Clinical Practice Guidelines for Antimicrobial Prophylaxis in Surgery
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Medical Review(S) Clinical Review
CENTER FOR DRUG EVALUATION AND RESEARCH APPLICATION NUMBER: 200327 MEDICAL REVIEW(S) CLINICAL REVIEW Application Type NDA Application Number(s) 200327 Priority or Standard Standard Submit Date(s) December 29, 2009 Received Date(s) December 30, 2009 PDUFA Goal Date October 30, 2010 Division / Office Division of Anti-Infective and Ophthalmology Products Office of Antimicrobial Products Reviewer Name(s) Ariel Ramirez Porcalla, MD, MPH Neil Rellosa, MD Review Completion October 29, 2010 Date Established Name Ceftaroline fosamil for injection (Proposed) Trade Name Teflaro Therapeutic Class Cephalosporin; ß-lactams Applicant Cerexa, Inc. Forest Laboratories, Inc. Formulation(s) 400 mg/vial and 600 mg/vial Intravenous Dosing Regimen 600 mg every 12 hours by IV infusion Indication(s) Acute Bacterial Skin and Skin Structure Infection (ABSSSI); Community-acquired Bacterial Pneumonia (CABP) Intended Population(s) Adults ≥ 18 years of age Template Version: March 6, 2009 Reference ID: 2857265 Clinical Review Ariel Ramirez Porcalla, MD, MPH Neil Rellosa, MD NDA 200327: Teflaro (ceftaroline fosamil) Table of Contents 1 RECOMMENDATIONS/RISK BENEFIT ASSESSMENT ......................................... 9 1.1 Recommendation on Regulatory Action ........................................................... 10 1.2 Risk Benefit Assessment.................................................................................. 10 1.3 Recommendations for Postmarketing Risk Evaluation and Mitigation Strategies ........................................................................................................................ -

Use of Ceftaroline Fosamil in Children: Review of Current Knowledge and Its Application
Infect Dis Ther (2017) 6:57–67 DOI 10.1007/s40121-016-0144-8 REVIEW Use of Ceftaroline Fosamil in Children: Review of Current Knowledge and its Application Juwon Yim . Leah M. Molloy . Jason G. Newland Received: November 10, 2016 / Published online: December 30, 2016 Ó The Author(s) 2016. This article is published with open access at Springerlink.com ABSTRACT infections, CABP caused by penicillin- and ceftriaxone-resistant S. pneumoniae and Ceftaroline is a novel cephalosporin recently resistant Gram-positive infections that fail approved in children for treatment of acute first-line antimicrobial agents. However, bacterial skin and soft tissue infections and limited data are available on tolerability in community-acquired bacterial pneumonia neonates and infants younger than 2 months (CABP) caused by methicillin-resistant of age, and on pharmacokinetic characteristics Staphylococcus aureus, Streptococcus pneumoniae in children with chronic medical conditions and other susceptible bacteria. With a favorable and those with invasive, complicated tolerability profile and efficacy proven in infections. In this review, the microbiological pediatric patients and excellent in vitro profile of ceftaroline, its mechanism of action, activity against resistant Gram-positive and and pharmacokinetic profile will be presented. Gram-negative bacteria, ceftaroline may serve Additionally, clinical evidence for use in as a therapeutic option for polymicrobial pediatric patients and proposed place in therapy is discussed. Enhanced content To view enhanced content for this article go to http://www.medengine.com/Redeem/ 1F47F0601BB3F2DD. Keywords: Antibiotic resistance; Ceftaroline J. Yim (&) fosamil; Children; Methicillin-resistant St. John Hospital and Medical Center, Detroit, MI, Staphylococcus aureus; Streptococcus pneumoniae USA e-mail: [email protected] L. -

Utility of the Digital Rectal Examination in the Emergency Department: a Review
The Journal of Emergency Medicine, Vol. 43, No. 6, pp. 1196–1204, 2012 Published by Elsevier Inc. Printed in the USA 0736-4679/$ - see front matter http://dx.doi.org/10.1016/j.jemermed.2012.06.015 Clinical Reviews UTILITY OF THE DIGITAL RECTAL EXAMINATION IN THE EMERGENCY DEPARTMENT: A REVIEW Chad Kessler, MD, MHPE*† and Stephen J. Bauer, MD† *Department of Emergency Medicine, Jesse Brown VA Medical Center and †University of Illinois-Chicago College of Medicine, Chicago, Illinois Reprint Address: Chad Kessler, MD, MHPE, Department of Emergency Medicine, Jesse Brown Veterans Hospital, 820 S Damen Ave., M/C 111, Chicago, IL 60612 , Abstract—Background: The digital rectal examination abdominal pain and acute appendicitis. Stool obtained by (DRE) has been reflexively performed to evaluate common DRE doesn’t seem to increase the false-positive rate of chief complaints in the Emergency Department without FOBTs, and the DRE correlated moderately well with anal knowing its true utility in diagnosis. Objective: Medical lit- manometric measurements in determining anal sphincter erature databases were searched for the most relevant arti- tone. Published by Elsevier Inc. cles pertaining to: the utility of the DRE in evaluating abdominal pain and acute appendicitis, the false-positive , Keywords—digital rectal; utility; review; Emergency rate of fecal occult blood tests (FOBT) from stool obtained Department; evidence-based medicine by DRE or spontaneous passage, and the correlation be- tween DRE and anal manometry in determining anal tone. Discussion: Sixteen articles met our inclusion criteria; there INTRODUCTION were two for abdominal pain, five for appendicitis, six for anal tone, and three for fecal occult blood. -

The Differences Between ICD-9 and ICD-10
Preparing for the ICD-10 Code Set: Fact Sheet 2 October 1, 2015 Compliance Date Get the Facts to be Compliant Alert: The new ICD-10 compliance date is October 1, 2015. The Differences Between ICD-9 and ICD-10 This is the second fact sheet in a series and is focused on the differences between the ICD-9 and ICD-10 code sets. Collectively, the fact sheets will provide information, guidance, and checklists to assist you with understanding what you need to do to implement the ICD-10 code set. The ICD-10 code sets are not a simple update of the ICD-9 code set. The ICD-10 code sets have fundamental changes in structure and concepts that make them very different from ICD-9. Because of these differences, it is important to develop a preliminary understanding of the changes from ICD-9 to ICD-10. This basic understanding of the differences will then identify more detailed training that will be needed to appropriately use the ICD-10 code sets. In addition, seeing the differences between the code sets will raise awareness of the complexities of converting to the ICD-10 codes. Overall Comparisons of ICD-9 to ICD-10 Issues today with the ICD-9 diagnosis and procedure code sets are addressed in ICD-10. One concern today with ICD-9 is the lack of specificity of the information conveyed in the codes. For example, if a patient is seen for treatment of a burn on the right arm, the ICD-9 diagnosis code does not distinguish that the burn is on the right arm. -

Approved Livestock Drug Registrations
Livestock Drug Labels‐Approved and Provisional Status Firm: Product Name, Brand or Trademark Product Category Provisional ADEPTUS NUTRITION INC NIMBLE MEGA NUTRIENT (S&E RECEIVED) Physiological (Structure/Function) Provisional ADEPTUS NUTRITION INC NIMBLE ULTRA (S & E Received) Physiological (Structure/Function) Provisional ADEPTUS NUTRITION INC NIMBLE SUPREME (S & E Received) Physiological (Structure/Function) Approved ADEPTUS NUTRITION INC ADEPTUS WOUND AND SKIN SPRAY Topical Approved AFS DISTRIBUTING DURASOLE Topical Approved AGRI LABORATORIES LTD FERRRODEX 100 Injectable Approved AGRI LABORATORIES LTD VITAMIN E‐300 Injectable Approved AGRI LABORATORIES LTD PROPYLENE GLYCOL Physiological (Structure/Function) Approved AGRI LABORATORIES LTD IODINE WOUND SPRAY Topical Approved AGRI LABORATORIES LTD AGRI‐MECTIN (IVERMECTIN) INJECTION FOR CATTLE AND SWINE (RD) Restricted Drug‐/‐Wormer Approved AGRI LABORATORIES LTD AGRI‐MECTIN (IVERMECTIN) POUR‐ON FOR CATTLE (RD) Restricted Drug‐/‐Wormer Approved AGRI LABORATORIES LTD DEXTROSE 50% Injectable Approved AGRI LABORATORIES LTD PROHIBIT (LEVAMISOL HYDROCHLORIDE) SOLUBLE DRENCH POWDER (RD) Restricted Drug‐/‐Wormer Approved AGRI LABORATORIES LTD KAO‐PEC ANTI‐DIARRHEAL LIQUID Physiological (Structure/Function) Approved AGRI LABORATORIES LTD AGRIMYCIN 200 (OXYTETRACYCLINE) (CA RX RD) Restricted Drug‐/‐Injectable Approved AGRI LABORATORIES LTD VITAMIN E‐AD 300 INJECTABLE TOCOPHEROL WITH A+D Injectable Approved AGRI LABORATORIES LTD VITAMIN A D INJECTION Injectable Approved AGRI LABORATORIES LTD FORTIFIED -
28912 Oxoid FDA Cartridge Tables:1
* Adapted in part from CLSI document M100-S23 (M02-A11) : “Disc diffusion supplemental tablesʼʼ Performance standards for antimicrobial susceptibility testing. The complete standard may be obtained from the Clinical and Laboratory Standards Institute, 940 West Valley Road, Suite 1400, Wayne, PA 19807. Test Cultures (zone diameters in mm) Antimicrobial Agent Disc Code Potency Resistant Intermediate Susceptible Amikacin AK 30 μg EnterobacteriaceaeK, P. aeruginosa, Acinetobacter spp., and Staphylococcus spp. ≤14 15-16 ≥17 Amoxycillin - Clavulanic Acid AMC 20/10 μg EnterobacteriaceaeE ≤13 14-17 ≥18 Staphylococcus spp.A,Q ≤19 — ≥20 Haemophilus spp.A,Y ≤19 — ≥20 AmpicillinC,n AMP 10 μg EnterobacteriaceaeE and Vibrio choleraef ≤13 14-16 ≥17 Staphylococcus spp.A,Q ≤28 — ≥29 Enterococcus spp.A,V,W,k,m ≤16 — ≥17 Haemophilus spp.Y ≤18 19-21 ≥22 Streptococcus spp. ß-Hemolytic GroupA,d — — ≥24 Ampicillin – Sulbactam SAM 10/10 μg EnterobacteriaceaeE, Acinetobacter spp., and Staphylococcus spp. ≤11 12-14 ≥15 Haemophilus spp.A,Y ≤19 — ≥20 Azithromycin AZM 15 μg Staphylococcus spp., Streptococcus spp Viridans Groupn, ß-Hemolytic Group, and S. pneumoniae) ≤13 14-17 ≥18 Neisseria meningitidisA,i — — ≥20 Haemophilus spp.A — — ≥12 Aztreonam ATM 30 μg EnterobacteriaceaeE ≤17 18-20 ≤21 P. aeruginosa ≤15 16-21 ≥22 Haemophilus spp.A — — ≥26 CAR 100 μg Carbenicillin Enterobacteriaceae ≤19 20-22 ≥23 Pseudomonas aeruginosaP ≤13 14-16 ≥17 CEC 30 μg Cefaclor Enterobacteriaceae and Staphylococcus spp. ≤14 15-17 ≥18 Haemophilus spp.Y ≤16 17-19 ≥20 MA 30 μg Cefamandole EnterobacteriaceaeD,E and Staphylococcus spp. ≤14 15-17 ≥18 CefazolinG KZ 30 μg Staphylococcus spp. -

12. What's Really New in Antibiotic Therapy Print
What’s really new in antibiotic therapy? Martin J. Hug Freiburg University Medical Center EAHP Academy Seminars 20-21 September 2019 Newsweek, May 24-31 2019 Disclosures There are no conflicts of interest to declare EAHP Academy Seminars 20-21 September 2019 Antiinfectives and Resistance EAHP Academy Seminars 20-21 September 2019 Resistance of Klebsiella pneumoniae to Pip.-Taz. olates) EAHP Academy Seminars 20-21 September 2019 https://resistancemap.cddep.org/AntibioticResistance.php Multiresistant Pseudomonas Aeruginosa Combined resistance against at least three different types of antibiotics, 2017 EAHP Academy Seminars 20-21 September 2019 https://atlas.ecdc.europa.eu/public/index.aspx Distribution of ESBL producing Enterobacteriaceae EAHP Academy Seminars 20-21 September 2019 Rossolini GM. Global threat of Gram-negative antimicrobial resistance. 27th ECCMID, Vienna, 2017, IS07 Priority Pathogens Defined by the World Health Organisation Critical Priority High Priority Medium Priority Acinetobacter baumanii Enterococcus faecium Streptococcus pneumoniae carbapenem-resistant vancomycin-resistant penicillin-non-susceptible Pseudomonas aeruginosa Helicobacter pylori Haemophilus influenzae carbapenem-resistant clarithromycin-resistant ampicillin-resistant Enterobacteriaceae Salmonella species Shigella species carbapenem-resistant fluoroquinolone-resistant fluoroquinolone-resistant Staphylococcus aureus vancomycin or methicillin -resistant Campylobacter species fluoroquinolone-resistant Neisseria gonorrhoae 3rd gen. cephalosporin-resistant -

Severe Sepsis and Septic Shock Antibiotic Guide
Stanford Health Issue Date: 05/2017 Stanford Antimicrobial Safety and Sustainability Program Severe Sepsis and Septic Shock Antibiotic Guide Table 1: Antibiotic selection options for healthcare associated and/or immunocompromised patients • Healthcare associated: intravenous therapy, wound care, or intravenous chemotherapy within the prior 30 days, residence in a nursing home or other long-term care facility, hospitalization in an acute care hospital for two or more days within the prior 90 days, attendance at a hospital or hemodialysis clinic within the prior 30 days • Immunocompromised: Receiving chemotherapy, known systemic cancer not in remission, ANC <500, severe cell-mediated immune deficiency Table 2: Antibiotic selection options for community acquired, immunocompetent patients Table 3: Antibiotic selection options for patients with simple sepsis, community acquired, immunocompetent patients requiring hospitalization. Risk Factors for Select Organisms P. aeruginosa MRSA Invasive Candidiasis VRE (and other resistant GNR) Community acquired: • Known colonization with MDROs • Central venous catheter • Liver transplant • Prior IV antibiotics within 90 day • Recent MRSA infection • Broad-spectrum antibiotics • Known colonization • Known colonization with MDROs • Known MRSA colonization • + 1 of the following risk factors: • Prolonged broad antibacterial • Skin & Skin Structure and/or IV access site: ♦ Parenteral nutrition therapy Hospital acquired: ♦ Purulence ♦ Dialysis • Prolonged profound • Prior IV antibiotics within 90 days ♦ Abscess -

Tube Feeding Using the Bolus Method | Memorial Sloan Kettering Cancer Center
PATIENT & CAREGIVER EDUCATION Tube Feeding Using the Bolus Method This information will help teach you how to use the bolus method to feed yourself and take your medications through your percutaneous endoscopic gastrostomy (PEG), gastrostomy tube (GT), or nasogastric tube (NGT). About Tube Feeding Tube feeding is when you get your nutrients through a feeding tube if you aren’t able to get enough through eating and drinking, or if you can’t swallow safely. Nutrients provide energy and help you heal. The bolus method is a type of feeding where a syringe is used to send formula through your feeding tube. The syringe you’ll use is called a catheter syringe. A catheter syringe doesn’t have a needle. It has a hole with a plunger in it. You draw up formula through the hole in the syringe then push the formula into your feeding tube with the plunger. A bolus refers to 1 “meal” of formula. You may have a feeding tube with a legacy connector or an ENFit connector. In this resource, we’ll show images of both types of connectors. For more information about your feeding tube, including how to manage side effects, read Tube Feeding Troubleshooting Guide. Tube Feeding Using the Bolus Method 1/11 Tube Feeding Guidelines Formula: __________ Total cans per day: ____________________ (8 ounces each) Calories per day: __________ You can choose the times of your feedings, as long as you reach your daily nutritional goals. Write in the times you prefer or your doctor, advanced practice provider (APP), or clinical dietitian nutritionist recommends. -
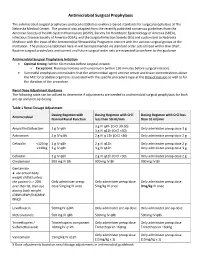
Antimicrobial Surgical Prophylaxis
Antimicrobial Surgical Prophylaxis The antimicrobial surgical prophylaxis protocol establishes evidence-based standards for surgical prophylaxis at The Nebraska Medical Center. The protocol was adapted from the recently published consensus guidelines from the American Society of Health-System Pharmacists (ASHP), Society for Healthcare Epidemiology of America (SHEA), Infectious Disease Society of America (IDSA), and the Surgical Infection Society (SIS) and customized to Nebraska Medicine with the input of the Antimicrobial Stewardship Program in concert with the various surgical groups at the institution. The protocol established here-in will be implemented via standard order sets utilized within One Chart. Routine surgical prophylaxis and current and future surgical order sets are expected to conform to this guidance. Antimicrobial Surgical Prophylaxis Initiation Optimal timing: Within 60 minutes before surgical incision o Exceptions: Fluoroquinolones and vancomycin (within 120 minutes before surgical incision) Successful prophylaxis necessitates that the antimicrobial agent achieve serum and tissue concentrations above the MIC for probable organisms associated with the specific procedure type at the time of incision as well as for the duration of the procedure. Renal Dose Adjustment Guidance The following table can be utilized to determine if adjustments are needed to antimicrobial surgical prophylaxis for both pre-op and post-op dosing. Table 1 Renal Dosage Adjustment Dosing Regimen with Dosing Regimen with CrCl Dosing Regimen with -

Product Monograph
Product Monograph PrORB-CEFUROXIME Cefuroxime Axetil Tablets, USP 250 mg and 500 mg cefuroxime/tablet Antibiotic Orbus Pharma Inc. Date of Preparation: February 25, 2009 20 Konrad Crescent Markham, Ontario Control #: 117041 L3R8T4 1 Product Monograph PrORB-CEFUROXIME Cefuroxime Axetil Tablets, USP 250 mg and 500 mg cefuroxime/tablet Antibiotic Actions and Clinical Pharmacology Cefuroxime axetil is an orally active prodrug of cefuroxime. After oral administration, cefuroxime axetil is absorbed from the gastrointestinal tract and rapidly hydrolyzed by nonspecific esterases in the intestinal mucosa and blood to release cefuroxime into the blood stream. Conversion to cefuroxime, the microbiologically active form, occurs rapidly. The inherent properties of cefuroxime are unaltered after its administration as cefuroxime axetil. Cefuroxime exerts its bactericidal effect by binding to an enzyme or enzymes referred to as penicillin-binding proteins (PBPs) involved in bacterial cell wall synthesis. This binding results in inhibition of bacterial cell wall synthesis and subsequent cell death. Specifically, cefuroxime shows high affinity for PBP 3, a primary target for cefuroxime in gram- negative organisms such as E. coli. Comparative Bioavailability Studies A two-way crossover, randomized, blinded, single-dose bioequivalence study was performed on 22 normal, healthy, non-smoking male subjects under fasting conditions. The rate and extent of absorption of cefuroxime axetil was measured and compared following a single oral dose (1 x 500 mg tablet) -

The Efficacy of Cefmetazole Against Pyelonephritis Caused by Extended
International Journal of Infectious Diseases 17 (2013) e159–e163 Contents lists available at SciVerse ScienceDirect International Journal of Infectious Diseases jou rnal homepage: www.elsevier.com/locate/ijid The efficacy of cefmetazole against pyelonephritis caused by extended-spectrum beta-lactamase-producing Enterobacteriaceae a, b c d a,e Asako Doi *, Toshihiko Shimada , Sohei Harada , Kentaro Iwata , Toru Kamiya a Department of Infectious Diseases, Rakuwakai Otowa Hospital, Otowachinji-cho 2, Yamashina-ku, Kyoto, Japan b Department of General Internal Medicine, Nara City Hospital, Nara, Japan c Department of Microbiology and Infectious Diseases, Toho University School of Medicine, Ota-ku, Tokyo, Japan d Division of Infectious Diseases, Kobe University Hospital, Chuo-ku, Kobe, Hyogo, Japan e Department of General Internal Medicine, Rakuwakai Otowa Hospital, Otowachinji-cho 2, Yamashina-ku, Kyoto, Japan A R T I C L E I N F O S U M M A R Y Article history: Objectives: Urinary tract infections (UTIs) caused by extended-spectrum beta-lactamase (ESBL)- Received 3 April 2012 producing Enterobacteriaceae are on the increase. Although cefmetazole is stable in vitro against the Accepted 26 September 2012 hydrolyzing activity of ESBLs, no clinical study has ever evaluated its role in infections caused by these Corresponding Editor: William Cameron, organisms. We therefore evaluated the efficacy of cefmetazole compared to carbapenems against Ottawa, Canada pyelonephritis caused by ESBL-producing Enterobacteriaceae. Methods: A retrospective chart review was conducted at a tertiary care hospital from August 2008 to July Keywords: 2010. Chart reviews were done for patients with ESBL-producing organisms in urine identified in the Extended-spectrum beta-lactamase (ESBL) microbiology database.