Talus Morphology and Its Functional Implications on the Ankle Joint
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Anterograde Fixation of Inverted Oblique Medial Malleolus Fractures
DOI: https://doi.org/10.30795/jfootankle.2021.v15.1230 Case Report Anterograde fixation of inverted oblique medial malleolus fractures: case report Sávio Manhães Chami1 , Thiago Lopes Lima1 , Alexandre Bustamante Pallottino1 , Breno Jorge Scorza1 , José Sérgio Franco 1,2, Rogério Carneiro Bitar3 1. Casa de Saúde São José, Rio de Janeiro, RJ, Brazil. 2. Universidade Federal do Rio de Janeiro, Rio de Janeiro, RJ, Brazil. 3.Hospital das Clínicas, Faculdade de Medicina de Ribeirão Preto, Ribeirão Preto, SP, Brazil. Abstract Fractures of the medial malleolus are common, with avulsion being the main trauma mechanism. In simple transverse fractures, re- trograde fixation with interfragmentary screws is the most common means of achieving anatomical reduction and absolute stability. However, greater attention must be paid in cases of inverted oblique fractures, which make traditional fixation difficult. We report a case in which anatomical reduction and stabilization were achieved using a reduction clamp and two headless compression screws placed anteriorly, resulting in a mechanically stable, safe and effective repair. Level of Evidence V, Therapeutic Studies; Expert Opinion. Keywords: Ankle Injuries/surgery; Bone screws; Fracture fixation, internal/methods; Range of motion, articular; Treatment outcome. Introduction In the medial malleolus, variation in the direction of the fracture line is responsible for different bone injury presen- Different mechanisms of trauma to the ankle result in diffe- tations, as well as the involvement of the deltoid ligament, (1-2) rent fracture patterns and associated ligament injuries . The especially its deep portion(6). precise identification of these injuries, as well as defining the Several techniques have been described for the internal fi- direction of the fracture line, is essential for the best surgical xation of medial malleolus fractures, the most common being planning and treatment. -

Volume 15, Issue 1, January-April
Volume 15, Issue 1, January-April Osteochondral lesions of the talus in adults J. Batista, G. Joannas, L. Casola, L. Logioco, G. Arrondo 1A Traumatic lesion with isolated cartilage injury (flap) Tx: arthroscopy, curettage, and microfractures. 1B Traumatic lesion (cartilage and subchondral bone injury) 1B.1 Lesion <10mm in diameter and <5mm of depth (superficial lesion) Tx: arthroscopy, curettage, and microfractures. 1B.2 Lesion >10mm in diameter and >5mm in depth Tx: fragment fixation with osteosynthesis, open surgery, osteochondral graft, or mosaicoplasty. 2A Non-traumatic isolated bone injury, subchondral cyst. Tx: retrograde drilling. 2B Non-traumatic open subchondral bone cyst with articular connection (progression of type 2A). 2B.1 Lesion measuring <10mm in diameter and <5mm in depth (superficial lesion). Tx: arthroscopy, curettage, and microfractures. 2B.2 Lesion measuring >10mm in diameter and >5mm in depth. Tx: open surgery, osteochondral graft, or mosaicoplasty. 3 Type 1 or 2 lesions associated with lateral instability of the ankle Tx: ligament repair. 4 With limb deformities 4A Types 1 or 2 lesions with hindfoot deformity = varus or valgus calcaneus Tx: varus or valgus calcaneal osteotomy. 4B Type 1 or 2 lesion with supramalleolar deformity of distal tibia (varus or valgus) Tx: varus or valgus supramalleolar osteotomy. Tx: treatment. Volume 15, Issue 1, January-April The Journal of the Foot & Ankle (eISSN 2675-2980) is published quarterly in April, August, and December, with the purpose of disseminating papers on themes of Foot and Ankle Medicine and Surgery and related areas. The Journal offers free and open access to your content on our website. All papers are already published with active DOIs. -

Ideal Medial Malleolar Screw Length Based on the Tibial Epiphyseal Scar Location in Weight Bearing CT’S Collin G
Ideal Medial Malleolar Screw Length Based on the Tibial Epiphyseal Scar Location in Weight Bearing CT’s Collin G. Messerly DPM, Keegan A. Duelfer DPM, Troy J. Boffeli DPM, FACFAS, Tyler K. Sorensen, DPM Regions Hospital / HealthPartners Institute for Education and Research - Saint Paul, MN Figure 1. Zone of Dense Bone in Medial Malleolar ORIF Figure 4. Measuring Distal – Most 5% to Medial Malleolus Table 2. Distance Between Epiphyseal Scar & Distal – Most 5% of RESULTS STATEMENT OF PURPOSE The epiphyseal scar is located in the distal The medial malleolus to distal – most 5% mark Tibia 97 WB ankle CT scans evaluated in uninjured ankles Medial malleolar fractures are one of the most common fracture types metaphysis of the tibia, and can oftentimes be was measured on the coronal WB CT slice with Measurement of interest Male: Mean ± SD Female: Mean ± SD (mm) In males < 60 years old there was a 12.75 mm zone of increased bone the widest medial malleolus. Screw threads observed in the ankle joint and have been long fixated with two screws; easily visualized on X-ray and CT scan (red line). (mm) density, as compared to 13.66 mm in those ≥ 60 which was not statistically The distal – most 5% of the tibia (distal to the beyond this point will purchase less dense bone however, the bone density of the distal tibia has potential for poor screw significant. purchase due to compromised bone density. This is especially true in elderly black line) contains dense bone with marked in the medullary canal with potential to not have Epiphyseal Scar to Medial Malleolus 12.75 ± 2.91 9.39 ± 2.38 In females < 60 years old there was 9.39 mm zone of increased bone populations with osteoporotic bone. -

PTA019: Anatomy & Physiology Manual
Anatomy & Physiology Full content for both the Level 2 Certificate in Fitness Instructing & Level 3 Certificate in Personal Training LEARN - INSPIRE - SUCCEED Contents Anatomy & Physiology for Exercise ………………………………………. Page 3 • The Musculoskeletal System ………………………………………. Page 3 • Energy Systems ………………………………………. Page 76 • The Cardiorespiratory System ………………………………………. Page 86 • The Neuroendocrine System ………………………………………. Page 105 Performance Training Academy 2 Chapter Two: Anatomy and Physiology Introduction This chapter is to be broken down into many sub-chapters, giving you a great reference point for your study as well as when needed once you are actively working as a Fitness Professional. It is of upmost importance that you continue to recap and learn further about the bio-mechanics and workings of the human body. A great fitness professional won’t just know how to programme for an individual, but will know how to help improve weaknesses and imbalances within the body, knowledge of Anatomy and Physiology is key to be able to do this. The Musculoskeletal System Unit Objectives Our first objective is to understand the biomechanics of the human body. We can do this by learning about the skeletal system, and then how the muscles are layered upon the skeleton. By the end of this unit we want you to have a good subject knowledge of the following: • The main bones of the skeleton • Joint types and joint actions • How exercise can create a strong and healthy skeletal system • The main muscles of the body • Muscle contractions and fibre types We will start by going through the skeletal system before bringing the muscles into the equation. This will allow you to build up your knowledge of bones and terminology before recapping them again by layering the muscles across specific joints. -

Skier Tibia (Leg) Fractures
Skier Tibia (Leg) Fractures In years past, the prototypical ski fracture was sustained at the lower part of the outside of the leg in the region of the ankle. However, in the past 10 years, with the advent of the modern ski boots and improvements in binding, the most commonly seen lower leg skier fracture is the tibia (or shinbone) fracture. 10% of these fractures are associated with a collision. Thus, 90 % are associated with an isolated fall or noncontact type of injury, which is generally the result of binding malfunctions and inappropriate release. The most common mechanism leading to a tibia (leg) fracture is a forward fall. Risk factors for sustaining a skier tibia fracture include: beginners or novice skiers, less than 20 years of age, higher outdoor temperatures, and increased snow depth. Non-risk factors include ski lengths, icy conditions, and male versus female sex. The modern ski boot very closely resembles an extremely well padded short leg cast in the treatment of many orthopaedic lower extremity fractures. It of course goes to a much higher level than the former shorter boot top-level varieties. The binding release and designs have been based on the fracture strength of the adult tibia (shin) bone at the top of the modern ski boot. The treatment of most skier leg fractures includes a closed reduction and cast application for variable periods of time, with or without weight bearing allowed. However, severe misalignments of the bones can lead to later bony prominences that may be incompatible with snug, rigid, high fitting ski boots. -

Medial Lateral Malleolus
Acutrak 2® Headless Compression Screw System 4.7 mm and 5.5 mm Screws Supplemental Use Guide—Medial & Lateral Malleolus Acumed® is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches that improve patient care. Acumed® Acutrak 2® Headless Compression Screw System—4.7 mm and 5.5 mm This guide is intended for supplemental use only and is not intended to be used as a stand-alone surgical technique. Reference the Acumed Acutrak 2 Headless Compression Screw System Surgical Technique (SPF00-02) for more information. Definition Indicates critical information about a potential serious outcome to the Warning patient or the user. Indicates instructions that must be followed in order to ensure the proper Caution use of the device. Note Indicates information requiring special attention. Acumed® Acutrak 2® Headless Compression System—Supplemental Use Guide—Medial & Lateral Malleolus Table of Contents System Features ...........................................2 Surgical Techniques ........................................ 4 Fibula Fracture (Weber A and B Fractures) Surgical Technique: Acutrak 2®—5.5 .......................4 Medial Malleolus Surgical Technique: Acutrak 2®—4.7 ......................10 Ordering Information ......................................16 Acumed® Acutrak 2® Headless Compression System—Supplemental Use Guide—Medial & Lateral Malleolus System Features Headless screw design is intended to minimize soft tissue irritation D Acutrak 2 Screws Diameter -

Assessment, Management and Decision Making in the Treatment Of
Pediatric Ankle Fractures Anthony I. Riccio, MD Texas Scottish Rite Hospital for Children Update 07/2016 Pediatric Ankle Fractures The Ankle is the 2nd most Common Site of Physeal Injury in Children 10-25% of all Physeal Injuries Occur About the Ankle Pediatric Ankle Fractures Primary Concerns Are: • Anatomic Restoration of Articular Surface • Restoration of Symmetric Ankle Mortise • Preservation of Physeal Growth • Minimize Iatrogenic Physeal Injury • Avoid Fixation Across Physis in Younger Children Salter Harris Classification Prognosis and Treatment of Pediatric Ankle Fractures is Often Dictated by the Salter Harris Classification of Physeal Fractures Type I and II Fractures: Often Amenable to Closed Tx / Lower Risk of Physeal Arrest Type III and IV: More Likely to Require Operative Tx / Higher Risk of Physeal Arrest Herring JA, ed. Tachdjian’s Pediatric Orthopaedics, 5th Ed. 2014. Elsevier. Philadelphia, PA. ISOLATED DISTAL FIBULA FRACTURES Distal Fibula Fractures • The Physis is Weaker than the Lateral Ankle Ligaments – Children Often Fracture the Distal Fibula but…. – …ligamentous Injuries are Not Uncommon • Mechanism of Injury = Inversion of a Supinated Foot • SH I and II Fractures are Most Common – SH I Fractures: Average Age = 10 Years – SH II Fractures: Average Age = 12 Years Distal Fibula Fractures Lateral Ankle Tenderness SH I Distal Fibula Fracture vs. Lateral Ligamentous Injury (Sprain) Distal Fibula Fractures • Sankar et al (JPO 2008) – 37 Children – All with Open Physes, Lateral Ankle Tenderness + Normal Films – 18%: Periosteal -

Clinical Efficacy of Extended Modified Posteromedial Approach Versus
Clinical ecacy of extended modied posteromedial approach versus posterolateral approach for surgical treatment of posterior pilon fracture: a retrospective analysis Qin-Ming Zhang Aliated Hospital of Jining Medical University Hai-Bin Wang Aliated Hospital of Jining Medical University Xiao-Yan Li Aliated Hospital of Jining Medical University Feng-Long Chu Aliated Hospital of Jining Medical University Liang Han Aliated Hospital of Jining Medical University Dong-Mei Li Aliated Hospital of Jining Medical University Bin Wu ( [email protected] ) Alited Hospital of Jining Medical University https://orcid.org/0000-0003-3707-0056 Research article Keywords: posterior pilon fracture, approach, fracture xation, buttress plate Posted Date: March 30th, 2020 DOI: https://doi.org/10.21203/rs.3.rs-19392/v1 License: This work is licensed under a Creative Commons Attribution 4.0 International License. Read Full License Page 1/12 Abstract Background: Posterior pilon fracture is a type of ankle fracture associated with poorer treatment results compared to the conventional ankle fracture. This is partly related to the lack of consensus on the classication, approach selection, and internal xation method for this type of fracture. This study aimed to investigate the clinical ecacy of posterolateral approach versus extended modied posteromedial approach for surgical treatment of posterior pilon fracture. Methods: Data of 67 patients with posterior pilon fracture who received xation with a buttress plate between January 2015 and December 2018 were retrospectively reviewed. Patients received steel plate xation through either the posterolateral approach (n = 35, group A) or the extended modied posteromedial approach (n = 32, group B). Operation time, intraoperative blood loss, excellent and good rate of reduction, fracture healing time, American Orthopaedic Foot & Ankle Society (AOFAS) Ankle- Hindfoot Scale score, and Visual Analogue Scale score were compared between groups A and B. -

Free Vascularized Fibula Graft with Femoral Allograft Sleeve for Lumbar Spine Defects After Spondylectomy of Malignant Tumors Acasereport
1 COPYRIGHT Ó 2020 BY THE JOURNAL OF BONE AND JOINT SURGERY,INCORPORATED Free Vascularized Fibula Graft with Femoral Allograft Sleeve for Lumbar Spine Defects After Spondylectomy of Malignant Tumors ACaseReport Michiel E.R. Bongers, MD, John H. Shin, MD, Sunita D. Srivastava, MD, Christopher R. Morse, MD, Sang-Gil Lee, MD, and Joseph H. Schwab, MD, MS Investigation performed at Massachusetts General Hospital, Boston, Massachusetts Abstract Case: We present a 65-year-old man with an L4 conventional chordoma. Total en bloc spondylectomy (TES) of the involved vertebral bodies and surrounding soft tissues with reconstruction of the spine using a free vascularized fibula autograft (FVFG) is a proven technique, limiting complications and recurrence. However, graft fracture has occurred only in the lumbar spine in our institutional cases. We used a technique in our patient to ensure extra stability and support, with the addition of a femoral allograft sleeve encasing the FVFG. Conclusions: Our technique for the reconstruction of the lumbar spine after TES of primary malignant spinal disease using a femoral allograft sleeve encasing the FVFG is viable to consider. he treatment of primary malignant neoplasms of the spine mended a magnetic resonance imaging (MRI), but the request currently mainly relies on surgery, often in conjunction with was denied by the insurance company, and the patient T 1-3 radiotherapy .Totalen bloc spondylectomy (TES) is a widely underwent a course of physical therapy with no benefitand accepted surgical technique and has lower reported recurrence rates progression of back pain and radiculopathy. Four months compared with patients who undergo intralesional surgery3,4. -

Common Stress Fractures BRENT W
COVER ARTICLE PRACTICAL THERAPEUTICS Common Stress Fractures BRENT W. SANDERLIN, LCDR, MC, USNR, Naval Branch Medical Clinic, Fort Worth, Texas ROBERT F. RASPA, CAPT, MC, USN, Naval Hospital Jacksonville, Jacksonville, Florida Lower extremity stress fractures are common injuries most often associated with partic- ipation in sports involving running, jumping, or repetitive stress. The initial diagnosis can be made by identifying localized bone pain that increases with weight bearing or repet- itive use. Plain film radiographs are frequently unrevealing. Confirmation of a stress frac- ture is best made using triple phase nuclear medicine bone scan or magnetic resonance imaging. Prevention of stress fractures is most effectively accomplished by increasing the level of exercise slowly, adequately warming up and stretching before exercise, and using cushioned insoles and appropriate footwear. Treatment involves rest of the injured bone, followed by a gradual return to the sport once free of pain. Recent evidence sup- ports the use of air splinting to reduce pain and decrease the time until return to full par- ticipation or intensity of exercise. (Am Fam Physician 2003;68:1527-32. Copyright© 2003 American Academy of Family Physicians) tress fractures are among the involving repetitive use of the arms, such most common sports injuries as baseball or tennis. Stress fractures of and are frequently managed the ribs occur in sports such as rowing. by family physicians. A stress Upper extremity and rib stress fractures fracture should be suspected in are far less common than lower extremity Sany patient presenting with localized stress fractures.1 bone or periosteal pain, especially if he or she recently started an exercise program Etiology and Pathophysiology or increased the intensity of exercise. -
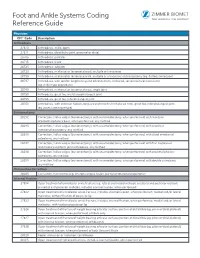
Foot and Ankle Systems Coding Reference Guide
Foot and Ankle Systems Coding Reference Guide Physician CPT® Code Description Arthrodesis 27870 Arthrodesis, ankle, open 27871 Arthrodesis, tibiofibular joint, proximal or distal 28705 Arthrodesis; pantalar 28715 Arthrodesis; triple 28725 Arthrodesis; subtalar 28730 Arthrodesis, midtarsal or tarsometatarsal, multiple or transverse 28735 Arthrodesis, midtarsal or tarsometatarsal, multiple or transverse; with osteotomy (eg, flatfoot correction) 28737 Arthrodesis, with tendon lengthening and advancement, midtarsal, tarsal navicular-cuneiform (eg, miller type procedure) 28740 Arthrodesis, midtarsal or tarsometatarsal, single joint 28750 Arthrodesis, great toe; metatarsophalangeal joint 28755 Arthrodesis, great toe; interphalangeal joint 28760 Arthrodesis, with extensor hallucis longus transfer to first metatarsal neck, great toe, interphalangeal joint (eg, jones type procedure) Bunionectomy 28292 Correction, hallux valgus (bunionectomy), with sesamoidectomy, when performed; with resection of proximal phalanx base, when performed, any method 28295 Correction, hallux valgus (bunionectomy), with sesamoidectomy, when performed; with proximal metatarsal osteotomy, any method 28296 Correction, hallux valgus (bunionectomy), with sesamoidectomy, when performed; with distal metatarsal osteotomy, any method 28297 Correction, hallux valgus (bunionectomy), with sesamoidectomy, when performed; with first metatarsal and medial cuneiform joint arthrodesis, any method 28298 Correction, hallux valgus (bunionectomy), with sesamoidectomy, when performed; with -

Geometric Variations in Load-Bearing Joints
University of Alberta Geometric Variations in Load-Bearing Joints by Kamrul Islam A thesis submitted to the Faculty of Graduate Studies and Research in partial fulfillment of the requirements for the degree of Master of Science in Structural Engineering Department of Civil and Environmental Engineering ©Kamrul Islam Fall 2012 Edmonton, Alberta Permission is hereby granted to the University of Alberta Libraries to reproduce single copies of this thesis and to lend or sell such copies for private, scholarly or scientific research purposes only. Where the thesis is converted to, or otherwise made available in digital form, the University of Alberta will advise potential users of the thesis of these terms. The author reserves all other publication and other rights in association with the copyright in the thesis and, except as herein before provided, neither the thesis nor any substantial portion thereof may be printed or otherwise reproduced in any material form whatsoever without the author's prior written permission. Dedication Dedicated to my dad, A.F.M. Shamsul Islam, my mom, Shahina Akhter Chowdhury, and my brother, Nazmul Islam Abstract The purpose of the current study was to investigate the geometric variations in the load-bearing joints among individuals. Two existing concepts in mathematics were introduced and their application in computational biomechanics was completely novel: 1) computing the depth of penetration between contact objects as an indirect measure of stress; and 2) computing the geometric similarity using the cubic root of volumetric ratio as a scaling law. Furthermore, an alternative geometric method to finite element analysis was proposed, which should be considered as a “proof of concept”.