Clinical Applications of Nuclear Medicine
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

BREAST IMAGING for SCREENING and DIAGNOSING CANCER Policy Number: DIAGNOSTIC 105.9 T2 Effective Date: January 1, 2017
Oxford UnitedHealthcare® Oxford Clinical Policy BREAST IMAGING FOR SCREENING AND DIAGNOSING CANCER Policy Number: DIAGNOSTIC 105.9 T2 Effective Date: January 1, 2017 Table of Contents Page Related Policies INSTRUCTIONS FOR USE .......................................... 1 Omnibus Codes CONDITIONS OF COVERAGE ...................................... 1 Preventive Care Services BENEFIT CONSIDERATIONS ...................................... 2 Radiology Procedures Requiring Precertification for COVERAGE RATIONALE ............................................. 3 eviCore Healthcare Arrangement APPLICABLE CODES ................................................. 5 DESCRIPTION OF SERVICES ...................................... 6 CLINICAL EVIDENCE ................................................. 7 U.S. FOOD AND DRUG ADMINISTRATION ................... 16 REFERENCES .......................................................... 18 POLICY HISTORY/REVISION INFORMATION ................ 22 INSTRUCTIONS FOR USE This Clinical Policy provides assistance in interpreting Oxford benefit plans. Unless otherwise stated, Oxford policies do not apply to Medicare Advantage members. Oxford reserves the right, in its sole discretion, to modify its policies as necessary. This Clinical Policy is provided for informational purposes. It does not constitute medical advice. The term Oxford includes Oxford Health Plans, LLC and all of its subsidiaries as appropriate for these policies. When deciding coverage, the member specific benefit plan document must be referenced. The terms -

Breast Scintimammography
CLINICAL MEDICAL POLICY Policy Name: Breast Scintimammography Policy Number: MP-105-MD-PA Responsible Department(s): Medical Management Provider Notice Date: 11/23/2020 Issue Date: 11/23/2020 Effective Date: 12/21/2020 Next Annual Review: 10/2021 Revision Date: 09/16/2020 Products: Gateway Health℠ Medicaid Application: All participating hospitals and providers Page Number(s): 1 of 5 DISCLAIMER Gateway Health℠ (Gateway) medical policy is intended to serve only as a general reference resource regarding coverage for the services described. This policy does not constitute medical advice and is not intended to govern or otherwise influence medical decisions. POLICY STATEMENT Gateway Health℠ does not provide coverage in the Company’s Medicaid products for breast scintimammography. The service is considered experimental and investigational in all applications, including but not limited to use as an adjunct to mammography or in staging the axillary lymph nodes. This policy is designed to address medical necessity guidelines that are appropriate for the majority of individuals with a particular disease, illness or condition. Each person’s unique clinical circumstances warrant individual consideration, based upon review of applicable medical records. (Current applicable Pennsylvania HealthChoices Agreement Section V. Program Requirements, B. Prior Authorization of Services, 1. General Prior Authorization Requirements.) Policy No. MP-105-MD-PA Page 1 of 5 DEFINITIONS Prior Authorization Review Panel – A panel of representatives from within the Pennsylvania Department of Human Services who have been assigned organizational responsibility for the review, approval and denial of all PH-MCO Prior Authorization policies and procedures. Scintimammography A noninvasive supplemental diagnostic testing technology that requires the use of radiopharmaceuticals in order to detect tissues within the breast that accumulate higher levels of radioactive tracer that emit gamma radiation. -

Lacrimal Scintigraphy
LACRIMAL SCINTIGRAPHY Lacrimal Scintigraphy RO Boer, Medical Centre, Alkmaar (Retired) NOTE: no changes have been made since the version of 2007 1. Introduction A standardised volume of 10 μl 99mTc pertechnetate is instilled into the patient’s conjunctival sac using a micro-pipette. In principle, the quantity must be as small as possible, since any increase in the very small tear reservoir can lead to contamination of the eyelids and thus adversely affect the interpretability of the investigation. In contradistinction to the already well-established xray investigation whereby at all times outside influence is exerted on the tear drainage, the aim of this tracer investigation is to study the natural tear drainage. Normally, tears are drained from the conjunctival sac to the lacrimal sac (saccus lacrimalis), then to the naso-lacrimalduct (ductus nasolacrimalis) and finally to the nose and pharynx. 2. Methodology This guideline is based on available scientific literature on the subject, the previous guideline (Aanbevelingen Nucleaire Geneeskunde 2007), international guidelines from EANM and/or SNMMI if available and applicable to the Dutch situation. 3. Indications Epiphora (watering of the eye) is the initial indication. The ability to adequately manipulate the lacrimal pathways in order to improve drainage is closely linked to the indication. This is often achived through surgical procedures such as DCR (dacryocystorhinostomy) or DCP (dacryocystorhinoplasty, ‘angioplasty’ of the lacrimal pathways). Thereafter, the effect of these interventions can be evaluated by means of lacrimal scintigraphy. 4. Relation to other diagnostic procedures The Anel test is performed by cannulating the lower lacrimal point and injecting physiological saline. When the system becomes patent, the patient will taste salt. -

Procedure Guideline for Breast Scintigraphy
Procedure Guideline for Breast Scintigraphy Iraj Khalkhali, Linda E. Diggles, Raymond Taillefer, Penny R. Vandestreek, Patrick J. Peller and Hani H. Abdel-Nabi Harbor-UCLA Medical Center, Terranee; Nuclear Imaging Consultants, Roseville, California; Hospital Hôtel-Dieu de Montreal, Montreal, Quebec, Canada; Lutheran General Hospital, Park Ridge, Illinois; and University of Buffalo, Buffalo, New York Key Words: breast scintigraphy;procedureguideline should be available, as well as sonograms, if J NucÃMed 1999; 40:1233-1235 obtained. 2. A breast physical examination must be performed by either the nuclear medicine physician or the PART I: PURPOSE referring physician. 3. The time of last menses and pregnancy and lactat- The purpose of this guideline is to assist nuclear medicine ing status of the patient should be determined. practitioners in recommending, performing, interpreting and reporting the results of 99mTc-sestamibi breast scintigraphy 4. Breast scintigraphy should be delayed at least 2 wk after cyst or fine-needle aspiration, and 4—6wk (mammoscintigraphy, scintimammography). after core or excisional biopsy. 5. The nuclear medicine physician should be aware of PART II: BACKGROUND INFORMATION AND DEFINITIONS physical signs and symptoms and prior surgical procedures or therapy. Breast scintigraphy is performed after intravenous admin istration of "mTc-sestamibi and includes planar and/or C. Precautions None SPECT. D. Radiopharmaceutical 1. Intravenous injection of 740-1110 MBq (20-30 PART III: COMMON INDICATIONS AND APPLICATIONS mCi) 99mTc-sestamibi should be administered in an A. Evaluate breast cancer in patients in whom mammog- arm vein contralateral to the breast with the sus raphy is not diagnostic or is difficult to interpret (e.g., pected abnormality. -

A Molecular Approach to Breast Imaging
Journal of Nuclear Medicine, published on January 16, 2014 as doi:10.2967/jnumed.113.126102 FOCUS ON MOLECULAR IMAGING A Molecular Approach to Breast Imaging Amy M. Fowler Department of Radiology, University of Wisconsin–Madison, Madison, Wisconsin malignant cells. A recent meta-analysis of the accuracy of 99mTc-sestamibi scintimammography as an adjunct to di- Molecular imaging is a multimodality discipline for noninvasively agnostic mammography for detection of breast cancer dem- visualizing biologic processes at the subcellular level. Clinical applications of radionuclide-based molecular imaging for breast onstrated a sensitivity of 83% and specificity of 85% (2). cancer continue to evolve. Whole-body imaging, with scinti- However, sensitivity was less for nonpalpable (59%) versus mammography and PET, and newer dedicated breast imaging palpable lesions (87%) despite comparable specificity, with systems are reviewed. The potential clinical indications and the no significant difference between planar and SPECT meth- challenges of implementing these emerging technologies are ods. Decreased sensitivity for nonpalpable, presumably presented. smaller, lesions is in part due to the limited spatial resolu- Key Words: molecular imaging; oncology; breast; PET; PET/ tion of conventional g cameras. CT; radiopharmaceuticals; breast cancer; breast-specific g im- In addition to 99mTc-sestamibi, the positron-emitting ra- aging; positron-emission mammography; positron-emission to- diopharmaceutical 18F-FDG accumulates in many types of mography cancer including breast. Meta-analyses of the accuracy of J Nucl Med 2014; 55:1–4 whole-body 18F-FDG PET used after standard diagnostic DOI: 10.2967/jnumed.113.126102 workup for patients with suspected breast lesions demon- strated sensitivities of 83%–89% and specificities of 74%– 80% (3,4). -

Evaluation of Nipple Discharge
New 2016 American College of Radiology ACR Appropriateness Criteria® Evaluation of Nipple Discharge Variant 1: Physiologic nipple discharge. Female of any age. Initial imaging examination. Radiologic Procedure Rating Comments RRL* Mammography diagnostic 1 See references [2,4-7]. ☢☢ Digital breast tomosynthesis diagnostic 1 See references [2,4-7]. ☢☢ US breast 1 See references [2,4-7]. O MRI breast without and with IV contrast 1 See references [2,4-7]. O MRI breast without IV contrast 1 See references [2,4-7]. O FDG-PEM 1 See references [2,4-7]. ☢☢☢☢ Sestamibi MBI 1 See references [2,4-7]. ☢☢☢ Ductography 1 See references [2,4-7]. ☢☢ Image-guided core biopsy breast 1 See references [2,4-7]. Varies Image-guided fine needle aspiration breast 1 Varies *Relative Rating Scale: 1,2,3 Usually not appropriate; 4,5,6 May be appropriate; 7,8,9 Usually appropriate Radiation Level Variant 2: Pathologic nipple discharge. Male or female 40 years of age or older. Initial imaging examination. Radiologic Procedure Rating Comments RRL* See references [3,6,8,10,13,14,16,25- Mammography diagnostic 9 29,32,34,42-44,71-73]. ☢☢ See references [3,6,8,10,13,14,16,25- Digital breast tomosynthesis diagnostic 9 29,32,34,42-44,71-73]. ☢☢ US is usually complementary to mammography. It can be an alternative to mammography if the patient had a recent US breast 9 mammogram or is pregnant. See O references [3,5,10,12,13,16,25,30,31,45- 49]. MRI breast without and with IV contrast 1 See references [3,8,23,24,35,46,51-55]. -

Evaluation of the Quantitative Accuracy of a Commercially-Available Positron Emission Mammography Scanner
The Texas Medical Center Library DigitalCommons@TMC The University of Texas MD Anderson Cancer Center UTHealth Graduate School of The University of Texas MD Anderson Cancer Biomedical Sciences Dissertations and Theses Center UTHealth Graduate School of (Open Access) Biomedical Sciences 8-2010 EVALUATION OF THE QUANTITATIVE ACCURACY OF A COMMERCIALLY-AVAILABLE POSITRON EMISSION MAMMOGRAPHY SCANNER Adam Springer Follow this and additional works at: https://digitalcommons.library.tmc.edu/utgsbs_dissertations Part of the Diagnosis Commons, Equipment and Supplies Commons, and the Other Medical Sciences Commons Recommended Citation Springer, Adam, "EVALUATION OF THE QUANTITATIVE ACCURACY OF A COMMERCIALLY-AVAILABLE POSITRON EMISSION MAMMOGRAPHY SCANNER" (2010). The University of Texas MD Anderson Cancer Center UTHealth Graduate School of Biomedical Sciences Dissertations and Theses (Open Access). 64. https://digitalcommons.library.tmc.edu/utgsbs_dissertations/64 This Thesis (MS) is brought to you for free and open access by the The University of Texas MD Anderson Cancer Center UTHealth Graduate School of Biomedical Sciences at DigitalCommons@TMC. It has been accepted for inclusion in The University of Texas MD Anderson Cancer Center UTHealth Graduate School of Biomedical Sciences Dissertations and Theses (Open Access) by an authorized administrator of DigitalCommons@TMC. For more information, please contact [email protected]. EVALUATION OF THE QUANTITATIVE ACCURACY OF A COMMERCIALLY- AVAILABLE POSITRON EMISSION MAMMOGRAPHY SCANNER -
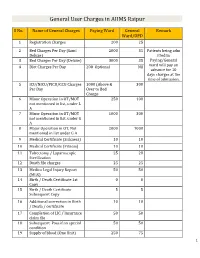
General User Charges in AIIMS Raipur
General User Charges in AIIMS Raipur S No. Name of General Charges Paying Ward General Remark Ward/OPD 1 Registration Charges 200 25 2 Bed Charges Per Day (Sami 2000 35 Patients being adm Deluxe) itted in 3 Bed Charges Per Day (Deluxe) 3000 35 Paying/General 4 Diet Charges Per Day 200 Optional Nil ward will pay an advance for 10 days charges at the time of admission. 5 ICU/NICU/PICU/CCU Charges 1000 (Above & 300 Per Day Over to Bed Charge 6 Minor Operation in OT/MOT 250 100 not mentioned in list, under L A 7 Minor Operation in OT/MOT 1000 300 not mentioned in list, under G A 8 Major Operation in OT, Not 2000 1000 mentioned in list under G A 9 Medical Certificate (Sickness) 10 10 10 Medical Certificate (Fitness) 10 10 11 Tubectomy / Laparoscopic 25 20 Sterilization 12 Death file charges 25 25 13 Medico Legal Injury Report 50 50 (MLR) 14 Birth / Death Certificate 1st 0 0 Copy 15 Birth / Death Certificate 5 5 Subsequent Copy 16 Additional correction in Birth 10 10 / Death / certificate 17 Completion of LIC / Insurance 50 50 claim file 18 Subsequent Pass if on special 50 50 condition 19 Supply of blood (One Unit) 250 75 1 20 Medical Board Certificate 500 500 On Special Case User Charges for Investigations in AIIMS Raipur S No. Name of Investigations Paying General Remark Ward Ward/OPD Anaesthsia 1 ABG 75 50 2 ABG ALONGWITH 150 100 ELECTROLYTES(NA+,K+)(Na,K) 3 ONLY ELECTROLYTES(Na+,K+,Cl,Ca+) 75 50 4 ONLY CALCIUM 50 25 5 GLUCOSE 25 20 6 LACTATE 25 20 7 UREA. -

Scintimammography and Gamma Imaging of the Breast and Axilla
MEDICAL POLICY POLICY TITLE SCINTIMAMMOGRAPHY AND GAMMA IMAGING OF THE BREAST AND AXILLA POLICY NUMBER MP-5.021 Original Issue Date (Created): 8/9/2002 Most Recent Review Date (Revised): 8/18/2020 Effective Date: 11/1/2020 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT VARIATIONS DISCLAIMER CODING INFORMATION REFERENCES POLICY HISTORY I. POLICY Scintimammography, breast-specific gamma imaging (BSGI), and molecular breast imaging (MBI) are considered investigational in all applications, including but not limited to its use as an adjunct to mammography or in staging the axillary lymph nodes. There is insufficient evidence to support a conclusion concerning the health outcomes or benefits associated with these procedures. Use of gamma detection following radiopharmaceutical administration for localization of sentinel lymph nodes in patients with breast cancer may be considered medically necessary. Policy Guidelines The most commonly-used radiopharmaceutical in breast-specific gamma imaging or molecular breast imaging is technetium 99m (Tc-99m) sestamibi. The most commonly used radiopharmaceuticals for sentinel lymph node detection using either lymphoscintigraphy or hand-held gamma detection include Tc 99mlabeled colloids (eg, sulfur colloid). Cross-references: MP-5.022 Radioimmunoscintigraphy Imaging Monoclonal Antibody Imaging with Indium- 111 Capromab Pendetide for Prostate Cancer II. PRODUCT VARIATIONS Top This policy is only applicable to certain programs and products administered by Capital BlueCross please see additional information below, and subject to benefit variations as discussed in Section VI below. Page 1 MEDICAL POLICY POLICY TITLE SCINTIMAMMOGRAPHY AND GAMMA IMAGING OF THE BREAST AND AXILLA POLICY NUMBER MP-5.021 III. DESCRIPTION/BACKGROUND Top Scintimammography, breast-specific gamma imaging (BSGI), and molecular breast imaging (MBI) use radiotracers with nuclear medicine imaging as a diagnostic tool for abnormalities of the breast. -

Scintimammography with a Hybrid SPECT/CT Imaging System
ANTICANCER RESEARCH 27: 557-562 (2007) Scintimammography with a Hybrid SPECT/CT Imaging System ORAZIO SCHILLACI, ROBERTA DANIELI, LUCA FILIPPI, PASQUALE ROMANO, ELSA COSSU, CARLO MANNI and GIOVANNI SIMONETTI Department of Biopathology and Diagnostic Imaging, University "Tor Vergata", Rome, Italy Abstract. Background: Planar scintimammography is useful carcinomas are evident on mammograms, especially in dense for characterizing breast lesions >10 mm. Our aim was to or dysplastic breasts (3); moreover, its specificity and positive evaluate Tc-99m sestamibi scintimammography with a hybrid predictive value are low because it cannot always (SPECT/CT) device for functional anatomical mapping (FAM). differentiate benign lesions from malignant ones (4). The Patients and Methods: Three planar images and a chest drawbacks of mammography have led to the development of SPECT/CT were performed with a hybrid device in 53 patients complementary modalities for breast cancer imaging, with mammographically suspicious lesions. The final including scintimammography, a nuclear medicine technique histopathological diagnosis was obtained after surgery. Results: that uses radiopharmaceuticals to detect malignant breast The planar images were positive in 27 out of 37 carcinomas tumours (5, 6). Scintimammography is conventionally (sensitivity 73%) and the SPECT/CT in 33 (sensitivity 89.2%). performed with planar acquisitions, which have a low The sensitivity of planar imaging and SPECT/CT was 42.9% sensitivity for lesions ≤10 mm (5). Recently, a new imaging and 71.4% in cancers ≤10 mm, and 91.3%, and 100% in device combining a dual-head, variable angle gamma camera cancers >10 mm, respectively. The specificity was 93.8% for with a low-dose X-ray tube has been introduced (7): this both planar and SPECT/CT imaging; accuracy was 79.2% for hybrid gamma camera/CT scanner provides cross-sectional planar scans and 90.6% for SPECT/CT. -

FDA-Approved Radiopharmaceuticals
Medication Management FDA-approved radiopharmaceuticals This is a current list of all FDA-approved radiopharmaceuticals. USP <825> requires the use of conventionally manufactured drug products (e.g., NDA, ANDA) for Immediate Use. Nuclear medicine practitioners that receive radiopharmaceuticals that originate from sources other than the manufacturers listed in these tables may be using unapproved copies. Radiopharmaceutical Manufacturer Trade names Approved indications in adults (Pediatric use as noted) 1 Carbon-11 choline Various - Indicated for PET imaging of patients with suspected prostate cancer recurrence based upon elevated blood prostate specific antigen (PSA) levels following initial therapy and non-informative bone scintigraphy, computerized tomography (CT) or magnetic resonance imaging (MRI) to help identify potential sites of prostate cancer recurrence for subsequent histologic confirmation 2 Carbon-14 urea Halyard Health PYtest Detection of gastric urease as an aid in the diagnosis of H.pylori infection in the stomach 3 Copper-64 dotatate Curium Detectnet™ Indicated for use with positron emission tomography (PET) for localization of somatostatin receptor positive neuroendocrine tumors (NETs) in adult patients 4 Fluorine-18 florbetaben Life Molecular Neuraceq™ Indicated for Positron Emission Tomography (PET) imaging of the brain to Imaging estimate β amyloid neuritic plaque density in adult patients with cognitive impairment who are being evaluated for Alzheimer’s disease (AD) or other causes of cognitive decline 5 Fluorine-18 -

Nuclear Medicine
2013 RSNA (Filtered Schedule) Sunday, December 01, 2013 10:45-12:15 PM • SSA18 • Room: S505AB • Nuclear Medicine (PET/CT in Oncology) 12:30-01:00 PM • CL-NMS-SUA • Room: S503AB • Nuclear Medicine - Sunday Posters and Exhibits (12:30pm - 1:00pm) 01:00-01:30 PM • CL-NMS-SUB • Room: S503AB • Nuclear Medicine - Sunday Posters and Exhibits (1:00pm - 1:30pm) 02:00-03:30 PM • RC111 • Room: S505AB • Multi-modal Imaging Workup for Alzheimer's Disease, Parkinson's Disease, and Related Disorders: Case-based App... Monday, December 02, 2013 08:30-10:00 AM • RC217 • Room: S504CD • PET-MR/Hyperpolarized MR 08:30-12:00 PM • VSNM21 • Room: S505AB • Nuclear Medicine Series: Assessment of Cancer Treatment Response: Updates 12:15-12:45 PM • CL-NMS-MOA • Room: S503AB • Nuclear Medicine - Monday Posters and Exhibits (12:15pm - 12:45pm) 12:45-01:15 PM • CL-NMS-MOB • Room: S503AB • Nuclear Medicine - Monday Posters and Exhibits (12:45pm - 1:15pm) 03:00-04:00 PM • SSE08 • Room: E353C • ISP: Gastrointestinal (Oncology: Staging and Distant Metastases) 03:00-04:00 PM • SSE19 • Room: S504CD • Nuclear Medicine (Quantitative Imaging) 03:00-04:00 PM • SSE20 • Room: S505AB • Nuclear Medicine (SPECT/CT) Tuesday, December 03, 2013 08:30-10:00 AM • MSCC31 • Room: S406A • Case-based Review of Nuclear Medicine: PET/CT Workshop-Head and Neck Cancers (In Conjunction with SNMMI) (An I... 08:30-10:00 AM • RC321 • Room: S102D • Medical Physics 2.0: Nuclear Imaging 08:30-10:00 AM • RC351 • Room: E353C • CT/PET in the Abdomen and Pelvis: How and When (How-to Workshop) (An Interactive Session) 08:30-12:00 PM • VSNM31 • Room: S505AB • Nuclear Medicine Series: Non-FDG PET Radiotracers in Oncology 10:30-12:00 PM • MSCC32 • Room: S406A • Case-based Review of Nuclear Medicine: PET/CT Workshop-Cancers of the Abdomen and Pelvis (In Conjunction with ..