Residency Essentials Full Curriculum Syllabus
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Splenic Artery Embolization for the Treatment of Gastric Variceal Bleeding Secondary to Splenic Vein Thrombosis Complicated by Necrotizing Pancreatitis: Report of a Case
Hindawi Publishing Corporation Case Reports in Medicine Volume 2016, Article ID 1585926, 6 pages http://dx.doi.org/10.1155/2016/1585926 Case Report Splenic Artery Embolization for the Treatment of Gastric Variceal Bleeding Secondary to Splenic Vein Thrombosis Complicated by Necrotizing Pancreatitis: Report of a Case Hee Joon Kim, Eun Kyu Park, Young Hoe Hur, Yang Seok Koh, and Chol Kyoon Cho Department of Surgery, Chonnam National University Medical School, Gwangju, Republic of Korea Correspondence should be addressed to Chol Kyoon Cho; [email protected] Received 11 August 2016; Accepted 1 November 2016 Academic Editor: Omer Faruk Dogan Copyright © 2016 Hee Joon Kim et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Splenic vein thrombosis is a relatively common finding in pancreatitis. Gastric variceal bleeding is a life-threatening complication of splenic vein thrombosis, resulting from increased blood flow to short gastric vein. Traditionally, splenectomy is considered the treatment of choice. However, surgery in necrotizing pancreatitis is dangerous, because of severe inflammation, adhesion, and bleeding tendency. In the Warshaw operation, gastric variceal bleeding is rare, even though splenic vein is resected. Because the splenic artery is also resected, blood flow to short gastric vein is not increased problematically. Herein, we report a case of gastric variceal bleeding secondary to splenic vein thrombosis complicated by necrotizing pancreatitis successfully treated with splenic artery embolization. Splenic artery embolization could be the best treatment option for gastric variceal bleeding when splenectomy is difficult such as in case associated with severe acute pancreatitis or associated with severe adhesion or in patients withhigh operation risk. -

Hepatic Hydrothorax Without Apparent Ascites and Dyspnea - a Case Report
Case Report DOI: 10.7860/JCDR/2018/37185.12181 I nternal Medicine Hepatic Hydrothorax without Apparent S ection Ascites and Dyspnea - A Case Report JING HE1, RASHA HAYKAL2, HONGCHUAN COVILLE3, JAYA PRAKASH GADIKOTA4, CHRISTOPHER BRAY5 ABSTRACT A 78-year-old female with a past medical history of alcoholic cirrhosis was hospitalised with recurrent lower gastrointestinal bleeding due to rectal ulcers. The ulcers were successfully treated with cautery and placement of clips. However, a recurrent large right-sided pleural effusion without apparent ascites and dyspnea were found incidentally during the hospitalisation. The initial fluid analysis was exudate based on Light’s criteria with high protein. The fluid analysis was repeated five days later, after rapid reaccumulation which revealed transudates. Other causes of pleural effusion like heart failure, renal failure or primary pulmonary diseases were excluded. Hepatic hydrothorax was considered and the patient was started with the treatment of Furosemide and Spironolactone. The atypical presentation of hepatic hydrothorax may disguise the diagnosis and delay the treatment. Therefore, for a patient with recurrent, unexplained unilateral pleural effusions, even with atypical fluid characterisation and in the absence of ascites, hepatic hydrothorax should still remain on the top differential with underlying cirrhosis to ensure optimal treatment. Keywords: Cirrhosis, Light criteria, Liver, Pleural effusion CASE REPORT Haemogram Levels Normal range A 78-year-old Caucasian female, with a past medical history of alcoholic cirrhosis, admitted for recurrent rectal bleeding secondary WBC 6.9 (4.5-11.0 thousands/mm3) to rectal ulcers and was successfully treated with cautery and Neutrophils % 78 H (50.0-75.0 %) placement of clips. -

Section 8 Pulmonary Medicine
SECTION 8 PULMONARY MEDICINE 336425_ST08_286-311.indd6425_ST08_286-311.indd 228686 111/7/121/7/12 111:411:41 AAMM CHAPTER 66 EVALUATION OF CHRONIC COUGH 1. EPIDEMIOLOGY • Nearly all adult cases of chronic cough in nonsmokers who are not taking an ACEI can be attributed to the “Pathologic Triad of Chronic Cough” (asthma, GERD, upper airway cough syndrome [UACS; previously known as postnasal drip syndrome]). • ACEI cough is idiosyncratic, occurrence is higher in female than males 2. PATHOPHYSIOLOGY • Afferent (sensory) limb: chemical or mechanical stimulation of receptors on pharynx, larynx, airways, external auditory meatus, esophagus stimulates vagus and superior laryngeal nerves • Receptors upregulated in chronic cough • CNS: cough center in nucleus tractus solitarius • Efferent (motor) limb: expiratory and bronchial muscle contraction against adducted vocal cords increases positive intrathoracic pressure 3. DEFINITION • Subacute cough lasts between 3 and 8 weeks • Chronic cough duration is at least 8 weeks 4. DIFFERENTIAL DIAGNOSIS • Respiratory tract infection (viral or bacterial) • Asthma • Upper airway cough syndrome (postnasal drip syndrome) • CHF • Pertussis • COPD • GERD • Bronchiectasis • Eosinophilic bronchitis • Pulmonary tuberculosis • Interstitial lung disease • Bronchogenic carcinoma • Medication-induced cough 5. EVALUATION AND TREATMENT OF THE COMMON CAUSES OF CHRONIC COUGH • Upper airway cough syndrome: rhinitis, sinusitis, or postnasal drip syndrome • Presentation: symptoms of rhinitis, frequent throat clearing, itchy -
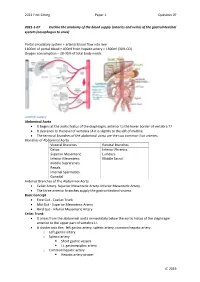
Arteries and Veins) of the Gastrointestinal System (Oesophagus to Anus)
2021 First Sitting Paper 1 Question 07 2021-1-07 Outline the anatomy of the blood supply (arteries and veins) of the gastrointestinal system (oesophagus to anus) Portal circulatory system + arterial blood flow into liver 1100ml of portal blood + 400ml from hepatic artery = 1500ml (30% CO) Oxygen consumption – 20-35% of total body needs Arterial Supply Abdominal Aorta • It begins at the aortic hiatus of the diaphragm, anterior to the lower border of vertebra T7. • It descends to the level of vertebra L4 it is slightly to the left of midline. • The terminal branches of the abdominal aorta are the two common iliac arteries. Branches of Abdominal Aorta Visceral Branches Parietal Branches Celiac. Inferior Phrenics. Superior Mesenteric. Lumbars Inferior Mesenteric. Middle Sacral. Middle Suprarenals. Renals. Internal Spermatics. Gonadal Anterior Branches of The Abdominal Aorta • Celiac Artery. Superior Mesenteric Artery. Inferior Mesenteric Artery. • The three anterior branches supply the gastrointestinal viscera. Basic Concept • Fore Gut - Coeliac Trunk • Mid Gut - Superior Mesenteric Artery • Hind Gut - Inferior Mesenteric Artery Celiac Trunk • It arises from the abdominal aorta immediately below the aortic hiatus of the diaphragm anterior to the upper part of vertebra LI. • It divides into the: left gastric artery, splenic artery, common hepatic artery. o Left gastric artery o Splenic artery ▪ Short gastric vessels ▪ Lt. gastroepiploic artery o Common hepatic artery ▪ Hepatic artery proper JC 2019 2021 First Sitting Paper 1 Question 07 • Left hepatic artery • Right hepatic artery ▪ Gastroduodenal artery • Rt. Gastroepiploic (gastro-omental) artery • Sup pancreatoduodenal artery • Supraduodenal artery Oesophagus • Cervical oesophagus - branches from inferior thyroid artery • Thoracic oesophagus - branches from bronchial arteries and aorta • Abd. -

Pathophysiology of Acid Base Balance: the Theory Practice Relationship
Intensive and Critical Care Nursing (2008) 24, 28—40 ORIGINAL ARTICLE Pathophysiology of acid base balance: The theory practice relationship Sharon L. Edwards ∗ Buckinghamshire Chilterns University College, Chalfont Campus, Newland Park, Gorelands Lane, Chalfont St. Giles, Buckinghamshire HP8 4AD, United Kingdom Accepted 13 May 2007 KEYWORDS Summary There are many disorders/diseases that lead to changes in acid base Acid base balance; balance. These conditions are not rare or uncommon in clinical practice, but every- Arterial blood gases; day occurrences on the ward or in critical care. Conditions such as asthma, chronic Acidosis; obstructive pulmonary disease (bronchitis or emphasaemia), diabetic ketoacidosis, Alkalosis renal disease or failure, any type of shock (sepsis, anaphylaxsis, neurogenic, cardio- genic, hypovolaemia), stress or anxiety which can lead to hyperventilation, and some drugs (sedatives, opoids) leading to reduced ventilation. In addition, some symptoms of disease can cause vomiting and diarrhoea, which effects acid base balance. It is imperative that critical care nurses are aware of changes that occur in relation to altered physiology, leading to an understanding of the changes in patients’ condition that are observed, and why the administration of some immediate therapies such as oxygen is imperative. © 2007 Elsevier Ltd. All rights reserved. Introduction the essential concepts of acid base physiology is necessary so that quick and correct diagnosis can The implications for practice with regards to be determined and appropriate treatment imple- acid base physiology are separated into respi- mented. ratory acidosis and alkalosis, metabolic acidosis The homeostatic imbalances of acid base are and alkalosis, observed in patients with differing examined as the body attempts to maintain pH bal- aetiologies. -

A STUDY of ANAMOLOUS ORIGIN of GLUTEAL ARTERIES IJCRR Section: Healthcare Sci
Research Article A STUDY OF ANAMOLOUS ORIGIN OF GLUTEAL ARTERIES IJCRR Section: Healthcare Sci. Journal Impact Factor Amudalapalli Siva Narayana1, M. Pramila Padmini2 4.016 1Tutor, Department of Anatomy, Gitam Institute of Medical Sciences Visakhapatnam, Andhrapradesh, India; 2Assistant Professor, Department of Anatomy, Gitam Institute of Medical Sciences, Visakhapatnam, Andhrapradesh, India. ABSTRACT Aim: The present study has been taken up to observe the branching pattern of internal iliac artery and its importance for the clinicians in their respective fields. Methodology: 45 pelvic halves were studied from dissected cadavers. The branches of gluteal arteries were traced carefully by separating the connective tissue surrounding the arteries. Result: In 4 cadavers, inferior gluteal artery was given off in the gluteal region, in 1 case it is given off from posterior division of internal iliac artery. In 1 case superior gluteal arose in common with internal pudendal artery. Conclusion: Vascular variations in the gluteal region are important for surgeons and anatomists. Key Words: Internal iliac artery, Gluteal arteries, Pelvic region, Internal pudendal artery INTRODUCTION The tributaries of internal iliac vein along with the main trunk were discarded to visualize the branches of IIA. Con- Each internal iliac artery is about 4 cm long and begins at the nective tissue surrounding the IIA was cleared. Parietal and common iliac bifurcation level with the intervertebral disc visceral branches were traced. Some of the branches of between L5 and S1 vertebrae and anterior to the sacroiliac IIA were traced till their exit from the pelvic cavity and are joint. As it passes downward across the brim of the pelvis it called parietal branches. -

Hepatic Hydrothorax: an Updated Review on a Challenging Disease
Lung (2019) 197:399–405 https://doi.org/10.1007/s00408-019-00231-6 REVIEW Hepatic Hydrothorax: An Updated Review on a Challenging Disease Toufc Chaaban1 · Nadim Kanj2 · Imad Bou Akl2 Received: 18 February 2019 / Accepted: 27 April 2019 / Published online: 25 May 2019 © Springer Science+Business Media, LLC, part of Springer Nature 2019 Abstract Hepatic hydrothorax is a challenging complication of cirrhosis related to portal hypertension with an incidence of 5–11% and occurs most commonly in patients with decompensated disease. Diagnosis is made through thoracentesis after exclud- ing other causes of transudative efusions. It presents with dyspnea on exertion and it is most commonly right sided. Patho- physiology is mainly related to the direct passage of fuid from the peritoneal cavity through diaphragmatic defects. In this updated literature review, we summarize the diagnosis, clinical presentation, epidemiology and pathophysiology of hepatic hydrothorax, then we discuss a common complication of hepatic hydrothorax, spontaneous bacterial pleuritis, and how to diagnose and treat this condition. Finally, we elaborate all treatment options including chest tube drainage, pleurodesis, surgical intervention, Transjugular Intrahepatic Portosystemic Shunt and the most recent evidence on indwelling pleural catheters, discussing the available data and concluding with management recommendations. Keywords Hepatic hydrothorax · Cirrhosis · Pleural efusion · Thoracentesis Introduction Defnition and Epidemiology Hepatic hydrothorax (HH) is one of the pulmonary com- Hepatic hydrothorax is defned as the accumulation of more plications of cirrhosis along with hepatopulmonary syn- than 500 ml, an arbitrarily chosen number, of transudative drome and portopulmonary hypertension. It shares common pleural efusion in a patient with portal hypertension after pathophysiological pathways with ascites secondary to por- excluding pulmonary, cardiac, renal and other etiologies [4]. -

Dr. ALSHIKH YOUSSEF Haiyan
Dr. ALSHIKH YOUSSEF Haiyan General features The peritoneum is a thin serous membrane Consisting of: 1- Parietal peritoneum -lines the ant. Abdominal wall and the pelvis 2- Visceral peritoneum - covers the viscera 3- Peritoneal cavity - the potential space between the parietal and visceral layer of peritoneum - in male, is a closed sac - but in the female, there is a communication with the exterior through the uterine tubes, the uterus, and the vagina ▪ Peritoneum cavity divided into Greater sac Lesser sac Communication between them by the epiploic foramen The peritoneum The peritoneal cavity is the largest one in the body. Divided into tow sac : .Greater sac; extends from diaphragm down to the pelvis. Lesser Sac .Lesser sac or omental bursa; lies behind the stomach. .Both cavities are interconnected through the epiploic foramen(winslow ). .In male : the peritoneum is a closed sac . .In female : the sac is not completely closed because it Greater Sac communicates with the exterior through the uterine tubes, uterus and vagina. Peritoneum in transverse section The relationship between viscera and peritoneum Intraperitoneal viscera viscera is almost totally covered with visceral peritoneum example, stomach, 1st & last inch of duodenum, jejunum, ileum, cecum, vermiform appendix, transverse and sigmoid colons, spleen and ovary Intraperitoneal viscera Interperitoneal viscera Retroperitoneal viscera Interperitoneal viscera Such organs are not completely wrapped by peritoneum one surface attached to the abdominal walls or other organs. Example liver, gallbladder, urinary bladder and uterus Upper part of the rectum, Ascending and Descending colon Retroperitoneal viscera some organs lie on the posterior abdominal wall Behind the peritoneum they are partially covered by peritoneum on their anterior surfaces only Example kidney, suprarenal gland, pancreas, upper 3rd of rectum duodenum, and ureter, aorta and I.V.C The Peritoneal Reflection The peritoneal reflection include: omentum, mesenteries, ligaments, folds, recesses, pouches and fossae. -

Review of Intra-Arterial Therapies for Colorectal Cancer Liver Metastasis
cancers Review Review of Intra-Arterial Therapies for Colorectal Cancer Liver Metastasis Justin Kwan * and Uei Pua Department of Vascular and Interventional Radiology, Tan Tock Seng Hospital, Singapore 388403, Singapore; [email protected] * Correspondence: [email protected] Simple Summary: Colorectal cancer liver metastasis occurs in more than 50% of patients with colorectal cancer and is thought to be the most common cause of death from this cancer. The mainstay of treatment for inoperable liver metastasis has been combination systemic chemotherapy with or without the addition of biological targeted therapy with a goal for disease downstaging, for potential curative resection, or more frequently, for disease control. For patients with dominant liver metastatic disease or limited extrahepatic disease, liver-directed intra-arterial therapies including hepatic arterial chemotherapy infusion, chemoembolization and radioembolization are alternative treatment strategies that have shown promising results, most commonly in the salvage setting in patients with chemo-refractory disease. In recent years, their role in the first-line setting in conjunction with concurrent systemic chemotherapy has also been explored. This review aims to provide an update on the current evidence regarding liver-directed intra-arterial treatment strategies and to discuss potential trends for the future. Abstract: The liver is frequently the most common site of metastasis in patients with colorectal cancer, occurring in more than 50% of patients. While surgical resection remains the only potential Citation: Kwan, J.; Pua, U. Review of curative option, it is only eligible in 15–20% of patients at presentation. In the past two decades, Intra-Arterial Therapies for Colorectal major advances in modern chemotherapy and personalized biological agents have improved overall Cancer Liver Metastasis. -

Pdf Manual (964.7Kb)
MD-17 , CONTENTS THE URINARY SYSTEM 4 THE REPRODUCTIVE SYSTEM 5 The Scrotum The Testis The Epididylnis The Ductus Deferens The Ejaculatory Duct The Seminal Vesicle The Spermatic Cord The Penis The Prostate Gland THE INGUINAL CANAL l) HERNIAS FURTIlER READING 10 MODEL KEY 1I Human Male Pelvis This life-size model shows the viscera and structures which form the urogenital system and some of the related anatomy such as the sig moid colon and rectum. The vascular supply to the viscera and support ing tissue is demonstrated, as well as that portion of the vascular system which continues into the lower extremity. The model is divided into right and left portions. The right portion shows a midsagittal section of the pelvic structures. The left represents a similar section, but the dissection is deeper. Two pieces are remov able on the left side; one piece includes the bladder, prostate, and semi nal vesicles, and the other includes the penis, left testicle, and scrotum. When all portions are removed, a deeper view of these structures and a deeper dissection of the pelvis can be seen. THE URINARY SYSTEM The portion of the urinary system shown depicts the ureter from the level of the 5th lumbar vertebra, where it passes the common iliac ar tery near the bifurcation of thi s artery into the external and internal iliac arteries. The ureter then passes toward the posterior portion of the bladder, beneath the vas deferens, and opens through the wall of the blad der at one cranial corner of the trigone on the bladder's interior. -

Guidelines for Potential Multiple Organ Donors (Adult). Part II
ARTIGO ESPECIAL Glauco Adrieno Westphal, Milton Diretrizes para manutenção de múltiplos órgãos Caldeira Filho, Kalinca Daberkow Vieira, Viviane Renata Zaclikevis, no potencial doador adulto falecido. Parte II. Miriam Cristine Machado Bartz, Ventilação mecânica, controle endócrino metabólico Raquel Wanzuita, Álvaro Réa-Neto, Cassiano Teixeira, Cristiano Franke, e aspectos hematológicos e infecciosos Fernando Osni Machado, Joel de Andrade, Jorge Dias de Matos, Guidelines for potential multiple organ donors (adult). Part II. Alfredo Fiorelli, Delson Morilo Lamgaro, Fabiano Nagel, Felipe Mechanical ventilation, endocrine metabolic management, Dal-Pizzol, Gerson Costa, José hematological and infectious aspects Mário Teles, Luiz Henrique Melo, Maria Emília Coelho, Nazah Cherif RESUMO das alterações hematológicas é igualmente Mohamed Youssef, Péricles Duarte, importante considerando as implicações Rafael Lisboa de Souza A atuação do intensivista durante a da prática transfusional inapropriada. manutenção do potencial doador falecido Ressalta-se ainda o papel da ventilação na busca da redução de perdas de doadores protetora na modulação inflamatória e e do aumento da efetivação de transplantes conseqüente aumento do aproveitamen- não se restringe aos aspectos hemodinâmi- to de pulmões para transplante. Por fim, cos. O adequado controle endócrino-me- assinala-se a relevância da avaliação crite- tabólico é essencial para a manutenção do riosa das evidências de atividade infecciosa aporte energético aos tecidos e do controle e da antibioticoterapia na busca do maior hidro-eletrolítico, favorecendo inclusive a utilização de órgãos de potenciais doadores estabilidade hemodinâmica. A abordagem falecidos. A presente diretriz é uma iniciativa conjunta da Associação de Medicina INTRODUÇAO Intensiva Brasileira (AMIB) e da Associação Brasileira de Transplantes de Órgãos (ABTO) e teve apoio de SC Durante a evolução para a morte encefálica (ME) ocorrem diversas alterações Transplantes - Central de Notificação fisiológicas como resposta à perda das funções do tronco cerebral. -

Part Innervation Blood Supply Venous Drainage
sheet PART INNERVATION BLOOD SUPPLY VENOUS DRAINAGE LYMPH DRAINAGE Roof: greater palatine & nasopalatine Mouth nerves (maxillary N.) Floor: lingual nerve (mandibular N.) Taste {ant 1/3}: chorda tympani nerve (facial nerve) Cheeks: buccal nerve (mandibular N.) Buccinator muscle: Buccal Nerve 1 (facial Nerve) Orbicularis oris muscle: facial nerve Tip: Submental LNs Tongue lingual artery (ECA) sides of ant 2/3: Ant 1/3: Lingual nerve (sensory) & tonsillar branch of facial artery lingual veins correspond to submandibular & chorda tympani (Taste) (ECA) the arteries and drain into IJV deep cervical LNs Post 2/3: glossopharyngeal N. (both) ascending pharyngeal artery post 1/3: Deep (ECA) cervical LNs greater palatine vein greater palatine artrey Palate Hard Palate: greater palatine and (→maxillary V.) (maxillary A.) nasopalatine nerves ascending palatine vein Deep cervical lymph ascending palatine artrey Soft Palate: lesser palatine and (→facial V.) nodes (facial A.) glossopharyngeal nerves ascending pharyngeal ascending pharyngeal artery vein PANS (secreto-motor) & Sensory: 2 Parotid gland Auriculotemporal nerve {Inferior salivary Nucleus → tympanic branch of glossopharyngeal N.→ Lesser petrosal nerve parasympathetic preganglionic fibres → otic ganglia → auriculotemporal nerve parasympathetic postganglionic fibres} sheet PART INNERVATION BLOOD SUPPLY VENOUS DRAINAGE LYMPH DRAINAGE PANS (secreto-motor): facial nerve Submandibular Sensory: lingual nerve gland {Superior salivary Nucleus → Chorda tympani branch from facial