Sphincter of Oddi Function and Dysfunction
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Anorectal Disorders Satish S
Gastroenterology 2016;150:1430–1442 Anorectal Disorders Satish S. C. Rao,1 Adil E. Bharucha,2 Giuseppe Chiarioni,3,4 Richelle Felt-Bersma,5 Charles Knowles,6 Allison Malcolm,7 and Arnold Wald8 1Division of Gastroenterology and Hepatology, Augusta University, Augusta, Georgia; 2Department of Gastroenterology and Hepatology, Mayo College of Medicine, Rochester, Minnesota; 3Division of Gastroenterology of the University of Verona, Azienda Ospedaliera Universitaria Integrata di Verona, Verona, Italy; 4Division of Gastroenterology and Hepatology and UNC Center for Functional GI and Motility Disorders, University of North Carolina at Chapel Hill, Chapel Hill, North Carolina; 5Department of Gastroenterology/Hepatology, VU Medical Center, Amsterdam, The Netherlands; 6National Centre for Bowel Research and Surgical Innovation, Blizard Institute, Queen Mary University of London, London, United Kingdom; 7Division of Gastroenterology, Royal North Shore Hospital, and University of Sydney, Sydney, Australia; 8Division of Gastroenterology, University of Wisconsin School of Medicine and Public Health, Madison, Wisconsin This report defines criteria and reviews the epidemiology, questionnaires and bowel diaries are correlated,5 some pathophysiology, and management of the following com- patients may not accurately recall bowel symptoms6; hence, mon anorectal disorders: fecal incontinence (FI), func- symptom diaries may be more reliable. tional anorectal pain, and functional defecation disorders. In this report, we examine the prevalence and patho- FI is defined as the recurrent uncontrolled passage of fecal physiology of anorectal disorders, listed in Table 1,and material for at least 3 months. The clinical features of FI provide recommendations for diagnostic evaluation and are useful for guiding diagnostic testing and therapy. management. These supplement practice guidelines rec- ANORECTAL Anorectal manometry and imaging are useful for evalu- ommended by the American Gastroenterological Associa- fl ating anal and pelvic oor structure and function. -

Comparative Anatomy of the Lower Respiratory Tract of the Gray Short-Tailed Opossum (Monodelphis Domestica) and North American Opossum (Didelphis Virginiana)
University of Tennessee, Knoxville TRACE: Tennessee Research and Creative Exchange Doctoral Dissertations Graduate School 12-2001 Comparative Anatomy of the Lower Respiratory Tract of the Gray Short-tailed Opossum (Monodelphis domestica) and North American Opossum (Didelphis virginiana) Lee Anne Cope University of Tennessee - Knoxville Follow this and additional works at: https://trace.tennessee.edu/utk_graddiss Part of the Animal Sciences Commons Recommended Citation Cope, Lee Anne, "Comparative Anatomy of the Lower Respiratory Tract of the Gray Short-tailed Opossum (Monodelphis domestica) and North American Opossum (Didelphis virginiana). " PhD diss., University of Tennessee, 2001. https://trace.tennessee.edu/utk_graddiss/2046 This Dissertation is brought to you for free and open access by the Graduate School at TRACE: Tennessee Research and Creative Exchange. It has been accepted for inclusion in Doctoral Dissertations by an authorized administrator of TRACE: Tennessee Research and Creative Exchange. For more information, please contact [email protected]. To the Graduate Council: I am submitting herewith a dissertation written by Lee Anne Cope entitled "Comparative Anatomy of the Lower Respiratory Tract of the Gray Short-tailed Opossum (Monodelphis domestica) and North American Opossum (Didelphis virginiana)." I have examined the final electronic copy of this dissertation for form and content and recommend that it be accepted in partial fulfillment of the equirr ements for the degree of Doctor of Philosophy, with a major in Animal Science. Robert W. Henry, Major Professor We have read this dissertation and recommend its acceptance: Dr. R.B. Reed, Dr. C. Mendis-Handagama, Dr. J. Schumacher, Dr. S.E. Orosz Accepted for the Council: Carolyn R. -

Reoperative Techniques and Management in Hirschsprung Disease: a Narrative Review
14 Review Article Reoperative techniques and management in Hirschsprung disease: a narrative review Farokh R. Demehri^, Belinda H. Dickie Department of Surgery, Boston Children’s Hospital, Boston, MA, USA Contributions: (I) Conception and design: All authors; (II) Administrative support: None; (III) Provision of study materials or patients: None; (IV) Collection and assembly of data: All authors; (V) Data analysis and interpretation: All authors; (VI) Manuscript writing: All authors; (VII) Final approval of manuscript: All authors Correspondence to: Farokh R. Demehri, MD. Department of Surgery, Boston Children’s Hospital, 300 Longwood Ave, Fegan 3, Boston, MA 02115, USA. Email: [email protected]. Abstract: The majority of children who undergo operative management for Hirschsprung disease have favorable results. A subset of patients, however, have long-term dysfunctional stooling, characterized by either frequent soiling or obstructive symptoms. The evaluation and management of a child with poor function after pull-through for Hirschsprung disease should be conducted by an experienced multidisciplinary team. A systematic workup is focused on detecting pathologic and anatomic causes of pull- through dysfunction. This includes an exam under anesthesia, pathologic confirmation including a repeat biopsy, and a contrast enema, with additional studies depending on the suspected etiology. Obstructive symptoms may be due to technique-specific types of mechanical obstruction, histopathologic obstruction, or dysmotility—each of which may benefit from reoperative surgery. The causes of soiling symptoms include loss of the dentate line and damage to the anal sphincter, which generally do not benefit from revision of the pull-through, and pseudo-incontinence, which may reveal underlying obstruction. A thorough understanding of the types of complications associated with various pull-through techniques aids in the evaluation of a child with postoperative dysfunction. -

Sphincter of Oddi: ERCP Plus Sphincterotomy – Yes Or No
Sphincter of Oddi: ERCP Plus Sphincterotomy – Yes or No Note: For debate purposes, the pro and con positions for patient management will be taken by the invited authors. However, actual decisions regarding patient care must involve discussion of the risks and benefits of each treatment considered. Case Presentation – Case developed by Ihab I. El Hajj, MD, MPH, Indiana University, Indianapolis, IN A 57-year-old Caucasian female with history of smoking and COPD, was in her usual state of health until two years ago, when she experienced recurrent “attacks” of right upper quadrant pain, nausea and occasional vomiting, suggestive of biliary colic. The patient was evaluated by her primary care physician and initial work- up, which included basic blood work, liver chemistries and transabdominal ultrasound, were negative. The patient responded partially to prn Zofran and omeprazole 40 mg once then twice daily. With the persistence of her symptoms, the patient was referred to a gastroenterologist. Esophagogastroduodenoscopy (EGD) with gastric biopsies revealed chronic inactive gastritis without Helicobacter pylori. HIDA scan suggested biliary dyskinesia with an ejection fraction of 22%. An elective laparoscopic cholecystectomy was performed. An intra- operative cholangiogram showed no filling defect in the common bile duct (CBD) and pathology demonstrated chronic cholecystitis with no gallstones. The patient was symptom-free for six months after surgery. She subsequently developed vague upper abdominal pain, intermittent nausea and irregular bowel movements. Labs, colonoscopy and repeat EGD were ASGE Leading Edge — Volume 4, No. 4 © American Society for Gastrointestinal Endoscopy normal. The patient was treated for suspected irritable bowel syndrome. She failed several medications including hyoscyamine, dicyclomine, amitriptyline, sucralfate, and GI cocktail. -

Transampullary Septectomy for Papillary Stenos S
HPB Surgery, 1996, Vol.9, pp.199-207 (C) 1996 OPA (Overseas Publishers Association) Reprints available directly from the publisher Amsterdam B.V. Published in The Netherlands Photocopying permitted by license only by Harwood Academic Publishers GmbH Printed in Malaysia Transduodenal Sphincteroplasty an.d Transampullary Septectomy for Papillary Stenos s S.B. KELLY and B.J. ROWLANDS Depa,rtment of Surgery, Institute of Clinical Science, Royal Victoria Hospital, Grosvenor Road, Belfast. BT12 6BJ (Received 10 February 1994) Twenty patients received transduodenal sphincteroplasty and transampullary septectomy between 1987 and 1993. Seven patients had post-cholecystectomy pain which was much improved or abolished in 5 of 7 patients at a mean follow-up of 4 years and 5 months. Four of five patients with chronic pancreatitis were improved at 3 years and 2 months. Three of five patients with recurrent acute pancreatitis were improved at 4 years and 5 months. One of three patients with chronic abdominal pain of hepatobiliary origin was improved at 3 years. Transduodenal sphincteroplasty and transampullary septectomy can relieve pain in patients with post-cholecystectomy pain, recurrent acute pancreatitis, chronic pancreatitis, and chronic abdominal pain of hepatobiliary origin, presumably by improving drainage of the obstructed ducts. KEY WORDS: Transduodenal sphincteroplasty transampullary septectomy papillary stenosis INTRODUCTION without hyperamylassaemia requires a transduodenal operation. Transduodenal sphincteroplasty and trans- The indications -

Online Supplement
Online Supplement Definition, discrimination, diagnosis, and treatment of central breathing disturbances during sleep. An ERS Statement Randerath W*#1, Verbraecken J*#2, Andreas S3, Arzt M4, Bloch KE5, Brack T6, Buyse B7, De Backer W2, Eckert DJ8, Grote L9, Hagmeyer L1, Hedner J9, Jennum P10, La Rovere MT11, Miltz C1, McNicholas WT12, Montserrat J13, Naughton M14, Pepin J-L15, Pevernagie D16, Sanner B17, Testelmans D7, Tonia T18, Vrijsen B7, Wijkstra P19, Levy P#15 *contributed equally as first authors #co-chaired the Task Force 1 Bethanien Hospital, Institute of Pneumology, Solingen, Germany 2 Dept of Pulmonary Medicine, Antwerp University Hospital and University of Antwerp, Edegem, Belgium 3 Cardiology and Pneumology, University Medical Center Göttingen, Germany and Lung Clinic Immenhausen, Krs. Kassel, Germany 4 Department of Internal Medicine II University Hospital Regensburg, Germany 5 University Hospital Zurich, Department of Pulmonology and Sleep Disorders Center, Zurich, Switzerland 6 Department of Internal and Pulmonary Medicine, Kantonsspital Glarus, Switzerland 7 Department of Pulmonary Medicine – KU Leuven, Leuven, Belgium 8 8 Neuroscience Research Australia (NeuRA) and the University of New South Wales, Sydney, New South Wales, Australia 9 Sleep Disorders Center, Dept. of Pulmonary Medicine, Sahlgrenska University Hospital, Göteborg, Sweden 10 Center for Healthy Aging and Danish Center for Sleep Medicine, Faculty of Health Sciences, University of Copenhagen, Denmark 1 11 Department of Cardiology, Fondazione S. Maugeri, IRCCS, Istituto Scientifico di Montescano (Pavia), Italy 12 Pulmonary and Sleep Disorders Unit, St. Vincent’s University Hospital and University College Dublin, Dublin, Ireland 13 Laboratori del Son, Hospital Clínic, Universitat de Barcelona, Barcelona, Spain. 14 General Respiratory and Transplantation, Alfred Hospital and Monash University, Melbourne, Victoria, Australia 15 Laboratoire du sommeil explorations fonct. -
![Mft•] ~;;I~ [I) I~ T?L3 ·Ilr!F·S; [,J ~ M](https://docslib.b-cdn.net/cover/6471/mft-i-i-i-t-l3-%C2%B7ilr-f%C2%B7s-j-m-706471.webp)
Mft•] ~;;I~ [I) I~ T?L3 ·Ilr!F·S; [,J ~ M
Mft•] ~;;I~ [I) I~ t?l3 ·ilr!f·S; [,j ~ M Hepatobiliary Imaging Update Maggie Chester and Jerry Glowniak Veterans Affairs Medical Center and Oregon Health Sciences University, Portland, Oregon and the gallbladder ejection fraction (EF) after the injection This is the first article in a four-part series on interventional of cholecystokinin (CCK) (Kinevac®, Squibb Diagnostics, nuclear medicine. Upon completion, the nuclear medicine New Brunswick, NJ). A brief description of the hepatic ex technologist should be able to (1) list the advantages of using traction fraction (HEF) was given; the technique used quan interventional hepatic imaging, (2) identify the benefit in tifies hepatocyte function more accurately than does excretion calculating HEF, and (3) utilize the HEF calculation method when appropriate. half-time. Since publication of the previous article (5), the HEF has become more widely used as a measure of hepatocyte function, and nearly all the major nuclear medicine software vendors include programs for calculating the HEF. Scintigraphic assessment of hepatobiliary function began in In this article, we will describe new observations and meth the 1950s with the introduction of iodine-131 C31 1) Rose ods used in hepatobiliary imaging. The following topics will bengal (1). Due to the poor imaging characteristics of 1311, be discussed: ( 1) the use of morphine as an aid in the diagnosis numerous attempts were made to find a technetium-99m 99 of acute cholecystitis, (2) the rim sign in the diagnosis of acute ( mTc) labeled hepatobiliary agent (2). The most useful of cholecystitis, and (3) methods for calculating the HEF. the several 99mTc-labeled agents that were investigated were the iminodiacetic acid (IDA) analogs, which were introduced MORPHINE-AUGMENTED CHOLESCINTIGRAPHY in the mid 1970s (3). -

Biliary Dyspepsia: Functional Gallbladder and Sphincter of Oddi Disorders
Chapter 7 Biliary Dyspepsia: Functional Gallbladder and Sphincter of Oddi Disorders Meena Mathivanan, Liisa Meddings and Eldon A. Shaffer Additional information is available at the end of the chapter http://dx.doi.org/10.5772/56779 1. Introduction Biliary-type abdominal pain is common and often presents a clinical challenge for physicians. True biliary colic consists of episodes of steady pain across the right upper quadrant and epigastric regions, lasting from 30 minutes to 6 hours [1]. Such abdominal pain, when it lasts longer than 6 hours, is likely due to complications of gallstone disease such as acute cholecys‐ titis or acute pancreatitis, or represents a non-biliary source of pain [1]. 1.1. Cholelithiasis, biliary pain and atypical dyspepsia Classical biliary pain that occurs in the setting of gallstones represents symptomatic choleli‐ thiasis. The symptoms associated with gallstones however are frequently confusing. In fact, only 13% of people with gallstones ever develop biliary pain when followed for 15–20 years [2], meaning that most (70-90%) patients with gallstones never experience biliary symptoms. Vague dyspeptic complaints like belching, bloating, flatulence, heartburn and nausea are not characteristic for biliary disease [3, 4]. Therefore, it is not surprising that cholecystectomy often fails to relieve such ambiguous symptoms in those with documented gallstones. In fact, cholecystectomy fails to relieve symptoms in 10-33% of patients with documented gallstones [5]. If the abdominal pain is misdiagnosed and instead due to functional gut disorders like irritable bowel syndrome, cholecystectomy would not provide a favorable outcome [4, 5, 6]. 1.2. Functional gallbladder disease Biliary-type abdominal pain (also termed biliary colic) in the context of a structurally normal gallbladder has been referred to as “biliary dyspepsia”. -

Copyrighted Material
Subject index Note: page numbers in italics refer to fi gures, those in bold refer to tables Abbreviations used in subentries abdominal mass patterns 781–782 GERD – gastroesophageal refl ux disease choledochal cysts 1850 perception 781 IBD – infl ammatory bowel disease mesenteric panniculitis 2208 periodicity 708–709 mesenteric tumors 2210 peripheral neurogenic 2429 A omental tumors 2210 pharmacological management 714–717 ABCB1/MDR1 484 , 633 , 634–636 abdominal migrane (AM) 712 , 2428–2429 physical examination 709–710 , 710 ABCB4 abdominal obesity 2230 postprandial 2498–2499 c h o l e s t e r o l g a l l s t o n e s 1817–1818 , abdominal pain 695–722 in pregnancy 842 1819–1820 a c u t e see acute abdominal pain prevalence 695 functions 483–484 , 1813 acute cholecystitis 784 rare/obscure causes 712–713 , 712 intrahepatic cholestasis of pregnancy 848 acute diverticulitis 794–796 , 795 , 1523–1524 , red fl ags 713 low phospholipid-associated 1527 relieving/aggravating factors 709 cholelithiasis 1810 , 1819–1820 , 2393 acute mesenteric ischemia 2492 right lower quadrant 794 m u t a t i o n p h e n o t y p e s 2392 , 2393 a c u t e p a n c r e a t i t i s 795 , 1653 , 1667 right upper quadrant 794 progressive familial intrahepatic cholestasis-3 acute suppurative peritonitis 2196 sickle cell crisis 2419 494 adhesions 713 s i t e 703 , 708 ABCB11 see bile salt export pump (BSEP) AIDS 2200 special pain syndromes 718–720 ABCC2/MRP2 485 , 494 , 870 , 1813 , 2394 , 2395 anxiety 706–707 sphincter of Oddi dysfunction 1877 ABCG2/BCRP 484–485 , 633 -
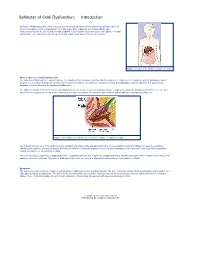
Sphincter of Oddi Dysfunction: Introduction
Sphincter of Oddi Dysfunction: Introduction Sphincter of Oddi dysfunction refers to structural or functional disorders involving the biliary sphincter that may result in impedance of bile and pancreatic juice flow. Up to 20% of patients with continued pain after cholecystectomy and 10–20% of patients with idiopathic recurrent pancreatitis may suffer from sphincter of Oddi dysfunction. This condition is more prevalent among middle-aged women for unclear reasons Figure 1. Location of the sphincter of Oddi in the body. What is Sphincter of Oddi Dysfunction? The sphincter of Oddi has three major functions: 1) regulation of bile and pancreatic flow into the duodenum, 2) diversion of hepatic bile into the gallbladder, and 3) the prevention of reflux of duodenal contents into the pancreaticobiliary tract. With the ingestion of a meal, the gallbladder contracts and there is a simultaneous decrease in the resistance in the sphincter of Oddi zone. The sphincter of Oddi consists of circular and longitudinal smooth muscle fibers surrounding a variable length of the distal bile and pancreatic duct. There are three discrete areas of muscle thickness, or mini sphincters: the sphincter papillae, the sphincter pancreaticus, and the sphincter choledochus (Figure 2). Figure 2. Mini sphincters, or discrete areas of muscle, comprise the sphincter of Oddi. The major physiologic role of the sphincter is the regulation of the flow of bile and pancreatic juice. Cholecystokinin (CCK) and nitrates decrease the resistance offered by the sphincter. Laboratory studies observing the effects of numerous peptides, hormones, and medications on the sphincter have suggested a multifactor control mechanism for the sphincter of Oddi. -

Guidelines for the Management of Postoperative Soiling in Children with Hirschsprung Disease
Pediatric Surgery International (2019) 35:829–834 https://doi.org/10.1007/s00383-019-04497-y REVIEW ARTICLE Guidelines for the management of postoperative soiling in children with Hirschsprung disease P. Saadai1,2 · A. F. Trappey1,2 · A. M. Goldstein3 · R. A. Cowles4 · L. De La Torre5 · M. M. Durham6 · E. Y. Huang7 · M. A. Levitt8 · K. Rialon9 · M. Rollins10 · D. H. Rothstein11 · J. C. Langer9 on behalf of The American Pediatric Surgical Association Hirschsprung Disease Interest Group Accepted: 6 June 2019 / Published online: 14 June 2019 © Springer-Verlag GmbH Germany, part of Springer Nature 2019 Abstract Although most children with Hirschsprung disease ultimately achieve functional and comfortable stooling, some will experi- ence a variety of problems after pull-through surgery. The most common problems include soiling, obstructive symptoms, enterocolitis, and failure to thrive. The purpose of this guideline is to present a rational approach to the management of postoperative soiling in children with Hirschsprung disease. The American Pediatric Surgical Association Hirschsprung Disease Interest Group engaged in a literature review and group discussions. Expert consensus was then used to summarize the current state of knowledge regarding causes, methods of diagnosis, and treatment approaches to children with soiling symptoms following pull-through for Hirschsprung disease. Causes of soiling after pull-through are broadly categorized as abnormalities in sensation, abnormalities in sphincter control, and “pseudo-incontinence.” A stepwise algorithm for the diagnosis and management of soiling after a pull-through for Hirschsprung disease is presented; it is our hope that this rational approach will facilitate treatment and optimize outcomes. Keywords Hirschsprung disease · Soiling · Incontinence · Pseudo-incontinence · Bowel management · Pull-through Background obstructive symptoms, enterocolitis and failure to thrive [1]. -

"Neural Interactions Between the Small Intestine and the Sphincter of Oddi" and "Sustainable Development for Economic, Social, and Environmental Health"
Bridgewater Review Volume 19 | Issue 1 Article 11 Jun-2000 Report From CART: "Neural Interactions Between the Small Intestine and the Sphincter of Oddi" And "Sustainable Development for Economic, Social, and Environmental Health" Recommended Citation (2000). Report From CART: "Neural Interactions Between the Small Intestine and the Sphincter of Oddi" And "Sustainable Development for Economic, Social, and Environmental Health". Bridgewater Review, 19(1), 25-26. Available at: http://vc.bridgew.edu/br_rev/vol19/iss1/11 This item is available as part of Virtual Commons, the open-access institutional repository of Bridgewater State University, Bridgewater, Massachusetts. duodenal neurons sending nerve fibers to the sphincter ofOddi. We deter CENTER FOR mined that these neurons synthesize excitatory neurotransmitters, which cause the sphincter muscle to contract. THE ADVANCEMENT We performed additional electro physiological studies to further exam OF RESEARCH ine this mechanism. These studies involved recording electrical activity from target neurons located within the AND TEACHING sphincter ofOddi while stimulating axons passing into the sphincter from CART grants enable faculty and results in over 600,000 cholecystec the duodenum. We demonstrated that librarians to pursue research projects. tomies (surgical removals ofthe the duodenal neurons sending projec "Neural Interactions Between the Small gallbladder) each year. tions to the sphincter ofOddi are capa Intestine and the Sphincter ofOddi" How does the sphincter ofOddi ble ofelectrically activating neurons and "Sustainable Development: The know when to open and when to close? located within the sphincter. Activation Search for Economic, Social, and Although we know that the nervous ofneurons in the sphincter ofOddi by Environmental Health" are among the system is involved, the exact mecha neurons in the duodenum is likely to projects which were recently awarded nisms ofits regulation are not entirely increase the contraction ofthis muscle, CART grants.