Hemimegalencephaly with Bannayan-Riley-Ruvalcaba Syndrome
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Advances in Understanding the Genetics of Syndromes Involving Congenital Upper Limb Anomalies
Review Article Page 1 of 10 Advances in understanding the genetics of syndromes involving congenital upper limb anomalies Liying Sun1#, Yingzhao Huang2,3,4#, Sen Zhao2,3,4, Wenyao Zhong1, Mao Lin2,3,4, Yang Guo1, Yuehan Yin1, Nan Wu2,3,4, Zhihong Wu2,3,5, Wen Tian1 1Hand Surgery Department, Beijing Jishuitan Hospital, Beijing 100035, China; 2Beijing Key Laboratory for Genetic Research of Skeletal Deformity, Beijing 100730, China; 3Medical Research Center of Orthopedics, Chinese Academy of Medical Sciences, Beijing 100730, China; 4Department of Orthopedic Surgery, 5Department of Central Laboratory, Peking Union Medical College Hospital, Peking Union Medical College and Chinese Academy of Medical Sciences, Beijing 100730, China Contributions: (I) Conception and design: W Tian, N Wu, Z Wu, S Zhong; (II) Administrative support: All authors; (III) Provision of study materials or patients: All authors; (IV) Collection and assembly of data: Y Huang; (V) Data analysis and interpretation: L Sun; (VI) Manuscript writing: All authors; (VII) Final approval of manuscript: All authors. Correspondence to: Wen Tian. Hand Surgery Department, Beijing Jishuitan Hospital, Beijing 100035, China. Email: [email protected]. Abstract: Congenital upper limb anomalies (CULA) are a common birth defect and a significant portion of complicated syndromic anomalies have upper limb involvement. Mostly the mortality of babies with CULA can be attributed to associated anomalies. The cause of the majority of syndromic CULA was unknown until recently. Advances in genetic and genomic technologies have unraveled the genetic basis of many syndromes- associated CULA, while at the same time highlighting the extreme heterogeneity in CULA genetics. Discoveries regarding biological pathways and syndromic CULA provide insights into the limb development and bring a better understanding of the pathogenesis of CULA. -

Level Estimates of Maternal Smoking and Nicotine Replacement Therapy During Pregnancy
Using primary care data to assess population- level estimates of maternal smoking and nicotine replacement therapy during pregnancy Nafeesa Nooruddin Dhalwani BSc MSc Thesis submitted to the University of Nottingham for the degree of Doctor of Philosophy November 2014 ABSTRACT Background: Smoking in pregnancy is the most significant preventable cause of poor health outcomes for women and their babies and, therefore, is a major public health concern. In the UK there is a wide range of interventions and support for pregnant women who want to quit. One of these is nicotine replacement therapy (NRT) which has been widely available for retail purchase and prescribing to pregnant women since 2005. However, measures of NRT prescribing in pregnant women are scarce. These measures are vital to assess its usefulness in smoking cessation during pregnancy at a population level. Furthermore, evidence of NRT safety in pregnancy for the mother and child’s health so far is nebulous, with existing studies being small or using retrospectively reported exposures. Aims and Objectives: The main aim of this work was to assess population- level estimates of maternal smoking and NRT prescribing in pregnancy and the safety of NRT for both the mother and the child in the UK. Currently, the only population-level data on UK maternal smoking are from repeated cross-sectional surveys or routinely collected maternity data during pregnancy or at delivery. These obtain information at one point in time, and there are no population-level data on NRT use available. As a novel approach, therefore, this thesis used the routinely collected primary care data that are currently available for approximately 6% of the UK population and provide longitudinal/prospectively recorded information throughout pregnancy. -

Orphanet Report Series Rare Diseases Collection
Marche des Maladies Rares – Alliance Maladies Rares Orphanet Report Series Rare Diseases collection DecemberOctober 2013 2009 List of rare diseases and synonyms Listed in alphabetical order www.orpha.net 20102206 Rare diseases listed in alphabetical order ORPHA ORPHA ORPHA Disease name Disease name Disease name Number Number Number 289157 1-alpha-hydroxylase deficiency 309127 3-hydroxyacyl-CoA dehydrogenase 228384 5q14.3 microdeletion syndrome deficiency 293948 1p21.3 microdeletion syndrome 314655 5q31.3 microdeletion syndrome 939 3-hydroxyisobutyric aciduria 1606 1p36 deletion syndrome 228415 5q35 microduplication syndrome 2616 3M syndrome 250989 1q21.1 microdeletion syndrome 96125 6p subtelomeric deletion syndrome 2616 3-M syndrome 250994 1q21.1 microduplication syndrome 251046 6p22 microdeletion syndrome 293843 3MC syndrome 250999 1q41q42 microdeletion syndrome 96125 6p25 microdeletion syndrome 6 3-methylcrotonylglycinuria 250999 1q41-q42 microdeletion syndrome 99135 6-phosphogluconate dehydrogenase 67046 3-methylglutaconic aciduria type 1 deficiency 238769 1q44 microdeletion syndrome 111 3-methylglutaconic aciduria type 2 13 6-pyruvoyl-tetrahydropterin synthase 976 2,8 dihydroxyadenine urolithiasis deficiency 67047 3-methylglutaconic aciduria type 3 869 2A syndrome 75857 6q terminal deletion 67048 3-methylglutaconic aciduria type 4 79154 2-aminoadipic 2-oxoadipic aciduria 171829 6q16 deletion syndrome 66634 3-methylglutaconic aciduria type 5 19 2-hydroxyglutaric acidemia 251056 6q25 microdeletion syndrome 352328 3-methylglutaconic -

349 D.R. Laub Jr. (Ed.), Congenital Anomalies of the Upper
Index A dermatological anomalies , 182 Abductor digiti minimi (ADM) transfer , 102–103 skeletal abnormalities , 182 Abductor pollicis brevis (APB) , 186–187 upper extremity anomalies , 182, 183 ABS. See Amniotic band syndrome (ABS) visceral anomalies , 182 Achondroplasia defi nition of , 179 classifi cation/characterization , 338 description , 32, 33 defi nition of , 337–338 epidemiology of , 181 genetics , 338 genetics and embryology management , 338 molecular etiology , 180 Acrocephalosyndactyly syndrome , 32, 33, 179 prenatal diagnosis , 180–181 Acrosyndactyly repair, ABS , 300–302 molecular basis of , 180 Adactylic group IV symbrachydactyly , 129, 131 postoperative care and complications , 187 Al-Awadi syndrome , 154 treatment Amniotic band syndrome (ABS) APB release , 186–187 acrosyndactyly repair , 300–302 border digits syndactylies , 184 anesthesia concerns of fi rst web space release , 186 induction and maintenance of anesthesia , 43 patient age , 183 postoperative concerns , 43 secondary revisions , 187 preoperative preparation , 42–43 symphalangism , 184 classifi cation , 298 syndactyly ( see Syndactyly) clinical presentation thumb radial clinodactyly , 186–187 acrosyndactyly , 297–298 type II apert hand , 187–188 digital malformation , 297 Apical ectodermal ridge (AER) , 3–5 distal skeletal bones tapering , 297–298 Arthrogryposis , 210 hand deformity , 297 classic arthrogryposis , 305–306, 308 complications , 302 classifi cation , 305, 306 constriction band release defi nition of , 229, 230, 305 Upton’s technique , 299, 301 de-rotation osteotomy, shoulder , 308, 309 z-plasty , 299–300 distal , 230–231 ( see Distal arthrogryposis) diagnosis of , 296 elbow treatment digital hypoplasia reconstruction , 302 muscle transfers , 310–311 etiology of , 295–296 nonoperative management , 308 preoperative considerations , 299 posterior elbow capsular release , 309 treatment , 299 radial head dislocations , 311 Amniotic constriction band syndrome. -

PTEN Hamartoma Tumor Syndromes
European Journal of Human Genetics (2008) 16, 1289–1300 & 2008 Macmillan Publishers Limited All rights reserved 1018-4813/08 $32.00 www.nature.com/ejhg PRACTICAL GENETICS In association with PTEN hamartoma tumor syndromes The PTEN hamartoma tumor syndromes (PHTS) are a collection of rare clinical syndromes characterized by germline mutations of the tumor suppressor PTEN. These syndromes are driven by cellular overgrowth, leading to benign hamartomas in virtually any organ. Cowden syndrome (CS), the prototypic PHTS syndrome, is associated with increased susceptibility to breast, thyroid, and endometrial cancer. PTEN is located on chromosome 10q22–23 and negatively regulates the prosurvival PI3K/Akt/mTOR pathway through its lipid phosphatase activity. Loss of PTEN activates this pathway and leads to increased cellular growth, migration, proliferation, and survival. Clinical management of patients with PHTS, particularly those with CS, should include early and frequent screening, surveillance, and preventive care for associated malignancies. Concomitant with improved understanding of the biology of PTEN and the PI3K/Akt/mTOR pathway, inhibitors of this pathway are being developed as anticancer agents. These medications could have applications for patients with PHTS, for whom no medical options currently exist. In brief Adult onset LD is considered a variant of CS character- ized by dysplastic gangliocytoma of the cerebellum PHTS is an autosomal dominant spectrum of hamarto- often leading to increased intracranial pressure, ataxia, matous overgrowth disorders with variable phenotypic and seizures. manifestations characterized by germline mutations of BRRS is characterized by the developmental delay, the tumor suppressor gene PTEN located at 10q22–23. macrocephaly, lipomas, hemangiomas, and pigmented These syndromes include Cowden syndrome (CS), speckled macules of the glans penis in males. -
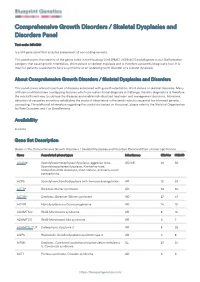
Blueprint Genetics Comprehensive Growth Disorders / Skeletal
Comprehensive Growth Disorders / Skeletal Dysplasias and Disorders Panel Test code: MA4301 Is a 374 gene panel that includes assessment of non-coding variants. This panel covers the majority of the genes listed in the Nosology 2015 (PMID: 26394607) and all genes in our Malformation category that cause growth retardation, short stature or skeletal dysplasia and is therefore a powerful diagnostic tool. It is ideal for patients suspected to have a syndromic or an isolated growth disorder or a skeletal dysplasia. About Comprehensive Growth Disorders / Skeletal Dysplasias and Disorders This panel covers a broad spectrum of diseases associated with growth retardation, short stature or skeletal dysplasia. Many of these conditions have overlapping features which can make clinical diagnosis a challenge. Genetic diagnostics is therefore the most efficient way to subtype the diseases and enable individualized treatment and management decisions. Moreover, detection of causative mutations establishes the mode of inheritance in the family which is essential for informed genetic counseling. For additional information regarding the conditions tested on this panel, please refer to the National Organization for Rare Disorders and / or GeneReviews. Availability 4 weeks Gene Set Description Genes in the Comprehensive Growth Disorders / Skeletal Dysplasias and Disorders Panel and their clinical significance Gene Associated phenotypes Inheritance ClinVar HGMD ACAN# Spondyloepimetaphyseal dysplasia, aggrecan type, AD/AR 20 56 Spondyloepiphyseal dysplasia, Kimberley -

Essential Genetics 5
Essential genetics 5 Disease map on chromosomes 例 Gaucher disease 単一遺伝子病 天使病院 Prader-Willi syndrome 隣接遺伝子症候群,欠失が主因となる疾患 臨床遺伝診療室 外木秀文 Trisomy 13 複数の遺伝子の重複によって起こる疾患 挿画 Koromo 遺伝子の座位あるいは欠失等の範囲を示す Copyright (c) 2010 Social Medical Corporation BOKOI All Rights Reserved. Disease map on chromosome 1 Gaucher disease Chromosome 1q21.1 1p36 deletion syndrome deletion syndrome Adrenoleukodystrophy, neonatal Cardiomyopathy, dilated, 1A Zellweger syndrome Charcot-Marie-Tooth disease Emery-Dreifuss muscular Hypercholesterolemia, familial dystrophy Hutchinson-Gilford progeria Ehlers-Danlos syndrome, type VI Muscular dystrophy, limb-girdle type Congenital disorder of Insensitivity to pain, congenital, glycosylation, type Ic with anhidrosis Diamond-Blackfan anemia 6 Charcot-Marie-Tooth disease Dejerine-Sottas syndrome Marshall syndrome Stickler syndrome, type II Chronic granulomatous disease due to deficiency of NCF-2 Alagille syndrome 2 Copyright (c) 2010 Social Medical Corporation BOKOI All Rights Reserved. Disease map on chromosome 2 Epiphyseal dysplasia, multiple Spondyloepimetaphyseal dysplasia Brachydactyly, type D-E, Noonan syndrome Brachydactyly-syndactyly syndrome Peters anomaly Synpolydactyly, type II and V Parkinson disease, familial Leigh syndrome Seizures, benign familial Multiple pterygium syndrome neonatal-infantile Escobar syndrome Ehlers-Danlos syndrome, Brachydactyly, type A1 type I, III, IV Waardenburg syndrome Rhizomelic chondrodysplasia punctata, type 3 Alport syndrome, autosomal recessive Split-hand/foot malformation Crigler-Najjar -

Craniosynostosis Precision Panel Overview Indications Clinical Utility
Craniosynostosis Precision Panel Overview Craniosynostosis is defined as the premature fusion of one or more cranial sutures, often resulting in abnormal head shape. It is a developmental craniofacial anomaly resulting from a primary defect of ossification (primary craniosynostosis) or, more commonly, from a failure of brain growth (secondary craniosynostosis). As well, craniosynostosis can be simple when only one suture fuses prematurely or complex/compound when there is a premature fusion of multiple sutures. Complex craniosynostosis are usually associated with other body deformities. The main morbidity risk is the elevated intracranial pressure and subsequent brain damage. When left untreated, craniosynostosis can cause serious complications such as developmental delay, facial abnormality, sensory, respiratory and neurological dysfunction, eye anomalies and psychosocial disturbances. In approximately 85% of the cases, this disease is isolated and nonsyndromic. Syndromic craniosynostosis usually present with multiorgan complications. The Igenomix Craniosynostosis Precision Panel can be used to make a directed and accurate diagnosis ultimately leading to a better management and prognosis of the disease. It provides a comprehensive analysis of the genes involved in this disease using next-generation sequencing (NGS) to fully understand the spectrum of relevant genes involved. Indications The Igenomix Craniosynostosis Precision Panel is indicated for those patients with a clinical diagnosis or suspicion with or without the following manifestations: ‐ Microcephaly ‐ Scaphocephaly (elongated head) ‐ Anterior plagiocephaly ‐ Brachycephaly ‐ Torticollis ‐ Frontal bossing Clinical Utility The clinical utility of this panel is: - The genetic and molecular confirmation for an accurate clinical diagnosis of a symptomatic patient. - Early initiation of treatment in the form surgical procedures to relieve fused sutures, midface advancement, limited phase of orthodontic treatment and combined 1 orthodontics/orthognathic surgery treatment. -

References Case Report Comment
None of the authors had any commercial interest in the findings presented. References 1. Faunfelder FT, LaBraico JM, Meyer SM. Adverse ocular reactions possibly associated with isotretinoin. Am J Ophthalmol 1985;100:534-7. 2. Jones H, Blanc D, Cunliffe WJ. 13-cis-retinoic acid and acne. Lancet 1980;II:1048-9. 3. Mathers WD, Shields WI, Sachdev MS, Petroll WM, Jester JV. Meibomian gland morphology and tear osmolarity: changes with Accutane therapy. Cornea 1991;10:286-90. 4. Peck GL, Yoder FW. Treatment of lamellar ichthyosis and other keratinising dermatoses with an oral synthetic retinoid. Lancet 1976;II:1172-4. Fig. 1. Photograph of an infant with Proteus syndrome showing the 5. Zouboulis Cc, Korge B, Akamatsu H, Xia L, Schiller S, characteristic skin changes and left-sided hemihypertrophy. Gollnick H, Orfanos CE. Effects of 13-cis-retinoic acid, all trans-retinoic acid, and acitretin on the proliferation, lipid synthesis and keratin expression of cultured human sebocytes (development quotient 66%) and was hypotonic, but had in vitro. J Invest Dermatol 1991;96:792-7. no focal neurological deficit. The head circumference was « W.C.-T. Chua 44 cm 3rd centile) and the left half of the skull was P.A. Martin larger than the right. G. Kourt Ocular abnormalities were observed; these were Sydney Eye Hospital limited to the left side, with the left eyeball being larger Sydney than the right, resulting in a severe degree of myopic New South Wales Australia anisometropia and amblyopia. There was a conjunctival capillary haemangioma in the left eye. The cornea was Dr Peter A. -

A Morpho-Etiological Description of Congenital Limb Anomalies Tayel SM,* Fawzia MM,† Niran a Al-Naqeeb,‡ Said Gouda,§ Al Awadi SA,§ Naguib KK§
[Downloaded free from http://www.saudiannals.net on Sunday, May 09, 2010] ORIGINAL ARTICLE A morpho-etiological description of congenital limb anomalies Tayel SM,* Fawzia MM,† Niran A Al-Naqeeb,‡ Said Gouda,§ Al Awadi SA,§ Naguib KK§ From the *Genetics Unit, Anatomy BACKGROUND: Limb anomalies rank behind congenital heart disease Department, Alexandria Faculty of as the most common birth defects observed in infants. More than 50 Medicine, Alexandria, Egypt classifications for limb anomalies based on morphology and osseous †Faculty of Allied Health Sciences, anatomy have been drafted over the past 150 years. The present work Kuwait University, Kuwait aims to provide a concise summary of the most common congenital limb ‡Neonatology Department, Adan anomalies on a morpho-etiological basis. Hospital, Kuwait PATIENTS AND METHODS: In a retrospective study, 70 newborns with §Kuwait Medical Genetics Centre, anomalies of the upper and/or lower limbs were ascertained through Maternity Hospital, Kuwait clinical examination, chromosomal analysis, skeletal surveys and other relevant investigations. Correspondence to: RESULTS: Fetal causes of limb anomalies represented 55.8% of the Shawky M Tayel, cases in the form of 9 cases (12.9%) with chromosomal aberrations Genetics Unit, (trisomy 13, 18 and 21, duplication 13q and deletion 22q) and 30 cases Anatomy Department, (42.9%) with single gene disorders. An environmental etiology for limb Alexandria Faculty of Medicine, anomalies was diagnosed in 11 cases (15.7%) as amniotic band disrup- Alexandria, Egypt. tion, monozygotic twin with abnormal circulation, vascular disruption Tel/Fax: 2-03-424-9150 (Poland sequence, sirenomelia and general vascular disruption) and an [email protected] infant with a diabetic mother. -

Hemimegalencephaly: Clinical Implications and Surgical Treatment
Childs Nerv Syst (2006) 22:852–866 DOI 10.1007/s00381-006-0149-9 SPECIAL ANNUAL ISSUE Hemimegalencephaly: clinical implications and surgical treatment C. Di Rocco & D. Battaglia & D. Pietrini & M. Piastra & L. Massimi Received: 24 May 2006 / Published online: 5 July 2006 # Springer-Verlag 2006 Abstract spherotomy is the most effective treatment to control seizure, Introduction Hemimegalencephaly (HME) is a quite rare and it also seems to provide good results on the psychomotor malformation of the cortical development arising from an development when performed early, as demonstrated by the abnormal proliferation of anomalous neuronal and glial literature review and by the personal series reported here (20 cells that generally leads to the hypertrophy of the whole children). The surgical therapy of HME, however, is still affected cerebral hemisphere. The pathogenesis of such a burdened by a quite high complication rate and mortality risk. complex malformation is still unknown even though several hypotheses are reported in literature. Keywords Hemimegalencephaly. Hemispherectomy . Background HME can occur alone or associated with neuro- Drug-resistant epilepsy. Epileptic outcome cutaneous disorders, such as neurofibromatosis, epidermal nevus syndrome, Ito’s hypomelanosis, and Klippel–Treno- nay–Weber syndrome. The clinical picture is usually domi- Introduction nated by a severe and drug-resistant epilepsy. Other common findings are represented by macrocrania, mean/severe mental Hemimegalencephaly is a rare congenital developmental retardation, unilateral motor deficit, and hemianopia. The EEG malformation of the brain characterized by the anomalous shows different abnormal patterns, mainly characterized by and dysplastic hypergrowth of one cerebral hemisphere or suppression burst and/or hemihypsarrhythmia. Although some of its lobes [4, 29, 62]. -

CASE REPORT 6-Month-Old Girl ONLINE EXCLUSIVE SIGNS & SYMPTOMS – Leg-Length Discrepancy
THE PATIENT CASE REPORT 6-month-old girl ONLINE EXCLUSIVE SIGNS & SYMPTOMS – Leg-length discrepancy – Asymmetric gluteal folds Beth P. Davis, DPT, MBA, and popliteal fossae FNAP; Amir Barzin, DO, MS; Cristen Page, MD, – Positive Galeazzi test MPH Emory University School of Medicine, Department of Rehabilitation Medicine, Division of Physical Therapy, Atlanta, Ga (Dr. Davis); Department of Family Medicine, School of Medicine, University of North Carolina at Chapel THE CASE Hill (Drs. Barzin and Page) A healthy 6-month-old girl born via spontaneous vaginal delivery to a 33-year-old mother [email protected] presented to her family physician (FP) for a routine well-child examination. The mother’s The authors reported no prenatal anatomy scan, delivery, and personal and family history were unremarkable. The potential conflict of interest patient was not firstborn or breech, and there was no family history of hip dysplasia. On prior relevant to this article. infant well-child examinations, Ortolani and Barlow maneuvers were negative, and the pa- tient demonstrated spontaneous movement of both legs. There was no evidence of hip dys- plasia, lower extremity weakness, musculoskeletal abnormalities, or abnormal skin markings. The patient had normal growth and development (50th percentile for height and weight, average Ages & Stages Questionnaire scores) and no history of infection or trauma. At the current presentation, the FP noted a leg-length discrepancy while palpating the bony (patellar and malleolar) landmarks of the lower extremities, but the right and left an- terior superior iliac spine was symmetrical. The gluteal folds and popliteal fossae were asym- metric, a Galeazzi test was positive, and the right leg measured approximately 2 cm shorter than the left leg.