Plantar Fasciitis Exercises
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Plantar Fascia-Specific Stretching Program for Plantar Fasciitis
Plantar Fascia-Specific Stretching Program For Plantar Fasciitis Plantar Fascia Stretching Exercise 1. Cross your affected leg over your other leg. 2. Using the hand on your affected side, take hold of your affected foot and pull your toes back towards shin. This creates tension/stretch in the arch of the foot/plantar fascia. 3. Check for the appropriate stretch position by gently rubbing the thumb of your unaffected side left to right over the arch of the affected foot. The plantar fascia should feel firm, like a guitar string. 4. Hold the stretch for a count of 10. A set is 10 repetitions. 5. Perform at least 3 sets of stretches per day. You cannot perform the stretch too often. The most important times to stretch are before taking the first step in the morning and before standing after a period of prolonged sitting. Plantar Fascia Stretching Exercise 1 2 3 4 URMC Orthopaedics º 4901 Lac de Ville Boulevard º Building D º Rochester, NY 14618 º 585-275-5321 www.ortho.urmc.edu Over, Please Anti-inflammatory Medicine Anti-inflammatory medicine will help decrease the inflammation in the arch and heel of your foot. These include: Advil®, Motrin®, Ibuprofen, and Aleve®. 1. Use the medication as directed on the package. If you tolerate it well, take it daily for 2 weeks then discontinue for 1 week. If symptoms worsen or return, then resume medicine for 2 weeks, then stop. 2. You should eat when taking these medications, as they can be hard on your stomach. Arch Support 1. -

Piriformis Syndrome Is Overdiagnosed 11 Robert A
American Association of Neuromuscular & Electrodiagnostic Medicine AANEM CROSSFIRE: CONTROVERSIES IN NEUROMUSCULAR AND ELECTRODIAGNOSTIC MEDICINE Loren M. Fishman, MD, B.Phil Robert A.Werner, MD, MS Scott J. Primack, DO Willam S. Pease, MD Ernest W. Johnson, MD Lawrence R. Robinson, MD 2005 AANEM COURSE F AANEM 52ND Annual Scientific Meeting Monterey, California CROSSFIRE: Controversies in Neuromuscular and Electrodiagnostic Medicine Loren M. Fishman, MD, B.Phil Robert A.Werner, MD, MS Scott J. Primack, DO Willam S. Pease, MD Ernest W. Johnson, MD Lawrence R. Robinson, MD 2005 COURSE F AANEM 52nd Annual Scientific Meeting Monterey, California AANEM Copyright © September 2005 American Association of Neuromuscular & Electrodiagnostic Medicine 421 First Avenue SW, Suite 300 East Rochester, MN 55902 PRINTED BY JOHNSON PRINTING COMPANY, INC. ii CROSSFIRE: Controversies in Neuromuscular and Electrodiagnostic Medicine Faculty Loren M. Fishman, MD, B.Phil Scott J. Primack, DO Assistant Clinical Professor Co-director Department of Physical Medicine and Rehabilitation Colorado Rehabilitation and Occupational Medicine Columbia College of Physicians and Surgeons Denver, Colorado New York City, New York Dr. Primack completed his residency at the Rehabilitation Institute of Dr. Fishman is a specialist in low back pain and sciatica, electrodiagnosis, Chicago in 1992. He then spent 6 months with Dr. Larry Mack at the functional assessment, and cognitive rehabilitation. Over the last 20 years, University of Washington. Dr. Mack, in conjunction with the Shoulder he has lectured frequently and contributed over 55 publications. His most and Elbow Service at the University of Washington, performed some of the recent work, Relief is in the Stretch: End Back Pain Through Yoga, and the original research utilizing musculoskeletal ultrasound in order to diagnose earlier book, Back Talk, both written with Carol Ardman, were published shoulder pathology. -
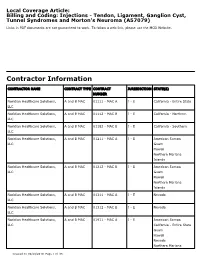
Billing and Coding: Injections - Tendon, Ligament, Ganglion Cyst, Tunnel Syndromes and Morton's Neuroma (A57079)
Local Coverage Article: Billing and Coding: Injections - Tendon, Ligament, Ganglion Cyst, Tunnel Syndromes and Morton's Neuroma (A57079) Links in PDF documents are not guaranteed to work. To follow a web link, please use the MCD Website. Contractor Information CONTRACTOR NAME CONTRACT TYPE CONTRACT JURISDICTION STATE(S) NUMBER Noridian Healthcare Solutions, A and B MAC 01111 - MAC A J - E California - Entire State LLC Noridian Healthcare Solutions, A and B MAC 01112 - MAC B J - E California - Northern LLC Noridian Healthcare Solutions, A and B MAC 01182 - MAC B J - E California - Southern LLC Noridian Healthcare Solutions, A and B MAC 01211 - MAC A J - E American Samoa LLC Guam Hawaii Northern Mariana Islands Noridian Healthcare Solutions, A and B MAC 01212 - MAC B J - E American Samoa LLC Guam Hawaii Northern Mariana Islands Noridian Healthcare Solutions, A and B MAC 01311 - MAC A J - E Nevada LLC Noridian Healthcare Solutions, A and B MAC 01312 - MAC B J - E Nevada LLC Noridian Healthcare Solutions, A and B MAC 01911 - MAC A J - E American Samoa LLC California - Entire State Guam Hawaii Nevada Northern Mariana Created on 09/28/2019. Page 1 of 33 CONTRACTOR NAME CONTRACT TYPE CONTRACT JURISDICTION STATE(S) NUMBER Islands Article Information General Information Original Effective Date 10/01/2019 Article ID Revision Effective Date A57079 N/A Article Title Revision Ending Date Billing and Coding: Injections - Tendon, Ligament, N/A Ganglion Cyst, Tunnel Syndromes and Morton's Neuroma Retirement Date N/A Article Type Billing and Coding AMA CPT / ADA CDT / AHA NUBC Copyright Statement CPT codes, descriptions and other data only are copyright 2018 American Medical Association. -

Tarsal Tunnel Syndrome: a Still Challenge Condition
Rev Bras Neurol. 55(1):12-17, 2019 TARSAL TUNNEL SYNDROME: A STILL CHALLENGE CONDITION SÍNDROME DO TÚNEL DO TARSO: UMA CONDIÇÃO AINDA DESAFIADORA Celmir de Oliveira Vilaça1,2, Bruno Pessoa3, Janaína de Moraes Silva4, Victor Hugo Bastos5, Diandra Martins5, Silmar Teixeira6, Victor Marinho6, Rossano Fiorelli7, Vanessa de Albuquerque Dinoa8; Marco Orsini7, 9 ABSTRACT RESUMO Tarsal tunnel syndrome is a rare, under diagnosed and often confu- A Síndrome do túnel do tarso é uma rara e subdiagnosticada neuro- sed neuropathy with other clinical entities. There is a lack of popula- patia geralmente confundida com outras entidades clínicas. Há falta tion studies on this disease. Herein, we performed a non-systematic de estudos populacionais sobre a doença. Assim sendo, realizamos review of articles between January 1992 and February 2018. Althou- uma revisão da literatura de artigos entre Janeiro de 1992 e fevereiro gh with a less complex anatomy comparing to the carpal tunnel, the de 2018. Apesar de possuir uma anatomia de menor complexidade tarsal tunnel is source of pain and some other conditions. Treatment comparada ao túnel do carpo, o túnel do tarso é origem de dor e involves conservative measures such as analgesics and physical the- algumas outras condições. O tratamento envolve medidas conserva- rapy rehabilitation or surgical procedures in case of conservative doras como analgésicos e terapia de reabilitação ou procedimentos treatment failure. Randomized control studies are lack and manda- cirúrgicos, em caso de falha do tratamento conservador. Estudos ran- tory for uncover the best modality of treatment for this condition. domizados são escassos e necessários para descoberta da melhor modalidade de tratamento desta condição. -

Advice and Exercises for Patients with Plantar Fasciitis
Advice and exercises for patients with plantar fasciitis This leaflet provides management advice and exercises for people diagnosed with plantar fasciitis, a condition causing pain in the heel, sole and /or arch of the foot. Structures of the foot The plantar fascia is a sheet or broad band of fibrous tissue that runs along the bottom of the foot. This tissue connects the heel to the base of the toes. Under normal circumstances, the plantar fascia supports the arch of the foot and acts as a shock absorbing “bow string” within the arch of the foot. With weight bearing, the foot flattens and the plantar fascia stretches, then springing you forward ready for the next step. While walking, the stresses placed on the foot can be one and a quarter times your body weight (this increases to two and three quarter times your body weight when running). Unsurprisingly then, that heel pain is common. If tension on this “bowstring” becomes too great, irritation or inflammation can occur causing pain. What is plantar fasciitis? Plantar fasciitis is a relatively common foot problem affecting up to 10-15% of the population. It can occur at any age. It is sometimes known as “policeman’s heel”. When placed under too much stress due to abnormal loading, the plantar fascia stretches causing micro tearing and degeneration of the tissue. It can lead to pain in the heel, across the sole of the foot and sometimes into the arch area of the foot too. These micro tears repair with scar tissue, which is less flexible than the fascia and can cause the problem to persist for many months. -

Tarsal Tunnel Syndrome Secondary to the Posterior Tibial Nerve Schwannoma
Case Report http://dx.doi.org/10.12972/The Nerve.2015.01.01.034 www.thenerve.net Tarsal Tunnel Syndrome Secondary to the Posterior Tibial Nerve Schwannoma Jung Won Song1, Sung Han Oh1, Pyung Goo Cho1, Eun Mee Han2 Departments of 1Neurosurgey, 2Pathology, Bundang Jesaeng General Hospital, Seongnam, Korea A 77-year-old female presented with complaint of burning pain and paresthesia along the medial aspect of ankle, heel and sole of the left foot. An ankle MRI, electromyelogram (EMG) with nerve conduction velocity (NCV) and pathologic findings were all compatible with Tarsal tunnel syndrome caused by the posterior tibial nerve Schwannoma. Operative release of the Tarsal tunnel and surgical excision of Schwannoma were performed under the microscopy. It is necessary to have a possible lump in mind when Tarsal tunnel syndrome is suspected, such as posterior tibial nerve Schwannoma. Key Words: Posterior Tibial NerveㆍSchwannomaㆍTarsal Tunnel Syndrome diagnose neurofibromatosis was insufficient. An ankle magne- tic resonance imaging (MRI) revealed about a 22×19×9 mm- INTRODUCTION sized ovoid soft tissue mass in the posterior ankle connected to the posterior tibial nerve. The mass lies beneath the flexor Although Schwannomas are the most common peripheral retinaculum of ankle and showed relatively strong enhance- nerve sheath tumor, Schwannoma of the posterior tibial nerve ment (Fig. 1). and it branch is a rare etiology causing Tarsal tunnel syndrome. The NCV study showed no response sensory nerve action We report a case of Tarsal tunnel syndrome caused by the pos- potentials of the left medial and lateral plantar nerves. Motor terior tibial nerve Schwannoma and mention surgical strategy conduction study of the deep peroneal and tibial nerves was with literature review. -

Pathogenesis, Diagnosis, and Treatment of the Tarsal-Tunnel Syndrome
CLEVELAND CLINIC QUARTERLY Volume 37, January 1970 Copyright © 1970 by The Cleveland Clinic Foundation Printed in U.S.A. Pathogenesis, diagnosis, and treatment of the tarsal-tunnel syndrome THOMAS E. GRETTER, M.D. Department o£ Neurology ALAN H. WILDE, M.D. Department of Orthopaedic Surgery N recent years many peripheral nerve compression syndromes have been I recognized. The carpal-tunnel syndrome, or compression of the median nerve at the wrist beneath the transverse carpal ligament, is the com- monest nerve entrapment syndrome. Less familiar but no less important is the tarsal-tunnel syndrome. Since the first case reports of the tarsal-tunnel syndrome by Keck1 and by Lam,2 in 1962, this syndrome is being diag- nosed with increasing frequency. Within the last two years 17 patients with the tarsal-tunnel syndrome have been treated at the Cleveland Clinic. Our report presents a review of the pathogenesis, diagnosis, and treatment of the tarsal-tunnel syndrome. Anatomy The tarsal tunnel is a canal formed on the medial side of the foot and ankle by the medial malleolus of the tibia and the flexor retinaculum. The flexor retinaculum spans the medial malleolus of the tibia and the medial tubercle of the os calcis (Fig. 1). The space beneath the ligament is divided by septae into four compartments. Each compartment contains one of the four structures of the tarsal tunnel. These structures are the pos- terior tibial tendon, flexor digitorum longus tendon, posterior tibial nerve, artery and veins, and the flexor hallucis longus tendon. Each tendon is invested with a separate synovial sheath. -

Foot and Ankle Disorders Capturing Motion with Ultrasound
VISIT THE AANEM MARKETPLACE AT WWW.AANEM.ORG FOR NEW PRODUCTS AMERICAN ASSOCIATION OF NEUROMUSCULAR & ELECTRODIAGNOSTIC MEDICINE Foot and Ankle Disorders Capturing Moti on With Ultrasound: Blood, Muscle, Needle, and Nerve Photo by Michael D. Stubblefi eld, MD Foot and Ankle Nerve Disorders Tracy A. Park, MD David R. Del Toro, MD Atul T. Patel, MD, MHSA Jeffrey A. Mann, MD AANEM 58th Annual Meeting San Francisco, California Copyright © September 2011 American Association of Neuromuscular & Electrodiagnostic Medicine 2621 Superior Drive NW Rochester, MN 55901 Printed by Johnson’s Printing Company, Inc. 1 Please be aware that some of the medical devices or pharmaceuticals discussed in this handout may not be cleared by the FDA or cleared by the FDA for the specific use described by the authors and are “off-label” (i.e., a use not described on the product’s label). “Off-label” devices or pharmaceuticals may be used if, in the judgment of the treating physician, such use is medically indicated to treat a patient’s condition. Information regarding the FDA clearance status of a particular device or pharmaceutical may be obtained by reading the product’s package labeling, by contacting a sales representative or legal counsel of the manufacturer of the device or pharmaceutical, or by contacting the FDA at 1-800-638-2041. 2 Foot and Ankle Nerve Disorders Table of Contents Course Objectives & Course Committee 4 Faculty 5 Tarsal Tunnel Syndromes 7 Tracy A. Park, MD First Branch Lateral Plantar Neuropathy: “Baxter’s Neuropathy” 17 David R. Del Toro, MD Foot Pain Related to Peroneal (Fibular) Nerve Entrapments (Deep and Superficial) and Digital Neuromas 25 Atul T. -

Top 10 Positional-Release Therapy Techniques to Break the Chain of Pain, Part 1 Timothy E
Sacred Heart University DigitalCommons@SHU All PTHMS Faculty Publications Physical Therapy & Human Movement Science 2006 Top 10 Positional-Release Therapy Techniques to Break the Chain of Pain, Part 1 Timothy E. Speicher Sacred Heart University David O. Draper Brigham Young University - Utah Follow this and additional works at: http://digitalcommons.sacredheart.edu/pthms_fac Part of the Physical Therapy Commons, and the Somatic Bodywork and Related Therapeutic Practices Commons Recommended Citation Speicher, Tim and David O. Draper. "Top-10 Positional-Release Therapy Techniques to Break the Chjin of Pain: Part 1. Athletic Therapy Today 11.5 (2006): 69-71. This Peer-Reviewed Article is brought to you for free and open access by the Physical Therapy & Human Movement Science at DigitalCommons@SHU. It has been accepted for inclusion in All PTHMS Faculty Publications by an authorized administrator of DigitalCommons@SHU. For more information, please contact [email protected], [email protected]. THERAPEUTIC MODALITIES David O. Draper, EdD, ATC, Column Editor Top 10 Positional-Release Therapy Techniques to Break the Chain of Pain, Part 1 Tim Speicher, MS, ATC, CSCS • Sacred Heart University David O. Draper, EdD, ATC • Brigham Young University OSITIONAL-RELEASE therapy (PRT) is a counterstrained tissue, decreasing abberent gamma and treatment technique that is gaining popu- alpha neuronal activity, thereby breaking the sustained P larity. The purpose of this two-part column contraction.1 Jones’s original work and PRT theory have -

Plantar Fasciitis Stage 1
PLANTAR FASCIITIS STAGE 1 ADVICE Avoid those activities which aggravate your pain (e.g walking or running). SETS & REPS: N/A FREQUENCY: N/A AVOID FLIP-FLOPS Avoid wearing flip-flops SETS & REPS: N/A FREQUENCY: N/A AVOID HIGH HEELS Avoid high heels. SETS & REPS: N/A FREQUENCY: N/A PLANTAR FASCIA ICE MASSAGE Place a frozen water bottle on the floor and roll the bottle back and forth under your foot for 10 minutes. Do this at the end of each day and after activity. SETS & REPS: 10 mins FREQUENCY: Daily PLANTAR FASCIA MASSAGE Sitting, place a golf ball on the floor and roll the ball around under your foot concentrating on the tight, tender areas. SETS & REPS: 2-5 mins FREQUENCY: As needed © 2013 The Rehab Lab Limited. Used under license. No reproduction permitted without permission. www.therehablab.com PLANTAR FASCIITIS STAGE 1 PRONE GLUTEAL CONTRACTION Lie face-down and place your hands on your buttock muscles. Contract your gluteals, feeling the muscles tightening beneath your hands and hold for 5 seconds. Relax and repeat. SETS & REPS: 10 reps FREQUENCY: 1-2 x daily GLUTEAL STRETCH Sit on a chair and place your ankle on your opposite knee. With both hands, gently push down the knee of the crossed leg. Maintaining a straight back, bend forwards from the hips until you feel a stretch. Hold. SETS & REPS: 2 minute hold FREQUENCY: 1-2 x daily HAMSTRING STRETCH Place your heel on a knee-height table/chair with your knee slightly bent and tilt your pelvis forwards. While keeping your back straight, lean forwards until you feel a stretch in your hamstring. -

Plantar Fasciitis: a Degenerative Process (Fasciosis) Without Inflammation
CLINICAL PATHOLOGY Plantar Fasciitis A Degenerative Process (Fasciosis) Without Inflammation Harvey Lemont, DPM* Krista M. Ammirati, BS* Nsima Usen, MPH* The authors review histologic findings from 50 cases of heel spur surgery for chronic plantar fasciitis. Findings include myxoid degeneration with fragmentation and degeneration of the plantar fascia and bone marrow vascular ectasia. Histologic findings are presented to support the thesis that “plantar fasciitis” is a degenerative fasciosis without inflammation, not a fasciitis. These findings suggest that treatment regimens such as serial corticosteroid injections into the plantar fascia should be reevalu- ated in the absence of inflammation and in light of their potential to induce plantar fascial rupture. (J Am Podiatr Med Assoc 93(3): 234-237, 2003) Plantar fasciitis is presumed to be synonymous with occur with long-distance running may induce an in- inflammation of the plantar fascia. In fact, the suffix flammatory process, leading to fibrosis or degenera- “-itis” inherently implies an inflammatory disease. tion, and Sewell5 stated that the pain of plantar inflam- However, is plantar fasciitis really an inflammatory mation may sometimes be secondary to periosteal disorder? inflammation of the os calcis. Although authors writ- Plantar fasciitis is widely described in the litera- ing on the subject describe inflammation as being ture as having a multifactorial and widely disputed present in plantar fasciitis, they provide no objective etiology. Interestingly, in 1965, Lapidus and Guidotti,1 clinical or histologic evidence to support their claims. in their article entitled “Painful Heel,” stated that “the In addition, when photomicrographs are provided, name of painful heel is used deliberately in prefer- they are often mislabeled as showing inflammation. -

Plantar Fasciitis Standard of Care
BRIGHAM AND WOMEN’S HOSPITAL Department of Rehabilitation Services Physical Therapy Standard of Care: Plantar Fasciitis Case Type / Diagnosis: (diagnosis specific, impairment/ dysfunction specific) ICD9 - 728.71 plantar fibromatosis Plantar fasciitis is an inflammatory condition that occurs as a result of overstressing the plantar fascia. It is the most common cause of inferior heel pain and has been diagnosed in patients from the ages of 8-80. 1-4 Plantar fasciitis affects approximately 10% of the population and is more commonly found in middle-aged women and younger male runners.2, 3, 5 A majority of the patients diagnosed with this inflammatory condition are over the age of 40.3 Bilateral symptoms can occur in 20-30% of those diagnosed with plantar fasciitis.6 However in these cases it is important to rule out other systemic processes such as rheumatoid arthritis, systemic lupus erythematosus, Reiter’s disease, gout and ankylosing spondylitis.3, 6 The primary symptom of plantar fasciitis is pain in the heel when the patient first rises in the morning and when the plantar fascia is palpated over it’s origin at the medial calcaneal tuberosity.2-4, 6, 7 The plantar fascia (aponeurosis) is a thick fibrous band of connective tissue that originates at the medial and lateral tuberosities of the calcaneus. It runs longitudinally and has 3 portions, medial, central, and lateral. At the midfoot level, the fascia divides into 5 separate bands, which blend with the flexor tendon sheaths and transverse metatarsal ligaments and attach at the base of each proximal phalange. The central portion of the plantar fascia is the largest section.