Non-Diabetic Retinal Vascular Disease”
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Fundus Signs in Temporal Arteritis
Br J Ophthalmol: first published as 10.1136/bjo.62.9.591 on 1 September 1978. Downloaded from British Journal of Ophthalmology, 1978, 62, 591-594 Fundus signs in temporal arteritis D. McLEOD, E. 0. OJI, E. M. KOHNER, AND J. MARSHALL From Moorfields Eye Hospital and Institute of Ophthalmology, London SUMMARY A patient with temporal arteritis developed a variety of ischaemic lesions in the eyes. Infarction of the inner retina and optic nerve head was delineated on presentation by white swelling in the retinal nerve fibre layer. The role of interrupted axoplasmic transport in the production of this sign is discussed. Outer retinal infarction was also noted on presentation and subsequently gave rise to striking pigmented scars. Temporal arteritis often presents with visual loss, the central venous tributaries were of normal and necropsy examination in such cases shows wide- calibre and colour. No abnormality of the inner spread disease of the ophthalmic artery and the retina was noted in the territory of supply of the extraocular course of its ciliary and retinal branches central retinal artery. (Henkind et al., 1970). The medial and lateral At first sight the left eye showed a similar ophthal- posterior ciliary arteries supply the optic nerve head, moscopic picture, with pale swelling of the nasal the outer retina, and, in 20 to 50% of individuals, part of the optic disc and a row of fluffy white by copyright. a variable area of inner retina contiguous with the cotton-wool spots crossing the papillomacular optic disc (Hayreh, 1969); the central retinal artery bundle (Fig. 2). -
RETINAL DISORDERS Eye63 (1)
RETINAL DISORDERS Eye63 (1) Retinal Disorders Last updated: May 9, 2019 CENTRAL RETINAL ARTERY OCCLUSION (CRAO) ............................................................................... 1 Pathophysiology & Ophthalmoscopy ............................................................................................... 1 Etiology ............................................................................................................................................ 2 Clinical Features ............................................................................................................................... 2 Diagnosis .......................................................................................................................................... 2 Treatment ......................................................................................................................................... 2 BRANCH RETINAL ARTERY OCCLUSION ................................................................................................ 3 CENTRAL RETINAL VEIN OCCLUSION (CRVO) ..................................................................................... 3 Pathophysiology & Etiology ............................................................................................................ 3 Clinical Features ............................................................................................................................... 3 Diagnosis ......................................................................................................................................... -

The Acute and Long-Term Ocular Effects of Accelerated Hypertension: a Clinical and Electrophysiological Study
THE ACUTE AND LONG-TERM OCULAR EFFECTS OF ACCELERATED HYPERTENSION: A CLINICAL AND ELECTROPHYSIOLOGICAL STUDY 1 2 2 3 3 L2 S. J. TALKS , , P. GOOD , C. G. CLOUGH , D. G. BEEVERS and P. M. DODSON Birmingham SUMMARY the invention of the ophthalmoscope in 1851 the Thirty-four patients with accelerated hypertension were causes of this disturbance could be described? clinically examined. The visual evoked potential (VEP) Leibreich,4 in 1859, was the first to describe and electroretinogram (ERG) were recorded: acutely 'albuminuric retinitis' in Bright's disease. However, in 12 patients, being repeated in 7 patients up to 6 it was not until 1914, after the invention of the Riva months later. In the remaining 22 patients these tests Rocci sphygmomanometer at the end of the nine were performed 2-4 years after presentation. Visual teenth century, that Volhard and Fahr6 related the acuity was 5.6/12 in 22 of 68 (32 %) eyes at presentation retinopathy to arterial hypertension. and 5.6/12 in 10 of 58 (19%) eyes at follow-up. The It was then realised that the fundal appearance cause of severest loss of vision appeared to be anterior was associated with the severity of the hypertension ischaemic optic neuropathy, found in 3 cases. During and with the prognosis of the patient. In 1939 Keith the acute stage 11 patients (92%) had abnormal VEPs et aC drew up a four-group grading system. Grade 3 and all had abnormal ERGs. The group mean PI00 (more recently called accelerated hypertensionS) latency, of the 7 patients (14 eyes) seen acutely and consisted of 'angiospastic retinitis', 'characterised followed up at 6 months, was 123.8 ms with significant especially by oedema, cotton wool patches, and recovery of latency (p<0.005) to 110.9 ms. -

Sickle Cell Retinopathy (SCR) in a Patient with Sickle Cell Trait - a Rare Case Report
Jemds.com Case Report Sickle Cell Retinopathy (SCR) in a Patient with Sickle Cell Trait - A Rare Case Report Vandana Panjwani1, Sachin Daigavane2, Sourya Acharya3, Madhumita Prasad4 1Department of Ophthalmology, Datta Meghe Institute of Medical Sciences (Deemed to Be University), J.N. Medical College, Sawangi (M), Wardha, Maharashtra, India. 2Department of Ophthalmology, Datta Meghe Institute of Medical Sciences (Deemed to Be University), J.N. Medical College, Sawangi (M), Wardha, Maharashtra, India. 3Department of Medicine, Datta Meghe Institute of Medical Sciences (Deemed to Be University), J.N. Medical College, Sawangi (M), Wardha, Maharashtra, India. 4Department of Ophthalmology, Datta Meghe Institute of Medical Sciences (Deemed to Be University), J.N. Medical College, Sawangi (M), Wardha, Maharashtra, India. INTRODUCTION Sickle cell trait is an inherited hematologic anomaly that affects 1 million to 3 million Corresponding Author: Dr. Sourya Acharya, Americans and 8 to 10 percent of African Americans. It also affects other races like Professor, Hispanics, south Asians, Caucasians from southern Europe, and people from Middle Department of Medicine, Eastern countries. Evidence based estimations suggests that more than 100 million Datta Meghe Institute of Medical people worldwide have sickle cell trait. Unlike sickle cell disease, where two genes Sciences (Deemed to be University), that cause the production of abnormal haemoglobin, individuals with sickle cell trait J.N. Medical College, Sawangi (M), carry only one defective gene and typically live normal lives. Extreme conditions such Wardha, Maharashtra, India. as severe dehydration and high-intensity physical activity can lead to serious health E-mail: [email protected] issues, including sudden death, for individuals with sickle cell trait. -

R Manifestations in Sickle Cell Disease ( SCD) in Children
Research Article Ocular manifestations in sickle cell disease ( SCD) in children Chavan Ravindra 1, Tiple Nishikant 2*, Chavan Sangeeta 3 {1Associate Professor, 2Assistant Professor, Department of Pediatrics } { 3Sr. Resident, Department of Ophthalmology} Shri.Vasantrao Naik Gover nment Medical College, Yavatmal, Maharashtra, INDIA. Email: [email protected] Abstract Introduction: Sickle cell disease (SCD) is autosomal recessive inherited condition characterized by presence of anomalous haemoglobin ‘S’ in the erythrocytes. Patients with SCD inherit an abnormal haemoglobin which becomes insoluble when deoxygenated and so distorts th e red cells and cause tissue infarction 1,2,3 . The organs mainly affected are spleen, the bones, the kidney, the lung and the skin. But any organ may be involved and the eyes are not exemption. Hence the study is taken up to find ocular manifestation in SCD in children. Aims and Objectives: To find out prevalence, nature and outcome of ocular manifestation in SCD in children’s. Material and Methods: This prospective study was conducted in pediatrics department of tertiary care hospital from Oct 2000 to April 2002. The study group includes SCD patients admitted in pediatrics ward and patients attending SCD speciality clinics, who were electrophoretica lly confirmed for diagnosis of sickle cell haemoglobinopathy. A detail history, clinical examination and routine investigation were done in each case. A systematic ophthalmological examination was meticulously done in every case which includes visual acuit y, intraocular tension measurement, slit lamp examination and fundus examination . Observation and Results: A total of 204 cases of SCD, who were electrophoretically confirmed for diagnosis of sickle cell haemoglobinopathy were enrolled during study period, out of which 120(58.82%) patients were homozygous “SS” and 84(41.17%) patients were heterozygous “AS” for SCD. -

MOC PORT/DOCK Practice Core Modules Content Outline
MOC PORT/DOCK Practice Core Modules Content Outline 1 Cataract and Anterior Segment (10%) 1.1 Basic Anatomical and Scientific Aspects 1.1.1 The Normal Lens 1.1.1.1 Anatomy 1.2 Assessment Techniques 1.2.1 History-Taking and Preoperative Examination of Ocular Structures 1.2.1.1 Take patient history 1.2.1.2 Examine ocular structures 1.2.1.3 Signs and symptoms 1.2.1.4 Indications for surgery 1.2.1.6 External examination 1.2.1.7 Slit-lamp examination 1.2.1.8 Fundus evaluation 1.2.1.9 Impact on visual functioning and quality of life 1.2.2 Measurement of Visual and Macular Function 1.2.2.1 Visual acuity testing 1.2.2.2 Test visual acuity 1.2.2.5 Visual field testing 1.2.2.6 Test visual field 1.2.2.7 Cataract's effect on visual acuity 1.2.2.8 Estimate cataract's effect on visual acuity 1.2.2.10 Measure visual (and macular) function 1.2.4.3 Evaluate glare disability: subjective and objective 1.3 Clinical Disease Conditions and Manifestations 1.3.1 Types of Cataract 1.3.1.1 Identify types of cataracts 1.3.2 Anterior Segment Disorders 1.3.2.1 Diagnose anterior segment disorders 1.3.2.2 Cataract associated with uveitis 1.3.2.3 Diabetes mellitus and cataract formation 1.3.2.4 Lens-induced glaucoma 1.3.2.4.1 Lens particle 1.3.2.4.2 Phacolytic 1.3.2.4.3 Phacomorphic Copyright and Use Policy for ABO Content Outlines © 2017 – American Board of Ophthalmology. -

Ophthalmology July 10-11, 2018 Bangkok, Thailand
J Clin Exp Ophthalmol 2018, Volume 9 conferenceseries.com DOI: 10.4172/2155-9570-C4-088 3rd International Conference on Ophthalmology July 10-11, 2018 Bangkok, Thailand Stage of Hypertensive Retinopathy among Patients who undergone Cataract Surgery in Zamboanga City Medical Center Jerne Kaz Niels B. Paber Dr.evangelista st, sta. Catalina Background: Individuals who are not known hypertensive are noted to have blurring of vision as an initial presentation. Preventable co- morbidity such as hypertension is essential in saving sight in patients with cataract. Objective: To determine the prevalence of hypertension and stage of hypertensive retinopathy among individuals who undergone cataract surgery and to identify the association between the stage of hypertension and the risk factors for hypertension and the stage of hypertensive retinopathy. Methods: This prospective study included 203 individuals. All of the participants were noted to have mature cataract surgery done and was noted to have followed up at Tzu Chi Eye center from July 1 2017 to March 30, 2018. The nature, significance and procedure of the study were explained to every identified respondent. There was only one ophthalmologist who saw the participants who enrolled in the study. Once they understood the study, a written informed consent was taken. They were asked to answer questions provided by the researcher and their laboratory results were recorded. A follow up after 2 weeks was done in order to determine the stage of retinopathy of the patients. Demographic variables, hypertensive retinopathy, history of hypertension, medication usage, compliance, ECG changes, proteinuria, creatinine, and cardiomegaly on chest x-ray, radiographic identification of Atheromatous aorta and fundoscopic examination were analyzed. -
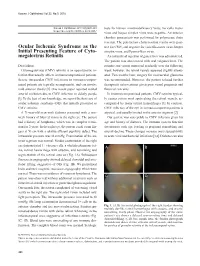
Ocular Ischemic Syndrome As the Initial Presenting Feature of Cyto
Korean J Ophthalmol Vol.32, No.5, 2018 Korean J Ophthalmol 2018;32(5):428-429 tests for human immunodeficiency virus, varicella zoster https://doi.org/10.3341/kjo.2018.0017 virus and herpes simplex virus were negative. An anterior chamber paracentesis was performed for polymerase chain reaction. The polymerase chain reaction results were posi- Ocular Ischemic Syndrome as the tive for CMV, and negative for varicella-zoster virus, herpes Initial Presenting Feature of Cyto- simplex virus, and Epstein-Barr virus. megalovirus Retinitis An intravitreal injection of ganciclovir was administered. The patient was also treated with oral valganciclovir. The Dear Editor, retinitis and vitritis improved gradually over the following Cytomegalovirus (CMV) retinitis is an opportunistic in- week; however, the retinal vessels appeared slightly attenu- fection that usually affects immunocompromised patients. ated. Two months later, surgery for neovascular glaucoma Severe intraocular CMV infections in immunocompro- was recommended. However, the patient refused further mised patients are typically asymptomatic, and can involve therapeutic interventions given poor visual prognosis and mild anterior uveitis [1]. One recent paper reported retinal financial concerns. arterial occlusion due to CMV infection in elderly people In immunocompromised patients, CMV retinitis typical- [1]. To the best of our knowledge, we report the first case of ly causes cotton wool spots along the retinal vessels, ac- ocular ischemic syndrome (OIS) that initially presented as companied by many retinal hemorrhages [1]. In contrast, CMV retinitis. CMV infection of the eye in immunocompetent patients is A 71-year-old man with diabetes presented with a one- atypical, and usually limited to the anterior segment [2]. -

Ocular Co-Morbidity in Patients with Refractive Errors in Nigeria
N igerian Journal of Ophthalmology 2011; 19(1): 19-24 Ocular Co-morbidity in Patients with Refractive Errors in Nigeria BO Adegbehingbe FWA CS, O Adeoye FWA CS, BA Adewara M BBS Ophthalmology Unit, Faculty of Clinical Sciences, Obafemi Awolowo University, Ile-Ife 1-4 ABSTRACT a high proportion of patients attend ing ophthalm ic clinics. Refractive errors can be easily d iagnosed , m easured and Purpose: To d eterm ine the pattern and prevalence of other corrected w ith spectacles or other refractive corrections to ocular problem s seen in patients w ith refractive errors attain normal vision. H ow ever, non correction or inad equate in a N igerian teaching hospital. correction of refractive errors becom es a m ajor cause of low Methods: A retrospective hospital-based review of all vision and even blind ness. Globally, there are 8 m illion consecutive patients w ho presented w ith signs and people w ho are blind and 153 m illion w ith visual sym ptom s of refractive errors at the Obafem i Aw olow o im pairm ent (presenting visual acuity <6/ 18 in the better University Teaching H ospitals Com plex betw een 1st eye) d ue to uncorrected refractive errors; this exclud es January 2007 and 31st August 2007. Patients w ho had a presbyopia.5 Poor visual outcom e in patients w ith refractive d iagnosis of refractive error and su bsequently had errors could be in part d ue to other associated ocular d etailed eye exam ination w ere includ ed in this stud y. -

Retinal Emergencies
When to Refer to RETINA Joseph M. Coney, MD February 17, 2017 Memphis, TN Financial Disclosure Commercial Interest What was received For what role Aerpio Grant Support Contracted Research Alcon Laboratories Grant Support Contracted Research Alimera Consulting Fee Consultant/Advisor Allergan Consulting Fee Consultant/Advisor Allergan Grant Support Contracted Research Apellis Grant Support Contracted Research Genentech Grant Support Contracted Research Genentech Consulting Fee Consultant/Advisor Hoffman La Roche Grant Support Contracted Research Lowy Medical Research Institute Grant Support Contracted Research Notal Vision Consulting Fee Consultant/Advisor Ohr Grant Support Contracted Research Ophthotech Grant Support Contracted Research Regeneron Equity Ownership Interest Regeneron Consulting Fee Consultant/Advisor Tyrogenex Grant Support Contracted Research Overview – Alphabet Soup . Endophthalmitis/IOI . VH . CRAO . CRVO/BRVO . PVD . NPDR/PDR . RD . ERM . NVI/NVA . MH . CNVM . VMT Endophthalmitis Hypopyon Hypopyon Bacterial Endophthalmitis . Types . Acute post-operative . Chronic post-operative . Bleb-associated . Endogenous . Intravitreal injection-related . Post-traumatic Bacterial Endophthalmitis . Course/Prognosis . Depends on . type of endophthalmitis . duration of time to presentation & Rx . virulence of organism . Bleb-associated, post-traumatic, endogenous endophthalmitis have poorest prognosis Bacterial Endophthalmitis . Presenting Symptoms . Decreased vision . Pain . Red eye . Swollen lid . Hypopyon . Most common organisms – Acute Post-op . Staphylococcus epidermidis (70%) . Other gram positives (24.2%) . Staph aureus (10%) . Streptococcus (9%) . Enterococcus (2.2%) Bacterial Endophthalmitis . Treatment . Prompt intervention critical to restore vision/salvage globe . Vitreous tap & intravitreal antibiotic injections can be done in office with no delays . In very severe or resistant cases, pars plana vitrectomy in operating room Central Retinal Artery Occlusion CRAO . Incidence . About 1:10,000 general patient visits . Most patients over 60 years . -

Eleventh Edition
SUPPLEMENT TO April 15, 2009 A JOBSON PUBLICATION www.revoptom.com Eleventh Edition Joseph W. Sowka, O.D., FAAO, Dipl. Andrew S. Gurwood, O.D., FAAO, Dipl. Alan G. Kabat, O.D., FAAO Supported by an unrestricted grant from Alcon, Inc. 001_ro0409_handbook 4/2/09 9:42 AM Page 4 TABLE OF CONTENTS Eyelids & Adnexa Conjunctiva & Sclera Cornea Uvea & Glaucoma Viitreous & Retiina Neuro-Ophthalmic Disease Oculosystemic Disease EYELIDS & ADNEXA VITREOUS & RETINA Blow-Out Fracture................................................ 6 Asteroid Hyalosis ................................................33 Acquired Ptosis ................................................... 7 Retinal Arterial Macroaneurysm............................34 Acquired Entropion ............................................. 9 Retinal Emboli.....................................................36 Verruca & Papilloma............................................11 Hypertensive Retinopathy.....................................37 Idiopathic Juxtafoveal Retinal Telangiectasia...........39 CONJUNCTIVA & SCLERA Ocular Ischemic Syndrome...................................40 Scleral Melt ........................................................13 Retinal Artery Occlusion ......................................42 Giant Papillary Conjunctivitis................................14 Conjunctival Lymphoma .......................................15 NEURO-OPHTHALMIC DISEASE Blue Sclera .........................................................17 Dorsal Midbrain Syndrome ..................................45 -

Erounds on Wednesday Mornings, the West LA VA Optometry Residents & Student Participate in Erounds
West Los Angeles VA Health Care Center, Los Angeles, CA eRounds On Wednesday mornings, the West LA VA Optometry residents & student participate in eRounds. An eRounds typically includes presentation of one or more illustrative cases of the condition under consideration. During the case presentations, trainees are asked to identify normal and abnormal findings, list ocular differential diagnoses, list systemic differential diagnoses when applicable, and state options for ocular (and systemic) management. This is usually followed by a presentation of information on the topic, which may include epidemiology, presenting signs and symptoms of the condition, clinical diagnostic testing, ancillary testing, ocular and systemic management, etc. Topics include: Acne rosacea Conjunctival actinic keratosis Conjunctivochalasis Entropion and ectropion Floppy eyelid syndrome Fat prolapse Herpetic eye disease Hyphema Neovascular glaucoma Corneal degenerations Squamous cell carcinoma of the eyelid Basal cell carcinoma of the eyelid Sebaceous carcinoma Pemphigoid Phthisis bulbi Ocular manifestations of Valsalva maneuver Xanthelasma Branch retinal artery occlusion Central retinal artery occlusion Giant cell arteritis Fibrinoplatelet retinal embolus Ophthalmic artery occlusion Multiple Hollenhorst plaques Solitary Hollenhorst plaque Best dystrophy Retinitis pigmentosa Cone-rod dystrophies Optic disc drusen Tilted disc syndrome Stargardt’s disease Diabetic retinopathy Diabetes mellitus and ocular media disorders Diabetes mellitus and neuro-ophthalmic disease