Neuro-Ophthalmological Emergency Disorders: a General View
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
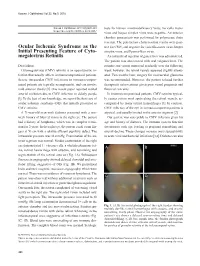
Ocular Ischemic Syndrome As the Initial Presenting Feature of Cyto
Korean J Ophthalmol Vol.32, No.5, 2018 Korean J Ophthalmol 2018;32(5):428-429 tests for human immunodeficiency virus, varicella zoster https://doi.org/10.3341/kjo.2018.0017 virus and herpes simplex virus were negative. An anterior chamber paracentesis was performed for polymerase chain reaction. The polymerase chain reaction results were posi- Ocular Ischemic Syndrome as the tive for CMV, and negative for varicella-zoster virus, herpes Initial Presenting Feature of Cyto- simplex virus, and Epstein-Barr virus. megalovirus Retinitis An intravitreal injection of ganciclovir was administered. The patient was also treated with oral valganciclovir. The Dear Editor, retinitis and vitritis improved gradually over the following Cytomegalovirus (CMV) retinitis is an opportunistic in- week; however, the retinal vessels appeared slightly attenu- fection that usually affects immunocompromised patients. ated. Two months later, surgery for neovascular glaucoma Severe intraocular CMV infections in immunocompro- was recommended. However, the patient refused further mised patients are typically asymptomatic, and can involve therapeutic interventions given poor visual prognosis and mild anterior uveitis [1]. One recent paper reported retinal financial concerns. arterial occlusion due to CMV infection in elderly people In immunocompromised patients, CMV retinitis typical- [1]. To the best of our knowledge, we report the first case of ly causes cotton wool spots along the retinal vessels, ac- ocular ischemic syndrome (OIS) that initially presented as companied by many retinal hemorrhages [1]. In contrast, CMV retinitis. CMV infection of the eye in immunocompetent patients is A 71-year-old man with diabetes presented with a one- atypical, and usually limited to the anterior segment [2]. -

Retinal Emergencies
When to Refer to RETINA Joseph M. Coney, MD February 17, 2017 Memphis, TN Financial Disclosure Commercial Interest What was received For what role Aerpio Grant Support Contracted Research Alcon Laboratories Grant Support Contracted Research Alimera Consulting Fee Consultant/Advisor Allergan Consulting Fee Consultant/Advisor Allergan Grant Support Contracted Research Apellis Grant Support Contracted Research Genentech Grant Support Contracted Research Genentech Consulting Fee Consultant/Advisor Hoffman La Roche Grant Support Contracted Research Lowy Medical Research Institute Grant Support Contracted Research Notal Vision Consulting Fee Consultant/Advisor Ohr Grant Support Contracted Research Ophthotech Grant Support Contracted Research Regeneron Equity Ownership Interest Regeneron Consulting Fee Consultant/Advisor Tyrogenex Grant Support Contracted Research Overview – Alphabet Soup . Endophthalmitis/IOI . VH . CRAO . CRVO/BRVO . PVD . NPDR/PDR . RD . ERM . NVI/NVA . MH . CNVM . VMT Endophthalmitis Hypopyon Hypopyon Bacterial Endophthalmitis . Types . Acute post-operative . Chronic post-operative . Bleb-associated . Endogenous . Intravitreal injection-related . Post-traumatic Bacterial Endophthalmitis . Course/Prognosis . Depends on . type of endophthalmitis . duration of time to presentation & Rx . virulence of organism . Bleb-associated, post-traumatic, endogenous endophthalmitis have poorest prognosis Bacterial Endophthalmitis . Presenting Symptoms . Decreased vision . Pain . Red eye . Swollen lid . Hypopyon . Most common organisms – Acute Post-op . Staphylococcus epidermidis (70%) . Other gram positives (24.2%) . Staph aureus (10%) . Streptococcus (9%) . Enterococcus (2.2%) Bacterial Endophthalmitis . Treatment . Prompt intervention critical to restore vision/salvage globe . Vitreous tap & intravitreal antibiotic injections can be done in office with no delays . In very severe or resistant cases, pars plana vitrectomy in operating room Central Retinal Artery Occlusion CRAO . Incidence . About 1:10,000 general patient visits . Most patients over 60 years . -

Eleventh Edition
SUPPLEMENT TO April 15, 2009 A JOBSON PUBLICATION www.revoptom.com Eleventh Edition Joseph W. Sowka, O.D., FAAO, Dipl. Andrew S. Gurwood, O.D., FAAO, Dipl. Alan G. Kabat, O.D., FAAO Supported by an unrestricted grant from Alcon, Inc. 001_ro0409_handbook 4/2/09 9:42 AM Page 4 TABLE OF CONTENTS Eyelids & Adnexa Conjunctiva & Sclera Cornea Uvea & Glaucoma Viitreous & Retiina Neuro-Ophthalmic Disease Oculosystemic Disease EYELIDS & ADNEXA VITREOUS & RETINA Blow-Out Fracture................................................ 6 Asteroid Hyalosis ................................................33 Acquired Ptosis ................................................... 7 Retinal Arterial Macroaneurysm............................34 Acquired Entropion ............................................. 9 Retinal Emboli.....................................................36 Verruca & Papilloma............................................11 Hypertensive Retinopathy.....................................37 Idiopathic Juxtafoveal Retinal Telangiectasia...........39 CONJUNCTIVA & SCLERA Ocular Ischemic Syndrome...................................40 Scleral Melt ........................................................13 Retinal Artery Occlusion ......................................42 Giant Papillary Conjunctivitis................................14 Conjunctival Lymphoma .......................................15 NEURO-OPHTHALMIC DISEASE Blue Sclera .........................................................17 Dorsal Midbrain Syndrome ..................................45 -

Ocular Ischemic Syndrome During Carotid Balloon Occlusion Testing
Ocular Ischemic Syndrome during Carotid Balloon Occlusion Testing Eric J. Russell, Kenneth Goldberg, James Oskin, Crystal Darling, and Onur Melen Summary: The use of a double-lumen balloon catheter for The use of a double-lumen balloon catheter for temporary occlusion testing of the internal carotid artery per temporary occlusion of the carotid artery permits mits simultaneous perfusion of the distal internal carotid artery simultaneous perfusion of the artery (with hepa (and ophthalmic artery) with heparinized saline. If saline is rinized saline) beyond the obstructing balloon. infused too rapidly, the result may be total or partial replace This helps to minimize the risk of distal throm ment of oxygenated blood within the ophthalmic artery. This replacement may produce the signs and symptoms of ocular boembolism, but saline replaces blood within the ischemic syndrome. These include ipsilateral orbital pain and carotid artery beyond the balloon. Too rapid an progressive uniocular visual loss. Simple technical adjustments infusion of saline, administered by a pressure In the performance of the occlusion test can prevent the devel pack, may result in total or partial replacement opment of this syndrome. Failure to recognize the cause of the of oxygenated blood within the ophthalmic artery observed visual loss may produce the false impression of a (Fig 1). This replacement produces the signs and positive occlusion test or may falsely suggest that a throm symptoms of ocular ischemic syndrome, includ boembolic complication has occurred. Awareness of the occur ing ipsilateral orbital pain and associated progres rence of this syndrome should prevent confusion concerning sive visual loss. the predictive result of provocative carotid occlusion testing. -

Clinical Applications of Non-Invasive Multimodality Imaging in The
The Egyptian Journal of Hospital Medicine (April 2021) Vol. 82 (3), Page 974-981 Clinical Applications of Non-Invasive Multimodality Imaging in The Evaluation of Ocular Ischemic Syndrome: A Case Study Abdulhamid Alghamdi Faculty of Medicine, Department of Ophthalmology, Taif University Email: [email protected]; Tel: +99 733 44 88 Fax: +99 733 4567 ABSTRACT Background: A 74 years old lady presented with bilateral sudden deterioration of vision over a period of 3 weeks. She is a known diabetic and hypertensive for the past 25 years. The patient denied associated neurological symptoms. The patient underwent a comprehensive non-invasive neuroimaging and retinal imaging. Case Presentation: The case study is about right sided occipital lobe infarction and right sided internal carotid artery stenosis with complete right ophthalmic artery occlusion resulted in right Ocular ischemic syndrome (OIS). Ocular findings showed normal swinging light reflex. Right eye showed rubiosis iridis, neovascularization of the disc. Left eye showed moderate non-proliferative diabetic retinopathy. There was lack of cerebellar and/or cortical constitutional symptoms. Magnetic resonance angiography (MRA) imaging showed compromised right side internal carotid system and complete occlusion of the right ophthalmic artery. Magnetic resonance imaging (MRI) showed as well isolated right sided occipital lobe infarction. The patient received neurological and ocular treatment. Conclusion: Painless sudden bilateral visual disturbance in an elderly individual should draw the clinician attention to possible cortical etiology inspite the absence of neurological symptoms. Non-invasive imaging techniques had been shown to be effective in the evaluation of symptomatic Ocular ischemic syndrome (OIS), which should be considered if the gold standards imaging techniques are relatively or absolutely contraindicated. -

Case Report of Ocular Ischemic Syndrome, Taif, Saudi Arabia
The Egyptian Journal of Hospital Medicine (January 2018) Vol. 70 (9), Page 1710-1713 Case Report of Ocular Ischemic Syndrome, Taif, Saudi Arabia Abdulmohsen Hamad Hamed Alhamyani1 , Sami Awd Alharthi, Sara Hussein A Gebril2 , Mohamed Ahmed Siddig,Osama A Alhaj , Nuha Mohamed Ahmed2, Talal Abdulrahman Althomali3 Taif medical college1, King Faisal hospital2, Taif university3 ,Taif ,Saudi Arabia ABSTRACT Background: Ocular ischemic syndrome (OIS) is more prevalent among male aged more than 50 years. Various disorders such as diabetes, hypertension, and peripheral vascular diseases are major risk factors responsible for OIS in aged male. Case report: This case study involves a 57-year-old male patient having history of diabetes, hypertension, slurred speech, hemiparesis and hypoesthesia of the right side of the body. The patient came with complain of red eye, pain and decreased vision in left eye. Complete left internal carotid artery obstruction, rubeosis iridis of the left eye, dots of hyphema of the left eye, bilateral hard exudates, significant macular edema and non-proliferative diabetic retinopathy were observed in the patient. In this case, in consultation with ophthalmology, surgery and medicine departments multidrug treatment procedure was followed. This multi- drug based therapy successfully controlled the condition of patient and improved the vision of patient. Keywords: Ocular ischemic syndrome, left internal carotid obstruction. INTRODUCTION prothrombin time 13.7 second were also Ocular ischemic syndrome (OIS ) affects vision determined to get comprehensive view of clinical and if not timely treated it may cause vision loss status of the patient. Complete blood count is [1]. Diabetes, stroke, cardiac vascular diseases, shown in table (1). -

Functional and Morphologic Study of Retinal Hypoperfusion Injury Induced
www.nature.com/scientificreports OPEN Functional and morphologic study of retinal hypoperfusion injury induced by bilateral common Received: 14 August 2018 Accepted: 20 November 2018 carotid artery occlusion in rats Published: xx xx xxxx Yali Qin 1,2, Meiqi Ji1,2, Tingting Deng3, Dan Luo2, Yingxin Zi1,2, Lin Pan3, Zhijun Wang2 & Ming Jin2 Retinal hypoperfusion injury is the pathophysiologic basis of ocular ischemic syndrome (OIS) which often leads to severe visual loss. In this study, we aimed to establish a rat model of retinal chronic hypoperfusion by bilateral common carotid artery occlusion (BCCAO) and observe changes in the retinal function and morphology. We found that model rats showed retinal arteriosclerosis, slight dilated retinal vein, small hemangiomas, hemorrhages, vascular segmental flling, and nonperfused areas after 2 weeks of BCCAO. In the model rats, the retinal circulation time was signifcantly prolonged by fuorescein fundus angiography (FFA), the latency of a and b waves was delayed and the amplitude was decreased signifcantly at each time point by electroretinogram (ERG), and the perfusion of the eyes continued to reduced. Morphologic and ultrastructural changes covered that the retinal ganglion cells (RGCs) presented obvious apoptosis and the thickness in the retinal layers were signifcantly thinner. Collectively, these fndings suggested that BCCAO induced retinal hypoperfusion injury in the model rats, thus providing an ideal animal model for the study of OIS. Retinal hypoperfusion injury is an ocular circulatory disorder caused by carotid artery stenosis or occlusion. It belongs to the category of ocular ischemic syndrome and is ofen associated with ischemic encephalopathy. Tis disorder has now become a subject of cross-disciplinary study involving both ophthalmology and neurology1. -

NIH Public Access Author Manuscript Int Ophthalmol Clin
NIH Public Access Author Manuscript Int Ophthalmol Clin. Author manuscript; available in PMC 2012 July 1. NIH-PA Author ManuscriptPublished NIH-PA Author Manuscript in final edited NIH-PA Author Manuscript form as: Int Ophthalmol Clin. 2011 ; 51(3): 27±36. doi:10.1097/IIO.0b013e31821e5960. Medical and Surgical Treatment of Neovascular Glaucoma Lisa C. Olmos, M.D., M.B.A. and Richard K. Lee, M.D., Ph.D. Bascom Palmer Eye Institute, University of Miami Miller School of Medicine Miami, FL INTRODUCTION Neovascular glaucoma (NVG) is an aggressive type of glaucoma, which often results in poor visual outcomes. Most NVG patients have severe underlying systemic and ocular pathology which causes NVG as a late presentation of their primary systemic and/or ocular disease. This makes NVG very difficult to treat. The key to adequate treatment of this devastating ocular disease is an understanding of its pathogenesis, which has recently been better elucidated. Weiss and colleagues first proposed the term “neovascular glaucoma” in 1963, when they described a severe glaucoma associated with the presence of new iris and angle vessels. (1) These patients present with elevated intraocular pressure (IOP) and neovascularization of the iris and angle, often with hyphema and other ocular findings, such as ectropion uveae (Figure 1). The myriad medical conditions resulting in NVG all lead to a final common pathway of profound retinal ischemia. This ischemia induces retinal production of vasoproliferative factors, including vascular endothelial growth factor (VEGF), which diffuse anteriorly and lead to anterior segment neovascularization of the iris (NVI) and neovascularization of the angle (NVA). -

Non-Diabetic Retinal Vascular Disease”
“Non-Diabetic Retinal Vascular Disease” Brad Sutton, O.D., F.A.A.O. Clinical Professor IU School of Optometry Indianapolis Eye Care Center Retinal Vascular Disease No financial disclosures Hypoperfusion Syndrome Occurs when the eye lacks blood perfusion secondary to carotid artery blockage or ophthalmic artery blockage. Terminology debate: venous stasis retinopathy vs. hypoperfusion syndrome Why is venous stasis retinopathy a poor term for this condition? Hypoperfusion Syndrome Patient may complain of dull, chronic ache in the affected eye Photostress issues / dazzle TIA symptoms may or may not be present (amaurosis fugax) Possible bruit / decreased pulse strength in carotid Hypoperfusion Syndrome Bruit at 30-85% blockage; swishing sound Bell vs. diaphragm Definitive diagnosis requires carotid imaging Hypoperfusion Syndrome Peripheral dot / blot hemorrhages Dilated veins Relatively spares the posterior pole Ocular Ischemic Syndrome With ocular NVD / NVE / NVI ischemic Iritis syndrome same Sluggish pupil findings plus……….. Conjunctival congestion Corneal Edema 80% unilateral / 20% bilateral Ocular Ischemic Syndrome Rare! Only 10% of eyes with 70+% blocked carotids 60% CF or worse VA by one year: 82% if NVI is present Teichopsia: colored afterimages after viewing lights More likely in patients with increased homocysteine and CRP Ocular Ischemic Syndrome When presented with Question about TIA these ocular findings……. Check carotids Arrange for carotid testing (Doppler has limits) ESR C-reactive protein CBC Ocular Ischemic Syndrome Treatment: Systemic management (diet, drugs, surgery) PRP / cryotherapy? Avastin / Lucentis / Eyelea? Five year mortality rate of 40% Sickle Cell Retinopathy Hemoglobinopathy affecting mostly AA (8% in US carry trait, .15% have SS dis.) 60,000 in US: 250,000 born yearly w-wide Malaria and natural selection (sickle trait carriers and sickle cell patients are resistant to malaria) AC, SA, SS, Sthal, SC. -

Ocular Ischaemic Syndrome
perim Ex en l & ta a l ic O p in l h Journal of Clinical & Experimental t C h f a o l m l a o Abdellaoui et al., J Clin Exp Opthamol 2018, 9:5 n l o r g u y o Ophthalmology J DOI: 10.4172/2155-9570.1000753 ISSN: 2155-9570 Case Report Open Access Ocular Ischaemic Syndrome Taoufik Abdellaoui*, Imane Tarib, Salem Joumany, Rachid Zerrouk, Karim Reda and Abdelbarre Oubaaz Department of Ophthalmology, Military teaching hospital Med-V, Rabat, Morocco *Corresponding author: Taoufik Abdellaoui, Department of Ophthalmology, Military teaching hospital Med-V, Rabat, Morocco, Tel: +212 639234211; E-mail: [email protected] Received date: August 09, 2018; Accepted date: September 24, 2018; Published date: September 28, 2018 Copyright: ©2018 Abdellaoui T, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Abstract Ocular ischaemic syndrome (OIS) is a severe form of chronic ischaemia of both anterior and posterior segments of the eye as well other orbital structures supplied by the ophthalmic artery. It is thought to be due to chronic hypoperfusion when carotid artery stenosis is greater than 90%. It typically affects patients during seventh decade or more, and it is usually associated with diabetes, heart and cerebrovascular disease. In rare cases, OIS may represent the first manifestation of a life-threatening carotid artery stenosis. This disease is often undiagnosed because it remains asymptomatic for a long period of time and has non-specific ocular manifestations. -

Orbital Ischemia, Ophthalmoparesis, and Carotid Dissection
© 1991 Raven Press, Ltd., New York !ourtlal of ClitJical Ne,mrophthaimoiosy 11(4): 284-287, 1991. Orbital Ischemia, Ophthalmoparesis, and Carotid Dissection Steven L. Galetta, M.D., Alan Leahey, M.D., Charles W. Nichols, M.D., and Eric C. Raps, M.D. We report a patient who developed an acute loss of vi Dissection of the carotid artery results when in sion in the left eye associated with proptosis, ophthal traluminal blood enters the arterial wall and sepa moparesis, conjunctival injection, and chemosis. Fun rates its component layers. Arterial dissections duscopy revealed optic disc swelling, and retinal whit may be spontaneous or secondary to minor ening consistent with an ophthalmic artery occlusion. Angiography disclosed bilateral carotid dissections pre trauma; others result from obvious blunt and pen sumably resulting from head trauma 11 days earlier. An etrating trauma to the head and neck (1). Neuro orbital ischemic syndrome may be a delayed manifesta ophthalmic complications of carotid dissection in tion of traumatic carotid dissection and precede cerebral clude amaurosis fugax (1), ischemic optic neurop hypoperfusion. athy (2,3), central retinal artery occlusion (3,4), Key Words: Orbital ischemia-Carotid dissection Ophthalmoparesis. Horner's syndrome (5), homonymous hemianop sia (6), abducens nerve palsy (7), and an ocular ischemic syndrome (8). Oculosympathetic paraly sis is the most common neuro-ophthalmologic finding in carotid dissection; it occurs in approxi mately 50% of patients (1,9). We report a patient who developed orbital ischemia and ophthalmo paresis following bilateral traumatic carotid dissec tion. CASE HISTORY Eleven days after an automobile accident, a 48 year-old man presented to the Scheie Eye Institute with a 4-hour history of painless visual loss in the left eye. -
Differential Diagnoses Symptoms and Other Useful Lists and Tables Signs for Ophthalmologists Case Presentations
Differential Diagnoses Symptoms and other Useful Lists and Tables Signs For Ophthalmologists Case Presentations Kenn Freedman MD PhD Department of Ophthalmology and Visual Sciences Texas Tech University Health Sciences Center Lubbock, Texas USA Acknowledgments and Disclaimer The differential diagnoses and lists contained herein are not meant to be exhaustive, but are to give in most cases the most common causes of many ocular / visual symptoms, signs and situations. Included also in these lists are also some less common, but serious conditions that must be “ruled-out”. These lists have been based on years of experience, and I am grateful for God’s help in developing them. I also owe gratitude to several sources* including Roy’s classic text on Ocular Differential Diagnosis. * Please see references at end of document This presentation, of course, will continue to be a work in progress and any concerns or suggestions as to errors or omissions or picture copyrights will be considered. Please feel free to contact me at [email protected] Kenn Freedman Lubbock, Texas - October 2018 Disclaimer: The diagnostic algorithm for the diagnosis and management of Ocular or Neurological Conditions contained in this presentation is not intended to replace the independent medical or professional judgment of the physician or other health care providers in the context of individual clinical circumstances to determine a patient’s care. Use of this Presentation The lists are divided into three main areas 1. Symptoms 2. Signs from the Eight Point Eye Exam 3. Common Situations and Case Presentations The index for all of the lists is given on the following 3 pages.