Contact Allergy—Emerging Allergens and Public Health Impact
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

A Diagnostic Approach to Pruritus
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by DigitalCommons@University of Nebraska University of Nebraska - Lincoln DigitalCommons@University of Nebraska - Lincoln U.S. Air Force Research U.S. Department of Defense 2011 A Diagnostic Approach to Pruritus Brian V. Reamy Christopher W. Bunt Stacy Fletcher Follow this and additional works at: https://digitalcommons.unl.edu/usafresearch This Article is brought to you for free and open access by the U.S. Department of Defense at DigitalCommons@University of Nebraska - Lincoln. It has been accepted for inclusion in U.S. Air Force Research by an authorized administrator of DigitalCommons@University of Nebraska - Lincoln. A Diagnostic Approach to Pruritus BRIAN V. REAMY, MD, Uniformed Services University of the Health Sciences, Bethesda, Maryland CHRISTOPHER W. BUNT, MAJ, USAF, MC, and STACY FLETCHER, CAPT, USAF, MC Ehrling Bergquist Family Medicine Residency Program, Offutt Air Force Base, Nebraska, and the University of Nebraska Medical Center, Omaha, Nebraska Pruritus can be a symptom of a distinct dermatologic condition or of an occult underlying systemic disease. Of the patients referred to a dermatologist for generalized pruritus with no apparent primary cutaneous cause, 14 to 24 percent have a systemic etiology. In the absence of a primary skin lesion, the review of systems should include evaluation for thyroid disorders, lymphoma, kidney and liver diseases, and diabetes mellitus. Findings suggestive of less seri- ous etiologies include younger age, localized symptoms, acute onset, involvement limited to exposed areas, and a clear association with a sick contact or recent travel. Chronic or general- ized pruritus, older age, and abnormal physical findings should increase concern for underly- ing systemic conditions. -

Pompholyx Factsheet Pompholyx Eczema (Also Known As Dyshidrotic Eczema/Dermatitis) Is a Type of Eczema That Usually Affects the Hands and Feet
12 Pompholyx factsheet Pompholyx eczema (also known as dyshidrotic eczema/dermatitis) is a type of eczema that usually affects the hands and feet. In most cases, pompholyx eczema involves the development of intensely itchy, watery blisters, mostly affecting the sides of the fingers, the palms of the hands and soles of the feet. Some people have pompholyx eczema on their hands and/or feet with other types of eczema elsewhere on the body. This condition can occur at any age but is usually seen in adults under 40, and is more common in women. The skin is initially very itchy with a burning sensation of heat and prickling in the palms and/or soles. Then comes a sudden crop of small blisters (vesicles), which turn into bigger weepy blisters, which can become infected, causing redness, pain, swelling and pustules. There is often subsequent peeling as the skin dries out, and then the skin can become red and dry with painful cracks (skin fissures). Pompholyx eczema can also affect the nail folds and skin around the nails, causing swelling (paronychia). What causes it? A reaction could be the result of contact with potential irritants such as soap, detergents, solvents, acids/alkalis, The exact causes of pompholyx eczema are not known, chemicals and soil, causing irritant contact dermatitis. Or although it is thought that factors such as stress, there could be an allergic reaction to a substance that is sensitivity to metal compounds (such as nickel, cobalt or not commonly regarded as an irritant, such as rubber or chromate), heat and sweating can aggravate this nickel, causing allergic contact dermatitis. -

Hand Dermatitis – Contact Dermatitis David E
3/2/2021 Hand Dermatitis – Contact Dermatitis David E. Cohen, M.D., M.P.H. Charles and Dorothea Harris Professor and Vice Chairman for Clinical Affairs Director of Allergic, Occupational and Environmental Dermatology New York University School of Medicine Department of Dermatology IEC 2021 Hand Eczema Virtual Symposium 1 •David E Cohen has declared the following financial interests: . Consultant and Honorarium: . Ferndale Laboratories, . Asana . Medimetriks . Leo . UCB . Cutanea [past] . Ferrer [past] . Celgene [past] . Novartis . Dermavant . FSJ . FIDE. (FIDE receives industry sponsorship from AbbVie, Almirall, Amgen, Bausch and Lomb, Bristol- Myers Squibb, Celgene Dermavant, Dermira, Janssen, Kyowa Hakko Kirin, LEO, Lilly, Novartis, Ortho Dermatologics, Pfizer, Sanofi Genzyme, Sun Pharma, UCB, Valeant) . Cosmetic Ingredient Review (CIR) •Stock or stock options: Dermira [past], Medimetriks [past], Brickell Biotech, Kadmon, Evommune, Timber •Board of Directors: Kadmon, Timber, Evommune, [Dermira-Past] I will discuss non-FDA approved patch test allergens, and emerging therapies 2 Hand Dermatitis • General population prevalence is 5% to 10% . Health care workers, exposed to wet work, frequent hand washing, and AD. Atopic dermatitis (AD) is recognized as the top risk factor Causes: • Exogenous: Irritant and Allergic Contact Dermatitis • Endogenous: Psoriasis, Dyshidrosis, Atopic Dermatitis, Nummular • ID • HYBRID • Spectrum for eczematous disease is vesicular and eroded to hyperkeratotic and fissured • Hand Psoriasis may have higher rates of allergic contact dermatitis. Int J Occup Environ Health. 2018 Jan 23:1-10. Ther Clin Risk Manag. 2020 Dec 31;16:1319-1332. doi: Contact Dermatitis. 2014 Jan;70(1):44-55. 10.2147/TCRM.S292504.eCollection 2020 Indian Dermatol Online J. 2012 Sep;3(3):177-81. -

Photodermatoses Update Knowledge and Treatment of Photodermatoses Discuss Vitamin D Levels in Photodermatoses
Ashley Feneran, DO Jenifer Lloyd, DO University Hospitals Regional Hospitals AMERICAN OSTEOPATHIC COLLEGE OF DERMATOLOGY Objectives Review key points of several photodermatoses Update knowledge and treatment of photodermatoses Discuss vitamin D levels in photodermatoses Types of photodermatoses Immunologically mediated disorders Defective DNA repair disorders Photoaggravated dermatoses Chemical- and drug-induced photosensitivity Types of photodermatoses Immunologically mediated disorders Polymorphous light eruption Actinic prurigo Hydroa vacciniforme Chronic actinic dermatitis Solar urticaria Polymorphous light eruption (PMLE) Most common form of idiopathic photodermatitis Possibly due to delayed-type hypersensitivity reaction to an endogenous cutaneous photo- induced antigen Presents within minutes to hours of UV exposure and lasts several days Pathology Superficial and deep lymphocytic infiltrate Marked papillary dermal edema PMLE Treatment Topical or oral corticosteroids High SPF Restriction of UV exposure Hardening – natural, NBUVB, PUVA Antimalarial PMLE updates Study suggests topical vitamin D analogue used prophylactically may provide therapeutic benefit in PMLE Gruber-Wackernagel A, Bambach FJ, Legat A, et al. Br J Dermatol, 2011. PMLE updates Study seeks to further elucidate the pathogenesis of PMLE Found a decrease in Langerhans cells and an increase in mast cell density in lesional skin Wolf P, Gruber-Wackernagel A, Bambach I, et al. Exp Dermatol, 2014. Actinic prurigo Similar to PMLE Common in native -

Steroid Use in Prednisone Allergy Abby Shuck, Pharmd Candidate
Steroid Use in Prednisone Allergy Abby Shuck, PharmD candidate 2015 University of Findlay If a patient has an allergy to prednisone and methylprednisolone, what (if any) other corticosteroid can the patient use to avoid an allergic reaction? Corticosteroids very rarely cause allergic reactions in patients that receive them. Since corticosteroids are typically used to treat severe allergic reactions and anaphylaxis, it seems unlikely that these drugs could actually induce an allergic reaction of their own. However, between 0.5-5% of people have reported any sort of reaction to a corticosteroid that they have received.1 Corticosteroids can cause anything from minor skin irritations to full blown anaphylactic shock. Worsening of allergic symptoms during corticosteroid treatment may not always mean that the patient has failed treatment, although it may appear to be so.2,3 There are essentially four classes of corticosteroids: Class A, hydrocortisone-type, Class B, triamcinolone acetonide type, Class C, betamethasone type, and Class D, hydrocortisone-17-butyrate and clobetasone-17-butyrate type. Major* corticosteroids in Class A include cortisone, hydrocortisone, methylprednisolone, prednisolone, and prednisone. Major* corticosteroids in Class B include budesonide, fluocinolone, and triamcinolone. Major* corticosteroids in Class C include beclomethasone and dexamethasone. Finally, major* corticosteroids in Class D include betamethasone, fluticasone, and mometasone.4,5 Class D was later subdivided into Class D1 and D2 depending on the presence or 5,6 absence of a C16 methyl substitution and/or halogenation on C9 of the steroid B-ring. It is often hard to determine what exactly a patient is allergic to if they experience a reaction to a corticosteroid. -
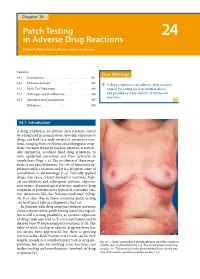
Patch Testing in Adverse Drug Reactions Has Not Always Been Appreciated, but There Is Growing a Interest in This Field
24_401_412 05.11.2005 10:37 Uhr Seite 401 Chapter 24 Patch Testing 24 in Adverse Drug Reactions Derk P.Bruynzeel, Margarida Gonçalo Contents Core Message 24.1 Introduction . 401 24.2 Pathomechanisms . 403 í A drug eruption is an adverse skin reaction 24.3 Patch Test Indications . 404 caused by a drug used in normal doses 24.4 Technique and Test Materials . 406 and presents a wide variety of cutaneous reactions. 24.5 Relevance and Consequences . 407 References . 408 24.1 Introduction A drug eruption is an adverse skin reaction caused by a drug used in normal doses. Systemic exposure to drugs can lead to a wide variety of cutaneous reac- tions, ranging from erythema, maculopapular erup- tions (the most frequent reaction pattern), acrovesic- ular dermatitis, localized fixed drug eruptions, to toxic epidermal necrolysis and from urticaria to anaphylaxis (Figs. 1, 2). The incidence of these erup- tions is not exactly known; 2%–5% of inpatients ex- perience such a reaction and it is a frequent cause of consultation in dermatology [1–3]. Topically applied drugs may cause contact dermatitis reactions. Topi- cal sensitization and subsequent systemic exposure may induce dermatological patterns similar to drug eruptions or patterns more typical of a systemic con- tact dermatitis, like the “baboon syndrome” (Chap. 16). It is clear that, in these situations, patch testing can be of great help as a diagnostic tool [4]. In patients with drug eruptions without previous contact sensitization, patch testing seems less logical, but is still a strong possibility, as systemic exposure of drugs may also lead to T-cell sensitization and to delayed type IV hypersensitivity reactions [5–8]. -

Clinical and Basic Immunodermatology Clinical and Basic Immunodermatology
Clinical and Basic Immunodermatology Clinical and Basic Immunodermatology Edited by Anthony A. Gaspari, MD Department of Dermatology University of Maryland School of Medicine Baltimore, MD USA Stephen K. Tyring, MD, PhD Department of Dermatology University of Texas Medical School at Houston Houston, TX USA Editors Anthony A. Gaspari, MD University of Maryland School of Medicine Baltimore, MD USA Stephen K. Tyring, MD, PhD University of Texas Medical School at Houston Houston, TX USA ISBN 978-1-84800-164-0 e-ISBN 978-1-84800-165-7 DOI 10.1007/978-1-84800-165-7 British Library Cataloguing in Publication Data A catalogue record for this book is available from the British Library Library of Congress Control Number: 2008923739 © Springer-Verlag London Limited 2008 Apart from any fair dealing for the purposes of research or private study, or criticism or review, as permitted under the Copyright, Designs and Patents Act 1988, this publication may only be reproduced, stored or transmitted, in any form or by any means, with the prior permission in writing of the publishers, or in the case of reprographic reproduction in accordance with the terms of licences issued by the Copyright Licensing Agency. Enquiries concerning reproduction outside those terms should be sent to the publishers. The use of registered names, trademarks, etc. in this publication does not imply, even in the absence of a specific statement, that such names are exempt from the relevant laws and regulations and therefore free for general use. Product liability: The publisher can give no guarantee for information about drug dosage and application thereof contained in this book. -

Immunodermatology
Editorial Volume 8:2,2021 Journal of Dermatology and Dermatologic Diseases ISSN: 2684-4281 Open Access Editorial Note on Immunodermatology Bindu Madhavi* Department of Biotechnology, Vignan’s University, Vadlamudi Editorial Immunodermatology studies the skin as an invulnerable organ of both health and infection. Many ranges, such as photographic immunology (impacts of ultraviolet light on skin resistance), provocative diseases, are uncommonly considered, For starters, unfavourably prone contact dermatitis and atopic inflammation of the skin, immune system-related skin conditions such as vitiligo and psoriasis, and finally, the immunology of microbial skin infections such as retrovirus contamination and impurity. This area has some experience treating non-susceptible interceptible skin diseases like lupus, bullous pemphigoid, pemphigus vulgaris, and other skin problems that can be safely intervened. The skin has a great influence on ensuring shape against infection as an unpredictable invulnerable organ. Inalienable resistance requires an early reaction to remote antigens, so it is not a specific pathogen, whereas an adjustable reaction to the differentiation of antigens and the advancement of memory is specific, but it takes more time to function. Infections have strengthened mechanisms to prevent their descendants from contaminating or discharging the skin-resistant reaction. By managing a rapid invulnerable response, with abnormal levels of protective antibodies to their target viral antigens, immunizations may safeguard against infections. -

Psoriasis Review
JULY 2018 VOL 14 NUMBER 2 PSORIASIS REVIEW Included in this Issue 1 Top 5 Research and Clinical Papers IPC’S SEMI-ANNUAL REVIEW OF THE • Clinically resolved psoriatic lesions TOP 5 PAPERS: JULY–DECEMBER 2017 contain psoriasis-specific IL-17- producing αβ T cell clones • Psoriasis and suicidality: A systematic Every 6 months, IPC’s board and councilors recommend and vote on articles that review and meta-analysis make the greatest impact on psoriasis research. The 5 papers that received the • An analysis of IL-36 signature genes most votes for articles published July through December 2017 are reviewed here. and individuals with IL1RL2 knockout Summaries and commentaries were written by this issue’s co-editors, Dr. Colby mutations validates IL-36 as a Evans, Evans Dermatology, Austin, Texas, United States, and Dr. Nancy Podoswa, psoriasis therapeutic target Hospital General Regional No. 1 Dr. Carlos MacGregor Sanchez Navarro, Mexican • Coronary plaque characterization in psoriasis reveals high-risk features Institute of Social Security, Mexico City, Mexico. that improve after treatment in a prospective observational study 1. Residual T-cell clones in both active and resolved • Association between skin and aortic vascular inflammation in patients psoriatic plaques may reinitiate disease if treatment with psoriasis: a case-cohort study stops using Positron Emission Tomography/ Computed Tomography Clinically resolved psoriatic lesions contain psoriasis-specific IL-17-producing 2 A Letter from the President αβ T cell clones. Matos TR, O’Malley JT, Lowry EL, et al. J Clin Invest. 2017 Nov 1;127(11):4031-4041. doi: 10.1172/JCI93396. Epub 2017 Sep 25. -

Clinical and Basic Immunodermatology Clinical and Basic Immunodermatology
Clinical and Basic Immunodermatology Clinical and Basic Immunodermatology Edited by Anthony A. Gaspari, MD Department of Dermatology University of Maryland School of Medicine Baltimore, MD USA Stephen K. Tyring, MD, PhD Department of Dermatology University of Texas Medical School at Houston Houston, TX USA Editors Anthony A. Gaspari, MD University of Maryland School of Medicine Baltimore, MD USA Stephen K. Tyring, MD, PhD University of Texas Medical School at Houston Houston, TX USA ISBN 978-1-84800-164-0 e-ISBN 978-1-84800-165-7 DOI 10.1007/978-1-84800-165-7 British Library Cataloguing in Publication Data A catalogue record for this book is available from the British Library Library of Congress Control Number: 2008923739 © Springer-Verlag London Limited 2008 Apart from any fair dealing for the purposes of research or private study, or criticism or review, as permitted under the Copyright, Designs and Patents Act 1988, this publication may only be reproduced, stored or transmitted, in any form or by any means, with the prior permission in writing of the publishers, or in the case of reprographic reproduction in accordance with the terms of licences issued by the Copyright Licensing Agency. Enquiries concerning reproduction outside those terms should be sent to the publishers. The use of registered names, trademarks, etc. in this publication does not imply, even in the absence of a specific statement, that such names are exempt from the relevant laws and regulations and therefore free for general use. Product liability: The publisher can give no guarantee for information about drug dosage and application thereof contained in this book. -

Practical Dermatology Methodical Recommendations
Vitebsk State Medical University Practical Dermatology Methodical recommendations Adaskevich UP, Valles - Kazlouskaya VV, Katina MA VSMU Publishing 2006 616.5 удк-б-1^«адл»-2о -6Sl«Sr83p3»+4£*łp30 А28 Reviewers: professor Myadeletz OD, head of the department of histology, cytology and embryology in VSMU: professor Upatov Gl, head of the department of internal diseases in VSMU Adaskevich IIP, Valles-Kazlouskaya VV, Katina МЛ. A28 Practical dermatology: methodical recommendations / Adaskevich UP, Valles-Kazlouskaya VV, Katina MA. - Vitebsk: VSMU, 2006,- 135 p. Methodical recommendations “Practical dermatology” were designed for the international students and based on the typical program in dermatology. Recommendations include tests, clinical tasks and practical skills in dermatology that arc used as during practical classes as at the examination. УДК 616.5:37.022.=20 ББК 55.83p30+55.81 p30 C Adaskev ich UP, Valles-Ka/.louskaya VV, Katina MA. 2006 OVitebsk State Medical University. 2006 Content 1. Practical skills.......................................................................................................5 > 1.1. Observation of the patient's skin (scheme of the case history).........................5 1.2. The determination of skin moislness, greasiness, dryness and turgor.......... 12 1.3. Dermographism determination.........................................................................12 1.4. A method of the arrangement of dropping and compressive allergic skin tests and their interpretation........................................................................................................ -

Hand Dermatitis: Review of Etiology, Diagnosis, and Treatment
J Am Board Fam Med: first published as 10.3122/jabfm.2009.03.080118 on 8 May 2009. Downloaded from Hand Dermatitis: Review of Etiology, Diagnosis, and Treatment Adam D. Perry, MD, and John P. Trafeli, MD Hand dermatitis is a common condition seen in the primary care setting. Occupational exposures and frequent hand washing often lead to symptoms that are irritating and may cause discomfort. Irritant dermatitis, atopic hand dermatitis and contact hand dermatitis account for at least 70% of all diagnoses. A unifying feature in most cases is an underlying disruption in the stratum corneum, altering its barrier function. Transepidermal water loss increases with barrier disruption and is exacerbated by additional exposure to water. Precise diagnosis and subsequent treatment present a considerable challenge, and hand dermatitis often becomes chronic. Initial treatment should be aimed at controlling inflammation and restoring the skin’s natural barrier. Common management recommendations include the avoidance of irritants and potential allergens along with the use of emollients and topical corticosteroids to de- crease inflammation. Simple petroleum-based emollients are very effective at restoring hydration and repairing the stratum corneum. Referral to a Dermatologist or an Allergist may be necessary for pa- tients who require patch testing or those with refractory symptoms. (J Am Board Fam Med 2009;22: 325–30.) Hand dermatitis represents a large proportion of It is estimated that 5% to 7% of patients with occupation-associated skin disease. The prevalence hand dermatitis are characterized as having chronic among the general population has been estimated or severe symptoms and 2% to 4% of severe cases copyright.