Henle's Ligament: a Comprehensive Review of Its Anatomy and Terminology Over Almost One and a Half Centuries
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

The Femoral Hernia: Some Necessary Additions
International Journal of Clinical Medicine, 2014, 5, 752-765 Published Online July 2014 in SciRes. http://www.scirp.org/journal/ijcm http://dx.doi.org/10.4236/ijcm.2014.513102 The Femoral Hernia: Some Necessary Additions Ljubomir S. Kovachev Department of General Surgery, Medical University, Pleven, Bulgaria Email: [email protected] Received 28 April 2014; revised 27 May 2014; accepted 26 June 2014 Copyright © 2014 by author and Scientific Research Publishing Inc. This work is licensed under the Creative Commons Attribution International License (CC BY). http://creativecommons.org/licenses/by/4.0/ Abstract Purpose: The anatomic region through which most inguinal hernias emerge is overcrowded by various anatomical structures with intricate relationships. This is reflected by the wide range of anatomic interpretations. Material and Methods: A prospective anatomic study of over 100 fresh cadavers and 47 patients operated on for femoral hernias. Results: It was found that the transver- salis fascia did not continue distally into the lymphatic lacuna. Medially this fascia did not reach the lacunar ligament, but was rather positioned above it forming laterally the vascular sheath. Here the fascia participates in the formation of a fossa, which varies in width and depth—the pre- peritoneal femoral fossa. The results did not confirm the presence of a femoral canal. The dis- tances were measured between the pubic tubercle and the medial margin of the femoral vein, and between the inguinal and the Cooper’s ligaments. The results clearly indicate that in women with femoral hernias these distances are much larger. Along the course of femoral hernia exploration we established the presence of three zones that are rigid and narrow. -

Sportsman's Hernia
International Surgery Journal Vagholkar K et al. Int Surg J. 2019 Jul;6(7):2659-2662 http://www.ijsurgery.com pISSN 2349-3305 | eISSN 2349-2902 DOI: http://dx.doi.org/10.18203/2349-2902.isj20192564 Review Article Sportsman’s hernia Ketan Vagholkar*, Shivangi Garima, Yash Kripalani, Shantanu Chandrashekhar, Suvarna Vagholkar Department of Surgery, D.Y. Patil University School of Medicine, Navi Mumbai, Maharashtra, India Received: 14 May 2019 Accepted: 30 May 2019 *Correspondence: Dr. Ketan Vagholkar, E-mail: [email protected] Copyright: © the author(s), publisher and licensee Medip Academy. This is an open-access article distributed under the terms of the Creative Commons Attribution Non-Commercial License, which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. ABSTRACT Sportsman’s hernia is a complex entity with injuries occurring at different levels in the groin region. Each damaged anatomical structure gives rise to a different set of symptoms and signs making the diagnosis difficult. The apprehension of a hernia is foremost in the mind of the surgeon. Absence of a hernia sac adds to the confusion. Hence awareness of this condition is essential for the general surgeon to avoid misdiagnosis. Keywords: Sportsman’s hernia, Gilmore's groin, Athletic pubalgia INTRODUCTION insert only anterior to the rectus muscle making it an area of potential weakness. The only structure protecting this Sportsman’s hernia also described as Gilmore’s groin is area is the transversalis fascia. The aponeurosis of an entity which is becoming increasingly common internal oblique and transversus abdominis fuse medially amongst athletes especially professional athletes such as to form the conjoint tendon before insertion into the footballers, hockey players etc.1,2 The diagnosis is pubic tubercle. -

Femoral Nerve Dimensions at the Inguinal Ligament and Inguinal Crease Levels: Implications for Femoral Nerve Block
Original article http://dx.doi.org/10.4322/jms.062413 Femoral nerve dimensions at the inguinal ligament and inguinal crease levels: implications for femoral nerve block OYEDUN, O. S.1*, RUKEWE, A.2 and FATIREGUN, A.3 1Gross Anatomy Lab, Department of Anatomy, Faculty of Basic Medical Sciences, University of Ibadan, +234 Ibadan, Oyo State, Nigéria 2Anaesthesia Unit, Accident and Emergency Department, University College Hospital, +234 Ibadan, Oyo State, Nigéria 3Department of Epidemiology and Medical Statistics, Faculty of Public Health, University of Ibadan, +234 Ibadan, Oyo State, Nigéria *E-mail: [email protected] Abstract Introduction: Femoral nerve block, when used solely or as a supplement to general anaesthesia, provides anaesthesia and analgesia to the anterior thigh. In spite of its established benefits, femoral nerve block is still underutilized in Nigeria. Our objective was to study the dimensions of femoral nerve at the level of the inguinal ligament and inguinal crease using a cadaveric model; no such data exists in Nigeria. Materials and Methods: Using 7 adult human cadavers (6 males and 1 female), the depth and thickness of the femoral nerve were measured at the levels of inguinal ligament and inguinal crease. The spatial relationship of femoral nerve to the surrounding structures was also observed. Result: The study showed a significantly wider thickness and shorter depth of the femoral nerve at the level of inguinal crease relative to inguinal ligament. Conclusion: We concluded that in centers where ultrasound and neurostimulation techniques for femoral nerve block in Nigerians are unavailable, the inguinal crease level where the femoral nerve is more superficial and wider in thickness would be the landmark of choice compared to the inguinal ligament level. -

Sportsmans Groin: the Inguinal Ligament and the Lloyd Technique
Rennie, WJ and Lloyd, DM. Sportsmans Groin: The Inguinal Ligament and the Lloyd Technique. Journal of the Belgian Society of Radiology. 2017; 101(S2): 16, pp. 1–4. DOI: https://doi.org/10.5334/jbr-btr.1404 OPINION ARTICLE Sportsmans Groin: The Inguinal Ligament and the Lloyd Technique WJ Rennie and DM Lloyd Groin pain is a catch all phrase used to define a common set of symptoms that affect many individuals. It is a common condition affecting sportsmen and women (1, 2) and is often referred to as the sportsman groin (SG). Multiple surgical operations have been developed to treat these symptoms yet no definitive imaging modalities exist to diagnose or predict prognosis. This article aims to discuss the anatomy of the groin, suggest a biomechanical pathophysiology and outline a logical surgical solution to treat the underlying pathology. A systematic clinical and imaging approach with inguinal ligament and pubic specific MRI assessment, can result in accurate selection for intervention. Close correlation with clinical examination and imaging in series is recommended to avoid misinterpretation of chronic changes in athletes. Keywords: Groin pain; Inguinal Ligament; MRI; Surgery; Lloyd release Introduction from SG is due to altered biomechanics, with specific pain Groin pain is a catch all phrase used to define a common symptoms that differ from those caused by inguinal or set of symptoms that affect many individuals. It is a com- femoral hernias. mon condition affecting sportsmen and women [1, 2] and is often referred to as the sportsman groin (SG). Multiple Anatomy of Sportsman’s Groin surgical operations have been developed to treat these The anatomical central structure in the groin is the pubic symptoms, yet no definitive imaging modalities exist to bone. -

Inguinofemoral Area
Inguinofemoral Area Inguinal Canal Anatomy of the Inguinal Canal in Infants and Children There are readily apparent differences between the inguinal canals of infants and adults. In infants, the canal is short (1 to 1.5 cm), and the internal and external rings are nearly superimposed upon one another. Scarpa's fascia is so well developed that the surgeon may mistake it for the aponeurosis of the external oblique muscle, resulting in treating a superficial ectopic testicle as an inguinal cryptorchidism. There also may be a layer of fat between the fascia and the aponeurosis. We remind surgeons of the statement of White that the external oblique fascia has not been reached as long as fat is encountered. In a newborn with an indirect inguinal hernia, there is nothing wrong with the posterior wall of the inguinal canal. Removal of the sac, therefore, is the only justifiable procedure. However, it is extremely difficult to estimate the weakness of the newborn's posterior inguinal wall by palpation. If a defect is suspected, a few interrupted permanent sutures might be used to perform the repair. Adult Anatomy of the Inguinal Canal The inguinal canal in the adult is an oblique rift in the lower part of the anterior abdominal wall. It measures approximately 4 cm in length. It is located 2 to 4 cm above the inguinal ligament, between the opening of the external (superficial) and internal (deep) inguinal rings. The boundaries of the inguinal canal are as follows: Anterior: The anterior boundary is the aponeurosis of the external oblique muscle and, more laterally, the internal oblique muscle. -

Describe the Anatomy of the Inguinal Canal. How May Direct and Indirect Hernias Be Differentiated Anatomically
Describe the anatomy of the inguinal canal. How may direct and indirect hernias be differentiated anatomically. How may they present clinically? Essentially, the function of the inguinal canal is for the passage of the spermatic cord from the scrotum to the abdominal cavity. It would be unreasonable to have a single opening through the abdominal wall, as contents of the abdomen would prolapse through it each time the intraabdominal pressure was raised. To prevent this, the route for passage must be sufficiently tight. This is achieved by passing through the inguinal canal, whose features allow the passage without prolapse under normal conditions. The inguinal canal is approximately 4 cm long and is directed obliquely inferomedially through the inferior part of the anterolateral abdominal wall. The canal lies parallel and 2-4 cm superior to the medial half of the inguinal ligament. This ligament extends from the anterior superior iliac spine to the pubic tubercle. It is the lower free edge of the external oblique aponeurosis. The main occupant of the inguinal canal is the spermatic cord in males and the round ligament of the uterus in females. They are functionally and developmentally distinct structures that happen to occur in the same location. The canal also transmits the blood and lymphatic vessels and the ilioinguinal nerve (L1 collateral) from the lumbar plexus forming within psoas major muscle. The inguinal canal has openings at either end – the deep and superficial inguinal rings. The deep (internal) inguinal ring is the entrance to the inguinal canal. It is the site of an outpouching of the transversalis fascia. -

Clinical Pelvic Anatomy
SECTION ONE • Fundamentals 1 Clinical pelvic anatomy Introduction 1 Anatomical points for obstetric analgesia 3 Obstetric anatomy 1 Gynaecological anatomy 5 The pelvic organs during pregnancy 1 Anatomy of the lower urinary tract 13 the necks of the femora tends to compress the pelvis Introduction from the sides, reducing the transverse diameters of this part of the pelvis (Fig. 1.1). At an intermediate level, opposite A thorough understanding of pelvic anatomy is essential for the third segment of the sacrum, the canal retains a circular clinical practice. Not only does it facilitate an understanding cross-section. With this picture in mind, the ‘average’ of the process of labour, it also allows an appreciation of diameters of the pelvis at brim, cavity, and outlet levels can the mechanisms of sexual function and reproduction, and be readily understood (Table 1.1). establishes a background to the understanding of gynae- The distortions from a circular cross-section, however, cological pathology. Congenital abnormalities are discussed are very modest. If, in circumstances of malnutrition or in Chapter 3. metabolic bone disease, the consolidation of bone is impaired, more gross distortion of the pelvic shape is liable to occur, and labour is likely to involve mechanical difficulty. Obstetric anatomy This is termed cephalopelvic disproportion. The changing cross-sectional shape of the true pelvis at different levels The bony pelvis – transverse oval at the brim and anteroposterior oval at the outlet – usually determines a fundamental feature of The girdle of bones formed by the sacrum and the two labour, i.e. that the ovoid fetal head enters the brim with its innominate bones has several important functions (Fig. -

Exploring Anatomy: the Human Abdomen
Exploring anatomy: the human abdomen An advanced look at the inguinal canal transcript Welcome to this video for exploring anatomy, the human abdomen. This video is going to outline the inguinal canal. So on the screen at the moment, we've got the anterior superior iliac spine and also the public bone. Here in the midline, we've got the pubic symphysis. And here, we can see the superior pubic ramus that has the public tubercle here. And here, we can see the pubic crest. This is the inferior pubic ramus. And here's the obturator foramen. So the first thing I'm going to draw out is the inguinal ligament. And the inguinal ligament forms the floor of the inguinal canal. So here we have the inguinal ligament-- the inguinal ligament. This forms the floor of the inguinal canal. It's the free edge of the external oblique muscle fibres, which I'm not going to draw on this diagram as they overcomplicate it. But you should be aware the external oblique muscle fibres run downwards and forwards. At the pubic tubercle, some fibres of the inguinal ligament reflect laterally and form the lacunar ligament. And some more of these fibres extend further laterally onto the pectineal line of the pubic bone. So here we're going to have the lacunar ligament, this lateral reflection of the inguinal ligament. Some fibres of the inguinal ligament also reflect superiorally and medially to blend with the muscles of the anterior and lateral abdominal wall. But I won't draw those in. -

Iliopectineal Ligament As an Important Landmark in Ilioinguinal Approach of the Anterior Acetabulum
International Journal of Anatomy and Research, Int J Anat Res 2019, Vol 7(3.3):6976-82. ISSN 2321-4287 Original Research Article DOI: https://dx.doi.org/10.16965/ijar.2019.274 ILIOPECTINEAL LIGAMENT AS AN IMPORTANT LANDMARK IN ILIOINGUINAL APPROACH OF THE ANTERIOR ACETABULUM: A CADAVERIC MORPHOLOGIC STUDY Ayman Ahmed Khanfour *1, Ashraf Ahmed Khanfour 2. *1 Anatomy department Faculty of Medicine, Alexandria University, Egypt. 2 Chairman of Orthopaedic surgery department Damanhour National Medical Institute Egypt. ABSTRACT Background: The iliopectineal ligament is the most stout anterior part of the iliopectineal membrane. It separates “lacuna musculorum” laterally from “lacuna vasorum” medially. This ligament is an important guide in the safe anterior approach to the acetabulum. Aim of the work: To study the detailed anatomy of the iliopectineal ligament demonstrating its importance as a surgical landmark in the anterior approach to the acetabulum. Material and methods: The material of this work included eight adult formalin preserved cadavers. Dissection of the groin was done for each cadaver in supine position with exposure of the inguinal ligament. The iliopectineal ligament and the three surgical windows in the anterior approach to the acetabulum were revealed. Results: Results described the detailed morphological anatomy of the iliopectineal ligament as regard its thickness, attachments and variations in its thickness. The study also revealed important anatomical measurements in relation to the inguinal ligament. The distance between the anterior superior iliac spine (ASIS) to the pubic tubercle ranged from 6.7 to 10.1 cm with a mean value of 8.31±1.3. The distance between the anterior superior iliac spine (ASIS) to the blending point of the iliopectineal ligament to the inguinal ligament ranged from 1.55 to 1.92 cm with a mean value of 1.78±0.15. -

Anterior Abdominal Wall
Abdominal wall Borders of the Abdomen • Abdomen is the region of the trunk that lies between the diaphragm above and the inlet of the pelvis below • Borders Superior: Costal cartilages 7-12. Xiphoid process: • Inferior: Pubic bone and iliac crest: Level of L4. • Umbilicus: Level of IV disc L3-L4 Abdominal Quadrants Formed by two intersecting lines: Vertical & Horizontal Intersect at umbilicus. Quadrants: Upper left. Upper right. Lower left. Lower right Abdominal Regions Divided into 9 regions by two pairs of planes: 1- Vertical Planes: -Left and right lateral planes - Midclavicular planes -passes through the midpoint between the ant.sup.iliac spine and symphysis pupis 2- Horizontal Planes: -Subcostal plane - at level of L3 vertebra -Joins the lower end of costal cartilage on each side -Intertubercular plane: -- At the level of L5 vertebra - Through tubercles of iliac crests. Abdominal wall divided into:- Anterior abdominal wall Posterior abdominal wall What are the Layers of Anterior Skin Abdominal Wall Superficial Fascia - Above the umbilicus one layer - Below the umbilicus two layers . Camper's fascia - fatty superficial layer. Scarp's fascia - deep membranous layer. Deep fascia : . Thin layer of C.T covering the muscle may absent Muscular layer . External oblique muscle . Internal oblique muscle . Transverse abdominal muscle . Rectus abdominis Transversalis fascia Extraperitoneal fascia Parietal Peritoneum Superficial Fascia . Camper's fascia - fatty layer= dartos muscle in male . Scarpa's fascia - membranous layer. Attachment of scarpa’s fascia= membranous fascia INF: Fascia lata Sides: Pubic arch Post: Perineal body - Membranous layer in scrotum referred to as colle’s fascia - Rupture of penile urethra lead to extravasations of urine into(scrotum, perineum, penis &abdomen) Muscles . -

ENDOSCOPIC ANATOMY of the GROIN; IMPLICATION for TRANSABDMOMINAL PREPERITOTONEAL HERNIORRHAPHY Saidi H
Review Anatomy Journal of Africa 1 (1): 2-10 (2012) ENDOSCOPIC ANATOMY OF THE GROIN; IMPLICATION FOR TRANSABDMOMINAL PREPERITOTONEAL HERNIORRHAPHY Saidi H. BSc, MBChB, MMed, FACS Department of Human Anatomy, University of Nairobi Correspondence: Prof. Saidi Hassan, Department of Human Anatomy, University of Nairobi. P.O. Box 30197 00100 Nairobi Email: [email protected] SUMMARY Hernia surgery is in many ways the quintessential case for demonstrating anatomy in action. Laparoscopic hernia surgery has a more recent history compared to open surgery. The demand for the procedure is increasing. The indications for laparoscopic herniorrhaphy include bilateral disease, recurrence following anterior repairs and patient preference. Anatomy of the lower anterolateral abdominal wall appreciated from a posterior profile compounds the challenge of a steep learning curve for the procedure. The iliopubic tract and Cooper’s ligaments, less obvious to anterior surgeons, are important sites for mesh fixation for laparoscopic surgeons. Their neural and vascular relations continue to receive plenty of mention in hernia literature as explanations for troublesome procedure-related morbidities. The one ‘rectangle’ (trapezoid of disaster), one ‘circle’ (of death) and two ‘triangles’ (of doom, of pain) geometric concepts denote application of anatomy in mapping the danger areas of the groin where dissection and staples for fixation should be minimized. INTRODUCTION costs and learning curve. However, patients who Groin hernia surgery is common globally with desire faster return to work and cosmetic around twenty million hernias repaired wounds are demanding the procedure from local worldwide annually (Heuvel et al., 2011). surgeons. This review reconstructs the pertinent Although open anterior approaches suffice for anatomy as a prerequisite and reminder for safe most unilateral hernias, the advantages of Transabdominal Preperitoneal (TAPPP) repair of shorter convalescence, lower pain scores, groin hernia. -
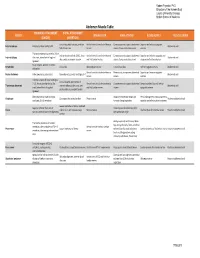
Abdomen Muscle Table PROXIMAL ATTACHMENT DISTAL ATTACHMENT MUSCLE INNERVATION MAIN ACTIONS BLOOD SUPPLY MUSCLE GROUP (ORIGIN) (INSERTION)
Robert Frysztak, PhD. Structure of the Human Body Loyola University Chicago Stritch School of Medicine Abdomen Muscle Table PROXIMAL ATTACHMENT DISTAL ATTACHMENT MUSCLE INNERVATION MAIN ACTIONS BLOOD SUPPLY MUSCLE GROUP (ORIGIN) (INSERTION) Linea alba, pubic tubercle, anterior Ventral rami of six inferior thoracic Compresses and supports abdominal Superior and inferior epigastric External oblique External surfaces of ribs 5–12 Abdominal wall half of iliac crest nerves viscera, flexes and rotates trunk arteries Thoracolumbar fascia, anterior 2/3 of Inferior borders of ribs 10–12, linea Ventral rami of six inferior thoracic Compresses and supports abdominal Superior and inferior epigastric and Internal oblique iliac crest, lateral half of inguinal Abdominal wall alba, pubis via conjoint tendon and first lumbar nerves viscera, flexes and rotates trunk deep circumflex iliac arteries ligament Body of pubis, anterior to rectus Pyramidalis Linea alba Iliohypogastric nerve Tenses linea alba Inferior epigastric artery Abdominal wall abdominis Ventral rami of six inferior thoracic Flexes trunk, compresses abdominal Superior and interior epigastric Rectus abdominis Pubic symphysis, pubic crest Xiphoid process, costal cartilages 5–7 Abdominal wall nerves viscera arteries Internal surfaces of costal cartilages Linea alba with aponeurosis of 7–12, thoracolumbar fascia, iliac Ventral rami of six inferior thoracic Compresses and supports abdominal Deep circumflex iliac and inferior Transversus abdominis internal oblique, pubic crest, and Abdominal wall