Intravenous Volume Replacement: Which Fluid and Why?
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Intravenous And/Or Peripheral Saline Lock Insertion and Maintenance
Policies & Procedures Title: INTRAVENOUS AND/OR PERIPHERAL SALINE LOCK INSERTION AND MAINTENANCE ID Number: 1118 Authorization Source: Nursing Date Revised: September 2013 [X] SHR Nursing Practice Committee Date Effective: May 1999 Date Reaffirmed: May 2015 Scope: SHR & Affiliates Any PRINTED version of this document is only accurate up to the date of printing 22-Jul-15. Saskatoon Health Region (SHR) cannot guarantee the currency or accuracy of any printed policy. Always refer to the Policies and Procedures site for the most current versions of documents in effect. SHR accepts no responsibility for use of this material by any person or organization not associated with SHR. No part of this document may be reproduced in any form for publication without permission of SHR. DEFINITIONS Flushing – Injection of a solution into the intravenous (IV) catheter/cap to prevent mixing of incompatible solutions and clean the catheter of blood or fibrin buildup. Turbulent flush technique – A method of flushing using a “stop-start” technique which “scrubs” the inside of the catheter lumen, preventing the build-up of fibrin or medication residue. 1. PURPOSE 1.1 To minimize the risks of infection and other complications associated with the insertion and maintenance of intravenous catheters. 2. POLICY 2.1 Who may start IV • RN/RPN/GN competent in IV starts (NICU-Level 2 orientated RN only) • Nursing Students under direct RN/GN/RPN/LPN/GPN supervision • LPN/GPN who have successfully completed the IV/Blood Administration Course • Home Intravenous Therapy Program (HITP) – RN’s only 2.2 A prescriber order is required to start an IV except in an emergency situation or for restarts. -

The National Drugs List
^ ^ ^ ^ ^[ ^ The National Drugs List Of Syrian Arab Republic Sexth Edition 2006 ! " # "$ % &'() " # * +$, -. / & 0 /+12 3 4" 5 "$ . "$ 67"5,) 0 " /! !2 4? @ % 88 9 3: " # "$ ;+<=2 – G# H H2 I) – 6( – 65 : A B C "5 : , D )* . J!* HK"3 H"$ T ) 4 B K<) +$ LMA N O 3 4P<B &Q / RS ) H< C4VH /430 / 1988 V W* < C A GQ ") 4V / 1000 / C4VH /820 / 2001 V XX K<# C ,V /500 / 1992 V "!X V /946 / 2004 V Z < C V /914 / 2003 V ) < ] +$, [2 / ,) @# @ S%Q2 J"= [ &<\ @ +$ LMA 1 O \ . S X '( ^ & M_ `AB @ &' 3 4" + @ V= 4 )\ " : N " # "$ 6 ) G" 3Q + a C G /<"B d3: C K7 e , fM 4 Q b"$ " < $\ c"7: 5) G . HHH3Q J # Hg ' V"h 6< G* H5 !" # $%" & $' ,* ( )* + 2 ا اوا ادو +% 5 j 2 i1 6 B J' 6<X " 6"[ i2 "$ "< * i3 10 6 i4 11 6! ^ i5 13 6<X "!# * i6 15 7 G!, 6 - k 24"$d dl ?K V *4V h 63[46 ' i8 19 Adl 20 "( 2 i9 20 G Q) 6 i10 20 a 6 m[, 6 i11 21 ?K V $n i12 21 "% * i13 23 b+ 6 i14 23 oe C * i15 24 !, 2 6\ i16 25 C V pq * i17 26 ( S 6) 1, ++ &"r i19 3 +% 27 G 6 ""% i19 28 ^ Ks 2 i20 31 % Ks 2 i21 32 s * i22 35 " " * i23 37 "$ * i24 38 6" i25 39 V t h Gu* v!* 2 i26 39 ( 2 i27 40 B w< Ks 2 i28 40 d C &"r i29 42 "' 6 i30 42 " * i31 42 ":< * i32 5 ./ 0" -33 4 : ANAESTHETICS $ 1 2 -1 :GENERAL ANAESTHETICS AND OXYGEN 4 $1 2 2- ATRACURIUM BESYLATE DROPERIDOL ETHER FENTANYL HALOTHANE ISOFLURANE KETAMINE HCL NITROUS OXIDE OXYGEN PROPOFOL REMIFENTANIL SEVOFLURANE SUFENTANIL THIOPENTAL :LOCAL ANAESTHETICS !67$1 2 -5 AMYLEINE HCL=AMYLOCAINE ARTICAINE BENZOCAINE BUPIVACAINE CINCHOCAINE LIDOCAINE MEPIVACAINE OXETHAZAINE PRAMOXINE PRILOCAINE PREOPERATIVE MEDICATION & SEDATION FOR 9*: ;< " 2 -8 : : SHORT -TERM PROCEDURES ATROPINE DIAZEPAM INJ. -
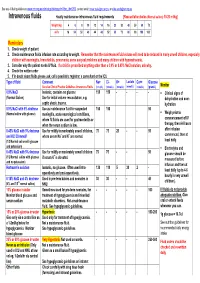

Intravenous Fluids
See also IV fluid guidelines at www.rch.org.au/clinicalguide/cpg.cfm?doc_id=5203, contact email: [email protected] or [email protected] Intravenous fluids Hourly maintenance intravenous fluid requirements [Resuscitation bolus (Normal saline): 10-20 ml/kg] Weight (kg) 4 6 8 10 12 14 16 20 30 40 50 60 70 ml/hr 16 24 32 40 44 48 52 60 70 80 90 100 100 Reminders 1. Check weight of patient 2. Check maintenance fluids infusion rate according to weight. Remember that the maintenance fluid volume will need to be reduced in many unwell children, especially children with meningitis, bronchiolitis, pneumonia, some surgical problems and many children with hyponatraemia. 3. Consider why the patient needs IV fluid. If a child is prescribed anything other than a 0.9% or 0.45% NaCl solution, ask why. 4. Check the written order 5. If in doubt about fluids please ask, call a paediatric registrar, a consultant or the ICU Type of fluid Comment Na+ Cl- K+ Lactate Ca++ Glucose See also Clinical Practice Guidelines Intravenous Fluids (mmol/L) (mmol/L) (mmol/L) (mmol/L) (mmol/L) (gram/L) Monitor 0.9% NaCl Isotonic, contains no glucose 150 150 - - - - Clinical signs of (Normal Saline) Use for initial volume resuscitation, e.g. dehydration and over- septic shock, trauma. hydration 0.9% NaCl with 5% dextrose Use as maintenance fluid for suspected 150 150 50 (Normal saline with glucose) meningitis, acute neurological conditions, Weigh prior to where IV fluids are used for gastroenteritis or commencement of IV when the serum sodium is low. -

(Haemagel) Versus 6% Hydroxyethyl Starch 200/0.5 (Haes-Steril) for Plasma Volume Expansion in Critically-Ill Patients Magdy Ali Omera, MD* , Salah A
Alexandria Journal of Anaesthesia and Intensive Care 44 Autoclaved Gelatin (Haemagel) Versus 6% Hydroxyethyl Starch 200/0.5 (Haes-steril) For Plasma Volume Expansion In Critically-ill Patients Magdy Ali Omera, MD* , Salah A. Ismail, MD* * Assistant Prof. of Anaesthesia, Faculty of Medicine, Suez Canal University. ABSTRACT Synthetic colloids are used to optimize hemodynamics in the critically ill patients and a debate about the most suitable one is still present. The influence of short term infusion of autoclaved gelatin (Haemagel) and 6% hydroxyethyl starch 200/0.5 (Haes-steril) on hemodynamic, respiratory, coagulation, renal and oncotic parameters were examined in a prospective randomized study. Method: Thirty patients suffering from systemic hypoperfusion due to sepsis in ICU of Suez Canal University Hospital were assigned into 2 equal groups. In GEL group: 1000 ml of Haemagel was infused within an hour, while in HES group: 1000 ml of 6% Haes-steril 200/0.5 was given within an hour. The hemodynamic, respiratory, hematological, coagulation, renal and colloidal osmotic pressure parameters were recorded before and after infusion of both colloids. Results: There was a significant similar increase in hemodynamic variables (Mean arterial pressure, central venous pressure, cardiac index, stroke volume index and left ventricular stroke work index) in both groups. Also, a significant improvement in tissue perfusion as judged by decreased arterial lactate was found. There were no significant differences in any of the measured respiratory parameters (respiratory rate, arterial oxygen saturation, arterial blood gases and intrapulmonary shunt) in the studied groups. No significant intergroup difference in any haemodynamic or respiratory variable was demonstrated. -

Clinical Pharmacology of Infusion Fluids
Clinical pharmacology of infusion fluids Robert G. Hahn Linköping University Post Print N.B.: When citing this work, cite the original article. Original Publication: Robert G. Hahn , Clinical pharmacology of infusion fluids, 2012, Acta Medica Lituanica, (19), 3. Licencee: Lithuanian Academy of Sciences http://www.lmaleidykla.lt/ojs/index.php/actamedicalituanica/index Postprint available at: Linköping University Electronic Press http://urn.kb.se/resolve?urn=urn:nbn:se:liu:diva-91319 ACTA MEDICA LITUANICA. 2012. Vol. 19. No. 3. P. 210–212 © Lietuvos mokslų akademija, 2012 Clinical pharmacology of infusion fluids Robert G. Hahn Fluids are used for intravenous infusion during practically all surgeries, but several different compositions are available on the market. Södertälje Hospital, Crystalloid fluids comprise lactated or acetated Ringer solutions, nor- Södertälje, Sweden; mal saline, Plasma-Lyte, hypertonic saline, and glucose. They lack allergic Anaesthesia and properties but are prone to cause peripheral tissue oedema. Their turn- Intensive Care, over is governed by physiological factors such as dehydration and drug Linköping University, effects. Sweden Colloid fluids include hydroxyethyl starch, albumin, dextran, and gela- tin. These fluids have various degrees of allergic properties and do not promote peripheral oedema. Their half-life is usually about hours. Factors increasing the turnover rate are poorly known but might include inflam- matory states. Current debates include the widespread use of normal saline, which should be replaced by Ringer’s or Plasma-Lyte in most situations, and the kidney damage associated with the use of starch in septic patients. New studies show that hypertonic saline does not improve survival or neuro- logical damage in prehospital care. -

High Volume Sinonasal Budesonide Irrigations for Chronic Rhinosinusitis
oepidem ac io m lo Rudmik, Adv Pharmacoepidemiol Drug Saf 2014, 3:2 r g a y h & P Advances in Pharmacoepidemiology & DOI: 10.4172/2167-1052.1000148 D n i r u s g e c ISSN: 2167-1052 S n a a f v e t d y A Drug Safety Review Article Open Access High Volume Sinonasal Budesonide Irrigations for Chronic Rhinosinusitis: An Update on the Safety and Effectiveness Luke Rudmik* Division of Otolaryngology–Head and Neck Surgery, Department of Surgery, University of Calgary, Calgary, Alberta, Canada Abstract Chronic rhinosinusitis (CRS) is a common inflammatory disease of the paranasal sinuses associated with severe impairments in patient quality of life, sleep, and productivity. Topical corticosteroid therapy is a key component to a successful management plan for patients with CRS. Delivering topical medical therapies using high-volume sinonasal irrigations are commonly used following endoscopic sinus surgery (ESS) due to its proven efficacy for improving drug delivery into the paranasal sinuses. Topical high volume budesonide irrigations have become a popular off- label management strategy for CRS with the purpose to improve topical steroid delivery into the sinonasal cavities. Early evidence outlined in this review suggests that high volume sinonasal budesonide irrigations are an effective treatment modality in patients with CRS following ESS. Overall it appears that short-term use of this therapy is likely safe, however, future studies will need to assess the safety of higher doses and longer-term therapy of budesonide irrigations in patients with CRS. Keywords: Chronic rhinosinusitis; Sinusitis; Sinonasal; Nasal; mixing an active topical medical agent with an isotonic saline solution Budesonide; Topical Steroid; Safety; Irrigations; Corticosteroid; followed by a low-pressure delivery into the nasal cavity using either a Effectiveness squeeze bottle or neti pot. -

The Effect of Dexamethasone on Chronic Pulmonary Oxygen Toxicity in Infant Mice
003 1-399818912504-0353$02.00/0 PEDIATRIC RESEARCH Vol. 25, No. 4, 1989 Copyright 0 1989 International Pediatric Research Foundation, Inc Printrd in G.S A The Effect of Dexamethasone on Chronic Pulmonary Oxygen Toxicity in Infant Mice N. OHTSU. R. L. ARIAGNO, T. E. SWEENEY, L. DAVIS, L. MOSES, R. PETRICEKS, I. DAEHNE, K. BENSCH, AND W. H. NORTHWAY, JK. De~~urtmcntsofRadiology, Pathology, Pediatrics, Stanfird University Medical Center, Stanbrd, Califhrnia 94305 ABSTRACT. The effect of dexamethasone (0.1, 1, and 5 ported in the clinical studies of Mammel et al. (1, 2) and Avery mg/kg/d given subcutaneously from d 14-18) was tested in et al. (3). infant mice continuously exposed from birth to either hu- midified air or 80% oxygen. Dexamethasone significantly decreased lung wet wt (p < 0.01), lung water (p < 0.021), METHODS lung dry wt, protein, and DNA (p < 0.001) in both air- Animal selection, environment, and drug administrution. In and oxygen-exposed animals. Dexamethasone, however, each experiment, two litters of naturally born C57BL mice were had no effect on lung compliance measured after animals weighed and sex identified within 24 h of birth. Natural litter were killed on d 18. It also had no effect on the increase in size was reduced to five by selecting the five animals with the the blood-air barrier thickness or decrease in the blood-air highest birth wt. Each of the five newborn mice was marked and exchange surface area seen in the 80% oxygen-exposed assigned a serial number which determined the treatment assign- mice. -

Maintenance Fluid Therapy with Saline, Dextrose-Supplemented Saline Or Lactated Ringer in Childhood: Short-Term Metabolic Effect
nutrients Article Maintenance Fluid Therapy with Saline, Dextrose-Supplemented Saline or Lactated Ringer in Childhood: Short-Term Metabolic Effects 1, 1,2,3, , 1 1 Alessandra Ricciuti y, Gregorio P. Milani * y , Silvia Tarantino , Roberta Ghilardi , Sebastiano A.G. Lava 4, Marco Alberzoni 2, Mario G. Bianchetti 5 and Carlo Agostoni 1,2,3 1 Pediatric Unit, Fondazione IRCCS Ca’ Granda Ospedale Maggiore Policlinico, 20122 Milan, Italy; [email protected] (A.R.); [email protected] (S.T.); [email protected] (R.G.); [email protected] (C.A.) 2 Department of Clinical Sciences and Community Health, Università degli Studi di Milano, 20122 Milan, Italy; [email protected] 3 Italian Society for Pediatric Gastroenterology Hepatology and Nutrition (SIGENP), 20126 Milan, Italy 4 Pediatric Cardiology Unit, Department of Pediatrics, Centre Hospitalier Universitaire Vaudois, and University of Lausanne, 1010 Lausanne, Switzerland; [email protected] 5 Università della Svizzera Italiana, 6900 Lugano, Switzerland; [email protected] * Correspondence: [email protected]; Tel.: +39-025-503-2266 These two authors equally contributed to the study. y Received: 29 March 2020; Accepted: 14 May 2020; Published: 17 May 2020 Abstract: Maintenance with isotonic fluids is recommended in children with gastroenteritis and failure of oral rehydration therapy. However, little is known on the short-term effects of the commonly prescribed intravenous solutions on metabolic balance in children. The aim of this study is to report on our experience with normal saline, dextrose-supplemented saline and lactated Ringer solution. Methods: A retrospective analysis from the charts of all previously apparently healthy children with acute gastroenteritis, mild to moderate dehydration and failure of oral rehydration, evaluated between January 2016 and December 2019 at our institution, was performed. -

Coagulation Effects of Mannitol in Combination with 0.9% Normal Saline Or Hydroxyethyl Starch in Patients Undergoing Supratentorial Craniotomy: a Preliminary Report
Original Article Coagulation effects of mannitol in combination with 0.9% normal saline or hydroxyethyl starch in patients undergoing supratentorial craniotomy: A preliminary report Hemanshu Prabhakar, Gyaninder Pal Singh, Parmod Kumar Bithal, Mani Kalaivani1 Abstract Background: Neurosurgical patients often require administration of both, mannitol and hydroxyethyl starch (HES). A recent in vitro study demonstrated that HES in combination with mannitol could disturb coagulation parameters and should be avoided in neurosurgical practice. The aim of our study was to evaluate coagulation abnormalities due to mannitol when administered alone and in combination with HES in patients undergoing craniotomy for various intracranial brain tumours. Materials and Methods: We enrolled 30 adult patients undergoing craniotomy. Patients were randomised into two groups using a computer generated randomisation chart. Interventions: Group A: Patients received 10 ml/kg 0.9% normal saline and 1 g/kg mannitol and Group B: Patients received 10 ml/kg, HES 130/0.4, and 1 gm/kg mannitol; immediately after induction of general anaesthesia. Rotational thromboelastography was done immediately after induction of general anaesthesia and 5 min after administration of mannitol. Measured parameters of blood coagulation were clotting time (CT) and clot formation time (CFT) with EXTEM and maximum clot firmness (MCF) with EXTEM and (FIBTEM). Results: Fourteen patients in each group completed the study. Insignificant change was noted in CT; CFT altered significantly from the baseline in both the groups (P < 0.05). MCF with FIBTEM did not change significantly from baseline (P > 0.05), but significantly differed between groups (P = 0.001). However, all values were in normal range. -

Physical Charaterization of Red Blood Cell Aggregation Daniel Amadeus Dominic Flormann
Physical charaterization of red blood cell aggregation Daniel Amadeus Dominic Flormann To cite this version: Daniel Amadeus Dominic Flormann. Physical charaterization of red blood cell aggregation. Biological Physics [physics.bio-ph]. Universität des Saarlandes, 2017. English. NNT : 2017GREAY002. tel- 01577838 HAL Id: tel-01577838 https://tel.archives-ouvertes.fr/tel-01577838 Submitted on 28 Aug 2017 HAL is a multi-disciplinary open access L’archive ouverte pluridisciplinaire HAL, est archive for the deposit and dissemination of sci- destinée au dépôt et à la diffusion de documents entific research documents, whether they are pub- scientifiques de niveau recherche, publiés ou non, lished or not. The documents may come from émanant des établissements d’enseignement et de teaching and research institutions in France or recherche français ou étrangers, des laboratoires abroad, or from public or private research centers. publics ou privés. THÈSE Pour obtenir le grade de DOCTEUR DE LA COMMUNAUTÉ UNIVERSITÉ GRENOBLE ALPES préparée dans le cadre d’une cotutelle entre la Communauté Université Grenoble Alpes et l’Universität des Saarlandes Spécialité : Physique pour les sciences du vivant Arrêté ministériel : 25 mai 2016 Présentée par Daniel Amadeus Dominic Flormann Thèse dirigée par M. Thomas Podgorski et M. Christian Wagner préparée au sein du Laboratoire Interdisciplinaire de Physique, Grenoble et de Experimentalphysik, Saarbrücken dans les Écoles doctorales de Physique de l’Université Grenoble Alpes et de Dekanat der Universität des Saarlandes -
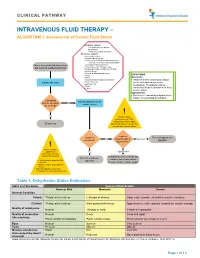
Intravenous Fluid Therapy – Algorithm 1
CLINICAL PATHWAY INTRAVENOUS FLUID THERAPY – ALGORITHM 1. Assessment of Overall Fluid Status Inclusion criteria: • All inpatients except those listed below • Patients pending admission Exclusion criteria: •Acute kidney injury •Chronic kidney disease •Endocrine or renal abnormalities leading to electrolyte derangements including DKA Patient who meets inclusion criteria •Oncology treatment protocol •Patients less than 30 days of age, and warrants supplemental fluids Including premature infants corrected for gestational age •Increased intracranial pressure •PICU DEFINITIONS •NICU Euvolemic: •Total Parenteral Nutrition dependent • Patient is at their ideal volume status Obtain vital signs •Pyloric Stenosis (neither dehydrated nor volume •Burn patients overloaded). The patient requires •Shock •Codes intravenous fluids to maintain their ideal volume status. Hypovolemic: • Patient is at least mildly dehydrated (see Table 1 for estimating dehydration) Can patient Assess patient’s current tolerate adequate No volume status enteral fluids? ! Yes Volume status assessment is 100% clinical. Do not rely upon Off pathway laboratory values to determine the patient’s volume status. Is patient Is patient Refer to hypovolemic No hypervolemic or Hypovolemic euvolemic? algorithm hypovolemic? ! Prior to starting a patient on Yes Hypervolemic maintenance IV fluids, consider the following: Reassess need for IV fluids and Refer to euvolemic consider issues with oncotic • Risk factors for abnormal ADH algorithm secretion pressure and/or cardiac output • Initial -

Hypertonic Saline (7.2%) in 6% Hydroxyethyl Starch Reduces Intracranial Pressure and Improves Hemodynamics in a Placebo-Controll
Continuing Medical Education Article Hypertonic saline (7.2%) in 6% hydroxyethyl starch reduces intracranial pressure and improves hemodynamics in a placebo-controlled study involving stable patients with subarachnoid hemorrhage* Gunnar Bentsen, MD; Harald Breivik, MD, DMSc, FRCA; Tryggve Lundar, MD, DMSc; Audun Stubhaug, MD, DMSc LEARNING OBJECTIVES On completion of this article, the reader should be able to: 1. Describe the effects of hypertonic saline (7.2% saline in 6% hydroxyethyl starch 200/0.5) on intracranial pressure. 2. Compare the effects of hypertonic with normal saline on cerebral perfusion pressure. 3. Use this information in a clinical setting. All authors have disclosed that they have no financial relationships with or interests in any commercial companies pertaining to this educational activity. Lippincott CME Institute, Inc., has identified and resolved all faculty conflicts of interest regarding this educational activity. Visit the Critical Care Medicine Web site (www.ccmjournal.org) for information on obtaining continuing medical education credit. Objective: To compare the effects of a bolus infusion of hyper- was ؊5.6 (range, ؊0.8 to ؊12.2) mm Hg after 64 (range, 40 to tonic saline hydroxyethyl starch with the effects of normal saline 115) mins. Mean difference in cerebral perfusion pressure change placebo) on intracranial pressure (ICP) and cerebral perfusion pres- between the groups (HSS ؊ normal saline) was 5.4 mm Hg (95%) and mean difference in ,(002. ؍ sure in patients with spontaneous subarachnoid hemorrhage. confidence interval, 2.2 to 8.6; p Design and Setting: Prospective, randomized, single-blinded, cardiac index change, measured as the area under the curve for placebo-controlled study in a university hospital.