CHAPTER Procedures on Urinary System 11
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Urology Services in the ASC
Urology Services in the ASC Brad D. Lerner, MD, FACS, CASC Medical Director Summit ASC President of Chesapeake Urology Associates Chief of Urology Union Memorial Hospital Urologic Consultant NFL Baltimore Ravens Learning Objectives: Describe the numerous basic and advanced urology cases/lines of service that can be provided in an ASC setting Discuss various opportunities regarding clinical, operational and financial aspects of urology lines of service in an ASC setting Why Offer Urology Services in Your ASC? Majority of urologic surgical services are already outpatient Many urologic procedures are high volume, short duration and low cost Increasing emphasis on movement of site of service for surgical cases from hospitals and insurance carriers to ASCs There are still some case types where patients are traditionally admitted or placed in extended recovery status that can be converted to strictly outpatient status and would be suitable for an ASC Potential core of fee-for-service case types (microsurgery, aesthetics, prosthetics, etc.) Increasing Population of Those Aged 65 and Over As of 2018, it was estimated that there were 51 million persons aged 65 and over (15.63% of total population) By 2030, it is expected that there will be 72.1 million persons aged 65 and over National ASC Statistics - 2017 Urology cases represented 6% of total case mix for ASCs Urology cases were 4th in median net revenue per case (approximately $2,400) – behind Orthopedics, ENT and Podiatry Urology comprised 3% of single specialty ASCs (5th behind -

Delineation of Privileges Urology Privileges Provider Name
Delineation Of Privileges Urology Privileges Provider Name: Privilege Requested Deferred Approved UROLOGY PRIVILEGES Criteria - New Applicants:: Board Certification or qualified for certification by the American Board of Urology. Criteria - Current Staff Members Only: Successful completion of an ACGME or AOA approved training program; OR demonstrated acceptable practice in the privileges being requested for a minimum of five (5) years. Proctoring Requirements: A minimum of eight (8) cases, in accordance with the Medical Staff Proctoring Protocol. GENERAL PRIVILEGES: Admit ___ ___ ___ Consultation Only Privileges ___ ___ ___ Surgical Assist Only ___ ___ ___ Local block anesthesia ___ ___ ___ Regional block anesthesia ___ ___ ___ Sedation analgesia ___ ___ ___ Criteria: Requires successful completion of the Sedation Assessment test. Additional criteria effective April 1, 2015: a) Evidence of current ACLS and/or PALS certification from the American Heart Association; AND b) Evidence of completion of an Airway Management Course a) Adult Sedation ___ ___ ___ b) Pediatric Sedation (17 years and under) ___ ___ ___ CATEGORY 1 - UROLOGY PRIVILEGES ___ ___ ___ Includes the management and coordination of care, treatment and services, including: medical history and physical evaluations, consultations and prescribing medication in accordance with DEA certificate. Urethral, bladder catheterization ___ ___ ___ Suprapubic, bladder aspiration ___ ___ ___ Page 1 Printed on Wednesday, December 10, 2014 Delineation Of Privileges Urology Privileges Provider -

Glickman Urological & Kidney Institute
C L E V E GLICKMAN UROLOGICAL L A N D C L I N I C & KIDNEY INSTITUTE | G L I C K 2019 Year in Review M The Cleveland Clinic Foundation A N 9500 Euclid Ave. / AC311 U R O Cleveland, OH 44195 L O G I C A L & K I D N E Y I N S T I T U T E | 2 0 1 9 Y E A R I N R E V I E W 19-URL-5068 22877_CCFBCH_19URL4030_19URL5068_ACG.indd 29-31 2/6/20 3:06 PM CONTENTS 3 Glickman Kidney & Urological Institute at a Glance 7 Message from the Chairman 9 Two Clinical Trials, One Ambitious Goal to Personalize Kidney Medicine 11 A New Paradigm for Advanced Prostate Cancer Clinical Trials 13 Another Landmark Year for Cleveland Clinic’s Kidney Transplant Program 15 Getting It Right: Nephrologists Are Working to Minimize the ‘White-Coat Effect’ for Patients with Hypertension 17 ‘A FitBit for the Bladder’: UroMonitor Takes Monitoring Out of the Clinic 19 Virtual Reality Tool to Offer New Way of Understanding Renal Physiology 21 First Kidney Transplant Performed Using Single-Port Robot 22 2019 Achievements 28 Resources for Physicians ON THE COVER Georges Nakhoul, MD, Director of the Center for Chronic Kidney Disease, launched a virtual reality program to enhance the renal physiology learning experience for trainees. 22877_CCFBCH_19URL4030_19URL5068_ACG.indd 32-34 2/6/20 3:06 PM CLEVELAND CLINIC GLICKMAN UROLOGICAL & KIDNEY INSTITUTE | 3 Glickman Urological AT A GLANCE & Kidney Institute The Glickman Urological BY THE NUMBERS & Kidney Institute’s (2019) activities encompass a unique combination of high- 132,663 volume and challenging OUTPATIENT VISITS clinical cases, extensive basic and translational scientific efforts, and 14,098 innovative laboratory SURGICAL CASES research conducted in an environment that nurtures the future leaders of its 21,255 DIALYSIS TREATMENTS specialties. -

Public Use Data File Documentation
Public Use Data File Documentation Part III - Medical Coding Manual and Short Index National Health Interview Survey, 1995 From the CENTERSFOR DISEASECONTROL AND PREVENTION/NationalCenter for Health Statistics U.S. DEPARTMENTOF HEALTHAND HUMAN SERVICES Centers for Disease Control and Prevention National Center for Health Statistics CDCCENTERS FOR DlSEASE CONTROL AND PREVENTlON Public Use Data File Documentation Part Ill - Medical Coding Manual and Short Index National Health Interview Survey, 1995 U.S. DEPARTMENT OF HEALTHAND HUMAN SERVICES Centers for Disease Control and Prevention National Center for Health Statistics Hyattsville, Maryland October 1997 TABLE OF CONTENTS Page SECTION I. INTRODUCTION AND ORIENTATION GUIDES A. Brief Description of the Health Interview Survey ............. .............. 1 B. Importance of the Medical Coding ...................... .............. 1 C. Codes Used (described briefly) ......................... .............. 2 D. Appendix III ...................................... .............. 2 E, The Short Index .................................... .............. 2 F. Abbreviations and References ......................... .............. 3 G. Training Preliminary to Coding ......................... .............. 4 SECTION II. CLASSES OF CHRONIC AND ACUTE CONDITIONS A. General Rules ................................................... 6 B. When to Assign “1” (Chronic) ........................................ 6 C. Selected Conditions Coded ” 1” Regardless of Onset ......................... 7 D. When to Assign -

Ureteroscopic Treatment of Larger Renal Calculi (>2 Cm)
Thomas Jefferson University Jefferson Digital Commons Department of Urology Faculty Papers Department of Urology 9-1-2012 Ureteroscopic treatment of larger renal calculi (>2 cm). Demetrius H. Bagley Thomas Jefferson University Kelly A. Healy Thomas Jefferson University Nir Kleinmann Thomas Jefferson University Follow this and additional works at: https://jdc.jefferson.edu/urologyfp Part of the Urology Commons Let us know how access to this document benefits ouy Recommended Citation Bagley, Demetrius H.; Healy, Kelly A.; and Kleinmann, Nir, "Ureteroscopic treatment of larger renal calculi (>2 cm)." (2012). Department of Urology Faculty Papers. Paper 45. https://jdc.jefferson.edu/urologyfp/45 This Article is brought to you for free and open access by the Jefferson Digital Commons. The Jefferson Digital Commons is a service of Thomas Jefferson University's Center for Teaching and Learning (CTL). The Commons is a showcase for Jefferson books and journals, peer-reviewed scholarly publications, unique historical collections from the University archives, and teaching tools. The Jefferson Digital Commons allows researchers and interested readers anywhere in the world to learn about and keep up to date with Jefferson scholarship. This article has been accepted for inclusion in Department of Urology Faculty Papers by an authorized administrator of the Jefferson Digital Commons. For more information, please contact: [email protected]. Arab Journal of Urology (2012) 10, 296–300 Arab Journal of Urology (Official Journal of the Arab -

Fy 2020 Acs Ipps
June 24, 2019 Seema Verma, Administrator Centers for Medicare & Medicaid Services Attention: CMS-1716-P P.O. Box 8013 Baltimore, MD 21244-1850 RE: Medicare Program; Hospital Inpatient Prospective Payment Systems for Acute Care Hospitals and the Long-Term Care Hospital Prospective Payment System and Proposed Policy Changes and Fiscal Year 2020 Rates; Proposed Quality Reporting Requirements for Specific Providers; Medicare and Medicaid Promoting Interoperability Programs Proposed Requirements for Eligible Hospitals and Critical Access Hospitals Dear Ms. Verma: On behalf of the over 80,000 members of the American College of Surgeons (ACS), we appreciate the opportunity to submit comments to the Centers for Medicare & Medicaid Services’ (CMS) proposed rule, Medicare Program; Hospital Inpatient Prospective Payment Systems for Acute Care Hospitals and the Long-Term Care Hospital Prospective Payment System and Proposed Policy Changes and Fiscal Year 2020 Rates; Proposed Quality Reporting Requirements for Specific Providers; Medicare and Medicaid Promoting Interoperability Programs Proposed Requirements for Eligible Hospitals and Critical Access Hospitals, published in the Federal Register on May 3, 2019. The ACS is a scientific and educational association of surgeons founded in 1913 to improve the quality of care for patients by setting high standards for surgical education and practice. Since a large portion of surgical care is provided in the inpatient hospital setting, the College has a vested interest in CMS’ Inpatient Prospective Payment System (IPPS) and related hospital quality improvement efforts, and we believe that we can offer insight to CMS’ proposed modifications to these policies for fiscal year (FY) 2020. Our comments below are presented in the order in which they appear in the proposed rule. -

EAU Guidelines Primary Urethral Carcinomas V2
Guidelines on Primary Urethral Carcinoma G. Gakis, J.A. Witjes, E. Compérat, N.C. Cowan, M. De Santis, T. Lebret, M.J. Ribal, A. Sherif © European Association of Urology 2013 TABLE OF CONTENTS PAGE 1. INTRODUCTION 3 2. METHODOLOGY 3 3. LEVEL OF EVIDENCE AND GRADE OF RECOMMENDATION 3 4. EPIDEMIOLOGY 4 5. ETIOLOGY AND RISK FACTORS 4 6. HISTOPATHOLOGY 5 7. CLASSIFICATION 5 7.1 TNM staging system 5 7.2 Tumour grade 6 8. SURVIVAL 6 8.1 Long-term survival after primary urethral carcinoma 6 8.2 Predictors of survival in primary urethral carcinoma 6 9. DIAGNOSIS AND STAGING 7 9.1 History 7 9.2 Clinical examination 7 9.3 Urinary cytology 7 9.4 Diagnostic urethrocystoscopy and biopsy 7 9.5 Radiological imaging 7 9.6 Regional lymph nodes 7 10. TREATMENT OF LOCALISED PRIMARY URETHRAL CARCINOMA 8 10.1 Treatment of localised primary urethral carcinoma in males 8 10.2 Treatment of localised urethral carcinoma in females 8 10.2.1 Urethrectomy and urethra-sparing surgery 8 10.2.2 Radiotherapy 8 11. MULTIMODAL TREATMENT IN ADVANCED URETHRAL CARCINOMA 9 11.1 Preoperative cisplatinum-based chemotherapy 9 11.2 Preoperative chemoradiotherapy in locally advanced squamous cell carcinoma of the urethra 9 12. TREATMENT OF UROTHELIAL CARCIMONA OF THE PROSTATE 10 13. FOLLOW-UP 10 14. REFERENCES 10 15. ABBREVIATIONS USED IN THE TEXT 15 2 PRIMARY URETHRAL CARCINOMAS - MARCH 2013 1. INTRODUCTION The European Association of Urology (EAU) Guidelines Group on Muscle-invasive and Metastatic Bladder Cancer has prepared these guidelines to deliver current evidence-based information on the diagnosis and treatment of patients with primary urethral carcinoma (UC). -

Icd-9-Cm (2010)
ICD-9-CM (2010) PROCEDURE CODE LONG DESCRIPTION SHORT DESCRIPTION 0001 Therapeutic ultrasound of vessels of head and neck Ther ult head & neck ves 0002 Therapeutic ultrasound of heart Ther ultrasound of heart 0003 Therapeutic ultrasound of peripheral vascular vessels Ther ult peripheral ves 0009 Other therapeutic ultrasound Other therapeutic ultsnd 0010 Implantation of chemotherapeutic agent Implant chemothera agent 0011 Infusion of drotrecogin alfa (activated) Infus drotrecogin alfa 0012 Administration of inhaled nitric oxide Adm inhal nitric oxide 0013 Injection or infusion of nesiritide Inject/infus nesiritide 0014 Injection or infusion of oxazolidinone class of antibiotics Injection oxazolidinone 0015 High-dose infusion interleukin-2 [IL-2] High-dose infusion IL-2 0016 Pressurized treatment of venous bypass graft [conduit] with pharmaceutical substance Pressurized treat graft 0017 Infusion of vasopressor agent Infusion of vasopressor 0018 Infusion of immunosuppressive antibody therapy Infus immunosup antibody 0019 Disruption of blood brain barrier via infusion [BBBD] BBBD via infusion 0021 Intravascular imaging of extracranial cerebral vessels IVUS extracran cereb ves 0022 Intravascular imaging of intrathoracic vessels IVUS intrathoracic ves 0023 Intravascular imaging of peripheral vessels IVUS peripheral vessels 0024 Intravascular imaging of coronary vessels IVUS coronary vessels 0025 Intravascular imaging of renal vessels IVUS renal vessels 0028 Intravascular imaging, other specified vessel(s) Intravascul imaging NEC 0029 Intravascular -

Urolithiasis
Guidelines on Urolithiasis C. Türk (chairman), T. Knoll (vice-chairman), A. Petrik, K. Sarica, M. Straub, C. Seitz © European Association of Urology 2012 TABLE OF CONTENTS PAGE 1. METHODOLOGY 7 1.1 Introduction 7 1.2 Data identification 7 1.3 Evidence sources 7 1.4 Level of evidence and grade of recommendation 7 1.5 Publication history 8 1.5.1 Summary of changes 8 1.6 References 9 2. CLASSIFICATION OF STONES 10 2.1 Stone size 10 2.2 Stone location 10 2.3 X-ray characteristics 10 2.4 Aetiology of stone formation 10 2.5 Stone composition 10 2.6 Risk groups for stone formation 11 2.7 References 12 3. DIAGNOSIS 12 3.1 Diagnostic imaging 12 3.1.1 Evaluation of patients with acute flank pain 13 3.1.2 Evaluation of patients for whom further treatment of renal stones is planned 14 3.1.3 References 14 3.2 Diagnostics - metabolism-related 15 3.2.1 Basic analysis - non-emergency stone patients 16 3.2.2 Analysis of stone composition 16 3.3 References 17 4. TREATMENT OF PATIENTS WITH RENAL COLIC 17 4.1 Renal colic 17 4.1.1 Pain relief 17 4.1.2 Prevention of recurrent renal colic 18 4.1.3 Recommendations for analgesia during renal colic 18 4.1.4 References 18 4.2 Management of sepsis in obstructed kidney 19 4.2.1 Decompression 19 4.2.2 Further measures 20 4.2.3 References 20 5. STONE RELIEF 21 5.1 Observation of ureteral stones 21 5.1.1 Stone-passage rates 21 5.2 Observation of kidney stones 21 5.3 Medical expulsive therapy (MET) 21 5.3.1 Choice of medical agent 22 5.3.1.1 Alpha-blockers 22 5.3.1.2 Calcium-channel blockers 22 5.3.1.2.1 Tamsulosin versus -

Case Report a Fragment of Foley Catheter Balloon As a Cause of Bladder Stone in Woman
Open Access Case report A fragment of Foley catheter balloon as a cause of Bladder stone in woman El Majdoub Aziz1,&, Mouad Amrani1, Khallouk Abdelhak1, Farih Moulay Hassan1 1Department of Urology, Hassan II Hospital University Center, Fez, Morocco &Corresponding author: El Majdoub Aziz, Department of Urology, Hassan II Hospital University Center, Fez, Morocco Key words: intravésical, foreign body, catheter balloon, recurrent urinary tract infections Received: 08/04/2015 - Accepted: 22/04/2015 - Published: 13/08/2015 Abstract Urinary bladder calculi are rarely seen in women and any history of previous pelvic surgery must, therefore, raise suspicion of an iatrogenic etiology. According to the literature, fewer than 2% of all bladder calculi occur in female subjects and, thus, their presence should provoke careful assessment of the etiology. We report one case of a fragment of Foley catheter balloon as a cause of Bladder stone in 28 years old woman. Weanalyzed the diagnosis, aspect and therapeutic management of this case which is the first described in literature to our knowledge. Pan African Medical Journal. 2015; 21:284 doi:10.11604/pamj.2015.21.284.6770 This article is available online at: http://www.panafrican-med-journal.com/content/article/21/284/full/ © El Majdoub Aziz et al. The Pan African Medical Journal - ISSN 1937-8688. This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/2.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Pan African Medical Journal – ISSN: 1937- 8688 (www.panafrican-med-journal.com) Published in partnership with the African Field Epidemiology Network (AFENET). -
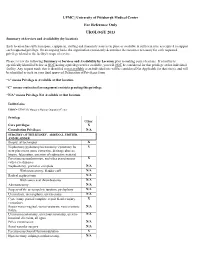
Summary of Services and Availability (By Location)
UPMC | University of Pittsburgh Medical Center For Reference Only UROLOGY 2013 Summary of Services and Availability (by location) Each location has sufficient space, equipment, staffing and financial resources in place or available in sufficient time as required to support each requested privilege. On an ongoing basis, the organization consistently determines the resources necessary for each requested privilege related to the facility's scope of service. Please review the following Summary of Services and Availability by Location prior to making your selections. If a facility is specifically identified below as NOT having a privilege/service available, you will NOT be considered for that privilege at that individual facility. Any request made that is identified as not available at an individual site will be considered Not Applicable for that site(s), and will be identified as such on your final approved Delineation of Privileges form. “x” means Privilege is Available at that location. “C” means contractual arrangement restricts granting this privilege. “N/A” means Privilege Not Available at that location. Facility Codes: UHOC= UPMC St. Margaret Harmar Outpatient Center Privilege UHOC Core privileges X Consultation Privileges N/A SURGERY OF THE KIDNEY, ADRENAL, URETER, AND BLADDER Biopsy, all techniques X Nephrotomy/pyelotomy/ureterotomy/ cystotomy for X stent placement, stone extraction, drainage abscess, biopsy, fulgeration, insertion of radioactive material Percutaneous nephroscopy, and other percutaneous X catheter techniques Nephrectomy, -

Surgical Management of Urolithiasis in Patients After Urinary Diversion
Surgical Management of Urolithiasis in Patients after Urinary Diversion Wen Zhong1, Bicheng Yang1, Fang He2, Liang Wang3, Sunil Swami4, Guohua Zeng1* 1 Department of Urology, the First Affiliated Hospital of Guangzhou Medical University, Guangdong Key Laboratory of Urology, Guangzhou, China, 2 Department of Gynecology and Obstetrics, the Third Affiliated Hospital of Guangzhou Medical University, Guangzhou, China, 3 Department of Biostatistics and Epidemiology, College of Public Health, East Tennessee State University, Johnson, Tennessee, United States of America, 4 Department of Epidemiology, College of Public Health and Health Professions, University of Florida, Gainesville, Florida, United States of America Abstract Objective: To present our experience in surgical management of urolithiasis in patients after urinary diversion. Patients and Methods: Twenty patients with urolithiasis after urinary diversion received intervention. Percutaneous nephrolithotomy, percutaneous based antegrade ureteroscopy with semi-rigid or flexible ureteroscope, transurethral reservoir lithotripsy, percutaneous pouch lithotripsy and open operation were performed in 8, 3, 2, 6, and 1 patients, respectively. The operative finding and complications were retrospectively collected and analyzed. Results: The mean stone size was 4.563.1 (range 1.5–11.2) cm. The mean operation time was 82.0611.5 (range 55–120) min. Eighteen patients were rendered stone free with a clearance of 90%. Complications occurred in 3 patients (15%). Two patients (10%) had postoperative fever greater than 38.5uC, and one patient (5%) suffered urine extravasations from percutaneous tract. Conclusions: The percutaneous based procedures, including percutaneous nephrolithotomy, antegrade ureteroscopy with semi-rigid ureteroscope or flexible ureteroscope from percutaneous tract, and percutaneous pouch lithotripsy, provides a direct and safe access to the target stones in patients after urinary diversion, and with high stone free rate and minor complications.