Dr. ALSHIKH YOUSSEF Haiyan
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Splenic Artery Embolization for the Treatment of Gastric Variceal Bleeding Secondary to Splenic Vein Thrombosis Complicated by Necrotizing Pancreatitis: Report of a Case
Hindawi Publishing Corporation Case Reports in Medicine Volume 2016, Article ID 1585926, 6 pages http://dx.doi.org/10.1155/2016/1585926 Case Report Splenic Artery Embolization for the Treatment of Gastric Variceal Bleeding Secondary to Splenic Vein Thrombosis Complicated by Necrotizing Pancreatitis: Report of a Case Hee Joon Kim, Eun Kyu Park, Young Hoe Hur, Yang Seok Koh, and Chol Kyoon Cho Department of Surgery, Chonnam National University Medical School, Gwangju, Republic of Korea Correspondence should be addressed to Chol Kyoon Cho; [email protected] Received 11 August 2016; Accepted 1 November 2016 Academic Editor: Omer Faruk Dogan Copyright © 2016 Hee Joon Kim et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Splenic vein thrombosis is a relatively common finding in pancreatitis. Gastric variceal bleeding is a life-threatening complication of splenic vein thrombosis, resulting from increased blood flow to short gastric vein. Traditionally, splenectomy is considered the treatment of choice. However, surgery in necrotizing pancreatitis is dangerous, because of severe inflammation, adhesion, and bleeding tendency. In the Warshaw operation, gastric variceal bleeding is rare, even though splenic vein is resected. Because the splenic artery is also resected, blood flow to short gastric vein is not increased problematically. Herein, we report a case of gastric variceal bleeding secondary to splenic vein thrombosis complicated by necrotizing pancreatitis successfully treated with splenic artery embolization. Splenic artery embolization could be the best treatment option for gastric variceal bleeding when splenectomy is difficult such as in case associated with severe acute pancreatitis or associated with severe adhesion or in patients withhigh operation risk. -

A CASE REPORT and LITERATURE REVIEW Dr. P
Original Research Paper Volume - 7 | Issue - 6 | June - 2017 | ISSN - 2249-555X | IF : 4.894 | IC Value : 79.96 Medical Science COMBINED ANOMALLY OF RIGHT HEPATIC ARTERY & RIGHT HEPATIC DUCT IN CHOLESYSTECTOMY: A CASE REPORT AND LITERATURE REVIEW Dr. Pankaj Kumar MBBS, MS, Assistant Professor, Medical College Hospital, 88 College Street, Sarkar Kolkata, West Bengal MBBS, MS, RMO cum Clinical Tutor, Medical College Hospital, 88 College Street, Dr. Shibaji Basu Kolkata, West Bengal Dr. Shibsankar MBBS, MS, Associate Professor, Medical College Hospital, 88 College Street, Ray Chaudhury Kolkata, West Bengal ABSTRACT In contrast to the conventional belief that ligation & division of the cystic artery & duct almost completes the operation we would like to say dissection in gall bladder fossa also may be very dangerous. We are presenting a case here to show how dangerous gall bladder fossa may be after an easy Calot's Triangle dissection. A 45 year old female with a history of biliary colic was scheduled for open cholecystectomy. After dissection in Calot's triangle & removal of gall bladder from liver bed it was seen that the right hepatic artery travels a long extra- hepatic course through gall bladder fossa before entering the liver near thefundus of the gall bladder. The right hepatic duct also seen to travel an unusually long extra-hepatic coursethrough the gall bladder fossa before entering into the liver. The right hepatic duct was punctured with fine needle to confirm the presence of bile. KEYWORDS : open cholecystectomy, aberrant right hepatic artery, aberrant right hepatic duct INTRODUCTION the gall bladder after giving off the cystic artery branch. -

Dissertation
A STUDY OF PREVALENCE AND ASSOCIATION OF HYPOTHYROIDISM AND SERUM LIPID PROFILE IN DIAGNOSED GALL STONE DISEASE AT TERTIARY CARE HOSPITAL Dissertation Submitted to THE TAMILNADU Dr. M.G.R MEDICAL UNIVERSITY In partial fulfilment of the requirements for the award of the degree of M.S. GENERAL SURGERY Branch I MAY 2019 CERTIFICATE I This is to certify that this dissertation entitled “A Study of Prevalence and Association of Hypothyroidism and Serum Lipid profile in diagnosed Gall Stone Disease at Tertiary Care Hospital” is a bonafide record of the work done by Dr. Soumya Shree under the supervision and guidance of Dr. R. Maheswari, M.S., Professor, Department of General Surgery, Sree Mookambika Institute of Medical Sciences, Kulasekharam. This is submitted in partial fulfilment of the requirement of The Tamilnadu Dr. M.G.R. Medical University, Chennai for the award of M.S. Degree in General Surgery. Dr. R. Maheswari, M.S., Dr. S. Soundara Rajan, M.S., [Guide] Professor & HOD, Professor, Department Of General Surgery Department Of General Surgery Sree Mookambika Institute of Sree Mookambika Institute of Medical Sciences [SMIMS] Medical Sciences [SMIMS] Kulasekharam, K.K District, Kulasekharam, K.K District, Tamil Nadu -629161 Tamil Nadu -629161 Dr. Rema V. Nair, M.D., D.G.O., [Director] Sree Mookambika Institute of Medical Sciences [SMIMS] Kulasekharam, K.K District, Tamil Nadu -629161 CERTIFICATE II This is to certify that this dissertation work “A Study of Prevalence and Association of Hypothyroidism and Serum Lipid profile in diagnosed Gall Stone Disease at Tertiary Care Hospital” of the candidate Dr. Soumya Shree with registration Number 221611703 for the award of M.S. -
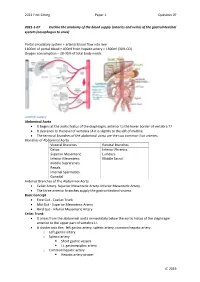
Arteries and Veins) of the Gastrointestinal System (Oesophagus to Anus)
2021 First Sitting Paper 1 Question 07 2021-1-07 Outline the anatomy of the blood supply (arteries and veins) of the gastrointestinal system (oesophagus to anus) Portal circulatory system + arterial blood flow into liver 1100ml of portal blood + 400ml from hepatic artery = 1500ml (30% CO) Oxygen consumption – 20-35% of total body needs Arterial Supply Abdominal Aorta • It begins at the aortic hiatus of the diaphragm, anterior to the lower border of vertebra T7. • It descends to the level of vertebra L4 it is slightly to the left of midline. • The terminal branches of the abdominal aorta are the two common iliac arteries. Branches of Abdominal Aorta Visceral Branches Parietal Branches Celiac. Inferior Phrenics. Superior Mesenteric. Lumbars Inferior Mesenteric. Middle Sacral. Middle Suprarenals. Renals. Internal Spermatics. Gonadal Anterior Branches of The Abdominal Aorta • Celiac Artery. Superior Mesenteric Artery. Inferior Mesenteric Artery. • The three anterior branches supply the gastrointestinal viscera. Basic Concept • Fore Gut - Coeliac Trunk • Mid Gut - Superior Mesenteric Artery • Hind Gut - Inferior Mesenteric Artery Celiac Trunk • It arises from the abdominal aorta immediately below the aortic hiatus of the diaphragm anterior to the upper part of vertebra LI. • It divides into the: left gastric artery, splenic artery, common hepatic artery. o Left gastric artery o Splenic artery ▪ Short gastric vessels ▪ Lt. gastroepiploic artery o Common hepatic artery ▪ Hepatic artery proper JC 2019 2021 First Sitting Paper 1 Question 07 • Left hepatic artery • Right hepatic artery ▪ Gastroduodenal artery • Rt. Gastroepiploic (gastro-omental) artery • Sup pancreatoduodenal artery • Supraduodenal artery Oesophagus • Cervical oesophagus - branches from inferior thyroid artery • Thoracic oesophagus - branches from bronchial arteries and aorta • Abd. -

Vessels and Circulation
CARDIOVASCULAR SYSTEM OUTLINE 23.1 Anatomy of Blood Vessels 684 23.1a Blood Vessel Tunics 684 23.1b Arteries 685 23.1c Capillaries 688 23 23.1d Veins 689 23.2 Blood Pressure 691 23.3 Systemic Circulation 692 Vessels and 23.3a General Arterial Flow Out of the Heart 693 23.3b General Venous Return to the Heart 693 23.3c Blood Flow Through the Head and Neck 693 23.3d Blood Flow Through the Thoracic and Abdominal Walls 697 23.3e Blood Flow Through the Thoracic Organs 700 Circulation 23.3f Blood Flow Through the Gastrointestinal Tract 701 23.3g Blood Flow Through the Posterior Abdominal Organs, Pelvis, and Perineum 705 23.3h Blood Flow Through the Upper Limb 705 23.3i Blood Flow Through the Lower Limb 709 23.4 Pulmonary Circulation 712 23.5 Review of Heart, Systemic, and Pulmonary Circulation 714 23.6 Aging and the Cardiovascular System 715 23.7 Blood Vessel Development 716 23.7a Artery Development 716 23.7b Vein Development 717 23.7c Comparison of Fetal and Postnatal Circulation 718 MODULE 9: CARDIOVASCULAR SYSTEM mck78097_ch23_683-723.indd 683 2/14/11 4:31 PM 684 Chapter Twenty-Three Vessels and Circulation lood vessels are analogous to highways—they are an efficient larger as they merge and come closer to the heart. The site where B mode of transport for oxygen, carbon dioxide, nutrients, hor- two or more arteries (or two or more veins) converge to supply the mones, and waste products to and from body tissues. The heart is same body region is called an anastomosis (ă-nas ′tō -mō′ sis; pl., the mechanical pump that propels the blood through the vessels. -

Portal Hypertensionand Its Radiological Investigation
Postgrad Med J: first published as 10.1136/pgmj.39.451.299 on 1 May 1963. Downloaded from POSTGRAD. MED. J. (I963), 39, 299 PORTAL HYPERTENSION AND ITS RADIOLOGICAL INVESTIGATION J. H. MIDDLEMISS, M.D., F.F.R., D.M.R.D. F. G. M. Ross, M.B., B.Ch., B.A.O., F.F.R., D.M.R.D. From the Department of Radiodiagnosis, United Bristol Hospitals PORTAL hypertension is a condition in which there branch of the portal vein but may drain into the right is an blood in the branch. abnormally high pressure Small veins which are present on the serosal surface portal system of veins which eventually leads to of the liver and in the surrounding peritoneal folds splenomegaly and in chronic cases, to haematem- draining the diaphragm and stomach are known as esis and melaena. accessory portal veins. They may unite with the portal The circulation is in that it vein or enter the liver independently. portal unique The hepatic artery arises normally from the coeliac exists between two sets of capillaries, i.e. the axis but it may arise as a separate trunk from the aorta. capillaries of the spleen, pancreas, gall-bladder It runs upwards and to the right and divides into a and most of the gastro-intestinal tract on the left and right branch before entering the liver at the one hand and the sinusoids of the liver on the porta hepatis. The venous return starts as small thin-walled branches other hand. The liver parallels the lungs in that in the centre of the lobules in the liver. -

The Diameter of the Originating Vein Determines Esophageal and Gastric Fundic Varices in Portal Hypertension Secondary to Posthepatitic Cirrhosis
CLINICS 2012;67(6):609-614 DOI:10.6061/clinics/2012(06)11 CLINICAL SCIENCE The diameter of the originating vein determines esophageal and gastric fundic varices in portal hypertension secondary to posthepatitic cirrhosis Hai-ying Zhou, Tian-wu Chen, Xiao-ming Zhang, Li-ying Wang, Li Zhou, Guo-li Dong, Nan-lin Zeng, Hang Li, Xiao-li Chen, Rui Li Sichuan Key Laboratory of Medical Imaging, and Department of Radiology, Affiliated Hospital of North Sichuan Medical College, Sichuan/China. OBJECTIVE: The aim of this study was to determine whether and how the diameter of the vein that gives rise to the inflowing vein of the esophageal and gastric fundic varices secondary to posthepatitic cirrhosis, as measured with multidetector-row computed tomography, could predict the varices and their patterns. METHODS: A total of 106 patients with posthepatitic cirrhosis underwent multidetector-row computed tomography. Patients with and without esophageal and gastric fundic varices were enrolled in Group 1 and Group 2, respectively. Group 1 was composed of Subgroup A, consisting of patients with varices, and Subgroup B consisted of patients with varices in combination with portal vein-inferior vena cava shunts. The diameters of the originating veins of veins entering the varices were reviewed and statistically analyzed. RESULTS: The originating veins were the portal vein in 8% (6/75) of patients, the splenic vein in 65.3% (49/75) of patients, and both the portal and splenic veins in 26.7% (20/75) of patients. The splenic vein diameter in Group 1 was larger than that in Group 2, whereas no differences in portal vein diameters were found between groups. -

Ligaments -Two-Layered Folds of Peritoneum That Attached the Lesser Mobile Solid Viscera to the Abdominal Wall
Ingegneria delle tecnologie per la salute Fondamenti di anatomia e istologia aa. 2019-20 Lesson 7. Digestive system and peritoneum Peritoneum, abdominal vessel and spleen PERITONEUM: General features = a thin serous membrane that line walls of abdominal and pelvic cavities and cover organs within these cavities •Parietal peritoneum -lines walls of abdominal and pelvic cavities •Visceral peritoneum -covers organs •Peritoneal cavity - potential space between parietal and visceral layer of peritoneum, in male, is a closed sac, but in female, there is a communication with exterior through uterine tubes, uterus, and vagina Function • Secretes a lubricating serous fluid that continuously moistens associated organs • Absorb • Support viscera Peritoneum Histology The peritoneum is a serosal membrane that consists of a single layer of mesothelial cells and is supported by a basement membrane. The layer is attached to the body wall and viscera by a glycosaminoglycan matrix that contains collagen fibers, vessels, nerves, macrophages, and fat cells. relationship between viscera and peritoneum • Intraperitoneal viscera -viscera completely surrounded by peritoneum, example, stomach, superior part of duodenum, jejunum, ileum, cecum, vermiform appendix, transverse and sigmoid colons, spleen and ovary • Interperitoneal viscera -most part of viscera surrounded by peritoneum, example, liver, gallbladder, ascending and descending colon, upper part of rectum, urinary bladder and uterus • Retroperitoneal viscera -some organs lie on the posterior abdominal -

Normal Gross and Histologic Features of the Gastrointestinal Tract
NORMAL GROSS AND HISTOLOGIC 1 FEATURES OF THE GASTROINTESTINAL TRACT THE NORMAL ESOPHAGUS left gastric, left phrenic, and left hepatic accessory arteries. Veins in the proximal and mid esopha- Anatomy gus drain into the systemic circulation, whereas Gross Anatomy. The adult esophagus is a the short gastric and left gastric veins of the muscular tube measuring approximately 25 cm portal system drain the distal esophagus. Linear and extending from the lower border of the cri- arrays of large caliber veins are unique to the distal coid cartilage to the gastroesophageal junction. esophagus and can be a helpful clue to the site of It lies posterior to the trachea and left atrium a biopsy when extensive cardiac-type mucosa is in the mediastinum but deviates slightly to the present near the gastroesophageal junction (4). left before descending to the diaphragm, where Lymphatic vessels are present in all layers of the it traverses the hiatus and enters the abdomen. esophagus. They drain to paratracheal and deep The subdiaphragmatic esophagus lies against cervical lymph nodes in the cervical esophagus, the posterior surface of the left hepatic lobe (1). bronchial and posterior mediastinal lymph nodes The International Classification of Diseases in the thoracic esophagus, and left gastric lymph and the American Joint Commission on Cancer nodes in the abdominal esophagus. divide the esophagus into upper, middle, and lower thirds, whereas endoscopists measure distance to points in the esophagus relative to the incisors (2). The esophagus begins 15 cm from the incisors and extends 40 cm from the incisors in the average adult (3). The upper and lower esophageal sphincters represent areas of increased resting tone but lack anatomic landmarks; they are located 15 to 18 cm from the incisors and slightly proximal to the gastroesophageal junction, respectively. -

Greater Omentum Connects the Greater Curvature of the Stomach to the Transverse Colon
Dr. ALSHIKH YOUSSEF Haiyan General features The peritoneum is a thin serous membrane Consisting of: 1- Parietal peritoneum -lines the ant. Abdominal wall and the pelvis 2- Visceral peritoneum - covers the viscera 3- Peritoneal cavity - the potential space between the parietal and visceral layer of peritoneum - in male, is a closed sac - but in the female, there is a communication with the exterior through the uterine tubes, the uterus, and the vagina ▪ Peritoneum cavity divided into Greater sac Lesser sac Communication between them by the epiploic foramen The peritoneum The peritoneal cavity is the largest one in the body. Divided into tow sac : .Greater sac; extends from diaphragm down to the pelvis. Lesser Sac .Lesser sac or omental bursa; lies behind the stomach. .Both cavities are interconnected through the epiploic foramen(winslow ). .In male : the peritoneum is a closed sac . .In female : the sac is not completely closed because it Greater Sac communicates with the exterior through the uterine tubes, uterus and vagina. Peritoneum in transverse section The relationship between viscera and peritoneum Intraperitoneal viscera viscera is almost totally covered with visceral peritoneum example, stomach, 1st & last inch of duodenum, jejunum, ileum, cecum, vermiform appendix, transverse and sigmoid colons, spleen and ovary Intraperitoneal viscera Interperitoneal viscera Retroperitoneal viscera Interperitoneal viscera Such organs are not completely wrapped by peritoneum one surface attached to the abdominal walls or other organs. Example liver, gallbladder, urinary bladder and uterus Upper part of the rectum, Ascending and Descending colon Retroperitoneal viscera some organs lie on the posterior abdominal wall Behind the peritoneum they are partially covered by peritoneum on their anterior surfaces only Example kidney, suprarenal gland, pancreas, upper 3rd of rectum duodenum, and ureter, aorta and I.V.C The Peritoneal Reflection The peritoneal reflection include: omentum, mesenteries, ligaments, folds, recesses, pouches and fossae. -

CHAPTER 6 Perineum and True Pelvis
193 CHAPTER 6 Perineum and True Pelvis THE PELVIC REGION OF THE BODY Posterior Trunk of Internal Iliac--Its Iliolumbar, Lateral Sacral, and Superior Gluteal Branches WALLS OF THE PELVIC CAVITY Anterior Trunk of Internal Iliac--Its Umbilical, Posterior, Anterolateral, and Anterior Walls Obturator, Inferior Gluteal, Internal Pudendal, Inferior Wall--the Pelvic Diaphragm Middle Rectal, and Sex-Dependent Branches Levator Ani Sex-dependent Branches of Anterior Trunk -- Coccygeus (Ischiococcygeus) Inferior Vesical Artery in Males and Uterine Puborectalis (Considered by Some Persons to be a Artery in Females Third Part of Levator Ani) Anastomotic Connections of the Internal Iliac Another Hole in the Pelvic Diaphragm--the Greater Artery Sciatic Foramen VEINS OF THE PELVIC CAVITY PERINEUM Urogenital Triangle VENTRAL RAMI WITHIN THE PELVIC Contents of the Urogenital Triangle CAVITY Perineal Membrane Obturator Nerve Perineal Muscles Superior to the Perineal Sacral Plexus Membrane--Sphincter urethrae (Both Sexes), Other Branches of Sacral Ventral Rami Deep Transverse Perineus (Males), Sphincter Nerves to the Pelvic Diaphragm Urethrovaginalis (Females), Compressor Pudendal Nerve (for Muscles of Perineum and Most Urethrae (Females) of Its Skin) Genital Structures Opposed to the Inferior Surface Pelvic Splanchnic Nerves (Parasympathetic of the Perineal Membrane -- Crura of Phallus, Preganglionic From S3 and S4) Bulb of Penis (Males), Bulb of Vestibule Coccygeal Plexus (Females) Muscles Associated with the Crura and PELVIC PORTION OF THE SYMPATHETIC -

Abdominal Oesophagus, Stomach
ABDOMINAL OESOPHAGUS, STOMACH Dr. Zahiri Transpyloric plane An upper transverse line =Addison's Plane located halfway between the jugular notch and the upper border of the pubic symphysis It is also said to lie roughly a hand's breadth beneath the xiphoid process of the human sternum. (9th costal cartilages and the lower border of the L1) Dr. Maria Zahiri Structures crossed the fundus of the gallbladder the origin of the superior mesenteric artery (termination of the superior mesenteric vein) hilum of the kidney the root of the transverse mesocolon duodenojejunal flexure Dr. Maria Zahiri intertubercular plane (or transtubercular lower transverse line midway between the upper transverse and the upper border of the pubic symphysis passing through the iliac tubercles L5 Dr. Maria Zahiri subcostal plane is a transverse plane which bisects the body at the level of the costal margin L3 Dr. Maria Zahiri interspinous line Transumbilical line (L3- L4) Dr. Maria Zahiri Deep surface of the anterior abdominal wall 3 ligament & peritoneal fold 3 peritoneal fossae Dr. Maria Zahiri median umbilical ligament Remnant of the embryonic urachus. It extends from the apex of the bladder to the umbilicus It is covered by the median umbilical fold Dr. Maria Zahiri medial umbilical ligament = cord of umbilical artery is a paired structure is covered by the medial umbilical folds It represents the remnant of the fetal umbilical arteries used as a landmark for surgeons exploring the medial inguinal fossa during laparoscopic inguinal hernia repair. Dr. Maria Zahiri lateral umbilical fold overlies the inferior epigastric artery (a branch of the external iliac artery remain functional after birth It originates just medial to the deep inguinal ring Dr.