Antimicrobial Resistance Gene Prevalence in a Population of Patients with Advanced Dementia Is
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Downloaded Skin Zaka Electronic Gmbh, Cologne, Germany)
Li et al. Microbiome (2021) 9:47 https://doi.org/10.1186/s40168-020-00995-7 RESEARCH Open Access Characterization of the human skin resistome and identification of two microbiota cutotypes Zhiming Li1,2†, Jingjing Xia3,4,5†, Liuyiqi Jiang3†, Yimei Tan4,6†, Yitai An1,2, Xingyu Zhu4,7, Jie Ruan1,2, Zhihua Chen1,2, Hefu Zhen1,2, Yanyun Ma4,7, Zhuye Jie1,2, Liang Xiao1,2, Huanming Yang1,2, Jian Wang1,2, Karsten Kristiansen1,2,8, Xun Xu1,2,9, Li Jin4,10, Chao Nie1,2*, Jean Krutmann4,5,11*, Xiao Liu1,12,13* and Jiucun Wang3,4,10,14* Abstract Background: The human skin microbiota is considered to be essential for skin homeostasis and barrier function. Comprehensive analyses of its function would substantially benefit from a catalog of reference genes derived from metagenomic sequencing. The existing catalog for the human skin microbiome is based on samples from limited individuals from a single cohort on reference genomes, which limits the coverage of global skin microbiome diversity. Results: In the present study, we have used shotgun metagenomics to newly sequence 822 skin samples from Han Chinese, which were subsequently combined with 538 previously sequenced North American samples to construct an integrated Human Skin Microbial Gene Catalog (iHSMGC). The iHSMGC comprised 10,930,638 genes with the detection of 4,879,024 new genes. Characterization of the human skin resistome based on iHSMGC confirmed that skin commensals, such as Staphylococcus spp, are an important reservoir of antibiotic resistance genes (ARGs). Further analyses of skin microbial ARGs detected microbe-specific and skin site-specific ARG signatures. -
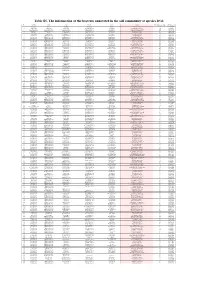
Table S5. the Information of the Bacteria Annotated in the Soil Community at Species Level
Table S5. The information of the bacteria annotated in the soil community at species level No. Phylum Class Order Family Genus Species The number of contigs Abundance(%) 1 Firmicutes Bacilli Bacillales Bacillaceae Bacillus Bacillus cereus 1749 5.145782459 2 Bacteroidetes Cytophagia Cytophagales Hymenobacteraceae Hymenobacter Hymenobacter sedentarius 1538 4.52499338 3 Gemmatimonadetes Gemmatimonadetes Gemmatimonadales Gemmatimonadaceae Gemmatirosa Gemmatirosa kalamazoonesis 1020 3.000970902 4 Proteobacteria Alphaproteobacteria Sphingomonadales Sphingomonadaceae Sphingomonas Sphingomonas indica 797 2.344876284 5 Firmicutes Bacilli Lactobacillales Streptococcaceae Lactococcus Lactococcus piscium 542 1.594633558 6 Actinobacteria Thermoleophilia Solirubrobacterales Conexibacteraceae Conexibacter Conexibacter woesei 471 1.385742446 7 Proteobacteria Alphaproteobacteria Sphingomonadales Sphingomonadaceae Sphingomonas Sphingomonas taxi 430 1.265115184 8 Proteobacteria Alphaproteobacteria Sphingomonadales Sphingomonadaceae Sphingomonas Sphingomonas wittichii 388 1.141545794 9 Proteobacteria Alphaproteobacteria Sphingomonadales Sphingomonadaceae Sphingomonas Sphingomonas sp. FARSPH 298 0.876754244 10 Proteobacteria Alphaproteobacteria Sphingomonadales Sphingomonadaceae Sphingomonas Sorangium cellulosum 260 0.764953367 11 Proteobacteria Deltaproteobacteria Myxococcales Polyangiaceae Sorangium Sphingomonas sp. Cra20 260 0.764953367 12 Proteobacteria Alphaproteobacteria Sphingomonadales Sphingomonadaceae Sphingomonas Sphingomonas panacis 252 0.741416341 -

Evaluation of MALDI Biotyper for Identification of Taylorella Equigenitalis and Taylorella Asinigenitalis Kristina Lantz Iowa State University
Iowa State University Capstones, Theses and Graduate Theses and Dissertations Dissertations 2017 Evaluation of MALDI Biotyper for identification of Taylorella equigenitalis and Taylorella asinigenitalis Kristina Lantz Iowa State University Follow this and additional works at: https://lib.dr.iastate.edu/etd Part of the Microbiology Commons, and the Veterinary Medicine Commons Recommended Citation Lantz, Kristina, "Evaluation of MALDI Biotyper for identification of Taylorella equigenitalis and Taylorella asinigenitalis" (2017). Graduate Theses and Dissertations. 16520. https://lib.dr.iastate.edu/etd/16520 This Thesis is brought to you for free and open access by the Iowa State University Capstones, Theses and Dissertations at Iowa State University Digital Repository. It has been accepted for inclusion in Graduate Theses and Dissertations by an authorized administrator of Iowa State University Digital Repository. For more information, please contact [email protected]. Evaluation of MALDI Biotyper for identification of Taylorella equigenitalis and Taylorella asinigenitalis by Kristina Lantz A thesis submitted to the graduate faculty in partial fulfillment of the requirements for the degree of MASTER OF SCIENCE Major: Veterinary Microbiology Program of Study Committee: Ronald Griffith, Major Professor Steve Carlson Matthew Erdman Timothy Frana The student author and the program of study committee are solely responsible for the content of this thesis. The Graduate College will ensure this thesis is globally accessible and will not permit -

Fish Bacterial Flora Identification Via Rapid Cellular Fatty Acid Analysis
Fish bacterial flora identification via rapid cellular fatty acid analysis Item Type Thesis Authors Morey, Amit Download date 09/10/2021 08:41:29 Link to Item http://hdl.handle.net/11122/4939 FISH BACTERIAL FLORA IDENTIFICATION VIA RAPID CELLULAR FATTY ACID ANALYSIS By Amit Morey /V RECOMMENDED: $ Advisory Committe/ Chair < r Head, Interdisciplinary iProgram in Seafood Science and Nutrition /-■ x ? APPROVED: Dean, SchooLof Fisheries and Ocfcan Sciences de3n of the Graduate School Date FISH BACTERIAL FLORA IDENTIFICATION VIA RAPID CELLULAR FATTY ACID ANALYSIS A THESIS Presented to the Faculty of the University of Alaska Fairbanks in Partial Fulfillment of the Requirements for the Degree of MASTER OF SCIENCE By Amit Morey, M.F.Sc. Fairbanks, Alaska h r A Q t ■ ^% 0 /v AlA s ((0 August 2007 ^>c0^b Abstract Seafood quality can be assessed by determining the bacterial load and flora composition, although classical taxonomic methods are time-consuming and subjective to interpretation bias. A two-prong approach was used to assess a commercially available microbial identification system: confirmation of known cultures and fish spoilage experiments to isolate unknowns for identification. Bacterial isolates from the Fishery Industrial Technology Center Culture Collection (FITCCC) and the American Type Culture Collection (ATCC) were used to test the identification ability of the Sherlock Microbial Identification System (MIS). Twelve ATCC and 21 FITCCC strains were identified to species with the exception of Pseudomonas fluorescens and P. putida which could not be distinguished by cellular fatty acid analysis. The bacterial flora changes that occurred in iced Alaska pink salmon ( Oncorhynchus gorbuscha) were determined by the rapid method. -

Assessing the Temporal Dynamics of the Lower Urinary Tract Microbiota and the Effects of Lifestyle
Loyola University Chicago Loyola eCommons Dissertations Theses and Dissertations 2019 Assessing the Temporal Dynamics of the Lower Urinary Tract Microbiota and the Effects of Lifestyle Travis Kyle Price Follow this and additional works at: https://ecommons.luc.edu/luc_diss Part of the Microbiology Commons Recommended Citation Price, Travis Kyle, "Assessing the Temporal Dynamics of the Lower Urinary Tract Microbiota and the Effects of Lifestyle" (2019). Dissertations. 3367. https://ecommons.luc.edu/luc_diss/3367 This Dissertation is brought to you for free and open access by the Theses and Dissertations at Loyola eCommons. It has been accepted for inclusion in Dissertations by an authorized administrator of Loyola eCommons. For more information, please contact [email protected]. This work is licensed under a Creative Commons Attribution-Noncommercial-No Derivative Works 3.0 License. Copyright © 2019 Travis Kyle Price LOYOLA UNIVERSITY CHICAGO ASSESSING THE TEMPORAL DYNAMICS OF THE LOWER URINARY TRACT MICROBIOTA AND THE EFFECTS OF LIFESTYLE A DISSERTATION SUBMITTED TO THE FACULTY OF THE GRADUATE SCHOOL IN CANDIDACY FOR THE DEGREE OF DOCTOR OF PHILOSOPHY PROGRAM IN MICROBIOLOGY AND IMMUNOLOGY BY TRAVIS KYLE PRICE CHICAGO, IL MAY 2019 i Copyright by Travis Kyle Price, 2019 All Rights Reserved ii ACKNOWLEDGMENTS I would like to thank everyone that made this thesis possible. First and foremost, I want to thank Dr. Alan Wolfe. I could not have asked for a better mentor. I don’t think there will ever be another period of my life where I grow as a scientist, as a professional, or as a person more than I did under your mentorship. -

Standoff Detection and Classification of Bacteria by Multispectral Laser-Induced Fluorescence
Adv. Opt. Techn. 2017; 6(2): 75–83 Research Article Open Access Frank Duschek*, Lea Fellner, Florian Gebert, Karin Grünewald, Anja Köhntopp, Marian Kraus, Peter Mahnke, Carsten Pargmann, Herbert Tomaso and Arne Walter Standoff detection and classification of bacteria by multispectral laser-induced fluorescence DOI 10.1515/aot-2016-0066 OCIS codes: 160.1435; 280.1415; 300.2530; 280.0280; Received December 2, 2016; accepted February 6, 2017; previously 000.3860. published online March 31, 2017 Abstract: Biological hazardous substances such as cer- tain fungi and bacteria represent a high risk for the broad 1 Introduction public if fallen into wrong hands. Incidents based on Hazardous bacteria represent a major threat to modern bio-agents are commonly considered to have unpredict- societies if released into the environment. Aerosols of bac- able and complex consequences for first responders and teria can occur naturally when infected animals or humans people. The impact of such an event can be minimized spread a pathogen, but they can also be released by acci- by an early and fast detection of hazards. The presented dents and as a terrorist attack. Once people are infected, approach is based on optical standoff detection apply- bacteria may easily spread aided by the fact that their detri- ing laser-induced fluorescence (LIF) on bacteria. The LIF mental effects can occur with a certain time delay. Therefore, bio-detector has been designed for outdoor operation fast and reliable detection and identification of bacteria is at standoff distances from 20 m up to more than 100 m. essential for the containment and the decontamination of The detector acquires LIF spectral data for two different affected areas and people. -

Metabolic Roles of Uncultivated Bacterioplankton Lineages in the Northern Gulf of Mexico 2 “Dead Zone” 3 4 J
bioRxiv preprint doi: https://doi.org/10.1101/095471; this version posted June 12, 2017. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted bioRxiv a license to display the preprint in perpetuity. It is made available under aCC-BY-NC 4.0 International license. 1 Metabolic roles of uncultivated bacterioplankton lineages in the northern Gulf of Mexico 2 “Dead Zone” 3 4 J. Cameron Thrash1*, Kiley W. Seitz2, Brett J. Baker2*, Ben Temperton3, Lauren E. Gillies4, 5 Nancy N. Rabalais5,6, Bernard Henrissat7,8,9, and Olivia U. Mason4 6 7 8 1. Department of Biological Sciences, Louisiana State University, Baton Rouge, LA, USA 9 2. Department of Marine Science, Marine Science Institute, University of Texas at Austin, Port 10 Aransas, TX, USA 11 3. School of Biosciences, University of Exeter, Exeter, UK 12 4. Department of Earth, Ocean, and Atmospheric Science, Florida State University, Tallahassee, 13 FL, USA 14 5. Department of Oceanography and Coastal Sciences, Louisiana State University, Baton Rouge, 15 LA, USA 16 6. Louisiana Universities Marine Consortium, Chauvin, LA USA 17 7. Architecture et Fonction des Macromolécules Biologiques, CNRS, Aix-Marseille Université, 18 13288 Marseille, France 19 8. INRA, USC 1408 AFMB, F-13288 Marseille, France 20 9. Department of Biological Sciences, King Abdulaziz University, Jeddah, Saudi Arabia 21 22 *Correspondence: 23 JCT [email protected] 24 BJB [email protected] 25 26 27 28 Running title: Decoding microbes of the Dead Zone 29 30 31 Abstract word count: 250 32 Text word count: XXXX 33 34 Page 1 of 31 bioRxiv preprint doi: https://doi.org/10.1101/095471; this version posted June 12, 2017. -

A Genomic Perspective on a New Bacterial Genus and Species From
Whiteson et al. BMC Genomics 2014, 15:169 http://www.biomedcentral.com/1471-2164/15/169 RESEARCH ARTICLE Open Access A genomic perspective on a new bacterial genus and species from the Alcaligenaceae family, Basilea psittacipulmonis Katrine L Whiteson1,5*, David Hernandez1, Vladimir Lazarevic1, Nadia Gaia1, Laurent Farinelli2, Patrice François1, Paola Pilo3, Joachim Frey3 and Jacques Schrenzel1,4 Abstract Background: A novel Gram-negative, non-haemolytic, non-motile, rod-shaped bacterium was discovered in the lungs of a dead parakeet (Melopsittacus undulatus) that was kept in captivity in a petshop in Basel, Switzerland. The organism is described with a chemotaxonomic profile and the nearly complete genome sequence obtained through the assembly of short sequence reads. Results: Genome sequence analysis and characterization of respiratory quinones, fatty acids, polar lipids, and biochemical phenotype is presented here. Comparison of gene sequences revealed that the most similar species is Pelistega europaea, with BLAST identities of only 93% to the 16S rDNA gene, 76% identity to the rpoB gene, and a similar GC content (~43%) as the organism isolated from the parakeet, DSM 24701 (40%). The closest full genome sequences are those of Bordetella spp. and Taylorella spp. High-throughput sequencing reads from the Illumina-Solexa platform were assembled with the Edena de novo assembler to form 195 contigs comprising the ~2 Mb genome. Genome annotation with RAST, construction of phylogenetic trees with the 16S rDNA (rrs) gene sequence and the rpoB gene, and phylogenetic placement using other highly conserved marker genes with ML Tree all suggest that the bacterial species belongs to the Alcaligenaceae family. -

Ribosomal Ribonucleic Acid Cistron Similarities and Deoxyribonucleic Acid Homologies of Neisseria , Kingella , Eikenella, Simons
INTERNATIONALJOURNAL OF SYSTEMATICBACTERIOLOGY, Apr. 1989, p. 185-198 Vol. 39, No. 2 0020-7713/89/020185-14$02.0010 Copyright 0 1989, International Union of Microbiological Societies Ribosomal Ribonucleic Acid Cistron Similarities and Deoxyribonucleic Acid Homologies of Neisseria , Kingella , Eikenella, Simonsiella, Alysiella, and Centers for Disease Control Groups EF-4 and M-5 in the Emended Family Neisseriaceae R. ROSSAU,ll- G. VANDENBUSSCHE,l S. THIELEMANS,l P. SEGERS,l H. GROSCH,2 E. GOTHE,2 W. MANNHEIM,2 AND J. DE LEY1* Laboratorium voor Microbiologie en microbiele Genetica, Rijksuniversiteit, Ledeganckstraat 35, B-9000 Gent, Belgium,' and Zentrum fur Hygiene und medizinische Mikrobiologie, Klinikum der Philipps- Universitat, 0-3550Marburg-Lahn, Federal Republic of Germany2 We detected distinct taxonomic relationships among the true Neisseria species, Kingella kingae, Kingella denitrGcans, Eikenella corrodens, all Simonsiella species, the type strain of Alysiellafiliformis, and members of Centers for Disease Control groups EF-4 and M-5. All these taxa constitute one large separate cluster having high levels of ribosomal ribonucleic acid cistron similarity (thermal denaturation temperature range, 74 to 81°C) in ribosomal ribonucleic acid superfamily 111. There are at least four subbranches. We found high deoxyribonucleic acid (DNA)-DNA homology values between Neisseria gonorrhoeae and some other true Neisseriu species and within the following species: Simonsiella muelleri, Simonsiella crassa, Simonsiella steedue, Kingella denitrificans, and Eikenella corrodens. All of the members of this large cluster have genome base compositions in the range from 42.8 to 57.7 mol% guanine plus cytosine. The molecular complexities of the genomic DNAs are 2.2 X lo9 to 2.7 x lo9 for Sirnonsiella and Alysiella species and 1.4 X lo9 to 1.8 X lo9 for the other members of this large cluster. -

Standoff Detection and Classification of Bacteria by Multispectral Laser-Induced Fluorescence
Adv. Opt. Techn. 2017; aop Research Article Open Access Frank Duschek*, Lea Fellner, Florian Gebert, Karin Grünewald, Anja Köhntopp, Marian Kraus, Peter Mahnke, Carsten Pargmann, Herbert Tomaso and Arne Walter Standoff detection and classification of bacteria by multispectral laser-induced fluorescence DOI 10.1515/aot-2016-0066 OCIS codes: 160.1435; 280.1415; 300.2530; 280.0280; Received December 2, 2016; accepted February 6, 2017 000.3860. Abstract: Biological hazardous substances such as cer- tain fungi and bacteria represent a high risk for the broad public if fallen into wrong hands. Incidents based on 1 Introduction bio-agents are commonly considered to have unpredict- Hazardous bacteria represent a major threat to modern able and complex consequences for first responders and societies if released into the environment. Aerosols of bac- people. The impact of such an event can be minimized teria can occur naturally when infected animals or humans by an early and fast detection of hazards. The presented spread a pathogen, but they can also be released by acci- approach is based on optical standoff detection apply- dents and as a terrorist attack. Once people are infected, ing laser-induced fluorescence (LIF) on bacteria. The LIF bacteria may easily spread aided by the fact that their detri- bio-detector has been designed for outdoor operation mental effects can occur with a certain time delay. Therefore, at standoff distances from 20 m up to more than 100 m. fast and reliable detection and identification of bacteria is The detector acquires LIF spectral data for two different essential for the containment and the decontamination of excitation wavelengths (280 and 355 nm) which can be affected areas and people. -

Middle Ear Microbiome Differences in Indigenous Filipinos with Chronic Otitis Media Due to a Duplication in the A2ML1 Gene Regie Lyn P
Santos-Cortez et al. Infectious Diseases of Poverty (2016) 5:97 DOI 10.1186/s40249-016-0189-7 SHORT REPORT Open Access Middle ear microbiome differences in indigenous Filipinos with chronic otitis media due to a duplication in the A2ML1 gene Regie Lyn P. Santos-Cortez1,9*, Diane S. Hutchinson2, Nadim J. Ajami2, Ma. Rina T. Reyes-Quintos3,4, Ma. Leah C. Tantoco3, Patrick John Labra4, Sheryl Mae Lagrana3, Melquiadesa Pedro3,ErasmoGonzalod.V.Llanes3,4, Teresa Luisa Gloria-Cruz3,4, Abner L. Chan3,4,EvaMariaCutiongco-delaPaz5,6, John W. Belmont7,10, Tasnee Chonmaitree8, Generoso T. Abes3,4, Joseph F. Petrosino2, Suzanne M. Leal1 and Charlotte M. Chiong3,4 Abstract Background: Previously rare A2ML1 variants were identified to confer otitis media susceptibility in an indigenous Filipino community and in otitis-prone US children. The goal of this study is to describe differences in the middle ear microbiome between carriers and non-carriers of an A2ML1 duplication variant that increases risk for chronic otitis media among indigenous Filipinos with poor health care access. Methods: Ear swabs were obtained from 16 indigenous Filipino individuals with chronic otitis media, of whom 11 carry the A2ML1 duplication variant. Ear swabs were submitted for 16S rRNA gene sequencing. Results: Genotype-based differences in microbial richness, structure, and composition were identified, but were not statistically significant. Taxonomic analysis revealed that the relative abundance of the phyla Fusobacteria and Bacteroidetes, and genus Fusobacterium were nominally increased in carriers compared to non-carriers, but were non-significant after correction for multiple testing. We also detected rare bacteria including Oligella that was reported only once in the middle ear. -

S1. the Genomes of the Order Burkholderiales (Taxid:80840) in The
S1. The genomes of the order Burkholderiales (taxid:80840) in the NCBI Genome List (http://www.ncbi.nlm.nih.gov/genome/browse/) 05-09-2014 N Organism/Name Kingdom Group SubGroup Size (Mb) Chr Plasmids Assemblies 1. Burkholderiales bacterium JGI 0001003-L21 Bacteria Proteobacteria Betaproteobacteria 0,070281 - - 1 2. Comamonadaceae bacterium JGI 0001003-E14 Bacteria Proteobacteria Betaproteobacteria 0,113075 - - 1 3. Candidatus Zinderia insecticola Bacteria Proteobacteria Betaproteobacteria 0,208564 1 - 1 4. Comamonadaceae bacterium JGI 0001013-A16 Bacteria Proteobacteria Betaproteobacteria 0,295955 - - 1 5. Oxalobacteraceae bacterium JGI 0001004-J12 Bacteria Proteobacteria Betaproteobacteria 0,301938 - - 1 6. Oxalobacteraceae bacterium JGI 0001002-K6 Bacteria Proteobacteria Betaproteobacteria 0,368093 - - 1 7. Burkholderiales bacterium JGI 0001003-J08 Bacteria Proteobacteria Betaproteobacteria 0,394907 - - 1 8. Burkholderiales bacterium JGI 0001002-H06 Bacteria Proteobacteria Betaproteobacteria 0,415398 - - 1 9. Pelomonas Bacteria Proteobacteria Betaproteobacteria 0,507844 - - 2 10. Leptothrix ochracea Bacteria Proteobacteria Betaproteobacteria 0,510792 - - 1 11. Oxalobacteraceae bacterium JGI 0001012-C15 Bacteria Proteobacteria Betaproteobacteria 0,640975 - - 1 12. Burkholderiales bacterium JGI 0001003-A5 Bacteria Proteobacteria Betaproteobacteria 0,686115 - - 1 13. Oxalobacteraceae bacterium JGI 001010-B17 Bacteria Proteobacteria Betaproteobacteria 0,825556 - - 1 14. Rhizobacter Bacteria Proteobacteria Betaproteobacteria 1,05799 - -