SCLERODERMA: Overview and Causes
Total Page:16
File Type:pdf, Size:1020Kb

Load more
Recommended publications
-

Understanding and Managing Scleroderma
Understanding and Managing Scleroderma A publication of Scleroderma Foundation 300 Rosewood Drive, Suite 105 Danvers, MA 01923 Maureen D. Mayes, M.D., M.P.H. Understanding and Understanding My notes and Managing Scleroderma Managing Scleroderma This booklet is intended to help people with scleroderma, their families and others interested ________________________ in learning more about the disease to better understand what scleroderma is, what effects ________________________ it may have, and what those with scleroderma can do to help themselves and their physicians ________________________ manage the disease. It answers some of the most frequently asked questions about ________________________ A publication of Maureen D. Mayes, M.D., M.P.H. Scleroderma Foundation 300 Rosewood Drive, Suite 105 scleroderma. Danvers, MA 01923 800-722-HOPE (4673) www.scleroderma.org www.facebook.com/sclerodermaUS www.twitter.com/scleroderma ________________________ Disclaimer The Scleroderma Foundation does not provide medical advice nor does it ________________________ endorse any drug or treatment mentioned herein. ________________________ The material contained in this booklet is presented for general information only. It is not intended to provide medical advice, to answer questions specific to the condition or problems of particular individuals, nor in ________________________ any way to substitute for the professional advice and care of qualified physicians. Mention of particular drugs and/or treatments is for ________________________ information purposes only and does not constitute an endorsement of said drugs and/or treatments. ________________________ Thanks! ________________________ The Scleroderma Foundation expresses its deep appreciation to the many ________________________ physicians whose efforts have led to this booklet. Special thanks are owed to Maureen D. Mayes, M.D., M.P.H., of the ________________________ University of Texas McGovern Medical School, Houston. -

The Voice of the Patient
The Voice of the Patient A series of reports from the U.S. Food and Drug Administration’s (FDA’s) Patient-Focused Drug Development Initiative Systemic Sclerosis Public Meeting: October 13, 2020 Report Date: June 30, 2021 Center for Drug Evaluation and Research (CDER) U.S. Food and Drug Administration (FDA) 1 Table of Contents Introduction ............................................................................................................................ 3 Overview of Systemic Sclerosis ................................................................................................................. 3 Meeting Overview ..................................................................................................................................... 3 Report Overview and Key Themes ............................................................................................................ 5 Topic 1: Disease Symptoms and Daily Impacts That Matter Most to Patients .......................... 6 Perspectives on Most Significant Symptoms ............................................................................................ 6 Overall Impact of Systemic Sclerosis on Daily Life .................................................................................... 9 Topic 2: Patient Perspectives on Treatments for Systemic Sclerosis ....................................... 11 Perspectives on Current Treatments ...................................................................................................... 11 Perspectives on Ideal -

A Review of the Evidence for and Against a Role for Mast Cells in Cutaneous Scarring and Fibrosis
International Journal of Molecular Sciences Review A Review of the Evidence for and against a Role for Mast Cells in Cutaneous Scarring and Fibrosis Traci A. Wilgus 1,*, Sara Ud-Din 2 and Ardeshir Bayat 2,3 1 Department of Pathology, Ohio State University, Columbus, OH 43210, USA 2 Centre for Dermatology Research, NIHR Manchester Biomedical Research Centre, Plastic and Reconstructive Surgery Research, University of Manchester, Manchester M13 9PT, UK; [email protected] (S.U.-D.); [email protected] (A.B.) 3 MRC-SA Wound Healing Unit, Division of Dermatology, University of Cape Town, Observatory, Cape Town 7945, South Africa * Correspondence: [email protected]; Tel.: +1-614-366-8526 Received: 1 October 2020; Accepted: 12 December 2020; Published: 18 December 2020 Abstract: Scars are generated in mature skin as a result of the normal repair process, but the replacement of normal tissue with scar tissue can lead to biomechanical and functional deficiencies in the skin as well as psychological and social issues for patients that negatively affect quality of life. Abnormal scars, such as hypertrophic scars and keloids, and cutaneous fibrosis that develops in diseases such as systemic sclerosis and graft-versus-host disease can be even more challenging for patients. There is a large body of literature suggesting that inflammation promotes the deposition of scar tissue by fibroblasts. Mast cells represent one inflammatory cell type in particular that has been implicated in skin scarring and fibrosis. Most published studies in this area support a pro-fibrotic role for mast cells in the skin, as many mast cell-derived mediators stimulate fibroblast activity and studies generally indicate higher numbers of mast cells and/or mast cell activation in scars and fibrotic skin. -

The Articular Manifestations of Progressive Systemic Sclerosis (Scleroderma) MURRAY BARON, PETER LEE, and EDWARD C
Ann Rheum Dis: first published as 10.1136/ard.41.2.147 on 1 April 1982. Downloaded from Annals ofthe Rheumatic Diseases, 1982, 41, 147-152 The articular manifestations of progressive systemic sclerosis (scleroderma) MURRAY BARON, PETER LEE, AND EDWARD C. KEYSTONE From the University of Toronto Rheumatic Disease Unit, The Wellesley Hospital, 160 Wellesley Street East, Toronto, Ontario, Canada M4Y 1J3 SUMMARY The articular manifestations of progressive systemic sclerosis (PSS) were studied in 38 patients. Of these, 66 % experienced joint pain and 61 % had signs of joint inflammation. Limita- tion of joint movement was seen in 45 %. Radiological abnormalities included periarticular osteoporosis (42 %), joint space narrowing (34%), and erosions (40%). Erosive disease did not correlate with disease duration, presence of rheumatoid factor, antinuclear antibodies, distal tuft resorption, or the extent of the scleroderma skin changes. Calcinosis was seen more frequently in those patients with articular erosions (67 %). Erosive osteoarthritis of the distal interphalangeal joints (7 patients) was associated with impaired finger flexion. Joint involvement in PSS occurs frequently and may resemble rheumatoid arthritis in the early stages but is less destructive. The occurrence of unrelated arthropathy, such as primary osteoarthritis, is not uncommon, and its differentiation from true PSS joint disease can be difficult. Articular manifestations are common in progressive spective study and fulfilling the preliminary diagnos- systemic sclerosis (scleroderma, PSS), and joint pain tic criteria for PSS1 were evaluated by one author is a frequent presenting feature of this disease.' Joint (M.B.). A history of joint manifestations was symptoms have been noted in 12 to 66% of patients obtained in each case according to a standard pro- http://ard.bmj.com/ at the time of diagnosis2`6 and in 24 to 97% of tocol. -

Scleroderma Phenotype'' This Information Is Current As of September 27, 2021
Autoantibodies to Fibrillin-1 Activate Normal Human Fibroblasts in Culture through the TGF-β Pathway to Recapitulate the ''Scleroderma Phenotype'' This information is current as of September 27, 2021. Xiaodong Zhou, Filemon K. Tan, Dianna M. Milewicz, Xinjian Guo, Constantin A. Bona and Frank C. Arnett J Immunol 2005; 175:4555-4560; ; doi: 10.4049/jimmunol.175.7.4555 http://www.jimmunol.org/content/175/7/4555 Downloaded from References This article cites 32 articles, 11 of which you can access for free at: http://www.jimmunol.org/content/175/7/4555.full#ref-list-1 http://www.jimmunol.org/ Why The JI? Submit online. • Rapid Reviews! 30 days* from submission to initial decision • No Triage! Every submission reviewed by practicing scientists • Fast Publication! 4 weeks from acceptance to publication by guest on September 27, 2021 *average Subscription Information about subscribing to The Journal of Immunology is online at: http://jimmunol.org/subscription Permissions Submit copyright permission requests at: http://www.aai.org/About/Publications/JI/copyright.html Email Alerts Receive free email-alerts when new articles cite this article. Sign up at: http://jimmunol.org/alerts The Journal of Immunology is published twice each month by The American Association of Immunologists, Inc., 1451 Rockville Pike, Suite 650, Rockville, MD 20852 Copyright © 2005 by The American Association of Immunologists All rights reserved. Print ISSN: 0022-1767 Online ISSN: 1550-6606. The Journal of Immunology Autoantibodies to Fibrillin-1 Activate Normal Human Fibroblasts in Culture through the TGF- Pathway to Recapitulate the “Scleroderma Phenotype”1 Xiaodong Zhou,2* Filemon K. Tan,* Dianna M. -

Systemic Scleroderma
Systemic scleroderma Description Systemic scleroderma is an autoimmune disorder that affects the skin and internal organs. Autoimmune disorders occur when the immune system malfunctions and attacks the body's own tissues and organs. The word "scleroderma" means hard skin in Greek, and the condition is characterized by the buildup of scar tissue (fibrosis) in the skin and other organs. The condition is also called systemic sclerosis because the fibrosis can affect organs other than the skin. Fibrosis is due to the excess production of a tough protein called collagen, which normally strengthens and supports connective tissues throughout the body. The signs and symptoms of systemic scleroderma usually begin with episodes of Raynaud phenomenon, which can occur weeks to years before fibrosis. In Raynaud phenomenon, the fingers and toes of affected individuals turn white or blue in response to cold temperature or other stresses. This effect occurs because of problems with the small vessels that carry blood to the extremities. Another early sign of systemic scleroderma is puffy or swollen hands before thickening and hardening of the skin due to fibrosis. Skin thickening usually occurs first in the fingers (called sclerodactyly) and may also involve the hands and face. In addition, people with systemic scleroderma often have open sores (ulcers) on their fingers, painful bumps under the skin (calcinosis) , or small clusters of enlarged blood vessels just under the skin (telangiectasia). Fibrosis can also affect internal organs and can lead to impairment or failure of the affected organs. The most commonly affected organs are the esophagus, heart, lungs, and kidneys. Internal organ involvement may be signaled by heartburn, difficulty swallowing (dysphagia), high blood pressure (hypertension), kidney problems, shortness of breath, diarrhea, or impairment of the muscle contractions that move food through the digestive tract (intestinal pseudo-obstruction). -

Fundamentals of Dermatology Describing Rashes and Lesions
Dermatology for the Non-Dermatologist May 30 – June 3, 2018 - 1 - Fundamentals of Dermatology Describing Rashes and Lesions History remains ESSENTIAL to establish diagnosis – duration, treatments, prior history of skin conditions, drug use, systemic illness, etc., etc. Historical characteristics of lesions and rashes are also key elements of the description. Painful vs. painless? Pruritic? Burning sensation? Key descriptive elements – 1- definition and morphology of the lesion, 2- location and the extent of the disease. DEFINITIONS: Atrophy: Thinning of the epidermis and/or dermis causing a shiny appearance or fine wrinkling and/or depression of the skin (common causes: steroids, sudden weight gain, “stretch marks”) Bulla: Circumscribed superficial collection of fluid below or within the epidermis > 5mm (if <5mm vesicle), may be formed by the coalescence of vesicles (blister) Burrow: A linear, “threadlike” elevation of the skin, typically a few millimeters long. (scabies) Comedo: A plugged sebaceous follicle, such as closed (whitehead) & open comedones (blackhead) in acne Crust: Dried residue of serum, blood or pus (scab) Cyst: A circumscribed, usually slightly compressible, round, walled lesion, below the epidermis, may be filled with fluid or semi-solid material (sebaceous cyst, cystic acne) Dermatitis: nonspecific term for inflammation of the skin (many possible causes); may be a specific condition, e.g. atopic dermatitis Eczema: a generic term for acute or chronic inflammatory conditions of the skin. Typically appears erythematous, -

Advances in Seborrheic Keratosis
A CME/CE-Certified Supplement to Original Release Date: December 2018 Advances in Seborrheic Expiration Date: December 31, 2020 Estimated Time To Complete Activity: 1 hour Participants should read the activity information, Keratosis review the activity in its entirety, and complete the online post-test and evaluation. Upon completing this activity as designed and achieving a passing score on FACULTY the post-test, you will be directed to a Web page that will Joseph F. Fowler Jr, MD Michael S. Kaminer, MD allow you to receive your certificate of credit via e-mail Clinical Professor and Director Associate Clinical Professor of Dermatology or you may print it out at that time. Contact and Occupational Yale Medical School The online post-test and evaluation can be accessed Dermatology New Haven, Connecticut at http://tinyurl.com/SebK2018. University of Louisville School of Adjunct Assistant Professor of Medicine Medicine (Dermatology), Warren Alpert Medical School Inquiries about continuing medical education (CME) Louisville, Kentucky of Brown University accreditation may be directed to the University of Providence, Rhode Island Louisville Office of Continuing Medical Education & Professional Development (CME & PD) at cmepd@ louisville.edu or (502) 852-5329. Designation Statement eborrheic keratosis (SK) has been called keratinizing surface.12 They can develop virtually The University of Louisville School of Medicine the “Rodney Dangerfield of skin lesions”— anywhere except for the palms, soles, and mucous designates this Enduring material for a maximum of 9 1.0 AMA PRA Category 1 Credit(s)™. Physicians should it earns little respect (as a clinical concern) membranes, but are most commonly observed claim only the credit commensurate with the extent of Sbecause of its benignity, commonality, usual on the trunk and face.6,13 The tendency to develop their participation in the activity. -

Linear Scleroderma “En Coup De Sabre” Coexisting with Plaque-Morphea
661 J Neurol Neurosurg Psychiatry: first published as 10.1136/jnnp.74.5.661 on 1 May 2003. Downloaded from SHORT REPORT Linear scleroderma “en coup de sabre” coexisting with plaque-morphea: neuroradiological manifestation and response to corticosteroids I Unterberger, E Trinka, K Engelhardt, A Muigg, P Eller, M Wagner, N Sepp, G Bauer ............................................................................................................................. J Neurol Neurosurg Psychiatry 2003;74:661–664 progression of skin lesions or any neurological abnormalities A 24 year old woman in the 33rd week of pregnancy during follow up. developed progressive neurological complications with On admission the patient was in the 33rd week of right sided hemiparesis in association with the occurrence pregnancy. She was fully oriented, had normal speech, and of linear scleroderma “en coup de sabre” (LSCS) and pre- presented with a right sided hemiparesis (grade 3/5, MRC existing plaque-morphea, already being treated by scale) with a positive Babinski sign on the right. There was no balneophototherapy. Further progression of neurological history of head trauma. symptoms led to a caesarean section with the delivery of a Routine laboratory testing and comprehensive serological healthy child. Brain magnetic resonance imaging (MRI) screening including antineutrophilic cytoplasmic antibodies showed focal T2 signal increases in the left frontoparietal (ANCA), anticardiolipin antibodies, and antibodies against region directly adjacent to the area of LSCS. -
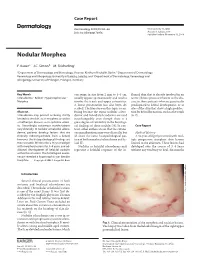
Nodular Morphea
Case Report Dermatology 2009;218:63–66 Received: July 13, 2008 DOI: 10.1159/000173976 Accepted: July 23, 2008 Published online: November 13, 2008 Nodular Morphea a b c F. Kauer J.C. Simon M. Sticherling a b Department of Dermatology and Venerology, Vivantes Klinikum Neukölln, Berlin , Department of Dermatology, c Venerology and Allergology, University of Leipzig, Leipzig , and Department of Dermatology, Venerology and Allergology, University of Erlangen, Erlangen , Germany Key Words can range in size from 2 mm to 4–5 cm, flamed skin that is already involved in an -Scleroderma ؒ Keloid ؒ Hypertrophic scar ؒ usually appear spontaneously and tend to active fibrotic process inherent to the dis Morphea involve the trunk and upper extremities. ease in those patients who are genetically A linear presentation has also been de- predisposed to keloid development, or at scribed. The literature on this topic is con- sites of the skin that show a high predilec- Abstract fusing because the terms ‘nodular sclero- tion for keloid formation, such as the trunk Scleroderma may present as being strictly derma’ and ‘keloidal scleroderma’ are used [6, 7] . limited to the skin, as in morphea, or within interchangeably even though there is a a multiorgan disease, as in systemic sclero- great degree of variability in the histologi- sis. Accordingly, cutaneous manifestations cal findings of these nodules [4] . In con- C a s e R e p o r t vary clinically. In nodular or keloidal sclero- trast, other authors stress that the cutane- derma, patients develop lesions that are ous manifestations may vary clinically, but Medical History clinically indistinguishable from a keloid; all share the same histopathological pat- A 16-year-old girl presented with mul- however, the histopathological findings are tern of both morphea/scleroderma and ke- tiple progressive morpheic skin lesions more variable. -

Hepatic Manifestations of Autoimmune Rheumatic Diseases ANNALS of GASTROENTEROLOGY 2005, 18(3):309-324309
Hepatic manifestations of autoimmune rheumatic diseases ANNALS OF GASTROENTEROLOGY 2005, 18(3):309-324309 Review Hepatic manifestations of autoimmune rheumatic diseases Aspasia Soultati, S. Dourakis SUMMARY the association between primary autoimmune rheumatolog- ic disease and associated hepatic abnormalities and the Autoimmune rheumatic diseases including Systemic Lu- pharmaceutical interventions that are related to liver dam- pus Erythematosus, Rheumatoid Arthritis, Sjogrens syn- age are presented. drome, Myositis, Antiphospholipid Syndrome, Behcets syndrome, Scleroderma and Vasculitides have been associ- Key words: Connective Tissue Disease, Systemic Lupus Ery- ated with hepatic injury by virtue of multisystem immune thematosus, Rheumatoid Arthritis, Sjogrens syndrome, and inflammatory involvement. Liver involvement preva- Myositis, Giant-Cell Arteritis, Antiphospholipid Syndrome, lence, significance and specific hepatic pathology vary. Af- Behcets syndrome, Scleroderma, Vasculitis, Steatosis, Nod- ter careful exclusion of potentially hepatotoxic drugs or co- ular Regenerative Hyperplasia, portal hypertension, Autoim- incident viral hepatitis the question remains whether liver mune Hepatitis, Primary Biliary Cirrhosis, Primary Scleros- involvement emerges as a manifestation of generalized con- ing Cholangitis nective tissue disease or it reflects an underlying primary liver disease sharing an immunological mechanism. Com- 1. Introduction monly recognised features include mild elevation of liver A variety of autoimmune rheumatic diseases -

Acitretin for Hypertrophic Lichen Planus Like Reaction in a Burn Scar
THE CUTTING EDGE SECTION EDITOR: GEORGE J. HRUZA, MD; ASSISTANT SECTION EDITORS: LYNN A. CORNELIUS, MD; JON STARR, MD Acitretin for Hypertrophic Lichen Planus–Like Reaction in a Burn Scar Steven Kossard, FACD; Phillip Artemi, FACD; Skin and Cancer Foundation Australia, Sydney The Cutting Edge: Challenges in Medical and Surgical Therapeutics REPORT OF A CASE men showed changes consistent with an early well- differentiated squamous cell carcinoma. A 60-year-old-man sustained a burn in childhood on the lower part of his right leg in a fire in a haystack. The area THERAPEUTIC CHALLENGE healed and remained as a stable scar for 50 years. Four months before presentation, he developed a series of hy- Squamous cell carcinoma may develop in the setting of pertrophic papules and plaques measuring up to 12 cm either a long-standing burn scar or hypertrophic lichen in diameter localized to the burn scar (Figure 1). The planus. Immunosuppressive agents, such as systemic cor- individual lesions were violaceous and hyperkeratotic. ticosteroids or cyclosporin, are used to treat lichen pla- There were no similar lesions at other skin sites or in- nus but inhibit cell-mediated immune responses that play volvement of his mucous membranes. The patient was a vital role in inhibiting the progression of skin cancers. taking warfarin sodium and digoxin, and 2 months after Clearly, the use of immunosuppressive drugs in our pa- the onset of his skin lesions, he began taking lisinopril tient, who had both a long-standing burn scar and le- for hypertension. sions resembling hypertrophic lichen planus, posed a po- Over the following 5 months, 4 skin biopsy speci- tential risk of enhancing tumor growth.