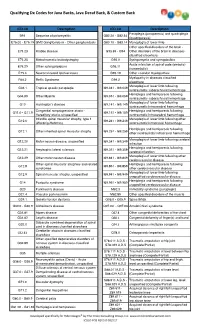
ICD-10 Backs
Qualifying Dx Codes for Java Backs, Java Decaf Back, & Custom Back ICD-10 Description ICD-10 Description Paraplegia (paraparesis) and quadriplegia B91 Sequelae of poliomyelitis G82.20 - G82.54 (quadriparesis) E75.00 - E75.19 GM2 Gangliosidosis - Other gangliosidosis G83.10 - G83.14 Monoplegia of lower limb Other specified disorders of the brain - E75.23 Krabbe disease G93.89 - G94 Other disorders of the brain in diseases classified elsewhere E75.25 Metachromatic leukodystrophy G95.0 Syringomyelia and syringobulbia Acute infarction of spinal code (embolic) E75.29 Other sphingolipidosis G95.11 (nonembolic) E75.4 Neuronal ceroid lipofuscinosis G95.19 Other vascular myelopathies Myelopathy in diseases classified F84.2 Rett's Syndrome G99.2 elsewhere Monoplegia of lower limb following G04.1 Tropical spastic paraplegia I69.041 - I69.049 nontraumatic subarachnoid hemorrhage Hemiplegia and hemiparesis following G04.89 Other Myelitis I69.051 - I69.059 nontraumatic subarachnoid hemorrhage Monoplegia of lower limb following G10 Huntington's disease I69.141 - I69.149 nontraumatic intracerebral hemorrhage Congenital nonprogressive ataxia - Hemiplegia and hemiparesis following G11.0 - G11.9 I69.151 - I69.159 Hereditary ataxia, unspecified nontraumatic intracerebral hemorrhage Infantile spinal muscular atrophy, type 1 Monoplegia of lower limb following other G12.0 I69.241 - I69.249 (Werdnig-Hoffman) nontraumatic intracranial hemorrhage Hemiplegia and hemiparesis following G12.1 Other inherited spinal muscular atrophy I69.251 - I69.259 other nontraumatic -

MR Images, Brain Lesions, and Deep Learning
applied sciences Review MR Images, Brain Lesions, and Deep Learning Darwin Castillo 1,2,3,* , Vasudevan Lakshminarayanan 2,4 and María José Rodríguez-Álvarez 3 1 Departamento de Química y Ciencias Exactas, Sección Fisicoquímica y Matemáticas, Universidad Técnica Particular de Loja, San Cayetano Alto s/n, Loja 11-01-608, Ecuador 2 Theoretical and Experimental Epistemology Lab, School of Optometry and Vision Science, University of Waterloo, Waterloo, ON N2L3G1, Canada; [email protected] 3 Instituto de Instrumentación para Imagen Molecular (i3M) Universitat Politècnica de València—Consejo Superior de Investigaciones Científicas (CSIC), E-46022 Valencia, Spain; [email protected] 4 Departments of Physics, Electrical and Computer Engineering and Systems Design Engineering, University of Waterloo, Waterloo, ON N2L3G1, Canada * Correspondence: [email protected]; Tel.: +593-07-370-1444 (ext. 3204) Featured Application: This review provides a critical review of deep/machine learning algo- rithms used in the identification of ischemic stroke and demyelinating brain diseases. It eval- uates their strengths and weaknesses when applied to real world clinical data. Abstract: Medical brain image analysis is a necessary step in computer-assisted/computer-aided diagnosis (CAD) systems. Advancements in both hardware and software in the past few years have led to improved segmentation and classification of various diseases. In the present work, we review the published literature on systems and algorithms that allow for classification, identification, and detection of white matter hyperintensities (WMHs) of brain magnetic resonance (MR) images, specifically in cases of ischemic stroke and demyelinating diseases. For the selection criteria, we used bibliometric networks. Of a total of 140 documents, we selected 38 articles that deal with the main objectives of this study. -

Sensorineural Hearing Loss Due to Vertebrobasilar Artery Ischemia
logy & N ro eu u r e o N p h f y o s l i a o l n o r Ohki, J Neurol Neurophysiol 2013, S8 g u y o J Journal of Neurology & Neurophysiology ISSN: 2155-9562 DOI: 10.4172/2155-9562.S8-005 ReviewResearch Article Article OpenOpen Access Access Sensorineural Hearing Loss Due to Vertebrobasilar Artery Ischemia– Illustrative Case and Literature Review Masafumi Ohki* Department of Otolaryngology, Saitama Medical Center, Japan Abstract Acute sensorineural hearing loss is commonly caused by peripheral vestibulocochlear disorders such as sudden deafness, Meniere’s disease, and Ramsay Hunt syndrome, but is rarely due to infarction of the vertebrobasilar artery. In this report, a case of right anterior inferior cerebellar artery syndrome presenting with sudden deafness and vertigo is described in order to feature acute sensorineural hearing loss due to vertebrobasilar artery ischemia, and sensorineural hearing loss due to vertebrobasilar artery ischemia is reviewed and discussed. A 79-year-old man presented with right acute sensorineural hearing loss preceded by occasional, minute-long periods of dizziness without cranial neural symptoms other than vestibulocochlear symptoms. Magnetic resonance imaging (MRI) revealed infarction of the right anterior inferior cerebellar artery territory. The vertebrobasilar artery supplies the vestibulocochlear organ, brainstem, and cerebellum, whose abnormalities are related to vestibulocochlear symptoms. Vertigo is a major symptom associated with vertebrobasilar artery ischemia. Further, acute sensorineural hearing loss is caused by hypoperfusion of the vertebrobasilar artery. Vertigo and/or acute sensorineural hearing loss could be a prodrome of subsequent infarction of the vertebrobasilar artery territory. The artery most often responsible for acute sensorineural hearing loss is the anterior inferior cerebellar artery, whereas ischemia of the basilar artery, the posterior inferior cerebellar artery, and the superior cerebellar artery rarely cause acute sensorineural hearing loss. -

Demyelination: What Is It and Why Does It Happen?
Demyelination: What Is It and Why Does It Happen? • Causes • Symptoms • Types • MS and Demyelination • Treatment and Diagnosis • Vaccines • Takeaway What is demyelination? Nerves send and receive messages from every part of your body and process them in your brain. Nerves allow you to speak, see, feel, and think. Many nerves are coated in myelin. Myelin is an insulating material. When it’s worn away or damaged, nerves can deteriorate, causing problems in the brain and throughout the body. Damage to myelin around nerves is called demyelination. Nerves Nerves are made up of neurons. Neurons are composed of a cell body, dendrites, and an axon. The axon sends messages from one neuron to the next. The axon also connects neurons to other cells, such as muscle cells. Some axons are extremely short. Others are 3 feet long. Some axons are covered in myelin. Myelin protects the axons and helps carry axon messages as quickly as possible. Myelin Myelin is made of membrane layers that cover an axon. This is similar to the idea of an electrical wire with coating to protect the metal underneath. Myelin allows a nerve signal to travel faster. In unmyelinated neurons, a signal can travel along the nerves at about 1 meter per second. In a myelinated neuron, the signal can travel 100 meters per second. Certain diseases can damage myelin. Demyelination slows down messages sent along axons and causes the axon to deteriorate. Depending upon the location of the damage, axon loss can cause problems with feeling, moving, seeing, hearing, and thinking clearly. CAUSES Causes of demyelination Inflammation is the most common cause of myelin damage. -

Cerebrospinal Fluid Analysis in Multiple Sclerosis Diagnosis: an Update
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by Archivio istituzionale della ricerca - Università di Palermo medicina Review Cerebrospinal Fluid Analysis in Multiple Sclerosis Diagnosis: An Update Bruna Lo Sasso 1, Luisa Agnello 1, Giulia Bivona 1 , Chiara Bellia 1 and Marcello Ciaccio 1,2,* 1 Institute of Clinical Biochemistry, Clinical Molecular Medicine and Laboratory Medicine, Department of Biomedicine, Neuroscience and Advanced Diagnostics, University of Palermo, 90100 Palermo, Italy; [email protected] (B.L.S.); [email protected] (L.A.); [email protected] (G.B.); [email protected] (C.B.) 2 Department Laboratory Medicine, University-Hospital, 90100 Palermo, Italy * Correspondence: [email protected]; Tel.: +39-091-23865701; Fax: +39-091-655-3275 Received: 25 March 2019; Accepted: 30 May 2019; Published: 4 June 2019 Abstract: Multiple sclerosis (MS) is an immune-mediated demyelinating disease of the central nervous system (CNS) with brain neurodegeneration. MS patients present heterogeneous clinical manifestations in which both genetic and environmental factors are involved. The diagnosis is very complex due to the high heterogeneity of the pathophysiology of the disease. The diagnostic criteria have been modified several times over the years. Basically, they include clinical symptoms, presence of typical lesions detected by magnetic resonance imaging (MRI), and laboratory findings. The analysis of cerebrospinal fluid (CSF) allows an evaluation of inflammatory processes circumscribed to the CNS and reflects changes in the immunological pattern due to the progression of the pathology, being fundamental in the diagnosis and monitoring of MS. The detection of the oligoclonal bands (OCBs) in both CSF and serum is recognized as the “gold standard” for laboratory diagnosis of MS, though presents analytical limitations. -

Central Pain: Clinical and Physiological J Neurol Neurosurg Psychiatry: First Published As 10.1136/Jnnp.61.1.62 on 1 July 1996
626Journal ofNeurology, Neurosurgery, and Psychiatry 1996;61:62-69 Central pain: clinical and physiological J Neurol Neurosurg Psychiatry: first published as 10.1136/jnnp.61.1.62 on 1 July 1996. Downloaded from characteristics David Bowsher Abstract spinothalamic pathway, its relays, or projec- Objectives-To study the clinical and tions may cause central pain,' and modern pathophysiological features of central radiological techniques have tended to con- pain due to damage to the CNS. firm this.9 '" Because of this, and of recent Methods-156 patients (mostly with considerations on pathophysiology,'5 '" the ischaemic strokes, some with infarct after condition is now known as "central poststroke subarachnoid haemorrhage and other pain (CPSP)"'.'7 Stroke is not the only condi- cerebral conditions; one with bulbar and tion causing such central pains of cerebral ori- others with spinal pathology) with central gin.' lxII 2' Furthermore, identical pains occur pain have been investigated clinically and after some spinal lesions.- 22 varying numbers instrumentally with respect to quantitative somatosensory perception thresholds and autonomic Patients function. Between 1983 and 1993, 156 patients have Results-Pain onset was immediate in a been referred to me, in whom a diagnosis of minority; and from a week or two up to central pain due to a cerebral or spinal lesion six years in > 60%. For those with supra- has been made. Of these, 112 (64 (57)%'Y spinal ischaemic lesions, the median age male) had a history of a stroke episode (cere- of onset was 59; dominant and non- brovascular accident, CVA patients), includ- dominant sides were equally affected.