Demyelination: What Is It and Why Does It Happen?
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Headache in Multiple Sclerosis from a Different Perspective: a Prospective Study
Volume 9 • Number 1 • March 2018 JOURNAL OF CLINICAL AND RESEARCHORIGINAL ARTICLEARTICLE EXPERIMENTAL INVESTIGATIONS Headache in Multiple Sclerosis from A Different Perspective: A Prospective Study Gökhan Özer¹, Ufuk Ergün², Levent Ertuğrul İnan³ 1 Sanko University Faculty of Medicine, Department of Neurology, Gaziantep, ABSTRACT Turkey Objective: It is known that patients with multiple sclerosis have a high incidence of headache. 2 Kırıkkale University School of Medicine, Kırıkkale, Turkey Although there is increasing evidence to suggest that periaqueductal gray matter (PAG) plays 3 Bozok University School of Medicine, a role in the pathophysiology of migraine headache, it is not known whether the type of Yozgat, Turkey headache may be a predictor of a MS relapse. Patients and Methods: The study enrolled 100 patients (68 females, 32 males) with clinically confirmed MS diagnosis established by McDonald diagnostic criteria. The type and duration of MS, MRI localization of lesions and cognitive status were recorded for all patients. Patients were questioned whether they experience headache during MS attacks. Results: Sixty-eight percent of the patients had headache and 32% of the patients were free of headache. Of the patients with headache, 16% had tension –type headache (TTH), 14% had migraine, 11% had primary stabbing headache (PSH), 8% had TTH+ migraine, 6% had PSH+ migraine, 6% had medication overuse headache , 2% had medication overuse headache + E-mail: [email protected] migraine, 2% had paroxysmal hemicrania, 1% had cervicogenic headache, 1% had chronic TTH, E-mail: [email protected] and 1% had unclassified headache. There was a statistically significant relationship between the E-mail: [email protected] presence of headache and MS relapse (p<0.001). -

Vaccination and Demyelination: Is There a Link? Examples with Anti
Vaccination and demyelination : Is there a link? Examples with anti-hepatitis B and papillomavirus vaccines Julie Mouchet Le Moal To cite this version: Julie Mouchet Le Moal. Vaccination and demyelination : Is there a link? Examples with anti-hepatitis B and papillomavirus vaccines. Human health and pathology. Université de Bordeaux, 2019. English. NNT : 2019BORD0015. tel-02134582 HAL Id: tel-02134582 https://tel.archives-ouvertes.fr/tel-02134582 Submitted on 20 May 2019 HAL is a multi-disciplinary open access L’archive ouverte pluridisciplinaire HAL, est archive for the deposit and dissemination of sci- destinée au dépôt et à la diffusion de documents entific research documents, whether they are pub- scientifiques de niveau recherche, publiés ou non, lished or not. The documents may come from émanant des établissements d’enseignement et de teaching and research institutions in France or recherche français ou étrangers, des laboratoires abroad, or from public or private research centers. publics ou privés. THÈSE PRÉSENTÉE POUR OBTENIR LE GRADE DE DOCTEUR DE L’UNIVERSITÉ DE BORDEAUX ÉCOLE DOCTORALE : Sociétés, Politique, Santé Publique (SP2) SPÉCIALITÉ : Pharmacologie option Pharmaco-épidémiologie, Pharmacovigilance Par Julie MOUCHET LE MOAL VACCINATION ET RISQUE DE DEMYELINISATION : EXISTE-T-IL UN LIEN ? EXEMPLES DES VACCINS ANTI-HEPATITE B ET ANTI-PAPILLOMAVIRUS Sous la direction de : Monsieur le Professeur Bernard Bégaud Soutenue publiquement le 29 Janvier 2019 Composition du jury Président : Christophe TZOURIO, Professeur des Universités -

Multiple Sclerosis Accepted: 15 May 2016 Receiving Tysabri
Iranian Journal Letter to Editor of Neurology Iran J Neurol 2016; 15(3): 175-176 Bacterial meningitis in a patient Received: 10 Mar 2016 with multiple sclerosis Accepted: 15 May 2016 receiving Tysabri Abdorreza Naser Moghadasi1, Soroor Advani2, Shiva Rahimi2 1 Multiple Sclerosis Research Center, Neuroscience Institute, Department of Neurology, Sina Hospital, Tehran University of Medical Sciences, Tehran, Iran 2 Department of Neurology, Sina Hospital, Tehran University of Medical Sciences, Tehran, Iran Keywords lesions (Figure 1-A) with no evidence of PML or Bacterial Meningitis; Multiple Sclerosis; Tysabri HSE encephalitis. Meningeal enhancement was seen after the injection of the contrast medium (Figure 1-B). The most important adverse effect of natalizumab is progressive multifocal leukoencephalopathy (PML).1 Apart from PML, there are reports of other cerebral infections including herpes simplex encephalitis (HSE)2,3 and cryptococcal meningitis4 in the literature. The patient was a 29-year-old woman, a known case of multiple sclerosis (MS) for at least 5 years. She was treated using natalizumab since 6 month before. She was under treatment with prednisolone 1 g daily for 5 days for optic neuritis, which was 2 weeks before the onset of symptoms of meningitis. Approximately three days before visiting the neurologist, a continuous headache in the left temporal lobe was developed. Figure 1. Periventricular lesions confirming the The patient was febrile at that time as well. diagnosis of multiple sclerosis (MS) in the FLAIR MRI Besides, two days before this, she had started view (A). Meningeal enhancement was seen after ciprofloxacin for treatment of a urinary gadolinium injection (B) tract infection. -

Clinical and MRI Clues and Pitfalls in the Diagnosis and Differential Diagnosis of Multiple Sclerosis
Clinical and MRI clues and pitfalls in the diagnosis and differential diagnosis of Multiple Sclerosis Aksel Siva, M.D. MS Clinic & Department Of Neurology Istanbul University Cerrahpaşa School of Medicine [email protected] MSParis2017 - 7th Joint ECTRIMS - ACTRIMS Meeting, 25 - 28 October 2017 Disclosure • Received research grants to my department from The Scientific and Technological Research Council Of Turkey - Health Sciences Research Grants numbers : 109S070 and 112S052.; and also unrestricted research grants from Merck-Serono and Novartis to our Clinical Neuroimmunology Unit • Honoraria or consultation fees and/or travel and registration coverage for attending several national or international congresses or symposia, from Merck Serono, Biogen Idec/Gen Pharma of Turkey, Novartis, Genzyme, Roche and Teva. • Educational presentations at programmes & symposia prepared by Excemed internationally and at national meetings and symposia sponsored by Bayer- Schering AG; Merck-Serono;. Novartis, Genzyme and Teva-Turkey; Biogen Idec/Gen Pharma of Turkey Introduction… • The incidence and prevalence rates of MS are increasing, so are the number of misdiagnosed cases as MS! • One major source of misdiagnosis is misinterpretation of nonspecific clinical and imaging findings and misapplication of MRI diagnostic criteria resulting in an overdiagnosis of MS! • The differential diagnosis of MS includes the MS spectrum and related disorders that covers subclinical & clinical MS phenotypes, MS variants and inflammatory astrocytopathies, as well as other Ab-associated atypical inflammatory-demyelinating syndromes • There are a number of systemic diseases in which either the clinical or MRI findings or both may mimic MS, which further cause confusion! Related publication *Siva A. Common Clinical and Imaging Conditions Misdiagnosed as Multiple Sclerosis. -

MR Images, Brain Lesions, and Deep Learning
applied sciences Review MR Images, Brain Lesions, and Deep Learning Darwin Castillo 1,2,3,* , Vasudevan Lakshminarayanan 2,4 and María José Rodríguez-Álvarez 3 1 Departamento de Química y Ciencias Exactas, Sección Fisicoquímica y Matemáticas, Universidad Técnica Particular de Loja, San Cayetano Alto s/n, Loja 11-01-608, Ecuador 2 Theoretical and Experimental Epistemology Lab, School of Optometry and Vision Science, University of Waterloo, Waterloo, ON N2L3G1, Canada; [email protected] 3 Instituto de Instrumentación para Imagen Molecular (i3M) Universitat Politècnica de València—Consejo Superior de Investigaciones Científicas (CSIC), E-46022 Valencia, Spain; [email protected] 4 Departments of Physics, Electrical and Computer Engineering and Systems Design Engineering, University of Waterloo, Waterloo, ON N2L3G1, Canada * Correspondence: [email protected]; Tel.: +593-07-370-1444 (ext. 3204) Featured Application: This review provides a critical review of deep/machine learning algo- rithms used in the identification of ischemic stroke and demyelinating brain diseases. It eval- uates their strengths and weaknesses when applied to real world clinical data. Abstract: Medical brain image analysis is a necessary step in computer-assisted/computer-aided diagnosis (CAD) systems. Advancements in both hardware and software in the past few years have led to improved segmentation and classification of various diseases. In the present work, we review the published literature on systems and algorithms that allow for classification, identification, and detection of white matter hyperintensities (WMHs) of brain magnetic resonance (MR) images, specifically in cases of ischemic stroke and demyelinating diseases. For the selection criteria, we used bibliometric networks. Of a total of 140 documents, we selected 38 articles that deal with the main objectives of this study. -

Cerebrospinal Fluid Analysis in Multiple Sclerosis Diagnosis: an Update
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by Archivio istituzionale della ricerca - Università di Palermo medicina Review Cerebrospinal Fluid Analysis in Multiple Sclerosis Diagnosis: An Update Bruna Lo Sasso 1, Luisa Agnello 1, Giulia Bivona 1 , Chiara Bellia 1 and Marcello Ciaccio 1,2,* 1 Institute of Clinical Biochemistry, Clinical Molecular Medicine and Laboratory Medicine, Department of Biomedicine, Neuroscience and Advanced Diagnostics, University of Palermo, 90100 Palermo, Italy; [email protected] (B.L.S.); [email protected] (L.A.); [email protected] (G.B.); [email protected] (C.B.) 2 Department Laboratory Medicine, University-Hospital, 90100 Palermo, Italy * Correspondence: [email protected]; Tel.: +39-091-23865701; Fax: +39-091-655-3275 Received: 25 March 2019; Accepted: 30 May 2019; Published: 4 June 2019 Abstract: Multiple sclerosis (MS) is an immune-mediated demyelinating disease of the central nervous system (CNS) with brain neurodegeneration. MS patients present heterogeneous clinical manifestations in which both genetic and environmental factors are involved. The diagnosis is very complex due to the high heterogeneity of the pathophysiology of the disease. The diagnostic criteria have been modified several times over the years. Basically, they include clinical symptoms, presence of typical lesions detected by magnetic resonance imaging (MRI), and laboratory findings. The analysis of cerebrospinal fluid (CSF) allows an evaluation of inflammatory processes circumscribed to the CNS and reflects changes in the immunological pattern due to the progression of the pathology, being fundamental in the diagnosis and monitoring of MS. The detection of the oligoclonal bands (OCBs) in both CSF and serum is recognized as the “gold standard” for laboratory diagnosis of MS, though presents analytical limitations. -

Acute Disseminated Encephalomyelitis Or Multiple Sclerosis: Can the Initial Presentation Help in Establishing a Correct Diagnosi
636 REVIEW Acute disseminated encephalomyelitis or multiple sclerosis: can the initial presentation help in establishing a correct Arch Dis Child: first published as on 20 May 2005. Downloaded from diagnosis? R C Dale, J A Branson ............................................................................................................................... Arch Dis Child 2005;90:636–639. doi: 10.1136/adc.2004.062935 The differential diagnosis of CNS white matter disease is and MS cases must manifest disseminated disease of the CNS (more than one clinical or broad, and can be divided into vascular, metabolic, radiological site). Diseases isolated to specific infective, or inflammatory aetiologies. Isolated areas of the CNS (isolated optic neuritis, trans- inflammatory disorders of the CNS are often associated verse myelitis, and brain stem dysfunction) are considered distinct from both ADEM and MS with demyelination, and the two terms (inflammatory and (clinically and prognostically), and will not be demyelinating) are often used in conjunction. When the discussed in this review.89 disease is monophasic, the term acute disseminated 1 DEMOGRAPHICS encephalomyelitis (ADEM) is used. ADEM typically occurs Monophasic ADEM is more common in children, as a post-infectious phenomenon, and by definition, must whereas MS is more common in adults. Between be an isolated (monophasic) episode. If a relapse occurs 2.7% and 4.4% of MS presentations occur in children less than 16 years of age.8 Mikaeloff et al shortly after the ADEM presentation in association with a showed a mean age of 7.1 years and 12.0 years in further infection or steroid withdrawal, the term MDEM paediatric ADEM and MS patients respectively.8 (multiphasic disseminated encephalomyelitis) is used. -
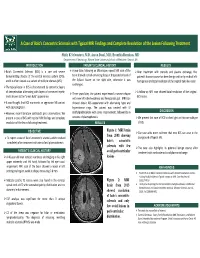
A Case of Balo's Concentric Sclerosis with Typical MRI Findings and Complete Resolution of the Lesion Followi
A Case of Balo’s Concentric Sclerosis with Typical MRI Findings and Complete Resolution of the Lesion Following Treatment Shitiz K Sriwastava, M.D, Aaron Desai, M.D, Evanthia Bernitsas, MD Department of Neurology, Wayne State University School of Medicine, Detroit, MI INTRODUCTION PATEINT’S CLINCIAL HISTORY RESULTS Balo’s Concentric Sclerosis (BCS) is a rare and severe A year later, following an MS relapse, repeat MRI scan of the After treatment with steroids and plasma exchange, the demyelinating disease of the central nervous system (CNS), brain showed a small enhancing focus at the posterior level of patient’s disease course has been benign with only residual left and it is often viewed as a variant of multiple sclerosis (MS). the Sylvian fissure on the right side, otherwise it was hemiparesis and total resolution of the original Balo‐like lesion. unchanged. The typical lesion in BCS is characterized by concentric layers of demyelination alternating with layers of preserved myelin A follow‐up MRI scan showed total resolution of the original Three years later, the patient experienced a severe relapse and is known as the “onion bulb” appearance. BCS lesion. with new left‐sided weakness and hemiparetic gait. MRI scan It was thought that BCS represents an aggressive MS variant showed classic BCS appearance with alternating hypo and with poor prognosis. hyperintense rings. The patient was treated with IV DISCUSSION However, recent literature contradicts prior observations. We methylprednisolone with some improvement, followed by 6 present a case of BCS with typical MRI findings and complete sessions of plasmapheresis. We present this case of BCS to shed light on this rare subtype resolution of the lesion following treatment. -

Updated Criteria for Diagnosing Multiple Sclerosis
r e v i e w a r t i c l e Updated criteria for diagnosing Multiple Sclerosis or in the case of progressive MS, a slow or step- Key take home messages wise progression of disability over a period of • The diagnostic criteria for MS have at least six months been recently updated • and objective clinical evidence of lesions in • These criteria should only be applied two or more distinct sites in the white matter to populations in whom MS is of the central nervous system common and patients who present • with no more satisfactory explanation. Peter Brex with typical symptoms for which no The Schumacher criteria were purely clinical, MB BS, MD, FRCP is a Consultant Neurologist at King’s College Hospital better explanation can be found although investigations were encouraged (blood, NHS Foundation Trust. He trained in • All patients with suspected MS should urine, chest X-ray, CSF analysis) to exclude London and was appointed to his current have an MRI brain scan; spinal cord alternative conditions. role in 2005. He specialises in multiple imaging is not mandatory Over the next few years modifications to the sclerosis, with a particular interest in early 2,3 prognostic markers and the management • Unmatched oligoclonal bands in the Schumacher criteria were published but in 1983 of MS during pregnancy. CSF can be used as a substitute for the Schumacher criteria were replaced by criteria demonstrating dissemination in time, developed by a committee chaired by Charles allowing an earlier diagnosis than was Poser (1923 – 2010).4 The Poser criteria incorpor- previously possible ated laboratory and clinical tests developed in the previous decade to support the diagnosis with ‘paraclinical evidence’ of lesions. -

Increased Tissue Pressure Induces Demyelinated Lesions and Necroses in the Brain
American Journal of Neuroscience Original Research Paper Increased Tissue Pressure Induces Demyelinated Lesions and Necroses in the Brain 1Helmut Barz, 2Ulrich Barz and 3Almut Schreiber 1Department of Neuropathology, Dietrich-Bonhoeffer Hospital Neubrandenburg, Mecklenburg-West-Pomerania, Germany 2Martin-Luther-Universität Halle-Wittenberg, Halle, Saxony-Anhalt, Germany 3Consultant Occupational Health Physician, Institut Für Arbeits-und Sozialhygiene, Aktiengesellschaft, Dresden, Saxony, Germany Article history Abstract: A general brain edema increases the size of the brain tissue and Received: 08-12-2014 stretches the elastic neuronal and glial fibers. Myelinated fibers are more Revised: 20-01-2015 elastic than unmyelinated fibers. The stretching of the neuronal fibers leads Accepted: 12-03-2015 particular in regions of the white matter or areas surrounded by myelinated fiber tracts to an increased tissue pressure. This physical principle can be Corresponding Author: Helmut Barz the reason for demyelination and tissue necrosis. The higher the tissue Department of Neuropathology, pressure, the lower the blood perfusion. We support the pressure-hypothesis Dietrich-Bonhoeffer Hospital by comparison with well-known pressure related pathologies of the nervous Neubrandenburg, Mecklenburg- system and other organs. One convincing example is the central pontine West-Pomerania, Germany myelinolysis. A general or local tissue edema may lead especially in the Email: [email protected] periventricular and the deep white matter, but also in the cerebellum, the brain stem and the spinal cord to the formation of hypoxemic lesions. In consequence, this could result in diseases like leukoaraiosis, Binswanger encephalopathy, idiopathic intracranial hypertension and Multiple Sclerosis (MS). In cases of brain tissue swelling, capsula-like structures may lead to a rapid increase in tissue pressure within the enclosed areas. -

Neurodegeneration and Neuroprotection in Multiple Sclerosis and Other Neurodegenerative Diseases ⁎ Suhayl Dhib-Jalbut , Douglas L
Journal of Neuroimmunology 176 (2006) 198–215 www.elsevier.com/locate/jneuroim Conference report Neurodegeneration and neuroprotection in multiple sclerosis and other neurodegenerative diseases ⁎ Suhayl Dhib-Jalbut , Douglas L. Arnold, Don W. Cleveland, Mark Fisher, Robert M. Friedlander, M. Maral Mouradian, Serge Przedborski, Bruce D. Trapp, Tony Wyss-Coray, V. Wee Yong UMDNJ-Robert Wood Johnson Medical School, New Brunswick, NJ, United States McGill University, Montreal, Quebec, Canada UCSD, San Diego, CA, United States University of Massachusetts, Worcester, MA, United States Harvard Medical School, Boston, MA, United States Columbia University, New York, NY, United States The Cleveland Clinic, Cleveland, OH, United States Stanford University, Paolo Alto, CA, United States University of Calgary, Calgary, Alberta, Canada Received 3 March 2006; accepted 6 March 2006 Abstract Multiple sclerosis is considered a disease of myelin destruction; Parkinson's disease (PD), one of dopaminergic neuron depletion; ALS, a disease of motor neuron death; and Alzheimer's, a disease of plaques and tangles. Although these disorders differ in important ways, they also have common pathogenic features, including inflammation, genetic mutations, inappropriate protein aggregates (e.g., Lewy bodies, amyloid plaques), and biochemical defects leading to apoptosis, such as oxidative stress and mitochondrial dysfunction. In most disorders, it remains uncertain whether inflammation and protein aggregation are neurotoxic or neuroprotective. Elucidating the mechanisms -

Multiple Sclerosis (MS) What Do I Need to Know?
I’m Caring for a Veteran with Multiple Sclerosis (MS) What Do I Need to Know? Physical and Mental Changes to Expect Symptoms of multiple sclerosis (MS) can vary greatly from Veteran to Veteran and from time to time in the same person. For instance, one person with MS may experience abnormal fatigue and another person may have severe vision problems. While one person with MS may have loss of balance, muscle coordination or tremors — making walking and everyday tasks difficult to perform — another person may have slurred speech and memory issues. Some Facts These problems may be permanent or may come and go. Depression is frequently experienced by MS patients and can have a significant What is Multiple Sclerosis? impact on quality of life. Multiple sclerosis (MS) is an Physical changes may include: visual disturbances; difficulty in unpredictable, often disabling controlling strength and movements; impaired coordination and balance; disease of the central nervous numbness; tingling; sensitivity to heat and cold; bladder control problems; system that interrupts the flow of urinary tract infections; mild to severe fatigue and weakness information within the brain and between the brain and the body Mental changes may include: problems with memory and concentration and stops people from moving. Emotional changes may include: mood swings, ranging from depression Symptoms range from numbness to euphoria and tingling to blindness and paralysis. The progress, severity, and specific symptoms of MS in any one What Does This Mean for Me? person cannot yet be predicted. MS affects not only the Veterans with the illness, but also family members Treatment may include: and friends.