Gastric Varices Secondary to Splenic Vein Occlusion Due to Pancreatic
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Splenic Artery Embolization for the Treatment of Gastric Variceal Bleeding Secondary to Splenic Vein Thrombosis Complicated by Necrotizing Pancreatitis: Report of a Case
Hindawi Publishing Corporation Case Reports in Medicine Volume 2016, Article ID 1585926, 6 pages http://dx.doi.org/10.1155/2016/1585926 Case Report Splenic Artery Embolization for the Treatment of Gastric Variceal Bleeding Secondary to Splenic Vein Thrombosis Complicated by Necrotizing Pancreatitis: Report of a Case Hee Joon Kim, Eun Kyu Park, Young Hoe Hur, Yang Seok Koh, and Chol Kyoon Cho Department of Surgery, Chonnam National University Medical School, Gwangju, Republic of Korea Correspondence should be addressed to Chol Kyoon Cho; [email protected] Received 11 August 2016; Accepted 1 November 2016 Academic Editor: Omer Faruk Dogan Copyright © 2016 Hee Joon Kim et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Splenic vein thrombosis is a relatively common finding in pancreatitis. Gastric variceal bleeding is a life-threatening complication of splenic vein thrombosis, resulting from increased blood flow to short gastric vein. Traditionally, splenectomy is considered the treatment of choice. However, surgery in necrotizing pancreatitis is dangerous, because of severe inflammation, adhesion, and bleeding tendency. In the Warshaw operation, gastric variceal bleeding is rare, even though splenic vein is resected. Because the splenic artery is also resected, blood flow to short gastric vein is not increased problematically. Herein, we report a case of gastric variceal bleeding secondary to splenic vein thrombosis complicated by necrotizing pancreatitis successfully treated with splenic artery embolization. Splenic artery embolization could be the best treatment option for gastric variceal bleeding when splenectomy is difficult such as in case associated with severe acute pancreatitis or associated with severe adhesion or in patients withhigh operation risk. -

General Signs and Symptoms of Abdominal Diseases
General signs and symptoms of abdominal diseases Dr. Förhécz Zsolt Semmelweis University 3rd Department of Internal Medicine Faculty of Medicine, 3rd Year 2018/2019 1st Semester • For descriptive purposes, the abdomen is divided by imaginary lines crossing at the umbilicus, forming the right upper, right lower, left upper, and left lower quadrants. • Another system divides the abdomen into nine sections. Terms for three of them are commonly used: epigastric, umbilical, and hypogastric, or suprapubic Common or Concerning Symptoms • Indigestion or anorexia • Nausea, vomiting, or hematemesis • Abdominal pain • Dysphagia and/or odynophagia • Change in bowel function • Constipation or diarrhea • Jaundice “How is your appetite?” • Anorexia, nausea, vomiting in many gastrointestinal disorders; and – also in pregnancy, – diabetic ketoacidosis, – adrenal insufficiency, – hypercalcemia, – uremia, – liver disease, – emotional states, – adverse drug reactions – Induced but without nausea in anorexia/ bulimia. • Anorexia is a loss or lack of appetite. • Some patients may not actually vomit but raise esophageal or gastric contents in the absence of nausea or retching, called regurgitation. – in esophageal narrowing from stricture or cancer; also with incompetent gastroesophageal sphincter • Ask about any vomitus or regurgitated material and inspect it yourself if possible!!!! – What color is it? – What does the vomitus smell like? – How much has there been? – Ask specifically if it contains any blood and try to determine how much? • Fecal odor – in small bowel obstruction – or gastrocolic fistula • Gastric juice is clear or mucoid. Small amounts of yellowish or greenish bile are common and have no special significance. • Brownish or blackish vomitus with a “coffee- grounds” appearance suggests blood altered by gastric acid. -

Congestive Cholecystopathy; a Frequent Sonographic Sign of Evolving Esophageal Varices in Cirrhotics
Congestive Cholecystopathy; A Frequent Sonographic Sign of Evolving Esophageal Varices in Cirrhotics KHALID REHMAN YOUSAF, MIAN SAJID NISAR*, SALMAN ATIQ, AZHAR HUSSAIN*, AMNA RIZVI*, M. ISMAIL KHALID YOUSAF, ZAHID MANSOOR. Departments of Radiology and * Medicine, Omer Hospital, Lahore, Pakistan. Correspondence to Dr. Khalid Rehman Yousaf, Radiologist, New Radiology Department, SIMS/ S.H.L. Cell 923009458404 Email: [email protected] ABSTRACT Background: Gallbladder wall congestion (congestive cholecystopathy) is frequent sonographic feature demonstrated in patients with chronic liver disease. Hypoalbuminemia is still considered as a most probable cause of gallbladder wall thickness in cirrhotics. Objective: To demonstrate and establish congestive cholecystopathy as a consistent sonographic sign of developing portal hypertension and its association with evolving esophageal varices in Child’s class B (compensated) and C (decompensated) cirrhotic patients. Methodology: This cross-sectional study was conducted in Department of Radiology in collaboration with Department of Medicine, Omer Hospital, Lahore, between September 2009 and January 2011. We included 103 randomly sampled cirrhotic patients (67 men, 36 women; age range 38-79 years) who were clinically categorized into Class B and Class C liver disease through modified Child Pugh Classification. Upper gastrointestinal video endoscopy was performed for assessment of esophageal varices in all patients according to Japanese Research Society. Gall bladder targeted transabdominal ultrasound was performed on gray scale as well as color Doppler. Gallbladder wall thickness (4mm as a reference upper normal limit), pattern of wall thickening (striated or non-striated) and flow in wall were evaluated. Results: Out of 103 patients, 57 (55.3%) cases were of Child’s B and 46 (44.7%) of Child’s C class. -

Editorial Has the Time Come for Cyanoacrylate Injection to Become the Standard-Of-Care for Gastric Varices?
Tropical Gastroenterology 2010;31(3):141–144 Editorial Has the time come for cyanoacrylate injection to become the standard-of-care for gastric varices? Radha K. Dhiman, Narendra Chowdhry, Yogesh K Chawla The prevalence of gastric varices varies between 5% and 33% among patients with portal Department of Hepatology, hypertension with a reported incidence of bleeding of about 25% in 2 years and with a higher Postgraduate Institute of Medical bleeding incidence for fundal varices.1 Risk factors for gastric variceal hemorrhage include the education Research (PGIMER), size of fundal varices [more with large varices (as >10 mm)], Child class (C>B>A), and endoscopic Chandigarh, India presence of variceal red spots (defined as localized reddish mucosal area or spots on the mucosal surface of a varix).2 Gastric varices bleed less commonly as compared to esophageal Correspondence: Dr. Radha K. Dhiman, varices (25% versus 64%, respectively) but they bleed more severely, require more blood E-mail: [email protected] transfusions and are associated with increased mortality.3,4 The approach to optimal treatment for gastric varices remains controversial due to a lack of large, randomized, controlled trials and no clear clinical consensus. The endoscopic treatment modalities depend to a large extent on an accurate categorization of gastric varices. This classification categorizes gastric varices on the basis of their location in the stomach and their relationship with esophageal varices.1,5 Gastroesophageal varices are associated with varices along -

The Anatomy of Th-E Blood Vascular System of the Fox ,Squirrel
THE ANATOMY OF TH-E BLOOD VASCULAR SYSTEM OF THE FOX ,SQUIRREL. §CIURUS NlGER. .RUFIVENTEB (OEOEEROY) Thai: for the 009m of M. S. MICHIGAN STATE COLLEGE Thomas William Jenkins 1950 THulS' ifliillifllfllilllljllljIi\Ill\ljilllHliLlilHlLHl This is to certifg that the thesis entitled The Anatomy of the Blood Vascular System of the Fox Squirrel. Sciurus niger rufiventer (Geoffroy) presented by Thomas William Jenkins has been accepted towards fulfillment of the requirements for A degree in MEL Major professor Date May 23’ 19500 0-169 q/m Np” THE ANATOMY OF THE BLOOD VASCULAR SYSTEM OF THE FOX SQUIRREL, SCIURUS NIGER RUFIVENTER (GEOFFROY) By THOMAS WILLIAM JENKINS w L-Ooffi A THESIS Submitted to the School of Graduate Studies of Michigan State College of Agriculture and Applied Science in partial fulfillment of the requirements for the degree of MASTER OF SCIENCE Department of Zoology 1950 \ THESlSfi ACKNOWLEDGMENTS Grateful acknowledgment is made to the following persons of the Zoology Department: Dr. R. A. Fennell, under whose guidence this study was completed; Mr. P. A. Caraway, for his invaluable assistance in photography; Dr. D. W. Hayne and Mr. Poff, for their assistance in trapping; Dr. K. A. Stiles and Dr. R. H. Manville, for their helpful suggestions on various occasions; Mrs. Bernadette Henderson (Miss Mac), for her pleasant words of encouragement and advice; Dr. H. R. Hunt, head of the Zoology Department, for approval of the research problem; and Mr. N. J. Mizeres, for critically reading the manuscript. Special thanks is given to my wife for her assistance with the drawings and constant encouragement throughout the many months of work. -
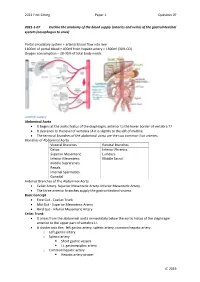
Arteries and Veins) of the Gastrointestinal System (Oesophagus to Anus)
2021 First Sitting Paper 1 Question 07 2021-1-07 Outline the anatomy of the blood supply (arteries and veins) of the gastrointestinal system (oesophagus to anus) Portal circulatory system + arterial blood flow into liver 1100ml of portal blood + 400ml from hepatic artery = 1500ml (30% CO) Oxygen consumption – 20-35% of total body needs Arterial Supply Abdominal Aorta • It begins at the aortic hiatus of the diaphragm, anterior to the lower border of vertebra T7. • It descends to the level of vertebra L4 it is slightly to the left of midline. • The terminal branches of the abdominal aorta are the two common iliac arteries. Branches of Abdominal Aorta Visceral Branches Parietal Branches Celiac. Inferior Phrenics. Superior Mesenteric. Lumbars Inferior Mesenteric. Middle Sacral. Middle Suprarenals. Renals. Internal Spermatics. Gonadal Anterior Branches of The Abdominal Aorta • Celiac Artery. Superior Mesenteric Artery. Inferior Mesenteric Artery. • The three anterior branches supply the gastrointestinal viscera. Basic Concept • Fore Gut - Coeliac Trunk • Mid Gut - Superior Mesenteric Artery • Hind Gut - Inferior Mesenteric Artery Celiac Trunk • It arises from the abdominal aorta immediately below the aortic hiatus of the diaphragm anterior to the upper part of vertebra LI. • It divides into the: left gastric artery, splenic artery, common hepatic artery. o Left gastric artery o Splenic artery ▪ Short gastric vessels ▪ Lt. gastroepiploic artery o Common hepatic artery ▪ Hepatic artery proper JC 2019 2021 First Sitting Paper 1 Question 07 • Left hepatic artery • Right hepatic artery ▪ Gastroduodenal artery • Rt. Gastroepiploic (gastro-omental) artery • Sup pancreatoduodenal artery • Supraduodenal artery Oesophagus • Cervical oesophagus - branches from inferior thyroid artery • Thoracic oesophagus - branches from bronchial arteries and aorta • Abd. -

Correlation of Portal Vein Size with Esophageal Varices Severity in Patients with Cirrhosis of Liver with Portal Hypertension
International Journal of Scientific and Research Publications, Volume 5, Issue 1, January 2015 1 ISSN 2250-3153 Correlation of Portal Vein Size with Esophageal Varices Severity in Patients with Cirrhosis of Liver with Portal Hypertension. Dr. K.V.L. Sudha Rani*, Dr. B. Sudarsi**, Dr. R. Siddeswari***, Dr. S. Manohar, **** * M.D., Asst. Prof. of Medicine ** M.D., Asst Prof. of Medicine *** M.D., Prof. of Medicine ****M.D., Prof. & HOD of Medicine. Abstract- This study was conducted to correlate the portal vein Complications of cirrhosis include portal hypertension, diameter measured by ultrasound to development of oesophageal spontaneous bacterial peritonitis, hepato renal syndrome, hepatic varices in patients with cirrhosis of liver with portal encephalopathy and hematological abnormalities. hypertension. Portal vein is formed by confluence of superior mesenteric 92 patients with cirrhosis admitted in OGH were selected for vein and splenic vein. Portal hypertension is defined as elevation the study USG was conducted in all patients to note portal vein of hepatic venous pressure gradient more than 5 mmHg. Portal size and splenic size. Upper GI endoscopy was done to detect hypertension is caused by. 1) Increased intra hepatic resistance to presence of varices with different grades. passage of blood flow through the liver due to cirrhosis and 2) In this study 65 patients had varices. Out of 65 patients 30 increased splanchnic blood flow secondary to vasodilation with had large varices (Grade III & IV) of 65 patients, 53 patients in splanchnic vascular bed. with varices have portal vein diameter > 13 mm patients, with Congestive splenomegaly is common in patients with portal small varices and those without varices portal vein diameter is < hypertension. -

Chapter 156: Upper Gastrointestinal Bleeding
8/23/2018 Principles and Practice of Hospital Medicine, 2e > Chapter 156: Upper Gastrointestinal Bleeding Stephen R. Rotman; John R. Saltzman INTRODUCTION Key Clinical Questions What is the timing and treatment of peptic ulcer disease? What are the factors in diagnosis and treatment of aortoenteric fistula? What treatments are available for each etiology of upper GI bleeding? What is the appropriate management and follow-up of variceal bleeding? How do you estimate the severity of bleeding so that you can triage appropriate patients to the ICU, medical floor, or observation unit? Which patients are more likely to rebleed and hence require continued observation in the hospital aer their bleeding has apparently stopped, and for how long? Upper gastrointestinal (GI) bleeding is responsible for over 300,000 hospitalizations per year in the United States. An additional 100,000 to 150,000 patients develop upper GI bleeding during hospitalizations. The annual cost of treating nonvariceal acute upper GI bleeding in the United States exceeds $7 billion. Upper GI bleeding is defined as a bleeding source in the GI tract proximal to the ligament of Treitz. The presentation varies depending on the nature and severity of bleeding and includes hematemesis, melena, hematochezia (in rapid upper GI bleeding), and anemia with heme-positive stools. Bleeding can be associated with changes in vital signs, including tachycardia and hypotension including orthostatic hypotension. Given the range of presentations, pinpointing the nature and severity of GI bleeding may be a challenging task. The natural history of nonvariceal upper GI bleeding is that 80% of patients will stop bleeding spontaneously and no further urgent intervention will be needed. -

Banana May Be Forbidden After Endoscopic Variceal Ligation: a Case Report
Case Report Banana may be forbidden after endoscopic variceal ligation: a case report Yingying Li1,2#, Xiaozhong Guo1#, Zhaohui Bai1,3, Xiaodong Shao1, Ran Wang1, Hongyu Li1, Xingshun Qi1 1Department of Gastroenterology, General Hospital of Northern Theater Command (formerly General Hospital of Shenyang Military Area), Shenyang 110840, China; 2Postgraduate College, Jinzhou Medical University, Jinzhou 121001, China; 3Postgraduate College, Shenyang Pharmaceutical University, Shenyang 110840, China #These authors contributed equally to this work. Correspondence to: Dr. Xingshun Qi, MD; Prof. Hongyu Li. General Hospital of Northern Theater Command (formerly General Hospital of Shenyang Military Area), No. 83 Wenhua Road, Shenyang 110840, China. Email: [email protected]; [email protected]. Abstract: Acute variceal hemorrhage (AVH) is a devastating complication of liver cirrhosis. Endoscopic variceal ligation (EVL) is a useful endoscopic treatment for AVH with few complications. However, the issue regarding management of early re-bleeding after EVL still needs to be concerned. Furthermore, the dietary principle after EVL is unclear. There is no consensus regarding what food should be eaten after EVL. In this paper, we reported a patient who ate a banana after an EVL and then developed early re-bleeding episodes. Keywords: Endoscopic variceal ligation (EVL); portal hypertension; banana; re-bleeding; dietary Received: 02 November 2018; Accepted: 27 January 2019; Published: 20 February 2019. doi: 10.21037/tgh.2019.01.11 View this article at: http://dx.doi.org/10.21037/tgh.2019.01.11 Introduction Case presentation Acute variceal hemorrhage (AVH) is a lethal consequence On May 24, 2018, a 41-year-old male was admitted to of portal hypertension in liver cirrhosis patients (1,2). -

Overview of Esophageal and Gastric Varices
pISSN 2287-2728 eISSN 2287-285X https://doi.org/10.3350/cmh.2020.0022 Review Clinical and Molecular Hepatology 2020;26:444-460 Managing liver cirrhotic complications: Overview of esophageal and gastric varices Cosmas Rinaldi Adithya Lesmana1,2, Monica Raharjo1, and Rino A. Gani1 1Division of Hepatobiliary, Department of Internal Medicine, Dr. Cipto Mangunkusumo National General Hospital, Medical Faculty Universitas Indonesia, Jakarta; 2Digestive Disease & GI Oncology Centre, Medistra Hospital, Jakarta, Indonesia Managing liver cirrhosis in clinical practice is still a challenging problem as its progression is associated with serious complications, such as variceal bleeding that may increase mortality. Portal hypertension (PH) is the main key for the development of liver cirrhosis complications. Portal pressure above 10 mmHg, termed as clinically significant portal hypertension, is associated with formation of varices; meanwhile, portal pressure above 12 mmHg is associated with variceal bleeding. Hepatic vein pressure gradient measurement and esophagogastroduodenoscopy remain the gold standard for assessing portal pressure and detecting varices. Recently, non-invasive methods have been studied for evaluation of portal pressure and varices detection in liver cirrhotic patients. Various guidelines have been published for clinicians’ guidance in the management of esophagogastric varices which aims to prevent development of varices, acute variceal bleeding, and variceal rebleeding. This writing provides a comprehensive review on development of PH and varices in liver cirrhosis patients and its management based on current international guidelines and real experience in Indonesia. (Clin Mol Hepatol 2020;26:444-460) Keywords: Liver cirrhosis; Hypertension, Portal; Esophageal and gastric varices INTRODUCTION tes, hepatic encephalopathy, coagulation dysfunction, hepatorenal syndrome, and even cardiac and pulmonary complications. -

Dr. ALSHIKH YOUSSEF Haiyan
Dr. ALSHIKH YOUSSEF Haiyan General features The peritoneum is a thin serous membrane Consisting of: 1- Parietal peritoneum -lines the ant. Abdominal wall and the pelvis 2- Visceral peritoneum - covers the viscera 3- Peritoneal cavity - the potential space between the parietal and visceral layer of peritoneum - in male, is a closed sac - but in the female, there is a communication with the exterior through the uterine tubes, the uterus, and the vagina ▪ Peritoneum cavity divided into Greater sac Lesser sac Communication between them by the epiploic foramen The peritoneum The peritoneal cavity is the largest one in the body. Divided into tow sac : .Greater sac; extends from diaphragm down to the pelvis. Lesser Sac .Lesser sac or omental bursa; lies behind the stomach. .Both cavities are interconnected through the epiploic foramen(winslow ). .In male : the peritoneum is a closed sac . .In female : the sac is not completely closed because it Greater Sac communicates with the exterior through the uterine tubes, uterus and vagina. Peritoneum in transverse section The relationship between viscera and peritoneum Intraperitoneal viscera viscera is almost totally covered with visceral peritoneum example, stomach, 1st & last inch of duodenum, jejunum, ileum, cecum, vermiform appendix, transverse and sigmoid colons, spleen and ovary Intraperitoneal viscera Interperitoneal viscera Retroperitoneal viscera Interperitoneal viscera Such organs are not completely wrapped by peritoneum one surface attached to the abdominal walls or other organs. Example liver, gallbladder, urinary bladder and uterus Upper part of the rectum, Ascending and Descending colon Retroperitoneal viscera some organs lie on the posterior abdominal wall Behind the peritoneum they are partially covered by peritoneum on their anterior surfaces only Example kidney, suprarenal gland, pancreas, upper 3rd of rectum duodenum, and ureter, aorta and I.V.C The Peritoneal Reflection The peritoneal reflection include: omentum, mesenteries, ligaments, folds, recesses, pouches and fossae. -

Vessels and Circulation
CARDIOVASCULAR SYSTEM OUTLINE 23.1 Anatomy of Blood Vessels 684 23.1a Blood Vessel Tunics 684 23.1b Arteries 685 23.1c Capillaries 688 23 23.1d Veins 689 23.2 Blood Pressure 691 23.3 Systemic Circulation 692 Vessels and 23.3a General Arterial Flow Out of the Heart 693 23.3b General Venous Return to the Heart 693 23.3c Blood Flow Through the Head and Neck 693 23.3d Blood Flow Through the Thoracic and Abdominal Walls 697 23.3e Blood Flow Through the Thoracic Organs 700 Circulation 23.3f Blood Flow Through the Gastrointestinal Tract 701 23.3g Blood Flow Through the Posterior Abdominal Organs, Pelvis, and Perineum 705 23.3h Blood Flow Through the Upper Limb 705 23.3i Blood Flow Through the Lower Limb 709 23.4 Pulmonary Circulation 712 23.5 Review of Heart, Systemic, and Pulmonary Circulation 714 23.6 Aging and the Cardiovascular System 715 23.7 Blood Vessel Development 716 23.7a Artery Development 716 23.7b Vein Development 717 23.7c Comparison of Fetal and Postnatal Circulation 718 MODULE 9: CARDIOVASCULAR SYSTEM mck78097_ch23_683-723.indd 683 2/14/11 4:31 PM 684 Chapter Twenty-Three Vessels and Circulation lood vessels are analogous to highways—they are an efficient larger as they merge and come closer to the heart. The site where B mode of transport for oxygen, carbon dioxide, nutrients, hor- two or more arteries (or two or more veins) converge to supply the mones, and waste products to and from body tissues. The heart is same body region is called an anastomosis (ă-nas ′tō -mō′ sis; pl., the mechanical pump that propels the blood through the vessels.