Fundus Signs in Temporal Arteritis
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Microsurgical Anatomy of the Central Retinal Artery
Original Article Microsurgical Anatomy of the Central Retinal Artery Matias Baldoncini1,2, Alvaro Campero2,3, Gabriel Moran1, Maximiliano Avendan˜ o1, Pablo Hinojosa-Martı´nez1, Marcela Cimmino1, Pablo Buosi1, Valeria Forlizzi1, Joaquı´n Chuang1, Brian Gargurevich1 - BACKGROUND: The central retinal artery (CRA) has INTRODUCTION been described as one of the first branches of the he central retinal artery (CRA) is described as one of the ophthalmic artery.It arises medial to the ciliary ganglion first branches of the ophthalmic artery. It arises medial to and after a sinuous path within the orbital cavity it pene- T the ciliary ganglion, and after a sinuous path inside the trates the lower surface of the dura mater that covers the orbital cavity, penetrates the lower surface of the dura mater that optic nerve, approximately 1 cm behind the eyeball. How- covers the optic nerve, approximately 1 cm behind the eyeball. ever, the numerous anatomic descriptions that were made After a short journey inside this meninge, it crosses the cranial of the CRA have been insufficient or unclear in relation to nerve to be located in its center and travels until it reaches the optical papilla where it divides into several branches. During this certain characteristics that are analyzed in the present entire journey, the CRA does not present any anastomoses, study. considering it as a terminal branch.1-4 However, the descriptions that many investigators make about - METHODS: An electronic literature search was made in some of thesecharacteristics of the CRA differ with the classic the PubMed database and a cadaver dissection was per- disposition] (Tables 1e12).5-40 The numerous anatomic de- formed on 11 orbits fixed in formaldehyde. -

THE CENTRAL ARTERY of the RETINA*T H
Br J Ophthalmol: first published as 10.1136/bjo.44.5.280 on 1 May 1960. Downloaded from Brit. J. Ophthal. (1960) 44, 280. THE CENTRAL ARTERY OF THE RETINA*t H. A STUDY OF ITS DISTRIBUHTION AND ANASTOMOSES BY SOHAN SINGH AND RAMJI DASS Department ofAnatomy, Government Medical College, Patiala, India THERE is little unanimity regarding the distribution and anastomoses of the central artery of the retina. According to Frangois and Neetens (1954, 1956) and Fran9ois, Neetens, and Collette (1955), the central artery of the retina is completely devoid of branches, while according to Wolff (1939) and Behr (1935) it is free from branches only in its intraneural course. Magitot (1908), Quain (1909), Beauvieux and Ristitch (1924), Wolff (1940), Bignell (1952), Wybar (1956), and Steele and Blunt (1956) on the other hand demon- strated branches from all parts of its course. Most investigators agree that this artery contributes to the blood supply of the optic nerve, but Francois and others (1954, 1955, 1956) affirm that this is not the case. The presence of a central artery of the optic nerve described by Behr (1935), Wolff (1939, 1954), Francois and others (1954, 1955, 1956), and Wybar (1956), is denied by Beauvieux and Ristitch (1924) and Steele and Blunt (1956). Beauvieux and Ristitch (1924), Kershner (1943), Frangois and others http://bjo.bmj.com/ (1954, 1955, 1956), and Steele and Blunt (1956) say there are no anastomoses between the central retinal and other arteries, but Vail (1948), Wybar (1956), and several other authors have observed and described them. The lamina cribrosa is the only site at which these anastomoses have been studied in any detail, and in this case too, contradictory views have been expressed. -
Reverberating Flow Pattern in the Central Retinal Artery in Cerebral
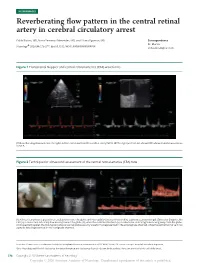
NEUROIMAGES Reverberating flow pattern in the central retinal artery in cerebral circulatory arrest Pablo Blanco, MD, Mar´ıa Fernanda Men´endez, MD, and Liliana Figueroa, MD Correspondence Dr. Blanco Neurology 2020;94:276-277. doi:10.1212/WNL.0000000000008918 ® [email protected] Figure 1 Transcranial Doppler and central retinal arteries (CRA) waveforms (A) Reverberating flow pattern in the right (and left, not shown) middle cerebral artery (MCA). (B) The right (and left, not shown) CRA showed similar waveforms to MCA. Figure 2 Technique for ultrasound assessment of the central retinal arteries (CRA) flow (A) A linear transducer is placed in an axial position over the globe, with the eyelids closed and covered by a generous amount of gel. (B) In color Doppler, the CRA (a) is coded red, indicating flow moving toward the globe (G), while the central retinal vein (v) is coded blue, indicating flow moving away from the globe. (C) In spectral Doppler, the CRA typically shows low resistance velocity waveforms (represented in the anterograde channel), while the central retinal vein has a phasic flow (represented in the retrograde channel). From the “Centro Unico´ Coordinador de Ablacion´ e Implante Provincia de Buenos Aires (CUCAIBA)” Team, “Dr. Emilio Ferreyra” Hospital, Necochea, Argentina. Go to Neurology.org/N for full disclosures. Funding information and disclosures deemed relevant by the authors, if any, are provided at the end of the article. 276 Copyright © 2020 American Academy of Neurology Copyright © 2020 American Academy of Neurology. Unauthorized reproduction of this article is prohibited. A 49-year-old woman developed signs of brain death after when obtaining flow signals through the cranial bone is not a severe traumatic brain injury. -

The Ophthalmic Artery Ii
Brit. J. Ophthal. (1962) 46, 165. THE OPHTHALMIC ARTERY II. INTRA-ORBITAL COURSE* BY SOHAN SINGH HAYREHt AND RAMJI DASS Government Medical College, Patiala, India Material THIS study was carried out in 61 human orbits obtained from 38 dissection- room cadavers. In 23 cadavers both the orbits were examined, and in the remaining fifteen only one side was studied. With the exception of three cadavers of children aged 4, 11, and 12 years, the specimens were from old persons. Method Neoprene latex was injected in situ, either through the internal carotid artery or through the most proximal part of the ophthalmic artery, after opening the skull and removing the brain. The artery was first irrigated with water. After injection the part was covered with cotton wool soaked in 10 per cent. formalin for from 24 to 48 hours to coagulate the latex. The roof of the orbit was then opened and the ophthalmic artery was carefully studied within the orbit. Observations COURSE For descriptive purposes the intra-orbital course of the ophthalmic artery has been divided into three parts (Singh and Dass, 1960). (1) The first part extends from the point of entrance of the ophthalmic artery into the orbit to the point where the artery bends to become the second part. This part usually runs along the infero-lateral aspect of the optic nerve. (2) The second part crosses over or under the optic nerve running in a medial direction from the infero-lateral to the supero-medial aspect of the nerve. (3) The thirdpart extends from the point at which the second part bends at the supero-medial aspect of the optic nerve to its termination. -

A Review of Central Retinal Artery Occlusion: Clinical Presentation And
Eye (2013) 27, 688–697 & 2013 Macmillan Publishers Limited All rights reserved 0950-222X/13 www.nature.com/eye 1 2 1 2 REVIEW A review of central DD Varma , S Cugati , AW Lee and CS Chen retinal artery occlusion: clinical presentation and management Abstract Central retinal artery occlusion (CRAO) is an that in turn place an individual at risk of future ophthalmic emergency and the ocular ana- cerebral stroke and ischaemic heart disease. logue of cerebral stroke. Best evidence reflects Although analogous to a cerebral stroke, there that over three-quarters of patients suffer is currently no guideline-endorsed evidence for profound acute visual loss with a visual acuity treatment. Current options for therapy include of 20/400 or worse. This results in a reduced the so-called ‘standard’ therapies, such as functional capacity and quality of life. There is sublingual isosorbide dinitrate, systemic also an increased risk of subsequent cerebral pentoxifylline or inhalation of a carbogen, stroke and ischaemic heart disease. There are hyperbaric oxygen, ocular massage, globe no current guideline-endorsed therapies, compression, intravenous acetazolamide and although the use of tissue plasminogen acti- mannitol, anterior chamber paracentesis, and vator (tPA) has been investigated in two methylprednisolone. None of these therapies randomized controlled trials. This review will has been shown to be better than placebo.5 describe the pathophysiology, epidemiology, There has been recent interest in the use of and clinical features of CRAO, and discuss tissue plasminogen activator (tPA) with two current and future treatments, including the recent randomized controlled trials on the 1Flinders Comprehensive use of tPA in further clinical trials. -

Anatomy of the Ophthalmic Artery: Embryological Consideration
REVIEW ARTICLE doi: 10.2176/nmc.ra.2015-0324 Neurol Med Chir (Tokyo) 56, 585–591, 2016 Online June 8, 2016 Anatomy of the Ophthalmic Artery: Embryological Consideration Naoki TOMA1 1Department of Neurosurgery, Mie University Graduate School of Medicine, Tsu, Mie, Japan Abstract There are considerable variations in the anatomy of the human ophthalmic artery (OphA), such as anom- alous origins of the OphA and anastomoses between the OphA and the adjacent arteries. These anatomi- cal variations seem to attribute to complex embryology of the OphA. In human embryos and fetuses, primitive dorsal and ventral ophthalmic arteries (PDOphA and PVOphA) form the ocular branches, and the supraorbital division of the stapedial artery forms the orbital branches of the OphA, and then numerous anastomoses between the internal carotid artery (ICA) and the external carotid artery (ECA) systems emerge in connection with the OphA. These developmental processes can produce anatomical variations of the OphA, and we should notice these variations for neurosurgical and neurointerventional procedures. Key words: ophthalmic artery, anatomy, embryology, stapedial artery, primitive maxillary artery Introduction is to elucidate the anatomical variation of the OphA from the embryological viewpoint. The ophthalmic artery (OphA) consists of ocular and orbital branches. The ocular branches contribute to Embryology and Anatomy the blood supply of the optic apparatus, namely, the of the OphA optic nerve and the retina, and the orbital branches supply the optic adnexae, such -

A Study of Surgical Approaches to Retinal Vascular Occlusions
SURGICAL TECHNIQUE A Study of Surgical Approaches to Retinal Vascular Occlusions William M. Tang, MD; Dennis P. Han, MD Objective: To develop a surgical approach to retinal vas- nulations of central retinal arteries were successful in 0 cular occlusive diseases. of 2 procedures, and cannulations of central retinal veins were successful in 2 of 4 procedures. Arteriovenous Methods: Surgical manipulations were performed on the sheathotomies were successful in 4 of 7 procedures. In retinal vasculature to explore the feasibility of retinal vas- the in vivo model, surgical penetration of retinal blood cular surgery. In a human cadaver eye model (25 proce- vessels was accomplished in 5 of 6 eyes. Immediately post- dures, 21 eyes), we performed (1) cannulations of retinal operatively, thrombus formation with obstruction of the blood vessels with a flexible stylet and (2) arteriovenous retinal vasculature was observed. At 2 weeks postopera- sheathotomies. Histological findings were correlated with tively, the retinal vasculature was completely patent. surgical outcomes. In an in vivo model (6 eyes, 5 animals), we examined the technical feasibility and anatomical out- Conclusions: Multiple surgical techniques aimed at as- come of surgical penetration of retinal blood vessels. sisting recanalization of occluded retinal vasculature have been evaluated. Retinal vascular surgery has become more Results: Cannulations of branch retinal arterioles were feasible and deserves further investigation. successful in 7 of 9 procedures, cannulations of branch retinal venules were successful in 1 of 3 procedures, can- Arch Ophthalmol. 2000;118:138-143 ETINAL ARTERY and vein oc- endovascular therapy can lead to reversal clusions are among the of retinal vascular occlusions. -

Anatomy of the Periorbital Region Review Article Anatomia Da Região Periorbital
RevSurgicalV5N3Inglês_RevistaSurgical&CosmeticDermatol 21/01/14 17:54 Página 245 245 Anatomy of the periorbital region Review article Anatomia da região periorbital Authors: Eliandre Costa Palermo1 ABSTRACT A careful study of the anatomy of the orbit is very important for dermatologists, even for those who do not perform major surgical procedures. This is due to the high complexity of the structures involved in the dermatological procedures performed in this region. A 1 Dermatologist Physician, Lato sensu post- detailed knowledge of facial anatomy is what differentiates a qualified professional— graduate diploma in Dermatologic Surgery from the Faculdade de Medician whether in performing minimally invasive procedures (such as botulinum toxin and der- do ABC - Santo André (SP), Brazil mal fillings) or in conducting excisions of skin lesions—thereby avoiding complications and ensuring the best results, both aesthetically and correctively. The present review article focuses on the anatomy of the orbit and palpebral region and on the important structures related to the execution of dermatological procedures. Keywords: eyelids; anatomy; skin. RESU MO Um estudo cuidadoso da anatomia da órbita é muito importante para os dermatologistas, mesmo para os que não realizam grandes procedimentos cirúrgicos, devido à elevada complexidade de estruturas envolvidas nos procedimentos dermatológicos realizados nesta região. O conhecimento detalhado da anatomia facial é o que diferencia o profissional qualificado, seja na realização de procedimentos mini- mamente invasivos, como toxina botulínica e preenchimentos, seja nas exéreses de lesões dermatoló- Correspondence: Dr. Eliandre Costa Palermo gicas, evitando complicações e assegurando os melhores resultados, tanto estéticos quanto corretivos. Av. São Gualter, 615 Trataremos neste artigo da revisão da anatomia da região órbito-palpebral e das estruturas importan- Cep: 05455 000 Alto de Pinheiros—São tes correlacionadas à realização dos procedimentos dermatológicos. -

Central Retinal Artery Occlusion and Cerebral Stroke Central Retinal Artery Occlusion
Correspondence 1422 Sir, 3 Hayreh SS, Zimmerman MB. Fundus changes in Central retinal artery occlusion and cerebral stroke central retinal artery occlusion. Retina 2007; 27: 276–289. 4 Hayreh SS, Zimmerman MB, Kimura A, Sanon A. Aspects of the review by Varma and colleagues1 conspire Central retinal artery occlusion. Retinal survival time. to amplify the confusion that surrounds central retinal Exp Eye Res 2004; 78: 723–736. artery occlusion (CRAO). First, they report that a foveal 5 McLeod D. Letter to the editor: partial central retinal artery cherry-red spot is present in 90% of eyes examined occlusion offers a unique insight into the ischemic penumbra. within 1 week of CRAO onset, whereas only 58% show Clin Ophthalmol 2012; 6: 9–22. concomitant macular opacification. Surely these ‘classic’ CRAO signs must co-exist? D McLeod Second, Varma and colleagues discuss ‘transient’ CRAO, a small subgroup of eyes in the Iowa CRAO Academic Department of Ophthalmology, classification characterised by CRA reopening by the Manchester Royal Eye Hospital, Manchester, UK time of initial presentation and fluorescein E-mail: [email protected] angiography.2,3 They state that ‘transient’ CRAO is ‘analogous to a transient ischaemic attack affecting the Eye (2013) 27, 1422; doi:10.1038/eye.2013.219; published eye’ since ‘restoration of blood flow y results in online 4 October 2013 symptom resolution’.1 This is not the case. The Iowa classification dispenses with terminological convention by labelling events as ‘transient’ even though complete reversal of symptoms and signs is precluded by a Sir, duration of ischaemic anoxia exceeding 4 h (inner retina’s Reply: ‘Central retinal artery occlusion and cerebral maximum survival time).4 They also state that ‘transient’ stroke’ CRAO presents ‘greatly varied fundus findings’.1 This is not the case. -

Anatomic and Embryologic Analysis of the Dural Branches of the Ophthalmic Artery
Published January 7, 2021 as 10.3174/ajnr.A6939 REVIEW ARTICLE ADULT BRAIN Anatomic and Embryologic Analysis of the Dural Branches of the Ophthalmic Artery S. Bonasia, S. Smajda, G. Ciccio, and T. Robert ABSTRACT SUMMARY: The ophthalmic artery has one of the most fascinating embryologic developments among the craniofacial arteries. Most of the ophthalmic artery orbital branches develop from the formation and regression of the stapedial artery and share their origin with dural branches of the ophthalmic artery. The concomitant embryologic development of the ophthalmic artery and mid- dle meningeal artery explains adequately the important varieties of anastomosis between these 2 arteries. It also explains the pres- ence of many dural branches from the ophthalmic artery. In this review, we focused on dural branches of the ophthalmic artery with the description of rare variations possible, in particular the ophthalmic artery origin of the middle meningeal artery and the ophthalmic artery origin of the marginal tentorial artery. ABBREVIATIONS: dAVF ¼ dural arteriovenous fistula; ECA ¼ external carotid artery; MMA ¼ middle meningeal artery; MTA ¼ marginal tentorial artery; OA ¼ ophthalmic artery; PDOA ¼ primitive dorsal ophthalmic artery; PVOA ¼ primitive ventral ophthalmic artery; SA ¼ stapedial artery he ophthalmic artery (OA) is a very fascinating artery for its Informed consent was obtained from all individual partici- Tcomplex embryologic development and also for numerous vas- pants included in the study. cular anastomoses developed with branches of the external carotid artery (ECA). The role of the OA in supplying the History dura is not well-known, but the understanding of the dural Meyer,1 in 1887, considered a pioneer in the orbital vascular anat- function of the OA and also of its possible variations is a cor- omy, was the first to precisely describe all branches of the oph- nerstone for surgical and endovascular treatment of dural thalmic artery, including its dural territory. -

Systemic Disease with a Twist of Neuro
6/14/2021 Systemic Disease Straight Up…. AOA’s definition of Optometry approved Sept 2012 with a Twist of Neuro! Doctors of optometry (ODs) are the independent primary health care Beth A. Steele, OD, FAAO professionals for the eye. Optometrists examine, diagnose, treat, and [email protected] manage diseases, injuries, and disorders of the visual system, the eye, and associated structures as well as identify related systemic conditions affecting the eye. PREVENTION Not just this… TREATING THE WHOLE PATIENT But also this… MEDICAL OPTOMETRY …..where do we fit in? 1 6/14/2021 29 AA F Hx ESRD, on dialysis Blood Pressure Classifications and Referral Guidelines (adapted from the Joint National Committee on Detection, Evaluation, and Treatment of High Blood Pressure –JNC 7, no symptoms, visual or systemic 2003) Hypotension normal Pre‐ HTN Stage 1Stage 2 Critical High Point Systolic < 90 < 120 120‐139 140‐ 159 ≥160 >180 Diastolic < 60 < 80 80 ‐ 89 90‐99 ≥100 >110 Refer Refer Evaluate or refer From: 2014 Evidence-Based Guideline for the Management of High Blood Pressure in Adults: Report From the Panel Members within 2 within 1 immediately or BP 159/116 Appointed to the Eighth Joint National Committee (JNC 8) months month within 1 week JNC vs. ACC/AHA Guidelines All values ~10mmHg lower than JNC • 2017 ACC/AHA Clinical Practice Guidelines lowered thresholds by 10mmHg for diagnosis and treatment goals! • 26% increase in US prevalence HTN • Very controversial 2 6/14/2021 Atherosclerotic cardiovascular disease (ASCVD) risk calculator • 10‐year risk of CVD • http://tools.acc.org/ASCVD‐Risk‐Estimator/ • age >65 • atherosclerosis or risk of developing it (e.g. -

Retina/Vitreous 2017-2019
Academy MOC Essentials® Practicing Ophthalmologists Curriculum 2017–2019 Retina/Vitreous *** Retina/Vitreous 2 © AAO 2017-2019 Practicing Ophthalmologists Curriculum Disclaimer and Limitation of Liability As a service to its members and American Board of Ophthalmology (ABO) diplomates, the American Academy of Ophthalmology has developed the Practicing Ophthalmologists Curriculum (POC) as a tool for members to prepare for the Maintenance of Certification (MOC) -related examinations. The Academy provides this material for educational purposes only. The POC should not be deemed inclusive of all proper methods of care or exclusive of other methods of care reasonably directed at obtaining the best results. The physician must make the ultimate judgment about the propriety of the care of a particular patient in light of all the circumstances presented by that patient. The Academy specifically disclaims any and all liability for injury or other damages of any kind, from negligence or otherwise, for any and all claims that may arise out of the use of any information contained herein. References to certain drugs, instruments, and other products in the POC are made for illustrative purposes only and are not intended to constitute an endorsement of such. Such material may include information on applications that are not considered community standard, that reflect indications not included in approved FDA labeling, or that are approved for use only in restricted research settings. The FDA has stated that it is the responsibility of the physician to determine the FDA status of each drug or device he or she wishes to use, and to use them with appropriate patient consent in compliance with applicable law.