Understanding Your Lab Tests
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Increase of Urinary Putrescine In3,4-Benzopyrene Carcinogenesis
[CANCER RESEARCH 38, 3509-3511, October 1978] 0008-5472/78/0038-0000$02.00 Increase of Urinary Putrescine in 3,4-Benzopyrene Carcinogenesis and Its Inhibition by Putrescine Keisuke Fujita,1 Toshiharu Nagatsu, Kan Shinpo, Kazuhiro Maruta, Hisahide Takahashi, and Atsushi Sekiya Institute for Comprehensive Medical Science ¡K.F., K. S., K. M.], Research Center for Laboratory Animals ¡H.T.¡,and Department of Pharmacology ¡A.S.¡, Fujita-Gakuen University School of Medicine, Toyoake, Aichi 470-11, Japan, and Laboratory of Cell Physiology, Department of Life Chemistry, Graduate School at Nagatsuta, Tokyo Institute of Technology, Yokohama 227, Japan ¡T.N.¡ ABSTRACT were included. Thirty female BALB/c mice, 19 to 20 weeks old and 25 to 30 g body weight, were given s.c. injections of A significant increase in putrescine was noted in the 2.52 mg of 3,4-benzopyrene in 0.5 ml of tricaprylin (Group urine of mice with experimental s.c. tumors induced by a B) or of 2.52 mg of 3,4-benzopyrene plus 10 mg of putres single injection of 3,4-benzopyrene solution (2.52 mg of cine dissolved in 0.5 ml of tricaprylin (Group B + P). As 3,4-benzopyrene in 0.5 ml of tricaprylin). When 10 mg of controls, 30 mice were given injections of 0.5 ml of tricapry putrescine were added to the 3,4-benzopyrene solution, lin (Group C), and 15 mice received 10 mg of putrescine in the development of tumors was completely inhibited and 0.5 ml of tricaprylin (Group P). -

MEDICAL DIRECTIVE Point of Care Glucose Meter Testing And
MEDICAL DIRECTIVE Point of Care Glucose Meter Testing and Treatment for Out-Patients with Suspected Hypoglycemia in the Diabetes Education Program Approved by/Date: Medical Advisory Comm. – June 25, 2013 Authorizing physician(s) Dr. Rachel Chong Dr. Angeline Chong Dr. Theodore Monchesky Authorized to whom Nurses and dietitians working in the diabetes education program at LH who have received education and validation of glucose meter testing according to Ontario Laboratory Accreditation Standards (OLA). Patient Description / Population Any outpatient 18 years of age or older at LH exhibiting signs or symptoms of hypoglycemia. Any outpatient 18 years of age or older suspected of having hypoglycemia. Medical Directive Description/Physician’s Order The nurse/dietitian will obtain a capillary blood sample from a patient’s finger upon suspecting hypoglycemia. The nurse/dietitian will perform a blood glucose meter test, and treat hypoglycemia as per protocol outlined below. Patient/Population Description: All LH Patients 18 years and over registered with the LH Diabetes Education Program. Contraindications to implementing the Protocol: • Patients unwilling or unable to provide blood sample. • Patient less than 18 years of age • Refusal of patient/family consent for testing and/or treatment; call code blue and 911 immediately Originating Committee: RNS Program Council – Feb 26, 2013 Medical Advisory Committee: June 25, 2013 This material has been prepared solely for the use at Lakeridge Health. Lakeridge Health accepts no responsibility for use of this material by any person or organization not associated with Lakeridge Health. No part of this document may be reproduced in any form for publication without the permission of Lakeridge Health. -

Diabetes Control in Thyroid Disease
In Brief Thyroid disease is commonly found in most types of diabetes. This article defines the prevalence of thyroid disease in diabetes and elucidates through case studies the assessment, diagnosis, and clinical management of thyroid disease in diabetes. Diabetes Control in Thyroid Disease Thyroid disease is a pathological state abnormality. Several studies, including that can adversely affect diabetes con- the Colorado study, have documented trol and has the potential to negative- a higher prevalence of thyroid disease Jennal L. Johnson, MS, RNC, FNP, ly affect patient outcomes. Thyroid in women, with prevalence rates rang- BC-ADM, CDE disease is found commonly in most ing from 4 to 21%, whereas the rate in forms of diabetes and is associated men ranges from 2.8 to 16%.1 with advanced age, particularly in Thyroid disease increases with age. In type 2 diabetes and underlying the Colorado study, the 18-year-olds autoimmune disease in type 1 dia- had a prevalence rate of 3.5% com- betes. This article defines the preva- pared with a rate of 18.5% for those lence of thyroid disease in diabetes, ≥ 65 years of age. discusses normal physiology and The prevalence of thyroid disease in screening recommendations for thy- diabetes has been estimated at 10.8%,2 roid disease, and elucidates through with the majority of cases occurring as case studies the assessment, diagnosis, hypothyroidism (~ 30%) and subclini- and clinical management of thyroid cal hypothyroidism (~ 50%).2 Hyper- disease and its impact on diabetes. thyroidism accounts for 12%, and postpartum thyroiditis accounts for Thyroid Disease Prevalence 11%.2 Of the female patients with The prevalence of thyroid disease in type 1 diabetes, 30% have thyroid dis- the general population is estimated to ease, with a rate of postpartum thy- be 6.6%, with hypothyroidism the roid disease three times that of the most common malady.1 Participants normal population. -

Predictors of Autoimmune Hemolytic Anemia in Beta-Thalassemia
Blood Cells, Molecules and Diseases 79 (2019) 102342 Contents lists available at ScienceDirect Blood Cells, Molecules and Diseases journal homepage: www.elsevier.com/locate/bcmd Predictors of autoimmune hemolytic anemia in beta-thalassemia patients with underlying red blood cells autoantibodies T ⁎ Monia Ben Khaleda,b, , Monia Ouedernia,b, Nessrine Sahlia,b, Nawel Dhouibb, Ahmed Ben Abdelazizc, Samia Rekayaa,b, Ridha Koukia,b, Houda Kaabid, Hmida Slamad, Fethi Melloulia,b, Mohamed Bejaouia,b a Faculty of Medicine, University of Tunis El Manar, Tunis, Tunisia b Pediatric Immuno-Hematology Unit, Bone Marrow Transplantation Center Tunis, Tunis, Tunisia c Information System Directions, Sahloul University Hospital, Sousse, Tunisia d National Center of Blood Transfusion, Tunis, Tunisia ARTICLE INFO ABSTRACT Editor: Mohandas Narla In beta-thalassemia patients, erythrocyte autoantibodies can remain silent or lead to Autoimmune Hemolytic Keywords: Anemia (AIHA).The aim of this study was to identify predictors of AIHA in beta-thalassemia patients with Autoimmune hemolytic anemia positive Direct Antiglobulin Test (DAT), in Tunisia. Thalassemia This longitudinal prognosis study was carried out on beta-thalassemia patients with a positive confirmed Transfusion DAT. Predictors of AIHA were identified the Kaplan-Meier method. A Cox model analysis was used to identify Autoantibodies independent predictors. Red blood cells Among 385 beta thalassemia patients, 87 developed positive DAT (22.6%). Autoimmune hemolytic anemia Direct antiglobulin test was occurred in 25 patients. Multivariate analysis showed that AIHA was independently associated with beta- thalassemia intermedia and similar family history of AIHA. Splenectomy in patients with positive DAT was independently associated with an increased risk of AIHA (HR = 6.175, CI: 2.049–18.612, p < 0.001). -

Effect of Thyroid Hormones on Kidney Function in Patients After
www.nature.com/scientificreports OPEN Efect of Thyroid Hormones on Kidney Function in Patients after Kidney Transplantation Benjamin Schairer1, Viktoria Jungreithmayr2, Mario Schuster2, Thomas Reiter 1, Harald Herkner3, Alois Gessl4, Gürkan Sengölge1* & Wolfgang Winnicki 1 Elevated levels of thyroid-stimulating-hormone (TSH) are associated with reduced glomerular fltration rate (GFR) and increased risk of developing chronic kidney disease even in euthyroid patients. Thyroid hormone replacement therapy has been shown to delay progression to end-stage renal disease in sub-clinically hypothyroid patients with renal insufciency. However, such associations after kidney transplantation were never investigated. In this study the association of thyroid hormones and estimated GFR (eGFR) in euthyroid patients after kidney transplantation was analyzed. In total 398 kidney transplant recipients were assessed retrospectively and association between thyroid and kidney function parameters at and between defned time points, 12 and 24 months after transplantation, was studied. A signifcant inverse association was shown for TSH changes and eGFR over time between months 12 and 24 post transplantation. For each increase of TSH by 1 µIU/mL, eGFR decreased by 1.34 mL/min [95% CI, −2.51 to −0.16; p = 0.03], corresponding to 2.2% eGFR decline, within 12 months. At selected time points 12 and 24 months post transplantation, however, TSH was not associated with eGFR. In conclusion, an increase in TSH between 12 and 24 months after kidney transplantation leads to a signifcant decrease in eGFR, which strengthens the concept of a kidney- thyroid-axis. Interactions between thyroid hormones and kidney function have been suggested in previous studies. -

Metabolic Regulation of Heme Catabolism and Bilirubin Production
Metabolic Regulation of Heme Catabolism and Bilirubin Production. I. HORMONAL CONTROL OF HEPATIC HEME OXYGENASE ACTIVITY Arne F. Bakken, … , M. Michael Thaler, Rudi Schmid J Clin Invest. 1972;51(3):530-536. https://doi.org/10.1172/JCI106841. Research Article Heme oxygenase (HO), the enzyme system catalyzing the conversion of heme to bilirubin, was studied in the liver and spleen of fed, fasted, and refed rats. Fasting up to 72 hr resulted in a threefold increase in hepatic HO activity, while starvation beyond this period led to a gradual decline in enzyme activity. Refeeding of rats fasted for 48 hr depressed hepatic HO activity to basal values within 24 hr. Splenic HO was unaffected by fasting and refeeding. Hypoglycemia induced by injections of insulin or mannose was a powerful stimulator of hepatic HO. Glucose given together with the insulin abolished the stimulatory effect of the latter. Parenteral treatment with glucagon led to a twofold, and with epinephrine to a fivefold, increase of hepatic HO activity; arginine, which releases endogenous glucagon, stimulated the enzyme fivefold. These stimulatory effects of glucagon and epinephrine could be duplicated by administration of cyclic adenosine monophosphate (AMP), while thyroxine and hydroxortisone were ineffective. Nicotinic acid, which inhibits lipolysis, failed to modify the stimulatory effect of epinephrine. None of these hormones altered HO activity in the spleen. These findings demonstrate that the enzymatic mechanism involved in the formation of bilirubin from heme in the liver is stimulated by fasting, hypoglycemia, epinephrine, glucagon, and cyclic AMP. They further suggest that the enzyme stimulation produced by fasting may be […] Find the latest version: https://jci.me/106841/pdf Metabolic Regulation of Heme Catabolism and Bilirubin Production I. -

Emerging and Dynamic Biomedical Uses of Ferritin
pharmaceuticals Review Emerging and Dynamic Biomedical Uses of Ferritin Brian Chiou and James R. Connor * Department of Neurosurgery, Penn State College of Medicine, Hershey, PA 17033, USA; [email protected] * Correspondence: [email protected]; Tel.: +1-717-531-4541 Received: 24 October 2018; Accepted: 12 November 2018; Published: 13 November 2018 Abstract: Ferritin, a ubiquitously expressed protein, has classically been considered the main iron cellular storage molecule in the body. Owing to the ferroxidase activity of the H-subunit and the nucleation ability of the L-subunit, ferritin can store a large amount of iron within its mineral core. However, recent evidence has demonstrated a range of abilities of ferritin that extends well beyond the scope of iron storage. This review aims to discuss novel functions and biomedical uses of ferritin in the processes of iron delivery, delivery of biologics such as chemotherapies and contrast agents, and the utility of ferritin as a biomarker in a number of neurological diseases. Keywords: ferritin; iron; iron delivery; nanotechnology; nanocage; drug delivery; inflammation; serum biomarker 1. Ferritin Introduction Ferritin, a protein originally identified in 1937 by Vilém Laufberger [1], is a ubiquitously expressed iron storage protein most commonly characterized by its ability to accumulate and store up to 4500 atoms of iron [2]. Ferritin consists of 24 subunits, typically comprised of different ratios of the H and L chain subunit. The ratios vary by organ and even by cell type. Importantly, the different subunits have divergent functions—H-ferritin utilizes ferroxidase activity that is necessary for the oxidation of ferrous (Fe2+) to ferric (Fe3+) iron while L-ferritin contains acidic residues on the surface cavity of the protein that facilitate ferroxidase turnover and are crucial for the nucleation of ferric iron within the core of the fully formed protein. -

Cold Type Autoimmune Hemolytic Anemia- a Rare Manifestation Of
Dematapitiya et al. BMC Infectious Diseases (2019) 19:68 https://doi.org/10.1186/s12879-019-3722-z CASE REPORT Open Access Cold type autoimmune hemolytic anemia- a rare manifestation of infectious mononucleosis; serum ferritin as an important biomarker Chinthana Dematapitiya1*, Chiara Perera2, Wajira Chinthaka1, Solith Senanayaka1, Deshani Tennakoon1, Anfas Ameer1, Dinesh Ranasinghe1, Ushani Warriyapperuma1, Suneth Weerarathna1 and Ravindra Satharasinghe1 Abstract Background: Infectious mononucleosis is one of the main manifestations of Epstein – Barr virus, which is characterized by fever, tonsillar-pharyngitis, lymphadenopathy and atypical lymphocytes. Although 60% of patients with IMN develop cold type antibodies, clinically significant hemolytic anemia with a high ferritin level is very rare and validity of serum ferritin as an important biomarker has not been used frequently. Case presentation: 18-year-old girl presented with fever, malaise and sore throat with asymptomatic anemia, generalized lymphadenopathy, splenomegaly and mild hepatitis. Investigations revealed that she had cold type autoimmune hemolysis, significantly elevated serum ferritin, elevated serum lactate dehydrogenase level with serological evidence of recent Epstein Barr infection. She was managed conservatively and her hemoglobin and serum ferritin levels normalized without any intervention following two weeks of the acute infection. Conclusion: Cold type autoimmune hemolytic anemia is a rare manifestation of infectious mononucleosis and serum ferritin is used very rarely as an important biomarker. Management of cold type anemia is mainly supportive and elevated serum ferritin indicates severe viral disease. Keywords: Infectious mononucleosis (IMN), Hemolytic anemia, Ferritin Background mainly Mycoplasma pneumoniae and infectious mono- Epstein – Barr virus is one of the most ubiquitous human nucleosis (IMN). Diagnosis of cold type AIHA due to viruses, infecting more than 95% the adult population IMN is confirmed by demonstrating red cell aggregates in worldwide. -

Jaundice Protocol
fighting childhood liver disease Jaundice Protocol Early identification and referral of liver disease in infants fighting childhood liver disease 36 Great Charles Street Birmingham B3 3JY Telephone: 0121 212 3839 yellowalert.org childliverdisease.org [email protected] Registered charity number 1067331 (England & Wales); SC044387 (Scotland) The following organisations endorse the Yellow Alert Campaign and are listed in alphabetical order. 23957 CLDF Jaundice Protocol.indd 1 03/08/2015 18:25:24 23957 3 August 2015 6:25 PM Proof 1 1 INTRODUCTION This protocol forms part of Children’s Liver Disease Foundation’s (CLDF) Yellow Alert Campaign and is written to provide general guidelines on the early identification of liver disease in infants and their referral, where appropriate. Materials available in CLDF’s Yellow Alert Campaign CLDF provides the following materials as part of this campaign: • Yellow Alert Jaundice Protocol for community healthcare professionals • Yellow Alert stool colour book mark for quick and easy reference • Parents’ leaflet entitled “Jaundice in the new born baby”. CLDF can provide multiple copies to accompany an antenatal programme or for display in clinics • Yellow Alert poster highlighting the Yellow Alert message and also showing the stool chart 2 GENERAL AWARENESS AND TRAINING The National Institute of Health and Clinical Excellence (NICE) has published a clinical guideline on neonatal jaundice which provides guidance on the recognition, assessment and treatment of neonatal jaundice in babies from birth to 28 days. Neonatal Jaundice Clinical Guideline guidance.nice.org.uk cg98 For more information go to nice.org.uk/cg98 • Jaundice Community healthcare professionals should be aware that there are many causes for jaundice in infants and know how to tell them apart: • Physiological jaundice • Breast milk jaundice • Jaundice caused by liver disease • Jaundice from other causes, e.g. -

Bone Marrow (Stem Cell) Transplant for Sickle Cell Disease Bone Marrow (Stem Cell) Transplant
Bone Marrow (Stem Cell) Transplant for Sickle Cell Disease Bone Marrow (Stem Cell) Transplant for Sickle Cell Disease 1 Produced by St. Jude Children’s Research Hospital Departments of Hematology, Patient Education, and Biomedical Communications. Funds were provided by St. Jude Children’s Research Hospital, ALSAC, and a grant from the Plough Foundation. This document is not intended to take the place of the care and attention of your personal physician. Our goal is to promote active participation in your care and treatment by providing information and education. Questions about individual health concerns or specifi c treatment options should be discussed with your physician. For more general information on sickle cell disease, please visit our Web site at www.stjude.org/sicklecell. Copyright © 2009 St. Jude Children’s Research Hospital How did bone marrow (stem cell) transplants begin for children with sickle cell disease? Bone marrow (stem cell) transplants have been used for the treatment and cure of a variety of cancers, immune system diseases, and blood diseases for many years. Doctors in the United States and other countries have developed studies to treat children who have severe sickle cell disease with bone marrow (stem cell) transplants. How does a bone marrow (stem cell) transplant work? 2 In a person with sickle cell disease, the bone marrow produces red blood cells that contain hemoglobin S. This leads to the complications of sickle cell disease. • To prepare for a bone marrow (stem cell) transplant, strong medicines, called chemotherapy, are used to weaken or destroy the patient’s own bone marrow, stem cells, and infection fi ghting system. -

Leukocyte Esterase Activity in Vaginal Fluid of Pregnant and Non-Pregnant Women with Vaginitis/Vaginosis and in Controls
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by PubMed Central Infect Dis Obstet Gynecol 2003;11:19–26 Leukocyte esterase activity in vaginal fluid of pregnant and non-pregnant women with vaginitis/vaginosis and in controls Per-Anders Mårdh 1, Natalia Novikova 1, Ola Niklasson 1, Zoltan Bekassy 1 and Lennart Skude 2 1Department of Obstetrics and Gynecology, University Hospital, Lund and 2Department of Clinical Chemistry, County Hospital, Halmstad, Sweden Objectives: Todeterminethe leukocyteesterase (LE) activity invaginal lavage fluid ofwomen with acuteand recurrentvulvovaginal candidosis (VVC and RVVC respectively), bacterial vaginosis(BV), and in pregnant and non-pregnantwomen without evidenceof the threeconditions. Also tocompare the resultof LEtestsin women consultingat differentweeks inthe cycle andtrimesters of pregnancy.The LEactivity was correlatedto vaginal pH, numberof inflammatory cells instained vaginal smears,type of predominatingvaginal bacteria andpresence of yeast morphotypes. Methods: Onehundred and thirteen women with ahistoryof RVVC,i.e. with at least fourattacks of the conditionduring the previousyear and who had consultedwith anassumed new attack ofthe condition,were studied.Furthermore, we studied16 women with VVC,15 women with BV,and 27 women attendingfor control of cytological abnormalities, who all presentedwithout evidenceof either vaginitisor vaginosis. Finally, 73 pregnantwomen wereinvestigated. The LEactivity invaginal fluid duringdifferent weeks inthe cycle of 53 of the women was measured. Results: Inthe non-pregnantwomen, anincreased LE activity was foundin 96, 88, 73 and56% of those with RVVC,VVC and BV andin the non-VVC/BVcases,respectively. In 73% of pregnantwomen inthe second trimester,and 76% of thosein the third,the LEtestwas positive.In all groupsof non-pregnantwomen tested, the LEactivity correlatedwith the numberof leukocytesin vaginal smears,but it didnot in those who were pregnant.There was nocorrelation between LE activity andweek incycle. -
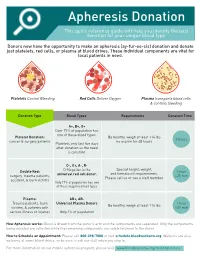
Apheresis Donation This Quick Reference Guide Will Help You Identify the Best Donation for Your Unique Blood Type
Apheresis Donation This quick reference guide will help you identify the best donation for your unique blood type. Donors now have the opportunity to make an apheresis (ay-fur-ee-sis) donation and donate just platelets, red cells, or plasma at blood drives. These individual components are vital for local patients in need. Platelets Control Bleeding Red Cells Deliver Oxygen Plasma transports blood cells & controls bleeding Donation Type Blood Types Requirements Donation Time A+, B+, O+ Over 75% of population has one of these blood types. Platelet Donation: Be healthy, weigh at least 114 lbs 2 hours cancer & surgery patients no aspirin for 48 hours Platelets only last five days after donation so the need is constant. O-, O+, A-, B- Special height, weight, Double Red: O-Negative is the 1 hour and hematocrit requirements. surgery, trauma patients, universal red cell donor. +25 min Please call us or see a staff member accident, & burn victims Only 17% of population has one of these negative blood types Plasma: AB+, AB- Trauma patients, burn Universal Plasma Donors 1 hour Be healthy, weigh at least 114 lbs victims, & patients with +30 min serious illness or injuries Only 4% of population How Apheresis works: Blood is drawn from the donor’s arm and the components are separated. Only the components being donated are collected while the remaining components are safely returned to the donor How to Schedule an Appointment: Please call 800-398-7888 or visit schedule.bloodworksnw.org. Walk-ins are also welcome at some blood drives, so be sure to ask our staff when you stop in.