Use of Violent Restraints - System
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Evaluation and Management of Children and Adolescents with Acute Mental Health Or Behavioral Problems
CLINICAL REPORT Guidance for the Clinician in Rendering Pediatric Care Evaluation and Management of Children and Adolescents With Acute Mental Health or Behavioral Problems. Part I: Common Clinical Challenges of Patients With Mental Health and/or Behavioral Emergencies Thomas H. Chun, MD, MPH, FAAP, Sharon E. Mace, MD, FAAP, FACEP, Emily R. Katz, MD, FAAP, AMERICAN ACADEMY OF PEDIATRICS, COMMITTEE ON PEDIATRIC EMERGENCY MEDICINE, AND AMERICAN COLLEGE OF EMERGENCY PHYSICIANS, PEDIATRIC EMERGENCY MEDICINE COMMITTEE INTRODUCTION This document is copyrighted and is property of the American Academy of Pediatrics and its Board of Directors. All authors have Mental health problems are among the leading contributors to the global fi led confl ict of interest statements with the American Academy of Pediatrics. Any confl icts have been resolved through a process 1 burden of disease. Unfortunately, pediatric populations are not spared of approved by the Board of Directors. The American Academy of mental health problems. In the United States, 21% to 23% of children and Pediatrics has neither solicited nor accepted any commercial involvement in the development of the content of this publication. 2, 3 adolescents have a diagnosable mental health or substance use disorder. Clinical reports from the American Academy of Pediatrics benefi t from Among patients of emergency departments (EDs), 70% screen positive for expertise and resources of liaisons and internal (AAP) and external 4 reviewers. However, clinical reports from the American Academy of at least 1 mental health disorder, 23% meet criteria for 2 or more mental Pediatrics may not refl ect the views of the liaisons or the organizations health concerns, 5 45% have a mental health problem resulting in impaired or government agencies that they represent. -

September 9, 2015 Andrew M. Slavitt, Acting Administrator Centers For
September 9, 2015 Andrew M. Slavitt, Acting Administrator Centers for Medicare and Medicaid Services Department of Health and Human Services 200 Independence Avenue, S.W. Washington, DC 20201 Attention: CMS–3260-P – Reform of Requirements for Long-Term Care Facilities Submitted Electronically Dear Mr. Slavitt: We are writing on behalf of California Advocates for Nursing Home Reform to comment on the proposed regulations to reform the Requirements of Participation for Long-Term Care Facilities that were published in the Federal Register on July 16, 2015. CANHR is a statewide, nonprofit advocacy organization dedicated to improving the choices, care and quality of life for California’s long term care consumers, their families and loved ones. This letter solely addresses our comments concerning dementia care and chemical restraints. We are submitting comments on other aspects of the proposed regulations by separate letter. The rewrite of the Requirements of Participation presents a once-in-a-generation opportunity to finally stop the pervasive chemical restraint of nursing home residents who suffer from dementia and to establish a humane standard of care that will achieve the goals of the Nursing Home Reform Law of 1987. CMS must seize this opportunity to comprehensively address this enduring public health crisis or it will doom another generation of dementia victims to the horrific abuses they face in nursing homes today. Ending this abuse is the defining issue of our time in nursing homes. Nearly 30 years after the Reform Law required nursing homes to offer compassionate care in a homelike setting, far too many facilities routinely drug residents with dementia into submission. -

Hospital Isolation and Restraint
RULES OF DEPARTMENT OF MENTAL HEALTH AND DEVELOPMENTAL DISABILITIES DIVISION OF MENTAL HEALTH SERVICES CHAPTER 0940-3-6 HOSPITAL ISOLATION AND RESTRAINT TABLE OF CONTENTS 0940-3-6-.01 Scope 0940-3-6-.11 Behavioral Criteria for Release 0940-3-6-.02 Definitions 0940-3-6-.12 Monitoring and Assessment of Continued 0940-3-6-.03 Purpose of Isolation or Restraint Need 0940-3-6-.04 Application of This Chapter 0940-3-6-.13 Location of Use 0940-3-6-.05 Policies and Procedures 0940-3-6-.14 Termination 0940-3-6-.06 Initiation of Isolation or Physical Restraint in 0940-3-6-.15 Notification of Legal Surrogates the Absence of a Licensed Independent 0940-3-6-.16 Notification of Family/Significant Other Practitioner 0940-3-6-.17 Internal Reviews 0940-3-6-.07 Authorization 0940-3-6-.18 Performance Improvement Activities 0940-3-6-.08 Length of Authorization 0940-3-6-.19 Training 0940-3-6-.09 Renewal 0940-3-6-.20 Reporting 0940-3-6-.10 Assessments 0940-3-6-.01 SCOPE. (1) This chapter applies to all facilities providing inpatient mental health services in a hospital without regard to source of licensure, certification or accreditation. Isolation and restraint may be used in such settings only in compliance with this chapter. (2) Isolation or restraint in mental health treatment settings other than hospitals is governed by chapters applicable to those settings. Chemical restraint is permissible only in a hospital and in compliance with this chapter. Authority: T.C.A. §§4-4-103, 4-5-202, 4-5-204, 33-1-120, 33-1-302, 33-1-305, 33-1-309, 33-2-301, and 33-2-302. -
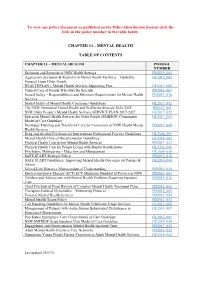
Chapter 13 – Mental Health Table of Contents
To view any policy document as published on the Policy Distribution System click the link on the policy number in the table below. CHAPTER 13 – MENTAL HEALTH TABLE OF CONTENTS CHAPTER 13 – MENTAL HEALTH PD/IB/GL NUMBER Seclusion and Restraint in NSW Health Settings PD2020_004 Aggression, Seclusion & Restraint in Mental Health Facilities – Guideline GL2012_005 Focused Upon Older People HEALTHPLAN – Mental Health Services Supporting Plan GL2012_006 Clinical Care of People Who May Be Suicidal PD2016_007 Sexual Safety – Responsibilities and Minimum Requirements for Mental Health PD2013_038 Services Sexual Safety of Mental Health Consumers Guidelines GL2013_012 The NSW Aboriginal Mental Health and Wellbeing Strategy 2020-2025 IB2021_002 NSW Older People’s Mental Health Services SERVICE PLAN 2017-2027 GL2017_022 Specialist Mental Health Services for Older People (SMHSOP) Community GL2017_003 Model of Care Guideline Discharge Planning and Transfer of Care for Consumers of NSW Health Mental PD2019_045 Health Services Drug and Alcohol Psychosocial Interventions Professional Practice Guidelines GL2008_009 Mental Health Clinical Documentation Guidelines GL2014_002 Physical Health Care within Mental Health Services PD2017_033 Physical Health Care for People Living with Mental Health Issues GL2021_006 Psychiatric Malingering – Detection and Management GL2009_016 SAFE START Strategic Policy PD2010_016 SAFE START Guidelines: Improving Mental Health Outcomes for Parents & GL2010_004 Infants School-Link Initiative Memorandum of Understanding PD2010_020 -

Labette Health
LABETTE HEALTH POLICY AND PROCEDURE SUBJECT: RESTRAINT REFERENCE:A/N/SWING BED/ER APPROVED BY: Restraint Committee PAGE 1 OF 10 EFFECTIVE: SEPT/97 REVISED: FEB/JULY99 MAR/01, JAN/02, OCT/03, DEC/03 AUG/05/MAY/07/JULY/08, APR/09, OCT/09, APRIL/12 TITLE: RESTRAINT DEFINITIONS: A restraint is any manual method, physical or mechanical device, material, or equipment that immobilizes or reduces the ability of a patient to move his or her arms, legs, body, or head freely; or a drug or medication when it is used as a restriction to manage the patient’s behavior or restrict the patient’s freedom of movement and is not a standard treatment or dosage for the patient’s condition. Patients Who May Require Restraint 1. Non-violent or non-self destructive patients (Medical): patients who require restraints to prevent removal of tubes, lines, dressings, or to support medical healing or well-being. 2. Violent or self-destructive patients (Behavior): patients who display severely aggressive or destructive behavior that jeopardizes the immediate physical safety of the patient, staff, or others. This category includes patients for which a Dr. Strong might be called. POLICY: 1. It is the intent of Labette Health to be Restraint free. 2. All patients have the right to be free from restraints or seclusion of any form, imposed as a means of coercion, discipline, convenience, or retaliation by staff. 3. Labette Health does not use seclusion as a form of restraint. 4. Restraints shall be used only where alternative methods are not sufficient to protect patients or others from injury. -

Restraint Prevalence Tools
Restraint Prevalence Tools NURSING BEST PRACTICE GUIDELINES EVALUATION USER GUIDE November 2006 Disclaimer The opinions expressed in this publication are those of the authors. Publication does not imply any endorsement of these views by either of the participating partners of the Nursing Best Practice Research Unit, which include members of the University of Ottawa faculty and members of the Registered Nurses’ Association of Ontario (RNAO). 158 Pearl Street / 158, rue Pearl School of Nursing / Toronto ON M5H 1L3 CANADA École des sciences infirmières 451 Smyth 416 599-1925 Ottawa ON K1H 8M5 CANADA 416 599-1926 613 562-5800 (8407) 613 562-5658 http://www.nbpru.ca/ Nursing Best Practice Guidelines Evaluation User Guide Copyright © 2006 by the NBPRU Printed in Ottawa, Ontario, Canada All rights reserved. Reproduction, in whole or in part, of this document without the acknowledgement of the authors and copyright holder is prohibited. The recommended citation is: Davies B, Danseco E, Ploeg J, Heslin, K, Stansfield M, Santos J & Edwards, N. (2006). Nursing Best Practice Guideline Evaluation User Guide: Restraint Prevalence Tools. Nursing Best Practice Research Unit, University of Ottawa, Canada. pp. 1-20. Nursing Best Practice Guidelines Evaluation User Guide Acknowledgements This user guide was based on an evaluation project awarded to Barbara Davies and Nancy Edwards with the Registered Nurses’ Association of Ontario (RNAO) and funded by the Government of Ontario. The authors are grateful for the support of the Nursing Secretariat of the Ministry of Health and Long-Term Care (MOHLTC), in particular the Chief Nursing Officer, Sue Matthews. The authors would also like to acknowledge the contributions of Tazim Virani and RNAO staff, clinical sites that pilot-tested the evaluation tool, members of the evaluation team and project staff. -

The Lethal Consequences of Restraint
EQUIP FOR EQUALITY A SPECIAL REPORT from the Abuse Investigation Unit NATIONAL REVIEW OF RESTRAINT RELATED DEATHS OF CHILDREN AND ADULTS WITH DISABILITIES: The Lethal Consequences of Restraint UIP FO Q R E E TM Q Y U A L I T UIP FO Q R E E TM Q Y U A L I T Mission Established in 1985, the mission of Equip for Equality is to advance the human and civil rights of people with disabilities in Illinois. Equip for Equality is a private not- for-profit legal advocacy organization designated by the governor to operate the federally mandated Protection and Advocacy System (P&A) to safeguard the rights of people with physical and mental disabilities, including developmental disabilities and mental illness. Equip for Equality is the only comprehensive statewide advocacy organization for people with disabilities and their families. All individuals with a disability in Illinois (as defined by the ADA) are eligible for services, including children, senior citizens, and individuals in state-operated facilities, nursing homes, and community-based programs. Services, Programs, and Projects Abuse Investigation Unit works to prevent abuse, neglect, and deaths of children and adults with disabilities in community-based programs, nursing homes, and state institutions. The Unit works with public investigatory agencies to improve their performance and coordination with each other; conducts investigations of abuse and neglect cases; alerts service providers to dangerous conditions and practices. Public Policy Advocacy achieves changes in state legislation, public policies and programs to safeguard individual rights and personal safety, enhance choice and self- determination, and promote independence, productivity, and community integration. -

When and How to Use Restraints R T S E Learn About Possible Indications for Restraint, Types of Restraints, R F and How to Monitor Patients in Restraint
s t n i a When and how to use restraints r t s e Learn about possible indications for restraint, types of restraints, R f and how to monitor patients in restraint. o e s By Gale Springer, RN, MSN, PMHCNS-BC U e f ew things cause as much angst who are violent or aggressive, a for a nurse as placing a patient threatening to hit or striking staff, or S . Fin a restraint, who may feel his banging their head on the wall, who . n or her personal freedom is being need to be stopped from causing o taken away. But in certain situa - further injury to themselves or oth - s tions, restraining a patient is the on - ers. The goal of using such restraints u ly option that ensures the safety of is to keep the patient and staff safe c o the patient and others. in an emergency situation. For ex - F As nurses, we’re ethically obli - ample, a patient responding to hal - gated to ensure the patient’s basic lucinations that commands him or right not to be subjected to inap - her to hurt staff and lunge aggres - propriate restraint use. Restraints sively may need a physical restraint must not be used for coercion, to protect everyone involved. punishment, discipline, or staff con - venience. Improper restraint use Chemical restraint can lead to serious sanctions by the Chemical restraint involves use of state health department, The Joint a drug to restrict a patient’s move - Commission (TJC), or both. Use re - ment or behavior, where the drug straints only to help keep the pa - or dosage used isn’t an approved tient, staff, other patients, and visi - movement (such as when giving an standard of treatment for the pa - tors safe—and only as a last resort. -

Chemical Restraint in the ED ACEP Now
4/18/2017 Chemical Restraint in the ED ACEP Now Chemical Restraint in the ED December 1, 2012 by ACEP Now Chemical Restraint in the ED Sudden violence in the emergency department (ED) remains a common problem. Psychiatric disturbance, uncontrolled pain, intoxication, de-robing, and long wait times all contribute to the eruption of violence. Assaults involving health care workers in the United States occur at 4 times the rate seen in other industries1. Those predisposed to violent behavior include males, prisoners, intoxicated patients, or those with psychiatric illness1. When a patient begins to exhibit dangerous behavior, the emergency physician must be prepared to control the situation in a safe and eective manner. Chemical restraint via antipsychotic and benzodiazepine medication, used in an eort to facilitate medical workup and patient safety, enjoys a long standing safety and ecacy record. Chemical restraint avoids adverse consequences associated with physical restraint, which include hyperthermia, dehydration, rhabdomyolysis, and lactic acidosis. Chemical restraint is indicated when a patient poses a danger to himself, others, or hospital property. Techniques involving verbal de-escalation and provision of patient comfort always should be attempted prior to employment of forceful measures. Before receiving medications, the patient should be placed into physical restraints by appropriate security sta in an eort to avoid injury to the patient, sta, or environment.2 The most appropriate drug regimen for combative ED patients has been the subject of much study. CME Questionnaire Haloperidol and lorazepam “5 and 2” combination Available Online therapy for the violent medically undierentiated patient enjoys overwhelming support; however, rapid The CME test and evaluation form acting IM formulations of atypical antipsychotics are based on this article are located gaining popularity. -

January 18 2017 Regular Meeting
Northern Inyo Hospital January 18 2017 Regular Meeting January 18 2017 Regular Meeting - January 18 2017 Regular Meeting Agenda, January 18 2017 Regular Meeting Agenda, January 18 2017 Regular Meeting...............................................................2 Consent Agenda Financial and Statistical reports, November 2016..................................................18 2013 CMS Validation Survey Monitoring, January 2017 ........................................26 Minutes, December 14 2016 Regular Meeting.........................................................31 Chief of Staff Report Chief of Staff Report, January 2017 .........................................................................40 Med Staff Policy and Procedure Approvals ............................................................41 Healthcare Cost Solutions Backlog Coding Agreement Healthcare Cost Solutions Backlog Coding Agreement......................................109 Nursing Department Policy and Procedure Approvals CNO Policy and Procedure Approvals, January 2017..........................................122 Reach Air/Medical Services Agreement Reach Air/Medical Services Agreement ................................................................134 1 Powered by TCPDF (www.tcpdf.org) 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 2013 CMS Validation Survey Monitoring-January 2017 1. QAPI continues to receive and monitor data related to the previous CMS Validation Survey, including but not limited to, restraints, dietary process measures, case -

Report 2 of the Council on Science and Public Health
REPORT 2 OF THE COUNCIL ON SCIENCE AND PUBLIC HEALTH (June 2021) Use of Drugs to Chemically Restrain Agitated Individuals Outside of Hospital Settings (Reference Committee E) EXECUTIVE SUMMARY Objective. The term “excited delirium” (ExD) is controversial and lacks a defined set of behavioral signs and symptoms used to identify a person in distress and in need of urgent medical or psychiatric help. Additionally, several media reports have recently highlighted the use of ketamine and other sedative/hypnotic agents by non-medical professionals to chemically incapacitate a person for a law enforcement purpose, and in many cases, ExD is listed as the reason for the use of a sedative/hypnotic agent. The Board of Trustees has requested that the Council on Science and Public Health study the use of ketamine and chemical restraints in the context of “excited delirium” and report back to the House of Delegates. Methods. English-language reports were selected from a PubMed and Google Scholar search using the text terms “excited delirium,” “delirium,” “fatalities excited delirium,” “excited delirium restraint,” “excited delirium sedatives,” “excited delirium ketamine,” “police ketamine,” “EMS ketamine,” and “crisis response team.” Articles were filtered based on relevance. Additional articles were identified by manual review of the references cited in these publications. Searches of selected medical specialty society and international, national, and local government agency websites were conducted to identify clinical guidelines, position statements, and reports. Results. The assessment, diagnosis, and treatment of ExD remains controversial. Despite a lack of scientific evidence, a universally recognized definition, a clear understanding of pathophysiologic mechanisms, or a specific diagnostic test, law enforcement and EMS personnel are taught that ExD is a potentially deadly medical condition. -

Use of Physical Restraints in Neurosurgery: Guide for a Good Practice
23 Use of Physical Restraints in Neurosurgery: Guide for a Good Practice Ayten Demir Zencirci Ankara University, Faculty of Health Sciences, Nursing Department Turkey 1. Introduction Physical restraints are widely used in hospitals in many countries, especially during critical care, against a range of difficult clinical situations. They are intended to protect patients and their relatives from any harm to themselves: falling from beds, removing tubes, drains, and medical equipments from their bodies, and to ease patients’ control (Bower & McCullough, 2000). Weaning from artificial ventilation, recovering from acute illness can be a long and difficult process. The problem with critically ill patients is re-sedation, often needed to handle agitation and avoid treatment interference (Cohen et al., 2002). Sedatives lengthen hospitalization and complicate recovery (Westcott, 1995); therefore, the management of these patients can often be a dilemma (Hine, 2007). 1.1 What is a restraint? Physical restraint is (American Nurses Assosication, 2001) “any chemical or physical involuntary method restricting an individual's movement, physical activity, or normal access to the body.” Physical restraint is also defined as any device, material, or equipment attached to or near a person’s body, neither controlled nor easily removed by a patient and that deliberately prevents or intended to prevent free body movement to a position of choice or patients normal access to their body (Retsas, 1998). 1.2 History of physical restraint Physical restraint use in acute and intensive cares dates back long. While actions –against restraint were taken in England and France during the 19th century, its use in acute care settings in the US was assumed as a therapeutic and morally correct approach against accidents and injures (Bower & McCullough, 2000).