Role of RAI2 Protein in the Progression of Prostate and Breast Cancer
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Downloaded from Bioscientifica.Com at 09/27/2021 05:40:52PM Via Free Access 328 I J BUJALSKA and Others
327 Expression profiling of 11b-hydroxysteroid dehydrogenase type-1 and glucocorticoid-target genes in subcutaneous and omental human preadipocytes I J Bujalska1, M Quinkler1,3, J W Tomlinson1, C T Montague2, D M Smith2 and P M Stewart1 1Division of Medical Sciences, The Medical School, Institute of Biomedical Research, University of Birmingham, Edgbaston, Birmingham B15 2TT, UK 2Diabetes Drug Discovery, AstraZeneca, Alderley Park, Macclesfield, Cheshire SK10 4TG, UK 3Clinical Endocrinology, Campus Mitte, Charite´ Universita¨tsmedizin Berlin, Berlin, Germany (Requests for offprints should be addressed to P M Stewart; Email: [email protected]) Abstract Obesity is associated with increased morbidity and mortality from cardiovascular disease, diabetes and cancer. Although obesity is a multi-factorial heterogeneous condition, fat accumulation in visceral depots is most highly associated with these risks. Pathological glucocorticoid excess (i.e. in Cushing’s syndrome) is a recognised, reversible cause of visceral fat accumulation. The aim of this study was to identify depot-specific glucocorticoid-target genes in adipocyte precursor cells (preadipocytes) using Affymetrix microarray technique. Confluent preadipocytes from subcutaneous (SC) and omental (OM) adipose tissue collected from five female patients were treated for 24 h with 100 nM cortisol (F), RNA was pooled and hybridised to the Affymetrix U133 microarray set. We identified 72 upregulated and 30 downregulated genes by F in SC cells. In OM preadipocytes, 56 genes were increased and 19 were decreased. Among the most interesting were transcription factors, markers of adipocyte differentiation and glucose metabolism, cell adhesion and growth arrest protein factors involved in G-coupled and Wnt signalling. The Affymetrix data have been confirmed by quantitative real- time PCR for ten specific genes, including HSD11B1, GR, C/EBPa, C/EBPb, IL-6, FABP4, APOD, IRS2, AGTR1 and GHR. -

De Novo Transcriptome Analysis of White Teak (Gmelina Arborea Roxb
Yaya Lancheros et al. BMC Genomics (2021) 22:494 https://doi.org/10.1186/s12864-021-07777-x RESEARCH ARTICLE Open Access De novo transcriptome analysis of white teak (Gmelina arborea Roxb) wood reveals critical genes involved in xylem development and secondary metabolism Mary Luz Yaya Lancheros1, Krishan Mohan Rai2,3, Vimal Kumar Balasubramanian2,4, Lavanya Dampanaboina2, Venugopal Mendu2 and Wilson Terán1* Abstract Background: Gmelina arborea Roxb is a fast-growing tree species of commercial importance for tropical countries due to multiple industrial uses of its wood. Wood is primarily composed of thick secondary cell walls of xylem cells which imparts the strength to the wood. Identification of the genes involved in the secondary cell wall biosynthesis as well as their cognate regulators is crucial to understand how the production of wood occurs and serves as a starting point for developing breeding strategies to produce varieties with improved wood quality, better paper pulping or new potential uses such as biofuel production. In order to gain knowledge on the molecular mechanisms and gene regulation related with wood development in white teak, a de novo sequencing and transcriptome assembly approach was used employing secondary cell wall synthesizing cells from young white teak trees. Results: For generation of transcriptome, RNA-seq reads were assembled into 110,992 transcripts and 49,364 genes were functionally annotated using plant databases; 5071 GO terms and 25,460 SSR markers were identified within xylem transcripts and 10,256 unigenes were assigned to KEGG database in 130 pathways. Among transcription factor families, C2H2, C3H, bLHLH and MYB were the most represented in xylem. -

Nuclear Organization and the Epigenetic Landscape of the Mus Musculus X-Chromosome Alicia Liu University of Connecticut - Storrs, [email protected]
University of Connecticut OpenCommons@UConn Doctoral Dissertations University of Connecticut Graduate School 8-9-2019 Nuclear Organization and the Epigenetic Landscape of the Mus musculus X-Chromosome Alicia Liu University of Connecticut - Storrs, [email protected] Follow this and additional works at: https://opencommons.uconn.edu/dissertations Recommended Citation Liu, Alicia, "Nuclear Organization and the Epigenetic Landscape of the Mus musculus X-Chromosome" (2019). Doctoral Dissertations. 2273. https://opencommons.uconn.edu/dissertations/2273 Nuclear Organization and the Epigenetic Landscape of the Mus musculus X-Chromosome Alicia J. Liu, Ph.D. University of Connecticut, 2019 ABSTRACT X-linked imprinted genes have been hypothesized to contribute parent-of-origin influences on social cognition. A cluster of imprinted genes Xlr3b, Xlr4b, and Xlr4c, implicated in cognitive defects, are maternally expressed and paternally silent in the murine brain. These genes defy classic mechanisms of autosomal imprinting, suggesting a novel method of imprinted gene regulation. Using Xlr3b and Xlr4c as bait, this study uses 4C-Seq on neonatal whole brain of a 39,XO mouse model, to provide the first in-depth analysis of chromatin dynamics surrounding an imprinted locus on the X-chromosome. Significant differences in long-range contacts exist be- tween XM and XP monosomic samples. In addition, XM interaction profiles contact a greater number of genes linked to cognitive impairment, abnormality of the nervous system, and abnormality of higher mental function. This is not a pattern that is unique to the imprinted Xlr3/4 locus. Additional Alicia J. Liu - University of Connecticut - 2019 4C-Seq experiments show that other genes on the X-chromosome, implicated in intellectual disability and/or ASD, also produce more maternal contacts to other X-linked genes linked to cognitive impairment. -

Identification of a Microdeletion at Xp22.13 in a Taiwanese Family
Journal of Human Genetics (2011) 56, 8–11 & 2011 The Japan Society of Human Genetics All rights reserved 1434-5161/11 $32.00 www.nature.com/jhg ORIGINAL ARTICLE Identification of a microdeletion at Xp22.13 in a Taiwanese family presenting with Nance-Horan syndrome Hsiao-Mei Liao1, Dau-Ming Niu2,3, Yan-Jang Chen4,5, Jye-Siung Fang6, Shih-Jen Chen7 and Chia-Hsiang Chen8,9,10 Nance-Horan syndrome (NHS) is a rare X-linked disorder characterized by congenital cataracts, dental anomalies and mental retardation. The disease has been linked to a novel gene termed NHS located at Xp22.13. The majority of pathogenic mutations of the disease include nonsense mutations and small deletions and insertions that lead to truncation of the NHS protein. In this study, we identified a microdeletion of B0.92 Mb at Xp22.13 detected by array-based comparative genomic hybridization in two brothers presenting congenital cataract, dental anomalies, facial dysmorphisms and mental retardation. The deleted region encompasses the REPS2, NHS, SCML1 and RAI2 genes, and was transmitted from their carrier mother who presented only mild cataract. Our findings are in line with several recent case reports to indicate that genomic rearrangement involving the NHS gene is an important genetic etiology underlying NHS. Journal of Human Genetics (2011) 56, 8–11; doi:10.1038/jhg.2010.121; published online 30 September 2010 Keywords: array CGH; congenital cataract; mental retardation; microdeletion; Nance-Horan syndrome INTRODUCTION associated with patient with NHS or X-linked congenital cataract,6,12 Nance-Horan syndrome (NHS) (OMIM 302350) is a rare X-linked suggesting that genomic rearrangement also contributes to the genetic genetic disorder characterized by congenital cataracts, dental defects, etiology underlying the NHS. -

Refinement of the NHS Locus on Chromosome Xp22.13 and Analysis
European Journal of Human Genetics (2002) 10, 516 – 520 ª 2002 Nature Publishing Group All rights reserved 1018 – 4813/02 $25.00 www.nature.com/ejhg ARTICLE Refinement of the NHS locus on chromosome Xp22.13 and analysis of five candidate genes Annick Toutain*,1, Benoıˆt Dessay1, Nathalie Ronce1, Maria-Immacolata Ferrante2, Julie Tranchemontagne3, Ruth Newbury-Ecob4, Carina Wallgren-Pettersson5, John Burn6, Josseline Kaplan7, Annick Rossi8, Silvia Russo9, Ian Walpole10, James K Hartsfield11, Nina Oyen12, Andrea Nemeth13, Pierre Bitoun14, Dorothy Trump15, Claude Moraine1 and Brunella Franco2 1Service de Ge´ne´tique, Hoˆpital Bretonneau, Centre Hospitalo-Universitaire, Tours, France; 2Telethon Institute of Genetics and Medicine, Naples, Italy; 3Medical Genetics Division, Children’s Hospital, Montreal, Canada; 4Clinical Genetics Service, Institute of Child Health, Bristol Royal Hospital for Sick Children, Bristol, UK; 5Department of Medical Genetics, University of Helsinki, Finland; 6Institute of Human Genetics, Newcastle upon Tyne, UK; 7Service de Ge´ne´tique Me´dicale, Hoˆpital Necker-Enfants Malades, Paris, France; 8EFS, Bois Guillaume, France; 9Laboratorio Biologia Molecolare, Instituto Auxologico Italiano, Milano, Italy; 10Genetic Services, Princess Margaret Hospital for Sick Children, Perth, Australia; 11Department of Oral Facial Development, Oral Facial Genetics Section, Indiana University School of Dentistry, Indianapolis, Indiana, USA; 12Center for Medical Genetics and Molecular Medicine, Haukeland University Hospital, Bergen, Norway; 13Oxford Clinical Genetic Service, Department of Clinical Genetics, Oxford Radcliffe Hospital NHS Trust, Oxford, UK; 14SIDVA 91, Savigny sur Orge, France; 15Department of Medical Genetics, Cambridge Institute for Medical Research, University of Cambridge, UK Nance-Horan syndrome (NHS) is an X-linked condition characterised by congenital cataracts, dental abnormalities, dysmorphic features, and mental retardation in some cases. -

Book of Abstracts
PEMED 2018 Personalized and Precision Medicine International Conference June 25-27, 2018 Paris BOOK OF ABSTRACTS premc.org Personalized and Precision Medicine International Conference 2018 Table of Contents Polypharmacology of Anti-Cancer Antibodies 1 Prof. Yosef Yarden Population-wide data and text mining of electronic health records 2 Prof. Lars Juhl Jensen DIAGENODE: Epigenomics Profiling Services 3 Dr. Matteo Tosolini Pharmacogenomics and Epigenetics: Update and Future Directions 4 Prof. Matthias Schwab How can dendrimers contribute to precision/personalized medicine? 5 Prof. Anne-marie Caminade Novel Hot Spot Mutations in BCR-ABL1: a Personalised Medicine Approach in Chronic Myeloid Leukaemia 7 Dr. Erik Laurini, Dr. Suzana Aulic, Dr. Domenico Marson, Prof. Maurizio Fermeglia, Prof. Sabrina Pricl Cluster analysis of oncogenes associated with colorectal cancer 8 Dr. Dmitriy Babenko, Mrs. Yelena Babenko Influence of combined CYP3A4 and CYP3A5 single-nucleotide polymorphisms on tacrolimus exposure in kidney transplant recipients 10 Ms. Ibtissem Hannachi, Dr. Zohra CHADLI, Dr. Emna Kerkeni, Dr. Amel Chaabane, Dr. Nadia Ben Fredj, Prof. Naceur Boughattas, Prof. Karim Aouam Transient neonatal diabetes : multilocus methylation defects associated with novel ZFP57 mutation 11 Ms. Ameni Touati, Dr. Javier Errea, Prof. Sonia Nouri, Dr. Arreta Pereda, Dr. Aida Guith, Prof. Nabiha Mahd- haoui, Prof. Ali Saad, Prof. Guiomar Perez De Nanclares, Prof. Dorra H’mida Targeting the JNK-JUN pathway to reduce phenotypic plasticity and overcome therapy resistance in metastatic melanoma 12 Dr. Petranel Ferrao Pharmacogenomics of Sickle Cell Disease: Pain and Drug metabolism associated Gene Variants, and hydroxyurea-induced miRNAs 13 Ms. Khuthala Mnika, Prof. Wonkam Ambroise, Dr. Emile Chimusa, Prof. Collet Dandara, Dr. -

97857 RAI2 (D4W9P) Rabbit Mab
Revision 1 C 0 2 - t RAI2 (D4W9P) Rabbit mAb a e r o t S Orders: 877-616-CELL (2355) [email protected] 7 Support: 877-678-TECH (8324) 5 8 Web: [email protected] 7 www.cellsignal.com 9 # 3 Trask Lane Danvers Massachusetts 01923 USA For Research Use Only. Not For Use In Diagnostic Procedures. Applications: Reactivity: Sensitivity: MW (kDa): Source/Isotype: UniProt ID: Entrez-Gene Id: WB, IP H Endogenous 78 Rabbit IgG Q9Y5P3 10742 Product Usage Information Application Dilution Western Blotting 1:1000 Immunoprecipitation 1:50 Storage Supplied in 10 mM sodium HEPES (pH 7.5), 150 mM NaCl, 100 µg/ml BSA, 50% glycerol and less than 0.02% sodium azide. Store at –20°C. Do not aliquot the antibody. Specificity / Sensitivity RAI2 (D4W9P) Rabbit mAb recognizes endogenous levels of total RAI2 protein. Species Reactivity: Human Species predicted to react based on 100% sequence homology: Mouse, Rat, Bovine, Pig Source / Purification Monoclonal antibody is produced by immunizing animals with a synthetic peptide corresponding to residues surrounding Arg522 of human RAI2 protein. Background Retinoic acid-induced protein 2 (RAI2) is a 530 amino acid protein, encoded by the RAI2 gene on XP22.3 (1). RAI2 contains a central, proline-rich domain that is hypothesized to play a role in protein-protein interactions, and is expressed in a variety of embryonic and adult tissues (2). Beyond that, little is known about the biological functions of RAI2. Notably, a 2015 research study reported that suppressing RAI2 led to increased hematogenous dissemination of breast cancer cells to bone marrow, suggesting that RAI2 may function to negatively regulate tumor metastasis (3). -

New Possible Targetable Genes for Future Treatment of Mixed Lineage Leukemia Senol Dogan* International Burch University, Sarajevo, Bosnia and Herzegovina
etrics iom & B B f io o l s t a a n t Dogan, J Biom Biostat 2017, 8:3 r i s u t i o c J s Journal of Biometrics & Biostatistics DOI: 10.4172/2155-6180.1000349 ISSN: 2155-6180 Research Ar ticleArticle Open Access New Possible Targetable Genes for Future Treatment of Mixed Lineage Leukemia Senol Dogan* International Burch University, Sarajevo, Bosnia and Herzegovina Abstract Aim of study: Leukemia has different subtypes, which present unique clinical and molecular characteristics. MLL (Mixed Lineage Leukemia) is one of the new different subtypes than AML and ALL. Materials and Methods: Genomic characterization is the main key understanding the differences of MLL by analysis of differential gene expression, methylation patterns and mutational spectra that were compared and analyzed between MLL and AML types (n=197). Results: According to the genomic characterization of MLL, differentially expressed 114 genes were selected and 37 of them targeted genes having more than 2 fold expression change, including HOXA9, CFH, DDX4, MSH4, MSMB, TWIST1, ZSWIM2, POU6F2. To measure the aberrant methylation is the second genomic characterization of this research because the rearrangements of MLL gene leading to aberrant methylation. The methylation data were compared between cancer and control, so high methylated genes have been detected between MLL and AML types. The methylation loci were categorized into two groups: ≥ 10 fold difference and ≥ 5 and ≤ 10 fold difference. Some of the genes high methylated more than one location such as; RAET1E, HSD17B2, RNASE11, DGK1, POU6F2, NAGS, PIK3C2G, GADL1, and KRT13. In addition to that, analysis of somatic mutation gives us that CFH has the highest point mutation 9,92%. -

Mitotic Checkpoints and Chromosome Instability Are Strong Predictors of Clinical Outcome in Gastrointestinal Stromal Tumors
MITOTIC CHECKPOINTS AND CHROMOSOME INSTABILITY ARE STRONG PREDICTORS OF CLINICAL OUTCOME IN GASTROINTESTINAL STROMAL TUMORS. Pauline Lagarde1,2, Gaëlle Pérot1, Audrey Kauffmann3, Céline Brulard1, Valérie Dapremont2, Isabelle Hostein2, Agnès Neuville1,2, Agnieszka Wozniak4, Raf Sciot5, Patrick Schöffski4, Alain Aurias1,6, Jean-Michel Coindre1,2,7 Maria Debiec-Rychter8, Frédéric Chibon1,2. Supplemental data NM cases deletion frequency. frequency. deletion NM cases Mand between difference the highest setswith of theprobe a view isdetailed panel Bottom frequently. sorted totheless deleted theprobe are frequently from more and thefrequency deletion represent Yaxes inblue. are cases (NM) metastatic for non- frequencies Corresponding inmetastatic (red). probe (M)cases sets figureSupplementary 1: 100 100 20 40 60 80 20 40 60 80 0 0 chr14 1 chr14 88 chr14 175 chr14 262 chr9 -MTAP 349 chr9 -MTAP 436 523 chr9-CDKN2A 610 Histogram presenting the 2000 more frequently deleted deleted frequently the 2000 more presenting Histogram chr9-CDKN2A 697 chr9-CDKN2A 784 chr9-CDKN2B 871 chr9-CDKN2B 958 chr9-CDKN2B 1045 chr22 1132 chr22 1219 chr22 1306 chr22 1393 1480 1567 M NM 1654 1741 1828 1915 M NM GIST14 GIST2 GIST16 GIST3 GIST19 GIST63 GIST9 GIST38 GIST61 GIST39 GIST56 GIST37 GIST47 GIST58 GIST28 GIST5 GIST17 GIST57 GIST47 GIST58 GIST28 GIST5 GIST17 GIST57 CDKN2A Supplementary figure 2: Chromosome 9 genomic profiles of the 18 metastatic GISTs (upper panel). Deletions and gains are indicated in green and red, respectively; and color intensity is proportional to copy number changes. A detailed view is given (bottom panel) for the 6 cases presenting a homozygous 9p21 deletion targeting CDKN2A locus (dark green). -

Targeted Exome Sequencing Identifies PBX1 As Involved In
BASIC RESEARCH www.jasn.org Targeted Exome Sequencing Identifies PBX1 as Involved in Monogenic Congenital Anomalies of the Kidney and Urinary Tract † ‡ | | Laurence Heidet,* Vincent Morinière,* Charline Henry,§ Lara De Tomasi,§ ¶ | | ‡†† Madeline Louise Reilly,§ ¶ Camille Humbert,§ Olivier Alibeu,** Cécile Fourrage, †† †† †† Christine Bole-Feysot,** Patrick Nitschké, Frédéric Tores, Marc Bras, |‡‡ || Marc Jeanpierre, Christine Pietrement,§§ Dominique Gaillard, Marie Gonzales,¶¶ ††† ‡‡‡ ||| Robert Novo,*** Elise Schaefer, Joëlle Roume, Jelena Martinovic,§§§ Valérie Malan, † | | ‡ | | Rémi Salomon,* § Sophie Saunier,§ Corinne Antignac, § and Cécile Jeanpierre§ *Assistance Publique - Hôpitaux de Paris, Centre de référence des Maladies Rénales Héréditaires de l’Enfant et de l’Adulte, Paris, France; †Assistance Publique - Hôpitaux de Paris, Service de Néphrologie Pédiatrique, ‡Assistance Publique - Hôpitaux de Paris, Département de Génétique, and |||Assistance Publique - Hôpitaux de Paris, Service de Cytogénétique, Hôpital Universitaire Necker- Enfants malades, Paris, France; §Institut National de la Santé et de la Recherche Médicale Unité Mixte de Recherche 1163, Laboratory of Hereditary Kidney Diseases, **Genomic Platform, Institut National de la Santé et de la Recherche Médicale Unité Mixte de Recherche 1163, Paris Descartes Sorbonne Paris Cité University, and ††Bioinformatic Plateform, Paris Descartes Sorbonne Paris Cité University, Imagine Institute, Paris, France; |Paris Descartes Sorbonne Paris Cité University, Paris, France; ¶Paris -

A Locus for Isolated Cataract on Human Xp P J Francis, V Berry, a J Hardcastle, E R Maher, a T Moore, S S Bhattacharya
105 ORIGINAL ARTICLE J Med Genet: first published as 10.1136/jmg.39.2.105 on 1 February 2002. Downloaded from A locus for isolated cataract on human Xp P J Francis, V Berry, A J Hardcastle, E R Maher, A T Moore, S S Bhattacharya ............................................................................................................................. See end of article for J Med Genet 2002;39:105–109 authors’ affiliations ....................... Purpose: To genetically map the gene causing isolated X linked cataract in a large European Correspondence to: Professor S S Bhattacharya, pedigree. Department of Molecular Methods: Using the patient registers at Birmingham Women’s Hospital, UK, we identified and exam- Genetics, Institute of ined 23 members of a four generation family with nuclear cataract. Four of six affected males also had Ophthalmology, 11-43 complex congenital heart disease. Pedigree data were collated and leucocyte DNA extracted from Bath Street, London venous blood. Linkage analysis by PCR based microsatellite marker genotyping was used to identify the EC1V 9EL, UK; [email protected] disease locus and mutations within candidate genes screened by direct sequencing. Results: The disease locus was genetically refined to chromosome Xp22, withina3cMlinkage inter- Revised version received val flanked by markers DXS9902 and DXS999 (Zmax=3.64 at θ=0 for marker DXS8036). 4 November 2001 Accepted for publication Conclusions: This is the first report of a locus for isolated inherited cataract on the X chromosome. The 5 November 2001 disease interval lies within the Nance-Horan locus suggesting allelic heterogeneity. The apparent ....................... association with congenital cardiac anomalies suggests a possible new oculocardiac syndrome. ongenital cataract is the most common treatable cause reported, though in many other modes of inheritance appear of childhood blindness in the western world.1 In certain more likely. -
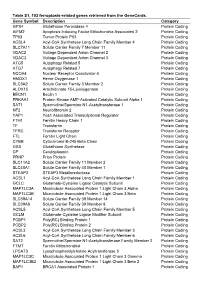
Table S1. 103 Ferroptosis-Related Genes Retrieved from the Genecards
Table S1. 103 ferroptosis-related genes retrieved from the GeneCards. Gene Symbol Description Category GPX4 Glutathione Peroxidase 4 Protein Coding AIFM2 Apoptosis Inducing Factor Mitochondria Associated 2 Protein Coding TP53 Tumor Protein P53 Protein Coding ACSL4 Acyl-CoA Synthetase Long Chain Family Member 4 Protein Coding SLC7A11 Solute Carrier Family 7 Member 11 Protein Coding VDAC2 Voltage Dependent Anion Channel 2 Protein Coding VDAC3 Voltage Dependent Anion Channel 3 Protein Coding ATG5 Autophagy Related 5 Protein Coding ATG7 Autophagy Related 7 Protein Coding NCOA4 Nuclear Receptor Coactivator 4 Protein Coding HMOX1 Heme Oxygenase 1 Protein Coding SLC3A2 Solute Carrier Family 3 Member 2 Protein Coding ALOX15 Arachidonate 15-Lipoxygenase Protein Coding BECN1 Beclin 1 Protein Coding PRKAA1 Protein Kinase AMP-Activated Catalytic Subunit Alpha 1 Protein Coding SAT1 Spermidine/Spermine N1-Acetyltransferase 1 Protein Coding NF2 Neurofibromin 2 Protein Coding YAP1 Yes1 Associated Transcriptional Regulator Protein Coding FTH1 Ferritin Heavy Chain 1 Protein Coding TF Transferrin Protein Coding TFRC Transferrin Receptor Protein Coding FTL Ferritin Light Chain Protein Coding CYBB Cytochrome B-245 Beta Chain Protein Coding GSS Glutathione Synthetase Protein Coding CP Ceruloplasmin Protein Coding PRNP Prion Protein Protein Coding SLC11A2 Solute Carrier Family 11 Member 2 Protein Coding SLC40A1 Solute Carrier Family 40 Member 1 Protein Coding STEAP3 STEAP3 Metalloreductase Protein Coding ACSL1 Acyl-CoA Synthetase Long Chain Family Member 1 Protein